Small Bowel Obstruction
description
Transcript of Small Bowel Obstruction

An unusual cause An unusual cause of small bowel of small bowel obstruction…obstruction…
Senior Clinicopathologic Senior Clinicopathologic ConferenceConference
Andrew S Kim, MDAndrew S Kim, MDApril 23, 2008April 23, 2008
Walter Reed Army Medical CenterWalter Reed Army Medical Center

History of Present IllnessHistory of Present Illness
49 y/o white male49 y/o white male Local to Landstuhl HospitalLocal to Landstuhl Hospital Presents to the ED with c/o acute onset Presents to the ED with c/o acute onset
N/V and worsening abdominal painN/V and worsening abdominal pain Intermittent abd pain x 1 weekIntermittent abd pain x 1 week ROS: Nausea, (+) bilious vomiting, ROS: Nausea, (+) bilious vomiting,
abdominal distensionabdominal distension

History of Present IllnessHistory of Present Illness
Recent trauma “pinned” between car and Recent trauma “pinned” between car and a tree 4-5 months priora tree 4-5 months prior
Diagnosis of CMML-2 at LandstuhlDiagnosis of CMML-2 at Landstuhl Discovered during workup of Discovered during workup of
thrombocytopenia for herniathrombocytopenia for hernia Diagnosis confirmed by both AFIP and Diagnosis confirmed by both AFIP and
Dana-Farber Cancer InstituteDana-Farber Cancer Institute

Other Past Medical/Surgical Other Past Medical/Surgical HistoryHistory
Benign Prostatic HypertrophyBenign Prostatic Hypertrophy Right ACL Repair ‘06 Right ACL Repair ‘06 Right Inguinal Hernia repair ‘05Right Inguinal Hernia repair ‘05 NKDANKDA Not currently taking any medicationsNot currently taking any medications

Social HistorySocial History
Lifetime nonsmoker, nondrinkerLifetime nonsmoker, nondrinker Retired Air Force LTC Retired Air Force LTC Remote travel hxRemote travel hx

Physical ExamPhysical Exam
Vitals: afebrile bp 130/80 hr 98 rr 20 Pox Vitals: afebrile bp 130/80 hr 98 rr 20 Pox 94% RA94% RA
GEN: moderate distress, WDWN, physically fit GEN: moderate distress, WDWN, physically fit WMWM
CV: normal, no MRGCV: normal, no MRG Pulm: clear to auscultation bilaterallyPulm: clear to auscultation bilaterally Ab: marked abdominal distension with midline Ab: marked abdominal distension with midline
abdominal fullness, mild tenderness to abdominal fullness, mild tenderness to palpation, decreased bowel sounds throughoutpalpation, decreased bowel sounds throughout
Lymph: no abnormalities notedLymph: no abnormalities noted

Labs/Path ReportsLabs/Path Reports Previous Labwork Previous Labwork
(11/06)(11/06) 4.94.9>12.7/38<92>12.7/38<92
50S/50S/33M33M; ; (AMC (AMC 1600)1600)
BMP normalBMP normal TP/Albumin normalTP/Albumin normal BCR-ABL (-)BCR-ABL (-) t(5; 12) (-)t(5; 12) (-)
ESR 6, CRP normalESR 6, CRP normal AFIP/Dana-Farber AFIP/Dana-Farber
report: CMML-2report: CMML-2
Admission Labwork Admission Labwork (3/07)(3/07) 7>9.7/29.4<1107>9.7/29.4<110
41S/54M 41S/54M (AMC (AMC 3600)3600)
140/3.7/106/26/25/140/3.7/106/26/25/0.90.9
TP/Albumin TP/Albumin 4.5/2.54.5/2.5 LFTs normalLFTs normal Coags normalCoags normal

Initial Hospital CourseInitial Hospital Course
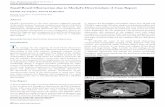
CT A/P: high grade obstruction in 3CT A/P: high grade obstruction in 3rdrd part part of the duodenumof the duodenum
Exploratory Laporotomy: Exploratory Laporotomy: Large inflammatory “tumor-like” mass Large inflammatory “tumor-like” mass
along entire base of mesentery with along entire base of mesentery with significant encasement of small bowelsignificant encasement of small bowel
OR report describes mass as tan OR report describes mass as tan colored, studded “glue-like” consistency colored, studded “glue-like” consistency of lesionof lesion

Initial Hospital CourseInitial Hospital Course
Initial path report and frozen sections not Initial path report and frozen sections not representative of malignant cells but representative of malignant cells but large “acute and chronic” inflammatory large “acute and chronic” inflammatory infiltrateinfiltrate
Intraoperative G- and J-tube placedIntraoperative G- and J-tube placed Transferred to WRAMC General surgery Transferred to WRAMC General surgery
serviceservice Continued intermittent, persistent Continued intermittent, persistent
obstructive sxobstructive sx GI, Heme-Onc consultsGI, Heme-Onc consults

Initial Hospital CourseInitial Hospital Course
Transferred from Gen Sg to Medicine Transferred from Gen Sg to Medicine wards due to improvement in his sxwards due to improvement in his sx
Treatment with high-dose steroids Treatment with high-dose steroids continuedcontinued
Meanwhile, tissue results from his ex-lap Meanwhile, tissue results from his ex-lap came back as well as BM Bx and came back as well as BM Bx and peripheral smear slides performed at peripheral smear slides performed at LRMCLRMC

Tissue slides and BM biopsy:Tissue slides and BM biopsy:
Dr. Jean KempDr. Jean KempDepartment of PathologyDepartment of Pathology
Walter Reed Army Medical Center Walter Reed Army Medical Center

Mesenteric Panniculitis Mesenteric Panniculitis 2x2x

Mesenteric Panniculitis Mesenteric Panniculitis 20x20x

Mesenteric Panniculitis Mesenteric Panniculitis 40x40x

CMML 2xCMML 2x

CMML 10xCMML 10x

CMML 20xCMML 20x

CMML 40xCMML 40x

CMML 100xCMML 100x

Summary Biopsy Results:Summary Biopsy Results:
Mesenteric Panniculitis slidesMesenteric Panniculitis slides atypical histiocytic infiltrate with mixed atypical histiocytic infiltrate with mixed
inflammatory cells, consistent with inflammatory cells, consistent with mesenteric panniculitis (AFIP)mesenteric panniculitis (AFIP)
CMMLCMML Diagnosis of CMML-1 vs CMML-2Diagnosis of CMML-1 vs CMML-2 (Confirmed by Dana-Farber cancer (Confirmed by Dana-Farber cancer
institute)institute)

Mesenteric Panniculitis: Mesenteric Panniculitis: DefinitionDefinition
Synonyms: Synonyms: sclerosing mesenteritissclerosing mesenteritis mesenteric lipodystrophy mesenteric lipodystrophy lipogranuloma of the mesenterylipogranuloma of the mesentery sclerosing lipogranulomatosissclerosing lipogranulomatosis primary liposclerosis of the mesentery primary liposclerosis of the mesentery
and multifocal subperitoneal sclerosisand multifocal subperitoneal sclerosis

Mesenteric Panniculitis: Mesenteric Panniculitis: EpidemiologyEpidemiology
Epidemiology: rare with no “true Epidemiology: rare with no “true epidemiology”epidemiology” Prevalence~1%Prevalence~1%
Age: 50-70s Age: 50-70s Male:Female 2:1Male:Female 2:1

Mesenteric Panniculitis: Mesenteric Panniculitis: EtiologiesEtiologies88
Infection or ischemiaInfection or ischemia Based on animal models, isolated case Based on animal models, isolated case
reportsreports Autoimmune causesAutoimmune causes
Thyroid disorders, AI pancreatitis, SLE, RPCThyroid disorders, AI pancreatitis, SLE, RPC Trauma/Surgery relatedTrauma/Surgery related
AFIP seriesAFIP series88
Paraneoplastic causesParaneoplastic causes Often the presenting complaintOften the presenting complaint
Largely only case reports and retrospectiveLargely only case reports and retrospective Poorly defined pathophysiologyPoorly defined pathophysiology

Mesenteric Panniculitis: Mesenteric Panniculitis: PresentationPresentation
Most common presenting sxMost common presenting sx1-31-3:: Abdominal pain (70%)Abdominal pain (70%) Diarrhea (25%)Diarrhea (25%) Wt loss (23%)Wt loss (23%) Small Bowel obstruction (24-36%)Small Bowel obstruction (24-36%)
Physical Exam with LUQ or epigastric Physical Exam with LUQ or epigastric mass in up to 50% of ptsmass in up to 50% of pts33
Labs usually normalLabs usually normal

Mesenteric Panniculitis: Mesenteric Panniculitis: DiagnosisDiagnosis
Differential Diagnosis includes all Differential Diagnosis includes all diseases of the mesenterydiseases of the mesentery
Combination of clinical hx and Combination of clinical hx and presentation, radiology and histology presentation, radiology and histology neededneeded

Mesenteric Panniculitis: Mesenteric Panniculitis: RadiologyRadiology
CT imaging : usually with findings of small CT imaging : usually with findings of small bowel mesenteric inflammatory processbowel mesenteric inflammatory process ““fat ring” sign and “tumor fat ring” sign and “tumor
pseudocapsule” somewhat specificpseudocapsule” somewhat specific4,54,5
MRI emerging as a potentially useful toolMRI emerging as a potentially useful tool66
presence of fibrous capsule not seen in presence of fibrous capsule not seen in other disease processesother disease processes
PET scan?PET scan?77
Mucosal preservation is a key difference Mucosal preservation is a key difference between mesenteric panniculitis and other between mesenteric panniculitis and other malignant processesmalignant processes

Mesenteric Panniculitis: Mesenteric Panniculitis: HistologyHistology
Most common findings: fibrous tissue, Most common findings: fibrous tissue, chronic inflammationchronic inflammation
Flow cytometry may be utilized if Flow cytometry may be utilized if lymphoma cannot be excluded on lymphoma cannot be excluded on histologic evaluationhistologic evaluation
Immunohistochemistry may be useful in Immunohistochemistry may be useful in determining GIST and mesenteric determining GIST and mesenteric fibromatosis from MPfibromatosis from MP

Mesenteric Panniculitis: Mesenteric Panniculitis: PrognosisPrognosis
Natural history not well understood Natural history not well understood Generally felt to be benign courseGenerally felt to be benign course Some trends noted in the literatureSome trends noted in the literature4-84-8
Idiopathic cases tend to have more Idiopathic cases tend to have more favorable prognosisfavorable prognosis
Patients who develop intestinal Patients who develop intestinal obstruction have worse prognosisobstruction have worse prognosis
Patients with underlying malignancy Patients with underlying malignancy have the worst prognosishave the worst prognosis

Mesenteric Panniculitis: Mesenteric Panniculitis: TreatmentTreatment7-107-10
No universally recognized standard of careNo universally recognized standard of care MEDICAL THERAPYMEDICAL THERAPY
Steroids: most used in literatureSteroids: most used in literature Tamoxifen, ProgesteroneTamoxifen, Progesterone ColchicineColchicine AzathioprineAzathioprine ThalidomideThalidomide CytoxanCytoxan
OTHER THERAPIESOTHER THERAPIES Radiation therapy not usefulRadiation therapy not useful Surgical role limitedSurgical role limited

Mesenteric Panniculitis: Mesenteric Panniculitis: Cause?Cause?
Trauma/Surgery relatedTrauma/Surgery related IschemiaIschemia Infectious causesInfectious causes Autoimmune causesAutoimmune causes Paraneoplastic causesParaneoplastic causes

What’s left?What’s left? Recent TraumaRecent Trauma InfectiousInfectious AutoimmuneAutoimmune ParaneoplasticParaneoplastic
Prior history of CMML-2 (more Prior history of CMML-2 (more aggressive form of CMML)aggressive form of CMML)
No other malignant processes identifiedNo other malignant processes identified

Chronic Myelomonocytic Chronic Myelomonocytic Leukemia: CMMLLeukemia: CMML
Dr. Michael Marte/Dr. Andre Cap Dr. Michael Marte/Dr. Andre Cap Department of Hematology-OncologyDepartment of Hematology-Oncology
Walter Reed Army Medical CenterWalter Reed Army Medical Center

CMML - A Disease in the Shadows
Clonal hematopoietic progenitor cell defect Occupies the nexus between MDS and MPD
Features of both, but consistent with neither Represents an epidemiologic difficulty
Many grouped with CML or with MDSAccounts for as much as 13% of “MDS”
Median age: 65-75 years Male: Female ratio 1.5-3:1

The Faces of CMML Clinically either MDS-like, or MPD-like
(MPD) - proliferative: dysplastic megakaryocytes (MDS) - marrow failure: anemia, thrombocytopenia
Diagnostic criteria: < 20% marrow blasts, < 5% peripheral blasts
otherwise MDS (RAEB-1 vs. RAEB-2) Absolute peripheral monocyte count > 1,000/μL for
3 months BCR/ABL negative WBC count?
If < 12,000/μL -> MDS; If > 12,000 -> MPD Cases split roughly evenly
Variable cytogenetics, essentially unhelpful

The Faces of CMML Similar to RAEB-1, RAEB-2 classification
CMML-1Marrow blasts < 10%Peripheral blasts < 5%
CMML-2Marrow blasts 10-19%Peripheral blasts 5-19%AUER rods and < 20% peripheral or
marrow blasts Progression to AML difficult to quantify, but
not uncommon

Diagnosis of CMML Differential diagnosis
CML BCR/ABL-negative MPDs MDS Chronic eosinophilic/neutrophilic leukemia
Helpful diagnostic strategies: BCR/ABL: most sensitive – PCR peripheral
blood Bone marrow biopsy with flow cytometry
CD4, 14, 43, 56, 68 positive and characteristic
Peripheral smear: Leukoerythroblastic appearance

CMML - Presentation Fatigue, fever, night sweats, weight loss Cytopenias
Infection: relative neutropenia Bleeding
Extramedullary hematopoiesis/leukemic infiltration Spleen, liver, skin, lymph nodes,
pulmonary parenchyma Splenomegaly/hepatomegaly in
proliferative disease

CMML - Treatments Hyperproliferative -> cytoreduce
Hydroxyurea is preferred agent Ara-C, etoposide, topotecan are second-line
Hypoproliferative Transfusions as needed Growth factor support if:
serum erythropoietiv < 500 mU/mL Fewer than 2 units PRBCs transfused per
month Hypomethylating agents
Decitabine, Azacitidine

CMML and TKIs Myeloproliferative CMML
Balanced translocations with resultant aberrant kinase activityTEL-PDGFRβ receptor
CMML-like disease in murine models Inhibited by SU11657 TKI (multi-kinase
inhibitor)TEL-Jak2 t(5;12)
Usually with pronounced eosinophilia 102% of CMML cases Responsive to Gleevec

Transplant
Represents the only curative option in CMML Preferentially reduce blast count prior to
transplant Allogeneic transplant preferred
GVL effect Minimal data with RIC transplantation 3Y DFS–39% (FHCRC), 5Y DFS– 18%(EBMT)
TRM as high as 52% Possibly improved in patients transplanted
early

Now back to our Now back to our patient…patient…

Subsequent Hospital Subsequent Hospital CourseCourse
Pt continued to require high dose steroidsPt continued to require high dose steroids Worsening malnutrition and persistent Worsening malnutrition and persistent
obstructive sxobstructive sx MICU transfers (multiple)MICU transfers (multiple)
Upper GI bleed, multiple episodesUpper GI bleed, multiple episodes Gram negative sepsis requiring MICU Gram negative sepsis requiring MICU
carecare Lactate >10Lactate >10
Daily high fevers to 103-104 continued Daily high fevers to 103-104 continued throughoutthroughout

Subsequent Hospital Subsequent Hospital CourseCourse
Discussions with patient and family Discussions with patient and family regarding potential therapeutic optionsregarding potential therapeutic options CTX versus bone marrow transplantCTX versus bone marrow transplant
Multiple conference calls CMML experts Multiple conference calls CMML experts at the Mayo Clinic in Rochester, at the Mayo Clinic in Rochester, MinnesotaMinnesota
Transferred to Mayo after 8 weeks of Transferred to Mayo after 8 weeks of inpatient care at Walter Reed Army inpatient care at Walter Reed Army Medical CenterMedical Center

The Mayo ClinicThe Mayo Clinic Initially offered “7+3” or decitabine for Initially offered “7+3” or decitabine for
CMML-2CMML-2 Received one course of EtoposideReceived one course of Etoposide
10 days into his hospital course there pt 10 days into his hospital course there pt experienced an acute clinical decline with experienced an acute clinical decline with neutropenia, fever, and hemodynamic neutropenia, fever, and hemodynamic collapse and deathcollapse and death Bone marrow biopsy repeated on Bone marrow biopsy repeated on
transfer with evidence of transfer with evidence of hemophagocytosishemophagocytosis

The Mayo ClinicThe Mayo Clinic ““Hemophagocytic Hemophagocytic
Syndrome” Syndrome” ((Hemophagocytic Hemophagocytic
lymphohistiocytosis)lymphohistiocytosis) Fever, HSMG, Fever, HSMG,
cytopenias and cytopenias and evidence of evidence of hemophagocytosihemophagocytosis on bone marrow s on bone marrow by macrophages, by macrophages, spleen or LN spleen or LN biopsybiopsy
www.healthsystem.virginia.edu/internet/hematology

Acknowledgements/QuestionsAcknowledgements/Questions
- Dr Marte/Dr Cap: WRAMC Heme-Onc- Dr Marte/Dr Cap: WRAMC Heme-Onc- Dr Kemp/Dr Schaffer: WRAMC Pathology- Dr Kemp/Dr Schaffer: WRAMC Pathology- Dr Fadell/Labovich: LRMC Dr Fadell/Labovich: LRMC
Heme-Onc/PathologyHeme-Onc/Pathology- Dr Rosco Gore: WRAMC IMDr Rosco Gore: WRAMC IM

ReferencesReferences
1. 1. Khachaturian, T, Hughes, J. Mesenteric panniculitis. West J Med 1988; Khachaturian, T, Hughes, J. Mesenteric panniculitis. West J Med 1988; 148:700148:700
2. Durst, AL, Freund, H. Mesenteric Pannicluitis: review of the literature. 2. Durst, AL, Freund, H. Mesenteric Pannicluitis: review of the literature. Surgery 1977; 81: 203.Surgery 1977; 81: 203.
3. Akram, S, Pardi, DS, et al. Sclerosing mesenteritis: clinical features, 3. Akram, S, Pardi, DS, et al. Sclerosing mesenteritis: clinical features, treatment, and outcomes in ninety-two patients. Clin Gastro Hepatol 2007; 5: treatment, and outcomes in ninety-two patients. Clin Gastro Hepatol 2007; 5: 589.589.
4. Horton, KM, Lawler, LP, et al. CT findings in sclerosing mesenteritis 4. Horton, KM, Lawler, LP, et al. CT findings in sclerosing mesenteritis (panniculitis): Spectrum of disease. Radiographics 2003; 23: 1561.(panniculitis): Spectrum of disease. Radiographics 2003; 23: 1561.
5. Sabate, JM, Torrubia, et al. Sclerosing mesenteritis: imaging findings in 5. Sabate, JM, Torrubia, et al. Sclerosing mesenteritis: imaging findings in seventeen patients. AJR Am J Roentgenol 1999; 172: 625.seventeen patients. AJR Am J Roentgenol 1999; 172: 625.
6. Emory, TS, Monihan JM, Carr, NJ, et al. Sclerosing mesenteritis, mesenteric 6. Emory, TS, Monihan JM, Carr, NJ, et al. Sclerosing mesenteritis, mesenteric panniculitis and mesenteric lipodystrophy: A single entity? Am J Surg Pathol panniculitis and mesenteric lipodystrophy: A single entity? Am J Surg Pathol 1997; 21: 392. 1997; 21: 392.
7. Ogden, WW, Bradburn, DM. Mesenteric Panniculitis: Review of twenty-seven 7. Ogden, WW, Bradburn, DM. Mesenteric Panniculitis: Review of twenty-seven cases. Ann Surg 1965; 161: 184. cases. Ann Surg 1965; 161: 184.
8. Bala, A, Coderre, SP et al. Treatment of sclerosing mesenteritis with 8. Bala, A, Coderre, SP et al. Treatment of sclerosing mesenteritis with corticosteroids and azathioprine. Can J Gastroent 2001; 15: 533.corticosteroids and azathioprine. Can J Gastroent 2001; 15: 533.
9. Genereau, T, Bellin, MF, et al. Demonstration of efficacy of combining 9. Genereau, T, Bellin, MF, et al. Demonstration of efficacy of combining steroids and colchicine in two patients with idiopathic sclerosing steroids and colchicine in two patients with idiopathic sclerosing mesenteritis. Dig Dis Sci 1996; 41: 684.mesenteritis. Dig Dis Sci 1996; 41: 684.
10. www.uptodateonline.com10. www.uptodateonline.com