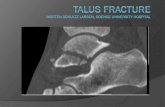
Talar Neck Fractures Presentation
-
Upload
jan-veloso -
Category
Documents
-
view
29 -
download
3
description
Transcript of Talar Neck Fractures Presentation

Talar Neck Fractures
By: Jan Veloso, MS3

Talar Neck Fractures
• Background• Classification System• Symptoms / MOI• Treatment• Sequelae
http://www.feinberg.northwestern.edu/bin/f/h/83-6a.png

Anatomy
• 7 major articulations • 60-70% articular cartilage• No muscular attachments• Bears most weight per surface area

Blood Supply
• Artery of the Tarsal Canal– Branch of Post Tibial A– MAJOR blood supply– Most susceptible to injury
• Deltoid Artery– Branch of Post Tibial A or
Artery of Tarsal Canal• Artery of Sinus Tarsi
– Branch of Anterior Tibial and Perforating Peroneal Arteries.

Background
• Approximately 1.5% of all foot fractures.• 50% of all Talar fractures are at the neck• Historically described as “aviator’s astragalus”

Classification System• Hawkins I
– Non-displaced, non-dislocated– 1 of 3 (sinus tarsi artery)– 0-15% AVN
• Hawkins II– Displaced with STJ dislocation– 2 of 3 (sinus tarsi + tarsal canal arteries)– Up to 40% AVN
• Hawkins III– Displaced with STJ and Ankle dislocation– All 3 sources damaged– Up to 84% AVN
• Hawkins IV (Canale and Kelly)– Displaced with STJ, Ankle, and TN
dislocation– All 3 sources damaged– Up to 100% AVN

Mechanism of Injury
• Historically described in plane crashes
• Axial load and hyperdorsiflexion
• 2 Theories:– Neck of Talus impacts
anterior Tibia– Bending forces cause Talus
to break at weakest point• Today, high speed motor
crash and falls from height

Imaging
• Plain radiographs– AP– Lateral– Ankle Mortise
• Canale view– Pronate 15°with beam 75°
from the horizontal plane– AP view of the talar neck
• CT scan• MRI• Bone Scan

Treatment
• High energy – Polytrauma!• Open vs Closed• Plain X-rays• Hawkins Classification
– Prognostic• Closed reduction
– Hawkins II or Hawkins III/IV if timely ORIF is not possible
– Goal is to reduce stress on soft tissue and decrease chance of NV damage and skin necrosis

Closed Reduction
1. Steinmann pin inserted through calcaneus
2. Traction is applied3. Foot is plantarflexed to
allign STJ4. Compression applied to
heel by pushing up and posterior
5. Thumb pressure is applied medial/lateral of talus to fine tune reduction

Percutaneous Fixation
• Useful in Hawkins I and reduced Hawkins II
• Non-comminuted fractures
• Two parallel 4.5mm partially threaded cannulated screws

Hawkins I
• Non-displaced and non-dislocated
• Canale et al treated with cast for 6-12 wks and NWB for up to 5 months.
• Percutaneous screw fixation– Early ROM, prevent
stiffness and equinus

ORIF
• Displacement >2-5mm, >5° rotation
• Comminuted fractures– Full vs Partial Threads
• Antero-medial and anterolateral incisions
• Med Mal osteotomy– For better visualization– Keep deltoid intact to
preserve blood supply

Sequelae
• Post-traumatic Osteoarthritis– Subtalar Joint– Ankle Joint
• Avascular Necrosis– Talar body collapse
• Malunion– 17.8%
• Nonunion– 5%

Post-Traumatic Arthritis
• Most common complication
• Overall rate of 67.8%• Halvorson et al found
AOFAS score of 52 vs 92 without arthritis
• Ankle Joint– 25.2%
• Subtalar Joint– 48.8%

Avascular Necrosis
• 2nd most common complication– Overall rate of 33.3%
• Most devastating complication– Halvorson et al found AOFAS score of 46.7 vs 76 without AVN
• Hawkins Classification– I – 0-15%– II – Up to 40% – III – Up to 84% – IV – Up to 100%
• Hawkins Sign– 6-8 wks after fracture

Avascular Necrosis
• Hawkins Sign– 6-8 wks or longer– Subchondral radiolucency– Disuse osteopenia and vascular
congestion• Canale et al.
– 23 patients (+) Hawkins Sign; 1 developed AVN
– 26 patients (-) Hawkins Sign; 20 developed AVN
• Schlerosis of Talar body• MRI
– Decreased signal in T1 and T2– High sensitivity
• Bone Scan– Decreased uptake, nonspecific

Avascular Necrosis
• Early time to fixation– Bellamy et al found no
correlation between longer time to fixation and AVN
• Extended NWB– Creep substitution can take
up to 36 months • Talectomy• TTC or other fusion• Talar prosthesis• Core decompression

Take Home Points
• Hawkins Classification has good prognostic value for AVN
• High rates of post-traumatic arthritis and AVN found in displaced fractures
• Proper reduction is critical in order to reduce chances of post-traumatic arthritis

Questions?

Citations
• Bellamy, JL. Keeling, JJ. Wenke, J. Hsu, JR. Does a longer delay in fixation of talus fractures cause osteonecrosis? Jornal of surgical orthopaedic advances. 20(1):34-37, 2011.
• Canale ST, Kelly FB. Fractures of the neck of the talus. Long-term evaluation of seventy-one cases. J Bone Joint Surg Am. 1978; 60: 143-156.
• Fernandez, ML. Wade, AM. Dabbah M. Juliano, PJ. Talar neck fractures treated with closed reductiona nd percutaneous screw fixation: A case series. The American Journal of Orthopedics. 2011;40(2): 72-77.
• Halvorson JJ. Winter BS. Teasdall RD. Scott AT. Talar neck fractures: A systematic review of the literature. The Journal of Foot & Ankle Surgery. 52 (2013) 56-61.
• Juliano, PJ. Dabbah, M. Harris, TG. Talar neck fractures. Foot and Ankle Clinics N Am. 9 (2004) 723-736.
• Lindvall E. Haidukewaych G. DiPasquale T. Herscovici D. Sanders R. Open reduction and stable fixation of isolated, displaced talar neck and body fractures. The Journal of Bone and Joint Surgery. 86(10):2229-2234, 2004.
• Metzger MJ, Levin JS, Clancy JT. Talar neck fractures and rates of avascular necrosis. J Foot Ankle Surg. 1999;38(2):154–162.
• Penny JN, Davis LA. Fractures and fracture-dislocations of the neck of the talus. J Trauma 1980; 20:1029 – 37.
• Sanders DW. Fractures of the Talus. Rockwood and Green’s Fractures in Adults 6th ed. Lippincott William and Wilsons. 2006.


![Femoral neck fractures dnbid lecture [complete]2014 nov](https://static.fdocuments.net/doc/165x107/5592e83c1a28ab2d698b4789/femoral-neck-fractures-dnbid-lecture-complete2014-nov.jpg)