Approach to patient with ovarian cysts
-
Upload
yahyia-al-abri -
Category
Health & Medicine
-
view
168 -
download
0
Transcript of Approach to patient with ovarian cysts

Approach to patient with Ovarian cysts
Done by: Yahyia Al-Abri90440

Outline
• Definition of ovarian cyst• Case scenario• How to approach
– History, physical examination , investigation, management.
• Functional ovarian cyst• Benign ovarian neoplasm • Mixed ovarian neoplasm • Ovarian cancer

ovarian cyst
• An ovarian cyst is a sac filled with liquid or semiliquid material that arises in an ovary.
• These cysts can develop in females at any stage of life, from the neonatal period to postmenopausal
• Most ovarian cysts, occur during infancy and adolescence, which are hormonally active periods of development.
• Most are functional in nature and resolve without treatment.



Case • 19 years old Omani lady, Unmarried,
Presented to the A&E with history of Abdominal left iliac fossa pain started 15 minutes prior coming to the hospital.
how will you approach this patient?

History Examination
Investigation Management
h o w w i l l y o u a p p r o a c h t h i s p a ti e n t ?

History
• Most patients with ovarian cysts are asymptomatic
• Pain or discomfort may occur in the lower abdomen
sudden, unilateral, sharp pelvic pain Cyst rupture
bilateral, dull pelvic pain. Theca-lutein cysts
painful and heavy periods and dyspareunia Endometriomas

History • Associated symptoms
– Patients may experience abdominal fullness, bloating and tenesmus.
• Irregularity of the menstrual cycle.• Young children may present with precocious puberty
(Granulosa-theca cell tumors) and early onset of menarche.
pressure on the bladder
Micturition may occur frequently
polycystic ovarian syndrome
infertility, oligomenorrhea,

Our case She described the pain as colicky, intermittent, located in
left iliac fossa radiates to the suprapubic area. Severe pain Pain better slightly on lying down No h/o of nausea or vomitting No h/o fever No urinary symptoms No PV bleeding. Her LMP was at 07/11/2015 Regular period

Our case
Past medical history: • She has similar episodes of pain since March
2015, several visits to the student clinic and A&E for the same complain
• CT abdomen was done(prominent ovaries with cysts likely functional) on 26/3/2015
• Follow up US on 20/9/2015: evidence of large cyst in left adnexa measuring 7.5x6.2 mm in size

What is your differential diagnosis ?
• Ovarian cyst accidents – cyst rupture,– haemorrhage – torsion
• Acute PID

Physical examination
• General examination • Abdominal examination • Pelvic examination

Physical examination
• A large cyst may be palpable on abdominal examination
• Functional cyts • mobile, unilateral, and not associated with ascites.
• Tender to palpation

Physical examination Signs Diagnosis
hirsutism, obesity, and acne Polycystic ovarian syndrome
hyperpyrexia complications of ovarian cysts, such as ovarian torsion
diffusely tender abdomen with rebound tenderness and guarding
hemorrhage or peritonitis
cachexia and weight loss, lymphadenopathy in the neck, shortness of breath, and signs of pleural effusion.
Advanced malignant disease
Tachycardia and hypotension. Hemorrhage due to cyst rupture
T

Our case
O/E:• vitals: normal • Abdomen:
– mild tenderness in the lower abdomen – no guarding ,no rigidity

Investigation (laboratory)
• No laboratory tests are diagnostic for ovarian cysts.
• Investigations aid in the differential diagnosis – Urinary pregnancy test– CBC ( Anemia + infection)– Urinalysis (UTI and stones)– Endocervical swabs– Cancer antigen 125

Investigation (radiology )
• Ultrasonography– primary imaging tool for a patient considered to
have an ovarian cyst– help to define a cyst’s morphologic characteristics– Follow up exclude ovarian neoplasm/show
resolution of a cyst – A normal ovary is 2.5-5 cm long, 1.5-3 cm wide,
and 0.6-1.5 cm thick

Ultrasonography
• simple ovarian cysts – uniformly thin, rounded wall and a unilocular – hypoechoic or anechoic.– They usually measure 2.5-15 cm in diameter, and
posterior acoustic enhancement
• Complex cysts – Multilocular ,thickening of the wall, projections
into the lumen or on the surface,

Radiology
• CT scanning – more sensitive but less specific than
ultrasonography in detecting ovarian cysts.– best in imaging hemorrhagic ovarian cysts or
hemoperitoneum due to cyst rupture– to distinguish other intra-abdominal causes
• CT scanning should be avoided in pregnancy,– MRI

Procedure
• Diagnostic laparoscopy– To inspect a suggestive adnexal cystic mass.– advantage of decreased morbidity, improved
postoperative recovery.

Our case
• Labs done in the A&E: - Hb 11.6 WCC 8.7 - U&E Normal- Tumor markers normal
• U/S pelvis done: – The right ovary is normal in size and appearance.
hyperechoic lesion about 5 cm on left ovary that is new from old scan that can be hemorrhagic complex cyst & can not rue out/in torsion

Calculation of the Risk Of Malignancy Index (RMI)
Risk of Malignancy Index = A x B x C. A cut-off value of 200 discriminate a benign from malignant mass with a Sensitivity of (87%) and a specificity of(97%).

Functional Cysts - Management• If the RMI is low and the cyst is considered to be functional.
– Wait and re-examine the patient after her next menses.
– Low-dose contraceptive agents may be given to suppress gonadotropin levels and prevent development of another cyst.
• If it is solid, painful, or fixed or has an elevated RMI.– surgical exploration may be necessary.
– Laparoscopic cystectomy to allow histologic evaluation may be needed to differentiate between a functional and a neoplastic ovarian cyst.

Ovarian Cyst Rupture
• Conservative in stable patient.
• Surgical care – laparoscopy or laparotomy, depending on clinical
presentation, amount of blood in the abdomen, patient stability.

Our case
PLAN:• consent taken for :
– Emergency laparoscopy ovarain cystectomy ,+/- salpingectomy +/- salpingo oopherectomy
– risk of converted to laparotomy ,risk of veesels ,bowel ,bladder injuries ,risk of thrombosis , risk of infection all explined to the pateint ,pateint`s father and mother
• Cross match, NPO• Shift direct from A&E to the OT

Our case Laproscopic findings:
– Left ovarian cystectomy– Post-op Diagnosis: hemorrhagic cyst with clots, No ovarian torsion– Findings: Normal R ovary , pelvis, uterus and upper abdomen
• Day 1 Post op: She is complaining of mild pain at surgical site.
- Mobilizing.- Voided well.- To be discharged with encouraging oral hydration and analgesia.- Appointment for tracing histopathology after 6 wks- Earlier to A&E if any complains as explained.

What are the differential diagnosis of ovarian mass?

Specific type Pathogenesis
Follicular cystsLutein cystPolycystic ovaries
Functional
Salpingo-oophoritisPyogenic oophoritis-puerperal, abortal, or related to an intrauterine deviceGranulomatous oophoritis
Inflammatory
Endometriomas Metaplastic
Premenarchal years-10% are malignantMenestruating years-15% are malignantPostmenopausal years-50% are malignant
Neoplastic

Functional cyst

follicular cysts
-Arise when physiologic release of the mature ovum fails (follicle fail to rupture).-Follicular growth continues.-Excessive stimulation by FSH.-Lack of the normal preovulatory LH surge.- 3 cm _Rarely grow larger than 10 cm.-Most are asymptomatic.-Larger cysts may cause pelvic discomfort or heaviness.-Thin-walled, unilocular-Usually unilaterally.

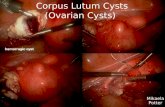
Corpus luteum cyst (lutein):
• Result when a corpus luteum fails to regress following the release of an ovum.
• It is the most common pelvic mass encountered within the 1st trimester.
• most spontaneously involute at the end of the 2nd trimester.
• -Most are asymptomatic and resolve with observation and analgesia but If persist => surgical.

Hemorrhagic corpus luteum cysts
• Results from invasion of ovarian vessels into corpus luteum
• They are more likely to cause symptoms and more likely to rupture.
• Ruptured hemorrhagic corpus luteum cysts can result in a Hemoperitoneum requiring surgery

Theca-lutein cysts
• hypertrophy of the theca interna cell layer in response to excessive stimulation from hCG.
• Present with – hydatidiform mole.– multiple gestation.– choriocarcinoma.– ovulation induction with gonadotropins or clomiphene.
• usually bilateral.• may become quite large (>30 cm) • characteristically regress slowly after the gonadotropin level falls.

luteoma of pregnancy
• Prolonged hCG stimulation during pregnancy leading to hyperplasic reaction of ovarian theca cells.
• Appear as brown to reddish-brown nodules that may be cystic or solid.
• Multifocal and usually bilateral• Can cause maternal virilization in 30% of women
and ambiguous genitalia in a female fetus. • regress spontaneously postpartum.


Benign neoplastic ovarian tumors
Divided by cell type of origin
Epithelial Stromal Germ cell
•Mucinous•Serous •Brenner
•Fibromas•Granulosa-theca cell tumors•Sertoli-Leydig cell tumors
•Benign cystic teratoma

US/Cytology PRESENTATION DESCRIPTION TYPE
•Often multilocular•Histologicaly contain Psammoma bodies (calcified concentric concretions)
10% bilateral
• most common is serous cystadenoma
•70 % benign•5-10%borderline malignant•20% to 25% are malignant
Serous
•Resembles endocervical epithelium•Often multilocular•Often associated with a mucocele of the appendix
Huge size,Often filling entire pelvis•may be complicated by pseudomyxoma peritonei
•85% benign•20% of epithelial tumors
Mucinous
•Has a large fibrotic component that encases epithelioid cells that resemble transitional cells of the bladder.
•a small, smooth solid ovarian neoplasm.
•usually benign•33% are associated with mucinous epithelial elements.
Brenner
1- Epithelial ovarian neoplasms


US/Cytology •PRESENTATION •DESCRIPTION TYPE
Form encapsulated, solid, smooth-surfaced tumor, composed of spindle- shaped cells.
• Non-functioning• associated with Meigs
syndrome
• benign Fibroma
-solid-yellow appearance-Histologic hallmark of cancer is small groups of cells known as Call-Exner bodies
Estrogen-producingfeminizing effects (precociouspuberty, menorrhagia,postmenopausal bleeding)
•Can be associated with endometrial cancer
•Inhibin is tumor marker
Granulosa-theca cell tumors (benign or
malignant)
Androgen-producing virilizing effects (hairsutism, deep voice, recession of front hair)
Can measure elevated androgens as tumor markers
Sertoli-leydig cell tumors (benign or
malignant)
Sex Cord–Stromal Ovarian Neoplasm

MCQ
• A 4-year-old girl is noted to have breast enlargement and vaginal bleeding. On physical examination, she is noted to have a 9-cm pelvic mass. Which of the following is the most likely etiology?
• A. Cystic teratomaB. DysgerminomaC. Endodermal sinus tumorD. Granulosa-theca cell tumorsE. Mucinous tumor

MCQ
A. Fitz-Hugh-Curtis syndromeB. Lung cancerC. Meig's syndromeD. Leriche's syndromeF. Liver failure
A 47 year old woman is admitted to the gynaecology ward after the discovery of an ovarian mass on an annual gynaecological checkup. On general examination she is found to have a distended abdomen, with possible ascites, and bilateral pleural effusions. Biopsy of the mass reveals a fibroma.
Given the signs and symptoms, what is the diagnosis?

Germ cell tumors
•Occur at any age.•Make up about 60% of ovarian neoplasms occurring in infants and children.
•Most common benign cystic teratoma (dermoid cyst).•10-15% are bilateral.• Slow growing tumor.•Diagnosed b/w 25-50 yrs of age.•<10 cm in diameter.

Teratomas
Dermoid cysts (teratomas) are one of the most common types of cysts , half are diagnosed in women between 25 and 50 years
Composed primarily of ectodermal tissue (sweat & sebaceous glands, hair follicles, and teeth), with some mesodermal and rarely endodermal elements

A dermoid cyst (mature cystic teratoma) after opening the abdomen.

Mixed Ovarian Neoplasms
• Ovarian tumor in which the neoplastic elements are composed of more than one cell type
• More solid than epithelia ovarian tumor • The most common is the cyst-adeno-fibroma.• It is benign but it may predispose to
malignant dysgerminoma.

Benign Ovarian Tumors- Management
• Benign epithelial ovarian neoplasms are generally treated by unilateral salpingo-oophorectomy.– cystectomy with preservation of the depending on the
neoplasm (cystic teratoma) and age of patient.– Gonadoblastoma, dysgenetic ovaries = bilateral
salpingo-oorphrectomy
• Appendectomy should also be done in mucinous cystadenoma. Because it is associated with a mucocele of the appendix

• Dermoid cyst (teratoma) • Granulosa cell tumour • Corpus luteum cyst • Mucinous cystadenoma • Follicular cyst • Serous cystadenoma
• If ruptures may cause pseudomyxoma peritonei
• The most common type of epithelial cell tumour
• May contain skin appendages, hair and teeth

MCQ
A. Follicular cystB. Teratoma (dermoid cyst)C. EndometriomaD. Ovarian adenocarcinomaE. Ovarian fibroma
A 20-year-old female presents with a 3 month history of abdominal pain. Abdominal ultrasound shows a 8cm mass in the right ovary. Histopathological analysis reveals Rokitansky's protuberance. What is the most likely diagnosis?

Ovarian cancer
• It is the leading cause of death from gynecologic cancer because it is difficult to detect before it disseminates.
• Most women with ovarian cancer are in the 5th or 6th decade of life.
• Population screening is not feasible because ultrasonography and available tumor markers, lack specificity and sensitivity for early-stage disease.

Ovarian Cancer- Clinical features
• In early-stage disease, vague abdominal pain or bloating – Other symptoms include dyspareunia, urinary frequency
or constipation and menstrual irregularity or Postmenopausal bleeding.
• In advanced-stage disease, patients most often present with abdominal pain or swelling (from the tumor itself or from associated ascites).
• In bimanual pelvic examination– a solid, irregular, fixed pelvic mass.

Ovarian Cancer- Management
• Depending on the stage of the cancer.
• In postmenopausal women they are best treated by a total abdominal hysterectomy and bilateral salpingo-oophorectomy.
• In premenopausal women , the contralateral ovary and the uterus can be preserved in some types.

References
• Essentials of obstetrics and gynecology,HACKER and MOORES.
• Medscape• Abduljabbar HS, Bukhari Y. Review of 244 cases
of ovarian cysts. Saudi Med J 2015; Vol. 36 (7)• www.ncbi.nlm.nih.gov/pubmed/21991700• https://www.womenshealth.gov/publications/
our-publications/fact-sheet/ovarian-cysts.html