Coronary Artery Disease By: Amanda Robinson. Facts Blood flows into the heart muscle by way of two...
-
Upload
candace-bradford -
Category
Documents
-
view
216 -
download
0
Transcript of Coronary Artery Disease By: Amanda Robinson. Facts Blood flows into the heart muscle by way of two...

Coronary Artery Disease
By: Amanda Robinson

Facts
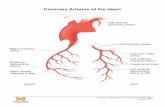
Blood flows into the heart muscle by way of two small vessels: the right and left coronary arteries.
They arise from the base of the aorta, just below the semilunar valves, and curve around the heart to supply the myocardium with nutrients and oxygen.


Statistics
CAD is the most common type of heart disease.
It is also the leading cause of death in the United States in both men and women.
Men are generally at greater risk of CAD than are women.
However, the risk for women increases after menopause.

Risk Factors
Modifiable- Smoking- Obesity- Exercise and inactivity- Stress and anger - High blood pressure - High cholesterol- Diabetes
Nonmodifiable- Age- Sex- Family history

Prevention
Stop smoking Have regular medical checkups Control your blood pressure Check your cholesterol Keep diabetes under control Get moving Eat healthy foods Maintain a healthy weight Manage stress

Etiology
Occurs when the coronary arteries become hardened, narrowed, or occluded by:
- Plaque build up - Blood clots - Damage or injury This buildup of plaque (cholesterol,
lipids, & cellular debris) is known as atherosclerosis.
- Obstructions of 75% or higher results in ischemia & increases the risk of death.



Pathophysiology
As the plaque increases in size, the insides of the coronary arteries get narrower and less blood can flow through them.
Eventually, oxygen and blood flow to the heart muscle is reduced or cutoff which can result in:
- Angina- Arrhythmias- Heart attack- Heart failure - Shortness of breath


Signs & Symptoms
Objective Data- Diaphoresis (sweating)- Syncope (fainting episode)- Dysrhythmias (irregularity
in normal heart rhythm)- Blood pressure changes
Subjective Data- Chest pain (Angina)- Shortness of breath
(SOB)- Fatigue- Palpitations (hard/rapid
beating pf the heart)- Weakness- Dizziness - Light-headedness

Labs & Diagnostics
An Electrocardiogram (ECG ) - Takes a record of the heart’s activity Echocardiogram (a visual record of the heart’s activity) Stress Test- A treadmill exercise or drug induced heart exercise activity with Persantine or
Adenosine Cardiac Catheterization- Measures the pressure and blood volume relationship within a heart to measure
cardiac competence by injecting a radio plaque dye into the arteries and taking x-rays)
Computerized Tomography Magnetic Resonance Imaging (MRI) CBC (identify levels of all blood-cell types in a sample) Serum Lipids (↑ HDL is desired, but LDL’s ↑ the risk of cardiovascular diseases) Serum Cardiac Markers - To test blood for Troponin I and Myoglobin which are proteins released in reaction to
myocardial injury

Cardiac Catheterization


Treatment
Life style changes- Smoking cessation- Healthy diet- Regular exercise Medication Therapy Surgical Interventions

Medications
Angiotensin-converting enzyme (ACE) inhibitors
- Captopril (Capoten) Beta blockers- Lopressor (Metoprolol) Calcium channel blockers- Cardizem (Diltiazem HCL) Cholesterol medications (Statins)- Atorvastatin (Lipitor) Angiotensin II Receptor Blockers- Diovan (Valsartan) Vasodilators- Nitroglycerin or Isosorbide

Surgical Interventions
Angioplasty (PTCC- Percutaneous transluminal coronary angioplasty)
- The insertion of a balloon into the clogged artery to break up plaque and open the artery.
Stent placement- The placement of an expandable, mesh like structure
designed to open the artery and maintain vessel patency by compressing arterial walls resulting in vasodilation.
Coronary artery bypass surgery (CABG) - A graft done to bypass the occluded area of the
arteries using the saphenous vein in the leg or a mammary artery).
Coronary brachytherapy- Radiation used to reopen an artery. Laser revascularization- A beam used to create tiny channels in heart walls
so new vessels can grow.



Nursing Interventions/Rationales
Monitor the patient’s vitals frequently
Auscultate the patient’s heart sounds
Assess patency of patient’s airways
Provide a low stimulus and stress free environment and/or maintain bed rest
Administer medications on time/regularly
Educate patient and family Provide the patient with
emotional support/physical comfort
To watch for condition changes in the patient
Assess heart dysrhythmias Check oxygenation status of
the patient To decrease cardiac excitement
and workload of the heart To relieve patient of any pain
he/she may have To prevent/manage the patients
condition To decrease the patients
fear/anxiety and pain

Patient Teaching
About the disease Purpose of therapies Proper procedures of
therapies and use of medications
Importance of stress management

Possible NANDA’s
Activity intolerance r/t ischemia pain or immobility Fatigue r/t decreased cardiac output and/or lack of
oxygenation Decrease cardiac output r/t cardiac insufficiency Ineffective coping r/t fear of/uncertainty about the
disease process Anxiety r/t change in health status or fear of death Pain r/t ischemia of the myocardial heart muscle Knowledge deficit r/t the disease process, risk
factors, and therapeutic management

Prognosis
Outcome is variable. Some people can maintain a
healthy life by changing diet, stopping smoking, and taking medications as long as they are closely monitored.
Others may require more drastic measures, such as surgery.
Everyone is different, but one important factor is detecting CHD early and treating it appropriately.