Common Orthopaedic Conditions Associated with Complex Neurodisability
description
Transcript of Common Orthopaedic Conditions Associated with Complex Neurodisability

Common Orthopaedic Conditions Associated with Complex
NeurodisabilityLindsey Hopkinson and Victoria Healey
Heads of Paediatric PhysiotherapyPhysiocomestoyou Ltd
www.physio4thekids.com

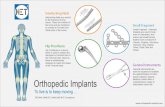
Contents Complex Neurodisability
At risk of developing: Hip displacement Scoliosis (spinal curve) Lower limb contractures- Hamstring Muscles- Adductors Muscles- Hip flexor Muscles- Calf muscle

Complex NeurodisabilityCerebral PalsyNeuromuscular DiseaseStrokeAcquired Head InjuryBrain TumourMetabolic DiseasesGenetic Syndromes

Neurodisability and Orthopaedic ConditionsGrowth of the
musculoskeletal systemWeightMuscle strengthAltered toneActive volitional
movement / wheelchair bound
Image from www.rch.org.au

Hip Development The hip joint can be described
as a ball and a socket The ball is the head of the
thigh bone and sits in the socket of the pelvis
At birth the socket is shallow and the head of the thigh bone is not placed deep within the socket
Normal motor development causes changes within the hip joint resulting in a mature adult stable hip joint over time
Children with neurodisability can have hip joint problems resulting in hip displacement

Hip Displacement Displacement is when part of
the ball is uncovered by the socket (migration percentage)
Reasons :- Decreased weight-bearing
forces altering the remodeling of the femur with growth
- Reduced ambulation / ability to walk (motor function)
- Muscle weakness - Abnormal tone in the muscles
around the hipImage from www.hipchicksunite.com

How to monitor your child’s hips as they GrowHip Surveillance
(Active screening programme) DISCUSS with your PHYSIOTHERAPIST
X-ray from 30 months unless clinical indication for x-ray prior to this for all children with a neurological disability

Possible indications for parents / carers of hip displacement
• Pain on movement (rotation / abduction)
• Leg length• Tightness within thigh
muscles• Change in sitting posture• Pain / change in walking
pattern of ambulant children
• Windswept posture Image from www.besbiz.eu.com

Scoliosis / spinal curve Your child’s therapist should
monitor your child’s spine as they grow
Muscle weakness / abnormal muscle tone increases the risk of scoliosis
Differing diagnosis will affect the risk of scoliosis for your child
Growth results in progression of pre existing spinal curves
Mobility

How to monitor your child’s spine Lead healthcare professional to
monitor EARLY as your child grows with Clinical examination
X-ray – Orthopaedic Consultant SPINAL
Observations Skin Creases Rib hump back and front Pelvis alignment in sitting /
posture in sitting LEANING OVER Pain Loss of sitting balance

Lower Limb Contractures - Hamstrings
Hamstrings:- 3 muscles are on
located at the back of the thigh.

Signs of shorteningHow to monitor for shortening:Ambulant- Crouch gait - Unable to straighten knees- Growth spurts- Feel
Non ambulant- Tilting pelvis backwards in wheelchair- Unable to sit with pelvis neutral and legs bent at 90 degrees so feet
on foot plates- Feel
** Physiotherapist clinical examination and observation of gait / sitting posture

Lower Limb Contractures – Hip Flexors
Hip Flexors (non ambulant children most at risk)
Muscles located at the front of the hip
Signs of shortening include:Raised buttocks when lay on
tummyUnable to lie on their back with leg
straightCrouch / anterior tilted pelvis
Image from www.edoszkop.com

ADDUCTOR MUSCLES Muscles located between your child’s inner thigh
Signs of shortening including:Scissoring Difficulty with dressing
and hygieneSitting postureWindswept posture
Image from www.wikipedia.org

CALF MUSCLES Soleus and gastrocnemius muscles – back of lower leg
How to monitor for shortening: Difficulty tolerating Splints
Ambulant: Walking on toes Heels flat but feet rolling
inwards
Non ambulant: Feet pointing downwards
Image from www.oandp.com

When we refer to Orthopaedic ConsultantsWalking Children: Unable to straighten knee(s) Unable to bring ankle to
neutral Asymmetric abduction of hip Foot deformities (foot turning
in or out - varus / valgus) Unable to straighten hip fully
to neutral (< 10⁰) Tight hamstring – popliteal
angle < 50⁰ degrees

When we refer to Orthopaedic Consultants Non walking children: Reduced hip abduction <40⁰ Pain Hamstring tightness 60⁰ < Unable to extend hips – hip flexion
contracture < 20⁰ Unable to straighten knees <20⁰ If toes pointing down more than
20⁰ In line with hip surveillance ANY at risk patients re spine / sign
of scoliosis EVEN if flexible

ConclusionEnsure as a parent you have discussed
orthopaedic monitoring with a member of your healthcare team and discussed hip and spine surveillance to ensure timely and optimal referral to the correct team.

QUESTIONS
?

www.physio4thekids.com