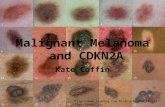
Malignant melanoma- risk factors (continued)
-
Upload
noble-osborne -
Category
Documents
-
view
29 -
download
0
description
Transcript of Malignant melanoma- risk factors (continued)

Malignant melanoma- risk factors (continued)
• Familial melanoma (10-15% of patients)• Dysplastic nevi • Large congenital nevi- about 6% develop MM

Clinical appearance
• ABCD criteria: Asymmetry Border irregularity Color variation Diameter->6mm


Growth patterns
• Radial growth:– Tendency of melanoma to grow horizontally
within the epidermis and superficial dermis, often for a prolonged time.
– During this stage ,melonoma cells do not have capacity to metastasize• lentigo maligna,• superficial spreading and• acral/mucosal lentiginous

• Vertical growth– The melanoma cells grows downwards into
deeper dermal layers– This event is clinically marked by the development
of a nodule in a relatively flat radial growth lesion– Develops capacity to metastasize

Clinicopathologic types of Malignant melanoma
• Lentigo maligna: -Sun-exposed areas of elderly white patients, usually
the face -Flat, slow-growing, prolonged in situ phase (ABCD
criteria) -Proliferation of atypical melanocytes along the basal
layer




Superficial spreading melanoma
• The most common type of melanoma (70%)• Most commonly diagnosed in the fourth and fifth
decades• Can occur in any location but more in intermittently
exposed skin• Macroscopic-ABCD criteria apply• Nodule appearance- usually implies deep invasion• Microscopically- uniform atypical melanocytes, single
and nesting




Acral lentiginous melanoma
• Appears on the palms, soles and subungual areas
• Diagnosed in older age groups• More common in black and oriental people • 10% of melanoma



Nodular melanoma
• Represents about 15% of melanomas• Can affect all body surfaces, mainly the
trunk, head and neck• Associated with short duration before
diagnosis• ABCD criteria do not apply: can present as well-circumscribed
smooth nodule in normal skin or in a nevus



• Microscopy:– Cells are arranged in the form of poorly formed
nests or nodules– The individual melanoma cells are • Large cells• Large irregular nuclei• Prominent red eosinophilic nucleoli



Laboratory methods
• Melanin stains- Fontana-Masson
• Immunohistochemistry- S-100 protein- HMB-45- more specific,


Spread and metastases
• Epidermis to papillary dermis, reticular dermis and subcutaneous fat
• Regional lymph node metastases are highly predictive of visceral metastases
• Distant metastases- liver, lungs, gastrointestinal tract, bone, CNS

Staging
• Tumor thickness (Breslow’s system)- most important prognostic factor. Measured from the top of the granular layer/ulcer base to the deepest tumor cell
-Stage I:Less than 1mm- -Stage II:Between 1to 2mm- -Stage III:Between 2 to 4mm- -Stage IV:Over 4mm-

Prognostic factors (continued)-Level of invasion
• Clark’s system: 5y survival level I- intraepidermal (in situ) 100% level II- in the papillary dermis 100% level III- filling the papillary dermis 88% level IV- in the reticular dermis 66% level V- in the subcutaneous fat 15%• Level of invasion has a significant impact on
survival






Prognostic factors- continued
• Ulceration- the second most important prognostic determinator of the primary tumor- bad prognosis
• Mitotic activity- relationship between mitotic activity and prognosis: high mitotic rate associated with a bad prognosis

Good Luck!……..