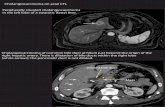
Cholangiocarcinoma - RWellner.ppt
-
Upload
jay-r-plogio -
Category
Documents
-
view
485 -
download
8
description
Transcript of Cholangiocarcinoma - RWellner.ppt

Cholangiocarcinoma
Rachel B. Wellner MD, MPH Rachel B. Wellner MD, MPH Mount Sinai HospitalMount Sinai Hospital
Department of SurgeryDepartment of Surgery
Team III ConferenceTeam III Conference

Definition of Cholangiocarcinoma
Bile duct cancers arising from ductal epithelial cells
Refers to cancers arising in the intrahepatic (~5-15%), perihilar (~60-70%), or distal (extrahepatic ~25%) biliary tree
Represents approx. 3% of all gastro-intestinal malignancies


Definition of Cholangiocarcinoma
Bismuth-Corlette Classification subdivides perihilar cholangiocarcinomas based on pattern of involvement of hepatic ducts Type I: tumors occurring below the confluence of the
left and right hepatic ductsType II : tumors reaching the confluenceTypes IIIA/IIIb: tumors occluding the common hepatic
duct and either the right or left hepatic duct Type IV: tumors that are multicentric, or that involve
the confluence and both the right or left hepatic duct
Klatskin tumors occur at the bifurcation of the proper hepatic duct


Risk Factors
Primary Sclerosing Cholangitis 0.6-1.5% annual incidence of cholangioCA.
Choledocal Cysts and Caroli’s Disease 0.7 % risk for first 10 years, 6.8 % risk for
second ten years, and 14.3 % thereafter Clonorchis and Opisthorchis Cholelithiasis and hepatolithiasis Toxic exposure (Thorotrast) Lynch syndrome II and multiple biliary
papillomatosis

Pathology
Adenocarcinoma (90%) Slow growing, locally invasive, mucin-producing Perineural spread, metastases uncommon
Three subtypes of adenocarcinoma Sclerosing
Majority of cholangiocarcinomas Characterized by an intense desmoplastic reaction Early ductal invasion leads to low resectability rates
Nodular Constricting annular lesion of the bile duct
Papillary Present as bulky masses occurring in the bile duct lumen Present early with biliary obstruction Highest resectability rates

Clinical
Triad Cholestasis Abdominal pain (30-50 %) Weight loss (30-50 %)
Pruritus (66 %) Clay-colored stools, dark urine. Jaundice (~90 %) Hepatomegaly RUQ mass Courvoisier's sign Intrahepatic cholangioCA typically presents without
biliary obstruction

Laboratory
Elevations in: Total bilirubin (>10 mg/dL) Direct bilirubin Alkaline phosphatase (usually increased 2- to
10-fold) 5'-nucleotidase Gamma glutamyltransferase
Transaminase levels initially normal With chronic biliary obstruction, liver
dysfunction may ensue with elevation in ALT/AST and PT

Differential Diagnosis
Choledocholithiasis Benign bile duct strictures (usually
postoperative), Sclerosing cholangitis Compression of the CBD (secondary to
chronic pancreatitis or pancreatic cancer)

Diagnosis
Tumor markers Serum CEA >5.2 ng/mL(sensitivity 68%,
specificity 82%) Biliary CEA CA 19-9
Radiographic studies Transabdominal ultrasound- may reveal ductal
dilatation (intrahepatic >6mm) CT/helical CT- can also detect vascular invasion
Helical CT (esp. portal venous phase)- can delinieate nodal basins
May be superior to MRI with respect to predicting resectability
MRCP- may be coming the imaging modality of choice (high PPV,NPV)

Diagnosis
Cholangiography ERCP or PTC Useful if suspected level of obstruction is distal Preoperative drainage of the biliary tree Obtain diagnostic bile samples or brush cytology
(low sensitivity) Endoscopic ultrasound
Useful for visualizing distal tumors and regional nodes
Can be used for EUS-guided biopsy of tumors and enlarged nodes
PET High glucose uptake of biliary duct epithelium
Angiography (rarely used) Staging laparoscopy


Diagnosis
Role of Staging laparoscopy Tissue diagnosis important in the setting of:
Strictures of unknown origin (e.g. bile duct stones, PSC)
Family/patient request for a definitive diagnosis
Prior to chemotherapy or radiation therapy


Management
Poor prognosis- avg. 5-year survival ~5-10%
Resectability rate superior for distal tumors resectability rates for intrahepatic 60%, perihilar
56%, and distal lesions 91% (Nakeeb A; Pitt HA, JHU 1996)
Negative margins achieved in 20-40% of proximal tumors cases, 50% of distal tumor cases
Current data in evolution

Management
Accepted guidelines for resectability (accurately determined at operative exploration) Absence of N2 nodal metastases or distant liver
metastases Absence of vascular (portal vein, hepatic artery)
invasion Absence of extrahepatic adjacent organ invasion Absence of disseminated disease

Management
Pre-operative biliary decompression Liver dysfunction increases postoperative
morbidity and mortality Arch Surg 2000 (Cherqui et. al.)
Study demonstrated increased post-op morbidity in jaundiced patients not undergoing pre-operative drainage (vs. nonjaundiced patients)
Pre-operative portal vein embolization Induce liver hypertrophy to increase limits of
safe resection No demonstrated improvement in clincial
outcome

Management
Surgical Procedures Distal lesions: pancreaticoduodenectomy (5-yr survival
rates 15-25%) Intrahepatic cholangiocarcinoma: hepatic resection (3-yr
survival rates 22- 66%) Perihilar cholangiocarcinoma (5-yr survival rates 10-
45%; outcomes in PSC patients dismal) Type I and II lesions: en bloc resection of
extrahepatic bile ducts and gallbladder with 5 to 10 mm bile duct margins, regional lymphadenectomy with Roux-en-Y hepaticojejunostomy.
Type III and Type IV lesions: hepatectomy and portal vein resection

Management
Adjuvant radiation therapy Adjuvant radiation aimed at achieving local contral,
decreased recurrence (no RCTs) Retrospective series demonstrate a benefit in patients
with incompletely resectable lesions Unclear benefit in patients with completely resected
tumors Adjuvant chemotherapy (mitomycin, 5-FU)
Benefit of adjuvant chemoradiotherapy for completely resected patients unclear
Some benefit seen when combined with radiation in patients with incomplete resection
Single multi-center prospective randomized trial (Japan, Takada et. al. in Cancer, 2002) showed no benefit with chemotherapy in patients with both curative and non-curative resections

Management
Neoadjuvant therapy Typically not offered to patients with
cholangiocarcinoma due to poor functional status at presentation
Used in selected patients (McMasters, Am J Surg 1997)
3/9 patients had a pathologic complete response (6/9 showed different degrees of histologic response)
Margin-negative resections were possible in all nine patients receiving neoadjuvant therapy.
Palliative treatment aimed at relieving biliary obstruction, pain50-90% of patients with cholangiocarcinoma present
with unresectable disease

References
Bismuth, H, Nakache, R, Diamond, T. Management strategies in resection for hilar cholangiocarcinoma. Ann Surg 1992; 215:31.
Cherqui, D, Benoist, S, Malassagne, B, et al. Major liver resection for carcinoma in jaundiced patients without preoperative biliary drainage. Arch Surg 2000; 135:302.
McMasters, KM, Tuttle, TM, Leach, SD, et al. Neoadjuvant chemoradiation for extrahepatic cholangiocarcinoma. Am J Surg 1997; 174:605.
Nakeeb, A, Pitt, HA, Sohn, TA, et al. Cholangiocarcinoma. A spectrum of intrahepatic, perihilar, and distal tumors. Ann Surg 1996; 224:463.
Roayaie, S, Guarrera, JV, Ye, MQ, et al. Aggressive surgical treatment of intrahepatic cholangiocarcinoma: predictors of outcomes. J Am Coll Surg 1998; 187:365.
Takada, T, Amano, H, Yasuda, H, et al. Is postoperative adjuvant chemotherapy useful for gallbladder carcinoma?. A phase III multicenter prospective randomized controlled trial in patients with resected pancreaticobiliary carcinoma. Cancer 2002; 95:1685.