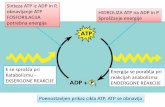
Sinteza ATP iz ADP in P, obnavljanje ATP HIDROLIZA ATP na ...
Water soluble vitamins Dr.S.Chakravarty, MD. A- ATP B- BIOTIN C- CO 2 REM - VOMIT MAIN ATP...
-
Upload
allison-welch -
Category
Documents
-
view
220 -
download
0
Transcript of Water soluble vitamins Dr.S.Chakravarty, MD. A- ATP B- BIOTIN C- CO 2 REM - VOMIT MAIN ATP...

Water soluble vitamins
Dr.S.Chakravarty, MD

A- ATPB- BIOTIN C- CO2 REM - VOMIT
MAIN ATP SYNTHESIS
DECREASEDATP Na+K+ PUMP FAILURE CELLS SWELL AND DIE
KAPLAN Step 1 notes

V.Imp SOURCE OF e0
-1 for ETC
Left untreated death !!
U T
DNA and RNA synthesis
KAPLAN Step 1 notes

SUBACUTRE COMBINED DEGENERATION
1)Regeneration of TETRAHYDROFOLATE (ACTIVE FOLATE )DNA and RNA synthesis
ANYTHING THAT DAMAGES LIVER OR ANYTHING THAT INCTREASED AST/ALT ACTIVITY INCREASED NEED FOR PLP
LESS HEMESMALL RBCs IRON NOT USED IRON DEPOSITED IN PRECURSORS OF RBCSSIDEROBLASTS
KAPLAN Step 1 notes

ATP
STOMACH ACIDITY AND VIT C Fe+3 Fe +2
CoA
KAPLAN Step 1 notes

Thiamine : B1 • Source : unpolished rice and whole wheat.(Aleurone layer OF CEREALS )• PARBOILED RICE IS RICH IN THIAMINE
Thiamin status is affected by:1. Food processing – washing, polishing etc.
2. Anti-thiamine factors – Fresh water and shell fish (thiaminases), pyrithiamine.
3. Ethanol ingestion / c/c alcoholism (MCC cause of DEFICIENCY ) Reduces thiamin intake Impairs intestinal absorption Alters phosphorylation of thiamin Increases excretion

Functions of B1:1. Enzyme cofactor: (Thiamine pyrophosphate TPP
or TDP)
A. Oxidative decarboxylation reactions Pyruvate dehydrogenase α-ketoglutarate dehydrogenase α-keto acid dehydrogenase – branched chain
amino acid metabolim.
B. Transketolation reactions Transketolase – HMP pathway

2. Thiamine Triphosphate (TTP)• Nerve conduction
1. Phosphorylation of membrane ion channels
2. Regulates sodium conductance
• Neurotransmission
1. Acetyl choline, Glutamate and GABA synthesis and utilization
2. Increase neurotransmitter levels in brain.

Measurement of thiamine status:
• Erythrocyte transketolase activity: Lab investigation for B1 deficiency.
xylulose-5-p + Ribose-5-p (ketose) (aldose)
Glyceraldehyde-3-p + Sedo-heptulose-7-p (aldose) (ketose)

Deficiency of B1:
• Beriberi Wet beriberi Dry beriberi Infantile beriberi
• Wernicke-Korsakoff syndrome:
• Polyneuritis:

Wet Beri Beri:Cardiovascular manifestations edema palpitations breathlessness fatigue distended neck veins
cause of death: high ouput cardiac failure
Shoshin beriberi: cyanosis, shock, cardiomegaly

Biochemical basis of wet beriberi:
Pyruvate Acetyl CoA (-) Lactate
Acidosis
Depression of vasomotor center
Decreased Vascular resistance Peripheral vasodilatation

Vasodilation
High cardiac output
Renin angiotensin aldosterone
system
Cardiac failure Sodium and water retention
Edema

Dry Beriberi (paralytic / nervous)
CNS manifestations: muscle weakness gait disturbance paralysis calf muscle tenderness
impairment of sensory, motor and reflex functions ( distal segment of limbs > proximal segment)

Infantile beri-beri:
• Maternal malnutrition
• Age group: 2 – 3 months
• 3 forms Cardiac (acute fulminating) Aphonic Pseudomeningitic

Cerebral Beri beri:
High risk groups: Alcoholism Chronic dialysis
Clinical features: Wernicke’s encephalopathy – ataxia, confusion and
opthalmoplegia.
Korsakoff psychosis – amnesia and confabulation – impairment of conceptual function decreased spontaneity and initiative

Biochemical basis:
• Defective energy metabolism ATP synthesis Altered functions of neurons Degeneration of myelin sheaths
• Defective nerve conductance and neurotransmission
• Synthesis of neurotransmitters

Reason for decreased Neurotransmitters:
Pyruvate Acetyl Co-A
Alpha keto Glutarate
TCA cycle
Glutamate
Acetyl choline B1
B6
GABA
PDH
Choline acetyl transferase
Glutamate decarboxylase

Riboflavin : B2
• Heat stable, light sensitive , luminescent vitamin – UV light
• Vitamin B2 , lactoflavin, Warburg’s yellow enzyme
• Source – whole cereals, legumes (beans), eggs , milk

Co-enzyme forms:
• FMN – Flavin Mono Nucleotide• FAD – Flavin Adenine Dinucletide
• Riboflavin FMN
FAD
Flavokinase
FAD
synthase

Functions:
• Integral component of electron transport chain ATP SYNTHESIS
–NADFMNCoQ• TCA cycle succinate dehydrogenase ATP SYNTHESIS • FATTY ACID OXIDATIONacyl CoA dehydrogenase ATP
SYNTHESIS • As a part of alpha ketoglutarate and isocitrate
dehydrogenase complex ( dihydrolipoate dehydrogenase)

Riboflavin deficiency:

Deficiency manifestations:• Glossitis - inflammation of tongue Magenta red colour(glossitis ), Fissures, Atrophy of lingual papillae
• Cheilosis: fissures in lips
• Angular stomatits: inflammation at corners of mouth
• Conjunctivitis
• Oral-ocular-genital syndrome Angular stomatitis photophobia scrotal dermatitis

Niacin: B3
• Exists in two forms– Nicotinic acid (Niacin)– Nicotinamide (Niacinamide)
• Two coenzyme forms of niacin– NAD+ – NADP+

Function:• Coenzymes are active participants in oxidation-reduction
reactions – Dehydrogenases • Function in at least 200 reaction in cellular metabolic
pathways• NAD+
– Participates in catabolic reactions – Electron and hydrogen ion acceptor
• NADP+– Anabolic reactions – Important in biochemical pathway for fatty-acid synthesis, steroid
and bile acid synthesis.

Tryptophan can be converted to Niacin:
Tryptophan FAD 3-OH-kynurenine kynureninase (-) B6 B6
3-OH-anthranallic acid
Xanthurenic acid Niacin

Deficiency manifestation:• Pellagra– Dementia, Diarrhea, Dermatitis– If not treated can cause death– Develops about 50 to 60 days after a niacin deficient
diet
• Early symptoms– Loss of appetite, weight loss, and weakness
• Mild symptoms– Indigestion, canker sores, vomiting, depression and
fatigue

Pellagra like symptoms can be seen with:
• Niacin deficiency
• Hartnup diseaseLess abspn of Trp
• Carcinoid syndromeexcess Trp going for Serotonin synthesis and less for Niacin synthesis
• Pyridoxine deficiencyKynureninase is not working
• INH (Isoniazid )administration ANTI-TUBERCULOUS DRUG damages liver and increased AST/ALT activity + directly inhibits PLP formation

Uses of Nicotinic acid
Atherosclerosis and Hyperlipidemias:
• By lowering VLDL levels and TG levels mainly .

Pyridoxine: B6
• Three forms :1. Pyridoxine2. Pyridoxal3. Pyridoxamine – antioxidant
Active form of B6 – Pyridoxal phosphate (PLP)

Functions of B6:• Aminoacid metabolism: 1. Transamination2. Deamination3. Decarboxylation4. Transulfuration
• Lipid metabolism : 1. Sphingomyelin synthesis2. Carnitine synthesis
• Carbohydrate metabolism : 1. Glycogenolysis – glycogen phosphorylase 2. Gluconeogenesis –formation of alpha keto acids

Functions:• Heme synthesis
• Catecholamine synthesis
• Niacin synthesis
• Modulation of hormone action – mainly steroids

Transamination reactions :
Aspartate transaminase (AST)
Alanine transaminase (ALT)
Aspartate + α-ketoglutarate
Oxaloacetate + Glutamate
Alanine + α-ketoglutarate
Pyruvate + Glutamate
PLP PLP
• Diagnostic enzymes in various liver diseases:
• Helps in Gluconeogenesis – aminoacid to ketoacids

Decarboxylation reactions:
• Glutamate decarboxylase : Glutamate GABA (inhibitory neurotransmittor)
• Histidine decarboxylase : Histidine Histamine
• DOPA decarboxylase: (catecholamine synthesis) DOPA Dopamine

Transsulfuration :
• Cystathionine β synthase: Homocysteine + serine Cystathionine
• Cystathionase: Cystathionine Homoserine + Cysteine
B6 deficiency Homocysteine
Cardiovascular disease
PLP
PLP

Modulation of hormone action B6 - Remove hormone-receptor complex from DNA
binding
Terminate the action of steroid hormone
B6 deficiency: • Enhances steroid hormone sensitivity• Increases risk for hormone dependent cancers of
breast and uterus

Drugs inactivating PLP:
• Alcohol
• Isoniazid - Anti tubercular
• Carbidopa – used with DOPA in parkinsonism • Penicillamine – chelating agent
• Oral contraceptive pills

Deficiency manifestation:• Neurological manifestations: Peripheral neuritis convulsions
Basis: Formation of catecholamine GABA levels Sphingolipid synthesis Demyelination
• Dermatitis - (pellagra like symptoms)
• Microcytic hypochromic Anemia – decreased formation of Heme

Diagnosis of B6 deficiency:
• Decreased AST and ALT activity
• Methionine load test – Homocysteine and cystathionine in urine.
• Tryptophan load test – Xanthurenic acid

Pantothenic acid: B5
• Contains Pantoic acid (derived from valine) and β-alanine (derived from aspartate)
• Carrier of acyl groups
• Involved in the metabolism of fat, proteins and carbohydrates
• Active form – Coenzyme A (Co-A) Acyl carrier protein.

Functions of Co-A:
1. Cellular metabolism – Co-A derivatives
2. Protein acetylation – Histones and Microtubules
3. Protein acylation – palmitoylation myristoylation of proteins – cell regulation.
4. Detoxification of drugs – acetylation

Cellular metabolism of Co-A:
• Acetyl Co-A• Malonyl Co-A• HMG Co-A• Fatty acyl Co-A• Acetoacetyl Co-A• Succinyl Co-A• Palmitoyl Co-A
TCA cyclefatty acid synthesissteroid metabolismTransportketone body synthesisHeme synthesissphinolipid synthesis

Deficiency manifestations;
• Fatigue, irritability low CoA levels energy production • Neurological symptoms Numbness, muscle cramps acetyl choline formation
• Burning foot syndrome :
• Hypoglycemia : decreased acylation of receptors – increased binding of insulin.

Biotin: B7• Co-enzyme for carboxylation reaction:• Carboxylation require Bicarbonate, ATP and Biotin.
• 5 carboxylation reactions :1. Acetyl Co-A carboxylase isoform –I –cytosol 2. Acetyl Co-A carboxylase isoform - II – outer mit3. Pyruvate carboxylase4. Methyl crotonyl Co-A carboxylase5. Propionyl Co-A carboxylase
Mitochondrial

Biotin deficiency: causes• Consumption of raw egg – Avidin ( binds
biotin)
• Dialysis

Features of biotin deficiency
• Vitamin H – (Haar and Haut) Hair and skin in German
• Biotin deficient facies – unusual fat distribution with a characteristic rash.
Symptoms : 1. Periorificial dermatitis2. Conjunctivitis3. Alopecia4. Neurological – Tingling and numbness ,
depression , lethargy.

Biochemical basis:
• CNS features : Defect in Pyruvate carboxylase lactic acidemia.
• Skin rash and hair loss – due to abnormal fatty acid metabolism mainly of omega -6 – fatty aicds.
• Biotinylation of histones – regulation of transcription and cell proliferation – is affected.

Folate metabolism:• Folic acid is present as various forms of Tetrahydrofolate :
• Acts as a co-enzyme by accepting, transfering, or modyfying one carbon units that are attached to N5 or N10 position of folate.
• Active one carbon donors:1. Formyl THF – purine synthesis2. Methylene THF – pyrimidine synthesis3. Methenyl THF4. Formimino THF
• Predominant form in plasma – methyl THF (reduced) and inactive.
Intermediates

Folate Dihydrofolate
THF
Purine synthesis
Pyrimidine synthesis
Methyl THF (reduced)
Homocysteine
Methionine
B 12Homocysteine methyl transferase
DHFR DHFR Formyl THFMethenyl THFMethylene THF
Folate metabolism:1. DNA synthesis
2. Conversion of Homocysteine to methionine
Methylene tetrahydrofolate reductase

Pyrimidine synthesis:
d-UMP d-TMP
Methylene THF
DHF
Thymidylate synthase
Purine synthesis:
Carbon 2 and 8 of the purine ring is donated by formyl THF

Dihydropteroate + PABA
Dihydrofolate
Dihydropteroate synthtase
Tetrahydrofolate
Dihydrofolate reductase
(-)
(-)
Sulfa drugs
Pyrimethamine
Methotrexate Trimethoprim
protozoa
Eukaryotes/humans
Bacteria

Deficiency of Folate :Causes : • Malabsorption syndromes
• Drugs – Valproic acid – Neural tube defects Sulfasalazine Methotrexate – DHFR inhibitors Alcohol –
• Increased demands – Pregnancy Lactation

Def manifestation:
• Megaloblastic anemia • Homocysteinuria
• Neural tube defects in fetus.

Anemia with MCV > 100• Megaloblastic anemia: form of anemia whose cellular and
nuclear features are characteristic of but not always specific for B12 or folate. It can affect leucocytes and platelets too.
• Macrocytic anemia : increased cell size of RBCs only. The cause can be anything. No changes to leucocytes and platelets.
• Pernicious anemia: reserved for B12 def due to lack of gastric Intrinsic factor. Infact most of the time these persons will not have anemia.

Vitamin B12
• Only animal source – vegetarians ??• Only water soluble vitamin that can be stored
upto some extent• Contains cobalt.
• Synthetic preparation : injectables 1. Hydroxycobalamin2. Cyanocobalamin – easily crystalized and
extracted from bacteria.

Vitamin B12
1. Methyl cobalamin – predominant function in plasma
• Converts homocysteine to methionine with transfer of methyl group from Methyl THF.
• Enzyme – homocysteine methyl transferase/methionine synthase
2. Deoxyadenosylcobalamin – mitochondrial
• Converts methylmalonyl Co-A to succinyl co-A• Enzyme – methyl malonyl Co-A mutase


Absorption of B12:
• Salivary glands – R binder (Haptocorrin-1)
• Gastric parietal cells – Intrinsic factor (IF) HCl – release B12 from food
• Binding of B12 and R-binder in stomach.
• Binds to IF + B12 in duodenum after action of pancreatic enzymes.
• Absorbed in the ileum – cubulin receptors
• Transported by (Haptocorrin -2)

Conversion of methyl malonyl Co-A to succinyl Co-A
Methyl malonyl Co-A mutase
(B12)

Deficiency manifestation:• Megaloblastic anemia
• Methylmalonic aciduria
• Neurological manifestation:
a) Myelopathy – myelin loss, axonal degeneration and Gliosisb) Larger fibres are affected – posterior and lateral columns –
Subacute combined degeneration of spinal chord. c) Loss of vibratory and position sense, ataxia. Intact motor
fibres

Causes :
• Vegan diet
• Pernicious anemia – atrophic gastritis
• Malabsorption syndrome – affecting ileum
• Bacterial overgrowth
• Short bowel syndrome
• Fish tapeworm – diphyllobothrium

Biochemical basis:• Hematological - Folate trap – decreased
methylation of DNA
• Neurological – 1. Abnormal propionate metabolism2. Accumulation of methyl malonyl Co-A –
toxin3. Abnormal fatty acid synthesis and
myelination

Megaloblastic anemia:Vitamin B12 def Folate Def
• Neurological manifestations present
• Methylmalonic aciduria • Pernicious anemia• Develops in years• Vegan diet• Absent• Schilling test
• Absent neurological manifestations
• Absent • Not related• Develops in months • Alcoholism • Neural tube defects in
foetus

Homocysteine
Cystathionine
Cysteine
Methionine
S- Adenosyl Methionine
(SAM)
S- Adenosyl Homocysteine
Methyl THF
THFB12
One carbon donors
PLP
PLP
Cystathionine β synthase
Cystathioninase
Homocysteine methyl transferase
Homocysteine metabolism:

Hyperhomocysteinemia:
• B6 def• Cystathionine beta synthase • Folate def• B12
Increased homocysteine and methionine
Increased homocysteineDecreased methionine
Increased methyl malonic acid in urine

Complications:
• Free sulfur – donates electrons to various molecules to reduce to form water.
• Now the sulfur of homocysteine reacts with sulfur of various proteins to form disulfide links and attach to proteins.
• Clinical features – marfanoid habitus, deep vein thrombosis, atherosclerosis, lens dislocation, joint contractures etc.

Schilling test :
• Stage 1 : oral vitamin B12 plus intramuscular vitamin B12
• Stage 2 : vitamin B12 and intrinsic factor
• Stage 3 : vitamin B12 and antibiotics
• Stage 4 : vitamin B12 and pancreatic enzymes

DHF
THFMethylene THF
Methyl THF
Methionine
Homocyeteine
SAM
SAH
Cystathionine
Cystathionine
B6
B6
B12
B6
MTHFR
DHFR
TSd-UMP
d-TMP
MethenylTHF
FormiminoTHF
THF
FIGLU
GLU
Formyl THF
THF
2 steps in purine synthesis
MS/HMT
Cystathionine beta synthase
Cystathioninase
Integrated metabolism:
SHMT
GlySer