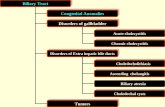
Pathogenesis of diseases of the gallbladder and biliary tract
description
Transcript of Pathogenesis of diseases of the gallbladder and biliary tract

Pathogenesis of diseases of the gallbladder and
biliary tract
John J O’Leary

Biliary tract disorders

Disease of intra-hepatic ducts
LARGE DUCT BILIARY OBSTRUCTION,
PRIMARY BILIARY CIRRHOSIS,
PRIMARY SCLEROSING CHOLANGITIS

LARGE DUCT BILIARY OBSTRUCTION
• Usually extrahepatic, rarely intrahepatic at porta hepatis• Causes - gallstones, tumours, strictures, biliary atresia• Effects on the liver:
Acini - perivenular (zone 3) cholestasis Portal tracts - bile duct proliferation at margins of tracts - neutrophil polymorph infiltrate - oedema of connective tissue Sometimes bile “infarcts” and bile lakes (duct rupture)
• Complications: - acute suppurative cholangitis (ascendingcholangitis).
- liver abscesses if untreated - secondary biliary cirrhosis if unrelieved
• Clinical features of cholestatic jaundice

PRIMARY BILIARY CIRRHOSIS
• A chronic cholestatic disease due to a non-suppurative destructive cholangitis of intrahepatic bile ducts, immune mediated
• F:M as 10:1. Age range 20-80years, peak at 40-50• May be associated with other autoimmune diseases• Very insidious onset, may be asymptomatic for decades, pruritis,
fatigue, xanthelasmas, leading to frank cholestatic jaundice, cirrhosis• 90-95% positive anti-mitochondrial antibodies (AMA) against E2 subunit
of pyruvate dehydrogenase complex inner mitochondrial membrane• Characteristically a granulomatous destruction of bile ducts. Leads to
ductopenia. Copper accumulates in periportal hepatocytes due to chronic cholestasis. Chronic inflammation in portal tracts with interface hepatitis. Portal fibrosis progresses to cirrhosis
• Liver biopsy used to confirm diagnosis and to stage the disease


PRIMARY SCLEROSING CHOLANGITIS
• A chronic cholestatic disease due to a non-specific inflammatory fibrosis of bile ducts, intrahepatic and extrahepatic
• M:F as 2:1. Affects mostly young men
• 70% have ulcerative colitis. Linkage with HLAB8, DR2, DR3. pANCA+
• May be associated with other rare fibrosing conditions
• May be asymptomatic, pruritis and cholestatic jaundice and then cirrhosis develop over many years
• Concentric fibrosis of bile ducts; may result in a scar at site of duct. Leads to ductopenia. Copper accumulates in periportal hepatocytes. Usually scanty lymphocytic infiltrate. Portal fibrosis progresses to cirrhosis. Liver biopsy used to confirm diagnosis and stage
• 10% at risk of developing cholangiocarcinoma



MISCELLANEOUS BILE DUCT DISEASES
• Acquired sclerosing cholangitis can occur in a number of conditions including AIDS.
• Bile duct injury can also occur with liver allografts, graft-versus-host-disease (GVHD), viral hepatitis, drugs, toxins, pyogenic infections, parasitic infestations and other rare conditions.

Disease of extra-hepatic bile ducts

• Biliary atresia is among several neonatal and childhood disorders such as the fibropolycystic disorders which include congenital hepatic fibrosis and various cystic conditions.
• Cholangitis – acute inflammation of the wall of bile ducts. Can result from obstruction of the biliary tree.
• Choledocholithiasis – presence of gallstones in the biliary tree

Cholangitis

Biliary atresia
• Neonatal cholestasis• Occurs in 1:10,000 live births• Complete obstruction of bile flow caused by destruction or
absence of all or part of the extra-hepatic bile ducts• Most likely an acquired inflammatory disorder on unknown cause• Most frequent cause of death from liver disease in early childhood• Features:
– Inflammation and fibrosing stricture of the hepatic or common bile duct
– Inflammation of the major intra-hepatic ducts with destruction– Features of biliary obstruction on biopsy– Peri-portal fibrosis within 3-6 months of birth

Biliary atresia


Gall bladder disorders

Cholelithiasis: gallstones
• Gallstones afflict 10% of the population• 80% of stones are cholesterol stones• Remainder: bilirubin calcium salts [pigment stones]• Risk factors:
– Demography [Europe, N & S America, Mexico]– Advancing age– Female sex– Obesity– Rapid weight reduction– Gallbladder stasis– Hyerlipidaemia– Chronic haemolytic syndromes– Biliary infection– Gastrointestinal disorders: [CD, CF, pancreatic insufficiency]

Gallstones

Cholecystitis
• Inflammation of the gallbladder• Acute and chronic• Almost always occurs in association with stones• May get empyema [pus] in the acute phase• Approx. 5-10% of gallbladders removed for acute
cholecystitis do not contain stones• Chronic: results from acute bouts and is commonly
associated with gallstones

Acute cholecystitis

Chronic cholecystitis

Carcinoma of the gallbladder
• Fifth most common cancer of the digestive tract• Most frequently occurs in the 7th decade of life• 5 year survival: 1%• Rarely resectable when found• Gallstones are present in 50-70% of cases• In Asia: parasitic and pyogenic disease associated• Symptoms:
– Abdominal pain, anorexia, jaundice, nausea and vomiting

Carcinoma of the gallbladder

Molecular progression of carcinoma of the gallbladder

2 molecular pathways fordevelopment of gallbladder carcinoma

Carcinoma of the extra-hepatic bile ducts [including the Ampulla of Vater]
• Cholangiocarcinomas• Extremely insidious onset, painless with progressive
jaundice• Hepatomegaly present in 50% of patients• Distended gallbladder in approx. 25% of patients• Features of extra-hepatic bile duct obstruction

Carcinoma of extra-hepatic bile ducts






![Surgical Management of Cholangiocarcinoma1].2... · ectable biliary cancerectable biliary cancer py prior to surgical exploration (HC = 59%, GB = 82%) nts with gallbladder cancer](https://static.fdocuments.net/doc/165x107/5f4dc0a6f6e64a3565033521/surgical-management-of-c-12-ectable-biliary-cancerectable-biliary-cancer.jpg)