MEASLES. Measles Highly contagious, acute exanthematous respiratory disease with a typical clinical...
-
Upload
vanessa-davidson -
Category
Documents
-
view
217 -
download
0
Transcript of MEASLES. Measles Highly contagious, acute exanthematous respiratory disease with a typical clinical...
Measles
Highly contagious, acute exanthematous respiratory disease with a typical clinical picture and a characteristic enanthem: Koplik’s spots
Family: Paramyxoviridae Genus: Morbillivirus
Classic measles: 1. Incubation 10-14/7
- enters through resp epithelium / conjunctiva, replicates locally,
spreads to regional lymphatic tissue -
disseminates to RES via blood stream
Classic measles: 2. Prodrome• 3 /7 but up to 8/7 - appearance of symptoms : fever, malaise, anorexia and then cough, coryza, conjunctivitis
- enanthem – Koplik’s spots
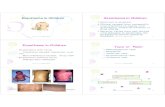
Koplik’s spots• Pathognomonic
• “Grains of salt against a red back ground”
• Occurs 48hr before rash• Often disappear with appearance of the rash
Classic Measles: 3. Exanthem Maculopapular, blanching Cranial-caudal progression Face – neck, trunk and extremities 3-4 / 7 later – fade, changes to
brownish colour with fine desquamation
Classical measles: 4. Recovery Clinical improvement after 48hrs
Rash fades after 3 days No more fever after > 3/7 after rash
appeared
Diagnosis of measles
WHO: laboratory diagnosis – IgM IgM: can be undetectable on the
first day of exanthem -- from 3rd day onwards for 30days
IgG: from day 7 of rash – peaks @ 14/7
False +: Parvo B19
Viral cultures from mononuclear cells resp secretions conjunctival swabs urine
Special facilities, difficult
Complications
Fever > 3/7 after onset of rash = complications
Developing countries – mortality 10%
Poor nutritional status Pregnant women Immunocompromised patients
Pneumonia
2’ bacterial pneumonia Streptococcus pneumonia
Streptococcus pyogenes Heamophilus influenza Staphylococcus aureus
Viral pneumonia – giant cell
Neurological complications Acute disseminated
encephalomeningitis
Subacute sclerosing panencephalitis
Acute disseminated encephalomyelitis
• Demyelinating • During recovery phase – within 2/52 of exanthem • Post-infectious auto-immune process• Fever, headache, neck stiffness, ataxia,
myoclonus, seizures, mental status
changes • LP : lymphocytic pleocytosis elevated protein• Residual neurological abnormalities
Subacute sclerosing panencephalitis• Progressively fatal degenerative CNS
disease• 7-10yrs after measles• ? Pathogenesis – persistent CNS measles
infection• Stages: stage 1 – soft neurological signs
stage 4 – severe deterioration,
flaccidity, decorticate
rigidity and
autonomic dysfunction
• Tracheobronchitis• Otitis media• Corneal ulceration and keratitis• Myocarditis• Pericarditis• Mesenteric lymphadenitis• Appendicitis• Diarrhoea
Modified measles
Similar to classic measles, but milder 17 – 21/7 Partial immunity - babies: transplacental transfer
of AB - live vaccine, with incomplete antibody response - rare: previous measles
Atypical measles
• Previously vaccinated with killed vaccine
• 7-14/7: fever, headache, cough, pleuritic pain
• Rash: from extremities to trunk (vesicular, petechial, purpuric,
urticarial)• Can cause severe illness• Not infective• IgM: @ onset of rash: titre< 1:5 day 10: 1:1280• Broad differential
Immune-supressed patients
• @ risk for severe, progressive measles• Atypical presentation: - absence of rash - any rash – purpura /
desquamating - giant cell pneumonia - measles inclusion body
encephalitis - up to 6/12 later• Deficient antibody synthesis • Biopsies
Isolation
Infective 5/7 before exanthem till 4/7 after it started
Aerosol spread Strict respiratory isolation Private room with negative air
ventilation Masks should be worn at all times
Contra-indications
HIV with CD4 < 200 Glucocorticoid therapy >2mg/kg 20mg alternate days - wait 1/12 Leukaemia in remission – wait 3/12 Pregnancy Gelatine allergy Thrombocytopenia
Post exposure prophylaxis: Immunoglobulin At risk: Immunocompromised Pregnancy Babies < 1yr
Within 6/7 of exposure
However, if not high risk and < 72hrs after exposure = Vaccinate