Chapter 19 Reproductive System Anatomy Male Reproductive System.
Reproductive System Honors Anatomy & Physiology. Male Anatomy.
-
Upload
bathsheba-williams -
Category
Documents
-
view
238 -
download
7
Transcript of Reproductive System Honors Anatomy & Physiology. Male Anatomy.

Reproductive System
Honors Anatomy & Physiology

Male Anatomy

Structures & Their functions
External Genetialia: Penis – copulatory organ
Shaft, glans (enlarged tip), prepuce (foreskin) Erectile (spongy) tissue – connective tissue, smooth muscle, and vascular
spaces Erection – sexual arousal triggers parasympathetic release of NO causing
arterioles to dilate, engorgement restricts drainage Testes (gonads)-1.5” x 1” sperm & testosterone production Scrotum – maintain testes temp 3oC lower than body temp
(retractable) Duct System (sympathetic control over ejaculation)
Epididymis –20 ft long, 20 days for sperm to become motile, may be stored for months (ejaculated by smooth muscle or phagocytized)
Ductus deferens – 18” long, thick smooth muscle Ejaculatory duct – through the prostate and empties into
urethra Urethra – both urine & sperm (has priority!)
3 regions: prostatic urethra, membranous, spongy

Semen Semen – milky white, sticky secretion of
sperm & secretions 2-5mL per ejaculation 20-150milliom sperm per mL Catabolism of fructose provides ATP for
flagella Prostaglandins stimulate uterine peristalsis Accessory Glands
Seminal vesicles – 60% of semen: yellow, viscous alkaline fluid w/fructose, ascorbic acid, prostaglandins enhancing sperm motility
Prostate Gland – 30% of semen: milky acidic fluid w/enzymes to activate sperm
Bulbourthral glands – pea sized glands secrete a thick clear mucus to neutralize acidic urine in urethra “pre-ejaculate”

Structure of the testis Surrounded by 2
membranes: Tunica vaginalis Tunica albuginea
Divided into 250-300 lobules
Ea/w 1-4 seminiferous tubules (sperm production)
Surrounded by myoid cells – contract to squeeze sperm out of testis into rete testis

Spermatogenesis Begins @ age 14 Makes ~400million
sperm/day Spermatogonia –
divide by mitosis @puberty some
become primary spermatocytes generating secondary spermatocytes
Producing non motile spermatotids

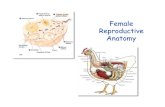
Female Anatomy

Female External Genitalia Vagina – 3-4” birth canal &
copulation organ 3 layers: outer fibroelastic,
smooth muscle, ridged mucosa
Acidic pH – antimicrobial but hostile to sperm
Hymen – vascular membrane in virgins
Mons pubis – fatty ridge Labia: majora & minora –
enclose the vestibule or entrance Vestibular glands – secrete
mucus Clitoris – innervated erectile
tissue hooded by prepuce

Ovaries
Produce Ova (eggs) & Sex hormones Ovarian ligament anchor to uterus & suspensory
ligament to pelvic wall Ovarian follicles ea/contains oocyte surrounded by
follicle cells Primordial follicle – 1 layer cells surround oocyte Primary follicle – 2 + layers of cells Secondary follicle – fluid filled cavity appears Graafian follicle – follicle bulges from ovary surface,
mature oocyte Ovulation – oocyte ejected from ovary Corpus luteum – follicle degenerates into scars/pits

Oogenesis Fetal period – oogonia divide by
mitosis (7 million) Primary oocytes
in primary follicles begin meiosis I, and stall in prophase I (2 milion)
Puberty 250,000 oocytes remain 1 selected every 28 days to
complete meiosis I, first polar body undergoes apoptosis, secondary oocyte is suspended in metaphase II when ovulated
<500 released over 40 years After fertilized, it completes
meiosis II, creating a second polar body that deteriorates and 1 large ovum

Ovarian Cycle @puberty pituitary releases FSH & LH
stimulating ovaries Follicular Phase (days 1-14)
Menstration (days 1-5 ) endometrium sheds Low estrogen & progesterone
Proliferative Phase (day 6-14) FSH & LH follicle growth estrogen (- feedback on release FSH & LH, +
feedback on estrogen) Endometrial lining thickens Cervical mucus thins
Ovulation (day 14) estrogen causes surge of LH & FSH, then
drops Ovary expels 2o oocyte w/corona radiata Mittlschmerz – abdominal pain due to
ovarian wall stretching Luteal /Secretory Phase (days 14-28)
estrogen progesterone (thickens endometrium) Corpus luteum degenerates
21-40 days, avg 28 days)

Female Duct System Uterine (fallopian) tubes
Receive ovulated oocyte About 4” long Fimbraie – ciliated finger like projections on distal
end create current to capture oocytes Infundibulum – funnel shaped structure Smooth muscle (peristalysis) & mucosa ciliated lining
Uterous (womb)- nourish fertilized ovum Inverted pear in size and shape 3 regions: fundus, body, & cervix 3 layers of wall:
Perimetrium – outermost layer Myometrium – smooth muscle Endometrium – 2 layers of mucosal lining (inner layer
sheds)

Menopause 20’s reproductive peak 30’s ovarian function
(quality of oocytes) declines, still ~100,000 oocytes left
By 50, only ~3 oocytes left Estrogen production
declines Menstrual periods erratic &
shorter, until ovulation & menstruation ceases
Menopause reached after 1 year w/o menstruation

Mammary Glands Produce milk by modified
sweat glands Areola – ring of
pigmented skin surrounding nipple
Ea gland/ 15-25 lobes consisting of lobules containing alveoli that produce milk
Milk passes into lactiferous ducts which open at nipple