THE ROLE OF SEMINAL VESICLE SECRETION (SVS) 7 PROTEIN IN BONE HOMEOSTASIS · THE ROLE OF SEMINAL...
Transcript of THE ROLE OF SEMINAL VESICLE SECRETION (SVS) 7 PROTEIN IN BONE HOMEOSTASIS · THE ROLE OF SEMINAL...

THE ROLE OF SEMINAL VESICLE SECRETION (SVS) 7 PROTEIN IN BONE
HOMEOSTASIS
WILLIAM CUNDAWAN, B. Sc B. MedSci (Hons)
This thesis is submitted to fulfil the requirements of the University of Western Australia
for the degree of
DOCTOR OF PHILOSOPHY 2013
The work presented in this thesis was performed at the University of Western Australia,
School of Pathology and Laboratory Medicine and School of Surgery, Centre for
Orthopaedic Research, QEII Medical Centre, Nedlands, Western Australia

Table of Contents Declaration 1
Scientific Abstract 2
Abstracts and Award 6
Acknowledgements 7
List of Figures 9
Abbreviations 12
CHAPTER 1: BONE BIOLOGY 17
1. Introduction to Bone Biology 18
1.1 Osteoclast 20
1.1.1 Osteoclast phenotype 20
1.1.2 Osteoclast differentiation and function 23
1.2 Osteoblast 30
1.2.1 Osteoblast phenotype 30
1.2.2 Osteoblast differentiation and function 32
1.3 Molecular Communication Between Osteoclasts and 37
Osteoblasts
1.3.1 Osteoblast regulation of the osteoclast 39
1.3.2 Osteoclast regulation of the osteoblast 42
1.3.3 Bidirectional signalling between osteoclasts and 44
osteoblasts
1.4 Bone Diseases 45
1.4.1 Osteoporosis 46
1.4.2 Osteopetrosis 47
1.4.3 Paget’s disease of bone (PDB) 48
CHAPTER 2: SEMINAL VESICLE SECRETION (SVS) 7 PROTEIN AND 50
LY-6 PROTEIN FAMILY
2.1 Introduction 51
2.2 Seminal vesicle secretion (Svs) 7 51
2.3 Svs7 as a secreted member of Ly-6 protein family and the 52
biological importance of other Ly-6 proteins
2.4 Identification of Ly-6 family member, Svs7, as a putative 57
osteoclast-derived coupling factor
CHAPTER 3: HYPOTHESIS AND AIMS 61
3.1 Hypothesis 62

3.2 Aims 62
CHAPTER 4: MATERIALS AND METHODS 64
4.1 Materials 65
4.1.1 Cell lines 65
4.1.2 Bacterial strain 65
4.1.3 Chemical reagents 65
4.1.4 Tissue culture reagents 67
4.1.5 Cytokines 67
4.1.6 Enzymes 67
4.1.7 Antibodies 68
4.1.8 Vectors 68
4.1.9 Purchased kits and systems 69
4.1.10 Oligonucleotide primers 69
4.1.11 Other materials 69
4.1.12 Software 71
4.1.13 Equipments 71
4.1.14 Centrifugation 73
4.2 Buffers and Solutions 73
4.2.1 General solutions 73
4.2.2 Media and agar 78
4.3 Animals 79
4.3.1 Svs7 transgenic (TG) mice generation 79
4.3.2 Svs7 knockout (KO) mice generation 79
4.3.3 Mouse tail tip DNA genotyping 79
4.3.4 MicroCT analysis 81
4.3.5 Histology on hindlimbs and prostate of Svs7 TG and KO 81
mice
4.3.5.1 Fixation, decalcification (for hindlimbs), tissue 81
processing, tissue embedding, and sectioning
4.3.5.2 Dewaxing and H&E staining 82
4.3.5.3 Dewaxing and TRAP staining 82
4.3.5.4 Processing, embedding, and sectioning of non- 83
decalcified bone samples
4.3.5.5 Goldner trichrome staining for the non- 84
decalcified bone samples

4.3.6 Double calcein labelling of Svs7 KO mice 84
4.4 General Methods 85
4.4.1 Isolation and culture of primary cells 85
4.4.1.1 Isolation and culture of bone marrow cells 85
4.4.1.2 Isolation and culture of spleen cells 86
4.4.1.3 Isolation and culture of calvarial osteoblasts 86
4.4.2 Cell culture of COS-7 cell line 86
4.4.3 Cryopreservation of cell lines for long-term storage 87
4.4.4 RNA extraction 87
4.4.5 RNA concentration measurement 88
4.4.6 RT reactions 88
4.4.7 Polymerase chain reaction (PCR) and quantitative 89
PCR (qPCR)
4.4.8 DNA agarose gel electrophoresis 92
4.5 Cell Biology 92
4.5.1 In vitro RANKL-induced osteoclastogenesis, TRAP 93
staining, and osteoclasts count
4.5.2 Analysis of osteoclast nuclei and area (osteoclast fusion 93
mechanism)
4.5.3 In vitro osteoclast bone resorption assay 94
4.5.3.1 Preparation of bone slices 94
4.5.3.2 Mature osteoclasts culture on bone slices 94
4.5.3.3 SEM and analysis of osteoclast resorption pits 95
4.5.3.4 Osteoclast bone resorption assays using Corning 95
Osteo Assay plates
4.5.4 CFU alkaline phosphatase (ALP) staining for osteoblast 96
differentiation assay
4.5.5 In vitro bone marrow stromal cells-derived osteoblasts bone 96
nodule formation (mineralization) assay
4.5.6 MTS proliferation assay on Svs7 KO BMM 96
4.6 Cloning Method 97
4.6.1 Restriction enzyme digestion of DNA 97
4.6.2 DNA extraction and purification from agarose gels 97
4.6.3 Cloning strategy and ligation to construct 98
pGEM-T Easy Svs7

4.6.4 Cloning strategy and ligation to construct 98
pcDNA3.1 Svs7-V5 His
4.6.5 Transformation and plating of the transformed cells 98
4.6.6 Bacterial culture and maintenance 98
4.6.7 Plasmid extraction and isolation 99
4.7 Experimental Methods 99
4.7.1 Cell transfection and collection of conditioned medium 99
expressing Svs7 protein
4.7.2 Luciferase assay 100
4.7.3 Flow cytometry analysis on fixed and stained Svs7 KO BM 100
cells
4.7.4 Fluo-4AM intracellular calcium assay on Svs7 KO osteoclast 101
4.7.5 Cell lysis procedure for Western Blot (WB) protein analysis 102
4.7.6 Velocity density gradient centrifugation 102
4.7.7 Measuring protein concentration 103
4.7.8 Western Blot (WB) SDS-PAGE system 103
4.7.8.1 Preparation of the SDS-PAGE system 103
4.7.8.2 Protein transfer to nitrocellulose membrane 105
4.7.8.3 WB reaction 105
4.7.8.4 Stripping the membranes 106
4.8 Statistical Analysis 106
CHAPTER 5: CHARACTERISATION OF SVS7 TRANSGENIC MICE 107
5.1 Introduction 108
5.2 Results 109
5.2.1 Tissue distribution of Svs7 gene 109
5.2.2 Generation of the Svs7 transgenic (TG) mice 109
5.2.3 Histological phenotyping of Svs7 TG mice 112
5.2.4 Body weight and radiographic assessment of Svs7 TG mice 112
5.2.5 MicroCT analysis of tibia, femur, and lumbar vertebrae of 112
Svs7 TG mice
5.2.6 Svs7 TG mice exhibit a normal bone mass 115
5.2.7 Histological assessment of Svs7 TG bones 115
5.2.8 Svs7 TG mice exhibit an unaffected osteoclast differentiation 121
in vitro
5.3 Discussion 121

CHAPTER 6: CHARACTERISATION OF SVS7 KNOCKOUT MICE 128
6.1 Introduction 129
6.2 Results 129
6.2.1 Genotyping and characterisation of Svs7 KO mice 129
6.2.2 Slow mice breeding process and gross body phenotypic 131
examination of Svs7 KO mice
6.2.3 Gross tissues phenotypic (macro vs. microscopic) 131
assessment of Svs7 KO mice
6.2.4 Svs7 KO mice exhibit a reduced bone mass phenotype 134
6.2.5 Svs7 KO bone histology 134
6.2.6 Bone formation activity in vivo is unaffected in Svs7 KO 139
mice
6.3 Discussion 139
CHAPTER 7: INVESTIGATION OF INTRINSIC CELLULAR 144
MECHANISM IN SVS7 KNOCKOUT MICE
(OSTEOCLAST AND OSTEOBLAST)
7.1 Introduction 145
7.2 Results – Part 1: Intrinsic cellular mechanism in osteoclasts 146
derived from Svs7 KO mice
7.2.1 Svs7 KO BMM cultures have increased osteoclastogenesis 146
in vitro
7.2.2 Svs7 KO osteoclasts are larger and have more nuclei than 146
WT
7.2.3 WT and Svs7 KO mice have comparable hematopoietic 149
stem cells (HSCs) and osteoclast progenitor cells
7.2.4 Svs7 KO mice exhibit unaltered expression levels of key 152
osteoclast marker genes
7.2.5 Osteoclast bone resorption activity is not affected in Svs7 152
KO mice
7.2.6 Svs7 KO osteoclasts are more sensitive to Ca2+ influx in 157
response to RANKL and extracellular Ca2+ stimulation
7.2.7 Svs7 KO mice exhibit elevated NFATc1 and ATP6v0d2 160
proteins expression during RANKL-induced osteoclastogenesis
7.2.8 Svs7 protein treatment inhibits the activation of NFAT 164
promoter luciferase activity

7.3 Results – Part 2: Osteoblasts from Svs7 KO mice are 166
phenotypically comparable to WT cells
7.3.1 Svs7 KO primary calvarial osteoblasts exhibit an 166
unaffected proliferation rate in vitro
7.3.2 No defect is observed in Svs7 KO alkaline phosphatase 166
(ALP) osteoblast differentiation in vitro
7.3.3 Svs7 KO osteoblasts exhibit an unaffected bone formation 169
activity in vitro
7.3.4 Analysis of osteoblast marker genes expression levels in 169
Svs7 KO mice
7.4 Discussion 172
CHAPTER 8: GENERAL SUMMARY AND FUTURE DIRECTIONS 176
8.1 Overview of thesis and general discussion 177
8.2 Future directions 184
8.2.1 The role of Svs7 in bone homeostasis 184
8.2.2 The role of Svs7 in osteoclast and osteoblast differentiation 185
and activation
CHAPTER 9: BIBLIOGRAPHY 188
APPENDIX 223

Declaration This is to certify that all the work contained herein was performed by myself, except
where indicated otherwise.
William Cundawan
W/Prof Jiake Xu
Assoc Prof Nathan Pavlos
W/Prof Minghao Zheng
Willi C d
W/Prof Minghao Zheng

2
Scientific Abstract Bone, a living tissue that forms our skeletal frame, is continuously remodelled
throughout life by the complementary activities of bone-resorbing osteoclasts and bone-
forming osteoblasts. The cell-to-cell interaction between osteoclasts and osteoblasts is
tightly regulated to achieve bone homeostasis and is governed by the production and
exchange of various coupling factors. However, the nature and identity of these factors
are still largely obscure. In search for novel osteoclast-derived coupling factors, we
have previously employed subtractive hybridization-based differential screening to
probe for differentially expressed genes between osteoclasts and their mononuclear
progenitors. Using this approach, we have successfully identified seminal vesicle
secretion (Svs) 7, known as calcium (Ca2+) transport inhibitor (Caltrin), as a candidate
gene that was robustly upregulated during receptor activator of NF-κB ligand
(RANKL)-induced bone marrow macrophages (BMM) differentiation into mature
osteoclasts (Davey 2008; Phan 2004). Svs7 is exclusively expressed by osteoclasts in
bone and liberated as a secreted factor.
Svs7 is a secreted member of Lymphocyte antigen (Ly)-6 protein family, sharing the
common three fingered proteins (TFP)/Ly-6/urokinase-type plasminogen activator
receptor (uPAR) motif, has been shown to be involved in several cellular signalling
pathways. Furthermore, previous observations by Davey 2008 describe the protective
effects of recombinant purified Svs7 protein (500μg/kg daily injection) against the loss
of trabecular bone volume, trabecular thickness, and trabecular number at the distal
femoral metaphysis of ovariectomised mice (oestrogen deficiency-induced bone loss
mouse model). From here, it was hypothesized that Svs7 might be an important
regulator of bone homeostasis. To address this, a two-armed approach was employed
using genetically modified mouse models. The first approach involved the generation
and characterisation of Svs7 transgenic (TG) mice. Following the confirmation that
Svs7 transgene was successfully incorporated and expressed at both the transcriptional
and protein levels, histological assessment of tissues, known to abundantly express Svs7
(i.e. prostate), from the TG mice was performed. Despite being successfully expressed,
no obvious morphological difference was observed in these prostate tissues between
WT and Svs7 TG mice. To further explore the potential role of Svs7 in bone, X-ray
analysis was performed. The result showed that there was no striking difference in
skeletons between WT and Svs7 TG mice. More precise Svs7 TG bone phenotypic
examination was conducted by performing microCT and histology analysis on

3
calvariae, proximal tibia, distal femur, and vertebral body of the lumbar bone. MicroCT
analysis together with histological assessment revealed that all major bone parameters
(trabecular bone volume, trabecular separation, trabecular thickness, and trabecular
number) were comparable between WT and Svs7 TG mice. Moreover, tartrate-resistant
acid phosphatase (TRAP) histology sections and histomorphometry data further
confirmed that there was no significant difference in the number of TRAP-positive
osteoclasts in the primary epiphysis between WT and Svs7 TG hindlimbs, implying that
Svs7 TG mice exhibit normal bone mass and structure. As Svs7 is exclusively
expressed in osteoclasts in bone, osteoclast formation was assessed by performing in
vitro time course of RANKL-induced osteoclastogenesis. The results indicated that
osteoclast formation in Svs7 TG mice was comparable to that of WT littermates. Thus,
Svs7 overexpression in Svs7 TG mice was insufficient to determine the physiological
role of Svs7 in bone.
Another approach to investigate the potential role of Svs7 in bone involved the
generation and characterisation of Svs7 global knockout (KO) mice. The deletion of
exon 2 and 3 of Svs7 gene, which encode for the TFP/Ly-6/uPAR domain, led to the
complete absence of Svs7 gene and protein in Svs7 KO mice. Despite an unexpectedly
slow mice breeding process, Svs7 KO mice displayed no overt gross body phenotype.
In addition, no obvious difference was observed in the phenotype of major organs and
tissues between WT and Svs7 KO mice, indicating that Svs7 is not a requirement for
organogenesis. To assess the potential bone phenotype of Svs7 KO mice, microCT
analysis on WT and Svs7 KO femurs was performed. The results showed that there
were significant reductions in trabecular bone volume and trabecular number in Svs7
KO mice compared to WT, suggesting that Svs7 KO mice exhibit a phenotype of
osteopenia/osteoporosis. Furthermore, this reduced bone mass phenotype was also
confirmed histologically in sections of Svs7 KO hindlimbs. TRAP histology sections
and histomorphometry data revealed that there was a trend of increase in osteoclast
number near growth plate region in Svs7 KO hindlimbs compared to WT, while no
significant difference in bone formation activity in vivo was observed between WT and
KO mice. Together, these results indicate that Svs7 is a novel regulator of bone
homeostasis, possibly owing to a defect in osteoclast differentiation observed in Svs7
KO mice.

4
To elucidate the intrinsic cellular mechanism underlying the osteoporotic phenotype of
Svs7 KO mice, a series of in vitro assays for osteoclast and osteoblast differentiation
and activity were performed. In vitro time course of RANKL-induced
osteoclastogenesis showed that there was a significant increase in osteoclast number in
Svs7 KO BMM cultures at day 3 and 5 of osteoclastogenesis compared to WT.
Interestingly, relative to WT, Svs7 KO-derived osteoclasts were significantly larger and
possessed more nuclei (i.e. ≥ 11) than WT at day 5 of osteoclastogenesis, while no
detectable defects in Svs7 KO early osteoclast progenitor and hematopoietic stem cell
populations were observed. Despite the increase in osteoclast number and size, there
was no significant difference in osteoclast bone resorption activity or the expression of
known osteoclast marker genes between WT and Svs7 KO mice, indicating that Svs7
has a potential intrinsic role in osteoclast differentiation but not in osteoclast activity.
By performing Fluo-4AM intracellular Ca2+ assays on WT and Svs7 KO osteoclasts, it
was found that KO osteoclasts were more sensitive to Ca2+ influx than WT in response
to RANKL and extracellular Ca2+ stimulation, implying that, together with the observed
larger osteoclast size in Svs7 KO BMM cultures, Svs7 may function as a regulator of
osteoclast fusion. Consistent with this position, western blot analysis on cell lysates of
time course RANKL-induced WT and Svs7 KO BMM differentiation into osteoclasts
showed a significant elevation in nuclear factor-activated T cell cytoplasmic 1
(NFATc1) (at day 3 of osteoclast differentiation) and a trend of increase in d2 subunit of
v0 domain of V-H+ATPase complex (ATP6v0d2) fusogenic protein expression in KO
osteoclasts compared to WT, indicating that Svs7 may regulate osteoclast fusion
through the Ca2+-NFATc1 signaling pathway, which has its main effect on ATP6v0d2
protein expression. On the other hand, no significant differences were observed in
osteoblast differentiation and mineralization activity in vitro between WT and Svs7 KO
mice.
In conclusion, these studies constitute the first comprehensive genetic approach to study
the involvement of Svs7 in bone. Moreover, these studies demonstrate that Svs7 KO
mice exhibit an osteoporotic phenotype, with a significant increase in osteoclast number
and size and no observable defects in osteoblast differentiation and activity in vitro and
in vivo. Through the Ca2+-NFATc1 signaling pathway, Svs7 has shown to regulate
osteoclast differentiation and fusion but not osteoclast activity. Therefore, Svs7 plays an
important regulatory role in the maintenance of bone homeostasis, via an autocrine

5
action on osteoclasts, and thus might represent a potential target for the management
and treatment of osteoclast-related bone diseases.

6
Abstracts and Award 1. Cundawan W, Tickner J, Abel T, Chim SM, Kular J, Zheng MH, Pavlos N, and Xu
J (2012) “Seminal Vesicle Secretion (SVS) VII, upregulated by RANKL in
Mature Osteoclasts, Regulates Osteoclast Precursor Proliferation,
Differentiation, and Bone Homeostasis”. Australian and Scientific Medical
Research (ASMR) Week Symposium, Perth, Western Australia. (Oral Presentation)
2. Cundawan W, Tickner J, Abel T, Chim SM, Kular J, Zheng MH, Pavlos N, and Xu
J (2012) “Seminal Vesicle Secretion (SVS) VII is expressed by mature
osteoclasts and acts to regulate osteoclast precursor proliferation,
differentiation, and bone homeostasis”. 2012 Annual Australian and New Zealand
Orthopaedic Research Symposium (ANZORS), Perth, Western Australia. (Oral
Presentation)
3. Cundawan W, Tickner J, Abel T, Chim SM, Kular J, Zheng MH, Pavlos N, and Xu
J (2012) “Seminal Vesicle Secretion (SVS) VII is expressed by mature
osteoclasts and acts to regulate osteoclast precursor proliferation,
differentiation, and bone homeostasis”. 22nd Annual Australian and New Zealand
Bone and Mineral Society (ANZBMS) Research Meeting, Perth, Western Australia.
(Oral Presentation)
4. Cundawan W, Tickner J, Abel T, Chim SM, Kular J, Zheng MH, Pavlos N, and Xu
J (2012) “Seminal Vesicle Secretion (SVS) VII is expressed by mature
osteoclasts and acts to regulate osteoclast precursor proliferation,
differentiation, and bone homeostasis”. Sir Charles Gairdner Hospital Medical
Research Month Symposium, Perth, Western Australia. (Oral Presentation) 2012
Scientific Young Investigator Award 5. Cundawan W, Tickner J, Abel T, Chim SM, Kular J, Zheng MH, Pavlos N, and Xu
J (2013) “Seminal Vesicle Secretion (Svs) 7 Protein is expressed by Mature
Osteoclasts and Acts to Regulate Osteoclast Fusion”. Combined Biological
Science Meeting (CBSM), Perth, Western Australia. (Poster Presentation)

7
Acknowledgements I would like to thank my coordinating supervisor, W/Prof Jiake Xu (UWA School of
Pathology and Laboratory Medicine) for giving me the chance to do PhD in medical
research and for your excellent supervision and care. My sincere warm appreciation and
thanks go to my co-supervisor, Assoc Prof Nathan Pavlos (UWA Centre for
Orthopaedic Research, School of Surgery) for his patience, guidance, and an excellent
supervision throughout my PhD years. Your unbelievable positive attitude in medical
research and your excellent example of the integrity in life has always been there to
support me to complete my study and to learn to become a better person each day. I
would also like to thank warmly W/Prof Minghao Zheng (UWA Centre for Orthopaedic
Research, School of Surgery) for his support and advices throughout my candidature
years.
My special thanks and huge appreciation go to Dr Tamara Abel (UWA CMCA) for
your tremendous help, technical support, and advices that have contributed a lot to this
study.
My special thanks also go to Dr Jennifer Tickner and Dr Shek Man Chim (both from
UWA School of Pathology and Laboratory Medicine) and Dr Taksum Cheng (UWA
Centre for Orthopaedic Research, School of Surgery) for the friendship, help, technical
support, and advices during my study.
For my special friends, Dr Ee Cheng Khor, Dr Jasreen Kular, Dickson Phiri, and
Chulwon Chang. Thank you and I cannot express it enough to you all for the true
friendship, support, and advice. Even though very few in number, your friendship holds
a special place in my life and has helped me tremendously during my study and will
always be during my life time here in Australia. I am so sorry I haven’t been able to
catch up with you guys for sometimes but I promise I will soon.
To Euphemie, Ying Hua, and Li (UWA Centre for Orthopaedic Research, School of
Surgery) and Jacob (UWA School of Pathology and Laboratory Medicine), thank you
so much for your expertise and assistance in histology. I am really happy to have had
experiences working with you guys during my study. Thank you Jay (UWA School of
Medicine and Pharmacology) for your assistance in using BMG machine during my

8
study and thank you Dr Kathy Heel (UWA School of Pathology and Laboratory
Medicine) for your help in my flow cytometry experiments.
To James Burgess, thank you so much for helping me to get connected to the school
network and printers, with me being the frequent office mover (3 different offices
during 3-years study in the School of Pathology and Laboratory Medicine). Thank you.
To all my lab colleagues from UWA School of Pathology and Laboratory Medicine:
Bay Sie, Vincent, Ben, Dian, Lin, Ryan, and Gaurav, and from UWA Centre for
Orthopaedic Research, School of Surgery: Pei Ying, Su, Zhu Xiang, Qin An, Lin Zhen,
Louis, and Colin, thank you for your friendship, help, supports, and laugh/fun that u
guys have provided during my study.
To my office colleagues, Laura, Li and Dagwin, thank you for your friendship and
support. My loneliness and emptiness in the office during my thesis writing was slowly
disappeared after you guys came in.
For my family, especially Ama, Mum and Dad, and my brothers, thank you so much for
the love, opportunity, supports, and trusts you have given me to complete my study in
Australia. Through your unconditional love, I remember and hold God blessing in my
life every day.
To my dearest love, Audrey Chan, my whole heart fills with gratitude of thankful and
love for you every day, as from nowhere earlier years in my life, now I can picture and
know who my self really is with your extremely strong perseverance and unconditional
love and trust for me. We had been tested really hard through times but we come on top
and God has really answered our prayers. With no doubt at all, my heart and soul want
to dedicate this thesis for you. Without you, who have filled my time with unconditional
love, companion, support, and prayers, I would not able to do it. ‘I Love You So Much
and I will never give up’.

9
List of Figures Page
Figure 1.1 The four important domains of polarized, multinucleated 21
osteoclasts
Figure 1.2 Cell-to-cell contact between osteoclast and osteoblast 25
Figure 1.3 Signalling pathways in osteoclast differentiation 26
Figure 1.4 ARF cycle in bone remodelling process 31
Figure 1.5 Osteoblast differentiation from mesenchymal stem cells 33
Figure 1.6 The Wnt/ββ-catenin signalling pathway in osteoblast 38
Figure 2.1 Consensus cysteine residues and a C-terminal consensus 53
sequence motif of CCXXXXCN (TFP/Ly-6/uPAR domain)
of Ly-6 proteins family
Figure 2.2 Identification of Svs7 gene using subtractive hybridization- 58
based differential screening in RAW264.7 cells culture with
RANKL stimulation
Figure 2.3 Svs7 is the most highly expressed Ly-6 gene by mature 59
osteoclasts, shown by the microarray heatmap analysis
Figure 2.4 Svs7 gene expression in osteoclast 60
Figure 4.1 Svs7 transgenic (TG) mice generation 79
Figure 4.2 Svs7 knockout (KO) mice generation 80
Figure 5.1 Tissue distribution of Svs7 mRNA expression 110
Figure 5.2 Generation of the Svs7 TG mice 111
Figure 5.3 Histological examination of prostate of Svs7 TG mice 113
Figure 5.4 Body weight and radiographic assessment of Svs7 TG mice 114
Figure 5.5 2D and 3D microCT images of proximal tibia, distal femurs, 116
and vertebral body of the lumbar bone of Svs7 TG mice
Figure 5.6 Svs7 TG mice exhibit a normal bone mass 118
Figure 5.7 Histological examination on H&E-stained decalcified Svs7 119
TG bone samples
Figure 5.8 Histological examination on goldner trichrome and TRAP- 122
stained non-decalcified femur sections of Svs7 TG mice
Figure 5.9 Bone histomorphometry analysis on NOc/BS (N/mm) of 124
TRAP-stained non-decalcified femur sections of Svs7 TG
mice
Figure 5.10 Svs7 TG mice exhibit an unaffected osteoclastogenesis 125

10
in vitro
Figure 6.1 Svs7 gene and protein were absent in Svs7 KO mice 130
Figure 6.2 Slow mice breeding process and gross body phenotypic 132
examination of Svs7 KO mice
Figure 6.3 Gross tissues phenotypic assessment of Svs7 KO mice 133
Figure 6.4 Svs7 KO mice exhibit a reduced bone mass phenotype 135
Figure 6.5 Svs7 KO bone histology 137
Figure 6.6 Bone histomorphometry analysis on TRAP-stained 140
decalcified femur sections of Svs7 KO mice
Figure 6.7 Svs7 KO mice exhibit an unaffected bone formation 141
activity in vivo
Figure 7.1 In vitro time course RANKL-induced Svs7 KO BMM 147
differentiation into mature osteoclasts
Figure 7.2 Svs7 KO osteoclasts are larger than WT 148
Figure 7.3 Svs7 KO osteoclasts have more nuclei than WT 150
Figure 7.4 Svs7 KO mice exhibit unaltered population of HSCs and 151
early osteoclast precursor
Figure 7.5 The deletion of the Svs7 gene does not affect MAPK and 153
NF-κκB signalling pathways in Svs7 KO osteoclast
precursor
Figure 7.6 Key osteoclast marker genes expression levels are not 154
affected in Svs7 KO mice
Figure 7.7 SEM analysis (on bone slices) for Svs7 KO osteoclast bone 155
resorption activity
Figure 7.8 Corning osteo plate analysis for Svs7 KO osteoclast bone 156
resorption activity
Figure 7.9 Svs7 KO osteoclasts are more sensitive to Ca2+ influx in 158
response to RANKL and extracellular Ca2+ stimulation
Figure 7.10 Svs7 KO osteoclasts have a significant increase in 161
NFATc1 protein expression during RANKL-
induced osteoclastogenesis
Figure 7.11 Svs7 KO osteoclasts have a trend of increase in 162
ATP6v0d2 protein expression during RANKL-
induced osteoclastogenesis
Figure 7.12 DCSTAMP protein expression appears to be unaffected 163

11
in Svs7 KO osteoclasts throughout the time course of
RANKL-induced osteoclastogenesis
Figure 7.13 Svs7 protein treatment inhibits NFAT promoter luciferase 165
activity
Figure 7.14 Svs7 KO primary calvarial osteoblasts exhibit an unaffected 167
proliferation rate in vitro
Figure 7.15 No defect is observed in Svs7 KO ALP osteoblast 168
differentiation in vitro
Figure 7.16 Svs7 KO osteoblasts exhibit an unaffected bone formation 170
activity in vitro
Figure 7.17 Analysis of osteoblast marker genes expression levels in 171
Svs7 KO mice
Figure 8.1 Hypothetical model of the role of Svs7 in the regulation of 182
osteoclast fusion through the Ca2+-NFATc1 signalling pathway
Supplementary Figure 1 Serum biochemistry measurement on calcium 224
and phosphate levels in Svs7 TG mice
Supplementary Figure 2 Svs7 protein detection at the secretory vesicles 225
fraction of osteoclasts

12
Abbreviations ALP Alkaline phosphatase
α-MEM Alpha minimum essential medium
AP-1 Activator Protein 1
ARF Activation (Bone resorption) reversal and formation
ARO Autosomal recessive osteopetrosis
ATF4 Activating transcription factor 4
ATP Adenosine Triphosphate
BFR Bone formation rate
BM Bone marrow
BMC Bone mineral content
BMD Bone mineral density
BMM Bone marrow macrophages
BMP Bone morphogenetic protein
BMSC Bone mesenchymal stem cell
BMU Basic multicellular unit
BV/TV Bone volume per tissue volume
Ca2+ Calcium
CA-II Carbonic anhydrase-II
Caltrin Calcium transport inhibitor
CaMKIV Calcium/Calmodulin-dependent kinase IV
cAMP Cyclic adenosine monophosphate
CCD Cleidocranial dysplasia
cDNA Complementary deoxyribonucleic acid
C/EBP CCAAT/enhancer binding protein
CFU Colony forming unit
ClCN Chloride channel
CLS Coffin-Lowry syndrome
CREB cAMP response element-binding protein
Csk C-terminus Src family kinase
CT-1 Cardiotrophin-1
CTP Cytidine triphosphate
CTR Calcitonin receptor
DAP12 DNAX-activating protein 12

13
DCSTAMP Dendritic cell-specific transmembrane protein
DHT dihydroxytestosterone
Dkk-1 Dickoff-1
DNA Deoxyribonucleic acid
DTT Dithiothreitol
DEXA Dual energy X-ray absorptiometry
ECM Extracellular matrix
EDTA Ethylene diamine tetracetic acid
ELISA Enzyme-linked immunosorbent assay
EMA European medicines agency
ERK Extracellular signal-regulated kinase
FAK Focal adhesion kinase
FBS Fetal bovine serum
FcRγ Fc receptor common gamma chain
FDA United States Food and drug administration
FGF Fibroblast growth factor
GPCR G-protein coupled receptor
GPI Glycosylphosphatidylinositol
H&E Haematoxylin and eosin
HSC Hematopoietic stem cell
HSCT Hematopoietic stem cell therapy
IBSP Integrin-binding sialoprotein
IGF Insulin-like growth factor
IκB Inhibitor of kappa B
IKK Inhibitor of kappa B kinase
IL-1 Interleukin-1
IP3 Inositol-1, 4, 5-triphosphate
IPTG Isoprophyl-β-D-thiogalactopyranoside
ITAM Immunoreceptor tyrosine-based activation motif
JNK c-Jun N-terminal kinase
KO Knockout
LDL Low density lipoprotein
LEF Lymphoid-enhancer factor
LRP LDL receptor-related protein
Ly-6 Lymphocyte antigen-6

14
M-CSF Macrophage colony stimulating factor
MAPK Mitogen-activated protein kinase
MAR Mineral apposition rate
MicroCT Microcomputed tomography
MITF Microphthalmia-associated transcription factor
MMP Matrix metalloproteinase
MRF Myogenic regulatory factor
mRNA Messenger ribonucleic acid
MSC Mesenchymal stem cell
nAChRs Nicotinic acetylcholine receptors
NADH Nicotinamide adenine dinucleotide
NADPH Nicotinamide adenine dinucleotide phosphate
NBF Neutral Buffered Formalin
NF-κB Nuclear factor kappa b
NFATc1 Nuclear factor-activated T-cell cytoplasmic 1
OB Osteoblast
OC Osteoclast
OCN Osteocalcin
OPG Osteoprotegerin
OPN Osteopontin
OPPG Osteoporosis-pseudoglioma syndrome
OSCAR Osteoclast-associated receptor
OSE Osteocalcin-specific element
Osx Osterix
OVX Ovariectomised
PAGE Polyacrylamide gel electrophoresis
PATE Prostate and testes-expressed protein
PBS Phosphate buffered saline
PCR Polymerase chair reaction
PDB Paget’s disease of bone
PIP2 Phosphatidylinositol-4, 5-bisphosphate
PLC Phospholipase C
PMSF Phenylmethylsulphonyl fluoride
PPAR Peroxisome proliferator-activated receptor
PTH Parathyroid hormone

15
Pyk2 Proline-rich tyrosine kinase 2
RANKL Receptor activator of NF-κB ligand
RGD Arginine-glycine-aspartic acid
RNA Ribonucleic acid
Rpm Revolutions per minute
RT Reverse transcription
S1P Sphingosine 1-phosphate
Sca-1 Stem cell antigen-1
SDS Sodium dodecyl sulphate
SEM Scanning electron microscopy
SEM (Statistics) Standard error mean
sFRP Secreted frizzled receptor protein
SLURP Secreted Ly-6/uPAR-related protein
SOCE Store-operated calcium entry
SOST Sclerostin
Sox Sex determining region Y-box
SPARC Secreted protein acidic and rich in cysteine
SQSTM1 Sequestosome 1
STAT Signal transducer and activator of transcription
SVC Seminal vesicle content
Svs7 Seminal vesicle secretion 7
TAE Tris-acetate EDTA
Tb.Sp Trabecular separation
Tb.Th Trabecular thickness
Tb.N Trabecular number
TBS Tris buffered saline
TCF T-cell factor
TCIRG1 T cell immune regulatory 1
TFP Three-fingered protein
TG Transgenic
TGF Transforming growth factor
TNF Tumour necrosis factor
TRAF Tumour necrosis factor receptor-associated factor
TRAP Tartrate-resistant acid phosphatase
TREM2 Triggering receptor-expressed on myeloid cells 2

16
TRPV4 Transient receptor potential vanilloid 4
uPAR Urokinase-type plasminogen activator receptor
V-H+ATPase Vacuolar- H+ATPase
WB Western blot
WT Wild type
X-gal 5-bromo-4-chloro-3-indolyl-β-D-galactoside

17
CHAPTER 1
BONE BIOLOGY

Chapter One – Bone Biology
18
1. Introduction to Bone Biology Bone is a living tissue whose function is to provide a skeletal frame in mammals and an
important organ for the formation of hematopoietic cells and the maintenance of a
normal level of blood calcium (Dvorak-Ewell et al. 2011; Takayanagi 2007). Bone is
continuously remodelled throughout life by two major resident cells, bone-resorbing
osteoclasts and bone-forming osteoblasts. Bone remodelling is an important metabolic
process regulating bone growth, structure and function during adult life (Boyle, Simonet
& Lacey 2003; Teitelbaum 2000a). A highly regulated cell-to-cell interaction between
osteoclasts and osteoblasts is governed by local and systemic factors, such as growth
factors, cytokines, and hormones (Karsenty & Wagner 2002; Zaidi 2007). A balance in
osteoclast and osteoblast activity is critical to maintain healthy bone mass (bone
homeostasis), otherwise perturbations in skeletal structure and function associated with
skeletal diseases may occur (Zaidi 2007). An uncoupled bone formation by the
osteoblast can result in osteopetrosis (an extreme high bone mass), while an excessive
bone resorption activity by osteoclasts underlies skeletal diseases such as osteoporosis
(an extreme low bone mass) and Paget’s disease of bone (PDB) (He et al. 2011; Raisz
2005b).
Osteoclasts are large terminally differentiated multinucleated cells, capable of resorbing
bones (Teitelbaum 2000a; Vaananen et al. 2000). Osteoclasts originate from
monocytes/macrophages lineage of hematopoietic stem cell, in which multinucleated
osteoclasts are formed by the fusion of mononuclear macrophage precursors
(Teitelbaum 2000a). On the other hand, osteoblasts are the only bone cells with the
ability to form bone (Harada & Rodan 2003). Osteoblasts are derived from multipotent
mesenchymal stem cells, which later express specific bone matrix proteins such as
osteopontin (OPN), osteocalcin (OCN), and type I collagen to be incorporated in newly
formed bones (Aubin et al. 2008; Ducy et al. 1997; Yoshida 2012). Fully differentiated
osteoblasts lay down bone matrix proteins in the osteoclasts resorbed compartment,
which are then mineralized to become calcified bone to complete bone remodelling
process.
The balance in activity between osteoclasts and osteoblasts is essential to the
maintenance of bone homeostasis. Disruption to this balanced system will greatly
contribute to the development of many skeletal diseases including osteoporosis,
osteopetrosis, PDB, and rheumatoid arthritis. Osteoporosis is a common skeletal disease

Chapter One – Bone Biology
19
occurring worldwide, in which there is excessive bone resorption activity by osteoclasts,
causing a decrease in bone mass and strength and microarchitectural deterioration of the
skeleton and hence having a higher risk of bone fragility fractures (Raisz 2005b). Bone
mineral density (BMD) measurement is used to diagnose osteoporosis and osteopenia
before fractures occur (Raisz 2005a). The current and still most acceptable treatment for
osteoporosis is using anti-resorptive agents such as nitrogen-containing
bisphosphonates, which include alendronate, risedronate, ibrandonate, and zoledronic
acid (Epstein 2006; Lewiecki 2011). These agents bind to the bone surface, causing
inactivation and programmed cell death when they are taken up by the osteoclasts.
Although this treatment is the current frontline therapy, it is unable to reverse the
structural damage caused by osteoporosis (Delmas 2002). More recently, clinical trials
have focused on the use of denosumab, a fully human immunoglobulin G2 monoclonal
antibody specific to Receptor Activator of NF-κB ligand (RANKL) (Kostenuik et al.
2009; Rizzoli, Yasothan & Kirkpatrick 2010). This drug is designed to block the
interaction between RANKL, expressed by osteoblasts, and its receptor RANK,
expressed by osteoclasts and their precursors, hence inhibiting osteoclast differentiation
and activation and causing a net increase in bone formation. The European Commission
and US Food and Drug Administration (FDA) have both approved Denosumab for
clinical use and to date, it shows promising results in treating postmenopausal
osteoporosis and bone loss in men associated with hormone ablation and prostate cancer
(EMA ; FDA ; Rizzoli, Yasothan & Kirkpatrick 2010). On the other hand, defects in
osteoclast differentiation (osteoclast-poor) and function (osteoclast-rich) are the
common cause of osteopetrosis, characterized by an abnormal high bone mass and a
defect in bone-marrow formation (Frattini et al. 2000; Guerrini et al. 2008; Sobacchi et
al. 2007; Takayanagi 2007). Together with PDB, these three skeletal diseases become a
huge burden in our society and they will be discussed later in this chapter.
Basic research examining the regulation of ‘cross-talk’ between osteoclasts and
osteoblasts is fundamental to the discovery of novel genes/proteins, which regulate
intercellular communication, and may help to uncover new therapies for the
management and treatment of many pathological bone diseases. Hence, this project will
focus on a novel osteoclast-secreted protein, Svs7, which has shown to have a role in
regulating bone homeostasis.

Chapter One – Bone Biology
20
1.1 Osteoclast
Osteoclasts are multinucleated, giant, bone resorbing cells that are terminally
differentiated and formed by the fusion of mononuclear progenitors of the
monocyte/macrophage lineage of hematopoietic stem cells (Suda et al. 1995;
Takayanagi 2007; Teitelbaum 2000a; Vaananen et al. 2000). Osteoclasts are located on
both endosteal and periosteal surfaces of bone (Li, Kong & Qi 2006). Activated
osteoclasts form resorption pits on bone and dentine slices by acid decalcification and
proteolytic degradation (Boyle, Simonet & Lacey 2003; MacDonald & Gowen 1993;
Suda et al. 1995; Takayanagi 2007) to produce irregular scalloped cavities (Howship
lacunae) on trabecular bone surfaces, or cylindrical Haversian canals in cortical bone
(Raisz 1999).
1.1.1 Osteoclast Phenotype
Osteoclasts exist in two functional states, the motile and the resorptive (active) states.
Motile osteoclasts are flattened, non-polarised cells, having membrane protrusions,
called lamellipodia, at their leading edge and podosome complexes in a row behind the
leading edge to help them to move from bone marrow to their resorptive sites. When
reaching their resorptive sites, osteoclasts become polarized and active by cytoskeletal
reorganization (Li, Kong & Qi 2006).
This cytoskeletal reorganization results in the formation of four important plasma
membrane domains: a ruffled border, sealing zone, functional secretory domain, and
basolateral membrane, as shown in Figure 1.1. The ruffled border, located inside the
sealing zone, presents finger-shaped projections of the osteoclast plasma membrane
juxtaposed to the bone matrix, which contain all acidification resorbing machinery
organelles (Li, Kong & Qi 2006). The sealing zone, which is composed of actin ring
structure, separates the resorptive lacuna from the rest of the cell; hence it is an
osteoclast-specific structure (Lakkakorpi et al. 1999; Li, Kong & Qi 2006). Osteoclastic
bone resorption activity takes place within the sealing zone.

Chapter One – Bone Biology
21
Legend
H+
Sealing Zone
Nucleus
V-H+ATPase
Functional Secretory Domain
Ruffled Border
BONE
Basolateral Domain
Resorptive Pit Cathepsin K
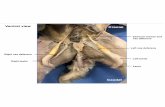
Figure 1.1 The four important domains of polarized, multinucleated osteoclasts.
Activated osteoclasts, by having cytoskeletal reorganization, have four crucial domains
when they attach on to bone surface; ruffled border, sealing zone, basolateral domain,
and functional secretory domain. H+ proton and proteases, such as Cathepsin K, are
secreted by the acidification machinery organelles, V-H+ATPase complex, located in
the ruffled border of the osteoclast to degrade bone matrix.

Chapter One – Bone Biology
22
Because of this sealed resorptive compartment, acidity maintenance, which is an
essential condition for bone degradation to occur, can be achieved. Osteoclasts
endocytose by-products of resorption through their basolateral domain and excrete them
through the functional secretory domain. During its bone resorption activity, osteoclasts
are dome-shaped and do not display lamellipodias.
Osteoclast precursors and mature osteoclasts express the tyrosine kinase receptor c-fms,
which is the receptor for macrophage-colony stimulating factor (M-CSF), and RANK, a
member of TNF receptor family, which is the receptor for RANKL (Suda et al. 1999;
Takayanagi 2007; Yasuda et al. 1998). Osteoclasts express tartrate-resistant acid
phosphatase (TRAP) (Hayman et al. 1996; Suda et al. 1997), which is widely used as a
specific histochemical marker of osteoclasts. Mice lacking TRAP activity exhibit a mild
osteopetrosis condition due to an intrinsic defect in osteoclast activity (Hayman et al.
1996). Osteoclasts also highly express the specific lysosomal cysteine protease,
Cathepsin K, which is the major bone matrix-degrading enzyme at low pH environment
(Drake et al. 1996; Gelb et al. 1996; Raisz 1999; Takayanagi 2007; Wilson et al. 2009).
Cathepsin K is responsible for the degradation of type I collagen during osteoclast bone
resorption activity. Hence because of its importance during osteoclast activity,
Cathepsin K-deficient mice show severe osteopetrosis, while in human, mutation in
Cathepsin K gene has been shown to result in pycnodysostosis, a condition
characterized by osteosclerosis and short stature (Gelb et al. 1996; Rachner, Khosla &
Hofbauer 2011; Saftig et al. 2000). Another specific osteoclast marker is matrix
metalloproteinase (MMP), MMP-9 (Nyman et al. 2011; Teti 2012). It belongs to the
gelatinase subfamily of the MMP and hence its substrate is gelatin or denatured
collagen (Ram, Sherer & Shoenfeld 2006). Together with cathepsin K, MMP-9
degrades the organic matrix of bone. Earlier, Haibo, Z et al., 1997 found that the
expression of MMP-9 gene was higher in osteoporotic bone tissues compared to normal
ones, indicating that MMP-9 plays a crucial role in the development of osteoporosis. In
many autoimmune diseases, such as multiple sclerosis and rheumatoid arthritis, the
level of MMP-9 expression is also found to be higher than normal controls (Gruber et
al. 1996; Leppert et al. 1998).
The above mentioned proteolytic enzymes are secreted at the ruffled border of activated
osteoclasts (Figure 1.1), which contains the osteoclast primary acidification machinery,
the vacuolar H+-adenosine triphosphatase (V-H+ATPase) complex (Vaananen et al.

Chapter One – Bone Biology
23
2000). This V-H+ATPase pump facilitates the secretion of hydrochloric acid (HCl)/H+
protons into resorption lacunae to create an acidic environment necessary for osteoclasts
to demineralize the hydroxyapatite of bone (Baron et al. 1985; Blair et al. 1989;
Kawasaki-Nishi, Nishi & Forgac 2003; Li, Kong & Qi 2006), followed by the secretion
of the proteolytic enzymes to degrade the organic bone matrix (Vaananen et al. 2000).
Hence, an enhanced bone resorption activity by osteoclasts parallels with a marked
expansion in ruffled border surface.
Osteoclast mononuclear precursors are able to fuse to become multinucleated cells
through an as yet unknown mechanism, which involves the fusogenic genes, Dendritic
cell-specific transmembrane protein (DCSTAMP) (Yagi 2005) and d2 subunit of V-
H+ATPase complex (ATP6v0d2) (Lee et al. 2006). The expression of both of these
fusogenic genes are upregulated during RANKL-induced osteoclastogenesis and are
transcriptionally regulated by Nuclear Factor-Activated T-cell cytoplasmic 1 (NFATc1)
transcription factor, the master regulator of osteoclast differentiation (Feng et al. 2008;
Kim et al. 2008). Osteoclast differentiation and fusion are completely disrupted in both
DCSTAMP and ATP6v0d2-deficient mice despite normal gene expression of other
osteoclast markers, resulting in an osteopetrotic condition (Lee et al. 2006; Yagi et al.
2005).
Another important marker of a mature osteoclast is the high expression of calcitonin
receptor (CTR). Calcitonin has been shown to inhibit osteoclast bone resorption activity
(Wallach et al. 1999; Li, Kong & Qi 2006) through its binding to CTR. Davey, R. A et
al. 2008 has shown that global CTR KO mice had a mild increase in bone formation and
had a normal serum calcium level, as well as unaffected osteoclast surface and activity
indicating a modest role of CTR in the regulation of basal state of bone turnover and
calcium homeostasis (Davey et al. 2008).
1.1.2 Osteoclast differentiation and function
Osteoclasts are differentiated from the monocyte/macrophage lineage of the
hematopoietic stem cells (Suda et al. 1995; Teitelbaum 2000a). Osteoclast
differentiation is induced by cell-to-cell contact between osteoclast precursors and
osteoblasts (Kong et al. 1999; Nakashima & Takayanagi 2011; Suda, Takahashi &
Martin 1992; Takayanagi 2007; Udagawa et al. 1990). M-CSF, secreted by osteoblasts,

Chapter One – Bone Biology
24
through binding to its receptor c-fms (Stanley et al. 1997) as shown in Figure 1.2,
promotes proliferation, differentiation, and survival of osteoclast progenitors, as shown
in Figure 1.3 (Suda et al. 1995; Takayanagi 2007), through the activation of
extracellular-signal-regulated-kinase (ERK) 1/2 (p42/44) and phosphoinositide 3-kinase
(PI3K)/AKT signalling pathways (Glantschnig et al. 2003; Oikawa & Yamada 2003;
Ross & Teitelbaum 2005; Sugatani 2005; Tanaka et al. 2003). Downstream signalling
pathway of ERK results in the activation of PU.1, a family member of E-twenty six
(ETS)-domain transcription factors, which then regulates the initial developmental
stages of macrophages and osteoclasts by controlling the expression of c-fms
(Takayanagi 2007; Tondravi et al. 1997). PU.1-deficient mice exhibit osteopetrosis
(Tondravi et al. 1997). Mice having non-functional M-CSF (M-CSF deficiency) have an
osteopetrotic condition and the administration of recombinant human M-CSF to these
mice has been shown to rescue the phenotype (Felix, Cecchini & Fleisch 1990; Yoshida
et al. 1990).
The osteoclast differentiation process is driven primarily by the binding of RANKL,
expressed as a membrane-bound cytokine on osteoblasts, to RANK on the osteoclast
surface (Figure 1.2), which leads to the activation (fusion, polarization and cytoskeletal
rearrangement, as described above in Section 1.1.1) of mature osteoclasts on the bone
surface (Burgess et al. 1999; Kong et al. 1999; Nakashima et al. 2011; Nakashima &
Takayanagi 2011). RANKL activates mature osteoclasts in a dose-dependent manner in
vitro and can also induce rapidly pre-existing osteoclasts to resorb bone in vivo (Boyle,
Simonet & Lacey 2003; Burgess et al. 1999; Fuller et al. 2002).
A number of osteoclast transcriptional factors have been shown to be involved in the
regulation of RANKL-induced osteoclastogenesis, in which one of them is a Nuclear
Factor of Activated T cell cytoplasmic 1 (NFATc1) (Takayanagi et al. 2002). The
NFAT transcription factor family was originally discovered in T cells and has been
shown to be involved in many biological systems (Crabtree & Olson 2002; Hogan et al.
2003).

Chapter One – Bone Biology
25
Legend
M-CSF
c-Fms
RANKL
RANK OPG
OSTEOCLAST OSTEOBLAST
OSTEOCLAST DIFFERENTIATION
Precursor cells Fusion Mechanism Osteoclast
Figure 1.2 Cell-to-cell contact between osteoclast and osteoblast. Osteoblasts
express RANKL (membrane-bound cytokine) and secrete M-CSF to induce
osteoclastogenesis. Osteoprotegerin (OPG), decoy receptor for RANKL, is also secreted
by osteoblasts to inhibit osteoclastogenesis and hence it is one of the negative regulators
of osteoclastogenesis.

Chapter One – Bone Biology
26
Plasma Membrane
Cytosol ITAM DAP12 /
FcRγ
TREM2 / OSCAR RANKL
RANK
ITAM Co-Stimulatory Pathway RANKL Pathway
M-CSF
c-Fms
TRAF6
Proliferation Cytoskeletal Reorganization Survival NFκB
c-Fos
AP-1
P
PLCγ
Ca2+
CaMKIV
Creb
NFATc1
Auto-amplification
Calcineurin
PU.1 AP-1 NFATc1 Creb MITF
Osteoclastic Genes DC-STAMP, Atp6v0d2, OSCAR, β3integrin, TRAP, Calcitonin receptor, Cathepsin K etc.
Blimp1
Anti-Osteoclastic Genes IRF-8, MafB, Bcl6 etc.
Transcription
IκB IκB P
Ubiquitination and degradation
Nucleus
Figure 1.3 Signalling pathways in osteoclast differentiation. The binding of M-CSF
to its receptor c-fms promotes proliferation, survival, and cytoskeletal organization of
osteoclast precursors and mature osteoclasts. The RANKL-RANK interaction activates
TRAF6, which leads to phosphorylation (degradation) of IκBα and activation of NFκB
through AP1 transcription factor. The co-activation of TREM2/OSCAR, which contains
DAP12/FcRγ domain, by calcium influx into the cell during RANKL signalling causes
the activation of Ca2+ signalling pathway. This pathway signals to PLCγ, which then
results in phosphorylation of calcineurin by calcium-dependent calmodulin kinase IV
(CaMKIV) and subsequent dephosphorylation (activation) of the master regulator of
osteoclastogenesis, NFATc1 by calcineurin. NFATc1 autoamplifies its gene to get a
robust induction, regulating the expression of many osteoclast genes such as
DCSTAMP, ATP6v0d2, Cathepsin K, and OSCAR. NFATc1 has also been shown to
regulate the expression of Blimp1 gene, which in turn regulates the expression of anti-
osteoclastogenic factors, such as MafB and Bcl6. (Figure adapted from Nakashima &
Takayanagi 2011; Kular et al. 2012)

Chapter One – Bone Biology
27
RANKL stimulation results in the induction of Ca2+ oscillation through the activation of
co-stimulatory signal of the immunoglobulin-like receptors, such as osteoclast
associated receptor (OSCAR) and triggering receptor-expressed on myeloid cells
(TREM) 2, and the subsequent association of immunoreceptor tyrosine-based activation
motif (ITAM)-containing molecules (DNAX-activating protein (DAP) 12 and Fc
receptor common gamma chain (FcRγ), as shown in Figure 1.3 (Koga et al. 2004; Kular
et al. 2012; Nakashima & Takayanagi 2011). This signalling pathway then leads to the
activation of NFATc1 via a calcium-calmodulin-calcineurin-dependent pathway
(Takayanagi et al. 2002). The NFATc1 promoter contains NFAT binding sites and
NFATc1 specifically auto-regulates (auto-amplifies) its own promoter during
osteoclastogenesis generating a robust induction (Figure 1.3). Activator protein 1
(AP1)-containing c-Fos and the continuous calcium signalling are essential for this
auto-amplification (Matsuo et al. 2004; Takayanagi et al. 2002; Takayanagi 2007).
Common cytokines, such as tumour necrosis factor (TNF), have been shown to induce
Ca2+ oscillations in human macrophages, which subsequently leads to the induction and
activation of NFATc1 transcription factor (Yarilina et al. 2011). NFATc1-deficient
embryonic cells fail to differentiate into mature osteoclasts under RANKL stimulation
and with overexpression of NFATc1, osteoclast precursors are able to differentiate into
active osteoclasts without the need for RANKL stimulation (Takayanagi et al. 2002).
NFATc1 has also been shown to directly regulate the gene expression of fusion-
mediating molecules, which are DCSTAMP and ATP6v0d2, as well as Cathepsin K,
TRAP, CTR, and OSCAR in cooperation with other transcription factors such as AP1,
PU.1, and microphthalmia-associated transcription factor (MITF), as shown in Figure
1.3 (Crotti et al. 2006; Kim et al. 2005; Kim et al. 2008; Lee et al. 2006; Matsumoto et
al. 2004; Nakashima & Takayanagi 2011; Takayanagi et al. 2002; Takayanagi 2007;
Yagi et al. 2005). NFATc1 regulation of these osteoclast genes has also been shown to
require the cooperation between cAMP response element-binding protein (CREB),
which is activated by Ca2+/Calmodulin-dependent kinases IV (CaMKIV), with NFATc1
(Figure 1.3) (Sato et al. 2006; Takayanagi 2007).
NF-κB is another essential transcription factor signalling pathway in osteoclastogeneis.
There are 5 NF-κB subunits, which are cRel (Rel), RelA (p65), RelB, NF-κB1 (p50),
and NF-κB2 (p52) (Karin, Yamamoto & Wang 2004; Takayanagi 2007; Xu et al. 2009).
Upon RANKL binding to its receptor RANK, the trimerization of RANK and TNF
receptor-associated factor (TRAF) 6 begins, which leads to the activation of the NF-κB

Chapter One – Bone Biology
28
signalling pathway (Figure 1.3) (Kobayashi et al. 2001). Its classical activation involves
the inhibitor κB (IκB) kinase (IKK) phosphorylation, followed by phosphorylation-
induced proteasomal degradation of IκB and subsequent NF-κB (RelA-p50 dimers)
translocation and activation in the nucleus to regulate a vast number of target genes
(Karin, Yamamoto & Wang 2004; Xu et al. 2009). On the other hand, the alternative
pathway depends on the homodimerization of IKK-α, followed by phosphorylation and
the proteasomal processing of p100 to p52, and the nuclear translocation of RelB-p52
dimers (Franzoso et al. 1997; Karin, Yamamoto & Wang 2004; Xu et al. 2009). Double
knockout (KO) mice for NF-κB subunit p50 and p52 exhibit severe osteopetrosis due to
the defect in osteoclastogenesis (Iotsova et al. 1997).
The AP-1 transcription factor complex is also essential for osteoclastogenesis (Wagner
& Eferl 2005). The family consists of Fos-related (FosB, Fra-1, Fra-2) and Jun-related
(c-Jun, JunB, JunD) genes (Grigoriadis et al. 1994). RANK-RANKL binding induces
AP-1 activation through the induction of its component, c-Fos, which is activated by
CaMKIV/CREB signalling pathway, as shown in Figure 1.3 (Sato et al. 2006;
Nakashima & Takayanagi 2011). Mice with c-Fos deficiency develop osteopetrosis due
to a defect in hematopoietic stem/precursor cells differentiation into osteoclasts
(Grigoriadis et al. 1994). A mutation in c-Jun gene has been shown to inhibit NFATc1-
induced osteoclastogenesis in vitro (Ikeda et al. 2004).
The proto-oncogene c-src, highly expressed by osteoclasts and concentrated on the
ruffled border membranes (Tanaka et al. 1992), is a non-receptor tyrosine kinase, which
regulates osteoclast polarization and activation. C-src-deficient mice show defects in
integrin-mediated intracellular signalling and ruffled border formation and hence
develop osteopetrosis (Boyce et al. 1992; Nakamura et al. 1998; Nakamura et al. 2001).
The c-src tyrosine kinase activity is regulated by phosphorylation and
dephosphorylation of the tyrosine residue located close to the C-terminus region
(Tanaka et al. 2003). Dephosphorylation of c-src induces its activation and C-terminus
Src family kinase (Csk) has been shown to be the negative regulator of c-src kinase
activity by inducing its phosphorylation state (Okada et al. 1991). Downstream
signalling pathway of c-src begins with the activation of αvβ3 integrin, which induces
Pyk2 (another non-receptor tyrosine kinase of the focal adhesion kinase (FAK) family)
tyrosine phosphorylation and subsequent its association with c-src via its SH2 domain
(Duong et al. 1998; Nakamura et al. 2012). This complex is then completed with the

Chapter One – Bone Biology
29
binding of p130Cas (Cas, Crk- associated substrate) to Pyk2 via its SH3 domain to
regulate the formation of actin rings (sealing zones), an essential step in osteoclast
activation (Lakkakorpi et al. 1999). Both Pyk2 and p130Cas are localised to the sealing
zones in resorbing osteoclasts and c-src-deficient mice have been shown to have a
decrease in activity of both molecules and subsequent defective ruffled border
formation (resulting in an osteopetrotic phenotype), indicating that both molecules are
downstream modulators of c-src (Boyce et al. 1992; Duong et al. 1998; Lakkakorpi et
al. 1999; Soriano et al. 1991).
Upon attachment to the bone surface, a multinucleated osteoclast polarizes to form 4
important domains; the sealing zone, basolateral domain, functional secretory domain,
and the ruffled border, as described before in Section 1.1.1. This process results in the
creation of an isolated extracellular microenvironment, which will then be acidified to
create a low pH environment. This acidification process is mediated by the secretion of
HCL/H+ protons into the resorptive microenvironment by the V-ATPases complex,
resulting in a pH of ~4.5 (Baron 1985; Teitelbaum 2000b). This first process degrades
the hydroxyapatite of bone, which is then followed by the osteoclast secretion of
Cathepsin K and MMPs to resorb the organic bone matrix (comprises primarily of type
I collagen) (Delaissé et al. 2003; Drake et al. 1996). Bone resorption by-products are
endocytosed through the basolateral domain, transported and excreted to the external
environment through the functional secretory domain of osteoclasts (Vaananen et al.
2000). Following the completion of bone resorption, osteoclasts undergo apoptosis.

Chapter One – Bone Biology
30
1.2 Osteoblast
After osteoclasts undergo apoptosis, bone remodelling process continues with the
reversal phase, at which bone resorption activity stops, followed by new bone formation
activity by osteoblasts to lay down new mineralized bone matrix at the resorption
lacunae. Hence, this bone remodelling process is tightly regulated to ensure that there is
an equal amount of bone resorbed and formed (bone homeostasis). Many other cells,
apart from osteoclast and osteoblast, have shown to be involved in bone remodelling
process, such as osteocytes, which are located within the bone matrix, and bone lining
cells, as shown in Figure 1.4 (MacDonald & Gowen 1993; N. A. Sims & J. H. Gooi
2008; Xiong et al. 2011). Together, these cells are commonly known as the basic
multicellular unit (BMU) of bone. This section will focus on the bone forming
osteoblast.
1.2.1 Osteoblast Phenotype
Osteoblasts are cuboidal mononuclear cells (Figure 1.2 and 1.4), which form and
deposit bone matrix (Long 2012). Osteoblasts are usually found in a single layer
adherent to periosteal or endosteal surfaces of bone (sites of active bone formation)
(Baker et al. 1992; MacDonald & Gowen 1993). As discussed before and shown in
Figure 1.2, osteoblasts express RANKL as its membrane-bound osteoclast
differentiation factor (Kong et al. 1999; Yasuda et al. 1998). Osteoblasts are stained
positive for alkaline phosphatase (ALP) and express a number of bone matrix proteins,
such as type I collagen (the major component of the organic bone matrix providing
strength and elasticity to the bone (Mundlos & Olsen 1997)), as well as osteonectin
(SPARC), OCN, OPN, and bone sialoprotein (IBSP) (Aubin & Triffitt 2002; Koga et al.
2005; Termine et al. 1984; Yoshida et al. 2012). These latter non-collagenous proteins
and ALP expression by osteoblasts are essential in the regulation of mineral deposition
and turnover and bone-cell activity (Clarke 2008; Kular et al. 2012). ALP knock out
mice have impaired growth and die before weaning as a consequence of defective bone
mineral deposition and abnormal morphology of osteoblasts (Narisawa, Fröhlander &
Millán 1997). Osteoblasts also express parathyroid hormone (PTH) receptor (PTH1R)
at which PTH exerts its role in regulating bone mass (Goltzman 2008). PTH1R is a
seven trans-membrane spanning receptor, which belongs to the B subfamily of G-
protein-coupled receptors (GPCRs) (Juppner et al. 1991). Mice having mutated PTH1R

Chapter One – Bone Biology
31
Bone lining cells Osteoclast
Osteoblast
Resorption Reversal Formation Mineralization
Osteoid
BONE Osteocyte
Figure 1.4 Osteoclast bone resorption activation, reversal, and new bone matrix
formation and mineralization by the osteoblast, known as ARF cycle, in bone
remodelling process. After a regulated bone resorption activity by osteoclasts, there is
then a reversal phase, where there are presumably osteoblast precursors and other cells
modifying the resorbed surface to attract osteoblasts. Then osteoblasts start to secrete
bone matrix protein (unmineralized bone matrix or osteoid), which is then mineralized.

Chapter One – Bone Biology
32
gene result in perinatal death with an abnormal skeleton (Soegiarto et al. 2001). PTH
has both anabolic and catabolic effects on bone, which will be discussed further in
osteoblast differentiation and function section.
1.2.2 Osteoblast differentiation and function
Osteoblasts, together with chondrocytes, adipocytes, and myoblasts, are derived from
undifferentiated mesenchymal stem cells (MSCs) (Dennis et al. 1999; Pittenger et al.
1999). This cellular differentiation is highly regulated by specific transcription factors
and growth factors, governing the MSCs to differentiate into each different lineage. Sex
determining region Y-box (Sox) 5, 6, and 9 are essential transcription factors regulating
the MSCs differentiation into chondrocytes (Akiyama et al. 2002; Harada & Rodan
2003), while the induction of CCAAT/enhancer binding proteins (C/EBP) α and the
nuclear hormone receptor peroxisome proliferator-activated receptor γ (PPAR)γ results
in the MSCs differentiation into adipocytes (Rosen et al. 2002). Myogenic regulatory
factors (MRFs), namely MyoD, Myf5, myogenin, and MRF4/Myf6, are required for
myogenic differentiation, as shown in Figure 1.5 (Parker et al. 2012).
The importance of the runt-related transcription factor 2 (Runx2) in osteoblasts
differentiation, as shown in Figure 1.5, has been shown by knockout mice having a
complete absence of osteoblasts/ossification (cartilaginous skeleton) and die shortly
after birth without breathing (Ducy et al. 1997; Komori et al. 1997; Otto et al. 1997).
The complete failure of osteoblast differentiation, shown by the absence of alkaline
phosphatase activity, is accompanied by failure of the bone marrow vascularization in
these mice. Heterozygous mice have a defect in intramembranous ossification,
corresponding to the human condition known as cleidocranial dysplasia (CCD – defect
in the closure of the cranial fontanelles) (Mundlos et al. 1997; Otto et al. 1997). Runx2
regulates osteoblast-specific bone matrix genes expression such as type I collagen,
OPN, OCN, and IBSP, hence it is required for osteoblast differentiation and activity
(Ducy et al. 1999). Runx2 has also been shown to be important for chondrocytes
maturation as there is delayed chondrocytes maturation in Runx2-deficient mice, and
the overexpression of Runx2 causes ectopic hypertrophic chondrocytes differentiation
and endochondral ossification (Inada et al. 1999; Ueta et al. 2001; Takeda et al. 2001).
These findings indicate that Runx2 regulates the differentiation of both hypertrophic
chondrocytes and osteoblasts

Chapter One – Bone Biology
33
MESENCHYMAL
STEM CELL
MYOCYTE
CHONDROCYTE
ADIPOCYTE
OSTEOBLAST PRECURSOR
MATURE OSTEOBLAST
Sox9 MRFs (MyoD)
C/EBPα PPARγ
OSTEOCYTE
BMP Osterix Runx2
BMP Osterix Runx2 PTH
BMP PTH
Apoptosis
LINING CELL
Figure 1.5 Osteoblast differentiation from mesenchymal stem cells (MSCs). With
specific transcription factors, mesenchymal stem cells can differentiate into myocytes,
chondrocytes, adipocytes, and osteoblasts. Specific transcription factors, Runx2 and
Osterix together with growth factors (BMP) and hormones (PTH) drive this MSCs
differentiation into osteoblast lineage. After new bone formation activity finishes,
osteoblasts can have one of three fates; they undergo apoptosis, become embedded in
the bone matrix as osteocytes, or become bone-lining cells. (Figure modified from Raisz
1999).

Chapter One – Bone Biology
34
(Inada et al. 1999; Ueta et al. 2001). Interestingly, it has been revealed that co-culture
system of ST2 bone marrow-derived mesenchymal pluripotent cell line (expressing
Runx2) with murine splenocytes results in the induction of osteoclast genes expression
and the formation of multinucleated osteoclasts (Baniwal 2012). This result has
successfully correlated with the previous study by Geoffroy et al. 2002, who showed
that overexpression of Runx2 in osteoblasts, under type I collagen promoter, could
cause an impairment in osteoblast maturation and an increase in osteoclastic bone
resorption, resulting in an osteopenic phenotype. Hence, together these studies support
the notion that temporal control of Runx2 expression is necessary for healthy bone
development.
The dual role of Runx2 has suggested that there must be another crucial transcription
factor that specifically drives MSCs differentiation into osteogenesis pathways, which is
now known as osterix (Osx) (Figure 1.5). Osx is a novel zinc finger–containing protein
that was originally identified in C2C12 skeletal muscle stimulated with BMP (a potent
stimulator of bone formation) (Harada & Rodan 2003; Nakashima et al. 2002). Osx-
homozygous null mice have a normal cartilaginous skeleton but lack osteoblast activity,
hence no mineralized bone matrix, and die shortly after birth (Nakashima 2002). In
these mice, chondrocytes are fully differentiated, hinting the specific role of Osx in
osteoblast differentiation (Nakashima et al. 2002). Runx2 expression is normal in these
mice, while Osx is absent in Runx2-deficient mice, indicating that Osx works
downstream of Runx2 signalling pathways to specifically induce osteoblast
differentiation. In this Runx2 downstream signalling pathway, further study on the
inhibition of bone formation activity in NFATc1-deficient osteoblasts has shown that
Osx forms a complex with NFATc1 transcription factor and this interaction regulates
Osx-dependent transcriptional activation of type I collagen in osteoblasts (Koga et al.
2005). Later, Baek, W. Y et al. (2009) showed an osteopenic phenotype with an
increase of trabecular bone but a decrease in cortical bone in Osx conditional KO mice
under the control of a 2.3-kb type I collagen promoter. In these mice, both bone
formation rate (BFR) and mineral apposition rate (MAR) were significantly reduced as
well as the expression of OCN bone matrix protein, indicating that Osx plays an
essential role in regulating osteoblast differentiation and bone formation during early
bone development (Baek et al. 2009). Recently, however it has been revealed that the
overexpression of Osx in primary osteoblasts inhibits the late stage of osteoblast
differentiation as shown by reduced expression of alkaline phosphatase and bone matrix

Chapter One – Bone Biology
35
proteins (type I collagen and OCN) and a decrease in mineralization, hence causing
osteopenic phenotype (Yoshida et al. 2012). Together these findings suggest that Osx is
essential for osteoblast differentiation at an early stage (in embryo and postnatal bone
development), but its level of expression at the late stage of osteoblast differentiation
requires a tight regulation for a healthy bone formation and maintenance.
From the study of Coffin-Lowry Syndrome (CLS) (X-linked mental retardation
associated with skeletal abnormalities) by Yang et al. 2004, it is then established that
activating transcription factor 4 (ATF4) is important in the maturation process of
osteoblast cell. ATF4 is critical substrate of RSK2, a gene mutated in CLS. ATF4 has
been shown to directly regulate the expression of osteocalcin in osteoblasts by binding
directly to osteocalcin-specific element (OSE) 1 of the osteocalcin gene promoter
region, hence ATF4 KO mice display delayed bone formation during embryonic
development and low bone mass during postnatal life (Long 2012; Yang et al. 2004).
Furthermore, as Runx2 has shown to bind to OSE2 (Ducy et al. 1997), further study has
illustrated that in the presence of C/EBP, ATF4 could form a complex and synergize
with Runx2 to induce osteocalcin expression (Tominaga et al. 2008).
Cytokines, growth factors, and hormones are also important regulators in osteoblast
differentiation and bone formation. Transforming growth factor (TGF)-β has been
shown to be one of the important regulators for osteoblast differentiation (Janssens et al.
2005; Zuo et al. 2012). This family has three isoforms; TGF-β1, 2, and 3, in which
TGF-β1 is the most abundant isoform in skeletal tissue and has its main role in postnatal
skeletal development and remodelling (Geiser et al. 1998; Janssens et al. 2005; Zuo et
al. 2012). Compared to wild-type (WT) mice, TGF-β1-null mice had significantly
decreased bone mineral content (BMC) and shorter tibia (Geiser et al. 1998). A research
on the role of TGF-β1 in osteoblast regulation shows that TGF-β1 induces early
osteoblast proliferation and bone matrix formation (Hock, Canalis & Centrella 1990).
Furthermore, a recent study has illustrated that TGF-β signal in promoting
osteoprogenitor proliferation, differentiation and to drive the commitment of MSCs to
the osteoblast lineage is through the activation of mitogen-activated protein kinases
(MAPKs), which are ERK1/2, c-Jun N-terminal kinase (JNK), and p38, and Smad2/3
signalling (Matsunobu et al. 2009). BMPs, which belong to TGF-β superfamily, have
also major roles in the skeletal development. BMPs signalling is initiated through
specific type I and II serine/threonine kinase receptors with a specific role in osteoblast

Chapter One – Bone Biology
36
differentiation, shown by type IB BMPR (Zhao et al. 2002). Mice overexpressing
truncated dominant-negative BMPR-IB targeted to osteoblasts have been shown to have
severely reduced bone mineral density, bone volume, and bone formation rates as there
were impairment of postnatal bone formation and inhibition of BMP2-induced
osteoblast differentiation (Zhao et al. 2002). Loss of both BMP-2 and -4 in developing
limbs has been shown to result in a severe impairment of osteogenesis (Bandyopadhyay
et al. 2006). Following the binding of BMPs to its receptor, Smad proteins (1, 5 and 8)
are phosphorylated and together with Smad4 then translocate to nucleus to interact with
Runx2 transcription factor to induce osteoblast differentiation (Chen, Zhao & Mundy
2004; Zuo et al. 2012). A recent study has shown that TGF-β1 acts synergistically to
enhance bone formation induced by BMP-2 (Tachi et al. 2011).
PTH has been well-known as a factor that can induce bone remodelling (N. A. Sims &
J. H. Gooi 2008). PTH binds and exerts its signalling through PTH1R, expressed by
osteoblasts (Goltzman 2008). Intermittent PTH treatment in rats has been shown to
increase osteoblast differentiation (increased cellular ALP activity) and hence resulted
in an increase in bone mineral density (Nishida et al. 1994). Kramer, I et al. 2010 have
shown that this PTH bone anabolism action is achieved by the suppression of bone
formation inhibitor, Sclerostin (SOST), which is secreted by osteocytes and embedded
deep in bone matrix. Interestingly, PTH (Keller & Kneissel 2005) and mechanical
stimulation (Robling, Bellido & Turner 2006) have been shown to regulate the
expression of sclerostin. Hence, both environmental and metabolic activities influence
the expression of sclerostin by osteocytes to regulate the anabolic effect of PTH
(Kramer et al. 2010). Interesting studies by Qiu et al. 2010 have shown that TGF-β type
II receptor (TβRII) directly phosphorylates PTH1R to facilitate the endocytosis process
of the TβRII-PTH1R complex, which ultimately leads to the downregulation of PTH
signal. This study indicates that there is an intimate cross talk between growth factors,
hormones, and/cytokines to regulate osteoblast differentiation and activation.
Osteoblast bone formation activity comes into two different processes, endochondral
and intramembranous ossification (Olsen, Reginato & Wang 2000). Endochondral
ossification involves the process of removal of terminally differentiated (hypertrophic)
chondrocytes, the resorption of cartilage matrix, the invasion by both vascular and
hematopoietic cells, and the synthesis of osteoid by migrating osteoblasts. This
ossification process is important for the formation of long bones, such as limbs and ribs

Chapter One – Bone Biology
37
(Long 2012; Olsen, Reginato & Wang 2000). On the other hand, intramembranous
ossification describes direct synthesis of bone matrix proteins by osteoblasts. Flat
bones, such as the skull and clavicle bones, are formed by the intramembranous
ossification process (Olsen, Reginato & Wang 2000). The canonical signalling pathway
governing this osteoblast bone formation activity is Wnt/β-catenin signalling pathway
(Kular et al. 2012; Zuo et al. 2012), as shown in Figure 1.6, in which TGF-β, BMP, and
PTH share the same pathway (Lin & Hankenson 2011). Wnt signalling begins with the
ligands binding to a receptor complex, composing low density lipoprotein (LDL)
receptor-related protein (LRP) 5/6 and frizzled receptor. This Wnt ligand binding causes
the activation of Dishevelled, which in turn block phosphorylation-induced
ubiquitination of β-catenin by glycogen synthase kinase (GSK)-3β. β-catenin is then
able to translocate into the nucleus to activate lymphoid enhancer factor (LEF)/T-cell
factor (TCF)-mediated osteoblast genes transcription (Kubota, Michigami & Ozono
2009; Kular et al. 2012). Various secreted inhibitors for Wnt/β-catenin are known,
which include Sclerostin (Li et al. 2005) and Dickoff-1 (Dkk-1) binding to LRP5/6
(Bafico et al. 2001) and secreted frizzled receptor protein (sFRP)-1 binding to Wnt
ligands, as shown in Figure 1.6 (Bodine et al. 2004; Kubota, Michigami & Ozono 2009;
Kular et al. 2012). The importance of Wnt/β-catenin signalling pathway in osteoblast
activity has been shown by a study of loss-of-function mutation in the LRP5 that results
in the development of a rare autosomal recessive osteoporosis-pseudoglioma syndrome
(OPPG) (Gong et al. 2001). The patients of this disease are blind and have early onset
of osteoporosis. Conversely, gain-of-function mutation of LRP5 associates with
autosomal dominant high bone mass (Boyden et al. 2002; Little et al. 2002; Van
Wesenbeeck et al. 2003). Besides forming a new bone matrix, osteoblast also functions
to regulate osteoclast differentiation and activation, through its osteoclastogenic
cytokine expression of RANKL, M-CSF, and OPG, which has been discussed
previously in Section 1.1.2.
1.3 Molecular Communication Between Osteoclasts and Osteoblasts
Intercellular communication between osteoclasts and osteoblasts is critically regulated
to achieve a healthy bone mass (bone homeostasis), as pertubations in this system will
result in the development of many pathological bone diseases (Zaidi 2007), as discussed

Chapter One – Bone Biology
38
Plasma Membrane
Cytosol LRP5/6
Wnt
Frizzled
Disheveled
Nucleus
GSK-3
Axin APC
β-catenin
TCF/LEF
β-catenin Target genes
DKK
SOST
Wnt sFRP
Disheveled
GSK-3
Axin APC
β-catenin
P
Proteosomal degradation
Figure 1.6 The Wnt/ββ-catenin signalling pathway in osteoblast. The binding of Wnt
to a receptor complex, LRP5/6 and Frizzled, causes the activation of Dishelved, which
in turn inhibits the phosphorylation-induced ubiquitination of β-catenin by GSK-3
activity. β-catenin is then free to translocate into the nucleus, where it activates
lymphoid enhancer factor (LEF)/T-cell factor (TCF)-mediated osteoblast genes
transcription. Dkk-1 and Sclerostin (SOST) have been shown to inhibit this signalling
by binding to LRP5/6, while sFRP-1 binds to Wnt, hence blocking its binding to
Frizzled receptor. (Figure adapted from Kular et al. 2012)

Chapter One – Bone Biology
39
later in this chapter. The communication can occur through a direct cell-to-cell contact
between osteoclasts and osteoblasts with RANKL-RANK signalling as the classical
pathway of osteoblast regulation of the osteoclast (discussed in more details in Section
1.3.1), secondly through diffusible paracrine factors, such as cytokines, chemokines,
growth factors, and proteins secreted by either cell acting on the other, and lastly
through factors that are deposited during osteoblast bone formation activity and
liberated during osteoclast bone resorption with latent and active form of TGF-β being
the classical example for this (Matsuo & Irie 2008).
1.3.1 Osteoblast regulation of the osteoclast
Osteoblasts secrete M-CSF and express RANKL, which are two critical factors driving
osteoclast differentiation and activation. M-CSF promotes osteoclast precursors
(monocytes/macrophages) and mature osteoclasts proliferation, survival, differentiation,
and cytoskeletal organization leading for activation (Glantschnig et al. 2003; Kodama et
al. 1991; Lagasse & Weissman 1997; Nakamura et al. 2001; Oikawa & Yamada 2003;
Ross & Teitelbaum 2005; Suda et al. 1995; Sugatani & Hruska 2005; Takahashi,
Udagawa & Suda 1999; Takayanagi 2007; Tanaka et al. 2003; Yoshida et al. 1990; Zou
et al. 2007). M-CSF signalling has been described previously in Section 1.1.2. Injection
of rhM-CSF two or three times a day for 14 days into osteopetrosis (Op/Op) mice has
been shown to result in an increase in the number of monocytes in the peripheral blood
and hence an increase in osteoclast number seen in the bone trabeculae in metaphyseal
and diaphyseal regions compared to the uninjected mice control (Kodama et al. 1991).
This M-CSF alone however is not sufficient to induce osteoclast differentiation from its
precursors. A physical contact between osteoblast/stromal cells and
monocyte/macrophages is required to drive this osteoclast differentiation (Suda,
Takahashi & Martin 1992). This is achieved by the interaction of RANKL, expressed as
a membrane-bound form on osteoblasts, and its receptor RANK, expressed on
osteoclast precursor cells (Takahashi, Udagawa & Suda 1999; Theill, Boyle &
Penninger 2002). RANKL KO mice have severe osteopetrosis and defective tooth
eruption as osteoclastogenesis is stopped at the pre-osteoclast stage (TRAP-negative
osteoclast precursors) (Kong et al. 1999). The RANKL-RANK interaction subsequently
induces trimerization of RANK and the recruitment of RANK main adaptor molecule,
TRAF6, for the activation of intracellular signalling as described in Section 1.1.2 and
shown in Figure 1.3, which is critical for differentiation and activation of osteoclasts

Chapter One – Bone Biology
40
(Kobayashi et al. 2001; Lomaga et al. 1999; Wong et al. 1999). RANKL expression has
been shown to be upregulated by osteoclastogenic factors, such as vitamin D3,
prostaglandin E2, PTH, IL-1, IL-6, IL-11, IL-17, and TNF-α (Horwood et al. 1998;
Kong et al. 1999; Lee & Lorenzo 1999; Nakamura et al. 2012; Theill, Boyle &
Penninger 2002; Yasuda et al. 1998). This RANKL-RANK system is closely regulated
by OPG, secereted by osteoblasts, which acts as a decoy receptor for RANKL (Yasuda
et al. 1998) (Figure 1.2). Mice lacking OPG have been shown to have severe
osteoporosis caused by enhanced osteoclast activity (Bucay et al. 1998; Nakamura et al.
2003).
TNF-α expression and secretion by osteoblasts (Bu et al. 2003; Gowen et al. 1990) have
shown to induce osteoclast differentiation and activity in the presence of M-CSF,
independent of RANKL signalling (Fuller et al. 2002). This signalling mechanism has
been confirmed by the robust induction of osteoclast differentiation and activity by
TNF-α in the presence of OPG. Fuller et al., 2002 has also shown that TNF-α enhances
the RANKL-induced osteoclast differentiation and activation through the formation of
actin ring. Further research by Yarilina, A et al. 2010 has shown the mechanism that
TNF induces a sustained calcium oscillation and subsequently NFATc1 activity in
macrophages to enhance osteoclastogenesis in the presence of RANKL. These results
indicate that TNF-α and RANKL work synergistically to drive osteoclast differentiation
and activation through both NF-κB and NFATc1 (through RANK co-stimulatory
pathway, OSCAR/TREM2, as shown in Figure 1.3) signalling pathways.
TGF-β1, as described previously in Section 1.2.2, is the most abundant TGF-β isoform,
expressed and secreted by osteoblasts during bone formation and stored in bone matrix
in its latent form (Hering et al. 2001; Horner et al. 1998; Huang et al. 2007; Pelton et al.
1991). Osteoclast bone resorption activity, through its lysosomal enzymes as described
in Section 1.1.2, has been shown to release and activate TGF-β1 (Oursler 1994;
Pfeilschifter & Mundy 1987; Zuo et al. 2012), which in turn at its high level TGF-β1
could attenuate or inhibit osteoclast differentiation (Janssens et al. 2005; Takai et al.
1998). The mechanism behind its inhibition in osteoclast differentiation, particularly in
in vivo bone remodelling context and in co-culture system, is through the suppression of
RANKL and enhancement of OPG expression by osteoblasts (Takai et al. 1998).
Besides this consistent result on how TGF-β could inhibit osteoclast differentiation,
many other studies have shown that co-stimulation of RANKL/M-CSF on the M-CSF-

Chapter One – Bone Biology
41
stimulated bone marrow cells or extremely pure osteoclast precursor population with
TGF-β could stimulate osteoclastogenesis through the activation of NF-κB pathway
(Kaneda et al. 2000; Koseki et al. 2002). Kim et al., 2005 however have also shown that
apart from RANKL-RANK-TRAF6 signalling pathway, osteoclastogenesis can be
induced through a co-stimulation of TNF-α and TGF-β, indicating that TGF-β indeed
has a regulatory role in osteoclast differentiation and in a big picture, bone remodelling
process, by being involved in the number of important osteoclastogenesis signalling
pathways and its interaction with a wide range of other growth factors, cytokines, and
hormones in bone microenvironment, which needs to be further elucidated. Osteoblast
has also shown to express and secrete BMP2 (Huang et al. 2007), which, together with
RANKL and M-CSF, can induce osteoclast differentiation and survival (Itoh et al.
2001), although the mechanism behind this is still unknown.
Recently, it has been discovered that conditioned medium of OPG-deficient calvarial
osteoblast could inhibit osteoclast formation and at the same time promoted osteoblast
bone formation activity (Hayashi et al. 2012). Through anion-exchange chromatography
and subsequent SDS-PAGE analysis on the protein fractions, the anti-osteoclastogenic
molecule has been found to be the axon guidance molecule, Semaphorin 3A (Sema3A).
It has been found that Sema3A inhibition of osteoclastogenesis before RANKL
stimulation is through its complex with a receptor complex of the ligand-binding
subunit Nrp1, which then binds to the class A plexins 1 (PlxnA1) to suppress its
signalling pathway of PlxnA1-TREM2-DAP12 (Hayashi et al. 2012). This results in the
severely impaired osteoclastic gene expression of Cathepsin K, TRAP, and NFATc1,
and hence the inhibition of osteoclast differentiation in the Sema3A-treated bone
marrow macrophages (BMMs) (Hayashi et al. 2012). In addition, Hayashi et al. 2012
also showed that the migration of BMMs were impaired in Sema3A-treated cells as the
RhoA activation, which is important in actin cytoskeletal rearrangement (Kruger,
Aurandt & Guan 2005), in response to M-CSF was abolished. On the other hand,
Sema3A KO mice have been shown to have a massive decrease in alkaline phosphatase
activity and bone nodule formation, which was also reflected in the suppression of
osteoblastic genes expression, such as Runx2, Osx, and osteocalcin, while at the same
time induced adipocyte differentiation (Hayashi et al. 2012). The mechanism behind
this phenotype was then revealed to be the significant reduction in genes expression of
most of the transcriptional target and nuclear accumulation of β-catenin (Hayashi et al.
2012), which is a critical factor in the canonical Wnt signalling pathway, as shown in

Chapter One – Bone Biology
42
Figure 1.6. The activation of small G protein Rac1, which has been shown to be
important in promoting β-catenin nuclear translocation (Wu et al. 2008), was also
reduced in Sema3A KO mice (Hayashi et al. 2012). Hence, Sema3A, a novel osteoblast-
secreted factor, has a major role in maintaining bone homeostasis by regulating both
osteoclast and osteoblast differentiation and activation.
Research on how osteoblast controls osteoclast activity still needs to be done. There is
an indication that osteoblast might control osteoclast activity by controlling the
secretion of bone matrix proteins, such as osteopontin (OPN) and bone sialoprotein
(IBSP) (containing arginine-glycine-aspartic acid (RGD) sequences), which are needed
by the osteoclast to attach to bone surface via its αvβ3 integrin (Murphy et al. 2005;
Ross & Teitelbaum 2005; Schaffner & Dard 2003; Yamamoto et al. 1998).
Furthermore, a recent study has shown that OPN can induce Ca2+ oscillation in
osteoclast, hence resulting in an enhanced NFATc1 activation (Tanabe et al. 2011).
However, the mechanism behind this signalling pathway together with other potential
bone matrix proteins in regulating osteoclastogenesis is still unknown and hence, further
study in this area is necessary.
1.3.2 Osteoclast regulation of the osteoblast
As the mechanism on how osteoblasts regulate osteoclast differentiation has been well
studied, the other way of communication, in which osteoclasts express factors to
regulate osteoblastogenesis, is still largely undiscovered. After osteoclast stops its bone
resorption activity, the ‘reversal’ (quiescent) and new bone formation phases begin,
when osteoblasts lay new bone matrix proteins in regulated manner in the resorbed
compartments (Everts et al. 2002; MacDonald & Gowen 1993; Natalie A. Sims &
Jonathan H. Gooi 2008; Zuo et al. 2012). Studies on nanotopography have shown that
osteoclasts might regulate osteoblast bone formation activity by using the size and
shape of its resorbed area (N. A. Sims & J. H. Gooi 2008).
Many cytokines and growth factors are released and activated during osteoclast bone
resorption activity and might stimulate osteoblast activity. One of the classical factors is
the insulin-like growth factor (IGF) I and II (Hayden, Mohan & Baylink 1995), with
IGF-II been the major growth factor stored in bone. IGFs, released in active form from
bone matrix during osteoclast bone resorption, stimulate osteoblast activity to initiate
site-specific bone formation in proportion to the resorbed bone volume (Hayden, Mohan

Chapter One – Bone Biology
43
& Baylink 1995). Furthermore, Zhang, M et al. 2002 has shown that OB-specific
deletion of type I IGF receptor (Igf1r) results in a significant decrease of trabecular
bone volume, trabecular number and connectivity, and hence an increase in trabecular
spacing. These mice show an osteoporotic phenotype. In vitro data showed that there
was a striking decrease in bone mineralization activity by the osteoblast of these mice
(Zhang et al. 2002). Study from Power, R. A et al. 2002 showed that IGF-I gene
expression was upregulated in ovariectomised (OVX) mice treated with fibroblast
growth factor (FGF), which mediated at least in part the increase in trabecular bone
volume in these mice compared to the vehicle–treated OVX group. These results show
the importance of osteoclast activity in the release and activation of cytokines and/or
growth factors from bone matrix to initiate and regulate bone formation activity by the
osteoblast.
The other well-known factor that regulates the migration of bone mesenchymal stem
cells (BMSCs) to the resorptive sites to couple bone resorption with formation is TGF-
β1 (Hughes, Aubin & Heersche 1992; Lucas 1989; Oreffo et al. 1989; Tang et al. 2009).
High level of active TGF-β1 has been shown to be present in conditioned medium from
osteoclast cultured on bone slices, hence bone resorption is critical for the release and
activation of TGF-β1 (Tang et al. 2009). By using a mouse model lacking TGF-β1 gene
and the injection of the osteogenic BMSCs with GFP tag into these mice, it was then
proved that in reference to WT TGF-β1 null mice had its transplanted BMSCs dispersed
in the bone marrow and only very few were detected at the bone surface, again showing
the importance of TGF-β1 for the migration of BMSCs to the bone surface (Tang et al.
2009). Furthermore, SMAD3 and 4 have been found to be the main signalling pathway
involved in TGF-β1-induced migration of BMSCs to bone surface (Tang et al. 2009).
Another factor that is secreted by osteoclasts and acts on osteoblasts is sphingosine 1-
phosphate (S1P). S1P enhances RANKL expression, as well as migration and survival
of osteoblast cells (Ryu et al. 2006). Recently, it has been discovered that S1P also has
an autocrine effect, where it regulates the migration of osteoclast precursors to and from
bone surface, hence it is holding a major role in a healthy bone remodelling process
(Ishii et al. 2009). This result has been supported by the osteoporotic phenotype of type
1 S1P receptor (S1PR1) KO mice, as there was an enhanced osteoclast attachment on
the bone surface and poor recirculation of S1P-driven osteoclast precursor to systemic
blood flow (Ishii et al. 2009).

Chapter One – Bone Biology
44
A recent study has found an osteoclast-expressed factor that regulates osteoblast
activity, which is now known as semaphorin 4D (Sema4D) (Negishi-Koga et al. 2011).
The gene expression of Sema4D is up regulated during RANKL-induced
osteoclastogenesis and a low expression is detected in osteoblasts (Negishi-Koga et al.
2011). The interaction between Sema4D, as an osteoclast membrane-bound factor, and
its receptor Plexin-B1 on osteoblasts causes the activation of the small GTPase RhoA.
This RhoA activation in turn, through Rho-associated protein kinase (ROCK) pathway,
suppresses IGF-I signalling and induces osteoblast motility, thereby suppressing
osteoblast differentiation and its bone formation activity (Negishi-Koga et al. 2011).
With regards to osteoblast motility in Sema4D KO mice model, they also showed that
there were few quiescent bone surfaces and a cluster of osteoblasts in close distance to
osteoclasts, indicating that Sema4D is required for regulating osteoblast localization,
through IGF-I signalling pathway, and hence the maintenance of quiescent surfaces
between osteoblasts and osteoclasts (Negishi-Koga et al. 2011).
Mature osteoclasts have also been found to express another cytokine called
cardiotrophin-1 (CT-1), which is able to regulate osteoblast differentiation and activity
(Walker et al. 2008). CT-1 treatment on murine stromal Kusa cells had resulted in dose-
dependently elevated ALP activity and bone nodules formation as well as an increase in
both STAT3 and ERK phosphorylation, resulting in an enhanced osteoblast activity
(Walker et al. 2008). This enhanced osteoblast activity has also been supported by the
finding that CT-1 induced 2-fold increase in Runx2 gene transcription activation by
using 6xOSE2 osteocalcin reporter assay. Lastly, by using CT-1 null mice model, in
vitro and in vivo experiments showed that not only there was a reduced osteoblast
activity, but also bigger osteoclasts (an increase in DCSTAMP gene expression) and
impaired bone resorption were also observed in reference to WT (Walker et al. 2008).
Hence CT-1 is another osteoclast-derived coupling factor that regulates both osteoclast
and osteoblast differentiation and activity (Walker et al. 2008).
1.3.3 Bidirectional signalling between osteoclasts and osteoblasts
Recent and promising studies in the coupling system between osteoclast and osteoblast
have shown that cell-to-cell contact between the two cells can directly regulate the
differentiation and activity of both cells. Eph receptors are tyrosine kinase receptors and
together with its ligand, Ephrin, are classified into A and B subgroups (mainly based on

Chapter One – Bone Biology
45
their structural homologies). The Eph-Ephrin interaction provides a bidirectional
signalling, producing forward (Eph) and reverse (Ephrin) signals (Irie et al. 2009;
Matsuo 2010; Zuo et al. 2012). EphrinB2, a membrane-bound ligand expressed by
osteoclasts, has shown to bind to its receptor EphB4, expressed by osteoblasts (Zhao et
al. 2006; Martin et al. 2010). This binding has been shown to result in the suppression
of osteoclastogenesis by inhibiting the NFATc1 signalling pathway (as reverse
signalling) and at the same time promotes osteoblast differentiation via the inhibition of
RhoA pathway as well as an enhanced ERK1/2 phosphorylation (as forward signalling)
in mouse (Zhao et al. 2006). Further research has shown that PTH can induce the gene
expression of EphrinB2 in osteoblasts (Allan et al. 2008), suggesting that this
EphrinB2-EphB4 interaction might contribute to the anabolic effect of PTH on
osteoblasts (Irie et al. 2009). Hence this cell-to-cell contact dependence communication
of EphrinB2-EphB4 has been proposed to be a crucial control for the transition from
resorption/osteoclast activation phase to renewal/bone formation phase (Irie et al. 2009).
Other Ephrin-Eph bidirectional signalling has been shown by the interaction of
EphrinA2, expressed by osteoclast precursors, with its receptor EphA2, expressed also
by osteoclast precursors (autocrine signalling) and osteoblasts (Irie et al. 2009).
Overexpression of both EphrinA2 and EphA2 in osteoclast precursors, producing both
forward and reverse signalling, has been shown to result in an enhanced osteoclast
differentiation through the phospholipase Cγ2 signalling pathway (Irie et al. 2009). On
the other end for osteoblasts, the forward signalling of EphA2 has shown to inhibit
osteoblast differentiation through the regulation of RhoA activity (Irie et al. 2009). To
finally conclude, by fine tuning the EphrinB2-EphB4 and EphrinA2-EphA2
bidirectional signalling pathways to inhibit osteoclast bone resorption activity and to
increase osteoblast bone formation activity, the bone remodelling process in
postmenopausal women could be corrected (Zuo et al. 2012).
1.4 Bone Diseases
Osteoclasts and osteoblasts, being the two main players in the bone environment,
coordinate with other bone cells (as shown in Figure 1.4) to achieve a healthy bone
mass that can avoid any structural defects and fractures in our skeleton (Dempster et al.
2012; Uthgenannt et al. 2007). As described earlier, bone remodelling process starts

Chapter One – Bone Biology
46
when bone-matrix is resorbed by osteoclasts and osteoblasts then lay down new organic
bone matrix, called osteoid, in the resorbed compartments in a balanced manner, which
eventually gets mineralized to form strong and healthy bone. Disruption in this system
will result in a number of pathological bone diseases, such as osteoporosis,
osteopetrosis, and Paget’s disease of bone (PDB).
1.4.1 Osteoporosis
Osteoporosis is characterised by a net bone loss and a decrease in bone strength, caused
generally by an excessive osteoclastic bone resorption (Kular et al. 2012; Riggs &
Melton 1983). As bone becomes weaker, susceptibility of fractures increases and
usually the signs show up after the initial fractures. The lifetime fracture risk for
osteoporotic patients could be as high as 40% (Burge et al. 2007; Melton et al. 1992;
Rachner, Khosla & Hofbauer 2011; Ray et al. 1997). Early diagnostic strategy for
osteoporotic condition includes the measurement of bone mineral density (BMD) of the
osteoporotic patients, which can be assessed by using dual x-ray absorptiometry (DXA),
and osteoporotic condition has been defined as a condition having a T score of less than
2.5, which is well more than 2.5 standard deviations below the average of a young adult
(Rachner 2011).
The two most important factors in osteoporosis are the loss of gonadal function, seen
mostly in postmenopausal women (Riggs & Melton 1983), and aging (Manolagas &
Jilka 1995). In postmenopausal period, there is an altered (upregulated) regulation of
many cytokines, such as IL-1, TNF-α, IL-6, which are potent inducers for osteoclast
differentiation and bone resorption activity (Horowitz 1993). As research progresses, it
is then known that the mediator of this increase in osteoclast activity is the upregulated
RANKL expression by osteoblasts and other cells (Eghbali-Fatourechi et al. 2003). On
the other hand, there is a continuous decline of osteoblast bone formation activity in
aged people, hence less bone formed in proportion to the demand for them (Manolagas
& Jilka 1995; Riggs & Melton 1983).
Treatment of osteoporosis mainly focuses on the prevention of further fractures. Firstly,
nutrition, life style (exercise), and dietary intake (calcium and Vitamin D) are all
important factors that can maximise our bone mass and can also slow down the rate of
bone loss and reduce fracture risk throughout life (Delmas 2002; Raisz 2005b). Anti-

Chapter One – Bone Biology
47
resorptive therapy, such as bisphosphonate (alendronate, risedronate, and ibandronate),
has been shown to reduce the incidence of fractures in both vertebral and non-vertebral
and in hip region (Rosen 2005). Osteoclasts take up bisphosphonate, which binds onto
bone surface, and undergo apoptosis, hence this treatment slows down the bone
remodelling process (Delmas 2002; Fleisch 2000). The anabolic agent, PTH, treatment
is only approved by FDA in 2002 and it has been shown that daily injection of PTH (N-
terminal portion) could increase bone formation, hence an increase in bone mass, while
only affected little on osteoclast bone resorption activity (Neer et al. 2001). Current
therapeutic treatments for osteoporosis have mainly focused on the bone remodelling
process, in which Denosumab, a novel recombinant human monoclonal RANKL-
specific antibody has been shown to suppress bone resorption, hence effectively reduces
vertebral, non-vertebral, and hip fractures (Dempster et al. 2012) in postmenopausal
women. Studies have been planned to look at the efficacy and safety profile of
Denosumab for the treatment of male osteoporosis and glucocorticoid-induced
osteoporosis as well as its long-term use out of 10 years with a bigger participant
(Rizzoli, Yasothan & Kirkpatrick 2010). Other novel treatments include the use of
Cathepsin K-specific inhibitor (another anti-resorptive therapy), odanacatib, and
antibodies against the inhibitors of bone formation (anabolic therapies), sclerostin and
Dkk-1, which all of them have shown promising pre-clinical and clinical results (Bone
et al. 2010; Gauthier et al. 2008; Heath et al. 2009; Ominsky et al. 2010; Rachner,
Khosla & Hofbauer 2011; Stoch et al. 2009).
1.4.2 Osteopetrosis
In contrast to osteoporosis, osteopetrosis is an autosomal recessive disorder
characterised by an abnormal high bone density. This ‘stone bone’ disease varies across
suffering individuals, with the most severe cases causing optical nerve compression and
death in childhood (Quarello et al. 2004).
Several mutations have been identified in human, including in RANKL and RANK
genes, which cause osteoclast-poor autosomal recessive osteopetrosis (ARO) (Guerrini
et al. 2008; Sobacchi et al. 2007). On the other hand, the defect in osteoclast bone
resorption activity, particularly connected to the V-H+ATPase acidification machinery
of osteoclasts, contribute to the infantile malignant osteoclast-rich ARO, which counts
for about 70% of cases (Villa et al. 2009). In 2000, Frattini, A et al has shown that 50%

Chapter One – Bone Biology
48
of osteoclast dysfunction cases in ARO was found to have mutation in TCIRG1
(encoding a3 subunit of V0 domain of V-H+ATPase proton pump), which resulted in
the formation of osteoclasts that were unable to resorb bone. Mutation in ClCN7
chloride channel has also been shown to be another cause of osteoclast-rich ARO
(Frattini et al. 2003; Kornak et al. 2001), although there is also a strong link between the
ClCN7 mutation and neurodegeneration (hinting the involvement of ClCN7 in the
nervous system) (Kasper et al. 2005). The less common cause of osteoclast-rich ARO is
carbonic anhydrase (CA)-II mutation, which is easily diagnosed as it is accompanied by
renal tubular acidosis and cerebral calcification (Sly et al. 1983). Specifically in
osteoclasts, loss of CA-II function causes osteoclasts unable to acidify (generating H+)
the intended resorbed bone compartment, hence preventing its bone resorption activity
(Whyte 1993).
The current curative treatment for ARO is total bone marrow transplant (allogeneic
hematopoietic stem cell therapy (HSCT)) (Eapen et al. 1998) and it has shown to cure
for RANK, TCIRG1, and CA-II mutations-caused osteopetrosis (Frattini et al. 2000;
Guerrini et al. 2008; McMahon et al. 2001). Meanwhile, mesenchymal cells (MSCs)
transplant and/or administration of exogenous RANKL administration are still on
clinical trials for the treatment of RANKL mutation-induced ARO (Villa et al. 2009).
1.4.3 Paget’s disease of bone (PDB)
Paget’s disease of bone (PDB) is characterised by a local increase in bone turnover and
usually has no symptoms (Selby 2005). It is a common disease with age, coming second
after osteoporosis. In this PDB pathological condition, there is an accelerated bone
remodelling activity in the affected areas of bone, which includes the presence of giant
and active multinucleated osteoclasts (Kanis 1991). The bone formation is also
increased but in a disorganised manner. These conditions then eventually lead to the
formation of woven bone, which can develop to form bone deformity and increases the
risk of fractures (Kanis 1991; Langston et al. 2007; Ralston & Layfield 2012).
The abnormality in osteoclast is the hallmark of PDB. They have an abnormal increase
in number and size, hence having more nuclei than normal controls (Roodman &
Windle 2005). The osteoclasts of PDB also have unique nuclear inclusions, which are
made up of microcylinders in paracrystalline arrays similar to nucleocapsids of

Chapter One – Bone Biology
49
paramyxovirus (Mills, Yabe & Singer 1988; Rebel et al. 1981). Further investigations
into osteoclast biology have shown that in in vitro osteoclastogenesis monocytes from
Paget’s patients were hyper-responsive to RANKL and 1,25-(OH)2 vitamin D3, hence
generating significantly more osteoclasts and having an increase in bone resorption,
compared to normal controls (Neale et al. 2000). This result is in line with the finding
that there was an upregulation of RANKL gene expression in pagetic-lesion-developed
stromal cells and in Paget’s patient bone samples compared to healthy controls (Menaa
2000).
To date, the original cause of PDB is still unknown. However mutation in the SQSTM1
gene has been identified to be the common and familial (being autosomal dominant-
transmitted disease) linkage to the development of PDB (Hocking et al. 2001; Laurin et
al. 2001). The exact recurrent mutation of this gene affects primarily on p62 protein
(Laurin et al. 2002), which binds to the deubiquitinating enzyme CYLD and plays an
important role in NF-κB signalling pathway (Jin et al. 2008). The binding of p62 to
CYLD inhibits RANKL-induced osteoclastogenesis by deubiquitinating TRAF6 (Jin et
al. 2008). Hence, the point mutation at p62 causes CYLD unable to bind to p62, which
eventually leads to TRAF6 ubiquitination and NF-κB signalling pathway activation. In
conclusion, SQSTM1 is the gene most frequently affected in PDB, besides numerous
evidences of involvement of other mutations in genes related to osteoclast
differentiation, such as CSF-1 (M-CSF-coding gene) and TNFRSF11A (RANK-coding
gene) (Albagha et al. 2010). The current management for PDB is by using
bisphosphonate (Kular et al. 2012; Langston et al. 2007; Ralston & Layfield 2012; Reid
et al. 2005).

50
CHAPTER 2
SEMINAL VESICLE SECRETION (SVS) 7 PROTEIN AND LY-6
PROTEIN FAMILY

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
51
2.1 Introduction
Highly regulated cell-to-cell communication between osteoclasts and osteoblasts is a
prerequisite for sustaining a healthy bone mass (Karsenty & Wagner 2002; Zaidi 2007).
As mentioned in Chapter 1, one of the methods to achieve this cell-to-cell
communication is through secretion of diffusible paracrine factors, which can be
cytokines, chemokines, growth factors, or proteins, by either cell acting on the other
(Matsuo & Irie 2008). As osteoblast regulation of the osteoclast differentiation and
activation has been well studied, research on osteoclast-expressed novel factors or
proteins regulating osteoclast (autocrine) and/or osteoblast (paracrine) differentiation
and function remains limited. The identification of novel intercellular coupling factors
will enhance our understanding on this basic regulation of osteoclast and osteoblast in
bone microenviroment and help uncover new targets and/or therapies for the treatment
of pathological bone diseases.
2.2 Seminal vesicle secretion (Svs) 7
Svs7 was originally identified in bovine seminal plasma (Rufo et al. 1982), and later in
reproductive tract fluid and seminal vesicle content (SVC) of guinea pig (Coronel, San
Agustin & Lardy 1988), rat and mouse (Coronel et al. 1992). Svs7 gene has been
identified to be at chromosome 9 in mouse and chromosome 11 in human (Margalit et
al. 2012; Turunen et al. 2011). Further study on the protein composition and
functionality shows that Svs7, a small 8538Da (99 amino acids) protein, is a secreted
protein, harbouring N-terminal sequence, which contains signal peptides, and lacking a
carboxyl-terminal glycosylphosphatidylinositol (GPI) moiety (Adermann et al. 1999;
Levitin et al. 2008; Luo, Lin & Chen 2001; Ploug et al. 1991; Turunen et al. 2011). By
binding to post-acrosomal region of head, midpiece, and tail region of the sperm (Luo,
Lin & Chen 2001; Margalit et al. 2012) and having cysteine residues (Figure 2.1) to
form disulphide bonds (Luo, Lin & Chen 2001), functionally mouse Svs7 has been
shown to inhibit Ca2+ influx across the membrane of the sperm cells during their transit
from vagina to oviduct in order to prevent premature acrosomal reaction and
spermatozoa hyperactivation (Coronel et al. 1992). Hence, Svs7 is also known as
calcium transport inhibitor (caltrin) (Coronel et al. 1992; Rufo et al. 1982). Any
biological modifications (reduction and/or alkylation) on these cysteine residues have

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
52
been shown to abolish this Ca2+ transport inhibitory activity of Svs7 (Coronel et al.
1992). The nature of the binding partners/sites of Svs7 protein has been shown to be
lipids, which are reported to be phosphotidylethanolamine and phosphotidylserine (Luo,
Lin & Chen 2001). This specific binding of Svs7 to the phospholipid liposomes of the
sperm cells has been shown to enhance sperm motility. However there is still no further
study showing the significances and possible downstream signalling pathways coming
from this binding/interaction.
Additionally, Svs7 is also known as Prostate and testes-expressed protein (PATE)-B,
whose gene has been shown to be highly expressed in prostate and interestingly lower
expression was detected in testes (Turunen et al. 2011). Not surprisingly, Svs7
expression has been shown to be regulated by androgen (Levitin et al. 2008). Castration
enhances the prostate gene expression of PATE-B, while the administration of
dihydroxytestosterone (DHT) has been shown to ablate this induction (Levitin et al.
2008). With the consensus cysteine residues domain, Svs7 /PATE-B has shared this
distinctive pattern with lymphocyte antigen (Ly)-6 family (Levitin et al. 2008; Turunen
et al. 2011). Both protein families share the characteristic of three-fingered proteins
(TFP)/Ly-6/urokinase-type plasminogen activator receptor (uPAR) consensus domain,
which is discussed in Section 2.3 below (Levitin et al. 2008; Turunen et al. 2011).
2.3 Svs7 as a secreted member of Ly-6 protein family and the
biological importance of other Ly-6 proteins
Svs7 is a secreted member of Ly-6 protein family, which shares the TFP/Ly-6/uPAR
common motif consisting of a conserved cysteine (C) residues (8-10 residues forming
disulphide bonds), and a carboxyl (C)-terminal consensus sequence motif of
CCXXXXCN, with X represents any amino acid residue, as shown in Figure 2.1
(Coronel et al. 1992; Southan et al. 2002; Turunen et al. 2011; Ushizawa et al. 2009).
This family also includes membrane-linked proteins, which are anchored to the plasma
membrane through a post-translationally added C-terminal GPI attachment (Margalit et
al. 2012; McKenzie et al. 1977; Ploug et al. 1991).

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
53
Svs7 SLURP-1 SLURP-2 Ly6a UPAR
Svs7 SLURP-1 SLURP-2 Ly6a UPAR
(Sca-1)
(Sca-1)
Figure 2.1 Consensus cysteine residues and a C-terminal consensus sequence motif
of CCXXXXCN (TFP/Ly-6/uPAR domain) of Ly-6 proteins family. Amino acids
alignment of Svs7 and other Ly-6 proteins (2 secreted proteins, SLURP-1 and -2 and 2
membrane-bound, Ly-6a (Sca-1) and uPAR) showing a consensus cysteine residues
(forming disulphide bonds) and a C-terminal consensus sequence motif of
CCXXXXCN (both features are shown in red-coloured letters), where X represents any
amino acid residue and the N stands for asparagine. These two features represent the
TFP/Ly-6/uPAR consensus domain of Ly-6 protein family.

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
54
For the purpose of this chapter, only two other secreted Ly-6 proteins named secreted
Ly-6/uPAR-related protein (SLURP)-1 (Adermann et al. 1999) and -2 (Tsuji et al.
2003), and two GPI-anchored proteins, Stem cell antigen (Sca)-1 (Bonyadi et al. 2003)
and uPAR (Ohkura et al. 1994), will be discussed with regard to their known biological
roles in order to reveal the current understanding of the significances of this protein
family in the human biological system, especially in bone biology.
After its identification as the first secreted Ly-6 protein (Adermann et al. 1999), further
research has shown that SLURP mRNAs (both 1 and 2) are expressed in variety of
tissues and organs, including spleen, thymus, and brain (Moriwaki et al. 2007;
Moriwaki et al. 2009). The study of SLURP-1 becomes more and more important since
the finding that mutation in this gene causes an autosomal recessive inflammatory
palmoplantar keratodema, Mal de Meleda (MDM) (Fischer et al. 2001), showing its
important expression in skin and keratinocytes (Arredondo et al. 2005; Chimienti et al.
2003)
These two pioneering studies have shown a crucial role of SLURP-1 as an α7 subunit of
nicotinic acetylcholine receptors (nAChRs) ligand to regulate keratinocytes
differentiation and apoptosis. SLURP-2, which shares substantial protein homology
with SLURP-1, is also expressed in skin and keratinocytes (Tsuji et al. 2003). It has
been reported that SLURP-2 binds to the α-3 nAChRs, which is important in preventing
keratinocytes apoptosis (Arredondo et al. 2006) and hence its gene expression was
shown to be upregulated by 3-fold in psoriatic lesional skin compared to healthy
controls (Tsuji et al. 2003). These results suggest the importance of SLURP-1 and -2 in
maintaining epidermal and keratinocytes homeostasis through their fine-tune regulation
of nAChRs signalling pathway. Because of structural homology within Ly-6 protein
family (shown in Figure 2.1), not surprisingly Svs7 has also been shown to regulate α7
nAChR and has no effect on other nAChR (Levitin et al. 2008). Even though there is
common functionality between these ly-6 proteins in regulating nAChRs, further
investigation, particularly for Svs7 in this signalling, is still required, as only one
published study is currently available in this topic. Furthermore, the detection of
SLURP-1 and -2 expression in T and B cells, bone marrow-derived dendritic cells, and
macrophages prompts future studies to elucidate the possible role of these two proteins
in immune system and possibly in bone homeostasis (Moriwaki et al. 2007).

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
55
Sca-1 (Ly-6A), an 18kDa GPI-linked Ly-6 protein, has been shown to be an important
factor in bone microenvironment as it is expressed by many different kinds of stem
cells, such as hematopoietic stem cells (HSCs), skeletal muscle stem cells, and
mammary epithelial stem cells, a subpopulation of bone marrow (BM) stromal cells
including osteoblasts, and Sca-1 KO mice exhibit age-dependent osteoporotic
phenotype as a result of defects in stem cell renewal capacity (Bonyadi et al. 2003;
Gussoni et al. 1999; Ito et al. 2003; Trevisan & Iscove 1995). Sca-1 KO mice have
healthy bone during adulthood, but with age they develop a massive decrease in bone
mass by having defects in self-renewal capacity of mesenchymal stem cells (MSCs)
specifically (Bonyadi et al. 2003). Consistent data has shown a significant decrease in
osteoprogenitor population (starting from 7-month old mice and onward) and markedly
reduced bone formation activity in in vitro colony-forming unit (CFU)-alkaline
phosphatase (ALP) and bone nodule formation assay of both Sca-1 KO primary murine
calvarial and BM stromal cell-derived osteoblasts, hence Sca-1 KO mice have a
significantly lower whole body bone mineral density (BMD) than controls (Bonyadi et
al. 2003; Holmes et al. 2007). As MSCs make a key component in HSCs niche (Ito et
al. 2003; Mansour et al. 2012), Sca-1 (an important antigen marker for both MSCs and
HSCs) holds a central role in maintaining the self-renewal capacity of stem cells, hence
it is one of crucial factors in maintaining homeostasis of bone microenvironment. Its
importance in bone homeostasis is further supported by its expression in mature
osteoclasts (>2-fold increase), shown in Figure 2.3, hence encouraging further research
of this gene in bone environment.
Lastly, uPAR is another GPI-linked Ly-6 protein (Ohkura et al. 1994). uPAR has been
well studied as the regulator of the plasminogen activation system by binding to its
ligand uPA and pro-uPA (Smith & Marshall 2010), showing its crucial role in the
degradation and clearance of fibrin clots (fibrinolysis) and the activation of MMP9 and
13 (Carmeliet et al. 1997). Besides its function in this proteolysis system, uPAR has
also been shown to be involved in many signalling pathways, governing cell motility,
invasion, proliferation, and survival (Smith & Marshall 2010), such as in mitogen-
activated protein kinases (MAPK) (Aguirre Ghiso 2002; Kjoller & Hall 2001; Liu et al.
2002; Vial, Sahai & Marshall 2003) and signal transducer and activator of transcription
(STAT) pathways (Degryse et al. 2005; Koshelnick et al. 1997; Lester et al. 2007). With
this involvement of uPAR in many biological systems, extensive studies have shown
that its expression is elevated during inflammation, tissue remodelling, and in many

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
56
human cancers (Del Rosso et al. 2008; Guerrini et al. 2008; Jacobsen & Ploug 2008).
Being GPI-anchored and therefore lacking transmembrane and intracellular domains,
uPAR must interact with transmembrane receptors to carry its role in regulating
intracellular signalling pathways (Smith & Marshall 2010). Many studies have shown
evidences that integrins are uPAR crucial co-receptor in signalling pathways (Madsen et
al. 2007; Smith & Marshall 2010; Zhang et al. 2003). Amongst many studies
elucidating the interaction of integrins isoforms and uPAR, αvβ3 integrin, which is
highly expressed by osteoclasts (Duong et al. 1998; Nakamura et al. 2012), has been
shown to interact with uPAR (Schiller et al. 2009; Smith, Marra & Marshall 2008; Wei
2008) and this interaction regulates subsequent signalling pathways, notably governing
cell proliferation and survival (MAPK pathway) (Woods et al. 2001) and cell motility
through the activation of Rho family small GTPase Rac (Kjoller & Hall 2001; Lester et
al. 2007; Smith, Marra & Marshall 2008; Vial, Sahai & Marshall 2003). This activation
of Rac has been shown to regulate downstream signalling pathway through p130Cas,
which is important for the formation of F-actin ring (sealing zone), a crucial step for
osteoclast bone resorption activity, as discussed in Chapter 1 Section 1.1.2 (Lakkakorpi
et al. 1999; Smith, Marra & Marshall 2008). With the binding of integrin to
extracellular matrix (ECM) proteins, such as vitronection (Lakkakorpi et al. 1999;
Nakamura et al. 2012), to induce its downstream signalling pathway, further research is
needed to confirm the role of uPAR in its interaction with integrins and ECM proteins
and many molecular details of uPAR signalling pathways, which still remain unclear
(Smith & Marshall 2010).

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
57
2.4 Identification of Ly-6 family member, Svs7, as a putative
osteoclast-derived coupling factor
Current research in our laboratory has focussed on elucidating novel factors, secreted by
osteoclast and/or osteoblast, which have potential roles in regulating either or both cells,
hence is crucial in maintaining bone homeostasis (Kular et al. 2012). Using subtractive
hybridization-based differential screening method on RAW264.7 cells with (mature
osteoclasts) and without (osteoclast precursors) RANKL stimulation, Phan 2004
identified Svs7 gene, only expressed by mature osteoclasts and not by osteoclast
precursors (Davey 2008), as shown in Figure 2.2. Furthermore, microarray heatmap
analysis on Svs7 and other Ly-6 genes expressions in mature osteoclasts (relative to
osteoclast precursors) shows that Svs7 is the most highly expressed gene by mature
osteoclasts amongst other Ly-6 genes (more than 10-fold increase in Svs7 gene
expression by mature osteoclasts) (Figure 2.3).
The initial study of this Ly-6 family member, Svs7, was then continued by investigating
its gene expression in other key bone cells. It is revealed that Svs7 is only expressed by
osteoclasts but not by osteoblasts or other key bone cells (Figure 2.4A) and its gene
expression is upregulated at day 3 and 5 during RANKL-induced differentiation of bone
marrow macrophages (BMM) into mature osteoclasts, in parallel with other known
osteoclast marker genes, such as TRAP, CTR, and NFATc1 (Figure 2.4B). Hence, Svs7
is a novel osteoclast-expressed factor.
In conclusion, with many Ly-6 genes have shown to be involved in many cellular
signalling pathways, such as uPAR in αvβ3 integrin signalling pathway, which is
crucial for osteoclast bone resorption activity, and Sca-1, being the central player for
stem cell renewal capacity, it was then of interest to elucidate the biological role of
Svs7, a novel osteoclast-expressed factor and shown to be the most highly expressed
Ly-6 gene by mature osteoclasts, in regulating osteoclast-osteoblast differentiation and
activation, hence in maintaining bone homoeostasis.

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
58
Driver Forward subtraction
Driver: RAW264.7
Svs7
RAW264.7 + RANKL
Figure 2.2 Identification of Svs7 gene using subtractive hybridization-based
differential screening in RAW264.7 cells culture with RANKL stimulation. (Top
panel) RAW264.7 cells were stimulated with RANKL to form multinucleated osteoclasts.
(Bottom panel) messenger RNA (mRNA) was extracted from osteoclasts and osteoclast
precursor RAW264.7 cells and was hybridized. Forward and reverse screening was done
to remove false positives and cDNA probes, labelled with 32p-dCTP (deoxycytidine
triphosphate), were used to isolate the clones. Among the isolated and sequenced
clones, Svs7 was identified, only expressed by mature osteoclasts and not by osteoclast
precursors. (Figure adapted from Davey, 2008)

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
59
-1 0 1
Precursor (P)
Mature (M)
Osteoclast
Acrv1 Ly6a Ly6c Ly6d Ly6e Ly6f Ly6g5b Ly6g5c Ly6g6c Ly6g6d Ly6g6e Ly6i Ly6k Lynx1 Psca Slurp1
Ratio (M/P)
Svs7
0.85 2.07 0.96 0.79 2.36 1.21 1.06 1.12 0.99 1.81 1.07 0.85 0.92 1.02 1.23 1.25
10.49
Figure 2.3 Svs7 is the most highly expressed Ly-6 gene by mature osteoclasts,
shown by the microarray heatmap analysis. RNA of osteoclast precursors (day 0 of
RANKL stimulation) and mature osteoclasts (day 5 of RANKL stimulation) were
reverse transcribed and hybridised for the microarray genes expression profile. The
relative (mature/precursor) gene expression analysis (expressed as fold
increase/decrease), particularly on Svs7 and some other Ly-6 genes expressions, was
carried out and it is clear that Svs7 is the most highly expressed gene by mature
osteoclast amongst other Ly-6 genes (more than 10-fold increase in Svs7 gene
expression by mature osteoclasts).

Chapter Two – Seminal Vesicle Secretion (Svs) 7 Protein and Ly-6 Protein Family
60
(A)
(B)
Svs7
β-actin
OB
C2C
12
BM
M
OC
RAW
264.
7
RAW
264.
7 +
RA
NK
L
β-actin
NFATc1
Svs7
ATP6v0d2
0 1 3 5
RANKL-stimulated
WT BMM day
TRAP
CTR
DCSTAMP
Figure 2.4 Svs7 gene expression in osteoclast. (A) RNA from myoblasts (C2C12),
murine stromal cells-derived osteoblasts culture (OB), BMM, day 5 RANKL-stimulated
BMM (osteoclasts (OC)), osteoclast precursor RAW264.7 cells, and RANKL-stimulated
RAW264.7 cells were subjected to reverse transcriptase-PCR (RT-PCR) reactions using
specific primers for Svs7 and β-actin as a house-keeping gene. Svs7 gene is only
expressed by osteoclasts but not by osteoblasts or other key bone cells. (B) RNA from
time course RANKL-induced differentiation of BMM into mature osteoclasts was
subjected to RT-PCR reactions using specific primers for Svs7 and other common
osteoclast marker genes. Svs7 gene expression is upregulated at day 3 and 5 during
RANKL-induced osteoclastogenesis (Svs7 is exclusively expressed by mature
osteoclasts). β-actin was used as a loading control.

61
CHAPTER 3
HYPOTHESIS AND AIMS

Chapter Three – Hypothesis and Aims
62
3.1 Hypothesis Bone is continuously remodelled throughout life via the interplay between key bone
resident cells; namely the bone-resorbing osteoclast, bone-forming osteoblast, and
mechano-sensing osteocytes. Bone homeostasis is thus maintained by the coordinated
activities between these cells. Disruption in the balance between bone resorption and
formation will result in the development of many pathological conditions, including
osteoporosis, osteopetrosis, and PDB, as described previously in Chapter 1 Section 1.4.
However, the complement of factors, crucially regulating this intimate intercellular
communication “coupling” between osteoclasts and osteoblasts, remain largely
unknown.
Svs7, a secreted Ly-6 family protein (Southan et al. 2002), was previously identified in
our laboratory as a candidate osteoclast-secreted “couling” factor (Davey 2008; Phan
2004). Svs7 gene expression is upregulated during RANKL-induced osteoclastogenesis,
indicating that Svs7 is exclusively expressed by mature osteoclasts in bone.
Furthermore, studies by Davey 2008 found that recombinant purified Svs7 protein
treatment could protect against loss of trabecular bone volume, trabecular thickness, and
trabecular number in ovariectomised mice (oestrogen deficiency-induced bone loss
mouse model (Aitken, Armstrong & Anderson 1972; Kalu 1991; Saville 1969)). When
considering these preliminary observations, together with the established importance of
Ly-6 family members in many intracellular signalling pathways (e.g. Sca-1, which is
also expressed by osteoclasts) and their crucial role in maintaining self-renewal capacity
of stem cells (Bonyadi et al. 2003; Holmes et al. 2007), it is conceivable that Svs7 acts
to similarly regulate osteoclast and/or osteoblast differentiation and activity and thus
may play an important role in the maintenance of bone homeostasis. Therefore, the
central hypothesis under investigation in this thesis is that Svs7 is an important
regulator of bone homeostasis via the modulation of osteoclast and/or osteoblast
differentiation and activation.
3.2 Aims To address this, the specific aims of this thesis are:
1. To investigate the physiological importance of Svs7 in bone homeostasis
through the generation and characterisation of:
(i) Mice overexpressing Svs7 (Transgenic)
(ii) Mice lacking Svs7 (Knockout)

Chapter Three – Hypothesis and Aims
63
2. To identify potential intrinsic cellular defects in osteoclasts and/or osteoblasts
derived from Svs7 mouse models
Collectively, these studies will shed light on the as yet unknown role of Svs7 in bone
cells function and uncover its precise role in the maintenance of bone homeostasis.

64
CHAPTER 4
MATERIALS AND METHODS

Chapter Four – Materials and Methods
65
4.1 Materials
4.1.1 Cell lines
Cell line Description Supplier
RAW264.7 (Subclone C4) Murine monocyte cell line Dr. A. I Cassady, Centre
for Molecular and Cellular
Biology, Department of
Biochemistry, University
of Queensland.
4.1.2 Bacterial Strain
Strain Description Supplier
DH5α cDNA insert cloning host,
propagation of plasmid
DNA
Invitrogen, Australia
4.1.3 Chemical reagents
Description Supplier
Acridine Orange Sigma-Aldrich, USA
Acrylamide 30% Bio-Rad Laboratories, USA
Agar Powder Oxoid, UK
Agarose Promega Corp, USA
Alizarin red Raymond A Lamb, UK
Aluminium Sulphate Sigma-Aldrich, USA
Ammonium persulfate Bio-Rad Laboratories, USA
Ampicillin Sigma-Aldrich, USA
(L) Ascorbic acid Sigma-Aldrich, USA
Bacto Yeast Extract Oxoid, UK
Bis-acrylamide Bio-Rad Laboratories, USA
Bovine Serum Albumin (BSA) Hyclone, USA
Chloroform Sigma-Aldrich, USA
Complete Protease Inhibitor Cocktail
Tablets
Roche, Germany
Dexamethasone Sigma-Aldrich, USA

Chapter Four – Materials and Methods
66
Dimethysulfoxide (DMSO) Sigma-Aldrich, USA
Ethanol Thermo Fisher Scientific, USA
Ethylene Diamine Tetra-acetic acid
(EDTA)
Acros, USA
Glacial Acetic Acid Thermo Fisher Scientific, USA
Glycerol Thermo Fisher Scientific, USA
Glycine Sigma-Aldrich, USA
Glutaraldehyde Thermo Fisher Scientific, USA
Haematoxylin Sigma-Aldrich, USA
Hydrochloric acid (HCl) VWR International, Australia
Isopropanol (Propan-2-ol) Thermo Fisher Scientific, USA
Isopropyl-β-D-thiogalactopyranoside
(IPTG)
Promega Corp, USA
β-mercaptoethanol Sigma-Aldrich, USA
Methanol Thermo Fisher Scientific, USA
5x MuLV Reverse Transcriptase Buffer Promega Corp, USA
Phenylmethylsulfonyl Fluoride (PMSF) Boehringer Mannheim Corp, USA
Probenecid Sigma-Aldrich, USA
Skim Milk Powder Standard market brand
Sodium Acetate (NaCH3COO) Merck, Australia
Sodium Chloride (NaCl) Thermo Fisher Scientific, USA
Sodium Dodecyl Sulphate (SDS) AppliChem, Germany
Sodium Hydroxide (NaOH) Sigma-Aldrich, USA
N, N, N’, N’-tetra-methyl-
ethylenediamine (TEMED)
Bio-Rad Laboratories, USA
Trisma Base Thermo Fisher Scientific, USA
Trisma Hydrochloride Thermo Fisher Scientific, USA
Triton X-100 Thermo Fisher Scientific, USA
Trizol Sigma-Aldrich, USA
Trypsin Gibco, Australia
Tryptone Oxoid, UK
Tween-20 Acros, USA
Xylene Thermo Fisher Scientific, USA

Chapter Four – Materials and Methods
67
4.1.4 Tissue culture reagents
Description Supplier
α-MEM (α-Modification of Eagle’s
Medium)
Gibco, Australia
D-MEM (Dulbecco’s-Modification of
Eagle’s Medium)-GlutaMaxTM-1
Gibco, Australia
Foetal Bovine Serum (FBS) Gibco, Australia
Hanks buffer (for Fluo-4AM calcium
assay)
Gibco, Australia
Opti-MEM Reduced Serum Medium Gibco, Australia
Penicillin-Streptomycin Gibco, Australia
Trypsin-EDTA (pH 7.0) Gibco, Australia
4.1.5 Cytokines
Description Supplier
M-CSF Produced in the laboratory in the form of
conditioned media of CMG 14-12 cells
RANKL-GST Produced in the laboratory as described
previously (Xu et al. 2000)
4.1.6 Enzymes
Description Supplier
Collagenase Sigma-Aldrich, USA
DNase I Sigma-Aldrich, USA
2xGoTaq Green Master Mix DNA
polymerase
Promega Corp, USA
M-MuLV Reverse Transcriptase Promega Corp, USA
Restriction Enzymes – HindIII, XhoI, SfuI Promega Corp, USA
RNase inhibitor Promega Corp, USA
SYBR Green Master Mix DNA polymerase Promega Corp, USA
T4 ligase Promega Corp, USA

Chapter Four – Materials and Methods
68
4.1.7 Antibodies
Description Supplier Dilution
Anti-mouse (β) actin
(JLA-20 clone)
Calbiochem 1:5000 (WB 1° Ab)
Anti-DCSTAMP (1A2
clone)
Millipore, USA 1:500 (WB 1° Ab)
Anti-ERK1/2 (V114a) Promega Corp, USA 1:5000 (WB 1° Ab)
Anti-p-ERK (E-4) Santa Cruz, USA 1:1000 (WB 1° Ab)
Anti-IκB-α (C-21) Santa Cruz, USA 1:1000 (WB 1° Ab)
Anti-SAPK/JNK (#9252) Cell Signalling, USA 1:1000 (WB 1° Ab)
Anti-phospho-SAPK/JNK
(#9251)
Cell Signalling, USA 1:1000 (WB 1° Ab)
Anti-NFATc1 BD Pharmingen, USA 1:1000 (WB 1° Ab)
Anti-p38 (#9212) Cell Signalling, USA 1:1000 (WB 1° Ab)
Anti-phospho-p38 (#9211) Cell Signalling, USA 1:1000 (WB 1° Ab)
Anti-Svs7 Institute of Medical and
Veterinary Science
(IMVS), South Australia
1:500 (WB 1° Ab)
Anti-mouse IgG
Peroxidase Conjugate
(A9917)
Sigma-Aldrich, USA 1:5000 (WB 2° Ab)
Anti-rabbit IgG Peroxidase
Conjugate (A0545)
Sigma-Aldrich, USA 1:5000 (WB 2° Ab)
PE Cy.7-conjugated anti-
CD3e
BD Pharmingen, USA 1:1000 (Flow cytometry)
FITC-conjugated CD45R BD Pharmingen, USA 1:1000 (Flow cytometry)
V450-conjugated CD11b BD Pharmingen, USA 1:1000 (Flow cytometry)
PE-conjugated cKit BD Pharmingen, USA 1:1000 (Flow cytometry)
APC-conjugated Sca-1 R&D systems, USA 1:20 (Flow cytometry)
4.1.8 Vectors
Description Supplier
pcDNA3.1/V5-His Invitrogen, Australia
pGEM-T Easy Vector Promega Corp, USA

Chapter Four – Materials and Methods
69
pNFAT-Luc2P (Luc2P/NFAT-
RE/Hygro)
Promega Corp, USA
4.1.9 Purchased kits and systems
Description Supplier
Alkaline phosphatase (ALP) staining kit Sigma-Aldrich, USA
CellTiter 96 Aqueous One Solution Cell
Proliferation Assay (MTS)
Promega Corp, USA
Fluo-4 AM calcium molecular probe
(F14201)
Invitrogen, Australia
Lipofectamine-2000 Transfection
Reagent
Invitrogen, Australia
Live/Dead Fixable Aqua Dead cell stain Invitrogen, Australia
Luciferase assay system (Substrate) Promega Corp, USA
QIAEXII Gel Extraction Kit (500) QIAGEN, Australia
Qiagen Plasmid plus midi kit QIAGEN, Australia
QIAprep spin miniprep QIAGEN, Australia
RNeasy RNA Extraction Kit QIAGEN, Australia
Western Lightening Ultra (Detection kit-
chemiluminescence substrate)
Perkin Elmer, USA
4.1.10 Oligonucleotide primers
Oligonucleotide primers for use in PCR reaction were purchased from GeneWorks,
Australia. Upon receipt, the oligos were resuspended in the recommended amount of
double-distilled water (ddH2O) to make up 100mM stock concentration. An aliquot of
20μl of each stock primer was transferred to a new 0.5ml tube and was diluted with
80μl of ddH2O (1 in 5 dilution) to make a working concentration of 20mM. Both stock
and aliquot primers were stored at -20°C until use.
4.1.11 Other materials
Description Supplier
100bp DNA ladder (250μl) Promega Corp, USA
1kb DNA ladder (250μl) Promega Corp, USA
6xDNA Blue/Orange Loading Dye Promega Corp, USA

Chapter Four – Materials and Methods
70
Baxter ddH2O Baxter, Australia
Biocoat collagen 1-coated 6-well plate Becton Dickinson, UK
Carbon steel surgical blade sterile Swann Morton, UK
Cell Culture Flask – T25, 75 Nunc, Denmark
Cell Culture Plates: 6-, 12-, 24-, 48-, and
96-wells
Nunc, Denmark
Cell Dissociation Solution (1x Non-
enzymatic)
Sigma-Aldrich, USA
Cell Scraper Sarstedt, Germany
Cell Strainer 100μm BD Biosciences, USA
Centrifuge Tubes – 5, 15 and 15ml Sarstedt, Germany
Corning Osteo Assay Plates Corning, USA
Cryogenic Vials (2ml) Simport, USA
DAKO aqueous mounting media Invitrogen, Australia
DePeX mounting media BDH Laboratory, UK
Double-sided carbon tape (12mm wide) ProSciTech, Australia
Filter paper Whatmans, GE Healthcare, USA
HybondTM C Nitrocellulose Membrane Amersham Biosciences, USA
Microcentrifuge tubes – 0.5, 1.5, and 2ml Sarstedt, Germany
Neubauer Haemocytometer Optik Labor, USA
Optical Bottom Plate Polymer (black
base)
Nunc, Denmark
Parafilm American National, USA
PCR tubes – 0.2ml Sarstedt, Germany
Petri dishes (90mm) Nunc, Denmark
Pin Type SEM mount (12.6mm diameter) ProSciTech, Australia
Pipette tips Sarstedt, Germany
Precision Plus Protein Standard Bio-Rad Laboratories, USA
Protein Assay Dye Reagent concentrate Bio-Rad Laboratories, USA
SEM paper storage box ProSciTech, Australia
Serological Pipettes – 5 and 10ml Sarstedt, Germany
SYBR safe DNA stain Invitrogen, Australia
Needle 23Gx1.25 (0.65x32mm) BD Biosciences, USA
Syringe 5cc/ml BD Biosciences, USA

Chapter Four – Materials and Methods
71
Transfer pipette – 1ml Sarstedt, Germany
MicroAmp optical adhesive film A&B Applied Biosystems, USA
4.1.12 Software
Description Supplier
CT analyser Version 1.10.1.0 Skyscan, Belgium
Dataviewer Version 1.4.3.0 Skyscan, Belgium
FlowJo Tree Star, USA
ImageJ 1.45s Wayne Rasband, NIH, USA
Microsoft Excel 2011 Microsoft Corp, USA
Microsoft Word 2011 Microsoft Corp, USA
NIS-Elements Basic Research Nikon, USA
NRecon Version 1.5.1.4 Skyscan, Belgium
ScanScope Aperio, USA
4.1.13 Equipment
Description Supplier
A&D HT-500 balance A&D Corp, Korea
Agarose Gel Comb Bio-Rad Laboratories, USA
Beckman J-6B centrifuge Beckman Instruments, USA
BH120 Gelman Sciences cell culture
hood
Gelman, Singapore
Binder 37°C incubator (not for cell
culture)
VWR international, Australia
Bio-Rad Gel Tray Bio-Rad Laboratories, USA
Bio-Rad power pack HC for Western
Blot
Bio-Rad Laboratories, USA
Bio-Rad Spectrophotometer Plus Bio-Rad Laboratories, USA
Canon Camera Canon, Japan
Class II biological safety cabinet Gelaire, Australia
Clemco fume hood Oliphant Pty Ltd, Australia
Clifton Cerastir (magnetic stirrer) Lomb Scientific, Australia
Diamond wafering blade Buehler, USA
Eppendorf Biophotometer plus Eppendorf, Germany

Chapter Four – Materials and Methods
72
Eppendorf 5430R centrifuge (including
for 4°C centrifugation)
Eppendorf, Germany
Eppendorf 5810R centrifuge (for cell
culture)
Eppendorf, Germany
Eppendorf MiniSpin Plus
Microcentrifuge
Eppendorf, Germany
Eppendorf Pipettes: 0.2-2μl, 2-20μl, 20-
200μl, 200-1000μl, multichannel
Eppendorf, Germany
Eppendorf Thermocycler Eppendorf, Germany
FACS Canto BD Pharmingen, USA
Forma Steri-cycle CO2 incubator Thermo Fisher Scientific, USA
FujiFilm ImageQuant LAS-3000 FujiFilm, Japan
FujiFilm ImageQuant LAS-4000 FujiFilm, Japan
Gelman Biological Safety Cabinet Class II Gelman, Singapore
Grant W14 water bath Selby Scientific and Medical, USA
Invitrogen Safe Imager 2.0 Invitrogen, Australia
Isomet low speed saw Buehler, USA
LabServ Incubator Biolab, Australia
Liquid nitrogen bucket Nulgene, USA
MaxQ4450 shaking incubator Thermo Fisher Scientific, USA
MilliQ Advantage A10 Millipore, USA
Mini-PROTEAN III Cell Electrophoresis Bio-Rad Laboratories, USA
Mini Trans-Blot Electrophoretic Transfer
Cell
Bio-Rad Laboratories, USA
Model 680 Microplate Reader Bio-Rad Laboratories, USA
Nikon Eclipse 50i Nikon, Japan
Nikon Eclipse Ti Nikon, Japan
PV-1 benchtop vortex Grant-bio Quantum Scientific, USA
Ratek Orbital Mixer Incubator Ratek Instruments, Australia
Ratek Rocking Platform Mixer Ratek Instruments, Australia
Skyscan 1072 microCT scanner Skyscan, Belgium
Skyscan 1174 microCT scanner Skyscan, Belgium
Tomy MicroOne mini centrifuge Tomy Tech, USA
TPS digital pH meter TPS, Australia

Chapter Four – Materials and Methods
73
UV Bench-top Transilluminator UVP, USA
4.1.14 Centrifugation
Centrifugation of 0.2ml PCR tubes at room temperature was performed using Tomy
MicroOne mini centrifuge. Other microcentrifuge tubes (0.5, 1.5, and 2ml) were
centrifuged using Eppendorf MiniSpin Plus Microcentrifuge. Centrifugation at 4°C was
carried out using Eppendorf 5430R centrifuge.
4.2 Buffers and Solutions All solutions were prepared using highly purified ddH2O and where applicable, were
sterilized either by autoclaving or filter sterilization. All chemicals were weighed using
A&D HT-500 balance (A&D Corp). The adjustment of pH was carried out using TPS
digital pH meter, calibrated with appropriate pH standards.
4.2.1 General solutions
Solutions Composition and Preparation
10% Ammonium persulphate 10% (w/v) ammonium persulphate
dissolved in ddH2O. Stored at 4°C.
Ampicilin 100mg/ml stock, dissolved in ddH2O, and
aliquoted to 1ml. Stored at -20°C.
0.2% BSA/PBS 0.2% (w/v) BSA dissolved in 1xPBS.
Stored at 4°C.
dNTPs 100mM stock solution for each dNTP
(dCTP, dATP, dTTP, dGTP). 25% (v/v)
of each constituent was mixed together to
yield a 25mM combined stock of dNTPs,
which was then diluted to 5mM with
ddH2O and stored as 200μl aliquots at -
20°C.
14% EDTA pH 7.4 14% (w/v) EDTA dissolved in ddH2O,
brought to pH 7.4 with NaOH.
Autoclaved and stored at room
temperature.
Eosin (containing phloxine) Stock solution: 1% (w/v) of eosin Y

Chapter Four – Materials and Methods
74
dissolved in ddH2O.
Phloxine stock solution: 1% (w/v)
phloxine B dissolved in ddH2O.
Working stock staining (per litre)
composed of 100ml of Eosin stock
solution, 10ml of phloxine stock solution,
780ml 95% ethanol and 4ml glacial acetic
acid.
Flow Cytometry Wash Buffer 50ml stock solution in 1xPBS; composed
of 1% FBS (500μl) and 0.1% (w/v)
sodium azide (0.05g). Stored at 4°C.
Fluo4-AM 1mM concentration made by dissolving
50μg of the dye in 45.58μl of 20%
pluronic acid.
Fluo4-AM/Hanks solution 4μl of Fluo4-AM/ml of
Hanks/probenecid required to make 4μM
concentration.
Haematoxylin (Gill’s) 1L stock solution made: 250ml of
ethylene glycol dissolved in 750ml of
ddH2O, added 6g of haematoxylin, 0.6g
of sodium iodate, 80g of aluminium
sulphate and 20ml of glacial acetic acid
to the mixture and stirred for an hour at
room temperature. Working
concentration of 1 in 5 of stock solution
used. Filtered and stored at room
temperature.
Hanks/Probenecid buffer Prepared 2mM probenecid in Hanks
buffer.
IPTG/X-gal 0.2M IPTG, 0.1M X-gal in
dimethylformamide. Stored at -20°C in
the dark.
Luciferase Lysis Buffer 500ml stock made: 1.51g of Tris-HCl
(pH 7.8), 0.37g of EDTA, 50ml of

Chapter Four – Materials and Methods
75
glycerol, and 5ml of Triton X-100
dissolved in ddH2O. Stored at 4°C.
10% Neutral Buffered Formalin (NBF) A mixture of 10% (v/v) formaldehyde
(100ml), 900 ml of ddH2O, 33mM
NaH2PO4 (4g), and 45mM Na2HPO4
(6.5g). Autoclaved and stored at room
temperature
4% Paraformaldehyde (PFA) 4% (w/v) in 1xPBS. Stored as 10ml
aliquots at -20°C.
1xPBS pH 7.4 100ml stock solution mixed with 900ml
of ddH2O to give 1x concentration, filter
sterilised and stored at room temperature.
PMSF 17.6mg/ml stock was prepared in
isopropanol. Stored as 1ml aliquots at -
20°C.
Pluronic acid (20%) Dissolving 0.2g of the pluronic in 1ml of
DMSO.
Red Blood Cell Lysis Buffer (Flow
cytometry)
500ml stock solution: 4.15g of
ammonium chloride (NH4Cl), 0.788g
Tris-HCl, 0.9ml 5% EDTA pH 8, mixed
with 450ml of ddH2O, pH adjusted to 7.4,
and the final volume was adjusted to
500ml with ddH2O. Filter sterilized and
stored at 4°C.
RipaRipa Lysis Buffer A mixture of 50mM Tris-HCl pH 7.5
(25ml), 150mM NaCl (15ml), 1%
Nonidet P (NP)-40 (5ml), 0.5% sodium
deoxycholate (2.5g), 0.1% SDS (0.5g),
adjusted to 500ml with ddH2O.
Autoclaved and stored at 4°C.
At the time of cell lysis: 100μg/ml of
PMSF, 1x cocktail protease inhibitor,
1mM Sodium orthovanadate, and
500μg/ml of DNaseI is freshly added to

Chapter Four – Materials and Methods
76
the required amount of the lysis buffer
10% SDS 10% (w/v) SDS dissolved in ddH2O.
Stored at room temperature.
4x SDS-PAGE Loading Buffer 4x stock solution composed of 240mM
Tris-HCl (2.4ml), pH adjusted to 6.8, 8%
(w/v) SDS (0.8g), 40% glycerol (4ml),
0.04% bromophenol blue (4mg), and 5%
β-mercaptoethanol (0.5ml), adjusted to
10ml with ddH2O. Stored at 4°C.
10x SDS-PAGE Running Buffer 10x stock solution; a mixture of 25mM
Trizma base (30.28g), 1.92M Glycine
(144.13g), and 1% (v/v) of 10% SDS
(100ml), adjusted to 1L with ddH2O.
Stored at room temperature.
SDS-PAGE Separating Gel Buffer A mixture of 1.5M Trizma base, 0.4%
SDS, prepared in ddH2O. pH adjusted to
8.8 (before addition of SDS). Stored at
room temperature.
SDS-PAGE Stacking Gel Buffer A mixture of 1M Trizma base, 0.4%
SDS, prepared in ddH2O. pH adjusted to
6.8 (before addition of SDS). Stored at
room temperature.
Solution A (Goldner’s trichrome stain) Prepared by mixing 0.075g of Ponceau
2R, 0.025g of acid fuchsin, 0.01g of
azophloxine, and 0.2ml of acetic acid
with 100ml of ddH2O.
Solution B (Goldner’s trichrome stain) Prepared by mixing 2g of orange G and
4g of phosphomolybdic acid with 100ml
of ddH2O. The solution was left to stand
at room temperature for a couple of days
for any precipitate to settle out and then
filtered before use.
Solution C (Goldner’s trichrome stain) Prepared by mixing 0.2g of light green
and 0.2ml of acetic acid with 100ml of

Chapter Four – Materials and Methods
77
ddH2O.
50x Tris-acetate EDTA (TAE) 50x stock solution made of 2M Trizma
base (242g), 5.71% (v/v) glacial acetic
acid (57.1ml), and 500mM EDTA
(100ml), adjusted to 1L with ddH2O.
Stored at room temperature. (1x TAE was
used by doing dilution of 50x stock
solution)
10x TBS 10x stock solution made of 0.5M Trizma
base (60.57g), 1.5M NaCl (87.66g)
dissolved in ddH2O, and pH adjusted to
7.4 with concentrated HCl and volume
adjusted to 1L. Stored at room
temperature.
1x TBS/Tween 1xTBS with additional of 0.1% (v/v)
Tween-20. Stored at room temperature.
TRAP Stain Solution A A mixture of 100mM sodium acetate
trihydrate (6.8g), 50mM sodium tartrate
dihydrate (5.8g), 0.22% glacial acetic
acid (1.1ml), pH adjusted to 5, and
volume adjusted to 500ml with ddH2O.
TRAP Stain (Complete) 5mg of AS-MX dissolved in 250μl of 2-
Ethoxyethanol (EGME) and 30mg of Fast
Red-Violet-LB salt dissolved in 50ml of
TRAP stain solution A. Stored as 10ml
aliquots at -20°C. Filtered before use.
0.1% Triton X-100/PBS 0.1% (v/v) stock solution (50μl of 100%
Triton X-100) in 50ml 1xPBS. Filter
sterilized and stored at 4°C.
Weigert’s iron haematoxylin Solution A prepared by mixing 1g of
haematoxylin (CI75290) with 100ml of
96% ethanol; Solution B prepared by
mixing 4ml of 30% Iron chloride, 1ml of
37% HCl with 100ml of ddH2O. Equal

Chapter Four – Materials and Methods
78
part of solution A and B were mixed to
make a working solution.
Western Blot Stripping Buffer A mixture of 62.5mM Tris-HCl (3.79g),
2% SDS (10g), pH adjusted to 6.7, and
then 100mM β-mercaptoethanol (3.5ml)
was then added. Volume adjusted to
500ml with ddH2O. Autoclaved and
stored at room temperature.
Western Blot Transfer Buffer A mixture of 25mM Trizma base (6.06g),
192mM glycine (28.8g), and 10%
methanol (200ml). Volume adjusted to
2L with ddH2O and stored at room
temperature.
4.2.2 Media and agar
Media and agar Composition and preparation
Luria Bertoni (LB) Broth A mixture of 10g/L Bacto-Tryptone, 5g/L
yeast extract, and 5g/L NaCl, dissolved in
ddH2O. Autoclaved and stored at room
temperature.
LB/Ampicillin (Amp) After autoclaving, LB was cooled at
room temperature until the temperature
drop to <70°C and then supplemented
with 1ml (100μg/ml) ampicillin.
LB/Amp Agar Plates Stock LB plus 15g/L agar. Autoclaved,
cooled at room temperature to <70°C,
supplemented with 1ml (100μg/ml)
ampicillin, and poured into petri dishes.
Stored at 4°C until use.
LB/Amp/IPTG/X-gal Agar Plates IPTG (0.012%) and X-gal (40μg/ml)
were spread onto LB/Amp plates and
allowed to dry prior to use.

Chapter Four – Materials and Methods
79
4.3 Animals 4.3.1 Svs7 transgenic (TG) mice generation
Svs7 gene was cloned into pcDNA3.1 V5-His (described in more details in cloning
method Section 4.6). After SfuI restriction enzyme digestion (as depicted in Figure 4.1),
the linearized DNA fragment, containing CMV promoter region, Svs7 coding sequence,
and BGH polyadenylation signal, was purified and used in blastocysts microinjection to
create TG mice.
SfuI SfuI
CMV promoter
Svs7 coding sequence V5 6xHis BGH polyadenylation signal
654bp 500bp 442bp
3,597bp 811bp
Svs7 transgene (6,000bp) Figure 4.1 Svs7 TG mice generation
4.3.2 Svs7 knockout (KO) mice generation
Briefly, a targeting vector and Cre-LoxP system (in SpeI and KpnI sites) were used to
excise exon 2 and 3 of Svs7 gene with PGK Neo cassette in 129/Sv embryonic stem
cells (ES) (Hayman et al. 1996; Mansour, Thomas & Capecchi 1988) (Figure 4.2). The
Svs7 KO ES cells were then injected into C57BL/6 blastocysts, which were then
transferred to the uterus of a recipient mouse (acting as a surrogate mother). The male
chimeras were then mated with female C57BL/6 mice and the resulted heterozygous
were then inter-crossed to yield Svs7 KO homozygous mice.
4.3.3 Mouse tail tip DNA genotyping
Mouse tail tip DNA genotyping was performed according to Jackson laboratory’s DNA
isolation protocol. Briefly, each mouse tail tip was transferred to a sterile PCR tube,
followed by the addition of 75μl of 25mM NaOH/0.2mM EDTA. The sample was then
placed in Eppendorf thermocycler at 98°C for an hour incubation, which was
subsequently followed by 15°C incubation until ready for the next step. Each sample
was then mixed with 75μl of 40mM Tris-HCl (pH 5.5) and centrifuged at 4,000rpm for
3 minutes at room temperature. Two μl of each DNA sample (supernatant) was then
used as a template in PCR DNA amplification and the rest of the samples were stored at
-20°C.

Chapter Four – Materials and Methods
80
Figure 4.2 Svs7 KO mice generation
PCR reaction was carried out with three primers detailed below.
Primers Sequence (5’-3’)
769 WT Rev GAC ATG TAG GTT AGA TCT GGG T
769 3’ GTG TGT CTG AGT ACA CTC TTG
GAT G
769 M 5’ TGG ATG CAA GTC AAG ACC TCC
TGT G
Svs7 transgene forward ATGATTCAGTGACGAAAT
Svs7 transgene reverse GAAGCTATTACACAAGTTTT
Each PCR genotyping reaction tube contained 12.5μl of 2xGoTaq DNA polymerase
Green Reaction Mix, 0.5μl of each primer, 9μl of ddH2O, and 2μl of tail tip DNA
sample to yield a final reaction volume of 25μl. The reaction tubes were mixed by
centrifugation using Tomy MicroOne centrifuge and then placed in the Eppendorf

Chapter Four – Materials and Methods
81
thermocycler for initial denaturation at 95°C for 5 minutes, followed by 35 cycles of
95°C for a minute, 58°C for 40 seconds, and 72°C for a minute. The DNA amplification
ended with the extension period at 72°C for 5 minutes.
4.3.4 ΜicroCT analysis
MicroCT analysis was carried out using Skyscan 1174 microCT scanner (Skyscan,
Belgium) by Dr Tamara Davey. Tibia, femur, and lumbar bones were imaged using an
X-ray tube with settings: 50kV, 800μA, with a 0.5mm aluminium filter, and 4000ms
exposure time. The scanning angular rotation was 180° and the angular increment step
was 0.4°. The images were reconstructed using NRecon skyscan software (settings:
level 2 smoothing, 32% beam hardening, and 12 rings artefact) and trabecular bone
distal to the proximal growth plate was selected for analysis. A region of 0.3mm from
the growth plate and 1mm in height was analysed. The parameters included trabecular
bone volume (bone volume over tissue volume (BV/TV)), trabecular number (Tb.N),
trabecular separation (Tb.Sp), and trabecular thickness (Tb.Th).
4.3.5 Histology on hindlimbs and prostate of Svs7 TG and KO mice
4.3.5.1 Fixation, decalcification (for hindlimbs), tissue processing, tissue embedding,
and sectioning
Hindlimbs from WT and Svs7 KO mice were dissected out and fixed in 10% NBF for
24 hours. The bones were then washed twice with 1xPBS and were kept in PBS
overnight to completely wash off the fixation solution. The bones were then transferred
into 70% ethanol and stored at 4°C until ready for decalcification and tissue processing.
Prior to decalcification, all non-bone tissues were removed and tibia and femur were
separated gently. The bones were washed once with PBS and then kept wet in PBS
overnight. The decalcification process began by resuspending the bones in excess of
14% EDTA (pH 7.4) and placed them in 37°C incubator for 5 days (with fresh EDTA
media change every day). When the bones became soft and flexible, they were ready for
tissue processing using the Leica TP1020 tissue processor (as shown in table 4.1
below). Before the tissue processing step, the bones were washed with PBS then 70%
ethanol.
Table 4.1 Tissue processing (Dehydration)
Station Reagent Time (minutes)
1 70% Ethanol 30
2 95% Ethanol 30

Chapter Four – Materials and Methods
82
3 95% Ethanol 45
4 100% Ethanol 60
5 100% Ethanol 60
6 100% Ethanol 60
7 Ethanol/Xylene 60
8 Xylene 90
9 Xylene 120
10 Paraffin wax 90
11 Paraffin wax 120
12 Paraffin wax 120
The processed bones were then paraffin-embedded and cut into 5μm thick sections,
performed by Mr Jacob Kenny from The School of Pathology and Laboratory
Medicine. Sections were adhered to microscopy glass slides and dried overnight at
37°C.
4.3.5.2 Dewaxing and H&E staining
Sections were dewaxed by bringing them into 3 changes of fresh xylene for 2 minutes
each. Sections were then rehydrated in 3 changes of 100% ethanol for a minute each,
followed by 95% and 70% ethanol also for a minute each. Sections were then washed in
running deionised ddH2O for about a minute. Sections were then removed from ddH2O
and immersed in Gill’s haematoxylin stain for 3 minutes. Excess stain was washed off
by rinsing the sections in ddH2O, followed by a minute wash in Scott’s tap water to
balance pH. The sections were then briefly washed in running deionised ddH2O before
bringing them into 2 changes of ethanol (in the order of 70% then 95% ethanol) for a
minute each. One % eosin staining was used to counterstain the section for a minute,
followed by dehydration in 3 changes of 100% ethanol for a minute each. Sections were
then immersed in 50% ethanol/50% xylene for 2 minutes first before going through 3
changes of xylene for 2 minutes each. Sections were mounted with DPX mounting
medium. The images were then taken using 4x objective magnification of Nikon Eclipse
Ti microscope.
4.3.5.3 Dewaxing and TRAP staining
Sections were dewaxed and rehydrated as described above. After washing in ddH2O,
excess liquid was removed from the sections (without causing drying to the section) and

Chapter Four – Materials and Methods
83
filtered TRAP stain was then added drop wise to the sections. The staining process was
then carried out at 37°C incubation in the dark for about 1-2 hours. After TRAP stain
was fully developed, the sections were rinsed in ddH2O before counterstaining them
with Gill’s haematoxylin for about 10 seconds. The sections were then rinsed in ddH2O
for a minute to remove excess of the counterstain, followed by a minute wash in Scott’s
tap water to balance pH. When the counterstain colour was too strong, 1% acid alcohol
(for 3 seconds on the sections) was used to wash off some of the counterstain, which
was then further adjusted by bringing them again into the Scott’s tap water for about 30
seconds. The sections were then briefly washed in running deionised ddH2O before
bringing them into 2 changes of ethanol (in the order of 70% then 95% ethanol) for a
minute each. After a brief wash in running deionised ddH2O, the TRAP-stained sections
were now ready to be mounted in DAKO aqueous mounting medium and DPX for long-
term storage. The images were then taken using 10x objective magnification of Nikon
Eclipse Ti microscope.
4.3.5.4 Processing, embedding, and sectioning of non-decalcified bone samples
After the process of extraction, fixation, and PBS wash of hindlimbs (as described in
Section 4.3.4.1) of WT and Svs7 TG mice, the undecalcified samples were then ready
for tissue processing using the Leica TP1020 tissue processor (as shown in table 4.2
below).
Table 4.2 Undecalcified tissue processing (Dehydration)
Station Reagent Time (minutes)
1 50% Ethanol 120
2 70% Ethanol 120
3 80% Ethanol 120
4 96% Ethanol 120
5 100% Ethanol 180
6 100% Ethanol 180
7 Xylene 60
8 Xylene 720
The samples were then washed twice and immersed in the infiltration reagent (89g of
methylmethacrylate (MMA), 10g of plasticiser, 1g of perkadox 16, and 0.01g of
tinogard tt (scavenger)) for 3-4 days at 4°C in vacuum conditions. Finally, the samples
were embedded in the infiltration reagent and immersed in 29°C water bath for 3 days

Chapter Four – Materials and Methods
84
to complete the polymerization process. Samples were then sectioned at the thickness of
5μm using the Leica RM2255 Automated Microtome. The processing, embedding, and
sectioning of undecalcified femur samples of Svs7 TG mice was performed by Miss
Euphemie Landao (Centre for Orthopaedic research, School of Surgery, UWA).
4.3.5.5 Goldner trichrome staining for the undecalcified bone samples
Prior to staining, the MMA resin was removed from the sections by incubating the
samples in 3 changes of methoxyethyl acetate (MEA) solution for 20 minutes each,
followed by 2 changes of xylene for 10 minutes each. The samples were then ready for
rehydration process by rinsing them briefly (about 10 to 15 seconds for each change) in
a decreasing row of ethanol (2 changes of 100%, 96%, 80%, 70%, and finally in 50%
ethanol). To complete the rehydration process, the samples were then rinsed briefly in 2
changes of ddH2O. The sections were then stained for nuclei using Weigert’s iron
haematoxylin for 20 minutes, followed by washing in ddH2O for a minute. The staining
was differentiated in acid alcohol for no more than 5 seconds, which was followed by
gentle wash in ddH2O. The sections were then incubated in solution A stain for 5
minutes and rinsed with 1% aqueous acetic acid after. The sections were treated with
solution B for approximately 3 minutes until collagen is decolourized, followed by a
brief rinse in 1% aqueous acetic acid. The sections were then finally stained in solution
C for 5 minutes and treated with 1% aqueous acetic acid for 5 minutes. The stained
sections were then dehydrated by a brief rinse in 100% ethanol and were cleared and
mounted. The mineralised bone is stained green, orange/red colour for osteoid,
blue/grey for nuclei, and purple for cartilage. The images were then taken using 10x
objective magnification of Nikon Eclipse Ti microscope.
4.3.6 Double calcein labelling of Svs7 KO mice
To analyse bone formation activity in vivo, 3 pairs of 3 month-old WT and Svs7 KO
mice were injected with calcium-binding fluorochrome dye, calcein, intraperitoneally,
twice (double labelling) seven days apart. The mice were sacrificed 2 days after the
second injection. The hindlimbs were extracted from mice and fixed in 10% NBF
followed by plastic embedding. The processing and sectioning of the plastic-embedded
tissues was carried out by our collaborator, Dr Jerry Feng, in China. Briefly, the
samples were first dehydrated at room temperature in gradual increase of ethanol
content; 50%, 70%, 80%, 96%, and lastly 2 changes of 100% ethanol for 5 hours each
step. Two changes of xylene, for 5 and 25 hours respectively, at room temperature were

Chapter Four – Materials and Methods
85
then used to finalise the dehydration process. The samples were then immersed in
infiltration reagent (89g of methylmethacrylate, 10g of plasticiser, 1g of perkadox 16,
and 0.01g of Tinogard® TT (scavenger)) for 3-4 days. Finally, the samples were
embedded in the infiltration reagent and immersed in 29°C water bath to complete the
polymerization process. Sections were then cut at the thickness of 5μm. The image of
double calcein labelling was taken using confocal microscopy and the distance between
2 labels was measured at 3 points along cortical bone using ImageJ software, which was
also performed by Dr Jerry Feng.
4.4 General Methods 4.4.1 Isolation and culture of primary cells
4.4.1.1 Isolation and culture of bone marrow cells
Bone marrow cells were extracted from tibia, femur, and humerus of WT and Svs7 KO
mice. First, the long bones were dissected out from the mice and placed in the 5ml tube
containing complete α-MEM medium (α-MEM medium supplemented with 10% FBS,
100U/ml Penicillin, and 100μg/ml Streptomycin). After all the samples have been
collected on the sterile bench, the isolation of bone marrow cells was achieved by
flushing the bone marrow cavity with the complete α-MEM medium using a 23G
needle. Bone marrow cells, which was suspended in α-MEM medium, was filtered
through a 100μm cell strainer on top of the 50ml tube. The bone marrow cell suspension
was then centrifuged at 1,500rpm for 5 minutes to pellet the cells. The cell pellet was
then resuspended in fresh complete α-MEM medium.
For osteoclast culture, bone marrow macrophages/monocytes (BMM) were resuspended
in complete α-MEM supplemented with 10ng/ml M-CSF in a T75 flask until reaching
confluency. The cells were then trypsinised (using 1xtrypsin for 15-20 minutes
incubation at 37°C 5% CO2 incubator), seeded at the required cell density into culture
plates (shown in table below), and cultured in the same medium as above with
additional stimulation of 100ng/ml RANKL. Culture medium was fully changed every
two days.
Cell culture plate for osteoclast culture Cell density
6-well (RNA and protein extraction, cell
transfection)
5x104 cells/2ml/well
48-well (Fluo4-AM calcium assay) 1.6x104 cells/500μl/well
96-well (Time-course RANKL-induced 6x103 cells/100μl/well

Chapter Four – Materials and Methods
86
osteoclastogenesis)
For osteoblast culture, bone marrow cells were counted and seeded directly into culture
plates and cultured in complete α-MEM medium. When they reached confluence, the
culture medium was then supplemented with osteoblast differentiation/mineralization
factors (10nM dexamethasone, 2mM β-glycerophosphate, and 50μg/ml ascorbate). Full
medium change was carried out every 3-4 days.
Cell culture plate for osteoblast culture Cell density
24-well 1x106 cells/ml/well
4.4.1.2 Isolation and culture of spleen cells
Spleen was dissected out from WT and Svs7 KO mice and placed into a 5 ml tube
containing complete α-MEM medium. Using the back of syringe, spleen was then
crushed against a cell strainer, which was on top of a 50ml tube, to release the cells.
Complete α-MEM medium was then pipetted into the cell strainer to wash the cells
through. The cell suspension was then centrifuged at 1,500rpm for 5 minutes to pellet
the cells. The cell pellet was then resuspended in complete α-MEM medium
supplemented with 10ng/ml M-CSF and transferred to a T75 culture flask until reaching
confluency and used for experimental purposes. All cell cultures were grown and
maintained in a 37°C cell culture incubator with 5% CO2.
4.4.1.3 Isolation and culture of calvarial osteoblasts
Calvariae from WT and Svs7 KO neonatal mice were dissected out from the head. After
the removal of skin and duramater, calvariae were subjected to four sequential 15
minutes digestions in an enzyme mixture containing 0.05% trypsin and 1.5U/ml
collagenase at 37°C incubation. Cell fractions of 2 to 4 were pooled and enzyme
activity was stopped by the addition of DMEM complete medium. The calvarial
osteoblasts were then plated at a density of 1x104 cells/ml/well in a 12-well plate for
MTS proliferation assay.
4.4.2 Cell culture of COS-7 cell line
The monkey kidney fibroblast-like cell line, COS-7 cells, were cultured in complete
DMEM-Glutamax-1 medium in a 37°C 5% CO2 cell incubator. Culture medium was
fully replenished every two days and cells were passaged upon reaching confluence.

Chapter Four – Materials and Methods
87
4.4.3 Cryopreservation of cell lines for long-term storage
When the cells were not needed for a while and they had reached confluence,
cryopreservation procedure of the cells was conducted. After culture medium had been
discarded, the cells in T75 flask were washed once with sterile 1xPBS and trypsinised
(for COS-7 cells to detach usually takes 3-5 minutes incubation at 37°C 5% CO2
incubator). To deactivate trypsin, about 5ml of fresh complete culture medium was
added to the flask and the cells in suspension was transferred to a sterile 50ml tube. To
pellet the cells, the tube was centrifuged at 1,500rpm for 5 minutes at room temperature.
Supernatant was then removed and the cells were resuspended in 92% FBS and 8%
DMSO and aliquoted into 1ml per sterile cryovial. Cryovials were then stored at -80°C
in ethanol/isopropanol-equilibrated Mr. Frosty freezing container. Cryovials can later be
stored in liquid nitrogen tank to virtually stop all biological activity of the cells and
hence for long-term storage.
4.4.4 RNA extraction
RNA extraction (for osteoclast cells grown in monolayer and for tissues/organs) was
carried out using Trizol RNA isolation protocol. Briefly, culture medium was aspirated
and cells grown in monolayer were washed once with 1xPBS. Cells were then lysed by
directly adding 1ml of trizol reagent/3.5cm diameter dish into the cultured plates,
followed by scraping the cells with the pipette tip. The sample suspension in trizol was
then pipetted up and down to completely homogenize the sample. The complete
homogenized sample was then transferred to a 1.5 ml tube and incubated for 5 minutes
at room temperature to allow complete dissociation of nucleoprotein complexes. The
sample was then centrifuged at 12,000rpm 4°C for 10 minutes to pellet cell debris. The
supernatant was then transferred to a new 1.5ml tube, followed by the additional of
0.2ml of chloroform/1ml of trizol reagent used. The sample was vigorously shaken for
15 seconds and then vortexed for another 15 seconds. The sample was incubated at
room temperature for 2-3 minutes and then centrifuged at 12,000rpm 4°C for 15
minutes to allow RNA release into a colourless upper aqueous phase. The aqueous RNA
was then transferred to a new 1.5ml tube and precipitated by mixing it with 0.5ml of
isopropyl alcohol/1ml of trizol reagent used. The sample was incubated at room
temperature for 10 minutes and centrifuged at 12,000rpm 4°C for 10 minutes to pellet
RNA. The supernatant was then completely discarded and the RNA pellet was washed
with 1ml of 75% ethanol/1ml of trizol reagent used, vortexed, and centrifuged at
7,500rpm 4°C for 5 minutes. The leftover ethanol was then removed and the washing

Chapter Four – Materials and Methods
88
procedure was repeated once more. The RNA pellet was air-dried for 10 minutes at
room temperature and 30μl of nuclease-free water was then added to the tube to
dissolve and resuspend the RNA pellet. RNA samples were then stored at -80°C until
required for reverse transcription (RT) reactions.
For the isolation and RNA extraction from tissues/organs, a pair of WT and Svs7 KO
mice was sacrificed and organs, such as bone, seminal vesicle, brain, heart, thymus,
lung, liver, spleen, stomach, kidney, intestine, skin, fat, and ovary, were extracted and
each of them was then placed in an individual sterile mortar. One full scoop of liquid
nitrogen was then added to the mortar and the frozen organ was subsequently crushed
by grinding it using a pestle. After uniform powder-form of the organ was observed in
the mortar, 1ml trizol solution was then added and the grinding procedure continued to
get a homogenous trizol mixture. The sample (in trizol) was then ready to be processed
as described above.
4.4.5 RNA concentration measurement
RNA concentration was measured before RT reaction was carried out. Eppendorf
Biophotometer Plus was used to measure RNA concentration. RNA samples were taken
out from -80°C storage and put on ice. Firstly, the spectrophotometer was blanked using
1μl of nuclease-free water, followed by 1μl of each RNA sample in concentration unit
of ng/μl. After measurement, the samples were returned to -80°C storage until ready for
RT reactions.
4.4.6 RT reactions
RT reaction was carried out using Promega enzymes. Each RNA concentration was
standardised to 1μg and hence the required volume for each RNA was adjusted to 2μl
with nuclease-free water. For the first reaction, each PCR tube contained 2μl of dNTP
mix (5mM), 0.25μl of Oligo(dT) first strand primer (100μM), 10.75μl of nuclease-free
water, and 2μl of RNA sample (1μg) for a total reaction volume of 15μl. The samples
were then mixed by a short spin (5 seconds) using Tomy MicroOne centrifuge and then
heated in Eppendorf thermocycler at 75°C for 3 minutes to disrupt the formation of
secondary structures. Immediately after, the tubes were centrifuged for another 5
seconds using Tomy MicroOne centrifuge and placed back on ice to prevent the re-
formation of secondary structures. The second reaction was then begun by adding a
reaction mix of 4μl of 5xRT buffer (Promega Corp), 0.5μl of RNase inhibitor (Promega

Chapter Four – Materials and Methods
89
Corp), and 0.5μl of M-MuLV RT (Promega Corp) to each reaction tube to yield the
final reaction volume of 20μl. The samples were then spined briefly for 5 seconds and
then placed in Eppendorf thermocycler for the 42°C incubation for an hour. Finally, the
samples were heated at 92°C for 10 minutes to inactivate the RT. All cDNAs were
stored at -20°C.
4.4.7 Polymerase Chain Reaction (PCR) and quantitative PCR (qPCR)
Briefly, each PCR reaction tube contained 7μl of 2x GoTaq green reaction mix, 0.5μl of
each 20μM primer (forward and reverse), 5μl of nuclease-free water, and 1μl of each
cDNA sample to yield a final reaction volume of 14μl. While for qPCR, 10μl total
reaction composed of 5μl of 2x SYBR green reaction mix (Promega), 0.2μl of a mixture
of 20μM forward and reverse primers (for each gene), 1μl of 1 in 3 diluted cDNA, and
3.8μl of nuclease-free water. Each gene at one time point had triplicate wells to get
average Ct value. After normalization of Ct values of test genes against the house-
keeping gene to get ΔCt, the fold induction of each gene (particularly for time course
RANKL-induced osteoclastogenesis) was calculated using the Livak relative gene
quantification method (as shown in the equation below), where the ΔCt of the test gene
for WT and Svs7 KO mice at each time point was normalized to the ΔCt of the test gene
for WT at day 0 of RANKL stimulation.
= 2-(ΔCt- ΔCt (of WT day 0))
= 2-ΔΔCT
The standard PCR/qPCR cycle was run consisting of initial denaturation at 94°C for 5
minutes, cycled at 94°C for 40 seconds, an annealing temperature (varied depends on
primers), and extension at 72°C for 40 seconds for 30 cycles. The reactions were
subjected to final extension step at 72°C for 7 minutes.
Table 4.3 Osteoclast and osteoblast marker genes primers sequences
Name Primer Sequence PCR Conditions
(Anneling
temperature and
number of cycle)
Size of Amplicon
(bp)
ββ-actin (For)
(House-keeping
gene)
CTG TCG AGT
CGC GTC CAC
CC
60°C 40 seconds,
30 cycles
200
ββ-actin (Rev) CCA CCA TCA

Chapter Four – Materials and Methods
90
(House-keeping
gene)
CAC CCT GGT
GCC
Svs7 (For) GCA GAT GCG
TTG CAA AAC
CTG GTG
60°C 40 seconds,
30 cycles
103
Svs7 (Rev) TCC TTG CAC
TGA GGC GAG
CAC
TRAP (For) CCC AAT GAT
GCA CTT CTG
CCC CAG
60°C 40 seconds,
30 cycles
131
TRAP (Rev) CAG CAC CAC
CCA TGA ATC
CTA CCT G
CTR (For) CAA GTC AGG
AGA GCC AGC
CGC
60°C 40 seconds,
30 cycles
116
CTR (Rev) GGG ATG CCA
ACG GCA GGG
TG
NFATc1 (For) TGA GGC TGG
TCT TCC GAG
TT
60°C 40 seconds,
30 cycles
90
NFATc1 (Rev) CGC TGG GAA
CAC TCG ATA
GG
DCSTAMP (For) CTT GCA ACC
TAT GGG CAA
AG
60°C 40 seconds,
30 cycles
246
DCSTAMP (Rev) TCA ACA GCT
CTG TCG TGA
CC
ATP6v0d2 (For) GTG TCC CAT
TCT TGA GTT
60°C 40 seconds,
30 cycles
110

Chapter Four – Materials and Methods
91
TGA GGC CG
ATP6v0d2 (Rev) CCG CAG GTG
GGG AAG AGG
GT
Runx2 (For) CGC ATT CCT
CAT CCC AGT
AT
60°C 40 seconds,
30 cycles
450
Runx2 (Rev) TGT AGG TAA
AGG TGG CTG
GG
Osterix (For) TTC CCT CAC
TCA TTT CCT
GG
60°C 40 seconds,
30 cycles
351
Osterix (Rev) GTA GGG AGC
TGG GTT AAG
GG
Alkaline
phosphatase /
ALP (For)
AAC TGC TGG
CCC TTG ACC
CCT
60°C 40 seconds,
30 cycles
186
Alkaline
phosphatase /
ALP (Rev)
TCC TGC CTC
CTT CCA CCA
GCA
Osteopontin /
OPN (For)
TCT GAT GAG
ACC GTC ACT
GC
60°C 40 seconds,
30 cycles
349
Osteopontin /
OPN (Rev)
TCT CCT GGC
TCT CTT TGG
AA
Osteocalcin / OCN
(For)
GCG CTC TGT
CTC TCT GAC
CT
60°C 40 seconds,
30 cycles
233
Osteocalcin / OCN
(Rev)
ATA GAT GCG
TTT GTA GGC
GG

Chapter Four – Materials and Methods
92
M-CSF (For) AGC CGA GAT
GTG GTG ACC
AAG CC
60°C 40 seconds,
30 cycles
125
M-CSF (Rev) AAG CCA GCC
AGA GGG GCC
AT
RANKL (For) TCT GTT CCT
GTA CTT TCG
AGC GCA G
60°C 40 seconds,
30 cycles
198
RANKL (Rev) TGT TGC AGT
TCC TTC TGC
ACG GC
OPG (For) GCC GTG CAG
AAG GAA CTG
CAA C
60°C 40 seconds,
30 cycles
126
OPG (Rev) GGT GTG CAA
ATG GCT GGG
CCT
4.4.8 DNA agarose gel electrophoresis
1.5% (w/v) agarose gel was used for PCR product gel electrophoresis in this study.
Briefly, 1.5g of agarose powder (Promega Corp) was melted in 100ml 1xTAE buffer,
followed by the addition of 5μl of SYBR safe DNA stain (after cooling period of melted
agar in room temperature for about 3 minutes). The melted agar was then poured into
the Bio-Rad mini- or wide-sub cell apparatus and allowed to set at room temperature
(15-20 minutes). DNA samples together with 4μl of 100bp or 1kb DNA ladder were
loaded onto the gel and the electrophoresis was run for 30 minutes at 90V. DNA bands
were visualized using FujiFilm LAS-4000. The images were edited by inverting the
original colour.
4.5 Cell Biology This section looks at the methods for in vitro RANKL-induced BMM
osteoclastogenesis, TRAP staining, osteoclasts count, and analysis of osteoclast nuclei
and area to analyse Svs7 KO osteoclast differentiation and fusion mechanism in
reference to WT, and bone resorption assay for osteoclast activity. For osteoblast

Chapter Four – Materials and Methods
93
differentiation and activity, CFU alkaline phosphatase and alizarin red staining would
be detailed.
4.5.1 In vitro RANKL-induced osteoclastogenesis, TRAP staining, and osteoclast
count
WT and KO BMM were cultured in complete α-MEM supplemented with M-CSF and
RANKL, as described previously in Section 4.4.1.1, in 96-well plates for 5-7 days with
full medium change every 2 days. When osteoclasts had been observed at day 5/7
cultured wells, the culture medium was then discarded and the cells were washed twice
with 1xPBS. The cells were then fixed in 4% PFA for 20 minutes at room temperature.
The fixed cells were then washed twice with PBS and TRAP stained. The staining was
carried out for 30-35 minutes incubation at 37°C incubator in order to induce TRAP
activity. The TRAP staining development was then observed under Nikon Eclipse Ti
microscope. When the TRAP stain colour was fully developed, the staining solution
was discarded and the cells were washed twice with PBS. The stained cells were then
kept wet in PBS for long-term storage. Osteoclast count was carried out using Nikon
Eclipse Ti under 10x objective magnification and only cells having 3 or more nuclei
were counted as osteoclasts.
4.5.2 Analysis of osteoclast nuclei and area (osteoclast fusion mechanism)
The analysis of osteoclast nuclei and area for osteoclast fusion mechanism was carried
out on osteoclasts at day 3 and 5 of RANKL-induced osteoclastogenesis. For osteoclast
nuclei analysis, 3 categories system had been chosen (Fujita et al. 2012). The system
consists of a group of osteoclasts having 3 to 5 nuclei, followed by 6 to 10, and 11 or
more nuclei groups. After osteoclasts had been TRAP stained, osteoclast pictures at day
3 and 5 (each time point had at least 3 wells, consisting of at least 6 images per well, for
each WT and KO pair) were taken using 10x objective magnification of Nikon Eclipse
Ti microscope integrated with NIS element software. The analysis of osteoclast nuclei
was done using ImageJ software and the average number of osteoclasts falling into each
category was presented as a ratio to total number of TRAP+ osteoclasts/well and the
final result was a representative of 3 biological repeats experiments. Osteoclast area
analysis was also carried out using ImageJ software, where each osteoclast outline, from
at least 3 wells, consisting of at least 6 images of 10x objective magnification per well,
for each time point (day 3 and 5) for each WT and KO pair, was drawn and its area in
μm2 was measured and analysed. The final result was presented as an average OC area

Chapter Four – Materials and Methods
94
(μm2) for day 3 and 5 of RANKL-induced osteoclastogenesis and from 3 biological
repeats.
4.5.3 In vitro osteoclast bone resorption assay
4.5.3.1 Preparation of bone slices
A small segment of shaft from bovine femur or tibia was used as a source for bone
slices for in vitro osteoclast bone resorption assay. The cortical bone was cut into slices,
having only 0.5mm in depth, using the Isomet low speed saw (Buehler) at a speed
setting of 4 with a diamond wafering blade (Buehler). The bone slices were cut from
those cortical bone slices, having only 5-6mm in diameter, using a hole-punch. The
bone slices were then sterilised and stored in 70% ethanol. Before use, the bone slices
were washed twice with sterile 1xPBS and left overnight in α-MEM medium at 4°C
with gentle shake. The following day the bone slices were ready to be seeded onto 96-
well plates for bone resorption assay.
4.5.3.2 Mature osteoclast culture on bone slices
RANKL-induced WT and Svs7 KO BMM osteoclastogenesis was carried out using
Biocoat collagen 1-coated 6-well plates for 5 days or until osteoclasts were formed.
Culture medium was discarded and osteoclasts were then washed once with sterile
1xPBS and detached from the plates using 500μl of non-enzymatic cell dissociation
solution (Sigma Aldrich)/well at 37°C 5% CO2 incubation (15-20 minutes). The cells
were then gently scraped off the bottom of the plate with a cell scraper and the cell
suspension was then transferred to a new 2ml tube for centrifugation (1,500rpm for 5
minutes) to pellet the cells. The cells were then resuspended in a 1.5ml tube containing
complete α-MEM medium supplemented with M-CSF and RANKL (same
concentration as mentioned in Section 4.4.1.1). One hundred μl of the cell suspension
was then added to each required well of 96-well plates, which already contained
sterilized bone slices. The culture plates were then incubated further for 2 days. After
incubation, the cells on bone slices were washed twice with PBS and fixed in 4% PFA,
followed by TRAP staining as described before at Section 4.5.1. Osteoclast pictures on
bone slices (at least 3 bone slices for each WT and KO) were taken for each WT and
KO pair for osteoclast count. To visualise bone resorption pits, osteoclasts were gently
scraped off bone slices using a toothbrush and ddH2O and bone slices were numbered
accordingly at the non-cell surface and gold coated to get ready for scanning electron
microscopy (SEM) analysis.

Chapter Four – Materials and Methods
95
4.5.3.3 SEM and analysis of osteoclast resorption pits
After coating, bone slices, which were attached on pins using double-sided carbon tape
(both from ProSciTech), were ready for Philip XL30 SEM analysis at the centre for
microscopy, characterization, and analysis (CMCA), The University of Western
Australia. The setting was: set for back-scattered electron (BSE), 200x magnification,
15kV electron speed, 14-15mm working distance, and 6mm spot size. After resizing,
SEM images were saved as TIFF files and ready for pit area measurement using ImageJ
software. The resorption pits were outlined and the area was expressed in μm2. The
average resorbed area was then divided by the average number of osteoclasts on the
bone slice to give the final result as a resorption pit area/osteoclast for WT versus Svs7
KO mice.
4.5.3.4 Osteoclast bone resorption assays using Corning Osteo Assay plates
Another method used in this study for analysis of WT and Svs7 KO osteoclast bone
resorption activity was Corning Osteo Assay plates (Corning). The wells of these plates
are coated with hydroxyapatite mineral surface to mimic the actual bone mineral
surface. Briefly, WT and KO BMM were cultured first in Biocoat collagen 1-coated 6-
well plates in the presence of RANKL and M-CSF for 5 days or until osteoclasts were
formed, as described above in Section 4.5.3.2. Then, instead of using sterilised bone
slices in 96-well plates, each 100μl of WT and KO osteoclast suspensions was seeded
onto Corning Osteo Assay wells (4 wells for TRAP staining and osteoclasts count and
the other 4 (a total of 8 wells or 1 strip for each WT and KO) for resorption pits
visualization) and cultured for additional 6 days with full media change (with same
concentration of M-CSF and RANKL as mentioned in Section 4.4.1.1) every 2 days.
The media was then aspirated and for TRAP-stained wells the procedure was the same
as described in Section 4.5.1. In order to visualise the resorbed pits, the culture wells
were first incubated with 100μl/well of 10% household bleach solution for 5 minutes at
room temperature to remove osteoclasts. The bleach solution was then removed and the
wells were washed twice with 150μl/well of ddH2O, followed by air-drying for 3-5
hours at room temperature. The osteoclast count was carried out on TRAP-stained
osteoclasts images and the pits were visualized under 10x and 20x objective
magnification of Nikon Eclipse Ti microscope. The plates were then stored with 200μl
of ddH2O in each well at 4°C for long-term storage.

Chapter Four – Materials and Methods
96
4.5.4 CFU alkaline phosphatase (ALP) staining for osteoblast differentiation assay
The ALP staining was purchased from Sigma Aldrich and the experiment was carried
out according to the protocol provided. Briefly for making 5ml ALP master mix
staining solution, 100μl of FBB alkaline solution was mixed with 100μl of sodium
nitrite solution and the mix was incubated for 2 minutes at room temperature. Four and
half ml of ddH2O was then added to the mixture, followed by the addition of 100μl of
Naphthol ASBI alkaline solution (kept in dark). The ALP staining was then added drop-
wise to the fixed bone-marrow stromal cell-derived osteoblasts and the plate was
incubated in the dark for 10-15 minutes (until blue/purple colour developed) at room
temperature. The positive colonies were then analysed and counted.
4.5.5 In vitro bone marrow stromal cell-derived osteoblast bone nodule formation
(mineralization) assay
WT and Svs7 KO BM cells were cultured in mineralization/differentiation medium
(complete α-MEM medium supplemented with 10nM dexamethasone, 2mM β-
glycerophosphate, and 50μg/ml ascorbate), as described previously in Section 4.4.1.1,
for 2-3 weeks until calcium depositions were observed. The medium was then discarded
and the cells were washed with 1xPBS. The cells were then fixed in 2.5%
glutaraldehyde for 15 minutes at room temperature. After fixation, the cells were
washed three times with PBS, followed by three times 70% ethanol washes and left to
dry completely at room temperature. One % alizarin red staining was then added to the
cells for 2 minutes, followed by three times 50% ethanol washes. The plates were then
allowed to dry completely at room temperature. To measure the total mineralized area,
the plates were scanned at 600dpi on Epson 3490 Photo scanner. The scanned images
(red stain for calcium deposition) were then converted to black (for the red-stained
calcium) and white colour and thresholded. With binary process on Image J software,
the total mineralized area was measured.
4.5.6 MTS proliferation assay on WT and Svs7 KO BMM
Proliferation assay on WT and Svs7 KO BMM was carried out using CellTiter 96
Aqueous One Solution Cell Proliferation Assay (MTS) (Promega). MTS compound is
bioreduced by metabolically active cells into coloured formazan (soluble in culture
medium), by presumably involving NADPH or NADH produced by dehydrogenase
enzymes. The assay was done by measuring the absorbance of formazan-incorporated
culture medium at 490nm using Bio-Rad spectrophotometer plus. The quantity of

Chapter Four – Materials and Methods
97
formazan (measured by the absorbance at 490nm), is directly proportional to the
number of living cells in culture wells. After reaching confluence in T75 culture flasks,
WT and Svs7 KO BMM were seeded with cell density of 6x103 cells/100μl/well on 96-
well plates and cultured in complete α-MEM medium supplemented with M-CSF.
Three individual 96-well plates were needed for each WT and KO BMM pair. The first
plate was used for standard curve (starting from 0, 6, to 96x103 cells density with an
exponential rise), with the absorbance read the next day after cell seeding procedure and
after the addition of 20μl/well of the MTS reagent, followed by incubation at 37°C 5%
CO2 in the dark for about 2-3 hours. The next 2 plates, which were for 24 and 48 hours
time points (each having quadruplicate wells for each WT and KO BMM), were read on
the next two days accordingly after the standard curve reading. The absorbance for 24
and 48 hours time points were then related back to the standard curve equation to get an
estimated cell number for each WT and KO for each time point.
4.6 Cloning Method 4.6.1 Restriction enzyme digestion of DNA
Restriction enzymes cut double-stranded DNA at the restriction site (specific sequence
bases) to release plasmid DNA, which can be used to check for a correct DNA insert,
for DNA sequence analysis, or for an intermediate step to release DNA insert for the
subsequent ligation reactions with other vectors. Digestion reaction contained 5μl (for
miniprep concentration) or 2μl (for midiprep concentration) of plamid DNA, 1μl of 10x
restriction enzyme buffer B, 0.5μl of each restriction enzyme (HindIII and XhoI), and
ddH2O to make up a final volume of 10μl. The reaction mix was incubated overnight at
37°C water bath. The following day, the reaction mix was mixed with 2μl of 6x loading
dye and electrophoresed together with 1kb and 100bp DNA ladder, and visualized on a
UV transilluminator. The gel was examined for the plasmid DNA insert (295bp for
Svs7 DNA insert, which was amplified by PCR using sense 5’
ATGATTCAGTGACGAAAT 3’ and antisense 5’ GAAGCTATTACACAAGTTTT 3’
primers constructed by Dr Tony Phan PhD).
4.6.2 DNA extraction and purification from agarose gels
The DNA insert was extracted from agarose gels using QIAEX II Gel purification kit
(Qiagen). The DNA band was excised from the gel using a sterile surgical blade and
transferred into a clean 1.5ml tube. Gel fragment was weighed and solubilised

Chapter Four – Materials and Methods
98
according to the manufacturer’s instructions. All DNA was eluted using sterile ddH2O
and used immediately or stored at -20°C until required.
4.6.3 Cloning strategy and ligation to construct pGEM-T Easy Svs7
Briefly, 0.5μl of pGEM-T Easy vector (Promega), 9μl of 2x rapid ligation buffer
(Promega), and 1μl of T4 ligase (Promega) were added to a sterile 0.5ml tube,
containing 7.5μl of the eluted Svs7 DNA insert in a total reaction volume of 18μl. The
reaction mix was incubated at 16°C overnight. Following ligation process, the DNA
was transformed into DH5α competent cells the next day.
4.6.4 Cloning strategy and ligation to construct pcDNA3.1 Svs7-V5 His
Svs7 DNA insert was digested from the T Easy vector using HindIII/XhoI restriction
enzymes and ligated into HindIII/XhoI site of the pcDNA3.1 V5 His mammalian
expression vector (Invitrogen). Briefly, 2μl of pcDNA3.1 vector, 1μl of 10x T4 ligase
buffer (Promega), and 1μl of T4 ligase (Promega) were transferred into a 0.5 ml tube,
containing 6μl of the purified Svs7 DNA, for a final reaction volume of 10μl. The final
mixture was incubated at 16°C overnight and transformed into DH5α competent cells
the next day.
4.6.5 Transformation and plating of the transformed cells
The ligation product was transferred to a 2ml tube, containing 100μl aliquot of E. Coli
DH5α competent cells, and mixed gently. The cells were incubated on ice for 30
minutes and then heat shocked at 42°C water bath for 90 seconds. The tube was
immediately cooled on ice for 2 minutes. One ml of LB broth was added to the cells and
incubated at 37°C 225rpm for an hour. The cells were then pelleted by centrifugation at
13,400rpm room temperature for a minute. The supernatant was then discarded and the
cells were resuspended in 100μl of fresh LB. Under aseptic conditions, the cells were
spread on LB/Amp/IPTG/Xgal (for pGEM-T Easy-Svs7 construct) or on LB/Amp
plates (for pcDNA3.1 Svs7-V5 His construct). The plate was dried, inverted, and
incubated overnight at 37°C.
4.6.6 Bacterial culture and maintenance
Briefly, 3 clones (for Svs7-V5 His-expressing clones) were picked from the plate using
a pipette tip per clone and dropped directly into a 10ml tube, containing 4ml LB and 4μl
(100mg/ml) of ampicillin. The cultures were incubated at 37°C at 225rpm for 8 hours

Chapter Four – Materials and Methods
99
and then transferred to a culture flask, containing 50ml LB/Amp (at the same
concentration as mentioned above), for every clone, followed by incubation overnight at
37°C at 225rpm in order to yield midiprep plasmids.
4.6.7 Plasmid extraction and isolation
Plasmid DNA was extracted from small-scale DH5α cultures (4ml LB/Amp culture
overnight) using QIAprep spin miniprep (Qiagen). The overnight bacterial culture was
transferred to a 1.5ml tube, cells were pelleted, and the plasmid DNA was extracted
according to the manufacturer’s protocol. Purified plasmid DNA was eluted from the
mini column using 100μl of sterile ddH2O and was stored at -20°C until ready for use.
Isolation of plasmid DNA from 50ml overnight cultures was performed using Qiagen
plasmid plus midiprep (Qiagen) and done according to the manufacturer’s protocol. For
long-term storage of cloned bacterial cultures, 3.2ml of cloned bacterial suspension was
mixed with 800μl of glycerol (20%) and stored at -80°C. The midiprep purified plasmid
was subjected to restriction enzyme digestion reactions to confirm the correct DNA
insert for Svs7 in the HindIII/XhoI site of the pcDNA3.1 V5 His mammalian expression
vector, prior to the transfection experiment into COS-7 cells.
4.7 Experimental Methods 4.7.1 Cell transfection and collection of conditioned medium expressing Svs7 protein
COS-7 cells, grown in a T75 flask until reaching confluency, were transfected with
either empty pcDNA3.1 plasmid (as a control) or pcDNA3.1 Svs7-V5 His (one flask for
each plasmid in order to get mass production of conditioned medium expressing Svs7)
using Lipofectamine-2000 transfection reagent (Invitrogen) in accordance with the
manufacturer’s protocol. A total of 24μg of each plasmid DNA was diluted in 1.5ml of
Opti-MEM reduced serum medium and mixed gently. Sixty μl of Lipofectamine reagent
was also diluted in 1.5ml of the Opti-MEM medium, mixed, and incubated at room
temperature for 5 minutes. The diluted Lipofectamine reagent was then added to each
diluted plasmid DNA to make a total volume of 3ml and the complex was then
incubated further for 20 minutes at room temperature. Each 3ml DNA-Lipofectamine
complex was then added drop-wisely to the corresponding flask using a transfer pipette
and mixed gently by rocking the plate back and forth. After 6 hours incubation at 37°C
5% CO2 cell culture incubator, the transfection medium was discarded from each flask
and the cells were washed twice with fresh Opti-MEM medium to wash away the
transfection reagent. Cells were then incubated in 10ml of fresh Opti-MEM medium and

Chapter Four – Materials and Methods
100
the collection of conditioned medium expressing Svs7 protein and control began the
next day (day 1) and performed daily for up to 6 days to generate plenty of conditioned
medium required for luciferase assay experiments. At the day of collection, each
conditioned medium (control and Svs7 plasmid) was collected and transferred to a clean
50ml tube, ready to be centrifuged for 10 minutes at 3,000rpm to pellet any dead cells.
The clean conditioned medium was then transferred to a clean 15ml tube and a 30μl
aliquot of each medium was transferred to a 1.5ml tube for western blot (WB) protein
analysis to test for the expression of Svs7 protein in the medium.
4.7.2 Luciferase assay
RAW264.7 cells, stably expressing NFAT promoter (stable transfection of RAW264.7 cells
with a GL4.30 (luc2P/NFAT-RE/Hygro) (Promega) (Singh et al. 2012)), were seeded
overnight on a 48-well plate with a cell density of 1.5x105 cells/500μl/well. With the
confirmation from WB analysis that Svs7 protein was successfully expressed in the
medium, the following day some wells were then pre-treated with 50% Svs7
conditioned medium and the rest with the control medium for an hour, followed by
100ng/ml RANKL stimulation overnight. The cells were then lysed using 100μl/well of
luciferase lysis buffer with the addition of 2mM DTT. The lysates were then collected
into 1.5ml tubes accordingly and centrifuged at 14,000rpm at 4°C for 20 minutes to
clear cellular debris. The clear lysates were then transferred to fresh 1.5ml tubes. Fifty
μl of each sample was then put into a clean white-bottom 96-well plate and mixed with
50μl of luciferase assay substrate (Promega). The luminescence reading was performed
using the BMG Polar Star Optima luminescence reader at UWA school of
Pharmacology and the NFAT luciferase activity was expressed as arbitrary unit (this
experiment had been assisted by Mingli Yang, a PhD candidate at Jiake Xu cell
signalling group, UWA School of Pathology and Laboratory Medicine).
4.7.3 Flow cytometry analysis on fixed and stained WT and Svs7 KO BM cells
BM cells were extracted from WT and Svs7 KO long bones as described in Section
4.4.11. The cell suspensions were then centrifuged at 1,500rpm for 5 minutes to pellet
the cells. One ml of red blood cell (RBC) lysis buffer was then added to the cells for a
minute, which was then followed by the addition of 9ml of 1xPBS to inactivate the
buffer activity. The cells were then pelleted and the supernatant was then replaced with
1ml of 1xPBS. The cells were then counted using Optik Labor haemocytometer for 106
cells in 50μl 1xPBS suspension for each WT and KO and also for controls (5 antibodies

Chapter Four – Materials and Methods
101
minus 1), unstained, and live/dead (L/D) cells, which were prepared from WT cells.
Antibodies master mix was then prepared for WT and KO test samples by diluting the
antibodies (FITC-CD45R, V450-CD11b, PE Cy.7-CD3e, PE-c-Kit, and APC-Sca-1) to
0.5μg in 50μl cold flow cytometry wash buffer. The diluted antibodies master mix was
then added to the 50μl of 106 cells suspension for a total volume of 100μl and mixed
gently by tapping. The mixture was then incubated in the dark on ice for 45 minutes.
The samples were washed with 500μl of wash buffer to dilute the antibodies and the
cells were then pelleted at 350 g centrifugation 4 °C for 5 minutes. After the removal of
supernatant, the samples were washed twice with 200μl of cold wash buffer at 350 g
centrifugation 4 °C for 5 minutes. The cells were then resuspended in 500μl wash
buffer. To prepare for L/D control, 250μl of cells suspension was aliquoted out and
snap-freezed in liquid nitrogen and mixed them again with the other 250μl of cells
suspension. One μl of L/D Aqua stain was then added into the 500μl cell suspension and
mixed well by gentle tapping. The L/D control sample was then incubated on ice in the
dark for 30 minutes. All the test and control samples were then spined down and the
cells were then washed once with 500μl of wash buffer. The cells were then
resuspended in 300μl of 1xBD Stabilizing Fixative and stored at 4°C in the dark
overnight for the next day analysis. For preparation of bead samples for compensation,
100μl of wash buffer was added into each labelled tube (1 tube for 1 antibody). One full
drop of each negative and positive beads was then added to the tube, followed by the
addition of the appropriate antibody (with the same concentration as mentioned above).
The 5 samples were then incubated in the dark at room temperature for 30 minutes.
Following the incubation, 1ml of wash buffer was then added to each tube and the beads
were then pelleted by 200 g centrifugation for 10 minutes. The supernatant was
discarded and the pellet was resuspended in 300μl of 1xBD stabilizing fixative and
stored at 4°C overnight together with the rest of samples for analysis the next day. Flow
cytometry analysis was performed using FACS Canto at CMCA, UWA. Lineage
negative (Lin-) population, which is regarded as early osteoclast precursors and
characterised as CD3e- CD45R- CD11blow/-, was gated first, followed by the analysis of
Sca-1+ c-Kit+ markers from Lin- population to deduce hematopoietic stem/progenitor
cells (HSCs) niche in the bone marrow of WT and KO mice.
4.7.4 Fluo-4AM intracellular calcium assay on WT and Svs7 KO osteoclasts
Hanks wash buffer for the assay was purchased from Gibco, Australia, while Fluo-4AM
calcium-binding dye kit was from Invitrogen, Australia. First, 20% pluronic acid was

Chapter Four – Materials and Methods
102
made by dissolving 0.2g of the pluronic in 1ml of DMSO. Subsequently, 1mM Fluo-
4AM was made by dissolving 50μg of the dye (provided in the kit) in 45.58μl of 20%
pluronic acid. The wash buffer in this assay was prepared by having 2mM probenecid
(stock of 1M) in Hanks buffer solution. Fluo-4AM working solution (Fluo-4AM/Hanks)
was then made by mixing 4μl of Fluo-4AM stock/ml (4μM) of Hanks/Probenecid
required for loading 250μl per well. Forty eight-well plates were used for this assay.
After aspirating culture medium from the wells upon the observation of osteoclasts on
coverslips, the cells were washed twice with 250μl of Hanks/Probenecid wash
buffer/well, followed by loading and incubating the cells with 250μl of Fluo-
4AM/Hanks/well for 45 minutes at room temperature in the dark. After incubation, the
cells were then washed once with the Hanks/Probenecid wash buffer and the cells were
incubated further for 20 mins in 200μl of the wash buffer at room temperature in the
dark. The cells were then washed 3 times with Hanks/Probenecid wash buffer and kept
in 200μl of the wash buffer for the initial baseline reading of fluorescence intensity
(calcium oscillation). Fluo-4 emits at green fluorescence channel (488nm excitation).
Nikon Eclipse Ti microscope with fluorescent light and incorporated NIS-Element
Basic research software were used in this calcium assay. The baseline reading (calcium
oscillation) was observed and recorded for 2 minutes using timelapse tool of the NIS
software. The assay then incorporated the addition of extracellular calcium (using
calcium chloride (CaCl)) of 5, 10, and 20mM concentrations and each fluorescence
intensity reading was recorded for 3 minutes following the initial baseline reading.
4.7.5 Cell lysis procedure for Western Blot (WB) protein analysis
Briefly, culture medium was aspirated and the cells were washed once with 1xPBS. The
cells were then lysed with 200μl/well (6-well plate) of RIPA lysis buffer, followed by
incubation on ice for 20 minutes. The cells were scrapped off the bottom of the plate
using a pipette tip and the cell lysates were collected into 1.5ml tubes and centrifuged at
12,000rpm at 4°C to pellet cellular debris. The clear cell lysates were then transferred to
fresh 1.5ml tubes and stored at -20°C until ready for protein concentration measurement
and WB analysis.
4.7.6 Velocity density gradient centrifugation
Velocity density gradient centrifugation was performed as previously described (Ng et
al. 2013; Pavlos et al. 2011). Briefly, ~107 osteoclasts were washed with ice-cold
1xPBS and scraped with 500ml of lysis buffer (50mM HEPES-KOH pH 7.2, 150mM

Chapter Four – Materials and Methods
103
NaCl, and 1mM MgCl2) supplemented with protease inhibitors: 1mM PMSF, 1mg/ml
aprotinin, 1mg/ml leupeptin, and 0.7mg/ml pepstatin (all from Sigma Aldrich). The cell
lysate was then homogenized by passing cells through a 25-gauge syringe (at least 10
strokes). Proteins were cleared by centrifugation at 3,000rpm for 15 minutes at 4°C.
Five hundreds ml of clarified supernatant was layered on top of 12ml of 5-20% linear
sucrose density gradient, which was prepared in the lysis buffer. Centrifugation was
then performed at 150,000g for 18 hours in a SW40 rotor (Beckman Coulter), followed
by the collection of 1ml protein fractions. An equal volume of fractions were analysed
in western blot system using rabbit polyclonal anti-Svs7 antibody. α-tubulin was used
as a loading control.
4.7.7 Measuring protein concentration
The Bio-Rad protein assay is a simple colorimetric assay for determining total protein
concentration. The Bio-Rad protein dye reagent was diluted 1 in 5 using ddH2O, while
protein samples were diluted 1 in 10 using 1xPBS. Two hundreds μl of the dye reagent
was then added per well to a 96-well plate. Ten μl of each protein standard (BSA/PBS
with concentration of 0, 0.05, 0.1 to 0.5mg/ml (an increment of 0.1mg/ml)), PBS
control, RIPA lysis buffer control, and protein samples (assayed in duplicate) was then
added to the dye, mixed gently, followed by incubation at room temperature for 5
minutes for colour development. The absorbance was read at 595nm wavelength using
the Bio-Rad Model 680 microplate reader.
4.7.8 Western Blot (WB) SDS-PAGE system
SDS-PAGE system is the most commonly used system to separate and analyze proteins
according to their size. To do that, sodium dodecyl sulfate (SDS), a detergent, denatures
and covers the protein primary structures with many negative charges by its negatively
charged sulfate group. Hence all proteins will migrate towards the positive pole (anode)
in an electric field. Finally polyacrylamide gel, with running electricity, will separate
proteins based on their size (Da). Hence, by using standard known protein samples,
relative molecular weight of unknown proteins and their distribution can be estimated
and examined using this SDS-PAGE system.
4.7.8.1 Preparation of the SDS-PAGE system
There are two different gels in this SDS-PAGE system, a stacking gel, where the protein

Chapter Four – Materials and Methods
104
samples are loaded onto, and a separating gel underneath, where the proteins run and
get separated based on their size. Electrophoresis of the SDS-PAGE system was carried
out using the Mini-Protean III Cell Electrophoresis System (Bio-Rad) casting apparatus.
10% and 17.5% separating gels were prepared as follows:
Separating Gel Components 10% 17.5%
MilliQ H2O 2.97ml 1.095ml
1.5M Tris-HCl, pH 8.8 1.875ml 1.875ml
10% SDS 75μl 75μl
30% Acrylamide/Bis 2.5ml 4.375ml
10% Ammonium persulfate
(APS) 75μl 75μl
TEMED 6μl 6μl
Total Volume 7.5ml 7.5ml
The separating gel final mixture was then carefully poured into a glass-gel sandwich to
about 1cm below the level of the well comb. Twenty % ethanol was slowly and evenly
overlaid on top of the separating mixture to remove any bubbles and to avoid oxidation
of the gel. The gel was then allowed to set at room temperature for 15-20 minutes. A
5% stacking gel was then prepared as follows:
5% Stacking Gel Components Volume
MilliQ H2O 2.062ml
1M Tris-HCl, pH 6.8 375μl
10% SDS 30μl
30% Acrylamide/Bis 500μl
10% APS 30μl
TEMED 3μl
Total Volume 3ml
As the separating gel set, a clear line was formed between the gel and the 20% ethanol.
The ethanol was then removed from the cast and the stacking gel mixture was poured
carefully into the sandwich on top of the separating gel. A 10 or 15-well comb was
immediately inserted into the stacking gel mixture and the gel was allowed to set at
room temperature for 15-30 minutes. After the gel polymerised, the comb was carefully

Chapter Four – Materials and Methods
105
removed and the glass-gel sandwich was then transferred into the SDS-PAGE tank
system, which was filled with 1xSDS-PAGE running buffer. Protein samples were then
prepared by adding right amount of 4xSDS-PAGE loading dye, containing 5% ß-
mercaptoethanol (which acts to break down disulphide bonds within and between
protein molecules), and subsequently boiled at 99°C using Eppendorf Thermomixer
Comfort for 5 minutes to denature the proteins. Each protein sample was then loaded
onto the stacking gel. A 10μl volume of Precision Plus protein standard (Bio-Rad) was
also loaded and run together with the protein samples for molecular weight analysis.
The electrophoresis was run at 100V for 120 minutes.
4.7.8.2 Protein transfer to nitrocellulose membrane
The Mini Trans-Blot Electrophoresis Transfer Cell (Bio-Rad) apparatus was set up
according to manufacturer's instructions. Two scotch pads and 6 Whatman 3MM papers
were pre-soaked in WB transfer buffer. Following electrophoresis, the glass-gel
sandwich was removed from the tank. One soaked scotch pad was placed onto the clear
side of the gel holder cassette, which was then overlaid by 3 pieces of the soaked
Whatman papers and a nitrocellulose membrane. The gel was slowly released from the
inside of the sandwich and the stacking gel was carefully separated and discarded away
from the separating gel. Finally, the separating gel was then carefully placed on top of
the nitrocellulose membrane, followed by another 3 soaked Whatman papers and the
second soaked scotch pad (respectively from the middle to the top). The gel holder
cassette was then closed and placed in the WB transfer tank filled with WB transfer
buffer and an ice block, making sure that the gel is facing the black terminal (cathode)
and the membrane is facing the red terminal (anode). The protein standard and samples
were transferred to the nitrocellulose membrane at a current of 0.03A overnight.
4.7.8.3 WB reaction
The next day following WB transfer, the gel cassette was removed from the WB
transfer tank and the membrane was carefully released from the separating gel, placed
on a square dish, and incubated with 10ml of 5% skim milk in 1xTBS-Tween (TBST)
solution for an hour at room temperature on the RATEX rocking platform mixer as a
blocking step in order to reduce non-specific antibody binding (background). After an
hour in blocking step, the skim milk was discarded and the membrane was then washed
once with TBST for 5 minutes at room temperature, followed by overnight incubation
in 10ml 1:1000 or 1:500 dilution of primary antibody (listed in Section 4.1.7

Chapter Four – Materials and Methods
106
Antibodies) in 1% skim milk/TBST at 4°C. The following day the membrane was
washed 3 times with TBST for 5 minutes/wash at room temperature, followed by an
hour room temperature incubation with 10ml 1:5000 dilution of goat peroxidase-
conjugated secondary antibody in 1% skim milk/TBST on the RATEX rocking platform
mixer. After incubation and removal of the secondary antibody, the membrane was
washed twice with TBST for 5 minutes/wash, followed by twice TBS washes each for 5
minutes. The detection of proteins by immuno-reaction was achieved using Western
Lightening Ultra Extra Sensitivity (Perkin Elmer) kit. Solution A and B (from the
Detection System) were pre-warmed at room temperature and 1:1 ratio mixture of these
2 solutions was then made in a 1.5ml microcentrifuge tube. The detection reagent
mixture was then incubated with the washed membrane for a minute at room
temperature in the dark. After the removal of excess detection reagent from the
membrane, chemiluminescence detection was performed using the FujiFilm LAS-4000.
4.7.8.4 Stripping the membranes
Briefly, the stripping buffer was pre-warmed to 55°C, while the used membranes were
washed once with TBST for 5 minutes. The wash solution was discarded and the
stripping buffer was then added to the membranes, followed by incubation at 55°C with
a gentle shake for 30-40 minutes. The membranes were washed twice with TBST for 5
minutes each. Finally, the membranes were ready for the next WB reaction starting at
the blocking step.
4.8 Statistical Analysis Experimental data are presented as mean ± SEM of 3 independent samples. Statistics
were performed using two-tailed Student t-test for each biological pair (at least 3
biological repeats), where p values < 0.05 or < 0.01 were considered significant.

107
CHAPTER 5
CHARACTERISATION OF SVS7 TRANSGENIC MICE

Chapter Five – Characterisation of Svs7 Transgenic Mice
108
5.1 Introduction Aforementioned, healthy bone mass is achieved largely by balanced yet complementary
activity between bone-resorbing osteoclasts and bone-forming osteoblasts. This bone
remodelling process is governed by several direct cell-to-cell interaction systems,
including between osteoclasts and osteoblasts, as exemplified by the binding of
EphrinB2, an osteoclast-expressed membrane-bound ligand, to its receptor EphB4,
expressed by osteoblasts (Martin et al. 2010; Zhao et al. 2006), and through the
secretion of growth factors, cytokines, and proteins by both cells (Zaidi 2007). Bone
diseases, such as osteoporosis and osteopetrosis, may therefore occur as a consequence
of the loss of coupling and communication between osteoclasts and osteoblasts
(Guerrini et al. 2008; Riggs & Melton 1983; Sobacchi et al. 2007; Villa et al. 2009).
Osteoporosis, by far the most common bone disease (Lerner 2006), is characterized by a
net bone loss, causing bones to become weaker and have a greater susceptibility of
fractures (Riggs & Melton 1983). Excessive osteoclast bone resorption (at the level
where more bone resorbed than formed) accompanies this pathological bone disease,
which is primarily seen in postmenopausal women (triggered by hormonal change)
(Riggs & Melton 1983) and in the elderly (Manolagas & Jilka 1995). As the cost for
management and treatment of osteoporosis and other bone diseases increases each year
(approximately to be $14 billions/year for 1.3 millions fractures in US (Lerner 2006;
Ray et al. 1997)), research has been focused on identifying novel factors, expressed by
osteoclasts and/or osteoblasts, that influence their differentiation and activation and
hence may be utilised as therapeutic targets for skeletal diseases.
In search of candidate coupling factors from osteoclasts, we have previously employed
subtractive hybridization-based differential screening method and identified Svs7 as a
novel osteoclast-expressed factor. Furthermore, studies from Davey 2008 suggested that
recombinant purified Svs7 protein treatment could enhance trabecular bone/tissue
volume, trabecular thickness, and trabecular number in ovariectomised mice (oestrogen
deficiency-induced bone loss mouse model (Aitken, Armstrong & Anderson 1972; Kalu
1991; Saville 1969)), implying that the administration of recombinant Svs7 protein
might be a potential anabolic factor and therefore be beneficial to the treatment of
osteoporosis. Hence, based on these initial data, the major aim of this thesis was to
explore the physiological role of Svs7 in bone homeostasis. To address this, a two-
armed approach was employed: 1. To generate transgenic (TG) mice overexpressing

Chapter Five – Characterisation of Svs7 Transgenic Mice
109
Svs7 and 2. To genetically ablate Svs7 globally in mice. The generation and
characterisation of mice overexpressing Svs7 are presented herein.
5.2 Results 5.2.1 Tissue distribution of Svs7 gene
As an initial step towards characterising the influence of Svs7 overexpression in mice,
the global expression pattern of Svs7 was first established in all major mouse tissues,
with osteoclast as a control. For this, organs and tissues were extracted from 12-week
old WT mice, snap frozen, and total RNA was extracted using Trizol method (as
described in Chapter 4 Section 4.4.4). Semi-quantitative reverse transcription PCR (RT-
PCR) reaction was then conducted across each tissue sample using specific primers for
Svs7 and densitometry analysis was performed to quantify the relative ratio of Svs7
expression in each tissue over β-actin, which served as a loading control. As expected,
Svs7 was most abundantly expressed in seminal vesicles (SV), which included prostate
tissue, with little to no expression observed in other tissues examined, including brain,
thymus, lung, liver, and stomach (Figure 5.1). In addition, Svs7 was detectable in
osteoclasts but not in total bone, possibly owing to low level of resident osteoclasts in
vivo (Figure 5.1). Thus, these data indicate that Svs7 is largely restricted to SV tissue
and osteoclasts.
5.2.2 Generation of the Svs7 transgenic (TG) mice
Having established the expression pattern of Svs7 in osteoclast and other peripheral
tissues, we proceeded with the generation of Svs7 TG mice. This was achieved by
microinjecting a linearized and purified pcDNA3.1 Svs7 V5-His transgene (confirmed
by agarose gel electrophoresis (lane 2) and shown in Figure 5.2A) into blastocysts, as
detailed in Chapter 4 Section 4.3.1 Figure 4.1. Following breeding, genotyping was
performed for the first six litters using specific primers for Svs7. The expression of the
Svs7 coding sequence (295bp) in litter number 4 and 5 was confirmed by gel
electrophoresis (Figure 5.2B). In order to confirm the transgenic expression of Svs7 at
the protein level, livers were extracted from 9-week old WT and Svs7 TG mice, snap
frozen, and subsequently crushed using sterile mortars and pestles. Protein extraction
was performed using Ripa lysis buffer. Western blot (WB) analysis on cleared liver
lysates from WT and Svs7 TG mice was conducted using rabbit polyclonal anti-Svs7
antibody. Unexpectedly, the result showed that although the expression of Svs7
transgene was successful, the TG mice only showed a modest increase in Svs7 protein

Chapter Five – Characterisation of Svs7 Transgenic Mice
110
0 0.2 0.4 0.6 0.8 1 1.2
OC Bone
Seminal vesicle Brain Heart
Thymus Lung Liver
Spleen Stomach
Kidney Intestine
Skin Fat
Ovary
Ratio to β-actin
Thym
us
Stom
ach
Intes
tine
Svs7
β-actin
Semina
l Ve
sicle
OC Bon
e
Brain
Heart
Lung
Li
ver
Splee
n
Kidney
Skin
Fat
Ovary
Figure 5.1 Tissue distribution of Svs7 mRNA expression. Selected organs and tissues
were extracted from 12-week old WT mice, snap frozen with liquid nitrogen, and RNA
extraction from these frozen tissues was performed using Trizol method. RT-PCR
reaction on these tissues samples was then performed using specific primers for Svs7.
Osteoclast RNA sample was used as a positive control. Densitometry analysis was
carried out using ImageJ software and the Svs7 gene expression in each tissue was
presented as a ratio to β-actin, which served as a loading control. The result showed that
Svs7 mRNA was abundantly expressed in SV (including prostate tissue) but
undetectable in other tissues, including bone, brain, thymus, lung, liver, and stomach.

Chapter Five – Characterisation of Svs7 Transgenic Mice
111
1 2 3 4 5 6
250bp
500bp Marker
WT TG
Svs7
β-actin
0
0.05
0.1
0.15
0.2
0.25
0.3
WT TG Sv
s7 p
rote
in e
xpre
ssio
n in
live
r (r
atio
to β
-act
in)
pcDNA3.1 Svs7-V5 His
pcDNA3.1 Svs7-V5 His linearised with SfuI
2 1 DNA
Ladder
6000bp
3000bp
(A) (B)
(C)
Figure 5.2 Generation of the Svs7 TG mice. (A) SfuI restriction enzyme digestion on
pcDNA3.1 Svs7 V5-His was performed to get the linearized form of the transgene
plasmid and the product was subsequently run and checked on agarose gel
electrophoresis, together with the undigested plasmid. The result showed a successful
generation of the linearized Svs7 transgene in lane 2 with size of about 6,000bp. The
linearized Svs7 transgene plasmid was then purified and microinjected into blastocysts
for the generation of Svs7 TG mice. (B) Genotyping for the first six litters using
specific primers for Svs7 and gel electrophoresis for the DNA genotyping products
showed that litter number 4 and 5 had successfully expressed Svs7 coding sequence
(295bp). (C) Livers were extracted from 9-week old WT and Svs7 TG mice and after
being snap-frozen with liquid nitrogen and crushed using sterile mortars and pestles, the
protein extraction was performed using Ripa lysis buffer. (Top panel) WB analysis on
these liver lysates using rabbit polyclonal anti-Svs7 antibody and (Bottom panel)
densitometry measurement using ImageJ software (at which Svs7 expression was
expressed as a ratio to β-actin that served as a loading control) revealed the modest
increase in Svs7 protein expression (about 2.5 fold increase) in Svs7 TG mice, relative
to the very low expression of Svs7 in WT.

Chapter Five – Characterisation of Svs7 Transgenic Mice
112
expression (about 2.5 fold increase, shown by densitometry measurement using ImageJ
software (Figure 5.2C)), which was relative to the very low expression of Svs7 in WT
liver lysate. β-actin served as a loading control. Together, these results reveal the
successful albeit modest expression of the Svs7 transgene in Svs7 TG mice.
5.2.3 Histological phenotyping of Svs7 TG mice
To begin to characterise the effect of Svs7 overexpression in TG mice, prostate tissues
were dissected from 9-week old (sex-matched) WT and Svs7 TG mice, fixed,
processed, embedded, sectioned, and Haematoxylin and eosin (H&E) stained for
histological examination. Prostate tissue was selected for closer phenotypic assessment
as it has the highest Svs7 gene expression amongst other organs. As shown in Figure
5.3, the histological assessment revealed no distinguishable differences in the size or
morphology of the prostate between WT and Svs7 TG mice, indicating that
overexpression of Svs7 does not influence prostate development or morphogenesis.
5.2.4 Body weight and radiographic assessment of Svs7 TG mice
To further assess the phenotype of Svs7 TG mice, the total body weight was next
assessed. Body weight measurements of 9-week old WT and Svs7 TG mice were
performed. Mice were sacrificed and each body weight was measured. The result
showed that there was no significance difference in body weight between WT and Svs7
TG mice (Figure 5.4A). Subsequently, the whole body of WT and Svs7 TG mice were
taken for X-ray analysis. The result showed that there was no striking difference in
skeletons between WT and Svs7 TG mice (Figure 5.4B Left panel). To further confirm
this result, the vertebrae were dissected from the pairs and taken for X-ray. Again, the
result showed that there was no difference in the vertebrae between WT and Svs7 TG
mice (Figure 5.4B Right panel). Together, these results indicate that there is no obvious
change in skeletons of Svs7 TG mice.
5.2.5 MicroCT analysis of tibia, femur, and lumbar vertebrae of Svs7 TG mice
To further elucidate the bone phenotype of Svs7 TG mice, the trabecular bone
architecture of the proximal tibia, distal femur, and vertebral body of the lumbar bone of
TG mice was investigated by microCT. For this, 9-week old WT and Svs7 TG mice
were sacrificed and tibia, femur, and lumbar vertebral bones were dissected from both,
fixed, and analysed by microCT. Representative 2D and 3D microCT images showed
no apparent difference in trabecular bone architecture at the proximal tibia, distal femur,

Chapter Five – Characterisation of Svs7 Transgenic Mice
113
WT TG Pr
osta
te
Figure 5.3 Histological examination of prostate of Svs7 TG mice. Prostates were
dissected from 9-week old WT and Svs7 TG mice, fixed, processed, embedded,
sectioned, and H&E stained for histological assessment. The result showed no obvious
difference in the size or morphology of the prostate between WT and Svs7 TG mice.
Hence, the Svs7 transgene expression does not appear to affect prostate development or
morphogenesis. Scale bars, 500μm.

Chapter Five – Characterisation of Svs7 Transgenic Mice
114
WT TG WT TG
WT TG Body
Weight (g) 18.71 ± 0.48 19.26 ± 0.20
(A)
(B)
Figure 5.4 Body weight and radiographic assessment of Svs7 TG mice. (A) Nine-
week old WT and Svs7 TG mice were sacrificed and their body weights measurements
were conducted using the A&D HT-500 balance. The result revealed that there was no
significant difference in body weight between WT and Svs7 TG mice. (B) (Left panel)
The whole body of the 9-week old WT and Svs7 TG mice were taken for X-ray
analysis. The result showed that there was no obvious difference in skeletons between
WT and Svs7 TG mice. (Right panel) To further confirm this result, the vertebrae were
dissected from these mice and taken for X-ray. The result confirmed that there was no
obvious change in skeletons of Svs7 TG mice. Data are presented as mean ± SEM.

Chapter Five – Characterisation of Svs7 Transgenic Mice
115
and at the vertebral body of the lumbar bone between WT and Svs7 TG mice (Figure
5.5), further confirming that there is no obvious change in overall bone architecture of
Svs7 TG mice.
5.2.6 Svs7 TG mice exhibit a normal bone mass
In addition to radiographic and microCT assessments of the bones of Svs7 TG mice, the
solid quantitative bone parameters were also assessed. Bone parameters, including
trabecular bone/tissue volume (BV/TV) (%), trabecular separation (Tb.Sp) (mm),
trabecular thickness (Tb.Th) (mm), and trabecular number (Tb.N) (1/mm), were
assessed from femurs of 9-week old WT and Svs7 TG mice, based on data obtained
from microCT analysis. The results revealed that there were no significant differences
in all bone parameters between WT and Svs7 TG mice (Figure 5.6). Hence, the bone
mass of Svs7 TG mice is comparable to their WT littermates.
5.2.7 Histological assessment of Svs7 TG bones
As a standard procedure for bone phenotype characterisation, histological examination
on both paraffin-embedded decalcified and plastic-embedded non-decalcified bone
samples from 9-week old WT and Svs7 TG mice was performed. First, calvarial, tibia,
femur, and lumbar bones were extracted from both WT and TG mice, fixed, decalcified,
processed, embedded, sectioned, and H&E stained for histological assessment, as
described in Chapter 4 Section 4.3.5. The other femurs from the same WT and TG pairs
of mice described above were not decalcified and processed for plastic embedding, as
described in Chapter 4 Section 4.3.5 starting at point 4.3.5.4. The non-decalcified
sections were then stained with goldner trichrome (bone stained green) and/or TRAP
(an osteoclast marker; red precipitates). By using goldner trichrome stain on non-
decalcified sections, the osteoid, which is the unmineralised organic component of bone
and stained orange/red, can be observed and used in the histomorphometry analysis.
The H&E-stained sections showed that there was no obvious difference in bone volume
architecture and periosteal thickness of calvarial bone between WT and Svs7 TG mice
(Figure 5.7A and B). Furthermore, there were also no apparent changes in trabecular
bone architecture and cortical bone at the metaphyseal region of tibia (Figure 5.7C and
D), femur (Figure 5.7E and F), and lumbar (Figure 5.7G and H) bones of Svs7 TG mice
relative to that of WT littermates. In support of these results, the goldner trichrome non-
decalcified femurs sections depicted normal and healthy appearances of trabecular bone
architecture and cortical thickness of Svs7 TG hindlimbs in comparison

Chapter Five – Characterisation of Svs7 Transgenic Mice
116
WT TG
Tibia
Femur
Lumbar

Chapter Five – Characterisation of Svs7 Transgenic Mice
117
Figure 5.5 2D and 3D microCT images of proximal tibia, distal femurs, and
vertebral body of the lumbar bone of Svs7 TG mice. Tibia, femur, and lumbar
vertebral bones were extracted from 9-week old WT and Svs7 TG mice, fixed, and
analysed using the Skyscan 1072 microCT system. The representative 2D and 3D
microCT images showed that there was no obvious difference in trabecular bone
architecture at the proximal tibia, distal femur, and at the vertebral body of the lumbar
bone between WT and Svs7 TG mice. These results further confirmed that there was no
obvious change in overall bone architecture of Svs7 TG mice. Scale bars, 500μm.

Chapter Five – Characterisation of Svs7 Transgenic Mice
118
WT TG n.s.
0
5
10
15
20
25
30
WT TG
BV
/TV
(%)
0 0.02 0.04 0.06 0.08
0.1 0.12 0.14 0.16 0.18
0.2
WT TG
Tb.
Sp (m
m)
n.s.
0
0.01
0.02
0.03
0.04
0.05
0.06
WT TG
Tb.
Th
(mm
) n.s.
0 0.5
1 1.5
2 2.5
3 3.5
4 4.5
5
WT TG
Tb.
N (1
/mm
)
n.s.
Figure 5.6 Svs7 TG mice exhibit a normal bone mass. Nine-week old WT and Svs7
TG mice were sacrificed and femurs were extracted from both, fixed, and analysed
using the Skyscan 1072 microCT system. The results showed that there were no
significant differences in all bone parameters (BV/TV (%), Tb.Sp (mm), Tb.Th (mm),
and Tb.N (1/mm)) between WT and Svs7 TG mice. Hence, Svs7 TG mice exhibit a
normal bone mass. Data are presented as mean ± SEM. Number of mice (n) = 2-
3/group. n.s. = no significance against WT. Scale bars, 500μm.

Chapter Five – Characterisation of Svs7 Transgenic Mice
119
WT TG
Calvarial
Tibia
Femur
Lumbar
(A) (B)
(C) (D)
(E) (F)
(G) (H)

Chapter Five – Characterisation of Svs7 Transgenic Mice
120
Figure 5.7 Histological examination on H&E-stained decalcified Svs7 TG bone
samples. (A and B) Calvarial, (C and D) tibia, (E and F) femur, and (G and H) lumbar
vertebral bones were extracted from 9-week old WT and Svs7 TG mice, fixed,
decalcified, processed, embedded, sectioned, and H&E stained for histological
examination. The representative images were taken with 10x objective magnification.
The results showed that there were no obvious differences in bone volume architecture
and periosteal thickness of the calvarial bone between WT (A) and Svs7 TG mice (B).
Furthermore, there were also no apparent changes in trabecular bone architecture and
cortical bone at the metaphyseal region of tibia (C and D), femur (E and F), and lumbar
(G and H) bones of Svs7 TG mice relative to that of WT littermates. Scale bars, 100μm.

Chapter Five – Characterisation of Svs7 Transgenic Mice
121
to that of WT (Figure 5.8A). Moreover, TRAP-stained sections and bone
histomorphometry analysis on number of osteoclasts/bone surface (NOc/BS) parameter
further revealed a comparable number of TRAP-positive osteoclasts near the growth
plate region between WT and Svs7 TG hindlimbs (Figure 5.8B and Figure 5.9,
respectively), which indicate that Svs7 TG mice exhibit a characteristic of healthy bone
remodelling process.
5.2.8 Svs7 TG mice exhibit an unaffected osteoclast differentiation in vitro
Having established that the bone architecture of Svs7 TG mice appeared phenotypically
to be comparable to WT littermates and as a final step towards characterising any
potential cell-specific influence of Svs7 overexpression in TG mice, the capacity of
bone marrow (BM) progenitor cells to differentiate into osteoclasts was assessed. For
this, 9-week old WT and Svs7 TG mice were sacrificed, which was followed by
isolation and culture of bone marrow macrophages (BMM) from long bones (tibia and
femur), as described in Chapter 4 Section 4.4.1.1. Upon confluency, the cells were
seeded into 96-well plates, ready for time course RANKL and M-CSF-induced
osteoclastogenesis. The result showed that there was no significant difference in
osteoclastogenesis between WT and Svs7 TG mice (Figure 5.10). Hence, this result
further supported the findings in the TRAP sections histological assessment and
histomorphometry data described above that Svs7 TG mice exhibited an unaffected
osteoclastogenesis in vitro and in vivo.
5.3 Discussion Bone homeostasis is maintained by balanced yet complementary activity between bone-
resorbing osteoclast and bone-forming osteoblast, in which many growth factors,
cytokines, and proteins, secreted by either or both cells, have been shown to have
regulatory roles in maintaining bone homeostasis (Kular et al. 2012; Martin et al. 2010;
Walker et al. 2008; Zaidi 2007; Zhao et al. 2006). Based on previous observations in
our laboratory, Svs7 has been identified to be exclusively expressed in mature
osteoclasts in bone and its gene expression is upregulated during RANKL-induced
osteoclastogenesis (as discussed in Chapter 2 Section 2.4). In addition, studies from
Davey 2008 suggested that recombinant purified Svs7 protein treatment could enhance
trabecular bone/tissues volume, trabecular thickness, and trabecular number in
ovariectomised mice (oestrogen deficiency-induced bone loss mouse model (Aitken,
Armstrong & Anderson 1972; Kalu 1991)).

Chapter Five – Characterisation of Svs7 Transgenic Mice
122
100μm 100μm
WT TG
500μm
500μm
500μm
500μ
500μm
μ
100μm
100μm
Gol
dner
tric
hrom
e
TRA
P (4
x ob
j.)
TRA
P (1
0x o
bj.)
(A)
(B)

Chapter Five – Characterisation of Svs7 Transgenic Mice
123
Figure 5.8 Histological examination on goldner trichrome (A) and TRAP (B)
stained non-decalcified femur sections of Svs7 TG mice. The other femurs from the
same pairs of WT and Svs7 TG mice described above were not decalcified and
processed for plastic embedding procedure. The non-decalcified sections were then
goldner trichrome (bone stained green) and TRAP (osteoclast stained red)-stained. In
support of the H&E sections results, (A) the goldner trichrome-stained sections depicted
normal and healthy appearances of trabecular bone architecture and cortical thickness of
Svs7 TG hindlimbs in comparison to that of WT littermates. (B) Accordingly, from
TRAP sections, it showed a comparable number of TRAP-positive osteoclasts near the
growth plate region between WT and Svs7 TG hindlimbs, indicating that Svs7 TG mice
exhibit a characteristic of healthy bone remodelling process. Together, these results
suggested normal bone phenotype and TRAP-positive osteoclasts number in Svs7 TG
hindlimbs. Scale bars for 4x obj. magnification images, 500μm; for 10x, 100μm.

Chapter Five – Characterisation of Svs7 Transgenic Mice
124
0 2 4 6 8
10 12 14 16 18
WT TG
NO
c/B
S (N
/mm
)
Figure 5.9 Bone histomorphometry analysis on NOc/BS (N/mm) of TRAP-stained
non-decalcified femur sections of Svs7 TG mice. Histomorphometry analysis was
performed on TRAP sections of non-decalcified femurs from WT and Svs7 TG mice
described above. No difference was observed in NOc/BS parameter between WT and
Svs7 TG mice. Data are presented as mean ± SEM. Number of mice (n) = 2/group.

Chapter Five – Characterisation of Svs7 Transgenic Mice
125
RANKL stimulation
WT
TG
n.s.
n.s. nn.s.
0
50
100
150
200
250
300
350
Day 0 Day 1 Day 3 Day 5
Num
ber o
f TR
AP+
mul
tinuc
leat
ed c
ells
(≥
3 n
ucle
i)/w
ell
WT
TG
Figure 5.10 Svs7 TG mice exhibit an unaffected osteoclastogenesis in vitro. BM
cells were isolated from long bones of 9-week old WT and Svs7 TG mice and cultured
in M-CSF supplemented complete medium until reaching confluency. The cells were
then seeded into 96-well plates and cultured for 5-day time course RANKL and M-CSF
stimulation with a fresh media change every 2 days. The result showed that there was
no significant difference in osteoclastogenesis between WT and Svs7 TG mice. Hence,
Svs7 TG mice exhibited an unaffected osteoclastogenesis in vitro. Data are presented as
mean ± SEM and are representative of three independent experiments. n.s. = no
significance against WT.

Chapter Five – Characterisation of Svs7 Transgenic Mice
126
Hence, these results have indicated that Svs7 might have a potential role in the
maintenance of bone homeostasis. In the present study, global tissue distribution of
Svs7 mRNA expression revealed that Svs7 was almost exclusively restricted to SV
(including prostate tissue) and a lesser degree in osteoclasts. In an effort to address this,
mice overexpressing the Svs7 transgene were generated by introducing the purified and
linearized pcDNA3.1 Svs7 V5-His transgene into WT mice by blastocysts
microinjection. Svs7 TG mice generation was confirmed by DNA tail tip genotyping
and agarose gel electrophoresis as well as WB analysis on cleared liver lysates from 9-
week old WT and TG mice to confirm the transgenic protein expression of Svs7.
Unfortunately, immunoblot assessment confirmed that there was only a modest increase
in Svs7 protein expression in Svs7 TG mice (about 2.5 fold increase in liver) relative to
WT. Although several factors, including post transcriptional and translational
regulations as well as hormonal change, could affect the relationship between the gene
and protein expression level (King et al. 2012; Levitin et al. 2008), these observations
suggested that global overexpression of Svs7 protein in Svs7 TG mice was only mildly
overexpressed above the endogenous level, which might have excluded the detection of
a clear tissue/bone phenotype in these TG mice.
Despite the modest increase in Svs7 expression in Svs7 TG mice, the assessment of the
gross tissue morphology and the bone phenotype of these mice were persevered. First,
the tissue histology of the prostate (including SV), which has the highest Svs7 gene
expression, was assessed. The result showed that Svs7 TG prostate appeared to have a
normal phenotype relative to that of WT. Hence, from this global tissue phenotype
characterisation study, the Svs7 transgene expression does not appear to affect organs
and tissues phenotype. Furthermore, the normal organ and tissue phenotype observed in
Svs7 TG mice correlated well with their comparable body weight with WT littermates.
To assess the potential bone phenotype of Svs7 TG mice, X-ray analysis on the whole
body and spine of WT and TG mice were performed. The result revealed that there was
no obvious change in skeletons of Svs7 TG mice. These findings were further supported
by the microCT analysis on trabecular bone architecture at proximal tibia, distal femur,
and vertebral body of the lumbar bone of Svs7 TG mice that showed no striking change
in the bone volume architecture at all three sites in these TG mice in reference to WT
counterparts. Moreover, the quantitative analysis on trabecular bone in the secondary
spongiosa region of distal femurs (Lee et al. 2006; Nishikawa et al. 2010) from WT and

Chapter Five – Characterisation of Svs7 Transgenic Mice
127
Svs7 TG mice clearly indicated that TG mice had a normal bone volume architecture,
by showing comparable statistics on all bone parameters (BV/TV (%), Tb.Sp (mm),
Tb.Th (mm), and Tb.N (1/mm)) to WT littermates. As a second standard procedure in
the bone phenotype characterisation, histological examination on both paraffin-
embedded decalcified (H&E stained) and plastic-embedded non-decalcified (goldner
trichrome and TRAP stained) bone samples of WT and Svs7 TG mice was performed.
Both H&E and goldner trichrome-stained sections demonstrated that there were no
marked differences in bone volume and periosteal thickness of the calvarial bone
between WT and Svs7 TG mice, together with no observable change in trabecular bone
architecture and cortical bone in the metaphyseal region of tibia, femur, and lumbar
bones of the TG mice relative to that of WT littermates. In line with the normal bone
mass and architecture observed in Svs7 TG mice, the TRAP sections and bone
histomorphometry data on number of osteoclasts/bone surface parameter showed that
there was no significant difference in the number of TRAP-positive osteoclasts near the
growth plate region between WT and Svs7 TG hindlimbs. These results, along with the
observed findings of unaltered calcium and phosphate serum levels (Supplementary
Figure 1), indicate the presence of healthy bone remodelling process in Svs7 TG mice.
Finally, in order to probe for potential intrinsic cell-specific influences in Svs7 TG
mice, in vitro RANKL-induced osteoclastogenesis assays on WT and TG BMM was
performed. The result revealed that, in reference to WT, indeed Svs7 TG mice exhibited
an unaffected osteoclastogenesis in vitro. Hence in conclusion, Svs7 TG mice showed
no obvious defects in organs and tissues (especially bone) phenotype. Through microCT
analysis and histological examination, Svs7 TG mice showed to have normal bone
volume and architecture. The indication of normal bone remodelling process in Svs7
TG mice to explain the observed phenotype had been illustrated by the histological
TRAP-stained hindlimbs sections, histomorphometry data, unaltered calcium and
phosphate serum levels, and in vitro osteoclastogenesis results that showed an
unaffected osteoclastogenesis in the TG mice. Thus, the Svs7 transgenic strategy did not
allow an accurate assessment of the potential role of Svs7 in bone homeostasis, likely
owing to the modest transgene protein expression of Svs7 in Svs7 TG mice. Therefore,
an alternative knockout strategy was required to gain better insights into the potential
role of Svs7 in the maintenance of bone homeostasis.

128
CHAPTER 6
CHARACTERISATION OF SVS7 KNOCKOUT MICE

Chapter Six – Characterisation of Svs7 Knockout Mice
129
6.1 Introduction Despite the naturally low gene expression of Svs7 in bone, as shown in Chapter 5
Figure 5.1, and with the initial studies that indicate Svs7 gene is upregulated during
RANKL-induced osteoclastogenesis together with other common osteoclast marker
genes (Chapter 2 Figure 2.4), it would be plausible to hold the hypothesis that Svs7 is
an important regulator of osteoclasts and/or osteoblasts differentiation and activation.
By considering that Svs7 is a secreted member of Ly-6 protein family, sharing common
TFP/Ly-6/uPAR motif (Coronel et al. 1992; Levitin et al. 2008; Southan et al. 2002;
Turunen et al. 2011; Ushizawa et al. 2009), and the importance of other Ly-6 members
in many cellular signalling pathways, such as shown by uPAR in αvβ3 integrin
signalling pathway (Schiller et al. 2009; Smith, Marra & Marshall 2008; Wei et al.
2008) and Sca-1, also expressed by osteoclasts (Chapter 2 Figure 2.3), in stem cell
renewal capacity (Bonyadi et al. 2003; Ito et al. 2003), the initial approach and
investigation using Svs7 TG mice was conducted but it had failed to provide accurate
insights into the potential role of Svs7 in the maintenance of bone homeostasis. Svs7
TG mice showed no obvious change in organs and tissues, especially in bone,
phenotype. Normal bone mass and architecture, with the addition of an unaffected
osteoclastogenesis in vitro, were observed in Svs7 TG mice. This might be partly due to
a weak level of Svs7 transgene protein expression in Svs7 TG mice.
Therefore, as an alternative approach to investigate the potential role of Svs7 in
regulating bone homeostasis, Svs7 global knockout (KO) mouse model was generated.
Hence, this chapter focuses on the characterisation of Svs7 global KO mice, with a
particular emphasis on the bone phenotype.
6.2 Results 6.2.1 Genotyping and characterization of Svs7 KO mice
DNA isolated from mouse tail tips was genotyped according to Jackson laboratory’s
DNA isolation protocol, as discussed in Chapter 4 Section 4.3.3, and DNA products
were PCR amplified using specific primers for Svs7 and run on a 1.5% agarose gel.
Figure 6.1A illustrates the 99 amino acids composition of Svs7 protein (Amino (N) to
carboxyl (C) terminal), encoded by 3 exons (each exon is separated by red dot), and the
importance of exon 2 and 3, which together encode for the common TFP/Ly-6/uPAR
domain, consisting of conserved cysteine residues and the consensus C-terminal
sequence motif of CCXXXXCN (‘X’ represents any amino acid and ‘N’ for asparagine

Chapter Six – Characterisation of Svs7 Knockout Mice
130
Svs7
β-actin
WT KO
1 2 3 4
Svs7
KO
Het
WT
NE
G
Exon 1 Exon 2 Exon 3
SP C-C-C-C-C
C-C-C-C-CN
Poly (A)
TFP/Ly-6/uPAR domain
Svs7 protein (99 aa):
MNSVTKISTLLIVILSFLCFVE.GLICNSCEKSRDSRCTMSQSRCVAKPGESCSTVS
HFV.GTKHVYSKQMCSPQCKEKQLNTGKKLIYIMCCEKNLCNSF
(A)
(B) (C)
Figure 6.1 Svs7 gene and protein were absent in Svs7 KO mice. (A) (Top panel)
Svs7 amino acids composition, encoded by 3 exons (each exon is separated by red rot),
showing consensus cysteine (red highlighted letter ‘C’) residues and the consensus C-
terminal sequence motif CCXXXXCN (‘X’ for any amino acid and ‘N’ for asparagine),
and (Bottom panel) the structure of Svs7 gene with exon 2 and 3 encoding for TFP/Ly-
6/uPAR domain (The structure of Svs7 gene was illustrated by Levitin et al. 2008). (B)
Agarose gel electrophoresis of mouse tail tip DNA genotyping product showing that the
deletion of exon 2 and 3 of Svs7 gene in Svs7 KO mice (lane 2) had produced a smaller
DNA product compared to WT (lane 1). (C) WB protein analysis on WT and Svs7 KO
seminal vesicle lysates showed that there was no Svs7 protein detected in the KO lysate.
β-actin served as a loading control.

Chapter Six – Characterisation of Svs7 Knockout Mice
131
residue) (Levitin et al. 2008). Deletion of these exons was confirmed by DNA analysis
using agarose gel electrophoresis. As shown in Figure 6.1B, Svs7 KO (lane 2) produced
a smaller DNA product compared to WT (lane 1), indicating that the exons had been
successfully deleted. To confirm Svs7 deletion at the protein level, western blot (WB)
analysis on seminal vesicle (SV) lysates from WT and Svs7 KO mice was performed.
As anticipated, the loss of exon 2 and 3 within Svs7 gene resulted in the complete
absence of Svs7 protein in Svs7 KO lysate, as shown in Figure 6.1C. β-actin served as a
loading control. Together, these results validate the deletion of Svs7 in Svs7 KO mice.
6.2.2 Slow mice breeding process and gross body phenotypic examination of Svs7
KO mice
Following the generation of heterozygous (Het) mice, the breeding process was
continued by setting up Het x Het crossing to produce WT and Svs7 KO littermates. As
shown in Figure 6.2A, amongst 71 newborn pups (39 for male and 32 for female), the
ratio of getting male WT and female Svs7 KO mice were only 12% and 16%
respectively, which are significantly lower than the expected 25% (Mendelian ratio),
suggesting that there was a slow breeding process and hence difficulty in getting
adequate WT and KO pairs littermates for both male and female pups. The possible
outcome of this slow mice breeding process was then investigated by first examining
the gross body phenotype of age- and sex-matched WT and Svs7 KO pairs littermates.
To achieve this, 12-week old WT and Svs7 KO mice were sacrificed and the two bodies
were laid side-by-side for examination and the representative images were taken. The
result depicted that there was no apparent defect in the gross body phenotype of Svs7
KO mice compared to WT in the same litter (Figure 6.2B). Collectively, although there
was a slow mice breeding process, Svs7 KO mice appeared to be similar in body size as
WT littermates.
6.2.3 Gross tissues phenotypic (macro vs. microscopic) assessment of Svs7 KO mice
To continue with the gross organs and tissues phenotype characterization of Svs7 KO
mice, 12-week old WT and KO pair littermates were sacrificed and general organs and
tissues were dissected from both mice and placed side-by-side for careful macroscopic
examination. The result showed that, in relative to WT, Svs7 KO organs and tissues
were comparable (Figure 6.3A). Furthermore, histology-prepared prostate (including
seminal vesicle) sections from WT and Svs7 KO mice were H&E stained for
microscopic assessment. No obvious difference in prostate tissue phenotype was

Chapter Six – Characterisation of Svs7 Knockout Mice
132
0
10
20
30
40
50
60
70
WT Het KO
Perc
enta
ge o
f mal
e pu
ps
0 5
10 15 20 25 30 35 40 45 50
WT Het KO
Perc
enta
ge o
f fem
ale
pups
(A)
(B) WT KO
Figure 6.2 Slow mice breeding process and gross body phenotypic examination of
Svs7 KO mice. (A) Amongst 71 newborn pups (39 for male and 32 for female), the
ratio of getting male WT and female Svs7 KO mice were 12% and 16% respectively,
which are well below than the expected 25%, suggesting that there was a slow mice
breeding process and subsequent difficulty in getting adequate WT and KO pairs
littermates for both male and female mice for experiments. (B) Twelve-week old WT
and Svs7 KO mice were sacrificed and laid side-by-side for gross body phenotypic
examination. The result showed that Svs7 KO mice appeared to be similar in body size
as WT littermates.

Chapter Six – Characterisation of Svs7 Knockout Mice
133
WT KO WT KO WT WT WT WT
WT WT WT WT WT
WT WT WT
KO KO KO KO
KO KO KO KO KO
KO KO KO
Tibia SV
(prostate) Testis Brain Heart Thymus
Lung Spleen Liver Stomach Kidney
Intestine Fat Ovary
WT KO
500μm 500μm
(A)
(B)
Figure 6.3 Gross tissues phenotypic assessment of Svs7 KO mice. (A) Organs and
tissues were extracted from 12-week old WT and Svs7 KO mice and placed side-by-
side for macroscopic examination. The result showed that Svs7 KO organs and tissues
were comparable to that of WT. (B) Prostates (including seminal vesicle) were extracted
from WT and Svs7 KO mice, fixed, processed, embedded, sectioned, and H&E stained
for histological assessment. The result depicted that there was no obvious difference in
prostate tissue phenotype between WT and Svs7 KO mice. Hence, the loss of the Svs7
gene did not appear to affect the organogenesis in Svs7 KO mice. Scale bars, 500μm.

Chapter Six – Characterisation of Svs7 Knockout Mice
134
observed between WT and Svs7 KO mice (Figure 6.3B). Together, these results
suggested that the deletion of the Svs7 gene did not appear to affect the organogenesis
in Svs7 KO mice.
6.2.4 Svs7 KO mice exhibit a reduced bone mass phenotype
As an initial step toward characterising the potential bone phenotype of Svs7 KO mice,
femurs were extracted from 15- and 30-week old WT and Svs7 KO mice, fixed, and
processed for microCT analysis, as detailed in Chapter 4 Section 4.3.4. Initially, no
striking phenotype was observed in Svs7 KO mice. Mice grew at lower ratio than the
expected without gross abnormality was observed. However, Svs7 KO mice exhibited a
progressive decline in bone mass with age as compared to WT littermates. The 2D and
3D microCT images of distal femurs from WT and Svs7 KO mice showed that Svs7
KO mice appeared to have less trabecular bone volume compared to WT littermates
(Figure 6.4A). Indeed, through the quantitative analysis on trabecular bone in secondary
spongiosa region (Lee et al. 2006; Nishikawa et al. 2010) of both WT and Svs7 KO
femurs, it was then revealed that KO bones had significantly lower bone/tissue volume
(BV/TV (%)) in both age (15- and 30-week old) groups and a significantly less
trabecular number (Tb.N (1/mm)) in the 30-week old group compared to WT (Figure
6.4B). However, there were no significant differences in trabecular separation (Tb.Sp
(mm)) and trabecular thickness (Tb.Th (mm)) in both age groups between WT and Svs7
KO mice (Figure 6.4B). Together, these results imply that Svs7 KO mice exhibit a
phenotype of osteopenia/osteoporosis.
6.2.5 Svs7 KO bone histology
The reduced bone volume in Svs7 KO mice prompted us to conduct a close examination
of the bone phenotype using histology and histomorphometry analysis. For this,
histology sections of decalcified femurs from 12-week old WT and Svs7 KO mice were
H&E and TRAP (as an osteoclast marker; red precipitates) stained. The H&E-stained
sections showed that, indeed, Svs7 KO femurs seemed to have less trabecular bone
volume in the secondary spongiosa region than WT (Figure 6.5A). In accordance with
this result, TRAP-stained sections depicted that Svs7 KO hindlimbs appeared to have a
trend of increase in the number of TRAP-positive osteoclasts near the growth plate
region compared to WT (Figure 6.5B). The bone histomorphometry analysis on TRAP-
stained femurs sections from WT and Svs7 KO mice for the number of

Chapter Six – Characterisation of Svs7 Knockout Mice
135
WT KO
0.02
0.04
0.06
15wk 30wk
Tb.T
h (m
m)
2
6
10
14
18
15wk 30wk
BV
/TV
(%)
1
2
3
4
5
15wk 30wk
Tb N
(1/m
m)
0.05 0.1 0.15 0.2 0.25 0.3
15wk 30wk
Tb S
p (m
m)
WT KO
n.s. n.s.
n.s. n.s.
n.s.
(A)
(B)

Chapter Six – Characterisation of Svs7 Knockout Mice
136
Figure 6.4 Svs7 KO mice exhibit a reduced bone mass phenotype. (A) 2D and 3D
(longitudinal and cross sections) microCT images of distal femurs from 15- and 30-
week old WT and Svs7 KO mice showed that the KO mice appeared to have less
trabecular bone volume compared to WT. (B) The quantitative microCT analysis on
bone parameters of femurs from 15- and 30-week old WT and Svs7 KO mice revealed
significantly reduced BV/TV (in both age groups) and trabecular number (Tb.N) (only
in the 30-week old mice) in Svs7 KO mice compared to WT. There were no significant
differences in trabecular separation (Tb.Sp) and trabecular thickness (Tb.Th) between
WT and Svs7 KO mice in both age groups. Hence, Svs7 KO mice exhibit a phenotype
of osteopenia/osteoporosis. Data are presented as mean ± SEM. * p < 0.05, n.s. = no
significance against WT. Scale bars, 500μm.

Chapter Six – Characterisation of Svs7 Knockout Mice
137
WT KO
H&
E TR
AP
(10x
obj
.) TR
AP
(20x
obj
.) (A)
(B)

Chapter Six – Characterisation of Svs7 Knockout Mice
138
Figure 6.5 Svs7 KO bone histology. (A) Fixed and decalcified femurs sections from
12-week old WT and Svs7 KO mice were H&E stained. The result showed that Svs7
KO hindlimbs appeared to have less trabecular bone volume in the secondary spongiosa
region compared to WT. (B) (Top panel) 10x and (Bottom panel) 20x objective
magnifications of representative images of TRAP (osteoclasts stained red)-stained WT
and Svs7 KO femurs sections showed a trend of increase in the number of TRAP-
positive osteoclasts near the growth plate region in KO hindlimbs relative to WT. Scale
bars for 4x obj. H&E sections, 500μm; for 10x and 20x obj. TRAP sections, 100μm.

Chapter Six – Characterisation of Svs7 Knockout Mice
139
osteoclasts/bone surface (NOc/BS (N/mm)) similarly indicated that there was a trend of
increase in TRAP-positive osteoclasts number in the KO hindlimbs compared to WT
(Figure 6.6). Therefore, the bone histology sections of Svs7 KO mice supported the
MicroCT data that there was a reduced bone volume and a trend of increase in the
number of TRAP-positive osteoclasts in Svs7 KO hindlimbs.
6.2.6 Bone formation activity in vivo is unaffected in Svs7 KO mice
To further characterize the Svs7 KO bone phenotype, double calcein labelling was
performed. For this purpose, 12-week old WT and Svs7 KO mice were subjected to the
calcium-binding fluorescent dye, calcein, injection. Calcein is incorporated into the
newly mineralized tissues and hence by giving the mice two injections (two labels)
seven days apart and measuring the distance between two labels using ImageJ software
(after images were taken using confocal microscopy), the difference in bone formation
activity (mineral apposition rate (MAR)) in vivo between WT and Svs7 KO mice can be
deduced. Analysis of plastic-embedded non-decalcified tibia sections from WT and
Svs7 KO mice by confocal microscopy (Figure 6.7A) and MAR measurement (Figure
6.7B) showed that there was no significant difference in bone formation activity in vivo
between WT and KO mice. Hence, Svs7 KO mice exhibit an unaffected bone formation
activity in vivo.
6.3 Discussion This study builds upon our previous observations that Svs7 is exclusively expressed by
mature osteoclasts but not by osteoblasts or other key bone cells and its gene expression
is upregulated during RANKL-induced osteoclastogenesis (as discussed in Chapter 2
Section 2.4 Figure 2.4). Here to directly address the possible role of Svs7 in bone
homeostasis, which had failed to be shown in our first approach and study using Svs7
TG mice, we generated Svs7-deficient mice. Svs7 KO mice generation was achieved by
the deletion of exon 2 and 3 of Svs7 gene. This deletion was then confirmed by DNA
tail tip genotyping and immunoblotting for Svs7 protein in Svs7 KO seminal vesicle
lysate, which demonstrated that Svs7 protein expression was lost in these KO mice.
Assessment of Svs7 KO mice breeding revealed that the ratio of male WT and female
Svs7 KO mice were well below 25% (12% and 16% respectively), which consequently
limited both the sample size and number of assays available for assessment. Although

Chapter Six – Characterisation of Svs7 Knockout Mice
140
0
2
4
6
8
10
12
WT KO
NO
c/B
S (N
/mm
) n.s.
Figure 6.6 Bone histomorphometry analysis on TRAP-stained decalcified femur
sections of Svs7 KO mice. Fixed and decalcified femurs sections from 12-week old
WT and Svs7 KO mice were TRAP stained and number of osteoclasts/bone surface
(NOc/BS (N/mm)) parameter was analysed. The result revealed that there was a trend of
increase in the number of TRAP-positive osteoclasts in Svs7 KO hindlimbs compared
to WT. Data are presented as mean ± SEM. Number of mice (n) = 3/group. n.s. = no
significance against WT.

Chapter Six – Characterisation of Svs7 Knockout Mice
141
0 0.2 0.4 0.6 0.8
1 1.2 1.4 1.6 1.8
2
WT KO
MA
R (μ
m/d
ay)
WT KO (A)
(B) n.s.
Figure 6.7 Svs7 KO mice exhibit an unaffected bone formation activity in vivo. (A)
Calcein double labelling confocal microscopy images of plastic-embedded non-
decalcified tibia sections from 12-week old WT and Svs7 KO mice showed that there
was no striking difference in bone formation activity between WT and KO mice. (B)
MAR analysis by measuring the distance between the two calcein labels (in each
section) revealed that there was no significant difference in bone formation activity in
vivo between WT and Svs7 KO mice. Hence, Svs7 KO mice exhibit an unaffected bone
formation activity in vivo. Data are presented as mean ± SEM and are representative of
three independent experiments. n.s. = no significance against WT. Scale bars, 10μm.

Chapter Six – Characterisation of Svs7 Knockout Mice
142
the precise reason for this is unclear, it may imply an important role of Svs7 in seminal
vesicle and fertility, which has been previously suggested by Coronel et al. 1992 that
Svs7 inhibits calcium (Ca2+) influx across the membrane of sperm cells during
fertilization to prevent premature acrosomal reaction and spermatozoa hyperactivation.
Despite this breeding limitation, the examination of the gross phenotype of body,
organs, and tissues, including histological assessment on prostate (the tissue which has
the highest Svs7 gene expression, as shown in Chapter 5 Figure 5.1), of Svs7 KO mice
relative to WT littermates (age- and sex-matched pairs) was successfully achieved. The
results showed that there were no apparent differences in body, organs, and tissues gross
phenotype between WT and Svs7 KO mice. Hence, the loss of the Svs7 gene does not
appear to affect the gross phenotype (macro- and microscopic) of body, organs, and
tissues of Svs7 KO mice.
Moreover, microCT analysis on trabecular bone volume and architecture in the
secondary spongiosa region of distal femurs from 15- and 30-week old WT and Svs7
KO mice (Lee et al. 2006; Nishikawa et al. 2010) revealed that the KO mice had
significantly reduced trabecular bone/tissue volume (BV/TV) at both age groups
compared to WT littermates. Consistently, there was a significant reduction in
trabecular number (Tb.N) in Svs7 KO hindlimbs, even though only in the 30-week old
mice group. The possibility that Svs7 KO mice exhibit a progressive decline in bone
mass with age, as compared to WT littermates, could play a significant role in this
microCT analysis. In line with these microCT results, H&E-stained sections of
decalcified femurs from 12-week old WT and Svs7 KO mice showed that there was an
obvious decrease in trabecular bone volume in the secondary spongiosa region of KO
hindlimbs relative to that of WT littermates. Subsequently, TRAP-stained sections and
bone histomorphometry analysis on the number of osteoclasts/bone surface (NOc/BS)
indicated that there was a trend of increase in the number of TRAP-positive osteoclasts
near the growth plate region of Svs7 KO hindlimbs compared to WT littermates.
Collectively, these results suggest that Svs7 KO mice exhibit a phenotype of reduced
bone mass (osteopenia/osteoporosis) and a trend of increase in osteoclasts number in
vivo, which could strongly indicate an alteration in osteoclast differentiation and/or
activation in the KO mice.
To further explore the possible cause of the reduced bone mass phenotype in Svs7 KO
mice, osteoblastic bone formation activity in vivo was investigated by performing

Chapter Six – Characterisation of Svs7 Knockout Mice
143
double calcein labelling (Hayashi et al. 2012) in 12-week old WT and Svs7 KO mice
and measuring the distance between two labels on the images of calcein-labelled plastic
embedded non-decalcified tibia sections to calculate mineral apposition rate (MAR).
The result showed that there was no significant difference in MAR between WT and
Svs7 KO mice. Hence, this finding indicates that Svs7 KO mice exhibit an unaffected
bone formation activity in vivo and that the alteration in osteoclast differentiation and/or
activation might be the major contributor to the osteoporotic phenotype observed in
Svs7 KO mice.
In conclusion, Svs7, a novel osteoclast-secreted factor (Supplementary Figure 2),
appears to be a candidate regulator of bone homeostasis. Svs7 KO mice exhibit an
osteopenic/osteoporotic phenotype and an unaffected bone formation activity in vivo,
but an elevated osteoclast number in KO hindlimbs suggests that Svs7 might influence
bone homeostasis via the regulation of osteoclast differentiation and/or activity.

144
CHAPTER 7
INVESTIGATION OF INTRINSIC CELLULAR MECHANISM IN
SVS7 KNOCKOUT MICE (OSTEOCLAST AND
OSTEOBLAST)

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
145
7.1 Introduction Bone homeostasis is achieved by balanced activities between bone-resorbing osteoclast
and bone-forming osteoblast. Various cytokines, proteins, and growth factors are
expressed and/or secreted by both osteoclasts and osteoblasts in a regulated manner to
create intercellular communication and regulation, crucial for the differentiation and
activation of each cell. RANKL and M-CSF, produced by osteoblasts, are two essential
cytokines for driving osteoclast differentiation and activation (Kodama et al. 1991;
Takahashi, Udagawa & Suda 1999). On the other hand, osteoclasts release the active
form of IGF-II from bone matrix during its bone resorption activity to stimulate and
initiate site-specific bone formation by osteoblasts (Hayden, Mohan & Baylink 1995).
Thus, an imbalance in this coupling system, which could come from defects in either or
both osteoclasts and osteoblasts, may lead to the development of many pathological
bone diseases, such as osteoporosis (reduced bone mass) and osteopetrosis (increased
bone mass).
The results presented in Chapter 6 demonstrate that Svs7 KO mice exhibit a reduced
bone mass phenotype, consistent with osteopenia/osteoporosis. Since osteoporosis is
attributed to an excessive bone resorption by osteoclasts (Riggs & Melton 1983) and/or
a decline in bone formation activity by osteoblasts (Manolagas & Jilka 1995), these
observations imply that the changes in osteoclasts and/or osteoblasts number and/or
activity might account for the reduced bone mass phenotype observed in Svs7 KO mice.
To address this, the present chapter focuses on the in vitro characterization of
osteoclasts (including their bone marrow macrophages (BMM) progenitors) and
osteoblasts from Svs7 KO mice. Parameters explored include Svs7 KO osteoclasts and
osteoblasts differentiation and activity and osteoclast fusion mechanism.
In addition, it has been well documented that calcium (Ca2+) signalling is essential in
the activation of NFATc1, the master regulator of osteoclastogenesis (Takayanagi et al.
2002). Amongst other osteoclast genes that are known to be transcriptionally regulated
by NFATc1, such as TRAP, cathepsin K, c-Src, and β3 integrin (Crotti et al. 2006;
Ikeda et al. 2006; Matsumoto et al. 2004; Takayanagi et al. 2002), it has been shown
that NFATc1 also crucially regulates fusion-mediating genes activation in osteoclasts,
which are DCSTAMP and ATP6v0d2 genes (Kim et al. 2008; Lee et al. 2006; Yagi et
al. 2005). In general, mononuclear preosteoclasts fuse together to become
multinucleated cells, which takes place around day 3 of RANKL-induced osteoclast

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
146
differentiation (osteoclastogenesis) and upon further RANKL stimulation they become
active and functional bone resorbing cells (Fujita et al. 2012; Kim et al. 2008). NFATc1
has been shown to bind to the promoter region of both fusogenic genes to induce their
expression. The inactivation of NFATc1 decreases the expression of these fusogenes
and attenuates osteoclast fusion (Kim et al. 2008). Hence, the overexpression of
ATP6v0d2 and DCSTAMP genes has been shown to rescue the NFATc1-deficient
osteoclast fusion defect (Kim et al. 2008). As Svs7 is known to regulate Ca2+ influx
across the membrane of sperm cells during fertilization (Coronel et al. 1992), it was
then plausible to investigate the potential role of Svs7 in Ca2+-NFATc1 signalling
pathway, particularly in the regulation of osteoclast fusion mechanism. Through a series
of in vitro experiments, the findings in this chapter indicate that Svs7 plays a role in
regulating osteoclast fusion through the NFATc1 signalling pathway.
7.2 Results – Part 1: Intrinsic cellular mechanism in osteoclasts
derived from Svs7 KO mice 7.2.1 Svs7 KO BMM cultures have increased osteoclastogenesis in vitro
First, the histomorphometry results obtained from Svs7 KO hindlimbs indicated that
there was a trend of increase in osteoclast number in vivo. Based on this observation, we
speculated that the reduced bone mass phenotype observed in Svs7 KO mice might be
due to an alteration in osteoclast differentiation and/or activation. To assess osteoclast
formation in Svs7 KO mice, in vitro 5-day time course (day 0, 1, 3, and 5) RANKL and
M-CSF-induced osteoclastogenesis assays on WT and KO bone marrow (BM) cells
were performed. At the end of the time course, the cells were fixed, TRAP stained and
osteoclasts (TRAP-positive cells having ≥ 3 nuclei) were counted. The result showed
that at day 3 and 5 of osteoclastogenesis, there were significantly more TRAP-positive
osteoclasts in Svs7 KO cultures compared to WT (Figure 7.1). Hence, in vitro
osteoclastogenesis was increased in Svs7 KO mice.
7.2.2 Svs7 KO osteoclasts are larger and have more nuclei than WT
Further investigation in in vitro osteoclastogenesis assay results showed that Svs7 KO
osteoclasts exhibited significantly larger spread area than WT at day 5 of RANKL-
induced osteoclastogenesis (Figure 7.2). Although there was no significant difference at
day 3 between WT and Svs7 KO osteoclasts (Figure 7.2), these results indicate that the
KO cells have an accelerated fusion process during differentiation. To further assess
this, osteoclasts were separated into three groups based on the number of nuclei per

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
147
0
20
40
60
80
100
120
140
160
180
Day 0 Day 1 Day 3 Day 5
Num
ber o
f TR
AP+
mul
tinuc
leat
ed c
ells
(≥
3 n
ucle
i)/w
ell
RANKL stimulation
WT
KO
WT
KO
Figure 7.1 In vitro time course RANKL-induced Svs7 KO BMM differentiation
into mature osteoclasts. BM cells from 12-week old WT and KO mice were cultured
for 5-day time course in the presence of M-CSF and RANKL with a fresh media change
every 2 days. Upon formation of osteoclasts, TRAP stain and osteoclast count were
performed. Svs7 KO cultures showed a significant increase in osteoclastogenesis
compared to WT at day 3 and 5 of RANKL-induced osteoclastogenesis. Data are
presented as mean ± SEM and are representative of three independent experiments. ** p
< 0.01 against WT. Scale bars, 100μm.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
148
0
10000
20000
30000
40000
50000
WT KO
Aver
age
OC
are
a (μ
m2 )
at d
ay 5
of
Ost
eocl
asto
gene
sis
0 2000 4000 6000 8000
10000 12000 14000 16000 18000
WT KO
Aver
age
OC
are
a (μ
m2 )
at d
ay 3
of
Ost
eocl
asto
gene
sis
n.s.
Figure 7.2 Svs7 KO osteoclasts are larger than WT. Analysis of osteoclast spread
area at day 3 and 5 of RANKL-induced osteoclastogenesis revealed that Svs7 KO
osteoclasts were significantly larger than WT at day 5 of osteoclastogenesis (Bottom
panel), while there was no significant difference at day 3 between both cells (Top
panel). Data are presented as mean ± SEM and are representative of three independent
experiments. * p < 0.05, n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
149
osteoclast (having 3-5, 6-10, or ≥ 11 nuclei), which were then added together and
expressed as a ratio to total TRAP-positive multinucleated cells per well. Based on this
quantification method, there were significantly more large osteoclasts, having ≥ 11
nuclei, in Svs7 KO cultures compared to WT at day 5 of osteoclastogenesis (Figure
7.3). These findings suggest that Svs7 might play a role in regulating osteoclast fusion.
7.2.3 WT and Svs7 KO mice have comparable hematopoietic stem cells (HSCs) and
osteoclast progenitor cells
As an increase in osteoclastogenesis was observed in Svs7 KO mice, it was then of
interest to further investigate the early lineage negative (Lin-) osteoclast precursor
(CD45R- CD3e- CD11b-/low) (Jacquin et al. 2006) and subsequent HSCs population (Lin-
Sca-1+ c-Kit+/LSK) (Kollet et al. 2006; Lymperi et al. 2011; Miyamoto et al. 2011) in
BM population of WT and Svs7 KO mice. To explore this, 12-week old WT and KO
mice were sacrificed and BM cells were then isolated from their long bones. Following
red blood cell lysis procedure, the cells were counted, antibodies were prepared in
master mix with the required dilutions, followed by cell incubation with antibodies and
overnight fixation, as detailed in Chapter 4 Section 4.7.3. Flow cytometry analysis was
performed on the following day using FACS Canto at CMCA, UWA. As shown in
Figure 7.4A, both WT and Svs7 KO BM had no significant differences in both HSCs
and early osteoclast progenitor populations.
Next, BM osteoclast progenitor proliferation was assessed. For this purpose, BM cells
were cultured in complete medium supplemented with M-CSF for 48 hours and were
subjected to MTS proliferation assay, which measures the metabolic activity of the
viable cells through the absorbance of the formazan product at 490nm excitation
wavelength. The result showed that there was no significant difference in proliferation
rate between WT and Svs7 KO BM osteoclast precursors over both 24 and 48 hours
time points (Figure 7.4B), which therefore implied that the loss of the Svs7 gene did not
alter the regulation of HSCs and early osteoclast precursor population and proliferation.
As early osteoclast precursor proliferation, growth, and survival is primarily mediated
by the mitogen-activated protein kinases (MAPKs) signalling pathway upon RANKL
stimulation, which includes ERK, c-Jun N-terminal Kinase (JNK), and p38 (Cobb &
Goldsmith 1995; Teitelbaum 2000), cell lysates of WT and Svs7 KO BM osteoclast
precursors, stimulated for an hour (0, 5, 10, 20, 30, and 60 minutes time points) with

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
150
0 0.2 0.4 0.6 0.8
1
WT KO WT KO WT KO
#3-5 #6-10 #11+ Rat
io to
tota
l num
ber o
f TR
AP+
mul
tinuc
leat
ed c
ells
(≥
3 n
ucle
i) (p
er w
ell)
Nuclei number at day 3 of osteoclastogenesis
0 0.2 0.4 0.6 0.8
1
WT KO WT KO WT KO
#3-5 #6-10 #11+ Rat
io to
tota
l num
ber o
f TR
AP+
mul
tinuc
leat
ed c
ells
(≥
3 n
ucle
i) (p
er w
ell)
Nuclei number at day 5 of osteoclastogenesis
n.s.
n.s. n.s.
n.s.
n.s.
Figure 7.3 Svs7 KO osteoclasts have more nuclei than WT. Analysis of number of
osteoclasts (based on their nuclei number) in ratio to total number of TRAP-positive
multinucleated cells showed that indeed Svs7 KO cultures had significantly more large
osteoclasts, having ≥ 11 nuclei, than WT at day 5 of osteoclastogenesis, which perfectly
correlates with the osteoclast spread area analysis described above. At day 3 of
osteoclast differentiation, both WT and Svs7 KO cultures had similar distribution of
osteoclast sizes. These findings suggest that Svs7 might play a role in the regulation of
osteoclast fusion. Data are presented as mean ± SEM and are representative of three
independent experiments. * p < 0.05, n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
151
(A)
(B)
0 5
10 15 20 25 30
WT KO
% o
f CD
11blo
w/C
D3e
- /CD
45R- (
Lin- )/
tota
l cel
ls
0
0.5
1
1.5
WT KO
% o
f Lin
- Sca
-1+ c
-Kit+
(LSK
) HSC
s/tot
al ce
lls n.s.
n.s.
0
5
10
15
20
25
30
35
40
24hrs 48hrs
Est
imat
ed c
ell c
umbe
r (x
103 )
Cell Proliferation
WT
KO
n.s.
n.s.
Figure 7.4 Svs7 KO mice exhibit unaltered population of HSCs and early
osteoclast precursor. (A) BM cells were extracted from long bones of 12-week old WT
and KO mice, followed by cell incubation with fluorophore-conjugated antibodies and
overnight fixation. Flow cytometry analysis was performed on the following day, which
revealed that there were no significant differences in Lin- early osteoclast precursor
(Left panel) and Lin- Sca-1+ c-Kit+ (LSK) HSCs population (Right panel) between WT
and Svs7 KO mice. (B) MTS proliferation assays on WT and Svs7 KO BM osteoclast
precursors showed that there was no significant difference in proliferation rate between
WT and KO cells over period of 24 and 48 hours time points. These findings suggested
that the loss of the Svs7 gene did not affect the regulation of HSCs and early osteoclast
precursor population and proliferation. Data are presented as mean ± SEM and are
representative of three independent experiments. n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
152
RANKL (50ng/ml), were subjected to WB analysis to explore the MAPK and IκB
(inhibitor of NF-κB) α signalling pathways. As shown in Figure 7.5A (WB result) and
B (densitometry analysis), there was no significant difference in the phosphorylation
(activation) of ERK, JNK, or p38 as well as in the IκBα degradation (NF-κB activation)
between WT and Svs7 KO mice, suggesting that the deletion of the Svs7 gene does not
affect early MAPK and NF-κB signalling pathways in osteoclast progenitor.
7.2.4 Svs7 KO mice exhibit unaltered expression levels of key osteoclast marker
genes
Next, the expression of osteoclast marker genes in Svs7 KO mice was examined. WT
and KO BM cells were extracted from long bones and, upon confluency, were cultured
for 5-day time course with RANKL and M-CSF stimulation. RNA was then extracted,
followed by reverse transcription (RT) and conventional semi-quantitative PCR
reactions. Forward and reverse primers for CTR, TRAP, NFATc1, DCSTAMP, and
ATP6v0d2 were run alongside Svs7 and β-actin as a loading control. As shown in
Figure 7.6A (agarose gel electrophoresis) and B (densitometry analysis), both WT and
Svs7 KO mice had comparable expression levels of key osteoclast marker genes, which
indicated that despite the increase in osteoclast number and size, the loss of the Svs7
gene did not alter the expression of key osteoclast marker genes.
7.2.5 Osteoclast bone resorption activity is not affected in Svs7 KO mice
To examine osteoclast activity, WT and Svs7 KO BMM-derived mature osteoclasts
cultured in collagen-coated 6-well plates, were detached and seeded onto bone slices
and cultured for 48 hours in RANKL-supplemented medium to initiate bone resorption.
An independent method using Corning osteo assay plates (containing bone
(hydroxyapatite)-like material), after the initial mature osteoclast culture in the
collagen-coated 6-well plates, was also performed, as described in Chapter 4 Section
4.5.3. After 48 hours, cells on either bone slices or Corning osteo assay wells were
fixed, TRAP stained, and number of osteoclasts per bone slice was counted, the surface
of bone slices was then visualised under scanning electron microscopy (SEM) and for
the Corning osteo wells the Nikon Microscope Ti was used to observe resorption pits.
By dividing the total resorbed area with the total osteoclast number on each sample,
resorbed pit area/cell result was then recorded as a representative of the osteoclast bone
resorption activity in WT and Svs7 KO mice. As shown in Figure 7.7 (SEM analysis)
and Figure 7.8 (Corning osteo plate analysis), there was no significant difference in the

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
153
0 5 10 20 30 60 0 5 10 20 30 60 WT KO
RANKL Stimulation mins
p-ERK1/2
β-actin
p-p38
p-JNK
IkBα
ERK1/2
p38
JNK
(A)
(B)
0 0.2 0.4 0.6 0.8
1 1.2 1.4 1.6
0 5 10 20 30 60
p-ER
K1/
2 ra
tio to
ER
K1/
2
RANKL stimulation (minute)
WT
KO
n.s. n.s.
n.s.
n.s.
n.s. n.s. WT
O
0
0.2
0.4
0.6
0.8
1
1.2
0 5 10 20 30 60
p-p3
8 ra
tio to
p38
RANKL stimulation (minute)
WT
KO
n.s. n.s. n.s. n.s. n.s.
n.s.
0 0.1 0.2 0.3 0.4 0.5 0.6 0.7 0.8
0 5 10 20 30 60
p-JN
K ra
tio to
β-a
ctin
RANKL stimulation (minute)
WT
KO
n.s. n.s.
n.s. n.s.
n.s. n.s. WT
O
0
0.2
0.4
0.6
0.8
1
1.2
0 5 10 20 30 60
IκB
α ra
tio to
β-a
ctin
RANKL stimulation (minute)
WT
KO
n.s. n.s. n.s.
n.s. n.s.
n.s.
Figure 7.5 The deletion of the Svs7 gene does not affect MAPK and NF-κB
signalling pathways in Svs7 KO osteoclast precursor. (A) Cell lysates of WT and
Svs7 KO BM osteoclast precursors, which were given short (an hour) RANKL
stimulation, were subjected to WB analysis and immunoblotted with specific antibodies
against MAPKs (ERK, JNK, and p38) and IκBα. MAPKs activation (phosphorylation)
and IκBα degradation appeared to be unaffected in Svs7 KO mice. (B) Densitometry
analysis was performed using ImageJ software and revealed that there was no
significant difference in the phosphorylation (activation) of ERK, JNK, or p38 as well
as in the IκBα degradation between WT and Svs7 KO mice, suggesting that the deletion
of the Svs7 gene does not affect early MAPK and NF-κB signalling pathways in
osteoclast progenitor. Data are presented as mean ± SEM and are representative of four
independent experiments. n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
154
β-actin
NFATc1
Svs7
ATP6v0d2
TRAP
CTR
DCSTAMP
0 1 3 5
RANKL-stimulated
BMM day 0 1 3 5
WT KO (A)
(B)
0 0.1 0.2 0.3 0.4 0.5 0.6 0.7 0.8
Day 0 Day 1 Day 3 Day 5
Svs7
gen
e ex
pres
sion
(ratio
to β
-act
in)
RANKL stimulation
WT
KO n.s. n.s.
0
0.1
0.2
0.3
0.4
0.5
Day 0 Day 1 Day 3 Day 5
CTR
gene
expr
essio
n (ra
tio to
β-a
ctin)
RANKL stimulation
WT
KO n.s. n.s.
n.s.
n.s.
0
0.2
0.4
0.6
0.8
1
1.2
Day 0 Day 1 Day 3 Day 5
TRAP
gen
e exp
ress
ion
(ratio
to β
-acti
n)
RANKL stimulation
WT
KO n.s.
n.s.
n.s. n.s.
0 0.1 0.2 0.3 0.4 0.5 0.6 0.7 0.8
Day 0 Day 1 Day 3 Day 5
NFA
Tc1
gene
expr
essio
n (ra
tio to
β-a
ctin
)
RANKL stimulation
WT
KO
n.s. n.s.
n.s. n.s.
0
0.2
0.4
0.6
0.8
1
1.2
1.4
Day 0 Day 1 Day 3 Day 5
DCS
TAM
P ge
ne e
xpre
ssio
n (ra
tio to
β-a
ctin
)
RANKL stimulation
WT
KO n.s.
n.s. n.s. n.s.
0 0.1 0.2 0.3 0.4 0.5 0.6 0.7 0.8
Day 0 Day 1 Day 3 Day 5
ATP6
v0d2
gen
e exp
ress
ion
(ratio
to β
-acti
n)
RANKL stimulation
WT
KO
n.s. n.s.
n.s. n.s.
Figure 7.6 Key osteoclast marker genes expression levels are not affected in Svs7
KO mice. (A) RNA of 5-day time course RANKL and M-CSF-stimulated WT and Svs7
KO BM cells was extracted and subjected to RT and semi-quantitative PCR reactions
with specific forward and reverse primers for Svs7 and key osteoclast marker genes
(CTR, TRAP, NFATc1, DCSTAMP, and ATP6v0d2). β-actin was used as a house-
keeping gene. The result showed that there were comparable expression levels of the
osteoclast marker genes between WT and Svs7 KO mice. (B) Densitometry analysis
was then performed using ImageJ software and it revealed that there were no significant
differences in the key osteoclast marker genes expression levels between WT and Svs7
KO mice (with the confirmation that Svs7 gene was absent in Svs7 KO mice). Data are
presented as mean ± SEM and are representative of four independent experiments. ** p
< 0.01, n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
155
0
50
100
150
200
250
300
WT KO
Res
orpt
ion
Pit A
rea
(μm
2 /cel
l)
n.s.
WT KO
Figure 7.7 SEM analysis (on bone slices) for Svs7 KO osteoclast bone resorption
activity. WT and Svs7 KO mature osteoclasts, grown in collagen-coated 6-well plates,
were detached and seeded onto bone slices and cultured for 48 hours in RANKL-
supplemented complete medium to initiate bone resorption. TRAP staining and
osteoclasts counting were subsequently performed, followed by visualization of
resorption pits by SEM. The osteoclast bone resorption activity was expressed as a total
resorbed pit area/cell. No significant difference in osteoclast activity was observed
between WT and Svs7 KO osteoclasts. Hence, osteoclast activity was not affected in
Svs7 KO mice. Data are presented as mean ± SEM and are representative of three
independent experiments. n.s. = no significance against WT. Scale bars, 200μm.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
156
0
2000
4000
6000
8000
10000
12000
WT KO
Res
orpt
ion
Pit A
rea
(μm
2 /ce
ll)
n.s.
WT KO
100μm 100μm
Figure 7.8 Corning osteo plate analysis for Svs7 KO osteoclast bone resorption
activity. After the initial WT and KO mature osteoclasts culture in collagen plates, the
cells were detached and seeded onto the Corning wells, each containing bone
(hydroxyapatite)-like material. Four wells were prepared for TRAP stain and osteoclast
count and the other four for resorption pits analysis. The osteoclast bone resorption
activity was expressed as a total resorbed area/cell. The result revealed that both WT
and Svs7 KO osteoclasts had a comparable bone resorption activity. Together, these
findings indicated that the osteoclast bone resorption activity was independent of Svs7.
Data are presented as mean ± SEM and are representative of four independent
experiments. n.s. = no significance against WT. Scale bars, 100μm.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
157
amount of resorbed area/cell between WT and Svs7 KO osteoclasts. Together, these
findings indicated that the osteoclast bone resorption activity was independent of Svs7.
7.2.6 Svs7 KO osteoclasts are more sensitive to Ca2+ influx in response to RANKL
and extracellular Ca2+ stimulation
Considering that Ca2+ influx/signalling, induced by RANKL, is a prerequisite for the
robust induction of NFATc1 activation-driven osteoclast differentiation and activation
(Takayanagi et al. 2002), together with the fact that Svs7 acts as a Ca2+ transport
inhibitor on the membrane of sperm cells during fertilization process, it was then of
interest to explore the potential impact of the deletion of the Svs7 gene on Ca2+ influx in
osteoclasts. To this end, WT and Svs7 KO BM were first cultured on coverslips in 48-
well plates with complete medium supplemented with RANKL and M-CSF until
osteoclasts were observed (5 days culture). The cells were then loaded with 4μM Fluo-
4AM intracellular Ca2+-binding dye and the change of fluorescence intensity inside the
cells was observed by time-lapse microscopy. The basal Ca2+ level reading was taken
for 2 minutes with every 2 seconds interval recorded for a total of 60 intervals. As
expected, the result showed that both WT and Svs7 KO osteoclasts had a trend of
increase in Ca2+ influx in response to RANKL stimulation overnight (Figure 7.9A).
Svs7 KO osteoclasts, however, appeared to have a higher increase in basal Ca2+ influx
response compared to WT, with about 0.055 increase in fluorescence intensity (ratio to
baseline reading) for KO and 0.04 fluorescence intensity increase for WT from 0 to 60
interval mark (Figure 7.9A). This finding indicated that Svs7 KO osteoclasts were more
sensitive to Ca2+ influx in response to RANKL and hence Svs7 might have a role in
regulating Ca2+ influx (transport) in osteoclasts. To further investigate this possibility,
the effects of adding extracellular Ca2+ (in the form of CaCl2) on the osteoclast Ca2+
response was assessed. Three concentrations of CaCl2 were used: 5, 10, and 20mM. The
period of this extracellular Ca2+ stimulation was recorded for 3 minutes (with 2 seconds
interval), following the 2 minutes reading of the basal Ca2+ level. In all three
concentrations, the addition of this extracellular Ca2+ at 60 interval mark (120 seconds;
the end of the basal Ca2+ level fluorescence reading) caused an initial sudden increase in
Ca2+ influx, as monitored by the corresponding increase in fluorescence intensity, in
both WT and Svs7 KO osteoclasts, as shown in Figure 7.9B ((i) 5mM, (ii) 10mM, and
(iii) 20mM CaCl2 concentration). The major difference in this initial sudden Ca2+ influx
between WT and Svs7 KO osteoclasts was at the addition of 5mM CaCl2 concentration
(Figure 7.9B(i)), at which the KO cells had a faster and steeper Ca2+ influx response

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
158
0.94
0.95
0.96
0.97
0.98
0.99
1
1.01
0 10 20 30 40 50 60 70
Fluo
resc
ence
inten
sity
(ratio
to b
aseli
ne)
Intervals
WT
KO
Basal Ca2+ level
0
0.2
0.4
0.6
0.8
1
1.2
1.4
0 20 40 60 80 100 120 140 160
Flu
ores
cenc
e in
tens
ity
(rat
io t
o ba
seli
ne)
Intervals
WT
KO
Addition of 5mM CaCl2
0
0.2
0.4
0.6
0.8
1
1.2
1.4
0 20 40 60 80 100 120 140 160 F
luor
esce
nce
inte
nsit
y (r
atio
to b
asel
ine)
Intervals
WT
KO
Addition of 10mM CaCl2
0
0.2
0.4
0.6
0.8
1
1.2
1.4
0 20 40 60 80 100 120 140 160
Flu
ores
cenc
e in
tens
ity
(rat
io to
bas
elin
e)
Intervals
WT
KO
Addition of 20mM CaCl2
Basal Ca2+ level Basal Ca2+ level
Basal Ca2+ level
0
20
40
60
80
100
120
140
160
180
5mM 10mM 20mM
Fina
l Ca2+
upt
ake
by m
atur
e os
teoc
last
s (%
of b
asel
ine)
Extracellular Ca2+ (CaCl2) stimulation
WT
KO
n.s.
n.s. n.s.
(A)
(B)
(C)
(i) (ii)
(iii)
Figure 7.9 Svs7 KO osteoclasts are more sensitive to Ca2+ influx in response to
RANKL and extracellular Ca2+ stimulation. (A) After overnight RANKL stimulation,
Fluo4 intracellular calcium dye was incubated with WT and Svs7 KO osteoclasts and
the basal Ca2+ level was read for 2 minutes with every 2 seconds interval recorded for a
total of 60 intervals. Svs7 KO osteoclasts showed to have a higher increase in basal

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
159
Ca2+ influx response compared to WT, with 0.055 increase in fluorescence intensity
(ratio to baseline) for KO and 0.04 fluorescence intensity increase for WT from 0 to 60
interval mark. (B) After the 60-interval mark, the cells were stimulated with 3 different
concentrations of CaCl2 (extracellular Ca2+), (i) 5, (ii) 10, and (iii) 20mM and the assay
was continued for another 3 minutes. In all 3 concentrations, the addition of
extracellular Ca2+ caused an initial sudden increase in Ca2+ influx in both WT and Svs7
KO osteoclasts, with the major difference between WT and KO response was observed
at the addition of 5mM CaCl2 concentration, at which KO osteoclasts had a faster and
steeper Ca2+ influx response (0.12 increase in fluorescence intensity from the basal level
(ratio to baseline)) than WT. However, this initial response in Svs7 KO osteoclasts was
disappeared as time progressed with WT and KO cells showed a similar trend of Ca2+
uptake. (C) Final Ca2+ uptake at the end of (each) extracellular CaCl2 stimulation was
expressed as a percentage increase (relative) over the baseline reading. The result
showed that there was no significant difference in final Ca2+ uptake (% of baseline) at
the end of each extracellular Ca2+ stimulation (5, 10, and 20mM) between WT and Svs7
KO osteoclasts. Collectively, these findings indicated that Svs7 KO osteoclasts were
more sensitive to Ca2+ influx in response to RANKL and extracellular Ca2+ stimulation
compared to WT. Data are presented as mean ± SEM. n.s. = no significance against
WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
160
(0.12 increase in fluorescence intensity from the basal level (ratio to baseline)) than
WT. Following this initial sudden Ca2+ influx response, the addition of extracellular
Ca2+ resulted in the similar and continuous pattern of Ca2+ uptake in both WT and Svs7
KO osteoclasts. Despite a comparable final Ca2+ uptake (percentage of final
fluorescence reading at the end of (each) extracellular Ca2+ stimulation to baseline
reading) between WT and Svs7 KO osteoclasts shown in Figure 7.9C, collectively,
these findings indicated that Svs7 KO osteoclasts were more sensitive to Ca2+ influx in
response to RANKL and extracellular Ca2+ stimulation compared to WT. Thus, it is
tempting to speculate that the dysregulated Ca2+ response might alter the Ca2+-NFATc1
signalling pathway in Svs7 KO osteoclast differentiation.
7.2.7 Svs7 KO mice exhibit elevated NFATc1 and ATP6v0d2 proteins expression
during RANKL-induced osteoclastogenesis
As indicated in Section 7.2.2, osteoclasts from Svs7 KO mice were significantly larger
and possessed more nuclei than WT. These findings indicated the possible involvement
of Svs7 in osteoclast fusion mechanism and, together with the finding that Svs7 KO
osteoclasts were more sensitive to Ca2+ influx in response to RANKL, it then led us to
hypothesize that Svs7 may be a negative regulator of NFATc1 expression and possibly
the fusogenic proteins, DCSTAMP and ATP6v0d2 (Lee et al. 2006; Yagi et al. 2005),
whose expressions have been shown to be regulated by NFATc1 (Kim et al. 2008;
Takayanagi et al. 2002; Takayanagi 2007). Since osteoclasts from Svs7 KO mice had
comparable mRNA expression levels of osteoclast marker genes, which included
NFATc1, DCSTAMP, and ATP6v0d2 genes, with WT during RANKL-induced
osteoclastogenesis (Figure 7.6), we reassured that Svs7 involvement in osteoclast fusion
might be linked to RANKL-induced ITAM co-stimulatory pathway activation, which
involves Ca2+ influx response and the subsequent activation of NFATc1 via
Ca2+/calmodulin-dependent calcineurin pathway (Koga et al. 2004; Takayanagi et al.
2002).
To explore the effects of the loss of the Svs7 gene on NFATc1 and fusogenic proteins
expression in osteoclasts, cell lysates of 5-day time course RANKL-induced WT and
Svs7 KO BMM were extracted and subjected to western blot (WB) analysis and
immunoblotted with specific NFATc1 (Figure 7.10), ATP6v0d2 (Figure 7.11), and
DCSTAMP (Figure 7.12) antibodies. As shown in Figure 7.10, there was a significant

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
161
0 1 2 3 5 0 1 2 3 5 WT KO
NFATc1
β-actin
RANKL Stimulation day
0
0.2
0.4
0.6
0.8
1
1.2
Day 0 Day 1 Day 2 Day 3 Day 5
Rat
io to
β-a
ctin
RANKL stimulation
WT
KO n.s. n.s.
n.s. n.s.
Figure 7.10 Svs7 KO osteoclasts have a significant increase in NFATc1 protein
expression during RANKL-induced osteoclastogenesis. Cell lysates of 5-day time
course RANKL-induced WT and Svs7 KO BMM were extracted and subjected to WB
protein analysis, immunoblotted with specific NFATc1 antibody. Densitometry analysis
was performed using ImageJ software and the NFATc1 protein expression was
expressed as a ratio to β-actin, which served as a loading control. There was a
significant increase in NFATc1 protein expression in Svs7 KO osteoclasts compared to
WT at day 3 of RANKL-induced osteoclastogenesis. Data are presented as mean ±
SEM and are representative of three independent experiments. ** p < 0.01, n.s. = no
significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
162
0 1 2 3 5 0 1 2 3 5 WT KO
ATP6v0d2
β-actin
RANKL Stimulation day
0
0.2
0.4
0.6
0.8
1
1.2
Day 0 Day 1 Day 2 Day 3 Day 5
Rat
io to
β-a
ctin
RANKL stimulation
WT
KO n.s. n.s.
n.s.
n.s. n.s.
Figure 7.11 Svs7 KO osteoclasts have a trend of increase in ATP6v0d2 protein
expression during RANKL-induced osteoclastogenesis. Cell lysates of 5-day time
course RANKL-induced WT and Svs7 KO BMM were extracted and subjected to WB
protein analysis, immunoblotted with specific ATP6v0d2 antibody. Densitometry
analysis was performed using ImageJ software and the ATP6v0d2 protein expression
was expressed as a ratio to β-actin, which served as a loading control. There was a
consistent trend of increase in ATP6v0d2 protein expression in Svs7 KO osteoclasts
compared to WT particularly at day 3 and 5 of RANKL-induced osteoclastogenesis.
Data are presented as mean ± SEM and are representative of four independent
experiments. n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
163
0 1 2 3 5 0 1 2 3 5
WT KO
DCSTAMP
β-actin
RANKL Stimulation day
0 0.1 0.2 0.3 0.4 0.5 0.6 0.7 0.8
Day 0 Day 1 Day 2 Day 3 Day 5
Rat
io to
β-a
ctin
RANKL stimulation
WT
KO
n.s.
n.s. n.s. n.s. n.s.
Figure 7.12 DCSTAMP protein expression appears to be unaffected in Svs7 KO
osteoclasts throughout the time course of RANKL-induced osteoclastogenesis. Cell
lysates of 5-day time course RANKL-induced WT and Svs7 KO BMM were extracted
and subjected to WB protein analysis, immunoblotted with specific DCSTAMP
monoclonal antibody. Densitometry analysis was performed using ImageJ software and
the DCSTAMP protein expression was expressed as a ratio to β-actin, which served as a
loading control. There was no significant difference in DCSTAMP protein expression
between WT and Svs7 KO osteoclasts throughout the time course of RANKL-induced
osteoclastogenesis. Data are presented as mean ± SEM and are representative of three
independent experiments. n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
164
increase in NFATc1 protein expression in Svs7 KO osteoclasts at day 3 of
osteoclastogenesis compared to WT. This finding implied that the dysregulated Ca2+
influx response, observed in Svs7 KO osteoclasts upon RANKL stimulation, might
account for the altered NFATc1 signalling, resulting in its stronger activation.
Subsequently, it was then revealed that the protein expression of ATP6v0d2 also
showed to have a trend of increase in Svs7 KO osteoclasts compared to WT,
particularly at day 3 and 5 of osteoclastogenesis (Figure 7.11). The DCSTAMP protein
expression, however, appeared to be unaffected in Svs7 KO mice, relative to WT,
throughout the time course of RANKL-induced osteoclastogenesis (Figure 7.12). These
findings suggest that Svs7 may play a crucial role in the regulation of osteoclast fusion
mechanism through the Ca2+-NFATc1 signalling pathway via modulation of the
expression of ATP6v0d2 but not DCSTAMP expression.
7.2.8 Svs7 protein treatment inhibits the activation of NFAT promoter luciferase
activity
Considering the increase in NFATc1 protein expression observed in Svs7 KO
osteoclasts (Figure 7.10), it was of further interest to investigate the effects of Svs7
protein treatment on NFAT promoter activation. After the successful cloning process of
Svs7 coding sequence (295bp) into HindIII/XhoI restriction enzyme site of the
pcDNA3.1 V5-His mammalian expression vector, as shown in Figure 7.13A, the
experiment was continued by transiently transfecting COS-7 cells, one group with the
Svs7 DNA construct and the other with pcDNA3.1 V5-His empty plasmid, which
served as a vehicle control. The conditioned medium (CM) was collected each day post
transfection and tested for Svs7 protein expression using WB analysis. Using rabbit
polyclonal anti-Svs7 antibody, Svs7 protein was detected to be successfully expressed
in the CM (Figure 7.13B). Luciferase assay was performed by stimulating RAW264.7
cells, stably expressing NFAT promoter and luciferase reporter gene, with either 50%
Svs7 CM or the vehicle control medium for an hour, followed by overnight RANKL
stimulation. The luminescence reading, which corresponds to the NFAT promoter
luciferase activity, was measured on the following day. The result showed that Svs7
protein treatment could significantly inhibit the activation of NFAT promoter (Figure
7.13C), further suggesting a regulatory role of Svs7 in NFAT promoter activation.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
165
pcDNA3.1 V5-His (5.5kbp)
Svs7 (295bp)
1kbp DNA ladder
75 50 36
25 20
15
10
kDa +C 1 2 3 5 6 7
Collected CM in Opti-MEM reduced serum medium (day post-transfection)
Svs7
(A) (B)
0
20000
40000
60000
80000
100000
120000
140000
vehicle SVS7
NFA
T lu
cife
rase
act
ivity
(A
rbitr
ary
unit)
(C)
Figure 7.13 Svs7 protein treatment inhibits NFAT promoter luciferase activity (A)
DNA agarose gel electrophoresis of a midiprep pcDNA3.1 Svs7 V5-His cloning
construct, which had been cut by HindIII/XhoI restriction enzymes, showed that Svs7
coding sequence (295bp) was successfully cloned into the pcDNA3.1 V5-His
mammalian expression vector. (B) After transient transfection of either the Svs7
construct or the vehicle control plasmid into COS-7 cells, WB analysis on the CM using
rabbit polyclonal anti-Svs7 antibody was performed to detect the expression of Svs7
protein. The result showed that Svs7 was detected to be successfully expressed in the
CM collected each day post transfection. (C) RAW264.7 cells, stably expressing NFAT
promoter and luciferase reporter gene, were pretreated with either 50% Svs7 CM or the
vehicle control medium for an hour, followed by overnight RANKL stimulation.
Luciferase assay was then performed on the following day and the result revealed that
Svs7 CM treatment significantly inhibited the activation of NFAT promoter. Data are
presented as mean ± SEM and are representative of three independent experiments. ** p
< 0.01 against vehicle.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
166
7.3 Results – Part 2: Osteoblasts from Svs7 KO mice are
phenotypically comparable to WT cells A balance in the cell-to-cell communication between osteoclasts and osteoblasts is the
prerequisite for achieving a healthy bone mass. Following the establishment of
increased osteoclastogenesis in vitro in Svs7 KO mice and the intrinsic role of Svs7 in
the regulation of osteoclast fusion mechanism through the Ca2+-NFATc1 signalling
pathway, in vitro Svs7 KO osteoblast phenotype was next assessed. To this end, Svs7
KO osteoblast differentiation and bone formation (mineralization) assays were then
performed.
7.3.1 Svs7 KO primary calvarial osteoblasts exhibit an unaffected proliferation
rate in vitro
To examine Svs7 KO osteoblast phenotype in vitro, Svs7 KO osteoblast proliferation
was investigated. To achieve this, WT and Svs7 KO neonatal mice were sacrificed and
the calvariae were dissected from both. After going through four series of collagenase
digestion, primary calvarial osteoblast cells were seeded overnight on 12-well plates,
ready for MTS proliferation assay and standard curve reading the next day. Two sets of
plates were incubated for 24 and 48 hours time points after the standard curve reading.
The result showed that at both time points there were comparable proliferation rates
between WT and Svs7 KO primary calvarial osteoblasts (Figure 7.14). Hence, this
finding suggested that Svs7 KO mice exhibited an unaffected osteoblast proliferation
rate in vitro.
7.3.2 No defect is observed in Svs7 KO alkaline phosphatase (ALP) osteoblast
differentiation in vitro
In order to examine if there is an osteoblast phenotype in Svs7 KO mice, ALP
osteoblast differentiation assays were performed. BM cells were extracted from long
bones of 12-week old WT and Svs7 KO mice and cultured in osteoblast differentiation
medium (complete medium supplemented with β-glycerophosphate and ascorbate) for
14 days in vitro. The ALP staining was then performed and the ALP-positive colonies
were analysed and counted. The result revealed that there was no significant difference
in colony forming unit (CFU)-ALP positive colonies formed between WT and Svs7 KO
osteoblast cultures (Figure 7.15), indicating that Svs7 KO mice had no defects in
osteoblast differentiation in vitro.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
167
0 2000 4000 6000 8000
10000 12000 14000 16000
Day 1 Day2
Estim
ated
cel
l num
ber
Cell Proliferation
WT
KO
n.s. n.s.
Figure 7.14 Svs7 KO primary calvarial osteoblasts exhibit an unaffected
proliferation rate in vitro. Calvariae were dissected from WT and Svs7 KO neonatal
mice and primary calvarial osteoblast cells were extracted from the calvariae through
serial collagenase digestion method. After the cells were seeded overnight, MTS
proliferation assay for standard curve reading was performed, followed by 24 and 48
hours time points incubation and the absorbance analysis. The result showed that there
were no significant differences in proliferation rate at both time points between WT and
Svs7 KO primary calvarial osteoblasts. Hence, this finding indicated that Svs7 KO mice
exhibited an unaffected osteoblast proliferation rate in vitro. Data are presented as mean
± SEM. n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
168
0
10
20
30
40
50
60
WT KO
Num
ber o
f CFU
-ALP
+
WT
KO
n.s.
Figure 7.15 No defect is observed in Svs7 KO ALP osteoblast differentiation in
vitro. BM cells were extracted from long bones of 12-week old WT and Svs7 KO mice
and cultured in osteogenic medium (complete medium supplemented with β-
glycerophosphate and ascorbate) for 14 days in vitro. The ALP staining was then
performed and the ALP-positive colonies were analysed and counted. The result
showed that there was no significant difference in CFU-ALP positive colonies formed
between WT and Svs7 KO osteoblast cultures, indicating that Svs7 KO mice had no
defects in osteoblast differentiation in vitro. Data are presented as mean ± SEM and are
representative of three independent experiments. n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
169
7.3.3 Svs7 KO osteoblasts exhibit an unaffected bone formation activity in vitro
To further confirm a normal bone formation activity in Svs7 KO osteoblasts in vivo,
shown by double calcein labelling experiment and mineral apposition rate (MAR)
analysis in Chapter 6 Figure 6.7, in vitro bone nodule formation (mineralization) assay
was performed. To this end, BM cells were extracted from long bones of 12-week old
WT and Svs7 KO mice and cultured for 14 days in osteogenic medium. Alizarin red
staining, which stains for calcium deposition in culture wells, was then performed.
Following the staining procedure, the culture plates were scanned and the total
mineralized nodules were measured using ImageJ software. The result showed that
there was no significant difference in total mineralized nodules formed between WT
and Svs7 KO osteoblast cultures (Figure 7.16). This finding therefore indicated that
Svs7 KO osteoblasts exhibited an unaffected bone formation activity in vitro.
7.3.4 Analysis of osteoblast marker genes expression levels in Svs7 KO mice
To complete the in vitro Svs7 KO osteoblast phenotype characterization, RT-PCR
reaction was performed on 14-day (0, 7 and 14 day time points) time course WT and
Svs7 KO BM cells differentiation into mature osteoblasts. For this, BM cells were
extracted from long bones of 12-week old WT and Svs7 KO mice and cultured in
osteogenic medium for 14 days. RNA was then extracted, followed by RT and semi
quantitative PCR reactions using specific primers for Runx2, Osterix, ALP, osteopontin
(OPN), osteocalcin (OCN), M-CSF, RANKL, and OPG. β-actin was used as a loading
control. Densitometry analysis was performed using ImageJ software and the expression
of each osteoblast gene was expressed as a ratio to β-actin. The result revealed that
there were no distinguishable differences in the expression levels of key osteoblast
marker genes between WT and Svs7 KO mice (Figure 7.17). This finding suggested
that Svs7 KO mice exhibited unaltered expression levels of osteoblast marker genes.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
170
0
2
4
6
8
10
12
WT KO
Min
eral
ized
nod
ules
(mm
2 )
WT
KO
n.s.
Figure 7.16 Svs7 KO osteoblasts exhibit an unaffected bone formation activity in
vitro. BM cells were extracted from long bones of 12-week old WT and Svs7 KO mice
and cultured in osteogenic medium for 14 days. Upon the formation of calcium
deposition, cells were fixed with 4% paraformaldehyde and alizarin red stain was then
applied to the culture wells, followed by total mineralized nodules measurement using
ImageJ software. The result showed that there was no significant difference in total
mineralized nodules formed between WT and Svs7 KO osteoblast cultures. This finding
indicated that Svs7 KO osteoblasts exhibited an unaffected bone formation activity in
vitro. Data are presented as mean ± SEM and are representative of three independent
experiments. n.s. = no significance against WT.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
171
ALP
WT KO
0 7 14 0 7 14 Runx2
Osterix
OPN
OCN
β-actin
RANKL
OPG
OB Differentiation day
M-CSF
0
0.1
0.2
0.3
0.4
0.5
0.6
0.7
Day 0 Day 7 Day 14
Runx
2 gen
e exp
ressio
n (ra
tio to
β-ac
tin)
OB Differentiation
WT
KO
0
0.2
0.4
0.6
0.8
1
Day 0 Day 7 Day 14
Oster
ix ge
ne ex
pres
sion
(ratio
to β-
actin
)
OB Differentiation
WT
KO
0 0.1 0.2 0.3 0.4 0.5 0.6 0.7 0.8 0.9
Day 0 Day 7 Day 14
ALP g
ene e
xpres
sion
(ratio
to β-
actin
)
OB Differentiation
WT
KO
0
0.2
0.4
0.6
0.8
1
1.2
Day 0 Day 7 Day 14
OPN
gene
expr
essio
n (ra
tio to
β-ac
tin)
OB Differentiation
WT
KO
0
0.2
0.4
0.6
0.8
1
1.2
Day 0 Day 7 Day 14
OCN
gene
expr
essio
n (ra
tio to
β-ac
tin)
OB Differentiation
WT
KO
0
0.1
0.2
0.3
0.4
0.5
Day 0 Day 7 Day 14
M-C
SF ge
ne ex
pres
sion
(ratio
to β-
actin
)
OB Differentiation
WT
KO
0
0.1
0.2
0.3
0.4
0.5
0.6
0.7
Day 0 Day 7 Day 14
RANK
L ge
ne ex
pres
sion
(ratio
to β-
actin
)
OB Differentiation
WT
KO
0 0.05
0.1 0.15
0.2 0.25
0.3 0.35
0.4
Day 0 Day 7 Day 14
OPG
gene
expr
essio
n (ra
tio to
β-ac
tin)
OB Differentiation
WT
KO
(A)
(B)
Figure 7.17 Analysis of osteoblast marker genes expression levels in Svs7 KO mice.
(A) BM cells were extracted from long bones of 12-week old WT and Svs7 KO mice
and cultured in osteogenic medium for 14 days. RNA was then extracted and subjected
to semi quantitative RT-PCR reactions using specific primers for Runx2, Osterix, ALP,
OPN, OCN, M-CSF, RANKL, and OPG. β actin served as a loading control. Agarose
gel electrophoresis depicted that there was no striking difference in the expression of
osteoblast marker genes between WT and Svs7 KO mice, as also shown in (B)
Densitometry analysis using ImageJ software, in which the expression of each
osteoblast gene was expressed as a ratio to β-actin. Data are representative of one
experiment.

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
172
7.4 Discussion As previously shown in Chapter 6, Svs7 KO mice exhibit a low bone mass phenotype,
which could have resulted from either a decrease in bone formation by osteoblasts
(Manolagas & Jilka 1995) and/or an excessive bone resorption activity by osteoclasts
(Riggs & Melton 1983). Therefore, the first part of this chapter explored the potential
intrinsic role of Svs7 in osteoclast differentiation (including osteoclast fusion
mechanism) and activation. First, a five-day time course of RANKL-induced WT and
Svs7 KO BMM revealed that KO cells had a significant increase in osteoclastogenesis
than WT, starting at day 3 and continued to day 5 of osteoclastogenesis. In addition to
this increase in the number of osteoclasts, Svs7 KO osteoclasts had also shown to have
significantly larger spread area and more nuclei than WT, indicating the potential
intrinsic role of Svs7 in the regulation of osteoclast fusion mechanism (Fujita et al.
2012; Lee et al. 2006; Yagi et al. 2005). The potential role of Svs7 in the regulation of
osteoclast fusion gained a huge interest because of the fact that the fusion process of
osteoclast precursors to differentiate into multinucleated osteoclasts starts at day 3
onwards during RANKL-induced osteoclastogenesis (Fujita et al. 2012; Kim et al.
2008), at which Svs7 gene expression is upregulated in osteoclasts (Chapter 2 Figure
2.4). With the additional results that showed the unaffected Svs7 KO BM population of
early osteoclast precursor (Lin-) and LSK HSCs, as well as MAPK (ERK, JNK, and p38
phosphorylation) and NF-κB (IκBα degradation) signalling pathways (Cobb &
Goldsmith 1995; Teitelbaum 2000) in Svs7 KO osteoclast progenitor relative to WT,
these findings suggest that Svs7 has a potential intrinsic regulatory role in osteoclast
fusion and has no effects on early osteoclast progenitor population and proliferation.
Since osteoclasts from Svs7 KO mice had a comparable mRNA expression of osteoclast
marker genes, such as NFATc1, DCSTAMP, and ATP6v0d2 fusogenes, with WT
during RANKL-induced osteoclastogenesis, we are therefore tempted to speculate that
Svs7 involvement in osteoclast fusion might be linked to RANKL-induced ITAM co-
stimulatory pathway activation, which involves Ca2+ influx response and the subsequent
activation of NFATc1 via Ca2+/calmodulin-dependent calcineurin pathway (Koga et al.
2004; Takayanagi et al. 2002).
Although there were more large osteoclasts in Svs7 KO BMM in vitro cultures, the total
resorbed area/cell, as an indication of the osteoclast bone resorption activity, was found
to be comparable between WT and Svs7 KO osteoclasts. Hence, this result indicates

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
173
that the osteoclast bone resorption activity is independent of Svs7. The study from Lee
et al. 2006 has also shown that despite osteoclast differentiation is affected in
ATP6v0d2-deficient mice, osteoclast bone resorption activity is normal in these mice,
indicating a sole role of ATP6v0d2 in osteoclast fusion process. It is then plausible to
speculate that the nature of increase in in vitro and in vivo osteoclastogenesis itself that
could have contributed to the osteoporotic phenotype observed in Svs7 KO mice.
Considering that Ca2+ influx/signalling, induced by RANKL, is a prerequisite for the
robust induction of NFATc1 activation-driven osteoclast differentiation and activation
(Hwang & Putney 2012; Kim et al. 2008; Takayanagi et al. 2002; Takayanagi 2007),
together with the fact that Svs7 acts as a Ca2+ transport inhibitor on the membrane of
sperm cells during fertilization process, it was then interesting to explore the potential
effect of the loss of the Svs7 gene on Ca2+ influx in osteoclasts. Fluo-4AM intracellular
calcium assays revealed that Svs7 KO osteoclasts were more sensitive to Ca2+ influx
(shown by a higher increase in fluorescence intensity in the basal Ca2+ level (ratio to
baseline)) in response to RANKL and extracellular Ca2+ stimulation (particularly at the
addition of 5mM concentration of CaCl2) than WT. Despite a comparable final Ca2+
uptake (percentage of final fluorescence reading at the end of extracellular Ca2+
stimulation to baseline reading) between WT and Svs7 KO osteoclasts, these findings
indicate that there is a dysregulated Ca2+ influx/transport in Svs7 KO osteoclasts.
NFATc1, a Ca2+-dependent transcription factor and a master regulator of
osteoclastogenesis, has been shown to regulate a number of osteoclast marker genes
expression, such as Cathepsin K, TRAP, CTR, OSCAR, and β3 integrin (Crotti et al.
2006; Kim et al. 2005; Matsumoto et al. 2004; Takayanagi et al. 2002), as well as the
two fusogenic factors, DCSTAMP and ATP6v0d2 (Kim et al. 2008; Lee et al. 2006;
Yagi et al. 2005). With the findings that indicate a dysregulated Ca2+ influx in Svs7 KO
osteoclasts in response to RANKL, there was then a strong indication that NFATc1 and
possibly the two fusogenic proteins expression might be affected in osteoclasts of Svs7
KO mice. To explore the effects of the loss of the Svs7 gene on NFATc1 and fusogenic
proteins expression in osteoclasts, cell lysates of 5-day time course of RANKL-induced
WT and Svs7 KO BMM were extracted and subjected to western blot (WB) analysis
and immunoblotted with specific NFATc1, ATP6v0d2, and DCSTAMP antibodies. The
results revealed that there was a significant increase in NFATc1 (at day 3 of
osteoclastogenesis) and a trend of increase in ATP6v0d2 protein expression in Svs7 KO

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
174
osteoclasts compared to WT, particularly at day 3 and 5 of RANKL-induced
osteoclastogenesis. Although DCSTAMP protein expression was found to be unaffected
in Svs7 KO osteoclasts, together these findings imply that the dysregulated Ca2+ influx,
observed in KO osteoclasts upon RANKL stimulation, might account for the altered
NFATc1 signalling, resulting in its stronger activation with the subsequent increase in
ATP6v0d2 fusogenic protein expression. Furthermore, the direct regulatory role of Svs7
in NFATc1 activation has been shown by the inhibitory effect of Svs7 protein treatment
on NFAT promoter luciferase activity. Although the possibility of direct regulatory role
of Svs7 in NFATc1 protein expression needs further investigation, collectively, these
results suggest that Svs7 may regulate osteoclast fusion mechanism through the Ca2+-
NFATc1 signalling pathway, which has its primary effect on the expression of
ATP6v0d2 but not DCSTAMP expression.
As bone homeostasis is maintained by the balanced cell-to-cell communication between
osteoclasts and osteoblasts, in vitro Svs7 KO osteoblast phenotype characterization was
next performed. To achieve this, Svs7 KO primary calvarial osteoblast proliferation was
investigated first. Calvariae were dissected from WT and Svs7 KO neonatal mice and
the primary calvarial osteoblast cells were extracted from the calvariae using serial
collagenase digestion method. MTS proliferation assays on standard and two time
points (24 and 48 hours incubation) were then performed. The result showed that at both
time points there were no significance differences in proliferation rate between WT and
Svs7 KO primary calvarial osteoblasts, indicating that Svs7 KO osteoblasts exhibit an
unaffected proliferation rate in vitro. Next, ALP osteoblast differentiation and bone
nodule formation (mineralization) assays were performed on WT and Svs7 KO BM-
derived osteoblasts. Following 14 days culture in osteogenic medium, ALP staining was
conducted to analyse osteoblast differentiation in vitro, while alizarin red staining was
used to stain for calcium deposition in mineralization assays. The results showed that
there were no significant differences in CFU-ALP positive colonies and total
mineralized nodules formed between WT and Svs7 KO osteoblast cultures. With the
previous double calcein labelling experiment and MAR analysis results that showed
Svs7 KO mice had a normal bone formation activity in vivo, together these results
indicate that Svs7 KO mice exhibit unaltered osteoblast differentiation in vitro and
osteoblast bone formation activity both in vitro and in vivo. Furthermore, through semi
quantitative RT-PCR reactions on 14-day time course of WT and Svs7 KO BM cells
differentiation into mature osteoblasts using specific primers for common osteoblast

Chapter Seven – Investigation of Intrinsic Cellular Mechanism in Svs7 Knockout Mice (Osteoclast and Osteoblast)
175
marker genes, it is then revealed that, relative to WT, Svs7 KO mice exhibit unaltered
expression levels of osteoblast marker genes.
So in conclusion, Svs7 has shown to have a role in regulating osteoclast differentiation
but not osteoclast activity. Svs7 KO mice have a significant increase in
osteoclastogenesis and osteoclast size (possessing larger spread area and more nuclei)
than WT, hence osteoclast fusion is affected in the KO mice. By performing
intracellular Ca2+ assays, WB analysis, and NFAT promoter luciferase assays, it is then
revealed that Svs7 has a role in the regulation of osteoclast fusion mechanism through
the Ca2+-NFATc1 signalling pathway and the subsequent ATP6v0d2 fusogenic protein
expression. As Svs7 KO mice have shown to have unaffected osteoblast proliferation,
differentiation, and bone formation activity, we are then tempted to speculate that the
loss of Svs7 regulation in osteoclast differentiation and fusion through the Ca2+-
NFATc1 signalling pathway is the likely cause for the osteoporotic phenotype observed
in the KO mice. Hence, Svs7 is a novel regulator of bone homeostasis, which acts in an
autocrine fashion to regulate osteoclast differentiation and fusion.

176
CHAPTER 8
GENERAL SUMMARY AND FUTURE DIRECTIONS

Chapter Eight – General Summary and Future Directions
177
8.1 Overview of Thesis and General Discussion Healthy bone during adult life is maintained by balanced yet complementary activities
of bone-resorbing osteoclasts and bone-forming osteoblasts and hence is tightly
regulated and governed by many local and systemic factors, such as growth factors,
cytokines, proteins, and hormones (Karsenty & Wagner 2002; Zaidi 2007). The
osteoblast regulation of osteoclast differentiation and activation has been well studied,
while the other way of communication, in which osteoclasts regulate osteoblasts
function, is still poorly understood. In search for novel osteoclast-derived factors,
subtractive hybridization-based differential screening method was employed to probe
for differentially expressed genes between osteoclasts (RANKL-stimulated RAW264.7
cells) and their mononuclear progenitors (RAW264.7 osteoclast precursors) (Phan 2004).
Subsequently, Svs7 gene was identified as a candidate gene, whose expression was
robustly upregulated during RANKL-induced osteoclastogenesis (Davey 2008; Phan
2004). Svs7 is exclusively expressed by osteoclasts in bone and synthesized as a
secreted factor.
Svs7 is a secreted member of Ly-6 family, which shares common TFP/Ly-6/uPAR
motif (a conserved 8-10 cysteine residues and a C-terminal consensus sequence motif of
CCXXXXCN) (Coronel et al. 1992; Southan et al. 2002; Turunen et al. 2011; Ushizawa
et al. 2009). Several Ly-6 genes have been shown to be involved in many cellular
signalling pathways, such as uPAR in αvβ3 signalling pathway (Schiller et al. 2009;
Smith, Marra & Marshall 2008; Wei et al. 2008) and Sca-1 in stem cell renewal
capacity (Bonyadi et al. 2003; Holmes et al. 2007; Ito et al. 2003). With this knowledge
together with the previous studies by Davey 2008, which showed that treatment with
recombinant purified Svs7 protein (daily injection of 500μg/kg protein) could protect
against loss of trabecular bone volume, trabecular thickness, and trabecular number at
the distal femoral metaphysis of ovariectomised mice (oestrogen deficiency-induced
bone loss mouse model (Aitken, Armstrong & Anderson 1972; Kalu 1991; Saville
1969)), it led us to hypothesize that Svs7 is an important regulator of bone homeostasis.
To investigate this potential role of Svs7 in bone homeostasis, Svs7 TG mice were
initially generated and characterised. Following the successful cloning and purification,
the linearized pcDNA3.1 Svs7-V5 His transgene was microinjected into blastocysts to
generate Svs7 TG mice. Assessment of Svs7 tissue distribution revealed that, in normal
WT mice, Svs7 was almost exclusively expressed in seminal vesicle (including

Chapter Eight – General Summary and Future Directions
178
prostate) with little to no expression in other tissues, including bone. In liver, the protein
expression of Svs7 in Svs7 TG mice was found to be low, which equalled to only ~2.5
fold increase relative to WT. It is possible that post transcriptional and translational
regulations as well as hormonal change might influence gene and protein expression
levels (King et al. 2012; Levitin et al. 2008) and therefore the use of osteoclast-specific
Svs7 TG mice and the subsequent detection of overexpressed Svs7 protein in bone
tissue of these TG mice should be considered in the future to induce direct bone cells-
specific responses. Global characterisation of Svs7 TG mice was further pursued by
performing histological assessment on TG organs and tissues (prostate). No obvious
change was observed in Svs7 TG prostate tissue phenotype relative to WT littermates,
suggesting that the overexpression of Svs7 does not affect the organogenesis in these
TG mice.
Next, the bone phenotype of Svs7 TG mice was assessed by X-ray, microCT, and
histology/histomorphometry analysis. Whole body X-ray of Svs7 TG mice showed that,
relative to WT, TG mice had phenotypically normal skeletons. Furthermore, microCT
analysis on trabecular bone at distal femoral metaphysis revealed comparable bone
parameters (trabecular bone volume, trabecular separation, trabecular thickness, and
trabecular number) between WT and Svs7 TG mice, indicating that the TG mice have
normal bone mass and architecture. Histology/histomorphometry analysis supported the
microCT data, which showed normal trabecular bone mass and structure at Svs7 TG
distal femurs and a comparable number of TRAP-positive osteoclasts observed near the
growth plate region of WT and TG hindlimbs. To confirm the osteoclast phenotype of
Svs7 TG mice, in vitro osteoclast differentiation assay was performed and the result
revealed that the TG mice exhibited an unaffected osteoclast differentiation, relative to
WT counterparts. Hence, this unaltered osteoclast differentiation is likely to have
contributed to the normal bone mass phenotype observed in Svs7 TG mice.
The normal bone phenotype of Svs7 TG mice therefore highlights two potential limiting
factors to the assessment of the potential role of Svs7 in the maintenance of bone
homeostasis. These factors are: (i) the naturally very low expression of Svs7 gene in
bone and (ii) the modest protein expression of Svs7 achieved in Svs7 TG mice.
Accordingly, the use of osteoclast-specific Svs7 TG mice in the future could potentially
induce a stronger expression of the Svs7 transgene and hence being able to trigger direct
bone cells-specific responses.

Chapter Eight – General Summary and Future Directions
179
The second approach utilised the generation and characterisation of Svs7 global KO
mice. This was achieved by deleting exon 2 and 3 of Svs7 gene, which together encode
for the TFP/Ly-6/uPAR domain, resulted in the complete absence of Svs7 gene and
protein in the KO mice. Breeding of Svs7 KO mice revealed that the ratio of male WT
and female Svs7 KO mice were well below than the expected mendelian ratio of 25%,
which consequently limited both sample size and number of assays possible for
assessment. As Svs7 has been shown to inhibit Ca2+ influx across the membrane of
sperm cells during fertilization to prevent premature acrosomal reaction and
spermatozoa hyperactivation (Coronel et al. 1992), this slow mice breeding process
could partly be due to a role for Svs7 in fertility process, which warrants investigation
in the future studies. Despite the slow mice breeding process, the gross body phenotype
of Svs7 KO mice appeared to be as normal as WT littermates. The global
characterisation of Svs7 KO mice was continued by performing macro- and microscopic
assessments on the KO mice organs and tissues phenotype. The results depicted that
there was no apparent difference in organs and tissues (including prostate histology
sections) phenotype between WT and Svs7 KO mice, therefore indicating that Svs7 KO
mice have no obvious defects in organs and tissues.
To directly investigate the role of Svs7 in bone, the bone phenotype of Svs7 KO mice
was assessed. To this end, microCT analysis on trabecular bone in the secondary
spongiosa of distal femurs (Lee et al. 2006; Nishikawa et al. 2010) from 15- and 30-
week old WT and Svs7 KO mice revealed that the KO mice had a significantly reduced
trabecular bone/tissue volume at both age groups and hence a significant decrease in
trabecular number (only in 30-week old group) compared to WT littermates. Hence,
these results not only suggest that Svs7 KO mice exhibit an osteoporotic phenotype but
also the possibility that the KO mice have a progressive decline in bone mass with age.
Consistent with these results, histology and histomorphometry analysis showed that
there was an obvious decrease in trabecular bone volume and a trend of increase in the
number of TRAP-positive osteoclasts, respectively, in Svs7 KO hindlimbs compared to
WT. Together, these results gave a strong indication that Svs7 KO mice might have an
alteration in osteoclast differentiation and/or activity, which could be the main
contributor to the osteoporotic phenotype of the KO mice. This position was further
supported by the finding that Svs7 KO mice exhibit an unaffected bone formation
activity in vivo, relative to WT, in double calcein labelling experiment and MAR
analysis. Considering that a naturally low Svs7 gene expression in bone is likely to have

Chapter Eight – General Summary and Future Directions
180
contributed to the mild phenotype observed in Svs7 KO mice, this study however has
shown that Svs7 is a potential regulator of bone homeostasis and the increase in
osteoclast number observed in the histomorphometry analysis of TRAP-stained sections
of Svs7 KO hindlimbs therefore hinted for a possible intrinsic role of Svs7 in osteoclast
differentiation and/or activation.
Next was the investigation of the intrinsic cellular mechanism underlying the
osteoporotic phenotype of Svs7 KO mice. In vitro time course RANKL-induced BMM
differentiation into osteoclasts revealed that Svs7 KO cultures had a significant increase
in osteoclast number compared to WT at day 3 and 5 of osteoclastogenesis. Hence,
these in vitro osteoclast differentiation data have correlated well with the
histomorphometry result, demonstrating that Svs7 KO mice have an alteration in
osteoclast differentiation. Furthermore, Svs7 KO osteoclasts were significantly larger
and possessed more nuclei (i.e. ≥ 11) than WT at day 5 of osteoclastogenesis, further
indicating that Svs7 regulates osteoclast fusion mechanism. Other possibility that the
loss of Svs7 gene might affect early bone marrow (BM) osteoclast progenitor
population was then investigated by performing flow cytometry analysis on WT and
Svs7 KO BM population for specific analysis on CD11b-/lowCD45R-CD3e- (Lin-) early
osteoclast precursor and Lin-Sca-1+c-Kit+ (LSK) hematopoietic stem cell population
(Jacquin et al. 2006; Kollet et al. 2006). The results showed that there were no
significant differences in both populations between WT and Svs7 KO mice. By
conducting MTS proliferation assay and MAPK (ERK, JNK, and p38 phosphorylation)
and NF-κB (IκBα degradation) signaling, which are important signaling pathways
governing early osteoclast precursor proliferation, growth, and survival (Cobb &
Goldsmith 1995; Teitelbaum 2000), WB analysis on WT and Svs7 KO early osteoclast
precursors, it was found that the KO mice exhibited unaltered proliferation and survival
of osteoclast precursor. Together, these results confidently suggest a role of Svs7 in
osteoclast fusion mechanism.
Despite the increase in osteoclast number and size in Svs7 KO BMM cultures, no
significant differences were observed in osteoclast bone resorption activity and key
osteoclast marker genes expression, including NFATc1 and fusogenic genes,
DCSTAMP and ATP6v0d2 (Kim et al. 2008; Lee et al. 2006; Yagi et al. 2005),
between WT and Svs7 KO mice. Hence, these results raise two possibilities for the role
of Svs7 in bone homeostasis. First, the osteoclast bone resorption activity is

Chapter Eight – General Summary and Future Directions
181
independent of Svs7. Previous studies by Lee et al. 2006 had presented similar results
that in ATP6v0d2-deficient mice, osteoclast differentiation and fusion were affected but
not osteoclast activity. Secondly, since osteoclast marker genes expression levels were
unaffected in Svs7 KO mice relative to WT, it is then possible that Svs7 involvement in
osteoclast fusion is linked to RANKL-induced ITAM co-stimulatory pathway
activation, which involves intracellular Ca2+ release from endoplasmic reticulum (ER)
store upon RANKL stimulation, followed by Ca2+ influx response through Ca2+
permeable channel (causing an increase of intracellular Ca2+ level) to sustain Ca2+
oscillation and the subsequent activation of NFATc1 via Ca2+/calmodulin-dependent
calcineurin pathway (Feske 2006; Hwang & Putney 2012; Kar, Nelson & Parekh 2011;
Koga et al. 2004; Lewis 2001; Takayanagi et al. 2002), as shown in the hypothetical
model of the role of Svs7 in osteoclasts (Figure 8.1).
To elucidate the possible mechanistic involvement of Svs7 in the osteoclast Ca2+
signalling pathway, Fluo-4AM intracellular calcium assay on WT and Svs7 KO
osteoclasts was performed. Upon RANKL stimulation (overnight), Svs7 KO osteoclasts
showed to have a higher increase in basal Ca2+ level than WT, which indicates that KO
osteoclasts are more sensitive to Ca2+ influx than WT in response to RANKL
stimulation. Furthermore, the addition of extracellular Ca2+ (especially at 5mM
concentration of CaCl2) caused a rapid and steep Ca2+ influx response in Svs7 KO
osteoclasts compared to WT littermates, although the final Ca2+ uptake (% of baseline)
between WT and KO osteoclasts was found to be comparable. Collectively, these
findings suggest that there is a dysregulated Ca2+ transport in Svs7 KO osteoclasts in
response to RANKL and extracellular Ca2+ stimulation, hence hinting the regulatory
role of Svs7, a novel osteoclast-secreted factor, in Ca2+ transport system in osteoclasts.
As NFATc1, a master regulator of osteoclastogenesis (Takayanagi et al. 2002), has been
shown to regulate osteoclast fusogens, such as DCSTAMP and ATP6v0d2 (Kim et al.
2008), the possibility that Svs7 regulates osteoclast fusion through the Ca2+-NFATc1
signalling pathway was further elucidated by performing WB analysis on cell lysates of
time course RANKL-induced WT and Svs7 KO BMM differentiation into mature
osteoclasts. Consistent with the possible role of Svs7 in regulating Ca2+ response in
osteoclasts, WB results showed that there was a significant increase in NFATc1 (at day
3 of osteoclastogenesis) and a trend of increase in ATP6v0d2 protein expression in Svs7
KO osteoclasts compared to WT.

Chapter Eight – General Summary and Future Directions
182
Plasma Membrane
Cytosol ITAM DAP12 /
FcRγ
TREM2 / OSCAR
RANKL
RANK
ITAM Co-Stimulatory Pathway RANKL Pathway
TRAF6
NF-κB
c-Fos
P
PLCγ
Ca2+
NFATc1
Auto-amplification Calcineurin
NFATc1 Transcription
IκB IκB P
Ubiquitination and degradation
Nucleus
ER
IP3
Calmodulin
Ca2+ channel (Orai1 or TRPV4 ??)
Ca2+
Svs7
22+
NFATc
Intracellular [Ca2+] increases
?
Osteoclastic Genes
DC-STAMP, ATP6v0d2, OSCAR, β3 integrin, TRAP, CTR, Cathepsin K
etc.
Figure 8.1 Hypothetical model of the role of Svs7 in the regulation of osteoclast
fusion through the Ca2+-NFATc1 signalling pathway. RANKL-induced late stage of
osteoclast differentiation (fusion) begins with the binding of RANKL to its receptor
RANK on osteoclast surface, which leads to the activation of NF-κB and ITAM co-
stimulatory signalling pathways. Subsequently, the production of IP3 by PLCγ causes
Ca2+ release from intracellular ER stores, which is accompanied by Ca2+ influx response
through Ca2+ permeable channel (Orai1 or TRPV4), to increase intracellular Ca2+ level
and at the same time to induce a long and sustain Ca2+ oscillation, necessary for the
Ca2+/calmodulin/calcineurin-dependent NFATc1 signalling pathway activation, which
has been shown to transcriptionally regulate a number of osteoclast marker genes
expression, such as DCSTAMP, ATP6v0d2, and OSCAR. Svs7, a novel osteoclast-
secreted factor, regulates Ca2+ influx/transport in osteoclasts by its possible
regulation/interaction with Orai1 or TRPV4 on osteoclast surface.

Chapter Eight – General Summary and Future Directions
183
With Svs7 KO DCSTAMP was found to be unaffected throughout the time course of
RANKL-induced osteoclastogenesis, these results indicate that Svs7 regulates osteoclast
fusion through the Ca2+-NFATc1 signalling pathway (Figure 8.1), with its main effect
on the ATP6v0d2 protein expression. The fact that only one affected fusogen can alter
osteoclast fusion has also been shown by previous studies from Hwang et al. 2012 that
showed that Orai1 (store-operated Ca2+ entry (SOCE) Ca2+ channel subunit)-deficient
mice had defects in osteoclast fusion, owing to the significant inhibition in NFATc1 and
ATP6v0d2 proteins expression but not DCSTAMP. With the fact that Orai1 provides
the major Ca2+ influx pathway for sustaining Ca2+ oscillation in hematopoietic stem
cells, from which osteoclasts are differentiated (Feske 2006; Hogan et al. 2003; Lewis
2001), and the reduced NFATc1 protein expression in Orai1 KO mice, it is tempting to
speculate that Svs7 regulates Ca2+ transport in osteoclasts through its regulation on
Orai1 (Figure 8.1). As the interaction between Svs7 and Orai1 still needs further
investigation, recent studies on transient receptor potential vanilloid (TRPV) 4 has also
shown its importance in Ca2+ entry for RANKL-induced mature osteoclast
differentiation, with TRPV4 KO mice having an impairment of mature osteoclast
differentiation and subsequent inhibition of bone resorption activity, caused by an
attenuation of Ca2+/calmodulin-NFATc1 signalling pathway (Masuyama et al. 2012;
Masuyama et al. 2008). Together, these results hint a complexity in the molecular
mechanism of Ca2+ entry and intracellular Ca2+ change during osteoclast differentiation
and the necessity for further and thorough investigation in the future (Kajiya 2012).
As bone homeostasis is maintained by balanced cell-to-cell communication between
osteoclasts and osteoblasts, the dissection into the cellular mechanism behind the
osteoporotic phenotype of Svs7 KO mice was further investigated by performing in
vitro osteoblast differentiation and mineralization assays. After confirming that, in
relative to WT, Svs7 KO primary calvarial osteoblasts exhibited an unaffected
proliferation rate, WT and KO BM differentiation into mature osteoblasts and its bone
formation activity after 14 days culture in osteogenic medium were assessed by
performing ALP and alizarin red staining, respectively. The results showed that there
were no significant differences in CFU-ALP positive colonies and total mineralized
nodules formed between WT and Svs7 KO osteoblast cultures. Together with the in
vivo calcein labelling and MAR analysis showing an unaffected bone formation activity
in Svs7 KO mice relative to WT, these results suggest that Svs7 KO mice have normal
osteoblast differentiation in vitro and exhibit an unaltered bone formation activity both

Chapter Eight – General Summary and Future Directions
184
in vitro and in vivo. The naturally low Svs7 gene expression in bone is in line with our
observations of a normal osteoblast phenotype in Svs7 KO mice. The use of osteoclast-
specific deletion of Svs7 should be considered in the future to further investigate the
possible paracrine effect of Svs7 in the regulation of osteoblast differentiation and/or
activity, together with the elucidation and confirmation of osteoclast-specific Svs7
autocrine effects.
In conclusion, this study has identified Svs7 as a regulator of bone homeostasis. Svs7
regulates osteoclast differentiation and fusion through the Ca2+-NFATc1 signalling
pathway but not osteoclast activity. With the increasing complexity in the molecular
mechanism of Ca2+ transport in osteoclasts, the regulatory role of Svs7 in this Ca2+
signalling pathway requires further investigation. The loss of Svs7 gene has been
observed not to affect osteoblast differentiation and activity. Collectively, this study
further improves our knowledge in the regulation of cell-to-cell communication
between osteoclasts and osteoblasts and hence Svs7 might represent as a therapeutic
agent against osteoclast-related osteolytic diseases.
8.2 Future Directions 8.2.1 The role of Svs7 in bone homeostasis
The studies presented here have uncovered the potential role of Svs7 in the maintenance
of bone homeostasis. By using Svs7 global KO mouse model, Svs7 has shown to
regulate osteoclast fusion through the Ca2+-NFATc1 signalling pathway. With regard to
the naturally low Svs7 gene expression in bone, including no detectable Svs7 protein
expression in WT osteoclast culture, in both culture medium and cell lysate, and the
modest phenotype observed in this study from both the Svs7 global TG and KO mice
models and still with knowledge that in the previous studies by Davey 2008 suggested
anabolic effects of treatment with recombinant purified Svs7 protein in ovariectomised
(OVX) mice, the possibility that Svs7 might still hold a more specific role in the
regulation and maintenance of bone homeostasis warrants further investigation.
First, to complete the characterisation and to confirm the bone phenotype of both Svs7
global TG and KO mice, extensive bone histomorphometry analysis, such as on
osteoclast and osteoblast area/bone surface (%), number of osteoblasts/bone surface
(N/mm), eroded area/bone surface (%), and osteoid area/bone surface (%), together with

Chapter Eight – General Summary and Future Directions
185
other essential bone parameters (trabecular bone/tissue volume, trabecular separation,
trabecular thickness, and trabecular number), should be performed in near future.
Next, to facilitate a more thorough investigation into the specific role of Svs7 in bone
homeostasis, the generation and characterisation of osteoclast-specific Svs7 conditional
TG and conditional KO mice should be performed. By incorporating common
osteoclast marker genes promoter sequence, such as Cathepsin K and TRAP, into the
targeting vectors and the use of Cre-LoxP system (Masuyama et al. 2012; Miyauchi et
al. 2010; Nakamura et al. 2007; Qin et al. 2011; Takeshita et al. 2013), osteoclast-
specific Svs7 TG and KO lines can be generated. Next, the overexpression of Svs7
protein in bone tissue and osteoclast culture (in conditioned medium and/or cell lysate)
of these osteoclast-specific TG mice should be investigated first to confirm the
successful generation of these Svs7 conditional TG mice. MicroCT and
histology/histomorphometry, together with double calcein labelling and MAR analysis,
for the bone phenotype characterisation of these osteoclast-specific Svs7 TG and KO
mice will certainly help to uncover the more specific role of Svs7 in the regulation and
maintenance of bone homeostasis, which might have been overlooked in the current
study.
8.2.2 The role of Svs7 in osteoclast and osteoblast differentiation and activation
Although these studies indicate a role for Svs7 in osteoclast fusion mechanism via the
Ca2+-NFATc1 signalling, this pathway still requires further investigation. Furthermore,
detailed investigation of in vitro osteoclast and osteoblast differentiation and activity for
the osteoclast-specific Svs7 TG and KO mice is required to confirm the regulatory role
of Svs7 in osteoclast differentiation and fusion and at the same time helps to uncover
the possible paracrine effects of Svs7 in osteoblast differentiation and activation. The
potential intrinsic role of Svs7 in the regulation of cell-to-cell communication between
osteoclast and osteoblast also requires further investigation using in vitro osteoclast and
osteoblast coculture systems.
Alternative quantitative measurements to better analyse osteoclast bone resorption
activity, e.g. measuring serum type I collagen cross-linked telopeptide (CTX) through
enzyme-linked immunosorbent assay (ELISA) (Lee et al. 2006), should be performed in
the future to rule out any direct effects of Svs7 in osteoclast activity. Serum
biochemistry measurement on Ca2+ and phosphate concentrations by using colorimetric

Chapter Eight – General Summary and Future Directions
186
assays (Masuyama et al. 2012) should also be performed to complement the analysis for
osteoclast bone resorption activity in vitro and in vivo.
The effect of retroviral induction (overexpression/rescue) on BMM-derived osteoclast
differentiation and activation should be tested alongside the characterisation of
osteoclast-specific Svs7 TG and KO mice to confirm the specific role of Svs7 in
osteoclasts. With difficulties in detecting Svs7 protein in culture medium (supernatant)
of RANKL-induced BMM differentiation into osteoclasts, immunofluorescence using
specific Svs7 antibody and imaging method using confocal microscopy on these
retrovirally-induced (overexpressed) osteoclasts (Pavlos et al. 2011; Qin et al. 2011)
should be carried out to locate specific expression of Svs7 in osteoclasts.
Intracellular Ca2+ measurement using fura-2 fluorescent probe on both osteoclasts and
osteoblasts of the osteoclast-specific Svs7 TG and KO mice, in which emission ratio of
alternated 340/380nm excitation wavelength can be recorded (Miyamoto et al. 2012), is
necessary to be performed to repeat the Fluo-4AM calcium assay results in this current
study and to confirm the potential regulatory role of Svs7 in both osteoclasts and
osteoblasts Ca2+ transport system, particularly in response to high extracellular Ca2+,
which remains poorly understood. The incorporation of thapsigargin, an ATPase Ca2+
transport inhibitor at ER store (Hwang & Putney Jr 2011), should also be considered in
the future intracellular Ca2+ study to specifically investigate the potential regulatory role
of Svs7 in Orai1-regulated Ca2+ influx in the store-operated Ca2+ entry (SOCE) system,
which has been shown to have a crucial role in mediating the Ca2+/NFATc1 signalling
pathway activation (Deng et al. 2009; Feske 2006; Feske 2009; Hogan et al. 2003;
Hwang & Putney 2012). Moreover, this future study on the potential role of Svs7 in the
regulation of Ca2+ transport in osteoblasts in response to high extracellular Ca2+ can give
another light of mechanism in the regulation and formation of Ca2+ phosphate
(Ca3(PO4)2) vesicles in osteoblasts, required for Ca2+ deposition on new bone-forming
surfaces (Boonrungsiman et al. 2012).
To further dissect the regulatory role of Svs7 in NFATc1 protein expression,
particularly in osteoclast fusion mechanism, first, cytoplasmic and nuclear fractionation
on cell lysates of time course RANKL-induced osteoclast differentiation should be
conducted and hence the results can therefore clearly demonstrate the effect of Svs7 in
the regulation of NFATc1 protein expression, both in cytoplasm and nucleus. Secondly,

Chapter Eight – General Summary and Future Directions
187
immunofluorescence and confocal microscopy should be performed on Svs7
conditional TG and KO-derived osteoclasts to detect and analyse NFATc1 translocation
into the nucleus and hence to confirm the regulatory role of Svs7 in NFATc1 signalling
pathway. The investigation of ATP6v0d2 and DCSTAMP fusogenic proteins
expression, two main players in osteoclast fusion mechanism (Kim et al. 2008; Lee et
al. 2006; Yagi et al. 2005), in the osteoclast-specific Svs7 TG and KO mice still needs
to be carried out to get a conclusive mark for the role of Svs7 in osteoclast fusion.
Finally, the putative binding of Svs7 on key bone cells, such as chondrocytes,
osteoclasts, osteoblasts, and osteocytes, and the potential interacting partner for Svs7 in
bone cells environment are still unknown and therefore need to be investigated. First,
flow cytometry experiments on bone cells, treated with recombinant purified Svs7
protein and stained with specific Svs7 antibody and fluorochrome-conjugated secondary
antibody, should be performed to detect and analyse the putative binding of Svs7 on
major bone cells. Secondly, to investigate the potential interacting partner for Svs7,
random screening using surface plasmon resonance (SPR) should be performed (Canalis
et al. 2010; Schneeweis, Willard & Milla 2005; Theoleyre et al. 2006). In this
technique, Svs7 protein, acting as a ligand, will be placed in the biosensor, while a clear
cell lysate of WT osteoclasts (‘the analyte’) containing numerous proteins, passes
through over the other side of the biosensor site. A protein-protein interaction will cause
a change in the refractive index, which is proportional to the mass added in the sensor
surface, followed by the measurement of dissociation constant (KD) of the interaction.
The protein-protein interaction can later be confirmed by performing co-
immunoprecipitation and/or pull down experiments (Masuyama et al. 2012; Pavlos et
al. 2011). The identification of Svs7 binding partner will lead us to a better
understanding about the role and function of Svs7 in bone microenvironment.
In conclusion, this study documents, for the first time, the role of Svs7 in bone
homeostasis. Svs7 has shown to play a role in regulating osteoclast fusion through the
Ca2+-NFATc1 signalling pathway. Considering the numerous limitations being
encountered in this study, including i) the low Svs7 overexpression in Svs7 TG mice
and ii) the modest phenotype observed in Svs7 KO mice (mild effects of Svs7 in
intracellular Ca2+ study and osteoclast fusion proteins expression), further investigation
is required to fully elucidate the precise contribution of Svs7 in osteoclast fusion and
maintenance of bone homeostasis.

188
CHAPTER 9
BIBLIOGRAPHY

Chapter Nine - Bibliography
189
Adermann, K, Wattler, F, Wattler, S, Heine, G, Meyer, M, Forssmann, W-g & Nehls, M
1999, 'Structural and phylogenetic characterization of human SLURP1, the first
secreted mammalian member of the Ly6/uPAR protein superfamily', Protein
science, vol. 8, no. 4, pp. 810-819.
Aguirre Ghiso, J 2002, 'Inhibition of FAK signaling activated by urokinase receptor
induces dormancy in human carcinoma cells in vivo', Oncogene, vol. 21, no. 16,
p. 2513.
Aitken, JM, Armstrong, E & Anderson, JB 1972, 'Osteoporosis after oophorectomy in
the mature female rat and the effect of estrogen and/or progesterone replacement
therapy in its prevention', J Endocrinol vol. 55, pp. 79-87.
Akiyama, H, Chaboissier, M-c, Martin, JF, Schedl, A & de Crombrugghe, B 2002, 'The
transcription factor Sox9 has essential roles in successive steps of the
chondrocyte differentiation pathway and is required for expression of Sox5 and
Sox6', Genes & development, vol. 16, no. 21, p. 2813.
Albagha, OME, Visconti, MR, Alonso, N, Langston, AL, Cundy, T, Dargie, R, Dunlop,
MG, Fraser, WD, Hooper, MJ, Isaia, G, Nicholson, GC, Montes, JD, Gonzalez-
Sarmiento, R, di Stefano, M, Tenesa, A, Walsh, JP & Ralston, SH 2010,
'Genome-wide association study identifies variants at CSF1, OPTN and
TNFRSF11A as genetic risk factors for Paget's disease of bone', Nature
Genetics, vol. 42, no. 6, pp. 520-U26.
Allan, E, Allan, K, Hausler, T, Wei, J, Gooi, J, Quinn, B, Crimeen Irwin, S, Pompolo,
N, Sims, M, Gillespie, J & Onyia, TJ 2008, 'EphrinB2 Regulation by PTH and
PTHrP Revealed by Molecular Profiling in Differentiating Osteoblasts', Journal
of bone and mineral research, vol. 23, no. 8, pp. 1170-1181.
Arredondo, J, Chernyavsky, AI, Jolkovsky, DL, Webber, RJ & Grando, SA 2006,
'SLURP2: A novel cholinergic signaling peptide in human mucocutaneous
epithelium', Journal of cellular physiology, vol. 208, no. 1, pp. 238-245.
Arredondo, J, Chernyavsky, AI, Webber, RJ & Grando, SA 2005, 'Biological effects of
SLURP-1 on human keratinocytes', J Invest Dermatol, vol. 125, no. 6, pp. 1236-
41.
Aubin, EJ & Triffitt, TJ 2002, 'Mesenchymal stem cells and osteoblast differentiation',
Principles of Bone Biology, London: Academic Press, pp. 59-81.
Aubin, J, Bilezikian, JP, Raisz, LG & Martin, TJ 2008, Mesenchymal Stem Cells and
Osteoblast Differentiation Principles of Bone Biology (Third Edition).

Chapter Nine - Bibliography
190
Baek, W-Y, Lee, M-A, Jung, JW, Kim, S-Y, Akiyama, H, de Crombrugghe, B & Kim,
J-E 2009, 'Positive Regulation of Adult Bone Formation by Osteoblast-Specific
Transcription Factor Osterix', Journal of bone and mineral research, vol. 24, no.
6, pp. 1055-1065.
Bafico, A, Liu, G, Yaniv, A, Gazit, A & Aaronson, SA 2001, 'Novel mechanism of Wnt
signalling inhibition mediated by Dickkopf-1 interaction with LRP6/Arrow', Nat
Cell Biol, vol. 3, no. 7, pp. 683-6.
Baker, AR, Hollingshead, PG, Pitts-Meek, S, Hansen, S, Taylor, R & Stewart, TA 1992,
'Osteoblast-specific expression of growth hormone stimulates bone growth in
transgenic mice', Mol Cell Biol, vol. 12, no. 12, pp. 5541-7.
Bandyopadhyay, A, Tsuji, K, Cox, K, Harfe, BD, Rosen, V & Tabin, CJ 2006, 'Genetic
Analysis of the Roles of BMP2, BMP4, and BMP7 in Limb Patterning and
Skeletogenesis', PLoS Genet, vol. 2, no. 12, p. e216.
Baron, R 1985, 'Cell-Mediated Extracellular Acidification and Bone Resorption:
Evidence for a Low pH in Resorbing Lacunae and Localization of a 100-kD
Lysosomal Membrane Protein at the Osteoclast Ruffled Border', The Journal of
cell biology, vol. 101, no. 6, pp. 2210-2222.
Baron, R, Neff, L, Louvard, D & Courtoy, PJ 1985, 'Cell-Mediated Extracellular
Acidification and Bone-Resorption - Evidence for a Low Ph in Resorbing
Lacunae and Localization of a 100-Kd Lysosomal Membrane-Protein at the
Osteoclast Ruffled Border', Journal of Cell Biology, vol. 101, no. 6, pp. 2210-
2222.
Blair, HC, Teitelbaum, SL, Ghiselli, R & Gluck, S 1989, 'Osteoclastic bone resorption
by a polarized vacuolar proton pump', Science, vol. 245, no. 4920, pp. 855-7.
Bodine, PVN, Zhao, WG, Kharode, YP, Bex, FJ, Lambert, AJ, Goad, MB, Gaur, T,
Stein, GS, Lian, JB & Komm, BS 2004, 'The Wnt antagonist secreted frizzled-
related protein-1 is a negative regulator of trabecular bone formation in adult
mice', Molecular endocrinology, vol. 18, no. 5, pp. 1222-1237.
Bone, HG, McClung, MR, Roux, C, Recker, RR, Eisman, JA, Verbruggen, N, Hustad,
CM, DaSilva, C, Santora, AC & Ince, BA 2010, 'Odanacatib, a cathepsin-K
inhibitor for osteoporosis: A two-year study in postmenopausal women with low
bone density', Journal of bone and mineral research, vol. 25, no. 5, pp. 937-947.
Bonyadi, M, Waldman, SD, Liu, D, Aubin, JE, Grynpas, MD & Stanford, WL 2003,
'Mesenchymal progenitor self-renewal deficiency leads to age-dependent

Chapter Nine - Bibliography
191
osteoporosis in Sca-1/Ly-6A null mice', Proceedings of the National Academy of
Sciences of the United States of America, vol. 100, no. 10, p. 5840.
Boonrungsiman, S, Gentleman, E, Carzaniga, R, Evans, ND, McComb, DW, Porter, AE
& Stevens, MM 2012, 'The role of intracellular calcium phosphate in osteoblast-
mediated bone apatite formation', Proceedings of the National Academy of
Sciences of the United States of America, vol. 109, no. 35, pp. 14170-14175.
Boyce, BF, Yoneda, T, Lowe, C, Soriano, P & Mundy, GR 1992, 'Requirement of
pp60c-src expression for osteoclasts to form ruffled borders and resorb bone in
mice', The Journal of clinical investigation, vol. 90, no. 4, pp. 1622-1627.
Boyden, LM, Mao, J, Belsky, J, Mitzner, L, Farhi, A, Mitnick, MA, Wu, D, Insogna, K
& Lifton, RP 2002, 'High Bone Density Due to a Mutation in LDL-Receptor-
Related Protein 5', The New England journal of medicine, vol. 346, no. 20, pp.
1513-1521.
Boyle, WJ, Simonet, WS & Lacey, DL 2003, 'Osteoclast differentiation and activation',
Nature, vol. 423, no. 6937, pp. 337-42.
Bu, R, Borysenko, CW, Li, Y, Cao, L, Sabokbar, A & Blair, HC 2003, 'Expression and
function of TNF-family proteins and receptors in human osteoblasts☆', Bone,
vol. 33, no. 5, pp. 760-770.
Bucay, N, Sarosi, I, Dunstan, CR, Morony, S, Tarpley, J, Capparelli, C, Scully, S, Tan,
HL, Xu, W, Lacey, DL, Boyle, WJ & Simonet, WS 1998, 'osteoprotegerin-
deficient mice develop early onset osteoporosis and arterial calcification', Genes
Dev, vol. 12, no. 9, pp. 1260-8.
Burge, R, Burge, B, Dawson Hughes, D, Solomon, J, Wong, A & King, A 2007,
'Incidence and Economic Burden of Osteoporosis-Related Fractures in the
United States, 2005-2025', Journal of bone and mineral research, vol. 22, no. 3,
pp. 465-475.
Burgess, TL, Qian, Y, Kaufman, S, Ring, BD, Van, G, Capparelli, C, Kelley, M, Hsu,
H, Boyle, WJ, Dunstan, CR, Hu, S & Lacey, DL 1999, 'The ligand for
osteoprotegerin (OPGL) directly activates mature osteoclasts', J Cell Biol, vol.
145, no. 3, pp. 527-38.
Canalis, E, Smerdel-Ramoya, A, Durant, D, Economides, AN, Beamer, WG & Zanotti,
S 2010, 'Nephroblastoma Overexpressed (Nov) Inactivation Sensitises
Osteoblasts to Bone Morphogenetic Protein-2, But Nov is Dispensable for
Skeletal Homeostasis', Endocrinology, vol. 151, no. 1, pp. 221-233.

Chapter Nine - Bibliography
192
Carmeliet, P, Moons, L, Lijnen, R, Baes, M, Lemaitre, V, Tipping, P, Drew, A,
Eeckhout, Y, Shapiro, S, Lupu, F & Collen, D 1997, 'Urokinase-generated
plasmin activates matrix metalloproteinases during aneurysm formation', Nat
Genet, vol. 17, no. 4, pp. 439-44.
Chen, D, Zhao, M & Mundy, GR 2004, 'Bone Morphogenetic Proteins', Growth
Factors, vol. 22, no. 4, pp. 233-241.
Chimienti, F, Hogg, RC, Plantard, L, Lehmann, C, Brakch, N, Fischer, J, Huber, M,
Bertrand, D & Hohl, D 2003, 'Identification of SLURP-1 as an epidermal
neuromodulator explains the clinical phenotype of Mal de Meleda', Human
molecular genetics, vol. 12, no. 22, pp. 3017-3024.
Clarke, B 2008, 'Normal bone anatomy and physiology', Clin J Am Soc Nephrol, vol. 3
Suppl 3, no. Supplement 3, pp. S131-9.
Cobb, MH & Goldsmith, EJ 1995, 'How MAP Kinases Are Regulated', Journal of
biological chemistry, vol. 270, no. 25, pp. 14843-14846.
Coronel, CE, San Agustin, J & Lardy, HA 1988, 'Identification and partial
characterization of caltrin-like proteins in the reproductive tract of the guinea
pig', Biol Reprod, vol. 38, no. 3, pp. 713-22.
Coronel, CE, Winnica, DE, Novella, ML & Lardy, HA 1992, 'Purification, structure,
and characterization of caltrin proteins from seminal vesicle of the rat and
mouse', Journal of biological chemistry, vol. 267, no. 29, pp. 20909-20915.
Crabtree, GR & Olson, EN 2002, 'NFAT signaling: choreographing the social lives of
cells', Cell, vol. 109 Suppl, no. 2, Supplement 1, pp. S67-79.
Crotti, TN, Flannery, M, Walsh, NC, Fleming, JD, Goldring, SR & McHugh, KP 2006,
'NFATc1 regulation of the human β3 integrin promoter in osteoclast
differentiation', Gene, vol. 372, no. 0, pp. 92-102.
Davey, RA, Turner, AG, McManus, JF, Chiu, WS, Tjahyono, F, Moore, AJ, Atkins, GJ,
Anderson, PH, Ma, C, Glatt, V, MacLean, HE, Vincent, C, Bouxsein, M,
Morris, HA, Findlay, DM & Zajac, JD 2008, 'Calcitonin receptor plays a
physiological role to protect against hypercalcemia in mice', J Bone Miner Res,
vol. 23, no. 8, pp. 1182-93.
Davey, T 2008, Functional characterisation of a novel osteoclast-derived factor.
Degryse, B, Resnati, M, Czekay, RP, Loskutoff, DJ & Blasi, F 2005, 'Domain 2 of the
urokinase receptor contains an integrin-interacting epitope with intrinsic
signaling activity: generation of a new integrin inhibitor', J Biol Chem, vol. 280,
no. 26, pp. 24792-803.

Chapter Nine - Bibliography
193
Del Rosso, M, Fibbi, G, Pucci, M, Margheri, F & Serrati, S 2008, 'The plasminogen
acitvation system in inflammation', Frontier in Bioscience, vol. 13, pp. 4667-
4686.
Delaissé, J-M, Andersen, TL, Engsig, MT, Henriksen, K, Troen, T & Blavier, L 2003,
'Matrix metalloproteinases (MMP) and cathepsin K contribute differently to
osteoclastic activities', Microscopy Research and Technique, vol. 61, no. 6, pp.
504-513.
Delmas, P 2002, 'Treatment of postmenopausal osteoporosis', Lancet, vol. 359, no.
9322, pp. 2018-2026.
Dempster, DW, Lambing, CL, Kostenuik, PJ & Grauer, A 2012, 'Role of RANK ligand
and denosumab, a targeted RANK ligand inhibitor, in bone health and
osteoporosis: a review of preclinical and clinical data', Clin Ther, vol. 34, no. 3,
pp. 521-36.
Deng, X, Wang, Y, Zhou, Y, Soboloff, J & Gill, DL 2009, 'STIM and Orai: Dynamic
Intermembrane Coupling to Control Cellular Calcium Signals', Journal of
biological chemistry, vol. 284, no. 34, pp. 22501-22505.
Dennis, JE, Merriam, A, Awadallah, A, Yoo, JU, Johnstone, B & Caplan, AI 1999, 'A
Quadripotential Mesenchymal Progenitor Cell Isolated from the Marrow of an
Adult Mouse', Journal of bone and mineral research, vol. 14, no. 5, pp. 700-
709.
Drake, FH, Dodds, RA, James, IE, Connor, JR, Debouck, C, Richardson, S, Lee-
Rykaczewski, E, Coleman, L, Rieman, D, Barthlow, R, Hastings, G & Gowen,
M 1996, 'Cathepsin K, but Not Cathepsins B, L, or S, Is Abundantly Expressed
in Human Osteoclasts', Journal of biological chemistry, vol. 271, no. 21, pp.
12511-12516.
Ducy, P, Starbuck, M, Priemel, M, Shen, J, Pinero, G, Geoffroy, V, Amling, M &
Karsenty, G 1999, 'A Cbfa1-dependent genetic pathway controls bone formation
beyond embryonic development', Genes Dev, vol. 13, no. 8, pp. 1025-36.
Ducy, P, Zhang, R, Geoffroy, V, Ridall, AL & Karsenty, G 1997, 'Osf2/Cbfa1: A
Transcriptional Activator of Osteoblast Differentiation', Cell, vol. 89, no. 5, pp.
747-754.
Duong, LT, Lakkakorpi, PT, Nakamura, I, Machwate, M, Nagy, RM & Rodan, GA
1998, 'PYK2 in osteoclasts is an adhesion kinase, localized in the sealing zone,
activated by ligation of alpha(v)beta3 integrin, and phosphorylated by src
kinase', The Journal of clinical investigation, vol. 102, no. 5, pp. 881-892.

Chapter Nine - Bibliography
194
Dvorak-Ewell, MM, Chen, TH, Liang, N, Garvey, C, Liu, B, Tu, C, Chang, W, Bikle,
DD & Shoback, DM 2011, 'Osteoblast extracellular Ca2+ -sensing receptor
regulates bone development, mineralization, and turnover', J Bone Miner Res,
vol. 26, no. 12, pp. 2935-47.
Eapen, M, Davies, SM, Ramsay, NK & Orchard, PJ 1998, 'Hematopoietic stem cell
transplantation for infantile osteopetrosis', Bone Marrow Transplant, vol. 22, no.
10, pp. 941-6.
Eghbali-Fatourechi, G, Khosla, S, Sanyal, A, Boyle, WJ, Lacey, DL & Riggs, BL 2003,
'Role of RANK ligand in mediating increased bone resorption in early
postmenopausal women', J Clin Invest, vol. 111, no. 8, pp. 1221-30.
EMA, 'European Public Assessment Report - Prolia', EMA website (online).
Epstein, S 2006, 'Update of current therapeutic options for the treatment of
postmenopausal osteoporosis', Clin Ther, vol. 28, no. 2, pp. 151-73.
Everts, V, Delaissé, J-M, Korper, W, Jansen, D, Tigchelaar-Gutter, W & Saftig, P 2002,
'The bone lining cell: its role in cleaning Howship's lacunae and initiating bone
formation', Journal of bone and mineral research, vol. 12, pp. 77-90.
FDA, 'FDA labelling information - Prolia (denosumab)', FDA website (online).
Felix, R, Cecchini, MG & Fleisch, H 1990, 'Macrophage colony stimulating factor
restores in vivo bone resorption in the op/op osteopetrotic mouse',
Endocrinology, vol. 127, no. 5, pp. 2592-4.
Feng, H, Cheng, T, Pavlos, NJ, Yip, KHM, Carrello, A, Seeber, R, Eidne, K, Zheng,
MH & Xu, J 2008, 'Cytoplasmic Terminus of Vacuolar Type Proton Pump
Accessory Subunit Ac45 Is Required for Proper Interaction with V0 Domain
Subunits and Efficient Osteoclastic Bone Resorption', Journal of biological
chemistry, vol. 283, no. 19, pp. 13194-13204.
Feske, S 2006, 'A mutation in Orai1 causes immune deficiency by abrogating CRAC
channel function', Nature, vol. 441, no. 7090, pp. 179-85.
Feske, S 2009, 'ORAI1 and STIM1 deficiency in human and mice: roles of store-
operated Ca2+ entry in the immune system and beyond', Immunological
Reviews, vol. 231, no. 1, pp. 189-209.
Fischer, J, Bouadjar, B, Heilig, R, Huber, M, Lefèvre, C, Jobard, F, Macari, F, Bakija-
Konsuo, A, Ait-Belkacem, F, Weissenbach, J, Lathrop, M, Hohl, D &
Prud’homme, J-F 2001, 'Mutations in the gene encoding SLURP-1 in Mal de
Meleda', Human molecular genetics, vol. 10, no. 8, pp. 875-880.

Chapter Nine - Bibliography
195
Fleisch, H 2000, 'Bisphosphanate in bone disease: from the laboratory to the patient, 4th
edn', San Diego: Academic Press.
Franzoso, G, Carlson, L, Xing, L, Poljak, L, Shores, EW, Brown, KD, Leonardi, A,
Tran, T, Boyce, BF & Siebenlist, U 1997, 'Requirement for NF-kappaB in
osteoclast and B-cell development', Genes Dev, vol. 11, no. 24, pp. 3482-96.
Frattini, A, Orchard, PJ, Sobacchi, C, Giliani, S, Abinun, M, Mattsson, JP, Keeling, DJ,
Andersson, A-K, Wallbrandt, P, Zecca, L, Notarangelo, LD, Vezzoni, P & Villa,
A 2000, 'Defects in TCIRG1 subunit of the vacuolar proton pump are
responsible for a subset of human autosomal recessive osteopetrosis.(Report)',
Nature Genetics, vol. 25, no. 3, p. 343.
Frattini, A, Pangrazio, A, Susani, L, Sobacchi, C, Mirolo, M, Abinun, M, Andolina, M,
Flanagan, A, Horwitz, EM, Mihci, E, Notarangelo, LD, Ramenghi, U, Teti, A,
Van Hove, J, Vujic, D, Young, T, Albertini, A, Orchard, PJ, Vezzoni, P & Villa,
A 2003, 'Chloride channel ClCN7 mutations are responsible for severe
recessive, dominant, and intermediate osteopetrosis', J Bone Miner Res, vol. 18,
no. 10, pp. 1740-7.
Fujita, K, Iwasaki, M, Ochi, H, Fukuda, T, Ma, C, Miyamoto, T, Takitani, K, Negishi-
Koga, T, Sunamura, S, Kodama, T, Takayanagi, H, Tamai, H, Kato, S, Arai, H,
Shinomiya, K, Itoh, H, Okawa, A & Takeda, S 2012, 'Vitamin E decreases bone
mass by stimulating osteoclast fusion', Nat Med, vol. 18, no. 4, pp. 589-94.
Fuller, K, Murphy, C, Kirstein, B, Fox, SW & Chambers, TJ 2002, 'TNFα Potently
Activates Osteoclasts, through a Direct Action Independent of and Strongly
Synergistic with RANKL', Endocrinology, vol. 143, no. 3, pp. 1108-1118.
Gauthier, JY, Chauret, N, Cromlish, W, Desmarais, S, Duong le, T, Falgueyret, JP,
Kimmel, DB, Lamontagne, S, Leger, S, LeRiche, T, Li, CS, Masse, F, McKay,
DJ, Nicoll-Griffith, DA, Oballa, RM, Palmer, JT, Percival, MD, Riendeau, D,
Robichaud, J, Rodan, GA, Rodan, SB, Seto, C, Therien, M, Truong, VL, Venuti,
MC, Wesolowski, G, Young, RN, Zamboni, R & Black, WC 2008, 'The
discovery of odanacatib (MK-0822), a selective inhibitor of cathepsin K', Bioorg
Med Chem Lett, vol. 18, no. 3, pp. 923-8.
Geiser, AG, Zeng, QQ, Sato, M, Helvering, LM, Hirano, T & Turner, CH 1998,
'Decreased bone mass and bone elasticity in mice lacking the transforming
growth factor-β1 gene', Bone, vol. 23, no. 2, pp. 87-93.

Chapter Nine - Bibliography
196
Gelb, BD, Shi, GP, Chapman, HA & Desnick, RJ 1996, 'Pycnodysostosis, a lysosomal
disease caused by cathepsin K deficiency', Science, vol. 273, no. 5279, pp. 1236-
8.
Geoffroy, V, Kneissel, M, Fournier, B, Boyde, A & Matthias, P 2002, 'High bone
resorption in adult aging transgenic mice overexpressing cbfa1/runx2 in cells of
the osteoblastic lineage', Mol Cell Biol, vol. 22, no. 17, pp. 6222-33.
Glantschnig, H, Fisher, JE, Wesolowski, G, Rodan, GA & Reszka, AA 2003, 'M-CSF,
TNFalpha and RANK ligand promote osteoclast survival by signaling through
mTOR/S6 kinase', Cell Death and Differentiation, vol. 10, no. 10, pp. 1165-77.
Goltzman, D 2008, 'Studies on the mechanisms of the skeletal anabolic action of
endogenous and exogenous parathyroid hormone', Arch Biochem Biophys, vol.
473, no. 2, pp. 218-24.
Gong, Y, Slee, RB, Fukai, N, Rawadi, G, Roman-Roman, S, Reginato, AM, Wang, H,
Cundy, T, Glorieux, FH, Lev, D, Zacharin, M, Oexle, K, Marcelino, J, Suwairi,
W, Heeger, S, Sabatakos, G, Apte, S, Adkins, WN, Allgrove, J, Arslan-
Kirchner, M, Batch, JA, Beighton, P, Black, GCM, Boles, RG, Boon, LM,
Borrone, C, Brunner, HG, Carle, GF, Dallapiccola, B, De Paepe, A, Floege, B,
Halfhide, ML, Hall, B, Hennekam, RC, Hirose, T, Jans, A, Jüppner, H, Kim,
CA, Keppler-Noreuil, K, Kohlschuetter, A, LaCombe, D, Lambert, M, Lemyre,
E, Letteboer, T, Peltonen, L, Ramesar, RS, Romanengo, M, Somer, H, Steichen-
Gersdorf, E, Steinmann, B, Sullivan, B, Superti-Furga, A, Swoboda, W, van den
Boogaard, M-J, Van Hul, W, Vikkula, M, Votruba, M, Zabel, B, Garcia, T,
Baron, R, Olsen, BR & Warman, ML 2001, 'LDL Receptor-Related Protein 5
(LRP5) Affects Bone Accrual and Eye Development', Cell, vol. 107, no. 4, pp.
513-523.
Gowen, M, Chapman, K, Littlewood, A, Hughes, D, Evans, D & Russell, G 1990,
'Production of tumor necrosis factor by human osteoblasts is modulated by other
cytokines, but not by osteotropic hormones', Endocrinology, vol. 126, no. 2, pp.
1250-5.
Grigoriadis, AE, Wang, ZQ, Cecchini, MG, Hofstetter, W, Felix, R, Fleisch, HA &
Wagner, EF 1994, 'c-Fos: a key regulator of osteoclast-macrophage lineage
determination and bone remodeling', Science, vol. 266, no. 5184, pp. 443-8.
Gruber, BL, Sorbi, D, French, DL, Marchese, MJ, Nuovo, GJ, Kew, RR & Arbeit, LA
1996, 'Markedly Elevated Serum MMP-9 (Gelatinase B) Levels in Rheumatoid

Chapter Nine - Bibliography
197
Arthritis: A Potentially Useful Laboratory Marker', Clinical Immunology and
Immunopathology, vol. 78, no. 2, pp. 161-171.
Guerrini, MM, Sobacchi, C, Cassani, B, Abinun, M, Kilic, SS, Pangrazio, A, Moratto,
D, Mazzolari, E, Clayton-Smith, J, Orchard, P, Coxon, FP, Helfrich, MH,
Crockett, JC, Mellis, D, Vellodi, A, Tezcan, I, Notarangelo, LD, Rogers, MJ,
Vezzoni, P, Villa, A & Frattini, A 2008, 'Human Osteoclast-Poor Osteopetrosis
with Hypogammaglobulinemia due to TNFRSF11A (RANK) Mutations', The
American Journal of Human Genetics, vol. 83, no. 1, pp. 64-76.
Gussoni, E, Soneoka, Y, Strickland, CD, Buzney, EA, Khan, MK, Flint, AF, Kunkel,
LM & Mulligan, RC 1999, 'Dystrophin expression in the mdx mouse restored by
stem cell transplantation', Nature, vol. 401, no. 6751, pp. 390-4.
Haibo, Z, Guoping, C, Jingyuan, D, Zhidao, X, Lan, W & Tongbo, Z 1997, 'Expression
of matrix metalloproteinase-9 mRNA in osteoporotic bone tissues', Journal of
Huazhong University of Science and Technology Medical Sciences vol. 17, no.
1, pp. 28-31.
Harada, S & Rodan, GA 2003, 'Control of osteoblast function and regulation of bone
mass', Nature, vol. 423, no. 6937, pp. 349-55.
Hayashi, M, Nakashima, T, Taniguchi, M, Kodama, T, Kumanogoh, A & Takayanagi,
H 2012, 'Osteoprotection by semaphorin 3A', Nature, vol. 485, no. 7396, pp. 69-
74.
Hayden, JM, Mohan, S & Baylink, DJ 1995, 'The insulin-like growth factor system and
the coupling of formation to resorption', Bone, vol. 17, no. 2, Supplement 1, pp.
S93-S98.
Hayman, AR, Jones, SJ, Boyde, A, Foster, D, Colledge, WH, Carlton, MB, Evans, MJ
& Cox, TM 1996, 'Mice lacking tartrate-resistant acid phosphatase (Acp 5) have
disrupted endochondral ossification and mild osteopetrosis', Development, vol.
122, no. 10, pp. 3151-3162.
He, Y, Staser, K, Rhodes, SD, Liu, Y, Wu, X, Park, SJ, Yuan, J, Yang, X, Li, X, Jiang,
L, Chen, S & Yang, FC 2011, 'Erk1 positively regulates osteoclast
differentiation and bone resorptive activity', PLoS ONE, vol. 6, no. 9, p. e24780.
Heath, D, Heath, A, Chantry, C, Buckle, L, Coulton, J, Shaughnessy, H, Evans, J,
Snowden, D, Stover, K & Vanderkerken, P 2009, 'Inhibiting Dickkopf-1 (Dkk1)
Removes Suppression of Bone Formation and Prevents the Development of
Osteolytic Bone Disease in Multiple Myeloma', Journal of bone and mineral
research, vol. 24, no. 3, pp. 425-436.

Chapter Nine - Bibliography
198
Hering, SFH, Isken, FFH, Knabbe, CFH, Janott, JFH, Jost, CFH, Pommer, AFH, Muhr,
GFH, Schatz, HFH & Pfeiffer, AFH 2001, 'TGF beta 1 and TGF beta 2 mRNA
and protein expression in human bone samples', Experimental and clinical
endocrinology & diabetes, vol. 109, no. 04, pp. 217-226.
Hock, JM, Canalis, E & Centrella, M 1990, 'Transforming Growth Factor-β Stimulates
Bone Matrix Apposition and Bone Cell Replication in Cultured Fetal Rat
Calvariae', Endocrinology, vol. 126, no. 1, pp. 421-426.
Hocking, LJ, Herbert, CA, Nicholls, RK, Williams, F, Bennett, ST, Cundy, T,
Nicholson, GC, Wuyts, W, Van Hul, W & Ralston, SH 2001, 'Genomewide
search in familial Paget disease of bone shows evidence of genetic heterogeneity
with candidate loci on chromosomes 2q36, 10p13, and 5q35', American journal
of human genetics, vol. 69, no. 5, pp. 1055-1061.
Hogan, PG, Chen, L, Nardone, J & Rao, A 2003, 'Transcriptional regulation by calcium,
calcineurin, and NFAT', Genes Dev, vol. 17, no. 18, pp. 2205-32.
Holmes, C, Khan, TS, Owen, C, Ciliberti, N, Grynpas, MD & Stanford, WL 2007,
'Longitudinal Analysis of Mesenchymal Progenitors and Bone Quality in the
Stem Cell Antigen-1–Null Osteoporotic Mouse', Journal of bone and mineral
research, vol. 22, no. 9, pp. 1373-1386.
Horner, A, Kemp, P, Summers, C, Bord, S, Bishop, NJ, Kelsall, AW, Coleman, N &
Compston, JE 1998, 'Expression and distribution of transforming growth factor-
beta isoforms and their signaling receptors in growing human bone', Bone, vol.
23, no. 2, pp. 95-102.
Horowitz, MC 1993, 'Cytokines and estrogen in bone: anti-osteoporotic effects',
Science, vol. 260, no. 5108, pp. 626-7.
Horwood, NJ, Elliott, J, Martin, TJ & Gillespie, MT 1998, 'Osteotropic Agents Regulate
the Expression of Osteoclast Differentiation Factor and Osteoprotegerin in
Osteoblastic Stromal Cells', Endocrinology, vol. 139, no. 11, p. 4743.
Huang, Z, Nelson, ER, Smith, RL & Goodman, SB 2007, 'The sequential expression
profiles of growth factors from osteoprogenitors [correction of
osteroprogenitors] to osteoblasts in vitro', Tissue Eng, vol. 13, no. 9, pp. 2311-
20.
Hughes, FJ, Aubin, JE & Heersche, JNM 1992, 'Differential chemotactic responses of
different populations of fetal rat calvaria cells to platelet-derived growth factor
and transforming growth factor β', Bone and Mineral, vol. 19, no. 1, pp. 63-74.

Chapter Nine - Bibliography
199
Hwang, S-Y & Putney Jr, JW 2011, 'Calcium signaling in osteoclasts', Biochimica et
Biophysica Acta (BBA) - Molecular Cell Research, vol. 1813, no. 5, pp. 979-
983.
Hwang, SY & Putney, JW 2012, 'Orai1-mediated calcium entry plays a critical role in
osteoclast differentiation and function by regulating activation of the
transcription factor NFATc1', FASEB J, vol. 26, no. 4, pp. 1484-92.
Ikeda, F, Nishimura, R, Matsubara, T, Tanaka, S, Inoue, J, Reddy, SV, Hata, K,
Yamashita, K, Hiraga, T, Watanabe, T, Kukita, T, Yoshioka, K, Rao, A &
Yoneda, T 2004, 'Critical roles of c-Jun signaling in regulation of NFAT family
and RANKL-regulated osteoclast differentiation', J Clin Invest, vol. 114, no. 4,
pp. 475-84.
Inada, M, Yasui, T, Nomura, S, Miyake, S, Deguchi, K, Himeno, M, Sato, M,
Yamagiwa, H, Kimura, T, Yasui, N, Ochi, T, Endo, N, Kitamura, Y, Kishimoto,
T & Komori, T 1999, 'Maturational disturbance of chondrocytes in Cbfa1-
deficient mice', Developmental Dynamics, vol. 214, no. 4, pp. 279-290.
Iotsova, V, Caamano, J, Loy, J, Yang, Y, Lewin, A & Bravo, R 1997, 'Osteopetrosis in
mice lacking NF-kappaB1 and NF-kappaB2', Nat Med, vol. 3, no. 11, pp. 1285-
9.
Irie, N, Takada, Y, Watanabe, Y, Matsuzaki, Y, Naruse, C, Asano, M, Iwakura, Y,
Suda, T & Matsuo, K 2009, 'Bidirectional Signaling through EphrinA2-EphA2
Enhances Osteoclastogenesis and Suppresses Osteoblastogenesis', Journal of
biological chemistry, vol. 284, no. 21, pp. 14637-14644.
Ishii, M, Egen, JG, Klauschen, F, Meier-Schellersheim, M, Saeki, Y, Vacher, J, Proia,
RL & Germain, RN 2009, 'Sphingosine-1-phosphate mobilizes osteoclast
precursors and regulates bone homeostasis.(LETTERS)(Report)', Nature, vol.
458, no. 7237, p. 524.
Ito, CY, Li, CYJ, Bernstein, A, Dick, JE & Stanford, WL 2003, 'Hematopoietic stem
cell and progenitor defects in Sca-1/Ly-6A–null mice', Blood, vol. 101, no. 2,
pp. 517-523.
Itoh, K, Udagawa, N, Katagiri, T, Iemura, S, Ueno, N, Yasuda, H, Higashio, K, Quinn,
JM, Gillespie, MT, Martin, TJ, Suda, T & Takahashi, N 2001, 'Bone
morphogenetic protein 2 stimulates osteoclast differentiation and survival
supported by receptor activator of nuclear factor-kappaB ligand', Endocrinology,
vol. 142, no. 8, pp. 3656-62.

Chapter Nine - Bibliography
200
Jacobsen, B & Ploug, M 2008, 'The Urokinase Receptor and its Structural Homologue
C4.4A in Human Cancer: Expression, Prognosis and Pharmacological
Inhibition', Current medicinal chemistry, vol. 15, no. 25, pp. 2559-2573.
Jacquin, C, Gran, DE, Lee, SK, Lorenzo, JA & Aguila, HL 2006, 'Identification of
multiple osteoclast precursor populations in murine bone marrow', J Bone Miner
Res, vol. 21, no. 1, pp. 67-77.
Janssens, K, ten Dijke, P, Janssens, S & Van Hul, W 2005, 'Transforming Growth
Factor-β1 to the Bone', Endocrine reviews, vol. 26, no. 6, pp. 743-774.
Jin, W, Cheng, M, Paul, EM, Babu, G, Lee, AJ, Reiley, W, Wright, A, Zhang, M, You,
J & Sun, SC 2008, 'Deubiquitinating enzyme CYLD negatively regulates RANK
signaling and osteoclastogenesis in mice.(Research article)', The Journal of
clinical investigation, vol. 118, no. 5, p. 1858.
Juppner, H, Abou-Samra, AB, Freeman, M, Kong, XF, Schipani, E, Richards, J,
Kolakowski, LF, Jr., Hock, J, Potts, JT, Jr., Kronenberg, HM & et al. 1991, 'A G
protein-linked receptor for parathyroid hormone and parathyroid hormone-
related peptide', Science, vol. 254, no. 5034, pp. 1024-6.
Kajiya, H 2012, 'Calcium signaling in osteoclast differentiation and bone resorption',
Advances in experimental medicine and biology, vol. 740, pp. 917-32.
Kalu, DN 1991, 'The ovariectomized rat model of postmenopausal bone loss', Bone and
Mineral, vol. 15, no. 3, pp. 175-191.
Kaneda, T, Nojima, T, Nakagawa, M, Ogasawara, A, Kaneko, H, Sato, T, Mano, H,
Kumegawa, M & Hakeda, Y 2000, 'Endogenous Production of TGF-β Is
Essential for Osteoclastogenesis Induced by a Combination of Receptor
Activator of NF-κB Ligand and Macrophage-Colony- Stimulating Factor', The
Journal of Immunology, vol. 165, no. 8, pp. 4254-4263.
Kanis, JA 1991, 'Pathophysiology and treatment of Paget's disease of bone', Martin
Dunitz Ltd.
Kar, P, Nelson, C & Parekh, AB 2011, 'Selective Activation of the Transcription Factor
NFAT1 by Calcium Microdomains near Ca2+ Release-activated Ca2+ (CRAC)
Channels', Journal of biological chemistry, vol. 286, no. 17, pp. 14795-14803.
Karin, M, Yamamoto, Y & Wang, QM 2004, 'The IKK NF-[kappa]B system: a treasure
trove for drug development.(Report)', Nature reviews. Drug discovery, vol. 3,
no. 1, p. 17.
Karsenty, G & Wagner, EF 2002, 'Reaching a genetic and molecular understanding of
skeletal development', Dev Cell, vol. 2, no. 4, pp. 389-406.

Chapter Nine - Bibliography
201
Kasper, D, Planells-Cases, R, Fuhrmann, JC, Scheel, O, Zeitz, O, Ruether, K, Schmitt,
A, Poet, M, Steinfeld, R, Schweizer, M, Kornak, U & Jentsch, TJ 2005, 'Loss of
the chloride channel ClC-7 leads to lysosomal storage disease and
neurodegeneration', EMBO J, vol. 24, no. 5, pp. 1079-91.
Kawasaki-Nishi, S, Nishi, T & Forgac, M 2003, 'Proton translocation driven by ATP
hydrolysis in V-ATPases', FEBS Lett, vol. 545, no. 1, pp. 76-85.
Keller, H & Kneissel, M 2005, 'SOST is a target gene for PTH in bone', Bone, vol. 37,
no. 2, pp. 148-58.
Kim, K, Lee, S-H, Ha Kim, J, Choi, Y & Kim, N 2008, 'NFATc1 Induces Osteoclast
Fusion Via Up-Regulation of Atp6v0d2 and the Dendritic Cell-Specific
Transmembrane Protein (DC-STAMP)', Molecular endocrinology, vol. 22, no.
1, pp. 176-185.
Kim, Y, Sato, K, Asagiri, M, Morita, I, Soma, K & Takayanagi, H 2005, 'Contribution
of nuclear factor of activated T cells c1 to the transcriptional control of
immunoreceptor osteoclast-associated receptor but not triggering receptor
expressed by myeloid cells-2 during osteoclastogenesis', Journal of biological
chemistry, vol. 280, no. 38, p. 32905.
King, AV, Welter, BH, Koushik, AB, Gordon, LN & Temesvari, LA 2012, 'A genome-
wide over-expression screen identifies genes involved in phagocytosis in the
human protozoan parasite, Entamoeba histolytica', PLoS ONE, vol. 7, no. 8, p.
e43025.
Kjoller, L & Hall, A 2001, 'Rac mediates cytoskeletal rearrangements and increased cell
motility induced by urokinase-type plasminogen activator receptor binding to
vitronectin', J Cell Biol, vol. 152, no. 6, pp. 1145-57.
Kobayashi, N, Kadono, Y, Naito, A, Matsumoto, K, Yamamoto, T, Tanaka, S & Inoue,
J 2001, 'Segregation of TRAF6-mediated signaling pathways clarifies its role in
osteoclastogenesis', EMBO J, vol. 20, no. 6, pp. 1271-80.
Kodama, H, Yamasaki, A, Nose, M, Niida, S, Ohgame, Y, Abe, M, Kumegawa, M &
Suda, T 1991, 'Congenital osteoclast deficiency in osteopetrotic (op/op) mice is
cured by injections of macrophage colony-stimulating factor', The Journal of
experimental medicine, vol. 173, no. 1, pp. 269-272.
Koga, T, Inui, M, Inoue, K, Kim, S, Suematsu, A, Kobayashi, E, Iwata, T, Ohnishi, H,
Matozaki, T, Kodama, T, Taniguchi, T, Takayanagi, H & Takai, T 2004,
'Costimulatory signals mediated by the ITAM motif cooperate with RANKL for
bone homeostasis', Nature, vol. 428, no. 6984, pp. 758-63.

Chapter Nine - Bibliography
202
Koga, T, Matsui, Y, Asagiri, M, Kodama, T, de Crombrugghe, B, Nakashima, K &
Takayanagi, H 2005, 'NFAT and Osterix cooperatively regulate bone formation',
Nat Med, vol. 11, no. 8, pp. 880-5.
Kollet, O, Dar, A, Shivtiel, S, Kalinkovich, A, Lapid, K, Sztainberg, Y, Tesio, M,
Samstein, RM, Goichberg, P, Spiegel, A, Elson, A & Lapidot, T 2006,
'Osteoclasts degrade endosteal components and promote mobilization of
hematopoietic progenitor cells', Nat Med, vol. 12, no. 6, pp. 657-64.
Komori, T, Yagi, H, Nomura, S, Yamaguchi, A, Sasaki, K, Deguchi, K, Shimizu, Y,
Bronson, RT, Gao, YH, Inada, M, Sato, M, Okamoto, R, Kitamura, Y, Yoshiki,
S & Kishimoto, T 1997, 'Targeted Disruption of Cbfa1 Results in a Complete
Lack of Bone Formation owing to Maturational Arrest of Osteoblasts', Cell, vol.
89, no. 5, pp. 755-764.
Kong, YY, Yoshida, H, Sarosi, I, Tan, HL, Timms, E, Capparelli, C, Morony, S,
Oliveira-dos-Santos, AJ, Van, G, Itie, A, Khoo, W, Wakeham, A, Dunstan, CR,
Lacey, DL, Mak, TW, Boyle, WJ & Penninger, JM 1999, 'OPGL is a key
regulator of osteoclastogenesis, lymphocyte development and lymph-node
organogenesis', Nature, vol. 397, no. 6717, pp. 315-323.
Kornak, U, Kasper, D, Bösl, MR, Kaiser, E, Schweizer, M, Schulz, A, Friedrich, W,
Delling, G & Jentsch, TJ 2001, 'Loss of the ClC-7 Chloride Channel Leads to
Osteopetrosis in Mice and Man', Cell, vol. 104, no. 2, pp. 205-215.
Koseki, T, Gao, Y, Okahashi, N, Murase, Y, Tsujisawa, T, Sato, T, Yamato, K &
Nishihara, T 2002, 'Role of TGF-β family in osteoclastogenesis induced by
RANKL', Cellular Signalling, vol. 14, no. 1, pp. 31-36.
Koshelnick, Y, Ehart, M, Hufnagl, P, Heinrich, PC & Binder, BR 1997, 'Urokinase
receptor is associated with the components of the JAK1/STAT1 signaling
pathway and leads to activation of this pathway upon receptor clustering in the
human kidney epithelial tumor cell line TCL-598', Journal of biological
chemistry, vol. 272, no. 45, pp. 28563-28567.
Kostenuik, PJ, Nguyen, HQ, McCabe, J, Warmington, KS, Kurahara, C, Sun, N, Chen,
C, Li, L, Cattley, RC, Van, G, Scully, S, Elliott, R, Grisanti, M, Morony, S, Tan,
HL, Asuncion, F, Li, X, Minsky, MS, Stolina, M, Dwyer, D, Dougall, WC,
Hawkins, N, Boyle, WJ, Simonet, WS & Sullivan, JK 2009, 'Denosumab, a
Fully Human Monoclonal Antibody to RANKL, Inhibits Bone Resorption and
Increases BMD in Knock-In Mice That Express Chimeric (Murine/Human)
RANKL', Journal of bone and mineral research, vol. 24, no. 2, pp. 182-195.

Chapter Nine - Bibliography
203
Kramer, I, Loots, GG, Studer, A, Keller, H & Kneissel, M 2010, 'Parathyroid hormone
(PTH)–induced bone gain is blunted in SOST overexpressing and deficient
mice', Journal of bone and mineral research, vol. 25, no. 2, pp. 178-189.
Kruger, RP, Aurandt, J & Guan, KL 2005, 'Semaphorins command cells to move', Nat
Rev Mol Cell Biol, vol. 6, no. 10, pp. 789-800.
Kubota, T, Michigami, T & Ozono, K 2009, 'Wnt signaling in bone metabolism', J Bone
Miner Metab, vol. 27, no. 3, pp. 265-71.
Kular, J, Tickner, J, Chim, SM & Xu, J 2012, 'An overview of the regulation of bone
remodelling at the cellular level', Clinical Biochemistry, no. 0.
Lagasse, E & Weissman, IL 1997, 'Enforced expression of Bcl-2 in monocytes rescues
macrophages and partially reverses osteopetrosis in op/op mice', Cell, vol. 89,
no. 7, pp. 1021-31.
Lakkakorpi, PT, Nakamura, I, Nagy, RM, Parsons, JT, Rodan, GA & Duong, LT 1999,
'Stable Association of PYK2 and p130Cas in Osteoclasts and Their Co-
localization in the Sealing Zone', Journal of biological chemistry, vol. 274, no.
8, pp. 4900-4907.
Langston, AL, Campbell, MK, Fraser, WD, Maclennan, G, Selby, P & Ralston, SH
2007, 'Clinical determinants of quality of life in Paget's disease of bone', Calcif
Tissue Int, vol. 80, no. 1, pp. 1-9.
Laurin, N, Brown, JP, Lemainque, A, Duchesne, A, Huot, D, Lacourciere, Y, Drapeau,
G, Verreault, J, Raymond, V & Morissette, J 2001, 'Paget disease of bone:
Mapping of two loci at 5q35-qter and 5q31', American journal of human
genetics, vol. 69, no. 3, pp. 528-543.
Laurin, N, Brown, JP, Morissette, J & Raymond, V 2002, 'Recurrent mutation of the
gene encoding sequestosome 1 (SQSTM1/p62) in Paget disease of bone', Am J
Hum Genet, vol. 70, no. 6, pp. 1582-8.
Lee, SH, Rho, J, Jeong, D, Sul, JY, Kim, T, Kim, N, Kang, JS, Miyamoto, T, Suda, T,
Lee, SK, Pignolo, RJ, Koczon-Jaremko, B, Lorenzo, J & Choi, Y 2006, 'v-
ATPase V0 subunit d2-deficient mice exhibit impaired osteoclast fusion and
increased bone formation', Nat Med, vol. 12, no. 12, pp. 1403-9.
Lee, SK & Lorenzo, JA 1999, 'Parathyroid hormone stimulates TRANCE and inhibits
osteoprotegerin messenger ribonucleic acid expression in murine bone marrow
cultures: correlation with osteoclast-like cell formation', Endocrinology, vol.
140, no. 8, pp. 3552-61.

Chapter Nine - Bibliography
204
Leppert, D, Ford, J, Stabler, G, Grygar, C, Lienert, C, Huber, S, Miller, KM, Hauser, SL
& Kappos, L 1998, 'Matrix metalloproteinase-9 (gelatinase B) is selectively
elevated in CSF during relapses and stable phases of multiple sclerosis', Brain,
vol. 121, no. 12, pp. 2327-2334.
Lerner, UH 2006, 'Bone Remodeling in Post-menopausal Osteoporosis', Journal of
Dental Research, vol. 85, no. 7, pp. 584-595.
Lester, RD, Jo, M, Montel, V, Takimoto, S & Gonias, SL 2007, 'uPAR induces
epithelial-mesenchymal transition in hypoxic breast cancer cells', J Cell Biol,
vol. 178, no. 3, pp. 425-36.
Levitin, F, Weiss, M, Hahn, Y, Stern, O, Papke, RL, Matusik, R, Nandana, SR, Ziv, R,
Pichinuk, E, Salame, S, Bera, T, Vincent, J, Lee, B, Pastan, I & Wreschner, DH
2008, 'PATE Gene Clusters Code for Multiple, Secreted TFP/Ly-6/uPAR
Proteins That Are Expressed in Reproductive and Neuron-rich Tissues and
Possess Neuromodulatory Activity', Journal of biological chemistry, vol. 283,
no. 24, pp. 16928-16939.
Lewiecki, EM 2011, 'Safety of long-term bisphosphonate therapy for the management
of osteoporosis.(Report)', Drugs, vol. 71, no. 6, p. 791.
Lewis, RS 2001, 'Calcium Signalling Mechanism in T Lymphocytes', Annual Revision
of Immunology, vol. 19, pp. 497-521.
Li, X, Zhang, Y, Kang, H, Liu, W, Liu, P, Zhang, J, Harris, SE & Wu, D 2005,
'Sclerostin binds to LRP5/6 and antagonizes canonical Wnt signaling', J Biol
Chem, vol. 280, no. 20, pp. 19883-7.
Li, Z, Kong, K & Qi, W 2006, 'Osteoclast and its roles in calcium metabolism and bone
development and remodeling', Biochemical and Biophysical Research
Communications, vol. 343, no. 2, pp. 345-350.
Lin, GL & Hankenson, KD 2011, 'Integration of BMP, Wnt, and notch signaling
pathways in osteoblast differentiation', J Cell Biochem, vol. 112, no. 12, pp.
3491-501.
Little, RD, Folz, C, Manning, SP, Swain, PM, Zhao, S-C, Eustace, B, Lappe, MM,
Spitzer, L, Zweier, S, Braunschweiger, K, Benchekroun, Y, Hu, X, Adair, R,
Chee, L, FitzGerald, MG, Tulig, C, Caruso, A, Tzellas, N, Bawa, A, Franklin, B,
McGuire, S, Nogues, X, Gong, G, Allen, KM, Anisowicz, A, Morales, AJ,
Lomedico, PT, Recker, SM, Van Eerdewegh, P, Recker, RR, Carulli, JP, Del
Mastro, RG, Dupuis, J, Osborne, M & Johnson, ML 2002, 'A Mutation in the
LDL Receptor–Related Protein 5 Gene Results in the Autosomal Dominant

Chapter Nine - Bibliography
205
High–Bone-Mass Trait', The American Journal of Human Genetics, vol. 70, no.
1, pp. 11-19.
Liu, D, Ghiso, JAA, Estrada, Y & Ossowski, L 2002, 'EGFR is a transducer of the
urokinase receptor initiated signal that is required for in vivo growth of a human
carcinoma', Cancer Cell, vol. 1, no. 5, pp. 445-457.
Liu, W, Toyosawa, S, Furuichi, T, Kanatani, N, Yoshida, C, Liu, Y, Himeno, M, Narai,
S, Yamaguchi, A & Komori, T 2001, 'Overexpression of Cbfa1 in osteoblasts
inhibits osteoblast maturation and causes osteopenia with multiple fractures.
(Article)', The Journal of cell biology, vol. 155, no. 1, p. 157.
Lomaga, MA, Yeh, WC, Sarosi, I, Duncan, GS, Furlonger, C, Ho, A, Morony, S,
Capparelli, C, Van, G, Kaufman, S, van der Heiden, A, Itie, A, Wakeham, A,
Khoo, W, Sasaki, T, Cao, Z, Penninger, JM, Paige, CJ, Lacey, DL, Dunstan,
CR, Boyle, WJ, Goeddel, DV & Mak, TW 1999, 'TRAF6 deficiency results in
osteopetrosis and defective interleukin-1, CD40, and LPS signaling', Genes Dev,
vol. 13, no. 8, pp. 1015-24.
Long, F 2012, 'Building strong bones: molecular regulation of the osteoblast lineage',
Nat Rev Mol Cell Biol, vol. 13, no. 1, pp. 27-38.
Lucas, PA 1989, 'Chemotactic response of osteoblast-like cells to transforming growth
factor beta', Bone, vol. 10, no. 6, pp. 459-63.
Luo, C-W, Lin, H-J & Chen, Y-H 2001, 'A Novel Heat-labile Phospholipid-binding
Protein, SVS VII, in Mouse Seminal Vesicle as a Sperm Motility Enhancer',
Journal of biological chemistry, vol. 276, no. 10, pp. 6913-6921.
Lymperi, S, Ersek, A, Ferraro, F, Dazzi, F & Horwood, NJ 2011, 'Inhibition of
osteoclast function reduces hematopoietic stem cell numbers in vivo', Blood,
vol. 117, no. 5, pp. 1540-9.
MacDonald, BR & Gowen, M 1993, 'The cell biology of bone', Baillieres Clin
Rheumatol, vol. 7, no. 3, pp. 421-43.
Madsen, CD, Ferraris, GM, Andolfo, A, Cunningham, O & Sidenius, N 2007, 'uPAR-
induced cell adhesion and migration: vitronectin provides the key', J Cell Biol,
vol. 177, no. 5, pp. 927-39.
Manolagas, SC & Jilka, RL 1995, 'Bone Marrow, Cytokines, and Bone Remodeling:
Emerging Insights into the Pathophysiology of Osteoporosis', The New England
journal of medicine, vol. 332, no. 5, pp. 305-311.

Chapter Nine - Bibliography
206
Mansour, A, Abou-Ezzi, G, Sitnicka, E, Jacobsen, SE, Wakkach, A & Blin-Wakkach, C
2012, 'Osteoclasts promote the formation of hematopoietic stem cell niches in
the bone marrow', J Exp Med, vol. 209, no. 3, pp. 537-49.
Mansour, SL, Thomas, KR & Capecchi, MR 1988, 'Disruption of the photo-oncogene
int-2 in mouse embryo-derived stem cells: a general strategy for targetting
mutations to non-selectable genes', Nature, vol. 336, pp. 348-352.
Margalit, M, Yogev, L, Yavetz, H, Lehavi, O, Hauser, R, Botchan, A, Barda, S, Levitin,
F, Weiss, M, Pastan, I, Wreschner, DH, Paz, G & Kleiman, SE 2012,
'Involvement of the prostate and testis expression (PATE)-like proteins in
sperm–oocyte interaction', Human Reproduction, vol. 27, no. 5, pp. 1238-1248.
Martin, TJ, Allan, EH, Ho, PWM, Gooi, JH, Quinn, JMW, Gillespie, MT, Krasnoperov,
V & Sims, NA 2010, 'Communication Between EphrinB2 and EphB4 Within the
Osteoblast Lineage', in Osteoimmunology, vol. 658, ed. Y Choi, Springer US,
pp. 51-60.
Masuyama, R, Mizuno, A, Komori, H, Kajiya, H, Uekawa, A, Kitaura, H, Okabe, K,
Ohyama, K & Komori, T 2012, 'Calcium/calmodulin-signaling supports TRPV4
activation in osteoclasts and regulates bone mass', Journal of bone and mineral
research, vol. 27, no. 8, pp. 1708-1721.
Masuyama, R, Vriens, J, Voets, T, Karashima, Y, Owsianik, G, Vennekens, R, Lieben,
L, Torrekens, S, Moermans, K, Bosch, AV, Bouillon, R, Nillius, B & Carmeliet,
G 2008, 'TRPV4-mediated calcium influx regulates terminal differentiation of
osteoclasts', Cell Metabolism, vol. 8, pp. 257-265.
Matsumoto, M, Kogawa, M, Wada, S, Takayanagi, H, Tsujimoto, M, Katayama, S,
Hisatake, K & Nogi, Y 2004, 'Essential role of p38 mitogen-activated protein
kinase in cathepsin K gene expression during osteoclastogenesis through
association of NFATc1 and PU.1', Journal of biological chemistry, vol. 279, no.
44, pp. 45969-45979.
Matsunobu, T, Torigoe, K, Ishikawa, M, de Vega, S, Kulkarni, AB, Iwamoto, Y &
Yamada, Y 2009, 'Critical roles of the TGF-β type I receptor ALK5 in
perichondrial formation and function, cartilage integrity, and osteoblast
differentiation during growth plate development', Developmental biology, vol.
332, no. 2, pp. 325-338.
Matsuo, K 2010, 'Eph and Ephrin Interactions in Bone ', Osteoimmunology, vol. 658,
pp. 95-103.

Chapter Nine - Bibliography
207
Matsuo, K, Galson, DL, Zhao, C, Peng, L, Laplace, C, Wang, KZQ, Bachler, MA,
Amano, H, Aburatani, H, Ishikawa, H & Wagner, EF 2004, 'Nuclear Factor of
Activated T-cells (NFAT) Rescues Osteoclastogenesis in Precursors Lacking c-
Fos', Journal of biological chemistry, vol. 279, no. 25, pp. 26475-26480.
Matsuo, K & Irie, N 2008, 'Osteoclast-osteoblast communication', Arch Biochem
Biophys, vol. 473, no. 2, pp. 201-9.
McKenzie, IF, Gardiner, J, Cherry, M & Snell, GD 1977, 'Lymphocyte antigens: Ly-4,
Ly-6, and Ly-7', Transplant Proc, vol. 9, no. 1, pp. 667-9.
McMahon, C, Will, A, Hu, P, Shah, GN, Sly, WS & Smith, OP 2001, 'Bone marrow
transplantation corrects osteopetrosis in the carbonic anhydrase II deficiency
syndrome', Blood, vol. 97, no. 7, pp. 1947-50.
Melton, LJ, Chrischilles, EA, Cooper, C, Lane, AW & Riggs, BL 1992, 'Perspective.
How many women have osteoporosis?', Journal of bone and mineral research,
vol. 7, no. 9, pp. 1005-10.
Menaa, C, Reddy, SV, Kurihara, N, Maeda, H, Anderson, D, Cundy, T, Cornish, J,
Singer, FR, Bruder, JM & Roodman, GD 2000, 'Enhanced RANK ligand
expression and responsivity of bone marrow cells in Paget's disease of bone', J
Clin Invest, vol. 105, no. 12, pp. 1833-8.
Mills, BG, Yabe, H & Singer, FR 1988, 'Osteoclasts in human osteopetrosis contain
viral-nucleocapsid-like nuclear inclusions', J Bone Miner Res, vol. 3, no. 1, pp.
101-6.
Miyamoto, H, Suzuki, T, Miyauchi, Y, Iwasaki, R, Kobayashi, T, Sato, Y, Miyamoto,
K, Hoshi, H, Hashimoto, K, Yoshida, S, Hao, W, Mori, T, Kanagawa, H,
Katsuyama, E, Fujie, A, Morioka, H, Matsumoto, M, Chiba, K, Takeya, M,
Toyama, Y & Miyamoto, T 2012, 'Osteoclast stimulatory transmembrane
protein and dendritic cell–specific transmembrane protein cooperatively
modulate cell–cell fusion to form osteoclasts and foreign body giant cells',
Journal of bone and mineral research, vol. 27, no. 6, pp. 1289-1297.
Miyamoto, K, Yoshida, S, Kawasumi, M, Hashimoto, K, Kimura, T, Sato, Y,
Kobayashi, T, Miyauchi, Y, Hoshi, H, Iwasaki, R, Miyamoto, H, Hao, W,
Morioka, H, Chiba, K, Kobayashi, T, Yasuda, H, Penninger, JM, Toyama, Y,
Suda, T & Miyamoto, T 2011, 'Osteoclasts are dispensable for hematopoietic
stem cell maintenance and mobilization', J Exp Med, vol. 208, no. 11, pp. 2175-
81.

Chapter Nine - Bibliography
208
Miyauchi, Y, Ninomiya, K, Miyamoto, H, Sakamoto, A, Iwasaki, R, Hoshi, H,
Miyamoto, K, Hao, W, Yoshida, S, Morioka, H, Chiba, K, Kato, S, Tokuhisa, T,
Saitou, M, Toyama, Y, Suda, T & Miyamoto, T 2010, 'The Blimp1-Bcl6 axis is
critical to regulate osteoclast differentiation and bone homeostasis', Journal of
Experimental Medicine, vol. 207, no. 4, pp. 751-762.
Moriwaki, Y, Watanabe, Y, Shinagawa, T, Kai, M, Miyazawa, M, Okuda, T,
Kawashima, K, Yabashi, A, Waguri, S & Misawa, H 2009, 'Primary sensory
neuronal expression of SLURP-1, an endogenous nicotinic acetylcholine
receptor ligand', Neuroscience Research, vol. 64, no. 4, pp. 403-412.
Moriwaki, Y, Yoshikawa, K, Fukuda, H, Fujii, YX, Misawa, H & Kawashima, K 2007,
'Immune system expression of SLURP-1 and SLURP-2, two endogenous
nicotinic acetylcholine receptor ligands', Life Sci, vol. 80, no. 24-25, pp. 2365-8.
Mundlos, S, Otto, F, Mundlos, C, Mulliken, JB, Aylsworth, AS, Albright, S, Lindhout,
D, Cole, WG, Henn, W, Knoll, JH, Owen, MJ, Mertelsmann, R, Zabel, BU &
Olsen, BR 1997, 'Mutations Involving the Transcription Factor CBFA1 Cause
Cleidocranial Dysplasia', Cell, vol. 89, no. 5, pp. 773-779.
Mundlos, S & Olsen, BR 1997, 'Heritable diseases of the skeleton. Part II: Molecular
insights into skeletal development-matrix components and their homeostasis',
The FASEB journal, vol. 11, no. 4, p. 227.
Murphy, MG, Cerchio, K, Stoch, SA, Gottesdiener, K, Wu, M & Recker, R 2005,
'Effect of L-000845704, an alphaVbeta3 integrin antagonist, on markers of bone
turnover and bone mineral density in postmenopausal osteoporotic women', J
Clin Endocrinol Metab, vol. 90, no. 4, pp. 2022-8.
Nakamura, I, Jimi, E, Duong, LT, Sasaki, T, Takahashi, N, Rodan, GA & Suda, T 1998,
'Tyrosine Phosphorylation of p130Cas Is Involved in Actin Organization in
Osteoclasts', Journal of biological chemistry, vol. 273, no. 18, pp. 11144-11149.
Nakamura, I, Lipfert, L, Rodan, GA & Duong, LT 2001, 'Convergence of αvβ3Integrin–
And Macrophage Colony Stimulating Factor–Mediated Signals on
Phospholipase Cγ in Prefusion Osteoclasts', The Journal of cell biology, vol.
152, no. 2, pp. 361-374.
Nakamura, I, Takahashi, N, Jimi, E, Udagawa, N & Suda, T 2012, 'Regulation of
osteoclast function', Mod Rheumatol, vol. 22, no. 2, pp. 167-77.
Nakamura, M, Udagawa, N, Matsuura, S, Mogi, M, Nakamura, H, Horiuchi, H, Saito,
N, Hiraoka, BY, Kobayashi, Y, Takaoka, K, Ozawa, H, Miyazawa, H &
Takahashi, N 2003, 'Osteoprotegerin regulates bone formation through a

Chapter Nine - Bibliography
209
coupling mechanism with bone resorption', Endocrinology, vol. 144, no. 12, pp.
5441-9.
Nakamura, T, Imai, Y, Matsumoto, T, Sato, S, Takeuchi, K, Igarashi, K, Harada, Y,
Azuma, Y, Krust, A, Yamamoto, Y, Nishina, H, Takeda, S, Takayanagi, H,
Metzger, D, Kanno, J, Takaoka, K, Martin, TJ, Chambon, P & Kato, S 2007,
'Estrogen Prevents Bone Loss via Estrogen Receptor α and Induction of Fas
Ligand in Osteoclasts', Cell, vol. 130, no. 5, pp. 811-823.
Nakashima, K, Zhou, X, Kunkel, G, Zhang, ZP, Deng, JM, Behringer, RR & de
Crombrugghe, B 2002, 'The novel zinc finger-containing transcription factor
Osterix is required for osteoblast differentiation and bone formation', Cell, vol.
108, no. 1, pp. 17-29.
Nakashima, T, Hayashi, M, Fukunaga, T, Kurata, K, Oh-Hora, M, Feng, JQ, Bonewald,
LF, Kodama, T, Wutz, A, Wagner, EF, Penninger, JM & Takayanagi, H 2011,
'Evidence for osteocyte regulation of bone homeostasis through RANKL
expression', Nature medicine, vol. 17, no. 10, pp. 1231-1234.
Nakashima, T & Takayanagi, H 2011, 'New regulation mechanisms of osteoclast
differentiation', Annals of the New York Academy of Sciences, vol. 1240, no. 1,
pp. E13-E18.
Narisawa, S, Fröhlander, N & Millán, JL 1997, 'Inactivation of two mouse alkaline
phosphatase genes and establishment of a model of infantile hypophosphatasia',
Developmental Dynamics, vol. 208, no. 3, pp. 432-446.
Neale, SD, Smith, R, Wass, JAH & Athanasou, NA 2000, 'Osteoclast differentiation
from circulating mononuclear precursors in Paget’s disease is hypersensitive to
1,25-dihydroxyvitamin D3 and RANKL', Bone, vol. 27, no. 3, pp. 409-416.
Neer, RM, Arnaud, CD, Zanchetta, JR, Prince, R, Gaich, GA, Reginster, J-Y,
HOdsman, AB, Eriksen, EF, Ish-Shalom, S, Genant, HK, Wang, O & Mitlak,
BH 2001, 'Effect of parathyroid hormone (1-34) in fractures and bone mineral
density in post menopausal women with osteoporosis', N. Engl. J. Med, vol. 344,
pp. 1434-1441.
Negishi-Koga, T, Shinohara, M, Komatsu, N, Bito, H, Kodama, T, Friedel, RH &
Takayanagi, H 2011, 'Suppression of bone formation by osteoclastic expression
of semaphorin 4D', Nature, vol. 17, no. 11.
Ng, PY, Cheng, TS, Zhao, H, Ye, S, Ang, ESM, Khor, EC, Feng, H, Xu, J, Zheng, MH
& Pavlos, N 2013, 'Disruption of the Dynein-Dynactin Complex Unveils Motor

Chapter Nine - Bibliography
210
Specific Function in Osteoclast Formation and Bone resorption', Journal of bone
and mineral research, vol. 1, pp. 119-34.
Nishida, S, Yamaguchi, A, Tanizawa, T, Endo, N, Mashiba, T, Uchiyama, Y, Suda, T,
Yoshiki, S & Takahashi, HE 1994, 'Increased bone formation by intermittent
parathyroid hormone administration is due to the stimulation of proliferation and
differentiation of osteoprogenitor cells in bone marrow', Bone, vol. 15, no. 6, pp.
717-723. [1994/12//].
Nishikawa, K, Nakashima, T, Hayashi, M, Fukunaga, T, Fukunaga, S, Kato, S,
Kodama, T, Takahashi, S, Calame, K & Takayanagi, H 2010, 'Blimp1-mediated
repression of negative regulators is required for osteoclast differentiation',
Proceedings of the National Academy of Sciences of the United States of
America, vol. 107, no. 7, pp. 3117-3122.
Nyman, JS, Lynch, CC, Perrien, DS, Thiolloy, S, O'Quinn, EC, Patil, CA, Bi, X, Pharr,
GM, Mahadevan-Jansen, A & Mundy, GR 2011, 'Differential effects between
the loss of MMP-2 and MMP-9 on structural and tissue-level properties of bone',
Journal of bone and mineral research, vol. 26, no. 6, pp. 1252-1260.
Ohkura, N, Inoue, S, Ikeda, K & Hayashi, K 1994, 'The two subunits of a phospholipase
A2 inhibitor from the plasma of Thailand cobra having structural similarity to
urokinase-type plasminogen activator receptor and LY-6 related proteins',
Biochemical and Biophysical Research Communications, vol. 204, no. 3, pp.
1212-8.
Oikawa, T & Yamada, T 2003, 'Molecular biology of the Ets family of transcription
factors', Gene, vol. 303, no. 0, pp. 11-34.
Okada, M, Nada, S, Yamanashi, Y, Yamamoto, T & Nakagawa, H 1991, 'CSK: a
protein-tyrosine kinase involved in regulation of src family kinases', Journal of
biological chemistry, vol. 266, no. 36, pp. 24249-52.
Olsen, BR, Reginato, AM & Wang, W 2000, 'Bone development', Annual Review of
Cell developmental biology, vol. 16, pp. 191-220.
Ominsky, M, Ominsky, F, Vlasseros, J, Jolette, S, Smith, B, Stouch, G, Doellgast, J,
Gong, Y, Gao, J, Cao, K, Graham, B, Tipton, J, Cai, R, Deshpande, L, Zhou, M,
Hale, D, Lightwood, A, Henry, A, Popplewell, A, Moore, M, Robinson, D,
Lacey, WS & Simonet, C 2010, 'Two doses of sclerostin antibody in
cynomolgus monkeys increases bone formation, bone mineral density, and bone
strength', Journal of bone and mineral research, vol. 25, no. 5, pp. 948-959.

Chapter Nine - Bibliography
211
Oreffo, RO, Mundy, GR, Seyedin, SM & Bonewald, LF 1989, 'Activation of the bone-
derived latent TGF beta complex by isolated osteoclasts', Biochem Biophys Res
Commun, vol. 158, no. 3, pp. 817-23.
Otto, F, Thornell, AP, Crompton, T, Denzel, A, Gilmour, KC, Rosewell, IR, Stamp,
GWH, Beddington, RSP, Mundlos, S, Olsen, BR, Selby, PB & Owen, MJ 1997,
'Cbfa1, a Candidate Gene for Cleidocranial Dysplasia Syndrome, Is Essential for
Osteoblast Differentiation and Bone Development', Cell, vol. 89, no. 5, pp. 765-
771.
Oursler, MJ 1994, 'Osteoclast synthesis and secretion and activation of latent
transforming growth factor beta', J Bone Miner Res, vol. 9, no. 4, pp. 443-52.
Parker, M, von Maltzahn, J, Bakkar, N, Al-Joubori, B, Ishibashi, J, Guttridge, D &
Rudnicki, M 2012, 'MyoD-dependent regulation of NF-kappaB activity couples
cell-cycle withdrawal to myogenic differentiation', Skeletal Muscle, vol. 2, no. 1,
p. 6.
Pavlos, NJ, Cheng, TS, Qin, A, Ng, PY, Feng, HT, Ang, ESM, Carrello, A, Sung, CH,
Jahn, R, Zheng, MH & Xu, JK 2011, 'Tctex-1, a Novel Interaction Partner of
Rab3D, Is Required for Osteoclastic Bone Resorption', Molecular and cellular
biology, vol. 31, no. 7, pp. 1551-1564.
Pelton, RW, Saxena, B, Jones, M, Moses, HL & Gold, LI 1991, 'Immunohistochemical
localization of TGF beta 1, TGF beta 2, and TGF beta 3 in the mouse embryo:
expression patterns suggest multiple roles during embryonic development', The
Journal of cell biology, vol. 115, no. 4, pp. 1091-1105.
Pfeilschifter, J & Mundy, GR 1987, 'Modulation of type beta transforming growth
factor activity in bone cultures by osteotropic hormones', Proc Natl Acad Sci U
S A, vol. 84, no. 7, pp. 2024-8.
Phan, T 2004, 'Functional characterization of an osteoclast-derived osteoblastic factor
(ODOF)', Unpublished PhD Thesis, The University of Western Australia, Perth.
Pittenger, MF, Mackay, AM, Beck, SC, Jaiswal, RK, Douglas, R, Mosca, JD,
Moorman, MA, Simonetti, DW, Craig, S & Marshak, DR 1999, 'Multilineage
potential of adult human mesenchymal stem cells', Science, vol. 284, no. 5411,
pp. 143-7.
Ploug, M, Ronne, E, Behrendt, N, Jensen, AL, Blasi, F & Dano, K 1991, 'Cellular
receptor for urokinase plasminogen activator. Carboxyl-terminal processing and
membrane anchoring by glycosyl-phosphatidylinositol', J Biol Chem, vol. 266,
no. 3, pp. 1926-33.

Chapter Nine - Bibliography
212
Qin, A, Cheng, TS, Lin, Z, Pavlos, NJ, Jiang, Q, Xu, J, Dai, KR & Zheng, MH 2011,
'Versatile roles of V-ATPases accessory subunit Ac45 in osteoclast formation
and function', PLoS ONE, vol. 6, no. 11, p. e27155.
Qiu, T, Xiangwei, Zhang, F, Clemens, TL, Wan, M & Cao, X 2010, 'TGF-[beta] type II
receptor phosphorylates PTH receptor to integrate bone remodelling
signalling.(Transforming growth factors)(Parathyroid hormones)(Report)',
Nature Cell Biology, vol. 12, no. 3, p. 224.
Quarello, P, Forni, M, Barberis, L, Defilippi, C, Campagnoli, MF, Silvestro, L, Frattini,
A, Chalhoub, N, Vacher, J & Ramenghi, U 2004, 'Severe malignant
osteopetrosis caused by a GL gene mutation', J Bone Miner Res, vol. 19, no. 7,
pp. 1194-9.
Rachner, TD, Khosla, S & Hofbauer, LC 2011, 'Osteoporosis: now and the future',
Lancet, vol. 377, no. 9773, pp. 1276-87.
Raisz, LG 1999, 'Physiology and pathophysiology of bone remodeling', Clin Chem, vol.
45, no. 8 Pt 2, pp. 1353-8.
Raisz, LG 2005a, 'Clinical practice. Screening for osteoporosis', N Engl J Med, vol.
353, no. 2, pp. 164-71.
Raisz, LG 2005b, 'Pathogenesis of osteoporosis: concepts, conflicts, and prospects', J
Clin Invest, vol. 115, no. 12, pp. 3318-25.
Ralston, SH & Layfield, R 2012, 'Pathogenesis of Paget disease of bone', Calcif Tissue
Int, vol. 91, no. 2, pp. 97-113.
Ram, M, Sherer, Y & Shoenfeld, Y 2006, 'Matrix metalloproteinase-9 and autoimmune
diseases', J Clin Immunol, vol. 26, no. 4, pp. 299-307.
Ray, NF, Chan, JK, Thamer, M & Melton, LJ 1997, 'Medical Expenditures for the
Treatment of Osteoporotic Fractures in the United States in 1995: Report from
the National Osteoporosis Foundation', Journal of bone and mineral research,
vol. 12, no. 1, pp. 24-35.
Rebel, A, Basle, M, Pouplard, A, Malkani, K, Filmon, R & Lepatezour, A 1981,
'Towards a viral etiology for Paget's disease of bone', Metab Bone Dis Relat Res,
vol. 3, no. 4-5, pp. 235-8.
Reid, IR, MIller, P, Lyles, K, Fraser, W, Brown, JP, Saidi, Y, Mesenbrink, P, Su, G,
Pak, J, Zelenakas, K, Luchi, M, Richardson, P & Hosking, D 2005, 'Comparison
of a single infusion of zoledronic acid with risendronate for Paget's disease',
New England Journal of Medicine, vol. 353, pp. 898-908.

Chapter Nine - Bibliography
213
Riggs, BL & Melton, LJ, 3rd 1983, 'Evidence for two distinct syndromes of involutional
osteoporosis', Am J Med, vol. 75, no. 6, pp. 899-901.
Rizzoli, R, Yasothan, U & Kirkpatrick, P 2010, 'Denosumab', Nat Rev Drug Discov,
vol. 9, no. 8, pp. 591-2.
Robling, AG, Bellido, T & Turner, CH 2006, 'Mechanical stimulation in vivo reduces
osteocyte expression of sclerostin', J Musculoskelet Neuronal Interact, vol. 6,
no. 4, p. 354.
Roodman, GD & Windle, JJ 2005, 'Paget disease of bone', J Clin Invest, vol. 115, no. 2,
pp. 200-8.
Rosen, CJ 2005, 'Clinical practice. Postmenopausal osteoporosis', N Engl J Med, vol.
353, no. 6, pp. 595-603.
Rosen, ED, Hsu, C-H, Wang, X, Sakai, S, Freeman, MW, Gonzalez, FJ & Spiegelman,
BM 2002, 'C/EBPα induces adipogenesis through PPARγ: a unified pathway',
Genes & development, vol. 16, no. 1, pp. 22-26.
Ross, FP & Teitelbaum, SL 2005, 'αvβ3 and macrophage colony-stimulating factor:
partners in osteoclast biology', Immunological Reviews, vol. 208, no. 1, pp. 88-
105.
Rufo, GA, Jr., Singh, JP, Babcock, DF & Lardy, HA 1982, 'Purification and
characterization of a calcium transport inhibitor protein from bovine seminal
plasma', J Biol Chem, vol. 257, no. 8, pp. 4627-32.
Ryu, J, Kim, HJ, Chang, EJ, Huang, H, Banno, Y & Kim, HH 2006, 'Sphingosine 1-
phosphate as a regulator of osteoclast differentiation and osteoclast-osteoblast
coupling', EMBO journal, vol. 25, no. 24, pp. 5840-5851.
Saftig, P, Hunziker, E, Everts, V & al, e 2000, 'Functions of cathepsin K in bone
resorption. Lessons from cathepsin K deficient mice', Adv Exp Med Biol, vol.
477, pp. 293-03.
Sato, K, Suematsu, A, Nakashima, T, Takemoto-Kimura, S, Aoki, K, Morishita, Y,
Asahara, H, Ohya, K, Yamaguchi, A, Takai, T, Kodama, T, Chatila, TA, Bito, H
& Takayanagi, H 2006, 'Regulation of osteoclast differentiation and function by
the CaMK-CREB pathway', Nat Med, vol. 12, no. 12, pp. 1410-6.
Saville, PD 1969, 'Changes in skeletal mass and fragility with castration in the rat; a
model of osteoporosis', J Am Geriatr Soc, vol. 17, pp. 155-166.
Schaffner, P & Dard, MM 2003, 'Structure and function of RGD peptides involved in
bone biology', Cell Mol Life Sci, vol. 60, no. 1, pp. 119-32.

Chapter Nine - Bibliography
214
Schneeweis, LA, Willard, D & Milla, ME 2005, 'Functional dissection of
osteoprotegerin and its interaction with receptor activator of NF-kappaB ligand',
J Biol Chem, vol. 280, no. 50, pp. 41155-64.
Schiller, HB, Szekeres, A, Binder, BR, Stockinger, H & Leksa, V 2009, 'Mannose 6-
phosphate/insuline-like growth factor 2 receptor limits cell invasion by
controlling alpha v beta 3 integrin expression and proteolytic processing of
uPAR', Molecular Biology of Cell, vol. 20, pp. 745-756.
Selby, P 2005, 'Paget's disease', Medicine, vol. 33, no. 12, pp. 66-67.
Sims, NA & Gooi, JH 2008, 'Bone remodeling: Multiple cellular interactions required
for coupling of bone formation and resorption', Seminars in Cell &
Developmental Biology, vol. 19, no. 5, pp. 444-451.
Sims, NA & Gooi, JH 2008, 'Bone remodeling: Multiple cellular interactions required
for coupling of bone formation and resorption', Semin Cell Dev Biol, vol. 19, no.
5, pp. 444-51.
Singh, P, van der Kraan, J, Xu, MT, Xu, M & Quinn 2012, 'Membrane-bound receptor
activator of NF-κB ligand (RANKL) activity displayed by osteoblasts is
differentially regulated by osteolytic factors', Biochemical and Biophysical
Research Communications, vol. 422, no. 1, pp. 48-53.
Sly, W, Hewett-emmett, D, Whyte, MP, Yu, Y-SL & Tashian, RE 1983, 'Carbonic
Anhydrase II Deficiency Identified as the Primary Defect in the Autosomal
Recessive Syndrome of Osteopetrosis with Renal Tubular Acidosis and Cerebral
Calcification', Proceedings of the National Academy of Sciences of the United
States of America, vol. 80, no. 9, pp. 2752-2756.
Smith, HW, Marra, P & Marshall, CJ 2008, 'uPAR promotes formation of the p130Cas-
Crk complex to activate Rac through DOCK180', Journal of Cell Biology, vol.
182, no. 4, pp. 777-790.
Smith, HW & Marshall, CJ 2010, 'Regulation of cell signalling by uPAR', Nat Rev Mol
Cell Biol, vol. 11, no. 1, pp. 23-36.
Sobacchi, C, Frattini, A, Guerrini, MM, Abinun, M, Pangrazio, A, Susani, L, Bredius,
R, Mancini, G, Cant, A, Bishop, N, Grabowski, P, Del Fattore, A, Messina, C,
Errigo, G, Coxon, FP, Scott, DI, Teti, A, Rogers, MJ, Vezzoni, P, Villa, A &
Helfrich, MH 2007, 'Osteoclast-poor human osteopetrosis due to mutations in
the gene encoding RANKL', Nature Genetics, vol. 39, no. 8, pp. 960-962.
Soegiarto, DW, Kiachopoulos, S, Schipani, E, Jüppner, H, Erben, RG & Lanske, B
2001, 'Partial Rescue of PTH/PTHrP Receptor Knockout Mice by Targeted

Chapter Nine - Bibliography
215
Expression of the Jansen Transgene', Endocrinology, vol. 142, no. 12, pp. 5303-
5310.
Soriano, P, Soriano, C, Montgomery, R & Geske, A 1991, 'Targeted disruption of the c-
src proto-oncogene leads to osteopetrosis in mice', Cell, vol. 64, no. 4, pp. 693-
702.
Southan, C, Cutler, P, Birrell, H, Connell, J, Fantom, KGM, Sims, M, Shaikh, N &
Schneider, K 2002, 'The characterisation of novel secreted Ly-6 proteins from
rat urine by the combined use of two-dimensional gel electrophoresis, microbore
high performance liquid chromatography and expressed sequence tag data',
Proteomics, vol. 2, no. 2, pp. 187-196.
Stanley, ER, Stanley, K, Berg, D, Lee, FJ, Lee, F, Pixley, Y & Wang, Y-G 1997,
'Biology and action of colony-stimulating factor-1', Molecular reproduction and
development, vol. 46, no. 1, pp. 4-10.
Stoch, SA, Zajic, J, Stone, DL, Miller, K, Van Dyck, MJ, Gutierrez, M, De Decker, L,
Liu, Q, Liu, BB, Scott, D, Panebianco, B, Jin, LT, Duong, K & Gottesdiener, JA
2009, 'Effect of the Cathepsin K Inhibitor Odanacatib on Bone Resorption
Biomarkers in Healthy Postmenopausal Women: Two Double-Blind,
Randomized, Placebo-Controlled Phase I Studies', Clinical pharmacology &
therapeutics, vol. 86, no. 2, pp. 175-182.
Suda, T, Jimi, E, Nakamura, I & Takahashi, N 1997, 'Role of 1 alpha, 25-
dihydroxyviD3 D3 in osteoclast differentiation and function', Methods Enzymol,
vol. 282, pp. 223-35.
Suda, T, Takahashi, N & Martin, TJ 1992, 'Modulation of osteoclast differentiation',
Endocrine reviews, vol. 13, pp. 66-80.
Suda, T, Takahashi, N, Udagawa, N, Jimi, E, Gillespie, MT & Martin, TJ 1999,
'Modulation of osteoclast differentiation and function by the new members of
the tumor necrosis factor receptor and ligand families', Endocr Rev, vol. 20, no.
3, pp. 345-57.
Suda, T, Udagawa, N, Nakamura, I, Miyaura, C & Takahashi, N 1995, 'Modulation of
osteoclast differentiation by local factors', Bone, vol. 17, no. 2 Suppl, pp. 87S-
91S.
Sugatani, T 2005, 'Akt1/Akt2 and mammalian target of rapamycin/Bim play critical
roles in osteoclast differentiation and survival, respectively, whereas Akt is
dispensable for cell survival in isolated osteoclast precursors', Journal of
biological chemistry, vol. 280, no. 5, pp. 3583-9.

Chapter Nine - Bibliography
216
Sugatani, T & Hruska, KA 2005, 'Akt1/Akt2 and mammalian target of rapamycin/bim
play critical roles in osteoclast differentiation and survival, respectively, whereas
Akt is dispensable for cell survival in isolated osteoclast precursors', Journal of
biological chemistry, vol. 280, no. 5, pp. 3583-3589.
Tachi, K, Takami, M, Sato, H, Mochizuki, A, Zhao, BH, Miyamoto, Y, Tsukasaki, H,
Inoue, T, Shintani, S, Koike, T, Honda, Y, Suzuki, O, Baba, K & Kamijo, R
2011, 'Enhancement of Bone Morphogenetic Protein-2-Induced Ectopic Bone
Formation by Transforming Growth Factor-beta 1', Tissue Engineering Part A,
vol. 17, no. 5-6, pp. 597-606.
Takahashi, N, Udagawa, N & Suda, T 1999, 'A New Member of Tumor Necrosis Factor
Ligand Family, ODF/OPGL/TRANCE/RANKL, Regulates Osteoclast
Differentiation and Function', Biochemical and Biophysical Research
Communications, vol. 256, no. 3, pp. 449-455.
Takai, H, Kanematsu, M, Yano, K, Tsuda, E, Higashio, K, Ikeda, K, Watanabe, K &
Yamada, Y 1998, 'Transforming Growth Factor-β Stimulates the Production of
Osteoprotegerin/Osteoclastogenesis Inhibitory Factor by Bone Marrow Stromal
Cells', Journal of biological chemistry, vol. 273, no. 42, pp. 27091-27096.
Takayanagi, H 2007, 'Osteoimmunology: shared mechanisms and crosstalk between the
immune and bone systems', Nature Reviews Immunology, vol. 7, no. 4, pp. 292-
304.
Takayanagi, H, Kim, S, Koga, T, Nishina, H, Isshiki, M, Yoshida, H, Saiura, A, Isobe,
M, Yokochi, T, Inoue, J, Wagner, EF, Mak, TW, Kodama, T & Taniguchi, T
2002, 'Induction and activation of the transcription factor NFATc1 (NFAT2)
integrate RANKL signaling in terminal differentiation of osteoclasts', Dev Cell,
vol. 3, no. 6, pp. 889-901.
Takeda, S, Bonnamy, JP, Owen, MJ, Ducy, P & Karsenty, G 2001, 'Continuous
expression of Cbfa1 in nonhypertrophic chondrocytes uncovers its ability to
induce hypertrophic chondrocyte differentiation and partially rescues Cbfa1-
deficient mice', Genes Dev, vol. 15, no. 4, pp. 467-81.
Takeshita, S, Fumoto, T, Matsuoka, K, Park, K-a, Aburatani, H, Kato, S, Ito, M &
Ikeda, K 2013, 'Osteoclast-secreted CTHRC1 in the coupling of bone resorption
to formation', The Journal of clinical investigation, vol. 123, no. 9, pp. 0-0.
Tanabe, N, Wheal, BD, Kwon, J, Chen, HH, Shugg, RPP, Sims, SM, Goldberg, HA &
Dixon, SJ 2011, 'Osteopontin Signals through Calcium and Nuclear Factor of
Activated T Cells (NFAT) in Osteoclasts A NOVEL RGD-DEPENDENT

Chapter Nine - Bibliography
217
PATHWAY PROMOTING CELL SURVIVAL', Journal of biological
chemistry, vol. 286, no. 46, pp. 39871-39881.
Tanaka, S, Nakamura, I, Inoue, J, Oda, H & Nakamura, K 2003, 'Signal transduction
pathways regulating osteoclast differentiation and function', J Bone Miner
Metab, vol. 21, no. 3, pp. 123-33.
Tanaka, S, Takahashi, N, Udagawa, N, Sasaki, T, Fukui, Y, Kurokawa, T & Suda, T
1992, 'Osteoclasts express high levels of p60c-src, preferentially on ruffled
border membranes', FEBS letters, vol. 313, no. 1, pp. 85-89.
Tang, Y, Wu, X, Lei, W, Pang, L, Wan, C, Shi, Z, Zhao, L, Nagy, TR, Peng, X, Hu, J,
Feng, X, Van Hul, W, Wan, M & Cao, X 2009, 'TGF-beta 1-˜“induced
migration of bone mesenchymal stem cells couples bone resorption with
formation', Nature medicine, vol. 15, no. 7, pp. 757-765.
Teitelbaum, SL 2000, 'Bone resorption by osteoclasts', Science, vol. 289, no. 5484, pp.
1504-8.
Termine, JD, Robey, PG, Fisher, LW, Shimokawa, H, Drum, MA, Conn, KM,
Hawkins, GR, Cruz, JB & Thompson, KG 1984, 'Osteonectin, bone
proteoglycan, and phosphophoryn defects in a form of bovine osteogenesis
imperfecta', Proceedings of the National Academy of Sciences, vol. 81, no. 7, pp.
2213-2217.
Teti, A 2012, 'Osteoclasts and hematopoesis', BoneKEy Reports, vol. 1, no. 46.
Theill, LE, Boyle, WJ & Penninger, JM 2002, 'RANK-L and RANK: T cells, bone loss,
and mammalian evolution', Annual Review of Immunology, vol. 20, pp. 795-823.
Theoleyre, S, Kwan Tat, S, Vusio, P, Blanchard, F, Gallagher, J, Ricard-Blum, S,
Fortun, Y, Padrines, M, Redini, F & Heymann, D 2006, 'Characterization of
osteoprotegerin binding to glycosaminoglycans by surface plasmon resonance:
role in the interactions with receptor activator of nuclear factor kappaB ligand
(RANKL) and RANK', Biochem Biophys Res Commun, vol. 347, no. 2, pp. 460-
7.
Tominaga, H, Tominaga, S, Maeda, M, Hayashi, S, Takeda, S, Akira, S, Komiya, T,
Nakamura, H & Akiyama, T 2008, 'CCAAT/Enhancer-binding Protein
 Promotes Osteoblast Differentiation by Enhancing Runx2 Activity with
ATF4', Molecular biology of the cell, vol. 19, no. 12, pp. 5373-5386.
Tondravi, MM, McKercher, SR, Anderson, K, Erdmann, JM, Quiroz, M, Maki, R &
Teitelbaum, SL 1997, 'Osteopetrosis in mice lacking haematopoietic
transcription factor PU.1', Nature, vol. 386, no. 6620, pp. 81-4.

Chapter Nine - Bibliography
218
Trevisan, M & Iscove, NN 1995, 'Phenotypic analysis of murine long-term hemopoietic
reconstituting cells quantitated competitively in vivo and comparison with more
advanced colony-forming progeny', J Exp Med, vol. 181, no. 1, pp. 93-103.
Tsuji, H, Okamoto, K, Matsuzaka, Y, Iizuka, H, Tamiya, G & Inoko, H 2003, 'SLURP-
2, a novel member of the human Ly-6 superfamily that is up-regulated in
psoriasis vulgaris', Genomics, vol. 81, no. 1, pp. 26-33.
Turunen, HT, Sipila, P, Pujianto, DA, Damdimopoulos, AE, Bjorkgren, I, Huhtaniemi, I
& Poutanen, M 2011, 'Members of the murine Pate family are predominantly
expressed in the epididymis in a segment-specific fashion and regulated by
androgens and other testicular factors', Reprod Biol Endocrinol, vol. 9, no. 1, p.
128.
Udagawa, N, Takahashi, N, Akatsu, T, Tanaka, H, Sasaki, T, Nishihara, T, Koga, T,
Martin, TJ & Suda, T 1990, 'Origin of Osteoclasts - Mature Monocytes and
Macrophages Are Capable of Differentiating into Osteoclasts under a Suitable
Microenvironment Prepared by Bone Marrow-Derived Stromal Cells',
Proceedings of the National Academy of Sciences of the United States of
America, vol. 87, no. 18, pp. 7260-7264.
Ueta, C, Iwamoto, M, Kanatani, N, Yoshida, C, Liu, Y, Enomoto-Iwamoto, M, Ohmori,
T, Enomoto, H, Nakata, K, Takada, K, Kurisu, K & Komori, T 2001, 'Skeletal
malformations caused by overexpression of Cbfa1 or its dominant negative form
in chondrocytes', J Cell Biol, vol. 153, no. 1, pp. 87-100.
Ushizawa, K, Takahashi, T, Hosoe, M, Kizaki, K, Hashizume, KH & Immo, A 2009,
'Characterization and Expression Analysis of SOLD1, a Novel Member of the
Retrotransposon-Derived Ly-6 Superfamily, in Bovine Placental Villi (SOLD1
in Bovine Placenta)', PLoS ONE, vol. 4, no. 6, p. e5814.
Uthgenannt, BA, Kramer, MH, Hwu, JA, Wopenka, B & Silva, MJ 2007, 'Skeletal self-
repair: stress fracture healing by rapid formation and densification of woven
bone', J Bone Miner Res, vol. 22, no. 10, pp. 1548-56.
Vaananen, HK, Zhao, H, Mulari, M & Halleen, JM 2000, 'The cell biology of osteoclast
function', J Cell Sci, vol. 113 ( Pt 3), no. 3, pp. 377-81.
Van Wesenbeeck, L, Cleiren, E, Gram, J, Beals, RK, Bénichou, O, Scopelliti, D, Key,
L, Renton, T, Bartels, C, Gong, Y, Warman, ML, de Vernejoul, M-C,
Bollerslev, J & Van Hul, W 2003, 'Six Novel Missense Mutations in the LDL
Receptor-Related Protein 5 (LRP5) Gene in Different Conditions with an

Chapter Nine - Bibliography
219
Increased Bone Density', The American Journal of Human Genetics, vol. 72, no.
3, pp. 763-771.
Vial, E, Sahai, E & Marshall, CJ 2003, 'ERK-MAPK signaling coordinately regulates
activity of Rac1 and RhoA for tumor cell motility', Cancer Cell, vol. 4, no. 1,
pp. 67-79.
Villa, A, Guerrini, MM, Cassani, B, Pangrazio, A & Sobacchi, C 2009, 'Infantile
malignant, autosomal recessive osteopetrosis: the rich and the poor', Calcif
Tissue Int, vol. 84, no. 1, pp. 1-12.
Wagner, EF & Eferl, R 2005, 'Fos/AP-1 proteins in bone and the immune system',
Immunol Rev, vol. 208, no. 1, pp. 126-40.
Walker, EC, McGregor, NE, Poulton, IJ, Pompolo, S, Allan, EH, Quinn, JMW,
Gillespie, MT, Martin, TJ & Sims, NA 2008, 'Cardiotrophin-1 Is an Osteoclast-
Derived Stimulus of Bone Formation Required for Normal Bone Remodeling',
Journal of bone and mineral research, vol. 23, no. 12, pp. 2025-2032.
Wallach, S, Rousseau, G, Martin, L & Azria, M 1999, 'Effects of calcitonin on animal
and in vitro models of skeletal metabolism', Bone, vol. 25, no. 5, pp. 509-516.
Wei, C, Moller, CC, Altintas, MM, Li, J, Schwarz, K, Zacchigna, S, Xie, L, Henger, A,
Schmid, H, Rastaldi, MP, Cowan, P, Kretzler, M, Parrilla, R, Bendayan, M,
Gupta, V, Nikolic, B, Kalluri, R, Carmeliet, P, Mundel, P & Reiser, J 2008,
'Modification of kidney barrier function by the urokinase receptor', Nature
medicine, vol. 14, no. 1, p. 55.
Whyte, MP 1993, 'Carbonic anhydrase II deficiency', Clin Orthop Relat Res, vol. 294,
no. 294, pp. 52-63.
Wilson, SR, Peters, C, Saftig, P & Bromme, D 2009, 'Cathepsin K activity-dependent
regulation of osteoclast actin ring formation and bone resorption', J Biol Chem,
vol. 284, no. 4, pp. 2584-92.
Wong, B, Wong, D, Besser, N, Kim, J, Arron, M, Vologodskaia, H & Hanafusa, Y
1999, 'TRANCE, a TNF Family Member, Activates Akt/PKB through a
Signaling Complex Involving TRAF6 and c-Src', Molecular cell, vol. 4, no. 6,
pp. 1041-1049.
Woods, D, Cherwinski, H, Venetsanakos, E, Bhat, A, Gysin, S, Humbert, M, Bray, PF,
Saylor, VL & McMahon, M 2001, 'Induction of β3-Integrin Gene Expression by
Sustained Activation of the Ras-Regulated Raf–MEK–Extracellular Signal-
Regulated Kinase Signaling Pathway', Molecular and cellular biology, vol. 21,
no. 9, pp. 3192-3205.

Chapter Nine - Bibliography
220
Wu, X, Tu, X, Joeng, KS, Hilton, MJ, Williams, DA & Long, F 2008, 'Rac1 Activation
Controls Nuclear Localization of β-catenin during Canonical Wnt Signaling',
Cell, vol. 133, no. 2, pp. 340-353.
Xiong, J, Onal, M, Jilka, RL, Weinstein, RS, Manolagas, SC & O'Brien, CA 2011,
'Matrix-embedded cells control osteoclast formation', Nat Med, vol. 17, no. 10,
pp. 1235-41.
Xu, J, Tan, L, Huang, X-H, Gao, R, Laird, D, Liu, S & Wysocki, M 2000, 'Cloning,
Sequencing, and Functional Characterization of the Rat Homologue of Receptor
Activator of NF-κB Ligand', Journal of bone and mineral research, vol. 15, no.
11, pp. 2178-2186.
Xu, J, Wu, HF, Ang, ESM, Yip, K, Woloszyn, M, Zheng, MH & Tan, RX 2009, 'NF-κB
modulators in osteolytic bone diseases', Cytokine & Growth Factor
Reviews, vol. 20, no. 1, pp. 7-17.
Yagi, M, Miyamoto, T, Sawatani, Y, Iwamoto, K, Hosogane, N, Fujita, N, Morita, K,
Ninomiya, K, Suzuki, T, Miyamoto, K, Oike, Y, Takeya, M, Toyama, Y &
Suda, T 2005, 'DC-STAMP is essential for cell-cell fusion in osteoclasts and
foreign body giant cells', Journal of Experimental Medicine, vol. 202, no. 3, pp.
345-351.
Yamamoto, M, Fisher, JE, Gentile, M, Seedor, JG, Leu, CT, Rodan, SB & Rodan, GA
1998, 'The integrin ligand echistatin prevents bone loss in ovariectomized mice
and rats', Endocrinology, vol. 139, no. 3, pp. 1411-9.
Yang, X, Matsuda, K, Bialek, P, Jacquot, S, Masuoka, HC, Schinke, T, Li, L,
Brancorsini, S, Sassone-Corsi, P, Townes, TM, Hanauer, A & Karsenty, G 2004,
'ATF4 Is a Substrate of RSK2 and an Essential Regulator of Osteoblast Biology:
Implication for Coffin-Lowry Syndrome', Cell, vol. 117, no. 3, pp. 387-398.
Yarilina, A, Xu, K, Chen, J & Ivashkiv, LB 2011, 'TNF activates calcium-nuclear factor
of activated T cells (NFAT)c1 signaling pathways in human macrophages',
Proceedings of the National Academy of Sciences of the United States of
America, vol. 108, no. 4, p. 1573.
Yasuda, H, Shima, N, Nakagawa, N, Yamaguchi, K, Kinosaki, M, Mochizuki, S,
Tomoyasu, A, Yano, K, Goto, M, Murakami, A, Tsuda, E, Morinaga, T,
Higashio, K, Udagawa, N, Takahashi, N & Suda, T 1998, 'Osteoclast
differentiation factor is a ligand for osteoprotegerin osteoclastogenesis-
inhibitory factor and is identical to TRANCE/RANKL', Proceedings of the

Chapter Nine - Bibliography
221
National Academy of Sciences of the United States of America, vol. 95, no. 7,
pp. 3597-3602.
Yoshida, C 2012, 'SP7 Inhibits Osteoblast Differentiation at a Late Stage in Mice
(Inhibition of Osteoblast Maturation by SP7)', PLoS ONE, vol. 7, no. 3, p.
e32364.
Yoshida, CA, Komori, H, Maruyama, Z, Miyazaki, T, Kawasaki, K, Furuichi, T,
Fukuyama, R, Mori, M, Yamana, K, Nakamura, K, Liu, W, Toyosawa, S,
Moriishi, T, Kawaguchi, H, Takada, K & Komori, T 2012, 'SP7 Inhibits
Osteoblast Differentiation at a Late Stage in Mice', PLoS ONE, vol. 7, no. 3, p.
e32364.
Yoshida, H, Hayashi, SI, Kunisada, T, Ogawa, M, Nishikawa, S, Okamura, H, Sudo, T,
Shultz, LD & Nishikawa, SI 1990, 'The Murine Mutation Osteopetrosis Is in the
Coding Region of the Macrophage Colony Stimulating Factor Gene', Nature,
vol. 345, no. 6274, pp. 442-444.
Zaidi, M 2007, 'Skeletal remodeling in health and disease', Nat Med, vol. 13, no. 7, pp.
791-801.
Zhang, F, Tom, CC, Kugler, MC, Ching, TT, Kreidberg, JA, Wei, Y & Chapman, HA
2003, 'Distinct ligand binding sites in integrin alpha3beta1 regulate matrix
adhesion and cell-cell contact', J Cell Biol, vol. 163, no. 1, pp. 177-88.
Zhang, M, Xuan, S, Bouxsein, ML, von Stechow, D, Akeno, N, Faugere, MC,
Malluche, H, Zhao, G, Rosen, CJ, Efstratiadis, A & Clemens, TL 2002,
'Osteoblast-specific knockout of the insulin-like growth factor (IGF) receptor
gene reveals an essential role of IGF signaling in bone matrix mineralization', J
Biol Chem, vol. 277, no. 46, pp. 44005-12.
Zhao, C, Irie, N, Takada, Y, Shimoda, K, Miyamoto, T, Nishiwaki, T, Suda, T &
Matsuo, K 2006, 'Bidirectional ephrinB2-EphB4 signaling controls bone
homeostasis', Cell Metabolism, vol. 4, no. 2, pp. 111-121.
Zhao, M, Harris, SE, Horn, D, Geng, Z, Nishimura, R, Mundy, GR & Chen, D 2002,
'Bone morphogenetic protein receptor signaling is necessary for normal murine
postnatal bone formation', The Journal of cell biology, vol. 157, no. 6, pp. 1049-
1060.
Zou, W, Kitaura, H, Reeve, J, Long, F, Tybulewicz, VL, Shattil, SJ, Ginsberg, MH,
Ross, FP & Teitelbaum, SL 2007, 'Syk, c-Src, the alphavbeta3 integrin, and
ITAM immunoreceptors, in concert, regulate osteoclastic bone resorption', J
Cell Biol, vol. 176, no. 6, pp. 877-88.

Chapter Nine - Bibliography
222
Zuo, C, Huang, Y, Bajis, R, Sahih, M, Li, YP, Dai, K & Zhang, X 2012,
'Osteoblastogenesis regulation signals in bone remodeling', Osteoporosis
International, vol. 23, no. 6, pp. 1653-1663.

223
APPENDIX

Appendix
224
Serum Biochemistry WT TG Calcium (mg/dL) 1.61 ± 0.31 1.46 ± 0.14
Phosphate (mg/dL) 2.07 ± 0.12 2.18 ± 0.15
Supplementary Figure 1. Serum biochemistry measurement on calcium and
phosphate levels in Svs7 TG mice. Nine-week old WT and Svs7 TG mice were
sacrificed and blood was extracted from both through cardiac puncture and allowed to
clot in room temperature for 20 minutes. The clotted blood was then centrifuged at
3,000rpm in room temperature for 15 minutes to release serum sample. Calcium and
phosphate serum biochemistry measurement was performed at PathWest Laboratory
Medicine of Western Australia and the result showed that there were comparable
calcium and phosphate levels between WT and Svs7 TG mice. Data are presented as
mean ± SEM. Number of mice (n) : 2/group.

Appendix
225
5% 20%
1 2 3 4 5 6 7 8 9 10 11 12 P OC
fraction:
Svs7
V-H+ATPase
α-tubulin
IB:
Supplementary Figure 2. Svs7 protein detection at the secretory vesicles fraction of
osteoclasts. Osteoclast fractions by sucrose gradient centrifugation were subjected to
WB analysis using rabbit polyclonal anti-Svs7 antibody. The result showed that Svs7
was successfully detected at fraction 3 and 4, which correspond to the fraction of
secretory vesicles. Hence, Svs7 is a novel osteoclast-secreted protein. V-H+ATPase
complex served as a positive control for osteoclast-specific marker protein and α-
tubulin was used as a loading control.