Treattnent of achalasia: Pneutnatic dilationdownloads.hindawi.com/journals/cjgh/1990/658025.pdf ·...
Transcript of Treattnent of achalasia: Pneutnatic dilationdownloads.hindawi.com/journals/cjgh/1990/658025.pdf ·...

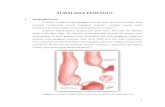
BENIGN ESOPHAGEAL DISEASE
Treattnent of achalasia: Pneutnatic dilation
G VANTRAPPEN, MD, Pl ID, J J ANSSENS, MD, PHD, P RUTGEERTS, MD, PHD
ABSTRACT: Forceful dilation of the cardia is the treatment of choice for achalasia. This therapy can be carried out using a homemade system or using commercially available dilators. Pneumatic dilation yields 77% good or excellent results in patients with achalasia, while 8. 7% have mo<lerate improvement and 14.4% are not improved. The main complication is perforation, occurring in 2.5%. Perforation can be treated medically with success. In the authors' series of now almost 1000 patients, only one died. Pneumatic dilation is a safe and effective procedure for the treatment of achalasia. Can J Gastroenterol 1990; 4(9):596-598
Key Words: Achalasia , Esophagus, Pneumatic dilation
Le traitement de l'achalasie
RESUME: La dilatation forceedu cardia est le traitementde choix de l'achalasie. Cette therapie peut s'effectuer au moyen d'un instrument mis au point par le praucien ou d'un dilatateur commercialise. La dilatation pneumatique donne 77% de resultats satisfaisants ou excellents, alors que 8, 7% des patients s'ameliorcnt modcrement et que 14,4% d'entre eux ne reagissent pas. La perforation survicnt clans 2,5% des cas et constitue la complication majeure; elle se traite medicalement avec succes. Dans notre serie de plus de 700 patients, un seul deces est survenu. La dilatation pneumatique est une procedure snre et efficace utilisee clans le traitement de l'achalasie.
THE CURRENT METHODS OF TREAT
ment of achalasia aim co improve the passage of food into the stomach by weakening the insufficiently relaxed sphincter (1-3). This can be achieved
by stretching it forcefully (dilation) or by dividing the ci rcular muscle (cardiomyotomy). Whatever treatment is chosen the sphinctenc function should be preserved sufficiently to prevent reflux.
Department ofMedicme, Division of Gasrroenrerology, University Hospital Gaschuisberg, Leuven, Belgium
Correspondence and reprints: Dr G Vancrappen. ProfessOT of Medicine, Head, Department of Medicme, Dwision of Gastroenterolog:v, Unwersity Hospital Gasthuisberg, Herestraat 49, 3000 Leuven, Belgium. Telephone (016) 2142 18
PNEUMATIC DILATION Homemade system: To obtain goo:l, long term results a forceful dilation ri the sphincter is neces~ary. Several methods are currently available. For many years a pneumatic system with sippy-cype dilator has been used(!). The dilator is assembled and thoroughly tested before each dilation (Figure I).
To faci litate the introduction of the dilator a latex balloon is mounted aroun<l the nylon bag. The day before dilation the patient swallows a stnng (Mersilene number 1) weighted by a mercury filled bag. The string becomes anchored in the small bowel and acts as a guide for the dilator. If the esophagui is markedly widened and sigmoid. shaped, the mercury filled bag may fa,! to pass inco the stomach spontaneously. It may be possible to introduce it mto the stomach with the help of a fibre. optic endoscope, or a Seldinger catheter may gently be passed under fluoroscopic control into the stomach and used instead of the Mersilene string as a guide for the dilator. Before introducing the balloon, a metal wire with an eye at the end is threaded over the string into the stomach, providing a rigid guide which ensures safe imroduc, tion of the <lilacor. If it is not possible to pass this ngid wire over the string, a
596 CAN J 0ASTR0ENTEROL VOL 4 No 9 DECEMBER l99i)

7 lillillilMII I Ii lliill ii iii I ii fPilWVIIPCIIII Cllli IOI~
2 ""®"'''"'"'"'mnmnmmmm,muu~
] '""f """''''''"""''"''''": ... ~
Figure 1) Mounting of the pneumatic dilator. Two latex balloons (condoms), one inside the other, s11TTounded by a nylon bag, are mounted on a mewl spiral terminated by an oli11e bougie ( I) (Mueller, Chicago). The nylon bags (2) ha11e a length of 15 cm and a dimneter of 3 co 5 cm, depending upon rhe bag selected. At both ends the diameter of the bag wpers to about I .5 cm. A 50 cm nylon ribbon is sewn to the proximal end of the bag (3). On this ribbon a mark is made which 111d1cates 40 cm from rhe middle of the bag. ft also helps to ensure that the entire dilator, bag and spiral swy wgecher when the dilator is pulled back at the end of the procedure. A poly11inyl cube with a noncompress1ble end (the tubing from an intra11enous infusion set) is inserted between the balloons ( 4) When balloons and bags are ligated at both extremities ( 5) , insufflation of air through the polyvinyl tube produces a cylinder, the diameter and shape of which are determined by the nylon bag. Pressure 111 the balloon can be measured by connecting the poly11inyl tube to a sphygmomanomecer
more flexible wire should be used. If even such a flexible wire fails to enter deeply enough into the stomach, the dilator may be passed directly over the Mersilene string. The dilator is pushed down until the middle of the balloon reaches the level of the cardia (about 41 cm from the incisor teeth). The correct position of the balloon is a lways checked by fluoroscopy. In most cases an indentation on the left lateral aspect of the inflated balloon inJicates the
level of the diaphragm. The balloon 1s then insufflated to a pressure of 200 mmHg for the first minute, then to 300 mmHg for an additional minute. Initially a balloon with a diameter of 3 cm is used; at each subsequent session the calibre of the dilator is increased. Nylon bags with diameters of 3, 3.5, 3.8, 4 .2, 4 .5 and exceptionally 5 cm should be avai lable. Three to four dilations are performed in most patients until the criteria for adequate dilation
CAN J GASTROENTEROL VOL 4 No 9 DECEMI\ER 1990
Pneumatic dilation
are met. These incluJe J1sappearance or substanrial reduction of the pressure in the lower esophageal sphmcter and , on fluoroscnpy, easy emptying of the esophagus anJ wiJenmg of the previously narrow lower esophageal segment.
A liquid diet is given for a couple of Jays and the esophagus evacuated before the first dilation m order to
prevent aspiration pneumonia. The Jilation is performed with the patient in the upright position (standing or sitting} co avoid aspLrnt1on nf secrettcms into the airways. If pam becomes severe, J1lation is stoppeJ. If the patient fails to cooperate suffic iently because of youth or mental disease, dilation is abandoned. Usually pain disappears or diminishes considerably within 2 mins after dilation ends. Analgesics arc not given. A small amount of blood on the dilator as ll 1s removed is normal and does not mJicate a complication. Patients must refrain from Jrinkmg or eating for 2 h after Jilatil)n. If pain persists longer, perforatinn must be suspected. In that case, it is of the utmost importance that the pat ienr nm take anythmg hy mouth anJ he given antibiotics as soon as possible. If the patient's condition 1s good 2 h after dilation, no other measures are necessary. Commercially available sys tems: Microvas1ve achalasia dilators have 30, 35 and 40 mm diameter polyethylene balloons of length LO cm anJ mounted on a I 00 cm long, 7 French shaft. Placement over a flexible gu1dewire b easy. This system is suitable for t reatment of the maiority of cases a !though the homemade system can better be aJapted to a particular patient.
RESULTS OF DILATION In the years 1957-85 the authors
treated 700 patients by thi~ method of pneumatic dilation. The immediate results were excellent. After the first dilation there was considerable improvement of dysphagia. By the end of treatment all patients stated that they were ahle to eat without distress. Regurgitation also Jisappeared completely. Attacks of substernal pain did nor always Jisappear immediately; m some
597

V ANmAPPEN el al
cases it tonk several weeks before relief was obtained, although crampy pain was less severe than before dilation. Most patients gained weight rnpidly.
Late results could he evaluated for 93% of patients. They were subdivided into four groups according to the following cmeria. Group l kxcellent results) included pauents who were completely free from symptoms. Group 2 (good results) comprised patients who experienced dysphagia or pain of short duration only occasionally: les~ than once a week there was hesitancy of food retrosternally, lasting from a few seconds co a couple of minutes, and d1sappeanng on fluid intake; there was no weight loss or regurgitation. Group 3 ( moderate results) pauents expenenceJ Jysphagia at least once a week. The sensation of food sticking in the esophagus did not last longer than a few minutes and d1J not prevent the patient from finishing his or her meal. It was not accompanied by regurgitation or weight loss. TI1ese patients were markedly improved compared with the pretreatment situation. Group 4 (poor results) patients had frequent dysphagia, 1cgurgitat1on or weight loss, or daily retrostemal pain.
At the time of evaluation, 77°/o of the patients had good or excellent results, 8. 7% moderate results anJ 14.4% poor results; 93% of patients were significantly unproved hy treatment. The results of pneumatic Ji lat ion m patients with diffuse esophageal spasm were less satisfactory.
COMPLICATIONS OF DILATION
The major immediate complication of dilation is perforation of the esophagus at the cardia. Up to 1985 the authors had treatcJ 700 patients and performeJ usually three ()r four pneumatic dilations per patient. Perfora tion occurreJ m 2.5% of the patients. A diagnosis of perforation was
598
maJc whenever extravasation of contrast material coulJ be demonstrated radiologically.
It is very important after each dilarnm to observe the patient carefully for possihle complications. A perforation must be suspected if the pam docs n0t d11rnnish 30 to 60 mins after dilation or if it becomes worse. Crampy pains similar to attacks experienced spontaneously hefore treatment may be expected. However, if pain radiates to the back or left lower thorax, o r if respiration becomes painful, perforation must be suspected. After a few hours breath sounds may Jiminish and there may be ep1gastric tenderness. A rad1ograph may show blurring of the left coscophrenic angle or a pleural effusion. HyJropneumothorax occurred only once m this series and was associated with a ir in the mediastinum.
Whenever a patient expenenced prolonged or abnormally severe pam after dilation, oral feeding was stopped and parenteral treatment with broad spect rum antibiotics started. The next day a radiographic examination with gastrografin was performed to check whether there was a perforation. If not, oral feeding was resumed a:, soon as the fever passed. If there was a perforation, broad spectrum antibiotics, analgesics and parenteral feeding were continued. Pleural aspiration or suction Jramage were sometimes indicated. The majority of these patients improved considerably after about three days of conservative therapy. After that, food could be administered through a gastric tube, but this was not started immediately as it could cause vomiting. [( surgical repair of the perforation was deemed necessary, 1t was best performeJ shortly after the acc ident. Residual abscesses of mediastinum of pleural cavity may require subsequent surgical dramage.
Perforation of the carJ1a, caused by pneumatic dilation, can usually be sue-
cessfully treated cnnservauvely. M~ patients with proven perforation healed completely after parenteral alimentatlon and broad spectrum anti· biorics for one or two weeks. Sometimes a pleural effusion was aspirateJ. Two patients had to be treated by 1ur• gical drainage of the mediastmum. Only one of the 700 patients <lied, a woman 83-ycar:;-olJ to whom fooJ was given by mistake, in spite ofa ra<l1olog1• cally demonstrated perfmat1cm.
Other complications were prolonged pam, a peak fever or a sterile pleural effusion. The overall complication rate was 4. "3%. Late complicatiom were rare after pneumatic dilation. In the authors' experience symptomauc reflux occurred m less than l %.
CONCLUSION Pneumatic dilation is che treatmcnc
of choit.e for most pauents with achalasi,1. It is a safe procedure in experienced handl> and can he used even
when the esophagus 1s widened and tortuous or when the patient is cachccuc. A previously unsuccessful Heller operation 1s not a contramd1cation to pneumatic d ilation, if organic ohstruction can be ruled out. The 1mmcJiatc and long term results compare favorab. ly w1th those of surgery, and stcnosmg reflux esophagitis is rare after pneumatic dilation.
REFERENCES I. V,mtrnppen G, l lellcmam J, Dcloof W,
Valembo1s P, VanJenhrouckeJ. Treat· ment of achalas1a with pneumatic Jilatat1ons. Gut 197 1, 12:268-75.
2. Vantrappcn G, Van Go1Jscnhoven G, Verbeke S, Van Den Bcrghc G, VanJcnhrouckc J. ManomctnL stuJ1cs m achalas1a of rht• carJia, before and after, pneumatic dilatiom Gastrocnterology 1963;45: 117-25.
1. Vantrappcn G, Jans.sem J, l lcllcmamJ, Core mans G . Achalasia, Jiffu,c csoph,1geal sp,ism, and related motil1ty disorders. Ga,trocntcrology, 1979; 76:450-7.
CAN J CASTROENTl'ROL VOL 4 No 9 nu ·EMBER 1m

Submit your manuscripts athttp://www.hindawi.com
Stem CellsInternational
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
MEDIATORSINFLAMMATION
of
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Behavioural Neurology
EndocrinologyInternational Journal of
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Disease Markers
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
BioMed Research International
OncologyJournal of
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Oxidative Medicine and Cellular Longevity
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
PPAR Research
The Scientific World JournalHindawi Publishing Corporation http://www.hindawi.com Volume 2014
Immunology ResearchHindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Journal of
ObesityJournal of
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Computational and Mathematical Methods in Medicine
OphthalmologyJournal of
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Diabetes ResearchJournal of
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Research and TreatmentAIDS
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Gastroenterology Research and Practice
Hindawi Publishing Corporationhttp://www.hindawi.com Volume 2014
Parkinson’s Disease
Evidence-Based Complementary and Alternative Medicine
Volume 2014Hindawi Publishing Corporationhttp://www.hindawi.com