Small bowel obstruction secondary to mobile phone ... Journal … · Small bowel obstruction...
Transcript of Small bowel obstruction secondary to mobile phone ... Journal … · Small bowel obstruction...

International Journal of Case Reports and Images, Vol. 10, 2019. ISSN: 0976-3198
Int J Case Rep Images 2019;10:101080Z01AN2019. www.ijcasereportsandimages.com
Naughton et al. 1
CASE REPORT PEER REVIEWED | OPEN ACCESS
Small bowel obstruction secondary to mobile phone ingestion: A minimally invasive approach to retrieval
Ailish Patricia Naughton, Darren Patrick Moloney, Michael Boland, Dara Kavanagh
ABSTRACT
We describe the case of a 34-year-old gentleman who was admitted with a two-day history of colicky abdominal pain and constipation. This developed seven days after the patient ingested a mobile telephone while on temporary release from prison. Computed tomography of his abdomen and pelvis (CT AP) showed distal small bowel obstruction without perforation due to an intraluminal foreign body. Due to the location of the telephone and the patient’s symptoms operative management was deemed necessary. The patient was explored laparoscopically and the involved segment was exteriorized. An enterotomy was performed to retrieve the phone in a similar manner to the management of a gallstone. His postoperative course was uncomplicated and he was discharged home after five days.
Keywords: Enterotomy, Foreign body, Obstruc-tion
How to cite this article
Naughton AP, Moloney DP, Boland M, Kavanagh D. Small bowel obstruction secondary to mobile phone ingestion: A minimally invasive approach to retrieval. Int J Case Rep Images 2019;10:101080Z01AN2019.
Ailish Patricia Naughton1, Darren Patrick Moloney1, Michael Boland1, Dara Kavanagh1
Affiliation: 1Tallaght University Hospital, Dublin 24, Ireland.Corresponding Author: Dr. Ailish Patricia Naughton, Tallaght University Hospital, Dublin 24, Ireland; Email: [email protected]
Received: 29 September 2019Accepted: 28 November 2019Published: 26 December 2019
Article ID: 101080Z01AN2019
*********
doi: 10.5348/101080Z01AN2019CR
INTRODUCTION
Foreign body ingestion is an uncommon cause of an acute abdomen in adults. Although relatively common in children, in adults it is a rarer presentation [1]. Approximately 80% of ingested foreign bodies pass through the gastrointestinal (GI) tract without any complication [2–5]. Endoscopic retrieval is a viable option in 10–20% of cases [5], but largely depends on whether it is amenable to retrieve the foreign body in this way, for example, direct laryngoscopy may be an option in pharyngeal foreign bodies whereas oesophagogastroduodenoscopy (OGD) may be useful in the retrieval of foreign bodies in the distal foregut. Typically, less than 1% of cases require surgical intervention [1], usually if bowel obstruction or pneumoperitoneum is present. There are no clear guidelines on surgical management of foreign bodies causing obstruction of the small bowel, therefore management varies on the clinical scenario, clinician preference, and, to a certain degree, patient’s wishes. The prisoner population has higher rates of intentionally ingested foreign bodies than the general population [6, 7]. There is also a higher risk of foreign body ingestion requiring endoscopic or surgical intervention in the prisoner population. This is thought to be largely as a result of intentional ingestion of harmful objects [8, 9].
CASE REPORT
A 34-year-old man ingested a mobile phone while on temporary release from prison. Five days later he began to develop acute severe periumbilical abdominal pain. This was associated with constipation, although he was passing small amounts of flatus. He vomited multiple times. He alerted prison officers to his ingestion of the phone and was transferred to his local hospital where he

International Journal of Case Reports and Images, Vol. 10, 2019. ISSN: 0976-3198
Int J Case Rep Images 2019;10:101080Z01AN2019. www.ijcasereportsandimages.com
Naughton et al. 2
underwent initial management and investigation and was later transferred to a tertiary referral unit for definitive management.
His medical history was significant for previous open appendicectomy in childhood. He had no history of previous foreign body ingestion. He denied thoughts of self-harm, grandiose delusions, and auditory hallucinations. He had no previous psychiatric history or psychiatric admissions. He denied previous history of drug abuse. He was a current smoker with a 20 pack-year history.
On examination in the emergency department, he was found to have suprapubic and periumbilical tenderness with mild distension. He did not have signs of localized peritonism. He was vitally stable except for a mild tachycardia at 94 beats per minute.
InvestigationsLactate was within normal range at 1.4 mmol/L. His
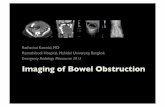
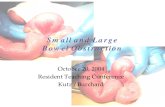
white cell count was mildly elevated at 11.48 × 109/L, predominantly a neutrophilia of 9.56 × 109/L. All other blood tests were within normal reference ranges. Plain film abdomen indicated a foreign body in the lower abdomen (Figure 1). There was no free air visible under the diaphragm on chest X-ray. Computed tomography of the abdomen and pelvis (CT AP) showed a distal small bowel obstruction with strong suspicion for transition point at the site of the ingested mobile phone level in the distal small bowel located within the pelvis (Figures 2 and 3). The phone was described as being located in the midline, anterior to the sacral promontory, within the distal small bowel. The ileum was collapsed distal to this point. There were no signs perforation or intra-abdominal collection.
Differential DiagnosisGiven the patient’s clinical picture and radiological
findings, the patient was diagnosed with a small bowel obstruction secondary to foreign body ingestion. It was decided that the patient should be transferred to the tertiary referral center for ongoing management of his condition with a view to definitive surgical management the next day.
TreatmentDue to the location of the phone in the distal small
bowel, an attempt at endoscopic retrieval was not a viable option. Conservative management was deemed inappropriate due to both the clinical presentation of the patient with abdominal tenderness and the finding of distal small bowel obstruction on CT AP. The decision was therefore made to proceed with surgical retrieval of the phone. It was decided to manage the case similar to that of a gallstone ileus. Following informed consent the patient was transferred to the operating room for emergency exploration.
The patient underwent general anesthetic and was placed in supine position. A single 1.2 g dose of amoxicillin/clavulanic acid was given at induction. A longitudinal 10 mm port site was sited inferior to umbilicus via the Hasson technique. Two additional 5 mm ports were placed in the left iliac fossa and left flank under direct vision. Initial intraperitoneal findings showed dilated and decompressed small bowel loops. The cecum, appendiceal stump, and terminal ileum were identified in the right iliac fossa. Starting at the
Figure 1: Plain film of abdomen highlighting foreign body. (A) Dilated loops of jejunum. (B) Mobile phone.
Figure 2: Sagittal cut from CT abdomen and pelvis highlighting foreign body. (C) Mobile phone.

International Journal of Case Reports and Images, Vol. 10, 2019. ISSN: 0976-3198
Int J Case Rep Images 2019;10:101080Z01AN2019. www.ijcasereportsandimages.com
Naughton et al. 3
terminal ileum, a small bowel walk was performed in order to locate the mobile phone. The mobile phone was found in the distal jejunum. There was a clear transition from dilated to collapsed small bowel. Overlying bowel appeared edematous, however, there were no signs of necrosis or perforation. Two noncrushing bowel graspers were placed both distal and proximal to the foreign body. The infraumbilical port site was converted into a 3 cm lower midline mini laparotomy. An AlexisTM (Applied Medical, CA, USA) wound protector was deployed. The bowel containing the foreign body was delivered through the laparotomy site. A longitudinal isoperistaltic enterotomy on the antimesenteric surface of the bowel was formed to facilitate retrieval of the phone. The phone was found to measure approximately 6 × 1.5 cm and was wrapped in plastic (Figures 4 and 5). Due to the healthy appearance of the distal bowel, primary transverse closure of the enterotomy was carried out in two layers with continuous mucosal 3/0 vicryl and interrupted seromuscular 3/0 Maxon sutures. The fascia was closed with round body 0 loop Maxon and skin was closed with 4/0 Monocryl. Twenty milliliters of
Figure 3: Coronal cut from CT abdomen and pelvis highlighting dilated proximal bowel loops. (D) Dilated jejunum.
Figure 4: Computed tomography three dimensional reconstruction showing foreign body anterior to pelvic promontory. (E) Mobile phone.
Figures 5(A and B): Intraoperative medical photography.
0.25% bupivacaine were administered at the port sites. There were no intraoperative complications and the patient returned to the ward to complete his recovery.
Outcome and Follow-upThe patient received standard postoperative
intravenous antimicrobial prophylaxis. Mechanical and pharmacological thromboprophylaxis were administered. His diet was incremented gradually over the initial three days. He was noted to have passed a bowel motion on day 2 postoperatively. The patient had an uncomplicated postoperative course and was discharged back to prison five days after his operation. He was followed up in the clinic as an outpatient and was found to be very well. He was subsequently discharged from the surgical unit.

International Journal of Case Reports and Images, Vol. 10, 2019. ISSN: 0976-3198
Int J Case Rep Images 2019;10:101080Z01AN2019. www.ijcasereportsandimages.com
Naughton et al. 4
DISCUSSION
Foreign body ingestion most commonly occurs in children, the elderly, those with psychiatric conditions or intellectual disability and prisoners [1]. A distinction should be made between accidental and intentional ingestion on presentation, as there is a relatively higher morbidity in intentional versus accidental ingestion [10]. Intentional ingestion of foreign objects is more common in the prison population than the general population [6, 7, 11]. This is hypothesized to be due to undiagnosed psychiatric disorders, impulsivity or potential secondary gain (e.g., transfer from a prison to a hospital). Most foreign bodies ingested by the general population will pass through the GI tract without any complication besides minor mucosal injury [5, 12]. Most complications occur at sites of physiological or pathological narrowing. Between 10% and 20% of cases will require endoscopy, and less than 1% of cases will develop complications requiring surgical intervention [1]. It has been shown that there are higher rates of surgical or endoscopic intervention required in the prison population who ingest foreign bodies, with up to 30% of patients requiring surgical intervention [13–15]. Of note a number of psychiatric diagnoses are associated with intentional foreign body ingestion, most commonly psychosis, pica, malingering, and personality disorders [16]. Therefore a psychiatric evaluation should be considered in patients presenting in this way.
Initial management depends on the type of foreign body that has been ingested and whether or not the patient is stable. High risk objects include those with sharp edges, objects greater than 6 × 2.5 cm, objects containing lead, or magnets swallowed along with a metal object. Any patient with a preexisting GI abnormality should also be classified as high risk [17]. Once the nature of the object has been determined, imaging should be done to assess its location. Most foreign bodies that pass through the pylorus will pass to the rectum without further complication [10]. The case we describe was unusual in that the mobile phone passed the pylorus before causing obstruction in the distal small bowel. Although a number of guidelines exist for endoscopic management of ingested foreign bodies, there are no such guidelines for the surgical management of foreign bodies in the small bowel. Therefore, management of such cases varies on a case by case basis.
Due to the location of the foreign body in this case, the decision was made to approach the surgical removal of the phone similarly to the management of a gallstone ileus. Gallstone ileus is defined as mechanical intestinal obstruction secondary to the impaction of one or more gallstones within the GI tract. The most common site of obstruction due to gallstone ileus is in the distal ileum [18]. Treatment generally involves an enterotomy with gallstone retrieval initially, which is followed in some cases by immediate or delayed repair of the fistula. The removal of the isolated gallstone by laparoscopy,
combined with a mini laparotomy was first described by Montgomery in 1993 [19]. This technique was further described by Moberg et al. and Yang et al. [20, 21]. In the setting of obstruction due to gallstone ileus, there has been reports of high conversion rates due to the degree of obstruction and lack of view [21]. Early recovery and low mortality are cited as a benefit of this laparoscopic approach similar to the current case [22]. Of note, in the case we describe the enterotomy was formed distal to the site of obstruction. This decision was made as the distal bowel was nonedematous and healthy. The obstruction was in the distal jejunum with healthy bowel present distal to this point. In contrast, in cases of gallstone ileus the enterotomy is usually performed proximal or at the site of obstruction. This is perhaps due to the terminal ileum being the most common site of impaction with a risk of encroaching on the ileocecal valve if closing a distal enterotomy [18].
CONCLUSION
1. Management of foreign body ingestion should be determined by the type of foreign body ingested, clinical findings, subjective symptoms, and foreign body location. There are no published guidelines on postpyloric obstruction secondary to foreign body.
2. Management of postpyloric small bowel obstruction may be managed in a similar manner to gallstone ileus.
3. The prisoner population is at higher risk of requiring endoscopic or surgical intervention after ingestion of a foreign body.
4. Intentional foreign body ingestion may be a presentation of an undiagnosed psychiatric disorder, such as psychosis, pica, malingering, and personality disorders. Psychiatric evaluation may be warranted in these cases.
5. The use of laparoscopic exploration described in this case allow for early mobilization, minimal postoperative analgesia, and early discharge from a hospital setting.
REFERENCES
1. Sung SH, Jeon SW, Son HS, et al. Factors predictive of risk for complications in patients with oesophageal foreign bodies. Dig Liver Dis 2011;43(8):632–5.
2. Wyllie R. Foreign bodies in the gastrointestinal tract. Curr Opin Pediatr 2006;18(5):563–4.
3. Uyemura MC. Foreign body ingestion in children. Am Fam Physician 2005;72(2):287–91.
4. Shivakumar AM, Naik AS, Prashanth KB, Yogesh BS, Hongal GF. Foreign body in upper digestive tract. Indian J Pediatr 2004;71(8):689–93.
5. Pavlidis TE, Marakis GN, Triantafyllou A, Psarras K, Kontoulis TM, Sakantamis AK. Management of ingested foreign bodies. How justifiable is a waiting policy? Surg Laparosc Endosc Percutan Tech 2008;18(3):286–7.

International Journal of Case Reports and Images, Vol. 10, 2019. ISSN: 0976-3198
Int J Case Rep Images 2019;10:101080Z01AN2019. www.ijcasereportsandimages.com
Naughton et al. 5
6. Blaho KE, Merigian KS, Winbery SL, Park LJ, Cockrell M. Foreign body ingestions in the Emergency Department: Case reports and review of treatment. J Emerg Med 1998;16(1):21–6.
7. Appelbaum KL, Savageau JA, Trestman RL, Metzner JL, Baillargeon J. A national survey of self-injurious behavior in American prisons. Psychiatr Serv 2011;62(3):285–90.
8. Magdalena Castiñeira C, Magdalena López C. Foreign body ingestion among prisoners. [Article in Spanish]. Rev Esp Enferm Dig 1994;85(4):254–6.
9. Velitchkov NG, Grigorov GI, Losanoff JE, Kjossev KT. Ingested foreign bodies of the gastrointestinal tract: Retrospective analysis of 542 cases. World J Surg 1996;20(8):1001–5.
10. Fung BM, Sweetser S, Wong Kee Song LM, Tabibian JH. Foreign object ingestion and esophageal food impaction: An update and review on endoscopic management. World J Gastrointest Endosc 2019;11(3):174–92.
11. Evans DC, Wojda TR, Jones CD, Otey AJ, Stawicki SP. Intentional ingestions of foreign objects among prisoners: A review. World J Gastrointest Endosc 2015;7(3):162–8.
12. Ikenberry SO, Jue TL, Anderson MA, et al. Management of ingested foreign bodies and food impactions. Gastrointest Endosc 2011;73(6):1085–91.
13. Bisharat M, O’Donnell ME, Gibson N, et al. Foreign body ingestion in prisoners – the Belfast experience. Ulster Med J 2008;77(2):110–4.
14. Weiland ST, Schurr MJ. Conservative management of ingested foreign bodies. J Gastrointest Surg 2002;6(3):496–500.
15. Barros JL, Caballero A Jr, Rueda JC, Monturiol JM. Foreign body ingestion: Management of 167 cases. World J Surg 1991;15(6):783–8.
16. Gitlin DF, Caplan JP, Rogers MP, Avni-Barron O, Braun I, Barsky AJ. Foreign-body ingestion in patients with personality disorders. Psychosomatics 2007;48(2):162–6.
17. Ambe P, Weber SA, Schauer M, Knoefel WT. Swallowed foreign bodies in adults. Dtsch Arztebl Int 2012;109(50):869–75.
18. Clavien PA, Richon J, Burgan S, Rohner A. Gallstone ileus. Br J Surg 1990;77(7):737–42.
19. Montgomery A. Laparoscope-guided enterolithotomy for gallstone ileus. Surg Laparosc Endosc 1993;3(4):310–4.
20. Moberg AC, Montgomery A. Laparoscopically assisted or open enterolithotomy for gallstone ileus. Br J Surg 2007;94(1):53–7.
21. Yang D, Wang Z, Duan ZJ, Jin S. Laparoscopic treatment of an upper gastrointestinal obstruction due to Bouveret’s syndrome. World J Gastroenterol 2013;19(40):6943–6.
22. Bircan HY, Koc B, Ozcelik U, Kemik O, Demirag A. Laparoscopic treatment of gallstone ileus. Clin Med Insights Case Rep 2014;7:75–7.
*********
Author ContributionsAilish Patricia Naughton – Conception of the work, Design of the work, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolvedDarren Patrick Moloney – Conception of the work, Design of the work, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolvedMichael Boland – Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolvedDara Kavanagh – Conception of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone.
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Conflict of InterestAuthors declare no conflict of interest.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Copyright© 2019 Ailish Patricia Naughton et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.

International Journal of Case Reports and Images, Vol. 10, 2019. ISSN: 0976-3198
Int J Case Rep Images 2019;10:101080Z01AN2019. www.ijcasereportsandimages.com
Naughton et al. 6
Access full text article onother devices
Access PDF of article onother devices