Cardiovascular Physiologyarjenh/lect3.pdf · • Mechanical events of the cardiac cycle 5555 2222...
Transcript of Cardiovascular Physiologyarjenh/lect3.pdf · • Mechanical events of the cardiac cycle 5555 2222...

Cardiovascular Physiology
Copyright © 2009 Pearson Education, Inc.
Lectures byJan Machart
University of Texas, Austin

Overview: Cardiovascular System
Ascending arteries
Left atrium
Right atrium
Coronary arteries
PulmonaryveinsPulmonary
arteriesSuperior vena cava
Arms
Lungs
Aorta
Capillaries ArteriesVeins
Head andBrain
Copyright © 2009 Pearson Education, Inc. Figure 14-1
Descending arteries
Abdominal aortaLeft ventricle
HeartRight ventricle
Renalveins
Renalarteries
Hepaticvein
Inferior vena cava
Ascending veins
Venous valve
Trunk
Kidneys
Pelvis andLegs
Liver Digestivetract
Hepatic artery
Hepatic portal vein

Pressure Gradient in Systemic Circulation
• Blood flows down pressure gradients
Copyright © 2009 Pearson Education, Inc. Figure 14-2

Pressure Change
• Pressure created by contracting muscles is transferred to blood
• Driving pressure for systemic flow is created by the left ventricle
• If blood vessels constrict, blood pressure
Copyright © 2009 Pearson Education, Inc.
• If blood vessels constrict, blood pressure increases
• If blood vessels dilate, blood pressure decreases
• Volume changes greatly affect blood pressure in CVS

Structure of the Heart
• The heart is composed mostly of myocardium
STRUCTURE OF THE HEART
Superiorvena cava
Aorta
Pulmonaryartery
Copyright © 2009 Pearson Education, Inc. Figure 14-7e–f
Diaphragm
(e) The heart is encased withina membranous fluid-filledsac, the pericardium.
Pericardium
(f) The ventricles occupy the bulk ofthe heart. The arteries and veins allattach to the base of the heart.
vena cava
Rightatrium
Auricle ofleft atrium
artery
Rightventricle
Leftventricle
Coronaryarteryand vein

Structure of the Heart
• The heart valves ensure one-way flowPulmonary
semilunar valve
Rightpulmonary
arteriesSuperior
vena cava
Left pulmonaryarteries
Aorta
Left pulmonaryveins
Copyright © 2009 Pearson Education, Inc. Figure 14-7g
(g) One-way flow through the heartis ensured by two sets of valves.
Right atrium Left atrium
Right ventricle
vena cava veins
Cusp of the AV(bicuspid) valve
Cusp of a right AV(tricuspid) valve
Chordae tendineae
Inferiorvena cava
Papillary muscles
Left ventricle
Descendingaorta

Cardiac Muscle
(a)
Copyright © 2009 Pearson Education, Inc. Figure 14-10(b)
Contractile fibers
Nucleus
Mitochondria
Cardiac muscle cell
Intercalated disk(sectioned)
Intercalated disk

Cardiac Muscle
• Excitation-contraction coupling and relaxation in cardiac muscle
1
2
3
910
2
1
Voltage-gated Ca 2+
channels open. Ca 2+
enters cell.
Ca2+ induces Ca 2+ releasethrough ryanodine
Action potential entersfrom adjacent cell.
ATP NCX
3 Na+
3 Na+
2 K+ Ca2+
Ca2+
ECF
ICF
Ca2+
RyR
Copyright © 2009 Pearson Education, Inc. Figure 14-11
4
5
6
7
8
9
10
776
5
8
4
3
2
Ca2+ ions bind to troponinto initiate contraction.
Relaxation occurs whenCa2+ unbinds from troponin.
Na+ gradient is maintainedby the Na +-K+-ATPase.
through ryanodinereceptor-channels (RyR).
Local release causesCa2+ spark.
Ca2+ is pumped backinto the sarcoplasmicreticulum for storage.
Ca2+ is exchanged withNa+ by the NCX antiporter.
Summed Ca 2+ sparkscreate a Ca 2+ signal.
ATP
Sarcoplasmic reticulum(SR)
Myosin
Actin
Relaxation
Ca2+ Ca2+
Ca2+ stores
T-tubule
L-typeCa2+
channel
Ca2+ sparks
Ca2+ signal
Contraction
Ca2+
SR

Myocardial Contractile Cells
• Action potential of a cardiac contractile cell
0
PX = Permeability to ion X
PK and PCa
PNa
PK and PCa
+20
–20
–40
0
1
2
3
Mem
bran
e po
tent
ial (
mV
)
Copyright © 2009 Pearson Education, Inc. Figure 14-13
44
0 100 200 300Time (msec)
–60
–80
–100
Phase Membrane channels
Na+ channels open
Na+ channels close
Ca2+ channels open; fast K + channels close
Ca2+ channels close; slow K + channels open
Resting potential
PNa
0
1
2
3
4
Mem
bran
e po
tent
ial (
mV
)

Electrical Conduction in Myocardial Cells
Membrane potentialof autorhythmic cel
Membrane potentialof contractile cell
Cells ofSA node
Copyright © 2009 Pearson Education, Inc. Figure 14-17
Contractile cell
SA node
Depolarizations of autorhythmic cellsrapidly spread to adjacent contractilecells through gap junctions.
Intercalated diskwith gap junctions

Electrical Conduction in the Heart 1111
2222
3333
4444
3333
2222
1111
THE CONDUCTING SYSTEMOF THE HEART
SA node
AV node
Internodalpathways
SA node
SA node depolarizes.
Electrical activity goesrapidly to AV node viainternodal pathways.
Depolarization spreadsmore slowly acrossatria. Conduction slowsthrough AV node.
Depolarization movesrapidly through ventricularconducting system to theapex of the heart.
Copyright © 2009 Pearson Education, Inc. Figure 14-18
5555
5555
4444
Purkinjefibers
Bundlebranches
AV bundle
AV node
pathwaysDepolarization wavespreads upward fromthe apex.

Electrical Conduction in the Heart 11111111
THE CONDUCTING SYSTEMOF THE HEART
SA node
AV node
Internodalpathways
SA node
SA node depolarizes.
Copyright © 2009 Pearson Education, Inc. Figure 14-18, step 1
Purkinjefibers
Bundlebranches
AV bundle
AV node
pathways

Electrical Conduction in the Heart 1111
22222222
1111
THE CONDUCTING SYSTEMOF THE HEART
SA node
AV node
Internodalpathways
SA node
SA node depolarizes.
Electrical activity goesrapidly to AV node viainternodal pathways.
Copyright © 2009 Pearson Education, Inc. Figure 14-18, steps 1–2
Purkinjefibers
Bundlebranches
AV bundle
AV node
pathways

Electrical Conduction in the Heart 1111
2222
3333
3333
2222
1111
THE CONDUCTING SYSTEMOF THE HEART
SA node
AV node
Internodalpathways
SA node
SA node depolarizes.
Electrical activity goesrapidly to AV node viainternodal pathways.
Depolarization spreadsmore slowly acrossatria. Conduction slowsthrough AV node.
Copyright © 2009 Pearson Education, Inc. Figure 14-18, steps 1–3
Purkinjefibers
Bundlebranches
AV bundle
AV node
pathways

Electrical Conduction in the Heart 1111
2222
3333
4444
3333
2222
1111
THE CONDUCTING SYSTEMOF THE HEART
SA node
AV node
Internodalpathways
SA node
SA node depolarizes.
Electrical activity goesrapidly to AV node viainternodal pathways.
Depolarization spreadsmore slowly acrossatria. Conduction slowsthrough AV node.
Depolarization movesrapidly through ventricularconducting system to theapex of the heart.
Copyright © 2009 Pearson Education, Inc. Figure 14-18, steps 1–4
4444
Purkinjefibers
Bundlebranches
AV bundle
AV node
pathways

Electrical Conduction in the Heart 1111
2222
3333
4444
3333
2222
1111
THE CONDUCTING SYSTEMOF THE HEART
SA node
AV node
Internodalpathways
SA node
SA node depolarizes.
Electrical activity goesrapidly to AV node viainternodal pathways.
Depolarization spreadsmore slowly acrossatria. Conduction slowsthrough AV node.
Depolarization movesrapidly through ventricularconducting system to theapex of the heart.
Copyright © 2009 Pearson Education, Inc. Figure 14-18, steps 1–5
5555
5555
4444
Purkinjefibers
Bundlebranches
AV bundle
AV node
pathwaysDepolarization wavespreads upward fromthe apex.

Electrical Conduction
• AV node• Routes the direction of electrical signals • Delays the transmission of action potentials
• SA node• Sets the pace of the heartbeat at 70 bpm
Copyright © 2009 Pearson Education, Inc.
• Sets the pace of the heartbeat at 70 bpm• AV node (50 bpm) and Purkinje fibers (25-40
bpm) can act as pacemakers under some conditions

Einthoven’s Triangle
Electrodes areattached to theskin surface.
Right arm Left arm
I
Copyright © 2009 Pearson Education, Inc. Figure 14-19
A lead consists of twoelectrodes, one positiveand one negative.
Left leg
II III

The Electrocardiogram
• Three major waves: P wave, QRS complex, and T wave
Copyright © 2009 Pearson Education, Inc. Figure 14-20

Electrical Activity
• Correlation between an ECG and electrical events in the heart
P
R
T
PQ or PR segment:PQ or PR segment:PQ or PR segment:PQ or PR segment:
conduction throughAV node and AVbundle
P wave: P wave: P wave: P wave: atrialdepolarizationSTARTSTARTSTARTSTART
The endThe endThe endThe end
P
Copyright © 2009 Pearson Education, Inc. Figure 14-21
P
Q
T
S P
T wave:T wave:T wave:T wave:
ventricularrepolarization
bundle
ELECTRICALEVENTSOF THE
CARDIACCYCLE
Repolarization
P
Q
P
Q
R
P
Q
R
T
S
R waveR waveR waveR waveP
Q
R
S
S waveS waveS waveS wave
Q
R
P
Q waveQ waveQ waveQ wave
Ventricles contract
ST segmentST segmentST segmentST segment
Atria contract
S

Electrical ActivityP wave: P wave: P wave: P wave: atrialdepolarization
ELECTRICALEVENTS
STARTSTARTSTARTSTART
P
Copyright © 2009 Pearson Education, Inc. Figure 14-21 (1 of 9)
EVENTSOF THE
CARDIACCYCLE

Electrical Activity
P
PQ or PR segment:PQ or PR segment:PQ or PR segment:PQ or PR segment:
conduction throughAV node and AVbundle
P wave: P wave: P wave: P wave: atrialdepolarization
ELECTRICALEVENTS
STARTSTARTSTARTSTART
P
Atria contract
Copyright © 2009 Pearson Education, Inc. Figure 14-21 (2 of 9)
EVENTSOF THE
CARDIACCYCLE

Electrical Activity
P
PQ or PR segment:PQ or PR segment:PQ or PR segment:PQ or PR segment:
conduction throughAV node and AVbundle
P wave: P wave: P wave: P wave: atrialdepolarization
ELECTRICALEVENTS
STARTSTARTSTARTSTART
P
Atria contract
Copyright © 2009 Pearson Education, Inc. Figure 14-21 (3 of 9)
EVENTSOF THE
CARDIACCYCLE
P
Q
Q waveQ waveQ waveQ wave

Electrical Activity
P
PQ or PR segment:PQ or PR segment:PQ or PR segment:PQ or PR segment:
conduction throughAV node and AVbundle
P wave: P wave: P wave: P wave: atrialdepolarization
ELECTRICALEVENTS
STARTSTARTSTARTSTART
P
Atria contract
Copyright © 2009 Pearson Education, Inc. Figure 14-21 (4 of 9)
EVENTSOF THE
CARDIACCYCLE
P
Q
P
Q
RR waveR waveR waveR wave
Q waveQ waveQ waveQ wave

Electrical Activity
P
PQ or PR segment:PQ or PR segment:PQ or PR segment:PQ or PR segment:
conduction throughAV node and AVbundle
P wave: P wave: P wave: P wave: atrialdepolarization
ELECTRICALEVENTS
STARTSTARTSTARTSTART
P
Atria contract
Copyright © 2009 Pearson Education, Inc. Figure 14-21 (5 of 9)
EVENTSOF THE
CARDIACCYCLE
P
Q
P
Q
RR waveR waveR waveR wave
S waveS waveS waveS wave
Q
R
P
Q waveQ waveQ waveQ wave
S

Electrical Activity
P
PQ or PR segment:PQ or PR segment:PQ or PR segment:PQ or PR segment:
conduction throughAV node and AVbundle
P wave: P wave: P wave: P wave: atrialdepolarization
ELECTRICALEVENTS
STARTSTARTSTARTSTART
P
Atria contract
Copyright © 2009 Pearson Education, Inc. Figure 14-21 (6 of 9)
EVENTSOF THE
CARDIACCYCLE
P
Q
P
Q
RR waveR waveR waveR waveP
Q
R
S
S waveS waveS waveS wave
Q
R
P
Q waveQ waveQ waveQ wave
Ventricles contract
ST segmentST segmentST segmentST segment
S

Electrical Activity
P
T wave:T wave:T wave:T wave:
ventricularrepolarization
PQ or PR segment:PQ or PR segment:PQ or PR segment:PQ or PR segment:
conduction throughAV node and AVbundle
P wave: P wave: P wave: P wave: atrialdepolarization
ELECTRICALEVENTS
Repolarization
STARTSTARTSTARTSTART
R
P
Atria contract
Copyright © 2009 Pearson Education, Inc. Figure 14-21 (7 of 9)
EVENTSOF THE
CARDIACCYCLE
P
Q
P
Q
R
P
Q
R
T
S
R waveR waveR waveR waveP
Q
R
S
S waveS waveS waveS wave
Q
R
P
Q waveQ waveQ waveQ wave
Ventricles contract
ST segmentST segmentST segmentST segment
S

Electrical Activity
P
Q
R
T
S P
T wave:T wave:T wave:T wave:
ventricularrepolarization
PQ or PR segment:PQ or PR segment:PQ or PR segment:PQ or PR segment:
conduction throughAV node and AVbundle
P wave: P wave: P wave: P wave: atrialdepolarization
ELECTRICALEVENTS
Repolarization
STARTSTARTSTARTSTART
R
The endThe endThe endThe end
P
Atria contract
Copyright © 2009 Pearson Education, Inc. Figure 14-21 (8 of 9)
EVENTSOF THE
CARDIACCYCLE
P
Q
P
Q
R
P
Q
R
T
S
R waveR waveR waveR waveP
Q
R
S
S waveS waveS waveS wave
Q
R
P
Q waveQ waveQ waveQ wave
Ventricles contract
ST segmentST segmentST segmentST segment
S

Electrical Activity
P
Q
R
T
S P
T wave:T wave:T wave:T wave:
ventricularrepolarization
PQ or PR segment:PQ or PR segment:PQ or PR segment:PQ or PR segment:
conduction throughAV node and AVbundle
P wave: P wave: P wave: P wave: atrialdepolarization
ELECTRICALEVENTS
Repolarization
STARTSTARTSTARTSTART
R
The endThe endThe endThe end
P
Atria contract
Copyright © 2009 Pearson Education, Inc. Figure 14-21 (9 of 9)
EVENTSOF THE
CARDIACCYCLE
P
Q
P
Q
R
P
Q
R
T
S
R waveR waveR waveR waveP
Q
R
S
S waveS waveS waveS wave
Q
R
P
Q waveQ waveQ waveQ wave
Ventricles contract
ST segmentST segmentST segmentST segment
S

Electrical Activity
• Comparison of an ECG and a myocardial action potential
(a)(a)(a)(a) The electrocardiogram represents the summedelectrical activity of all cells recorded from the
1 mV
1 sec
Copyright © 2009 Pearson Education, Inc. Figure 14-22
electrical activity of all cells recorded from thesurface of the body.
(b)(b)(b)(b) The ventricular action potential is recorded froma single cell using an intracellular electrode.Notice that the voltage change is much greaterwhen recorded intracellularly.
110mV
1 sec

Electrical Activity
• Normal and abnormal electrocardiograms
Copyright © 2009 Pearson Education, Inc. Figure 14-23

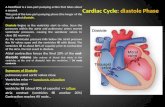
Mechanical Events
• Mechanical events of the cardiac cycle
5555
2222
1111 Late diastoleLate diastoleLate diastoleLate diastole————both sets ofchambers are relaxed andventricles fill passively.
Atrial systoleAtrial systoleAtrial systoleAtrial systole————atrial contractionforces a small amount ofadditional blood into ventricles.
STARTSTARTSTARTSTART
Isovolumic ventricularIsovolumic ventricularIsovolumic ventricularIsovolumic ventricularrelaxationrelaxationrelaxationrelaxation————as ventriclesrelax, pressure in ventriclesfalls, blood flows back intocusps of semilunar valvesand snaps them closed.
Copyright © 2009 Pearson Education, Inc. Figure 14-24
44443333 Isovolumic ventricularIsovolumic ventricularIsovolumic ventricularIsovolumic ventricular
contractioncontractioncontractioncontraction————first phase ofventricular contraction pushes AVvalves closed but does not createenough pressure to open semilunarvalves.
Ventricular ejectionVentricular ejectionVentricular ejectionVentricular ejection————as ventricular pressurerises and exceeds pressurein the arteries, the semilunarvalves open and blood isejected.
S1
S2

Mechanical Events1111 Late diastoleLate diastoleLate diastoleLate diastole————both sets of
chambers are relaxed andventricles fill passively.
STARTSTARTSTARTSTART
Copyright © 2009 Pearson Education, Inc. Figure 14-24, step 1

Mechanical Events
2222
1111 Late diastoleLate diastoleLate diastoleLate diastole————both sets ofchambers are relaxed andventricles fill passively.
Atrial systoleAtrial systoleAtrial systoleAtrial systole————atrial contractionforces a small amount ofadditional blood into ventricles.
STARTSTARTSTARTSTART
Copyright © 2009 Pearson Education, Inc. Figure 14-24, steps 1–2
S1

Mechanical Events
2222
1111 Late diastoleLate diastoleLate diastoleLate diastole————both sets ofchambers are relaxed andventricles fill passively.
Atrial systoleAtrial systoleAtrial systoleAtrial systole————atrial contractionforces a small amount ofadditional blood into ventricles.
STARTSTARTSTARTSTART
Copyright © 2009 Pearson Education, Inc. Figure 14-24, steps 1–3
3333 Isovolumic ventricularIsovolumic ventricularIsovolumic ventricularIsovolumic ventricular
contractioncontractioncontractioncontraction————first phase ofventricular contraction pushes AVvalves closed but does not createenough pressure to open semilunarvalves.
S1
S2

Mechanical Events
2222
1111 Late diastoleLate diastoleLate diastoleLate diastole————both sets ofchambers are relaxed andventricles fill passively.
Atrial systoleAtrial systoleAtrial systoleAtrial systole————atrial contractionforces a small amount ofadditional blood into ventricles.
STARTSTARTSTARTSTART
Copyright © 2009 Pearson Education, Inc. Figure 14-24, steps 1–4
44443333 Isovolumic ventricularIsovolumic ventricularIsovolumic ventricularIsovolumic ventricular
contractioncontractioncontractioncontraction————first phase ofventricular contraction pushes AVvalves closed but does not createenough pressure to open semilunarvalves.
Ventricular ejectionVentricular ejectionVentricular ejectionVentricular ejection————
as ventricular pressurerises and exceeds pressurein the arteries, the semilunarvalves open and blood isejected.
S1
S2

Mechanical Events
5555
2222
1111 Late diastoleLate diastoleLate diastoleLate diastole————both sets ofchambers are relaxed andventricles fill passively.
Atrial systoleAtrial systoleAtrial systoleAtrial systole————atrial contractionforces a small amount ofadditional blood into ventricles.
STARTSTARTSTARTSTART
Isovolumic ventricularIsovolumic ventricularIsovolumic ventricularIsovolumic ventricular
relaxationrelaxationrelaxationrelaxation————as ventriclesrelax, pressure in ventriclesfalls, blood flows back intocusps of semilunar valvesand snaps them closed.
Copyright © 2009 Pearson Education, Inc. Figure 14-24, steps 1–5
44443333 Isovolumic ventricularIsovolumic ventricularIsovolumic ventricularIsovolumic ventricular
contractioncontractioncontractioncontraction————first phase ofventricular contraction pushes AVvalves closed but does not createenough pressure to open semilunarvalves.
Ventricular ejectionVentricular ejectionVentricular ejectionVentricular ejection————
as ventricular pressurerises and exceeds pressurein the arteries, the semilunarvalves open and blood isejected.
S1
S2

Cardiac Cycle
• Left ventricular pressure-volume changes during one cardiac cycle
120
ESVD
Stroke volume EDV = End-diastolicvolumeESV = End-systolicvolume
KEYKEYKEYKEY
Left
vent
ricul
ar p
ress
ure
(mm
Hg)
Copyright © 2009 Pearson Education, Inc. Figure 14-25
80
40
0 65 100 135Left ventricular volume (mL)
AB
C
EDV
Onecardiaccycle
Left
vent
ricul
ar p
ress
ure
(mm
Hg)

Wiggers Diagram
P PT
0 100 200 300 400 500 600 700 800
120
AAAA
BBBB
60
90
Time (msec)
Electro-cardiogram
(ECG)
Pressure(mm Hg)
Dicrotic notch
QRScomplex
QRScomplex
Leftventicularpressure
DDDDLeft atrialpressure
30
Copyright © 2009 Pearson Education, Inc. Figure 14-26
135
0 CCCC
DDDD
EEEE
FFFF
S1 S2
65
Heart sounds
Leftventricular
volume (mL)
Atrialsystole
Atrialsystole
Atrialsystole
Atrialsystole
Ventricularsystole
Ventricularsystole
Ventriculardiastole
Isovolumicventricularcontraction
Earlyventricular
diastole
Lateventricular
diastole
pressure30

Stroke Volume and Cardiac Output
• Stroke volume• Amount of blood pumped by one ventricle
during a contraction• EDV – ESV = stroke volume
• Cardiac output
Copyright © 2009 Pearson Education, Inc.
• Cardiac output• Volume of blood pumped by one ventricle in a
given period of time• CO = HR × SV• Average = 5 L/min

Sympathetic neurons(NE)
Parasympatheticneurons (Ach)
Integrating center
Efferent path
Effector
Tissue response
Cardiovascularcontrol
center in medullaoblongata
KEYKEYKEYKEY
Autonomic Neurotransmitters Alter Heart Rate
Copyright © 2009 Pearson Education, Inc.
Na+ and Ca 2+ influx
Rate of depolarization
Heart rate
Muscarinic receptorsof autorhythmic cells
K+ efflux; Ca 2+ influx
Hyperpolarizes cell andrate of depolarization
Heart rate
ββββ1-receptors ofautorhythmic cells
Figure 14-27

Stroke Volume
• Frank-Starling law states• Stroke volume increase as EDV increases
• EDV is affected by venous return• Venous return is affected by
• Skeletal muscle pump
Copyright © 2009 Pearson Education, Inc.
• Skeletal muscle pump• Respiratory pump• Sympathetic innervation
• Force of contraction is affected by• Stroke volume• Length of muscle fiber and contractility of heart

Inotropic Effect
• The effect of norepinepherine on contractility of the heart
Copyright © 2009 Pearson Education, Inc. Figure 14-29

Stroke Volume and Heart Rate Determine Cardiac Output
determined by
is a function of
determined by
CARDIAC OUTPUTCARDIAC OUTPUTCARDIAC OUTPUTCARDIAC OUTPUT
Heart rateHeart rateHeart rateHeart rate
Rate of depolarizationin autorhythmic cells
Stroke volumeStroke volumeStroke volumeStroke volume
Force of contraction inventricular myocardium
Copyright © 2009 Pearson Education, Inc. Figure 14-31
is influenced by
which varies with
increases
increases
aided by
Due toparasympathetic
innervation
Sympatheticinnervation and
epinephrine
Venous returnVenous constriction
End-diastolicvolume
Contractility
Respiratorypump
Skeletal musclepump
Decreases Increases

Summary
• Cardiovascular system—anatomy review• Pressure, volume, flow, and resistance
• Pressure gradient, driving pressure, resistance, viscosity, flow rate, and velocity of flow
• Cardiac muscle and the heart
Copyright © 2009 Pearson Education, Inc.
• Cardiac muscle and the heart• Myocardium, autorhythmic cells, intercalated
disks, pacemaker potential, and If channels
• The heart as a pump• SA node, AV node, AV bundle, bundle
branches, and Purkinje fibers

Summary
• The heart as a pump (continued)• ECG, P wave, QRS complex, and T wave
• The cardiac cycle• Systole, diastole, AV valves, first heart sound,
isovolumic ventricular contraction, semilunar
Copyright © 2009 Pearson Education, Inc.
isovolumic ventricular contraction, semilunar valves, second heart sound, and stroke volume
• Cardiac output• Frank-Starling law, EDV, preload, contractility,
inotropic effect, afterload, and ejection fraction

Blood Flow and the Control of Blood
Pressure
Copyright © 2009 Pearson Education, Inc.
Lectures byJan Machart
University of Texas, Austin

Functional Model of the Cardiovascular SystemElastic arteries
Aorta
Aortic valve
Left heartLeft ventricle
Left atrium
Pulmonary veins
Mitral valve Arteriole withvariable radius
Exchange of
Copyright © 2009 Pearson Education, Inc. Figure 15-1
Right heart
Lungs
Right ventricle
Right atrium
Pulmonary arteryPulmonary valve
Tricuspid valve
Capillaries
Venae cavae
Venules
Exchange ofmaterial withcells
Expandable veins

Elastic Recoil in Arteries
1111
22221111
Ventricle contracts.
Semilunar valve opens.Arterioles
Copyright © 2009 Pearson Education, Inc. Figure 15-4a
3333 Aorta and arteries expand andstore pressure in elastic walls.
(a) Ventricular contraction(a) Ventricular contraction(a) Ventricular contraction(a) Ventricular contraction
2222
3333

Pressure Throughout the Systemic Circulation
• Blood pressure is highest in the arteries and decreases continuously as it flows through the circulatory system
Copyright © 2009 Pearson Education, Inc. Figure 15-5

Cuff pressure> 120 mm Hg
Cuff pressurebetween 80 and
Inflatablecuff
Pressuregauge
(a)(a)(a)(a)
(b)(b)(b)(b)
Measurement of Arterial Blood Pressure
Copyright © 2009 Pearson Education, Inc.
Stethoscope 120 mm Hg
Cuff pressure< 80 mm Hg
(c)(c)(c)(c)
Figure 15-7

Bloodvolume
Bloodpressure
leads to
triggers
Stimulus
Integrating center
Tissue response
Systemic response
Slow responseFast response
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
Compensationby
cardiovascularsystem
Vasodilation Cardiac output Excretion of fluid in urineblood volume
Bloodpressureto normal
Compensationby kidneys
Figure 15-9

Factors that Influence Mean Arterial Pressure
Copyright © 2009 Pearson Education, Inc. Figure 15-10

Arteriolar Resistance
Copyright © 2009 Pearson Education, Inc. Table 15-2

Distribution of Blood
• Distribution of blood in the body at rest
Copyright © 2009 Pearson Education, Inc. Figure 15-14

Blood Flow
• Blood flow through individual blood vessels is determined by vessel’s resistance to flow
Copyright © 2009 Pearson Education, Inc. Figure 15-15a

Blood Flow
• Flow ∝ 1/resistance
Copyright © 2009 Pearson Education, Inc. Figure 15-15b

Velocity of Blood Flow
• Velocity of flow depends on total cross-sectional area of the vessels
Copyright © 2009 Pearson Education, Inc. Figure 15-18

Fluid Exchange at a Capillary
• Hydrostatic pressure and osmotic pressure regulate bulk flow
Copyright © 2009 Pearson Education, Inc. Figure 15-19a

Fluid Exchange at a Capillary
Arteriole
Netabsorption
Netfiltration
Venule
Copyright © 2009 Pearson Education, Inc. Figure 15-19b
absorption
Lymphvessels
filtration
(b) Relationship between capillaries and lymph vessels(b) Relationship between capillaries and lymph vessels(b) Relationship between capillaries and lymph vessels(b) Relationship between capillaries and lymph vessels

Lymphatic System
Thoracic (left lymph) duct
Axillary lymph nodes
Lymphatics ofmammary gland
Spleen
Pelviclymph nodes
Thoracic duct
Thymus
Right lymph duct
Cervicallymph nodes
Lymphatics ofupper limb
Lumbarlymph nodes
Copyright © 2009 Pearson Education, Inc. Figure 15-20
Inguinallymph nodes
Blind-end lymphcapillaries in the tissuesremove fluid and filteredproteins.
Lymph fluid empties into the venous circulation.
Lymphaticsof lower limb

Edema
• Two causes• Inadequate drainage of lymph• Filtration far greater than absorption
• Disruption of balance between filtration and absorption
Copyright © 2009 Pearson Education, Inc.
absorption• Increase in hydrostatic pressure• Decrease in plasma protein concentration• Increase in interstitial proteins

Blood Pressure
• Components of the baroreceptor reflex
Medullarycardiovascularcontrol center
Change inblood
pressure
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Copyright © 2009 Pearson Education, Inc. Figure 15-22
Carotid and aorticbaroreceptors
pressure
Parasympatheticneurons
Sympatheticneurons
Veins
Arterioles
Ventricles
SA node

Change inblood
pressure
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc. Figure 15-22 (1 of 10)

Carotid and aorticbaroreceptors
Change inblood
pressure
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
baroreceptors
Figure 15-22 (2 of 10)

Medullarycardiovascularcontrol center
Carotid and aorticbaroreceptors
Change inblood
pressure
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
baroreceptors
Figure 15-22 (3 of 10)

Medullarycardiovascularcontrol center
Carotid and aorticbaroreceptors
Change inblood
pressure
Parasympatheticneurons
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
baroreceptors
Figure 15-22 (4 of 10)

Medullarycardiovascularcontrol center
Carotid and aorticbaroreceptors
Change inblood
pressure
Parasympatheticneurons
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
baroreceptors
Sympatheticneurons
Figure 15-22 (5 of 10)

Medullarycardiovascularcontrol center
Carotid and aorticbaroreceptors
Change inblood
pressure
Parasympatheticneurons
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
baroreceptors
Sympatheticneurons SA node
Figure 15-22 (6 of 10)

Medullarycardiovascularcontrol center
Carotid and aorticbaroreceptors
Change inblood
pressure
Parasympatheticneurons
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
baroreceptors
Sympatheticneurons SA node
Figure 15-22 (7 of 10)

Medullarycardiovascularcontrol center
Carotid and aorticbaroreceptors
Change inblood
pressure
Parasympatheticneurons
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
baroreceptors
Sympatheticneurons
Ventricles
SA node
Figure 15-22 (8 of 10)

Medullarycardiovascularcontrol center
Carotid and aorticbaroreceptors
Change inblood
pressure
Parasympatheticneurons
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
baroreceptors
Sympatheticneurons
Arterioles
Ventricles
SA node
Figure 15-22 (9 of 10)

Medullarycardiovascularcontrol center
Carotid and aorticbaroreceptors
Change inblood
pressure
Parasympatheticneurons
Integrating center
Stimulus
Efferent path
Effector
Sensory receptor
KEYKEYKEYKEY
Blood Pressure
Copyright © 2009 Pearson Education, Inc.
baroreceptors
Sympatheticneurons
Veins
Arterioles
Ventricles
SA node
Figure 15-22 (10 of 10)

Blood Pressure
• The baroreceptor reflex: the response to increased blood pressure
Copyright © 2009 Pearson Education, Inc.
pressure
Figure 15-23

Blood Pressure
• The baroreceptor reflex: the response to orthostatic hypotension
Copyright © 2009 Pearson Education, Inc.
hypotension
Figure 15-24

CVD: Risk Factors
• Not controllable• Sex• Age• Family history
• Controllable
Copyright © 2009 Pearson Education, Inc.
• Controllable• Smoking• Obesity• Sedentary lifestyle• Untreated hypertension

CVD: Risk Factors
• Uncontrollable genetic but modifiable lifestyle• Blood lipids
• Leads to atherosclerosis• HDL-C versus LDL-C
• Diabetes mellitus
Copyright © 2009 Pearson Education, Inc.
• Diabetes mellitus• Metabolic disorder contributes to development of
atherosclerosis

LDL and Plaque
• The development of atherosclerotic plaques (a) Normal arterial wall(a) Normal arterial wall(a) Normal arterial wall(a) Normal arterial wall
(b) Fatty streak(b) Fatty streak(b) Fatty streak(b) Fatty streak
Endothelial cells Elastic connective tissue Smooth muscle cells
Macrophages
Smooth muscle cells
LDL cholesterol accumulates
Copyright © 2009 Pearson Education, Inc. Figure 15-25
(b) Fatty streak(b) Fatty streak(b) Fatty streak(b) Fatty streak
(c) Stable fibrous plaque(c) Stable fibrous plaque(c) Stable fibrous plaque(c) Stable fibrous plaque
(d) Vulnerable plaque(d) Vulnerable plaque(d) Vulnerable plaque(d) Vulnerable plaque
A lipid core accumulatesFibrous scar tissue
Smooth muscle cells
Calcifications are depositedwithin the plaque.
Platelets
Macrophages

Hypertension
• The risk of developing cardiovascular disease doubles with each 20/10 mm Hg increase in blood pressure
• Essential hypertension has no clear cause other than hereditary
Copyright © 2009 Pearson Education, Inc.
other than hereditary
Figure 15-26

Hypertension
• Carotid and aortic baroreceptors adapt• Risk factor for atherosclerosis• Heart muscle hypertrophies
• Pulmonary edema • Congestive heart failure
Copyright © 2009 Pearson Education, Inc.
• Congestive heart failure
• Treatment• Calcium channel blockers, diuretics, beta-
blocking drugs, and ACE inhibitors

Myocardial infarction
Decreased oxygen supply to the heart due to blockage of one or more coronary arteries.
Copyright © 2009 Pearson Education, Inc.

Myocardial infarction
Drawing of the heart showing anterior left ventricl e wall infarction
Copyright © 2009 Pearson Education, Inc.

Myocardial infarction
Symptoms:
A person having an acute myocard infarct usually has sudden chest pain (called angina pectoris) that is felt behind the breast bone and sometimes travels to the left arm or the left side of the neck.
Additionally, the person may have shortness of breath, sweating, nausea, vomiting, abnormal heartbeats and anxiety.
Copyright © 2009 Pearson Education, Inc.
Areas of pain

Myocardial infarction
A cardiac troponin rise (as a marker of all heart muscle damage) accompanied by either typical symptoms, pathological Q waves, ST elevation or depression, or coronary intervention is diagnostic of MI (WHO).
Copyright © 2009 Pearson Education, Inc.

Myocardial infarction
• Etiology/Prevention:• Lifestyle: smoking, obesity, stress, exercise, …• Diseases: diabetes mellitus, hypertension, lipid disorders, …• Medication: antiplatelet drugs, beta blockers, ACE inhibitors,
statins, other antihypertensive drugs, …
Copyright © 2009 Pearson Education, Inc.
• Treatment angina pectoris: • The most specific medicine to treat angina is nitroglycerin. It is a
potent vasodilator that makes more oxygen available to the heart muscle.
• Beta blockers and calcium channel blockers act to decrease the heart's workload, and thus its requirement for oxygen.

Myocardial infarction
Percutaneous coronary intervention
• During PCI, a cardiologist feeds a deflated balloon or other device on a catheter from the inguinal femoral artery or radial artery up through blood vessels until they reach the site of blockage in the heart and X-ray imaging is used to guide the catheter threading.
• At the blockage, the balloon is inflated to open the artery, allowing blood to flow. • A stent is often placed at the site of blockage to permanently open the artery.
Copyright © 2009 Pearson Education, Inc.
Coronary angiography and angioplasty in acute myocardial infarction
left: RCA closedright: RCA successfully dilated
Coronary artery bypass grafting (CABG), which bypasses stenotic arteries by grafting vessels from elsewhere in the body, is an alternative treatment.

Myocardial infarction
Copyright © 2009 Pearson Education, Inc.

Myocardial infarction
Ischemic heart disease in context of other cardiovascular (related) diseases
Copyright © 2009 Pearson Education, Inc.

EHEALTH
Questions?
and/or
Copyright © 2009 Pearson Education, Inc.
and/or
Blood Pressure Measurement