Respiratory Distress Syndrome - Vydehi Institute of ... · Respiratory Distress Syndrome •...
Transcript of Respiratory Distress Syndrome - Vydehi Institute of ... · Respiratory Distress Syndrome •...

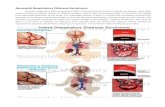
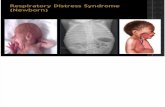
Respiratory Distress Syndrome
IAP UG Teaching slides 2015‐16
1

What the Medical student or primary care physician should know
• Purpose:• Simple intervention CPAP can save many preterm babies
with moderately severe RDS • Surfactant therapy – cost effective / life saving • ANS – prevention of RDS
• Detailed – skill to be acquired• ANS • RD scores
• Basic knowledge
IAP UG Teaching slides 2015‐16 2

Respiratory Distress Syndrome
• Respiratory distress due to ↓surfactant
• Most common cause of RD in premature
• PRIMARY ‐ Prematurity• Genetic
• SECONDARY ‐ Meconium Aspiration• Lung insult‐Asphyxia
IAP UG Teaching slides 2015‐16 3

RDS / HMD
• Preterm, GA 28 – 32 wk• <28wk GA 60‐80% • 32‐36wk GA 15‐30% • 37wk‐term
• Predisposing factors – Prematurity Birth Asphyxia LSCS Male sex Maternal Diabetes Rh Negative
IAP UG Teaching slides 2015‐16 4

Pathogenesis
↓ Surfactant
Alveolar Atelectasis
Hyaline Membrane Formation
Fibrinous ExudatesInterstitial Edema
↓ Lung Compliance
IAP UG Teaching slides 2015‐16 5

Pathogenesis
- Transient Tachypnea- Asphyxia- Hypothermia- Apnea
↓pH, ↓PO2, ↑PCO2↓ Surfactant
RDS
Prematurity- Familial Predisposition- C-Section
Alveolar Hypoperfusion
RL Shunt
Pulm. Vasoconstr.
ShockHypovolemia
Atelectasis
IAP UG Teaching slides 2015‐16 6

Clinical Features
• Usually a Preterm Baby• Respiratory Distress within 6 hrs of Life (usually within
minutes of birth)• SCR, ICR, Grunting, Cyanosis, Ala nasi Flaring*.• Auscultation: ↓ air entry ± fine rales• Apnea in extreme prematurity• Shock• Other features: Edema, ileus, & oliguria
IAP UG Teaching slides 2015‐16 7

Clinical Course
• Severe cases develop respiratory failure needing ventilation / surfactant / CPAP – and may tire and develop apnea / die if care not offered
• Mild cases – can be managed with only oxygen • Symptoms progress to peak in 3 days
• Improvement thereafter (often heralded by spontaneous diuresis)
IAP UG Teaching slides 2015‐16 8

Differential Diagnosis
• Early onset sepsis / congenital Pneumonia
• TTNB
• CHD (TAPVC)
IAP UG Teaching slides 2015‐169

Investigations
• Amniotic fluid – Lecithin to Sphingomyelin ratio• (L/S) ratio
• >2.5 = 0.5%, >2 =10% , • 1.5‐2 = 15‐20%, <1.5 = 60% risk of developing RDS• Blood & Meconium depress mature L/S ratio and may
elevate immature ratio• Exceptions : IDM, Asphyxia‐ can develop RDS even if ratio
ok
• Phosphatidylglycerol = present• Saturated Phosphatidylcholine (SPC) > 500 ug/dl
IAP UG Teaching slides 2015‐16 10

Investigations – Cont... Gastric Aspirate – Shake Test
• Mix 0.5 ml of gastric aspirate & 0.5 ml of absolute alcohol • Shake for 15 seconds & allow the solution to settle for 15
seconds• If no bubbles – 60 % chances of RDS• Small bubbles to the extent of 1/3rd of the circle of the
test tube – 20% chances of RDS• All around the circle – bubbles in two circle in some
places – bubbles in two row & above <1% chances of RDS
IAP UG Teaching slides 2015‐16 11

Investigations (cont…)
• Lamellar body counts (phospholipid “packages” produced by type2 alveolar cells) in amniotic fluid
• >50,000 lamellar bodies/μL → lung maturity
IAP UG Teaching slides 2015‐16 12

Investigations ‐ Contd..
• X‐Ray Chest:
• Reticulo granular pattern
• Air bronchogram
• Ground Glass opacity
• White wash appearance in severe RDS
IAP UG Teaching slides 2015‐16 13

X‐Ray ‐ RDS
IAP UG Teaching slides 2015‐16
14

Investigations – Cont... Related to Acute Care & DD
• Blood Gases – hypoxia and hypercarbia
• Echo – for associated PDA / exclude CHD
• Supportive care • Cranial Ultra sonography
• Blood Chemistry
• Sepsis ScreeningIAP UG Teaching slides 2015‐16 1
5

PREVENTION
• Induction of labour should preferably be delayed till lung maturity
• Prevent fetal asphyxia by antenatal & intranatal monitoring
• Antenatal Steroids (to Mother)• Betamethasone 12mg IM 2 doses in 24 hrs interval
(preferred)• Dexamethasone 4 doses in 12 hrs interval
IAP UG Teaching slides 2015‐16 16

Antenatal steroids
• Must be given to all mothers in preterm labor (<37 weeks)
• Decreases incidence of severe RDS, IVH, mortality by half
• Can be given even if mother has HTN, diabetes
IAP UG Teaching slides 2015‐16 17

Treatment SPECIFIC – Surfactant Therapy
• Types of surfactants:
• Natural – Bovine, Calf, Porcine
• Synthetic
• Timing of intervention:
• Prophylaxis (before onset of RD)
• Treatment (rescue – after onset of RD)
IAP UG Teaching slides 2015‐16 18

Surfactant therapy
• Given in to trachea
• Produces immediate improvement in lung condition
• Relatively costly drug
• No serious side effects in immediate period / long term
IAP UG Teaching slides 2015‐16 19

Supportive Rx
• Ventilatory Support ‐ CPAP & Positive pressure ventilation
• Maintain PaO2 50‐80 mm Hg (SpO2 85‐95%)
• Maintain PaCO2 45‐55 mm Hg
• O2 should be warm, humidified, & delivered by a blender
• Monitor O2 by concentration
IAP UG Teaching slides 2015‐16 20

Supportive Rx (Cont…)
• Shock – Fluids, inotropes
• Temperature Control
• Nutrition – TPN
• Sepsis Rx – Antibiotics till infection is ruled out
• Developmental friendly nursing policy
IAP UG Teaching slides 2015‐16 21

Complications
• Air leaks ‐ Pneumothorax, Pneumomediastinum, PIE, Pneumopericardium, Air Embolism
• PDA – look for & treat aggressively
• Infection – especially Nosocomial
• Intracranial hemorrhage – monitor USG
• Feed intolerance
IAP UG Teaching slides 2015‐16 22

Outcome in the Survivors
• Survival rates near 100 % with CPAP / ventilation and surfactant in babies > 28 weeks / 1000 gms
• No increased respiratory morbidity in future except in extreme preterm• In ELBW Bronchopulmonary dysplasia (BPD) (dependant on
oxygen or respiratory support for prolonged period) 5‐30%• Co‐existing morbidities in very preterm
• Retinopathy of prematurity (ROP) of <1250 g 7%
• Neurologic impairment – related to PVL, IVH, prematurity 10‐15%
IAP UG Teaching slides 2015‐16 3

RD score
1 2
RR 60‐80 >80
Retractions None Mild‐ mod Severe
Grunting None Audible by steth
Audible without steth
Breath sounds Good Decreased Very poor
Saturation Without oxygen
With < 40 % oxygen
High oxygen need
IAP UG Teaching slides 2015‐16
24

IAP UG Teaching slides 2015‐16 25