Diabetes Normal Anatomy andPhysiology. Pancreas Pancreas : abdominal organ responsible for exocrine...
-
Upload
david-reed -
Category
Documents
-
view
228 -
download
1
Transcript of Diabetes Normal Anatomy andPhysiology. Pancreas Pancreas : abdominal organ responsible for exocrine...

DiabetesDiabetes
Normal AnatomyNormal Anatomy
and and
PhysiologyPhysiology

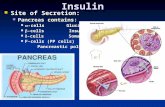
PancreasPancreas: abdominal organresponsible for exocrine secretionof digestive enzymes into the gut
And
Endocrine secretion of hormones of glucose control: insulin and glucagon

Pancreas:
Exocrine
And
Endocrine:Islets of Langerhans

GlucoseGlucose: 6 carbon sugar that is the principlesource of energy for cellular metabolism
Glucose circulates in the blood and is transportedinto cells for use as an energysource

GlucoseGlucose concentration in the blood is normally controlled between 3.6 and 11 mmol/L by various hormonal influences including:
Insulin and Glucagon

InsulinInsulin: peptide hormone released by beta cells of theIslets of Langerhansin response to rising levels of blood glucose
Acts by increasing cellular transport of glucose and increased storage of glucose

GlucagonGlucagon: peptide hormone released by alpha cells of theIslets of Langerhansin response to falling levels of blood glucose
Acts by increasing release of glucose from the liver by breakdown of glycogen

Alpha cells:
Glucagon
Beta cells:
Insulin

Diabetes mellitusDiabetes mellitus :
A metabolic disease caused by an absolute or relative lack of insulin resulting in abnormalities in carbohydrate, protein and lipid metabolism.

Diabetes mellitus:Diabetes mellitus:
Prevalence: 6% of the population
(estimate 30,000 in London area)
(120 diabetics in a 2,000 patient practice)

Diabetes mellitus:Diabetes mellitus:
Classfication:
Type 1 10% of diabetics(estimate 3,000 in London area)
Type 2 90% of diabetics(estimate 27,000 in London area)

PathophysiologyPathophysiology
Type 1 diabetes – beta cells are immunologically destroyed, eventually no insulin is produced
Type 2 diabetes – insulin secretion is reduced, target cells become relatively insulin resistant ( receptors and post-receptor activity

Comparison of type 1 and 2 Comparison of type 1 and 2
Type 1
10% of diabetics Age of onset – young Severe Requires insulin Normal build Little genetic component Autoimmune
Type 2
90% of diabetics Age of onset – 40+ Mild May require insulin,
usually diet or oral hypoglycemics
Obese Strong genetic
component

Diabetes Diabetes is characterized by:
Hyperglycemia
Loss of glucose (and water) in the urine
Paradoxical cellular starvation

SymptomsSymptoms of diabetes of diabetes
Polyuria (increased urination) Polydipsia (increased drinking) Weight loss Weakness Increased infections and impaired
healing Blurred vision

Lab tests - diagnosisLab tests - diagnosis
Normal range of fasting blood glucose:3.9 to 6.1 mmol/L
Diagnosis of DIABETES is based on
Random glucose >11.0 mmol/L + symptoms
or Fasting glucose
>6.9 mmol/L on 2 occasions

Medical managementMedical management
The tighter the glycemic control, the fewer complications– BUT – the more risk of getting hypoglycemic
IDEAL management Fasting glucose 4.0 – 7.0 mmol/L
Infection, stress, pregnancy, surgery will all disturb control

Treatment: Type 1Treatment: Type 1 Diet and physical acitivity plus
Insulin: usual starting dose about 20 units/day
(OD, BID, multiple, continuous infusion pump)
Testing 2-5 x/day
ACE inhibitors (captopril / ramipril) to control nephropathy
Cholesterol lowering drugs

Treatment: Type 2Treatment: Type 2 Diet and physical activity only (testing 2x/month)
+/- Oral hypoglycemics (increase insulin secretion, receptors or post-receptor activity) Sulphonylureas (glyburide = Diabeta)
(can induce hypoglycemia) Biguanides (metformin = Glucophage) Gamma-glucosidase inhibitor (acarbose =
Prandase
+/- Insulin

Lab tests - monitoringLab tests - monitoring Daily (or more) finger pick and glucometer
readings
Hb A1c (Normal = 4.0 to 6.0) A long term (3 month) measure of
diabetic control (glycosylated Hb)Good <7.0Fair 7.0 to 8.9Poor >9.0

Diabetic complicationsDiabetic complications
•Related to the strictness of glycemic control and are characterized as:
•Macrovascular complicationsatherosclerosis
•Microvascular complicationseye and kidney

ComplicationsComplications
Macrovascular
Stroke (2-5 X increased risk)MI (2-5 X increased
risk)Cutaneous ulcers (PVD)Amputation (40 X increased risk)

ComplicationsComplications
Microvascular
Retinopathy – blindness(20 X increased risk)
Cataracts (5 X risk)
Nephropathy – renal failure(25 X increased risk)

ComplicationsComplications
Neuropathy – numbness, tingling, pain, glove and stocking sensory deficits
Autonomic involvement
Infections secondary to impaired vascularity and PMN defects
Decreased duration and quality of life

Emergencies: ketoacidosisEmergencies: ketoacidosis In type 1 patients only
Marked hyperglycemia (high serum glucose) causes osmotic diuresis
Patient loses excess water, Na, K, and ketones released from the liver cause a metabolic acidosis
Precipitated by an infection, insulin error or omission, or occurs in a previously undiagnosed patient

Treated with insulin, fluid replacement, K replacement
Type 2 diabetics can have a much less serious variant of this called:Hyperglycemic hyperosmolar nonketotic state secondary to dehydration
Emergencies: ketoacidosisEmergencies: ketoacidosis

Emergencies: hypoglycemiaEmergencies: hypoglycemiaMay occur with an overdose of insulin / oral
medication or a missed meal
Only some oral medications cause hypoglycemia – (Sulfonylureas) Glyburide, Glicazide, Chlorpropamide
Patient gets diaphoretic, weak, shaky, palpitations, difficulty thinking, aggressive, vision changes and may lose consciousness

Emergencies: hypoglycemiaEmergencies: hypoglycemia
Patient needs glucose – a glass of juice, a candy, or if comatose, IV 50% glucose solution or IM glucagon (1 mg)
Some patients are totally unaware of their hypoglycemia until they lose consciousness

Dental managementDental management Assess control / severity / compliance (CSC)
Treatment plan modification (based on CSC) Possibly … None AM appointments Normal meds and diet pre-op Limit treatment duration Antibiotic coverage??? Post-op diet instructions Hospitalization / GA and NPO status Consultation with the MD

Dental managementDental management Assess control / severity /compliance
When were they first diagnosed
Type 1 vs Type 2
What medications are they taking (or diet only)
How much insulin do they use / how frequently
How often do they measure their glucose and what are their usual measurements

Dental managementDental management Assess control / severity / compliance
Frequency of hypoglycemic reactions (can they feel them coming on?)
Complications: brain, eye, heart, kidney, toes
How often and when last did they see their MD Did they take meds and have meals today
Be alert to changes in “control”

Dental managementDental management Assess control / severity / compliance
BRITTLENESS: poor control of diabetes as a function of the nature of the disease or other complicating factors such as infection (?dental abscess?)
COMPLIANCE: an indication of the patient’s willingness or ability to manage his/her medications or diet for optimal control

Dental conerns:Dental conerns:
Hypoglycemia during a procedure
Oral surgeries that will prevent the patients from getting their usual caloric requirements
Brittle diabetics (extreme fluctuations of hypo/hyperglycemia) – usually occurs after years of high dose insulin therapy

Dental conerns:Dental conerns:
Acute oral infections that precipitate hyperglycemia
Be more aggressive with antibiotics in patients with high sugars

Oral complicationsOral complications
Xerostomia secondary to dehydration
Mucosal fungal infection: candidiasis
Increased caries and periodontal disease

Oral complicationsOral complications
Poor post surgical wound healing
“Burning mouth syndrome” …diabetic neuropathy
Consult MD in suspicious patients

Questions?Questions?