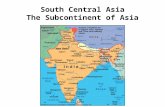
QUALITY STANDARDIZATION AND BIOLOGICAL SCREENING …Indian subcontinent contains 25,000 species of...
Transcript of QUALITY STANDARDIZATION AND BIOLOGICAL SCREENING …Indian subcontinent contains 25,000 species of...

i
QUALITY STANDARDIZATION AND BIOLOGICAL SCREENING OF MEDICINAL PLANTS – CALOTROPIS
GIGANTEA AND SPHAERANTHUS INDICUS
Thesis submitted in Partial Fulfillment for the award of Degree of Doctor of Philosophy in
Pharmacy
By Deepak Teotia
VINAYAKA MISSIONS UNIVERSITY
SALEM, TAMILNADU, INDIA
December-2013

ii
VINAYAKA MISSIONS UNIVERSITY
CERTIFICATE BY THE GUIDE
I, Dr. Prof. S.P. Chakrabarti, certify that the thesis entitled
“Quality standardization and biological screening of medicinal plants-
Calotropis gigantea and Sphaeranthus indicus”, submitted for the
award of Degree of Doctor of Philosophy by Mr. Deepak Teotia is the
record of research work carried out by him during the period from
Oct-2008 to Dec-2013 under my guidance and supervision and this
work has not formed the basis for the award of any degree, diploma,
associate-ship, fellowship or other titles in this University or any
other University or Institution of higher learning.
Place: Signature of the Supervisor with designation
Date:

iii
VINAYAKA MISSIONS UNIVERSITY
DECLARATION
I, Deepak Teotia, declare that the thesis entitled “Quality
standardization and biological screening of medicinal plants-
Calotropis gigantea and Sphaeranthus indicus”, submitted by me for
the award of Degree of Doctor of Philosophy is the record of work
carried out by me during the period from Oct-2008 to Dec-2013
under the guidance of Dr. Prof. S.P. Chakrabarti, Principal of I.M.T.
Puri and has not formed the basis for the award of any degree,
diploma, associate-ship, fellowship, titles in this University or any
other University or other similar institution of higher learning.
Place: Signature of the Candidate
Date:

iv
DEDICATED TO
MY GRANDPARENTS
AND
HUMANITY

v
ACKNOWLEDGEMENT
The dream of doing something in the field of research was no
less than climbing a mountain for me. Today, when I have reached
the summit, I want to express my special thanks of gratitude to all
those who were always beside me to help while I was stepping
forward in order to achieve my goal.
The list of people I need to thank will not fit to a single
acknowledgement section, I just mention some people whose
contribution is obvious.
First and foremost I submit my sincere thanks to Prof. Dr. K.
Rajendran, Dean Research, Vinayaka Missions University, Salem,
Tamilnadu, to pursue my research work.
I am indebted to my research supervisor, Dr. S. P. Chakrabarti.
It was an honour to work under him. I thank him for his sumptuous
suggestions, transcendent and evidence, criticisms to embellish my
study.
I express my sincere gratitude to Dr. S. S. Ajay, for his
contribution of time and ideas to make my PhD. experience
productive and stimulating. The joy and enthusiasm he has for
research was contagious and motivational for me, even during tough
times in the PhD. pursuit.

vi
I gratefully acknowledge the management of V. G. I., Greater
Noida, for providing me all the facilities required to complete my work.
I place on record my sincere gratitude to Dr. S. Singh for
providing animals for biological screening.
I am thankful to all my colleagues for their continuous
encouragement and suggestions. It gives me immense pleasure to
acknowledge lab mates Prashant Pathak and Deepak Sharma who
tirelessly helped me to prepare this thesis.
My thanks are extended to my family for their unconditional love
and encouragement which was my inspiration and driving force to
reach the goal. I am grateful to my parents who supported me in all
my pursuits.
Above all I am indebted to Almighty, who gave me the mental
strength to overcome all the difficulties faced by me in commencing
this thesis.
DEEPAK TEOTIA

vii
CONTENTS
S.No Title Page 1. INTRODUCTION 1
1.1 History of natural products 2 1.2 Significance of flora in the treatment
of ailments 5
1.3 Study of medicinal plants 7 1.4 Herbal medicine 8 1.5 Traditional medicine 8 1.6 The Rasayana concept of Ayurveda 10 1.7 Diabetes 10 1.8 Hyperlipidemia 20 1.9 Antioxidant 26 1.10 Anti-microbial agents 29 1.11 Muscle Relaxant 32
2. AIM AND OBJECTIVE 35 2.1 Need for study 36 2.2 Objectives 37 2.3 Methodology 38
3. PLANT PROFILE 40 3.1 Calotropis gigantea 41 3.2 Sphaeranthus indicus 43
4. LITERATURE 44 4.1 Sphaeranthus indicus 45 4.2 Calotropis gigantea 54
5. EXPERIMENTS 66 5.1 Collection and authentication of
plant material 67
5.2 Physical-chemical evaluation 67 5.3 Method of extraction 70 5.4 Identification of phytochemical
constituents 70
5.5 Total phenol and flavonoid contents 71 5.6 Drugs and chemicals used 72 5.7 Antidiabetic activity of extracts of
Calotropis gigantea 73
5.8 Antihyperlipidemic activity of extracts of Calotropis gigantea
77

viii
5.9 Hypoglycemic effect of Calotropis gigantea leaves via different routes of administration in normal and alloxan induced diabetic rats
80
5.10
Effect of Calotropis gigantea and Sphaeranthus indicus on glycemia and lipidemia in streptozotocin induced diabetic rats
83
5.11 Antioxidant activity of extracts of Calotropis gigantea
85
5.12 Antimicrobial activity of extracts of Calotropis gigantea
86
5.13 Effect of extract of Calotropis gigantea on the skeletal muscle of the rat
91
6. RESULTS AND DISCUSSION 93
6.1 Macroscopic and microscopic features 94 6.2 Physiochemical evaluation 107 6.3 Phytochemical evaluation 114 6.4 Hypoglycemic effects of extracts of
Calotropis gigantea 117
6.5 Hypoglycemic effect of Calotropis gigantea leaves via different routes of administration in normal and alloxan induced diabetic rats
124
6.6
Effect of Calotropis gigantea and Sphaeranthus indicus on glycemia and lipidemia in streptozotocin induced diabetic rats
132
6.7 Antioxidant activity 142 6.8 Antimicrobial activity 142 6.9 Muscle relaxant activity 149
7. SUMMARY AND CONCLUSION 153
8. REFERENCE 158
9. PUBLICATIONS 167

ix
LIST OF TABLES
S.NO TITLE PAGE
1. Stomatal number of upper surface of Calotropis gigantea (leaves)
100
2. Stomatal number of lower surface of Calotropis gigantea (leaves)
100
3. Vein islet number of Calotropis gigantea (leaves) per sq. mm
100
4. Veinlet termination number of Calotropis gigantea (leaves)
101
5. Palisade ratio of Calotropis gigantea (leaves) 101
6. Physicochemical parameters of Calotropis gigantea
109
7. Fluorescent analysis of leaves of Calotropis gigantea
110
8. Fluorescent analysis of root of Calotropis gigantea
111
9. Physicochemical parameters of Sphaeranthus indicus fruit
112
10. Fluorescent analysis of fruit of Sphaeranthus indicus
113
11. Preliminary phytochemical screening of various extracts of Calotropis gigantea
114
12. Preliminary phytochemical screening of various extracts of Sphaeranthus indicus fruit
116
13. Hypoglycemic effect of extracts of Calotropis gigantea in normal rats
118
14. Effect of extracts of Calotropis gigantea on oral glucose tolerance test
119
15. Anti-hyperglycemic effect of extracts of Calotropis gigantea on blood glucose level on streptozotocin-induced diabetes in rats
122
16.
Effect of water extract of Calotropis gigantea leaves on plasma glucose levels after intragastric (p.o) and intraperitoneal (i.p.) administration to normoglycemic rats
125
17. Plasma insulin levels in normoglycemic rats after intragastric (p.o.) and intraperitoneal
127

x
(i.p.) administration of water extract of Calotropis gigantea leaves
18.
Effect of water extract of Calotropis gigantea leaves on plasma glucose levels after intragastric (p.o) and intraperitoneal (i.p) administration to alloxan-diabetic rats
129
19.
Blood glucose levels in glucose loaded (0.25 g/kg BW) rats before and after the intravenous administration of water extract of Calotropis gigantea leaves
131
20.
Effects of treatment of 8 weeks with water extract (300 mg/kg BW) of Calotropis gigantea and Sphaeranthus indicus and a mixture of the two plants on fasting plasma glucose level in streptozotocin (STZ) diabetic rats
133
21.
Effect of water extract (300 mg/kg BW) of Calotropis gigantea and Sphaeranthus indicus and mixture of the two plants on plasma glucose tolerance in diabetic rats after 8 weeks
135
22.
Effect of water extract (300 mg/kg BW) of Calotropis gigantea and Sphaeranthus indicus and mixture of the two plants on plasma glucose tolerance in diabetic rats after 8 weeks
137
23.
Effect of water extract of Calotropis gigantea plus Sphaeranthus indicus on glycosylated haemoglobin, body weight, serum albumin, total proteins and creatinine, urine sugar and albumin values shown at the end of 8 weeks treatment
139
24. Effect of water extract of Calotropis gigantea plus Sphaeranthus indicus on the serum lipid profile in rats fed on high fat diet
141
25. Effect of water extract on liver and kidney weight in rats fed on high fat diet.
141
26. Test organism’s relative percentage inhibition (%)
145
27. MIC values of methanol and aqueous extracts of Calotropis gigantea on test organism
147

xi
28. Antimicrobial activity of Calotropis gigantea 147
29. Muscle relaxant activity of extract from Calotropis gigantea
151

xii
LIST OF FIGURES
S. No Figure Page
1. Parts of Calotropis gigantea 41
2. Fruit of Sphaeranthus indicus 43
3. Powder microscopy of Calotropis gigantea leaves
97
4. T.S. of leaf surface for quantitative analysis of Calotropis gigantea (stomata)
98
5. T.S. of leaf surface for quantitative analysis of Calotropis gigantea (Vein islet number and vein termination number)
99
6. Powder microscopy of Sphaeranthus indicus stem
102
7. Microscopy of Sphaeranthus indicus stem 103
8. Powder microscopy of leaf of Sphaeranthus indicus
104
9. Microscopy of Sphaeranthus indicus leaf 105
10. Microscopy of Sphaeranthus indicus root 106
11. Comparison of antioxidant activity of various extracts
142
12. Antimicrobial activity of Calotropis gigantea 144
13. Relative percentage inhibition of Calotropis gigantea
146
14. Muscle relaxant activity of Calotropis gigantea
149
15. Comparison of muscle relaxant activity of acetylcholine and test drug at different concentrations
150

1
1. INTRODUCTION

2
1. INTRODUCTION
1.1 History of natural products
The use of natural products as medicinal agents presumably
predates the earliest recorded history, as the earliest humans used
various but specific plants to treat illness.
In early 2700 BC, China traced to “The Emperor Shennung”, which
indicates the usefulness of plants for treating diseases.
“Ebers papyrus”, an Egyptian manuscript, written in 1550 BC deals
with the use of plants in Egyptian medicine.
Theophrastus (370 – 285 BC), a Greek native, proposed the
scientific classification of plants.
“Dioscorides De Materia Medica”, written in 77 AD has reported
the medicinal use of over 600 plants.
Ibn-al-Baitar (1197 – 1248 AD), a Muslim scientist, listed 1400
drugs and medicinal plants in his book “Kitab-al-Jami fi al-Adwiya al-
Mufrada.” (The book of simple drugs and food)
In the last decade, the global consumption of medicinal plants in
the herbal and nutraceutical industries have increased dramatically.
In British Columbia, Canada, there are more than 50 medicinal plants
species which are harvested for the herbal, nutraceutical and
pharmaceutical industries (Lantz 2001).

3
Indian subcontinent contains 25,000 species of vascular plants
and 7,800 medicinal drugs manufacturing units which consume 2000
tons of herbs annually.
Market of Ayurvedic medicines is expanding at the rate of 20%
annually. Sales of medicinal plants have grown by 25% in India
during 1987-2008.
Plant based drugs are used directly i.e. they can be collected,
dried and used as therapeutic agents (crude drug). Their extracted
constituents & active principles, reported by various chemical
processes, are employed as medicines.
The active principles or compounds with similar structure and
activity are synthesized chemically to produce synthetic drugs, used
in Allopathy or Modern System of medicine.
A comprehensive approach on medicinal plants was drawn by
WHO which includes:
Therapeutic classification of medicinal plants in different
countries.
Scientific criteria and methods for assessing the safety of
medicinal plant products.
International standards and specification for identification,
purity, strength and manufacturing practices.

4
Method for safe and effective use of medicinal plant products.
Designation of research and training centres for the study of
medicinal plants.
The use of natural plants for treatment of different ailments has
evolved significantly along with human evolution. Traditional
medicines, obtained from plants, have played a vital role in sustaining
disease free human existence on this planet, though now a day many
synthetic drugs are widely used because of their quick therapeutic
action. It is rather difficult to date back the origin of herbal medicines
as a means of therapy. In spite of overwhelming influence of modern
medicine and tremendous advances made on production of synthetic
drugs, traditional medicines have retained their importance in
therapy. Their effectiveness, low cost and comparative freedom from
serious toxic effects make these medicines not only popular but also
an acceptable mode of treating diseases even in modern times.
Traditional and folklore medicines, handed over from
generation to generation, are in household remedies and are now in
community practice. Traditional medicines have served as a source
of alternative medicine and new pharmaceutical healthcare
products. Medicinal plants are important tool for pharmacological

5
research. It is estimated that almost 70% modern medicines in India
are derived from natural products.
The history of medicine in India can be traced to the remote
past. The earliest mention of the medicinal use of plants is found in
the Rig Veda, perhaps the oldest repository of human knowledge,
had been written between 4500 and 1600 BC. In the works which
followed, particularly ayurveda, the properties of various drugs have
been given in detail.
1.2 Significance of flora in the treatment of ailments
In the dawn of human ‘Cultural Revolution’ the art of curing was
essentially magical and was based on logic than on scientific
evidence. Initially few plants, which were usually psychoactive, known
for their magical or psychedelic properties, were used. Later,
empirical medicine arose, which used many plants for the treatment
of various afflictions. This changed dramatically with the Materia
Medica published by Dioscorides and Dictionary of Economic Plants
of India by Watt, which describes the properties of the various drugs
of plant origin. The ancient civilization made an extensive use of
herbal drugs and their use were also well documented in the form of
pharmacopoeia (Lain, 1982).
India was not far behind and had an extensive pharmacopoeia
thousands of years ago. In many eastern cultures such as in India,

6
China and the Arab world, this experience was systematically
recorded and became the Materia Medica of the traditional systems
of medicine. Traditional medicine is a heterogeneous term that refers
to a broad range of ancient natural health care practices which
existed before the application of modern scientific methods to health
care (Pushpangadan, 1995). The traditional plant therapeutic
knowledge of Africa and South America, along with that of China and
India, has given several new drugs to modern medicine. More than
one hundred twenty molecules, used as vital drugs worldwide, have
been extracted from plants. Until 1930, around 90% of the official
medicines were of plant origin (Swain, 1972).
In the biomedical system that dominates the developed world,
there is an over-riding emphasis on research for synthetic therapeutic
compounds, though a certain amount of interest in medicinal plants
always persisted. Many developed countries, including Germany,
have legalized natural products as drugs and many pharmaceutical
organizations are now involved in preparation of plant based drugs by
using plant extracts.
The WHO, an agency of the United Nations, formed to deal with
matters of health in 1977, at its 30th world assembly, adopted a far
reaching resolution urging the governments of member countries, to
give “adequate importance to the utilization of their traditional

7
systems of medicine, with appropriate regulations to suit their national
health needs”. Traditional medicine was also defined as “the
therapeutic practices that have been in existence, often for hundreds
of years, before the development and spread of modern medicine
and are still in use today”.
Many authors have emphasized the value of conducting broad
ethnobotanical, ethnopharmacological and even clinic - therapeutical
research, on medicinal plants.
1.3 Study on medicinal plants
Varieties of reasons have been cited for the need of studying
medicinal plants. Most of the traditional knowledge about medicinal
plants had been in the form of oral knowledge that was lost with
persistent invasions and cultural adaptations. There was no uniform
or standard procedure for maintaining the inventory of these plants
and the knowledge about their medicinal properties. There was
prevalence of using plants and plant based products in various
contemporary and traditional systems of medicine, without any written
documentation or regulation. Therefore, it is essential that such uses
of natural products should be documented and studied for systematic
regulation and wide spread application. The leads for a significant
number of modern synthetic drugs have originated from isolated plant
ingredients, as the search for newer entities begins from either

8
derivatising existing drugs or from traditional or contemporary
medicinal systems. Therefore, it is essential that research on
pharmacological activity of plants, used extensively in traditional
medicines, should be carried out.
1.4 Herbal medicine
All major biomes on earth have been rich source of herbal
drugs even before the evolution of man on earth. By observing
different animals on earth and by using hit and trial methods, man
eventually learnt the use of different plants in treating different
ailments. Almost every regional culture, throughout the the world,
developed a indigenous therapy by using flora of that area. Many of
them kept proper records, which passed on generation to generation
and are still in use. Thus herbal medecines are indigenous in origin
which leads to development of major therapies like Ayurveda,
Homeopathy, Naturopathy, Traditional Chinese Herbalism, Traditional
Oriental medicine, Western Herbalism, etc.
1.5 Traditional medicine
The traditional system of medicine relies on a holistic
approach, i.e. employing crude drug or extract (singly or in
combination) with multiple constituents. Ayurveda, the traditional
system of medicine, has been practiced since 6000 BC. A group of
plants known as “Rasayanas” in Ayurveda have been extensively

9
used as rejuvenators for arresting the ageing process and to provide
resistance against various diseases including those induced by
psychosomatic disorders and promote general well being of an
individual. The “Rasayana” plants used for the day-to-day stress
faced by the individuals are known as adaptogens. They induce
nonspecific resistance of the organism against diverse aversive
assaults, which threatened to disturb internal homeostasis.
The development of drugs from medicinal plants for “primary
health care” (as inflammation, pain, fever, cough, ulcer, wound,
diarrhoea etc.) should be the first goal. This will increase the
popularity of herbal products and the pharmaceutical industries
engaged in herbal products might be able to enhance their export
potential, provided these pharmaceutical industries produce/provide
standardized and effective products. Hence there is an urgent need
to standardize each and every herbal drug/product and these
products should also be scientifically validated in order to have safe,
efficacious and reproducible medicine. To revitalize traditional
medicines, the efficacies claimed for their applications need to be
proved significantly. Even though many plants provide relief but only
those with pharmacologically conformed activity, should be
recommended for use in “primary health care”. (Jia and Zhang, 2005)

10
1.6 The Rasayana concept of Ayurveda
The word rasayana literally means, ‘the path that rasa takes’
(rasa: the primordial tissue or plasma; ayana: path). It is believed, in
Ayurveda, that the qualities of the rasa-dhatu influence the health of
other dhatus (tissues) of the body. Hence any medicine that improves
the quality of rasa (rasayanas) should strengthen or promote the
health of all tissues of the body. These rasayana plants are said to
possess the following properties: they prevent ageing, re-establish
youth, strengthen life and brain power, and prevent diseases. All of
which implies that they increase the resistance of the body against
any onslaught. Traditionally, these agents are used against a plethora
of seemingly diverse disorders with no pathophysiological connection
to modern medicinal science. Looking at these diverse applications
there appeared to be a possibility of identifying adaptogenic agents
from rasayanas. (Ramawat et al., 2004)
1.7 Diabetes
Diabetes mellitus or simply diabetes is a metabolic disorder
indicating high blood sugar levels.This may be either due to
malfunctioning of beta-cells of Islets of Langerhans of pancreas or
because insulin produced by pancreas is not taken up by the cells of
the body.

11
History of diabetes mellitus
Diabetes was known since ancient times and its control
measures were in use since the middle ages, the illumination of its
pathogenesis revealed mainly during the early 20th century. The major
events in this field were:
In 1899, Joseph Von Mering and Oskar Minkowski
conducted experiments on dogs and discovered the role
of pancreas in diabetes.
In 1910, Sir Edward Albert Sharpey Schafer coined the
term “insulin” and proposed that diabetes is due to
deficiency of insulin that was normally produced by
pancreas.
In 1921, the experiments conducted by Frederck Grant
Banting and Charles Herbert Best proved the endocrine
role of Islets of Langerhans of pancreas. They also
isolated insulin from bovine pancreas. This led to
availability of insulin-injections for treatment of diabetes
and for this Banting et al. was awarded the Nobel Prize in
medicine in 1923.
In 1922, clinical diagnosis of diabetes was made
available.

12
In 1935, Sir Harold Percival Himsworth classified diabetes
as Type I diabetes and Type II diabetes.
Identification of sulfonylurea for treating diabetes was
made in 1942.
The radioimmunoassay for insulin was discovered by
Rosalyn Yalow and Soloman Berson.
In 1988, Reaven introduced metabolic syndrome for
treatment of diabetes.
Thiazolidinediones were identified as antidiabetics in
1990.
Etymology
“Diabetes” is a Greek word which means “a passer through; a
siphon” and the world “Mellitus” comes from the Greek word which
means “Sweet”. Apparently, the Greeks named it thus because the
excessive amount of urine, diabetics produce (when blood glucose is
too high), attracted flies and bees because of the glucose content.
The attraction of ants towards the urine of a person was a test for
diabetes in ancient China.

13
Types of diabetes
Type I: Diabetes mellitus
Type I diabetes also referred to as IDDM (insulin dependent
diabetes mellitus or juvenile diabetes). In Type I diabetes beta cells of
Islets of Langerhans of pancreas are destroyed by body’s own
immune system and sufficient insulin is not produced. Type I diabetes
may be caused by an infection by virus. For example-Viruses of
Coxsackie family induce a subtype of Type I diabetes which is similar
to Type II diabetes.
Type II: Diabetes mellitus
Type II diabetes is characterized by “insulin resistance” as
insulin is not taken up by the cells.Type II diabetes is reffered to as
NIDDM (Non Insulin Dependent Diabetes Mellitus). Type II diabetes
is commonly noticed in people above the age of 40 years. Type II
may be caused due to haemochromatosis and polycystic ovary
syndrome, chronic use of steroids, genetic inheritance, and obesity.
Type II diabetes can be treated by changes in diet and exercise in the
initial stage and later, if required, with oral hypoglycemic agents like
sulfonylurea and biguanides as metformin.

14
Gestational diabetes
High blood glucose level in pregnant women, with no previous
diabetic history, is referred to as gestational diabetes and proceeds
as Type II diabetes mellitus.
Congenital diabetes
This involves deficiency of insulin secretion due to defects in
any of the genes responsible for production and secretion of the
insulin.
Other form of diabetes
Cystic fibrosis- related diabetes, Steroid induced diabetes and
monogenic diabetes.
Current status of diabetes
Diabetes mellitus is a group of syndromes which involves high
blood glucose levels and improper metabolism of lipids,
carbohydrates and proteins and an increased risk of complication
from vascular disease. Mostly patients can be classified clinically as
having either insulin dependent diabetes mellitus (IDDM, or Type I
diabetes) or non-insulin dependent diabetes mellitus (NIDDM, or
Type II diabetes). In insulin dependent diabetes mellitus, also called
as juvenile onset diabetes mellitus, destruction of beta cells of Islets
of Langerhans of pancreas takes place. Majority of cases are due to

15
attack on body’s immune system and antibodies that destroy cells
are detectable in blood (Type I A) but in some cases no cells’
antibodies are detected in blood (Type I B).
In non-insulin dependent diabetes mellitus there is no effect on
cell mass. The amount of insulin in blood circulation may be low,
normal or even high but no cell antibody is present. As a high
degree of genetic predisposition generaly has a late onset, (post
middle age) therefore, over 90% of the total cases are Type II
diabetes mellitus (Tripathi, 2003).
Diabetes is one of the most common non-communicable
diseases found globally. It is the fourth leading cause of death in most
developed countries and there is substantial evidence that it is an
epidemic in many developing and newly industrialized nations, thus
posing a serious threat to be met within 21st century. Diabetes is thus
one of the most challenging health problems in the 21st century.
Diabetes can now be found in almost every population in the world
and epidemiological evidence suggests that without effective
prevention and control programmes, diabetes is likely to continue to
rise globally. By the end of the 21st century the worldwide diabetes
will affect an estimated 151 million people, distributed among both
developed and developing countries. In Asia alone an estimated 85

16
million people are affected, this continent has both the biggest
proportion of current cases and the greatest projected increase for
future (Engelgau et al. 2003).
It is estimated that 3.2 million people die due to diabetes across
the world annually. It is also estimated that there are 35 to 40 million
diabetic in India now. Indians are genetically more prone to diabetes
and the World Health Organization (WHO) predicted that number of
diabetic in India would rise to 45 million by 2015 and 74 million by
2025. Diabetes mellitus is projected to affect Asians, specially the
Indians, and the most among all others in the world by 2025
(Ramachandran et al. 2002). WHO also issued a warning as India is
going to be diabetes capital of the world. In 2002, the WHO stated
that the total number of people worldwide with type II diabetes stood
at 176 million. This is estimated to rise to an estimated 370 million
people by 2030. In 2025, the world wide prevalence of diabetes in
adults will be increased by 35%, whereby the number of people with
diabetes will be increased by 122% (Ramachandran et al. 2002).
India will be the country with the largest number of diabetics in 2030
(an estimated 80.9 million) followed by China (an estimated 42
million) and the United states (an estimated 30 million). Diabetes has
a wide spread etiology right from the genetic code to daily diet of the
individual. It is a well known fact that sedentary life styles, obesity,

17
lack of physical work and consumption of food with little or no
therapeutic value are the major contributing factors. At present, the
oral antidiabetic agents belong to class sulfonylureas, biguanides, α-
glucosidase inhibitors, thiazolidenediones and meglitinide derivatives,
are used to treat Type II diabetes. The major limitations of these
drugs are their side effects. The high cost of modern treatment of
diabetes points out to a great need for the development of traditional
or alternative strategies for the prevention and treatment of diabetes.
Further, plants have always been an exemplary source of
modern drugs and many of currently available drugs have been
derived directly or indirectly from them. The ethanobotanical
information reports that about 800 plants may possess antidiabetic
potential.
Genetically Indians are more prone to diabetes
Indians are more prone to diabetes due to their food habits and
life style. Generally obesity and deposition of fat leads to diabetes.
Indians tend to be diabetic at an age of 45, 10 years earlier than in
western countries. 2% of the people in Indian villages are diabetic
and more than half of them are not aware of it.
15 million prescriptions were written for diabetes during
November, 2004 (across 291 towns with a population of > 1 lac).
There has been an increase of 10% in the prescriptions every year.

18
Above forty years of age group accounts for 80% of the total diabetes
prescriptions. Majority of the patients suffer from Type II diabetes.
Out of 100 diabetic patients nearly half of them suffer from a cardiac
ailment. 8% of them are also diagnosed for some neuropathy and
retinopathy.
Blood glucose (blood sugar) level
The normal fasting blood glucose level should be between 70-
110 mg/dl after an overnight fast (not eating anything after midnight).
The normal blood glucose level after 1.5 hours of intake of meal
should be between 90 - 140 mg/dl.
Complications in diabetes
Untreated, diabetes can cause many complications. Diabetic
ketoacidosis, nonketotic hyperosmolar coma include acute
complications of diabetes. Chronic complication includes
cardiovascular diseases, nephropathy (renal failure), and retinopathy
(retinal damage).
Symptoms of Type I diabetes
Increase in appetite, intake of water and urination, loss of body
weight, blurred vision, weakness along with pain in the muscles are
the symptoms of Type I diabetes.

19
Symptoms of Type II diabetes
Increase in appetite, intake of water and urination, loss of body
weight, blurred vision, weakness along with pain in the muscles,
delayed healing of wounds, increased susceptibility to infections,
dehydration, and muscle cramps, etc. are the symptoms of Type ll
diabetes.
Management of diabetes
Type I diabetes
Proper and timely treatment of diabetes is required, as well as a
control on lifestyle such as diet, exercise, stopping smoking, and
maintaining a healthy body weight. Blood sugar should be frequently
monitored and accordingly insulin injection should be taken along
with proper balanced diet, exercise and controlled lifestyle.
Now a days, surgical methods, like transplantation of pancreas,
are being used on experimental basis as a complete cure of Type I
diabetes. But at present the success rate is very limited.
Type II diabetes
Regular monitoring of blood glucose level is essential for proper
management of Type II diabetes. Frequent small meals on definite

20
intervals and light physical exercises like brisk walk of two to four
kilometers a day and yoga have proved to be very effective in
controlling Type II diabetes.
Type II diabetes can be managed by using oral hypoglycemic
agents like sulfonylurea and biguanides. Gastric bypass surgery has
been successful in morbid obesity and Type II diabetes mellitus.
1.8 Hyperlipidemia
Hyperlipidemia is defined as an abnormal elevation in blood
cholesterol, cholesterol esters, triglycerides or phospholipids. The
clinical importance of hyperlipidemia depends on which of these lipids
are elevated and to what extent. Studies have demonstrated that
elevated cholesterol levels are an independent and significant risk
factor for CHD (coronary heart disease). Hypertriglyceridemia has not
been established as an independent risk factor for CHD and is only
considered a marker for other underlying lipoprotein disorders.
Hyperlipidemia can be primary or secondary to some
generalized diseases (e.g. hypothyroidism). They are classified,
according to which lipoprotein particle is raised, into six phenotypes
(the Frederickson classification).
High blood cholesterol is mainly responsible for coronary artery
disease (CAD). A similar link has been shown for raised

21
concentrations of individual atherogenic lipoproteins, in particular the
low density lipoprotein (LDL) fraction. Coronary heart disease (CHD)
is one of the leading causes of morbidity and mortality in the United
States and other industrialized nations. Three of the treatable risk
factors for CHD are hypertension, cigarette smoking and
hypercholesterolemia. The term hyperlipidemia or more precisely
hyperlipoproteinemia refers to conditions in which the concentrations
of cholesterol and/or triglyceride rich lipoproteins are elevated above
normal levels. The term hyperlipidemia is restricted to conditions that
involve increased levels of triglycerides in plasma.
Lipids
Lipids are heterogeneous groups of compounds related to fatty
acids having the common property of being insoluble in water but
soluble in non polar solvents like ether, chloroform and benzene.
Types of lipids
Simple lipids
These are esters of fatty acids and alcohols. Simple lipids may
be of many types depending on the nature of fatty acid and nature of
alcohol present.

22
Compound lipids
These are esters of fatty acid and alcohol but contain certain
other groups according to which they are named like phospholipids,
sulfolipids, aminolipids, cerebrocides etc,
Neutral lipids
This term refers to uncharged lipids which are glycerides,
cholesterol and cholesterol esters.
Lipoproteins
Lipoproteins are particles with high molecular weight and
spherical shape that transport non-polar lipids, primarily triglycerides
(TG) and cholesteryl esters (CE) through the plasma. Every
lipoprotein particle comprises of a non-polar core in which many
molecules of hydrophobic lipids are packed to form oil droplets. This
core consists of triglycerides and cholesteryl esters in varying
proportions and it is hydrophobic in nature. The surface coat, which
surrounds the core, consists of phospholipids, unesterified cholesterol
and apoproteins, and is hydrophilic in nature. The apoproteins or
apolipoproteins are usually present on the surface of lipoproteins.
These proteins serve as an interface between the lipid and the
aqueous environments and also play crucial role in the regulation of
lipid transport and lipoprotein metabolism.

23
Classification of lipoproteins
The lipoproteins vary in composition, size, density and function.
They consist of chylomicrons, very low density lipoproteins (VLDL),
intermediate density lipoprotein (IDL), low-density lipoproteins (LDL)
and high density lipoproteins (HDL).
Lipoproteins are divided into following five major categories
depending on the basis of electrophoresis and ultracentrifugation:
Chylomicrons
Composed of exogenous or dietary triglycerides and carry that
from the intestine to liver, to skeletal muscles and to adipose tissues.
Their density is less than 0.95 gm/mL and diameter is 100-1000 nm.
They contain less than 2% protein, 8% cholesterol, 7% phospholipids
and 84% triglyceride and cholesterolester.
Very low density lipoproteins (VLDL)
Primarily composed of newly synthesised triglycerides and
accounts for 10 to 15% of total serum cholesterol in blood and their
density is 0.95-1.006 gm/mL and diameter is 30-80 nm. They contain
10% protein, 22% cholesterol, 18% phospholipids and 50%
triglyceride and cholesterolester.
Remnant particles or intermediate-density lipoproteins (IDL)
Composed of cholesterol esters and triglycerides, formed from
the degradation of VLDL and enables fats and cholesterol to move in

24
blood stream. Their density is 1.006-1.009 gm/mL and diameter is 25-
50 nm. They contain less than 18% protein, 29% cholesterol, 22%
phospholipids and 31% triglyceride and cholesterolester.
Low density lipoproteins (LDL)
Composed primarily of cholesterol and accounts for 60 to 70%
of total serum cholesterol and is the major artherogenic class of
lipoproteins and helps in the transport of cholesterol from the liver to
the body cells. Their density is 1.019-1.063 gm/mL and diameter is
18-28 nm. They contain 25% protein, 50% cholesterol, 21%
phospholipids and 8% triglyceride and cholesterolester.
High density lipoproteins (HDL)
Composed primarily of cholesterol and accounts for 20 to 30%
of total serum cholesterol and they collect cholesterol from the tissues
and carry that to the liver. .Their density is more than 1.063 gm/mL
and diameter is 5-15 nm. They contain less than 33% protein, 30%
cholesterol, 29% phospholipids and 4% triglyceride and
cholesterolester.
Etiology of hyperlipidemia
Hyperlipidemia can be caused by genetic predisposition,
through secondary causes (like underlying disease states, drugs, or
lifestyle), or both. The severe forms of hyperlipidemia are normally
observed in individuals with specific inherited traits that have resulted

25
in defects in lipid metabolism or transport (e.g. absence of LDL
receptors), patients with hereditary (primary) disease usually require
medication and intensive intervention to prevent morbidity associated
with the condition. Mild or moderate hyperlipidemia is most
commonly caused by some degree of inherited predisposition in
combination with one or more secondary causes.
Concomitant diseases, lifestyle and medications are the three
main secondary causes of hyperlipidemia. Hypothyroidism, nephritic
syndrome, diet high in saturated fats and cholesterol can contribute to
hypercholesterolemia. A high intake of fats, carbohydrates, total
calories and alcohol, as well as a sedentary lifestyle increases
triglyceride levels. Type II diabetes mellitus is a common cause of
hypertriglyceridemia that is aggravated by the associated obesity.
Treatment of hyperlipidemia
The decision to treat hyperlipidemia should not be taken lightly,
since therapy is likely to be life-long and is not without risk. At least
two readings of cholesterol should be obtained over 2-3 months.
Underlying diseases, which may cause hyperlipidemia, such as
hypothyroidism or liver disease, should be taken care of immediately.
The exact cholesterol concentration requiring treatment depends on
other risk factors: in a patient with established ischaemic heart
disease as low as 5.5mmol/L would be appropriate, while in

26
otherwise healthy patients, higher levels should be required. Drugs
may take several weeks to achieve their effects and frequent change
of drug is not advised. Combinations of drugs are sometimes
required.
Drugs used in treating hyperlipidemia
Bile acid sequestrants: Cholestyramine
Fibrates: Gemfibrizol Berizafibrate, ferofibrate
HMG CoA reductase inhibitors: simvastalin
Nicotinic acid.
1.9 Antioxidants
These are the group of compounds that wipe out free radical
oxygen in the body, and thus prevent damages due to oxidation of
cells. They are essential for good health and are found naturally in
many vegetables and fruits. Antioxidants act as radical scavengers,
hydrogen donors, peroxide decomposers, electron donors, enzyme
inhibitors, singlet oxygen quenchers, synergist and metal chelating
agents (Tiwari, 2001).

27
Antioxidants Defense System (ADS)
Antioxidant defense system (ADS) works against oxidative
stress of the cells and follows many lines of action. Antioxidants are
classified in four categories on the basis of their line of action.
Preventive antioxidants
They suppress the formation of free radicals.
Radicals scavenging antioxidants
They suppress the chain initiation and breaking of chain
propagation reaction.
Repair and de novo antioxidants
They include various enzymes which identify, destroy and
remove oxidatively modified proteins and thus also prevent deposition
of oxidised proteins.
Adoption antioxidants
They produce the signals which help in production and
transportation of suitable antioxidant to its site of action. (Halliwell,
1999)
Nutritional antioxidants
Vitamin A (retinol): it is synthesised in the body by using
provitamins present in carrot, papaya, spinach, sweet potatoes,
tomatoes, cabbage, etc. Cod liver oil, shark liver oil, milk, butter and
ghee are rich sources of vitamin A. Its recommended daily allowance

28
is 5000 I.U. per day for an adult person.Its antioxidant property is
responsible for the integrity of epithelial tissues.
Vitamin C (ascorbic acid): it is present in citrus and emblic
fruits, green vegetables, potatoes, tomatoes, berries, milk and liver. It
cannot be synthesised in human body. It helps in formation and
maintenance of collagen in the intercellular material of connective
tissues. It is required in tyrosine metabolism and utilization of iron. Its
daily intake should be about 30 mg.
Vitamin E (tocopherol): vegetable oils and liver of horses and
cattles are rich sources of vitamin E. It inhibits peroxide formation
which in turn prevents damage to membrane lipids. It also prevents
oxidation of unsaturated fats. Its daily requirement for an adult person
is 30 I.U.
Selenium: its antioxidant properties are known to reduce the
chances of prostate cancer, confirmed by recent studies carried out
by the National Health System of China. Its dietry sources are garlic,
nuts, grains, sunflower seeds, shellfish, red meat, chicken, etc.Plants
grown in selenium rich soils are also a good source of selenium.
Bio-flavonoids: dark berries, green tea and green coffee are
rich sources of bio-flavonoids which depicts antioxidant properties.
The non essential antioxidants include enzymes such as
glutathione peroxidase, superoxide dismutase and catalase, bilirubin

29
and omega 3 fattyacids, as they are naturally synthesised within
human body.
Free radicals
Cells, in human body, use oxygen to catabolise carbohydrates,
proteins and fats to get energy. Metabolically active cells produce by
products called free radicals which are highly reactive due to
presence of at least one unpaired electron. They are responsible for
oxidation reactions involved in energy production and functioning of
immune system, especially antibacterial cellular activities (Maxwell,
1995).
Excess of free radicals attack DNA, a cell’s genetic material
(Cancer) and blood vessels (cardiovascular diseases). They are also
implicated in arthritis, strokes, cataracts and degenerative health
problems such as diabetes, ischemia, dementia and aging. Fried
food, cigarette smoke, air and water pollution as well as toxins also
create free radicals.
1.10 Anti-microbial agents
Micro-organisms are the living organisms which can be seen
only under a microscope and consist of a single or a clump of cells.
They may be named as fungi, viruses, bacteria, protozoans, etc.
Antimicrobial agents are the drugs which either inhibit the growth or
kill the micro-organisms.Antibiotics are the drugs derived from living

30
organisms. Chemotherapeutic agents are the chemical substances
acting as antimicrobial agents. Bactericidals are the drugs which kill
bacteria. Bacteriostatics are the drugs which inhibit the growth of
bacterias.
History
The history of anti-microbial drugs can be divided into three
different stages:
Stage I: In 1619, alkaloid like Cinchona bark was used to treat
malaria, Ipecacuanha root was used to treat dysentery, etc.In this
century very few chemotherapeutic agents were known.
Stage II: This stage involved the use of synthetic compounds. In
1909, Paul Ehrlich discovered Salvarsan. Klarer and Mietzsch, in
1932, discovered Prontocil which liberates para-amino-benzene
sulfonamide and it was found effective against Streptococci
infections. In 1938, Sulphapyridene was discovered and found
effective against Pneumococcal pneumoniae and was followed by
Sulfathiozol and Sulfadiazene with improved antibacterial activity.
Stage III: This stage started with the use of antibiotics. Louis Pasteur
and Robert Koch observed inhibition of growth of Bacillus anthrasis.
In 1939, Renedudos reported tyrothricin. Floray and Chain purified
penicillin-G.

31
Even after the above mentioned discoveries a variety of
different classes of antibiotics have been discovered, but still the urge
for discovering new antibiotics is in progress.
Etymology
The term “antibacterial” is derived from Greek word vti (anti)
which means “against” and baktnplov (bakterion) which means
“bacteria”.The word “antibiotics” is derived from vti (anti) and biwtikoc
(biotikos) whch means “fill for life, lively”.
Medicinal Use
Antimicrobial agents are used in the treatment of infections
caused by bacteria, protozoa, virus, fungi, etc. Antimicrobial agents
are used for immune modulation. Antimicrobial agents are used to
prevent infections during and after the surgeries, prophylactics and in
various conditions of cancer.
Classification
Antimicrobial agents are classified on the basis of mechanism
of action, presence of chemical entity and spectrum of activity. The
major classes include antibiotics, antivirus, antifungal and anti
protozoa.
Antibiotics are the drug of choice for the treatment of almost all
type of infections, acquired infections and community acquired
infections. The superbugs have developed antibiotic resistance and

32
may lead to very serious diseases that are difficult to treat and may
result in death. Superbugs are developed both in the environment
and within the host organisms, which is why it is important to not
routinely disinfect and cleanse with antimicrobials or overuse
antibiotic medicines that may lead to evolution of resistant organisms
(Superbugs).
Development of resistance against a antimicrobial drug is very
frequent on prolong use. So there is always a need to find new
molecules or to derive new derivatives with better efficacy and fewer
side effects.
1.11 Muscle Relaxant
A muscle relaxant is a drug which affects skeletal
muscle function and decreases the muscle fatigue. Muscle relaxants
are used to provide relief from muscle spasm, muscle cramps,
muscle fatigue, musclular pain and hyperflexia. Muscle relaxants are
classified as neuromuscular blockers and spasmolytics.
Neuromuscular blockers are not centrally acting drugs. They interfere
with neuromuscular transmissions. They are used to produce
temporary paralysis during surgical procedures, intensive care and as
an emergency medicine. Spasmolytics act on central nervous system
and known as "centrally acting" muscle relaxants. They are used to

33
provide relief from musculoskeletal pain and spasms and to treat
spasticity in various neurological conditions.
History
In 16th century people of the Amazon Basin in South America
used poison-tipped arrows to produce death by paralysis. The active
compound identified as Curare became the basis of further studies in
the field of muscle relaxants. Scientific experiments determine the
role of tubocurarine and acetylcholine in transmissions at
neuromuscular end plates. Upto 1943, muscle relaxants were
established and used in anesthesia and surgery.
The U.S. Food and Drug Administration (FDA) approved the
use of Carisoprodol in 1959, metaxalone in August, 1962,
and cyclobenzaprine in August, 1977.
Mechanism
Muscle relaxants can be active at various sites which include
central nervous system, myelinated somatic nerves, unmyelinated
motor nerve, terminal nicotinic acetylcholine receptors muscle etc.
They inhibit transmissions at the end plate of neuromuscular
junctions.

34
After being adequately stimulated, an active potential is
generated due to which a nerve impulse get triggered at motor end
plate. This initiates influx of calcium ions which causes exocytosis of
synaptic vesicles containing acetylcholine leading to diffusion of
acetylcholine across the synaptic cleft. Acetylcholine may either be
hydrolysed by acetylcholine esterase or it may bind to the nicotinic
receptors. A confirmational change occurs in receptors due to binding
of two acetylcholine molecules which opens the sodium - potassium
channel. As a result Na+ & Ca++ enter the cell & K+ leave the cell
resulting in depolarization of the end plate leading to muscle
contraction.
There are two mechanisms to inhibit end plate function:
Non-depolarizing agents, like tubocurarine inhibit the binding of
acetylcholine to nicotinic receptors and hence prevents depolarization
of the end plate.
Depolarizing agents, like succinylcholine imitate acetylcholine to
sensitize nicotinic receptors to such an extent that it can no longer
initiate any action potential to cause muscle contraction.
Both of the above mentioned neuromuscular blockers are
structurally similar to acetylcholine.

35
2. AIM AND OBJECTIVE

36
2. AIM AND OBJECTIVE
2.1 Need for Study
Many oral hypoglycemic agents, herbal remedies like leaf
powder, pastes, decoctions, infusions and pills have been
recommended but no medicine is capable of giving the radical cure of
diabetes mellitus.
It has been found that about 75 plants posses’ hypoglycemic
activity but only few have been studied in detail.
Allium cepa, Anacardium occidentale, Coccinia indica
Clerodendrum phlomidis, Ficus benghalensis, Dolichos lablab, F.
glomerata, Enicostemma littorale, Gymnema sylvestre, Momordica
charantia, Olea europaea, Pterocarpus marsupium, Orthosiphon
spiralis, Rauwolfia serpentine, Cyamopsis tetragonoloba, Scoparia
dulcis, Syzygium cumini, etc have been tried on human beings but
not to an extent where they can be taken as a drug.
Despite of so much potential and scope of future development,
only 2% of the flora provided by nature is being used beneficially.
The use of herbs is highly beneficial to the community as they:-
are nutritious and good alternative medicines,
are safe and effective forms of ancient therapy,
have no side effects as allopathy system of medicine,

37
provide natural resistance power to the body, and
are used for healing purpose and maintaining the body balance
that help in regulating the body functions.
By using natural products, about 76 million people tend to look
new solutions to treat old problems related to diabetes.Therefore,
there is a need to search effective and safe drug for diabetes mellitus.
Herbal drugs are prescribed widely because of their effectiveness,
less side effects and relatively low costs, even when their biologically
active compounds are unknown.
2.2 Objectives
The experimental work has been designed to achieve the
following objectives:
Collection, identification and authentication of medicinal
plants- Calotropis gigantea and Sphaeranthus indicus and
their parts- leaves, roots and fruits.
Quality standardization of plant extracts by ash value,
extractive value, foreign matter, etc.
Phytochemical investigation of plant extracts by different
chemical tests i.e. alkaloids, glycosides, etc.
To investigate Calotropis gigantea and Sphaeranthus indicus
for antidiabetic activity, serum lipid profile and their effect on

38
liver and kidney weight.
To investigate Calotropis gigantea for antioxidant,
antimicrobial and muscle relaxant activity.
To give scientific evidence in support of the plants-
Calotropis gigantea and Sphaeranthus indicus for their
traditional use as folklore medicine.
Concluding the results.
2.3 Methodology
Collection, identification and authentication of medicinal
plants- Calotropis gigantea and Sphaeranthus indicus and
their parts- leaves, roots and fruits.
Quality standardization of plant extracts by ash value,
extractive value, foreign matter, moisture contents, etc.
Phytochemical investigation of plant extracts by different
chemical tests i.e. alkaloids, glycosides, etc.
Pharmacognostical evaluation including morphology and
microscopical investigations.
Evaluation of antihyperglycemic activity and lipid profile of
the extracts of selected medicinal plant on chemically
induced diabetic rats and their effect on weight of liver and
kidney.

39
Evaluation of antioxidant, antimicrobial and muscle relaxant
activities of the extracts of Calotropis gigantea.
Results and discussion.
Conclusion.
.

40
3. PLANT PROFILE

41
3. PLANT PROFILE
3.1 Calotropis gigantea
Figure 1: Parts of Calotropis gigantea
Family
Calotropis gigantea belongs to the family- Asclepiadaceae,
which is generally called milkweed or swallow-wort. It is a common
wasteland weed (Singh et al. 1996). Asclepiadaceae includes 280
genera and 2,000 species which are cosmopolitan in origin. They are
most abundant in tropical and sub-tropical regions and are rare in
cold regions. Some of the other plants belonging to the family
Asclepiadaceae are Milk weed or Silk weed (Asclepias syriaca L.),
Butterfly weed (Asclepias tuberosa L.) and Calotropis procera (Ait.).

42
Plant Description
Botanical name: Calotropis gigantea
Common names: Gigantic swallow wort, Madar
Height: 8 – 10 ft.
Leaf: arrangement – opposite; sessile
Flower: size- 2 inches; white to purple, rarely light green or yellow;
not scented
Fruits: follicles recurved, 1 or 2 follicles, second more often
suppressed, 3-4" long
Origin: India
Habitat: wasteland
Distribution: throughout India upto altitude of 900 m

43
3.2 Sphaeranthus indicus
Figure 2: Fruit of Sphaeranthus indicus
Family: Asteraceae
Botanical name: Sphaeranthus indicus
Common names: Mundi, Hapus, Gorkhmundi, Boddasoramu,
Kottak aranthai, Mirangani, Murisa, Ghundi, Belaunja, etc.
Morphology: a highly branched, strongly-scented annual weed with
winged stem
Leaf: obovate-oblong, narrowed at the base, dentate and serrate
Flower: compound heads, globose ovoid, glandular hairy, achene
staled; flowering time is November to January
Habitat: rice fields
Distribution: throughout India, Sri Lanka, Africa and Australia
Useful Parts: root, leaves, flowers and seed

44
4. LITERATURE

45
4. LITERATURE
4.1 Sphaeranthus indicus
4.1.1 Phytochemical investigation
Baslas KK et al. 1959; have isolated essential oils – methyl chavicol,
α- ionone, d- cadinine, p- methoxycinnamaldehyde, ocimene, α-
terpinene, citral, geraniol, geranyl acetate, β- ionone, sphaerene,
indicusene and sphaeranthol from Sphaeranthus indicus.
Baslas KK et al. 1960; have isolated yellowish green oil with
linolenic, linoleic, oleic, palmitic, stearic and arachidic acid from entire
plant of Sphaeranthus indicus.
Gupta Raj Kumar et al. 1967; have reported the presence of
stigmasterol, hentriacontane, β-sitosterol, and β-D-glucoside of β-
sitosterol.
Nigam SS et al. 1968; have reported the presence of the essential
oils in Sphaeranthus indicus - cadinene, α-ionone, β- caryophyllene,
p-methoxy cinnamaldehyde, eugenol, α-phellandrene, ocimene,
citral, α-terpinene, etc.
Gogte MG et al. 1986; have isolated hydroxylactones (I, II and III)
from Sphaeranthus indicus.

46
Sohni Jayant S et al. 1988; have isolated a new sesquitepene
lactone-7α-hydroxyeudesm-4-en-6,12-olide(I), a new sesquiterpene
acid, 2-hydroxycaustic acid (II), along with β-eudesmol and ilicic acid
from acetone extract of Sphaeranthus indicus.
Singh SK et al. 1989; have isolated (24S)-2-4-Ethyl cholesta-5, 22-
dien-3β-olβ-D-glucoside from Sphaeranthus indicus.
Atta-ur-Rahman et al. 1989; have isolated an antimicrobial
sesquiterpene lactone, 7-hydroxyfrullanolide from flowers of
Sphaeranthus indicus.
Shekhani MS et al. 1990; have reported an immunostimulant
sesquiterpene glycoside in flowers of Sphaerenthus indicus.
Shekhani MS et al. 1991; have isolated three eudesmanolide, 11α,
13-dihydro-3αn, 7α-dihydroxyfrullanolide, 11α, 13-dihydro-7α-hyroxy-
13-dihydroxyfrullanoide, 11α, 13-dihydro-7α-hydroxy-13-
methoxyfrullanolie from the flowers of Sphaeranthus indicus.
Rojatkar Supada R et al. 1992; have reported two known
eudesmanolide, two sesquiterpenoids, cryptomeridiol and 4-
epicryptomeridiol in Sphaeranthus indicus.
Chughtai MID et al. 1992; have isolated, purified and structural
elucidation was done of alkaloids in methonolic extract of flowers of
Sphaeranthus indicus. The presence of cyclopeptide alkaloidal ring
was confirmed.

47
Rojatkar Supada R et al. 1994; have obtained a new 5α, 7-
dihydroxy eudesmanolide (I) alogwith two known eudesmanolide (II,
III) (Z=0) from photooxidation of 7-hydroxy eudesmanolide (III)
[Z=H2]. The structures have been established by spectral data and
comparison with natural products.
OO
OHOH
CH2
O
OCH2
O
CH2
OH
Me Me
OH
I II
O
O
O
CH2
Me
OH
Me
III
Yadava RN et al. 1998; have reported the chemical evaluation of
leaves of Sphaeranthus indicus.

48
Yadava RN et al. 1998; have isolated 7-hydroxy-3’,4’-5,6,-
tetramethoxy flavone7-O-β-D-(1→4)-diglucoside from stem of
Sphaeranthus indicus.
OO
OO O
OMe
OMe
OMe
MeOOH
OH
CH2
CH2
OH
OH
OH
HO
HO
O
Yadava RN et al. 1999; have isolated a novel flavone glycoside, 5,
4’dihydroxy-3’-prenylbiochanin-7-O-β-D-galactoside from the leaves
0f Sphaeranthus indicus.
O
OMe
OH
OMe
H2C
O
CH C
CH3
CH3
OO
CH2
OH
OH
OH
HO

49
Pujar Prasad P et al. 2000; have isolated three new eudesmanolides
as 11α, 13-dihydro-3α, 7α-dihydroxy-4-5-epoxy-6β, 7-eudesmanolide
(I), 11α, 13-dihydro-7α-acetoxy-3β-hydroxy-6β-7-eudesm-4-enolide
(II), 3-keto-β-eudesmol (III) by spectral analysis.
O
HO
OH
Me
Me
O
MeO O
H
O
Me
MeHO
O
Me
H OAc
I II
Me
CO
CH2
H
CH3
OH
CH3
III
Jirovetz L et al. 2003; have isolated and analysed essential oils of
Sphaeranthus indicus flowers, roots, stems and leaves by GC-MS
and olfactoric methods. More than 95 volatile compounds were found.
The main components are β-eudesmol, 2,5-dimethoxy-p-cymene, β-
caryophyllene τ-cadinol, caryophyllene oxide and α-eudesmol, (Z)-
arteannuic alcohol, β-maaliene, β-eudesmol etc.

50
Lodha Vandana 2003; have reported the presence of essential oils
in capitula of Sphaeranthus indicus – (0.06 – 0.08%) by GC-MS
examination. The main constituents found were cadinene, ocimene,
citral, p-methoxy cinnamaldehyde, geraniol, eugenol, and geranyl
acetate.
Jadhav Ravindra B et al. 2004; have isolated a new eudesmanolide
from aerial part of Sphaeranthus indicus - 11α, 13-dihydo-3α, 7α-
dihydroxy frullanolide and 2α-dihydroxycostic acid.
Chandra Pal Bikas et al. 2001; have isolated (-) – frullanolide from
dried and powered flowers of Sphaeranthus indicus and reported
antifungal, antibacterial and antiprotozoal activity.
Kaul Pran N et al. 2005; have reported essential oils’ composition of
Sphaeranthus indicus on the basis of GC and GC-MS. Thirty eight
compounds, making up to 84.0% of oil content, were identified. The
major compounds were – 2, 5-dimethoxy-p-cymene, α-agarofuran,
10-epi-ϒ-eudesmol and selin –11- en-4α-ol.
Prashanth Kumar V et al. 2006; have isolated peptide alkaloids with
cytotoxic activity against various cancer cell lines. They are effective
in prophylaxis and treatment of cancers.
Prabhu Kirti S et al. 2006; have done pharmacogonostical
evaluation of Sphaeranthus indicus including physiochemical,
morphological and histological parameters.

51
Mitra Shanker Kumar et al. 2006; have isolated alkaloids
monoterpenes, sesquiterpenes, sesquiterpene lactones,
sesquiterpene lactone glycosides, diterpenes, triterpenoids, fatty acid
esters, hydrocarbons and amino acids. They have reported antitumor
activity in vitro of sesquiterpene lactone 7-hydroxy-eudesm-4-en-6,
12-olide (HAC-1).
Jadhav Ravindra B et al. 2007; have isolated two new
eudesmanolide from aerial part of Sphaeranthus indicus - 11α, 13-
dihydro-3α, 7α- dihydroxyeudesm-4-en-6α, 12-olide and 1, 4-en-6β,
7α-eudesmenolide-3, on the basis of spectral studies.
Mishra Bhuwan B et al. 2007; have isolated a novel flavanoid C-
glycoside, 5-hydroxy-7-methoxy-6-C-glycosylflavone (I), from aerial
parts of Sphaeranthus indicus.
Vikani KV et al. 2008; have developed HPTLC method to quantify 7-
hydroxy eudesmanolidde using mobile phase n-hexane: diethyl ether
(3:7) and scanning the plate at 213 nm.

52
4.1.2 Pharmacological investigation
Rao BGV Narasimha et al. 1970; have studied in vitro antimicrobial
efficiency of essential oils against Staphylococcus aureus, Vibrio
cholerae and Escherichia coli.
Dubey KS et al. 2000; have studied antimicrobial activities of
alcoholic & aqueous extracts of Sphaeranthus indicus against
Alternaria solani, Fusarium oxysporum, Pencillium pinophilum.
Sharma Manik et al. 2003; have tested a bicyclic sesquiterpene
lactone from petroleum ether extract of Sphaeranthus indicus on
most sensitive preimaginal stage of the mosquito Anopheles
stephensi at different time intervals.
Bafna AR et al. 2006; have studied the protective effect of bioactive
fraction of Sphaeranthus indicus against immunosupression induced
by cytotoxic agent cyclophosphamide in mice.
Sadaf Farzana et al. 2006; have studied wound healing activity in a
cream containing ethanolic extract of aerial part of Sphaeranthus
indicus in Guinea pigs.
Shirwaikar Annie et al. 2006; have studied in vitro antioxidant effect
of ethanolic extract of Sphaeranthus indicus.
Attaullah MD et al. 2006; have studied antimalarial effect and its
medicinal and therapeutic uses.

53
Ignacimuthu S et al. 2006; have studied antifeedant activity, against
4th instar larvae of Spodoptera litura, of methanol extract of
Sphaeranthus indicus.
Chauhan Vijay et al. 2007; have studied the anti-inflammatory
activity of extract of flowering and fruiting heads of the Sphaeranthus
indicus.
Bafna AR et al. 2007; have studied the effect of petroleum ether
extract of flower heads of Sphaeranthus indicus in increasing
phagocytic activity, hemagglutination antibody titer and delayed type
hypersensitivity in mice (Immunomodulatory activity).
Dubey LN et al. 2007; have studied the antimicrobial activity of
terphenoidal compound isolated from Sphaeranthus indicus against
Bacillus subtilis. 70% methanol extract was used.
Ram A Jeevan et al. 2007; have studied the antimicrobial activity of
essential oils and methanol extract of Sphaeranthus indicus against
Pseudomonas aeruginosa, Staphylococcus aureus, Micrococcus
luteus, Micrococcus roseus, Candida albicans and Candida tropicalis.
Razi Muhammad T et al. 2011; have studied antidiabetic activity of
methanolic extract of Sphaeranthus indicus in alloxan induced
diabetic rats.

54
4.2 Calotropis gigantea
4.2.1 Phytochemical investigation
Basu Kali Pada et al. 1934; have reported the presence of
calosterol, a sterol in the milky juice of Calotropis gigantea.
Basu Kali Pada et al. 1936; have reported the presence of
proteinase in the milky juice of Calotropis gigantea and have done its
purification and activation by ascorbic acid and glutathione.
Murti P Bhaskara Rama et al. 1945; have studied the chemical
composition of Calotropis gigantea flowers.
Balakrishna KJ et al. 1945; have reported the chemical constituents
of Calotropis gigantea from latex, root and bark, and found α - and β -
calotropeols gigantin (III) (cardiac poison), equal amount of resinols,
giganteol (II) and isogiganteol (III), wax and resin compound, acetic
acid isovaleric acid, β amyrin, α – calotropeol, β – calotropeol,
tetracyclic compounds, calcium oxalate and solid material like cardiac
poison similar to uscharin.
Biswas Bibhutybhusan et al. 1947; have examined the bast fiber
from Calotropis gigantea.
Anjaneyulu V et al. 1968; have isolated α- amyrin, β – amyrin,
taraxasterol, Ψ- taraxasterol, β – sitosterol, taraxasteryl acetate, 4 –

55
taraxasteryl benzoate from petroleum ether extract of 2.5 kg
Calotropis gigantea.
Tiwari SN et al. 1979; have reported the constituents of latex of
Calotropis gigantea by T.L.C. Out of 7 spots obtained, 3 were
identified as calotoxin, uscharin and calactin.
Abraham KI et al. 1979; have studied proteinases, calotropain F I
and F II from Calotropis gigantea latex.
Gowda D Channe et al. 1980; have reported a polysaccharide
isolated from seed- hairs of Calotropis gigantea. Structural studies of
hemicellulose were done.
Pal G et al. 1980; have isolated, crystallized and studied the
properties of calotropin D I and D II extracted from latex of Calotropis
gigantea.
Heinemann U et al. 1982; have reported the 3 – dimensional crystal
and molecular structure of crysteine protease and calotropin D I at
3.2- ANG resolution.
Rao K Sundar et al. 1983; have reported the percentage content of
oil and protein in the seed of Calotropis gigantea. The major essential
amino acids in the seed protein were phenylalanine, lysine and
histidine.
Inamdar Shashikala R et al. 1983; have reported the presence of
hemagglutinins (Lectins) in the latex of plant.

56
Thakur Swapnadip et al. 1984; have reported that hexane and
methyl alcohol soluble extracts of the latex coagulum of Calotropis
gigantea contains two new triterpene esters, 3’ – methylbutanoates
of α – amyrin and Ψ – taraxasterol.
Sengupta A et al. 1984; have reported autodigestion of two cysteine
proteinases, calotropin D I and calotropin D II isolated from latex of
Calotropis gigantea.
Bhattacharya D et al. 1985; have reported the ionization of phenolic
(OH) group in calotropin D I and D II isolated from latex of Calotropis
gigantea. Out of twelve tyrosine residues from calotropin D I and
thirteen tyrosine residues from calotropin D II, only four residues were
ionized reversibly in the pH range 8.9 – 10.7 with apparent value 9.7.
De Siba Prasad et al. 1988; have reported uscharidin, uzarigenin,
calactin and calotropin in Calotropis gigantea root by H.P.L.C. with
methyl alcohol as a solvent and detected at 226 nm.
Lakshminarayana G et al. 1988; have isolated surface and internal
lipids of Calotropis gigantea leaves. The surface lipids consisted of
22.2% of hydrocarbons, 20.7% of ester waxes, 7.9% of aldehydes,
4.6% of triacylglycerols, 20.0% of fatty acids, 13.2% of sterols, 3.3%
of diacylglycerols and 2.9% of monoacylglycerols. The internal lipids
contained monoglycerols. The glycolipids comprised of 2.4% of
esterified sterylglycosides, 8.4% of monogalactosyldiglycerides, 1.7%

57
of sterylglycosides, 2.3% of cerebrosides, 4.2% of
digalactosyldiglycerides and 27% of sulfoquinovosyldiglycerides. The
phospholipids were composed of 2.8% of cardiolipin, 5.6% of
phosphatidylglycerol, 4.0% of phosphatidylethanolamine, 3.6% of
phosphatidylinositol, 8.3% of phophatidylcholine and 1.2% of
phosphatidylserine. All internal lipid classes contain high amounts of
palmitic and linolenic acids whereas the surface lipids contained
palmitic and stearic acid as main components.
Vora Kalpit A et al. 1988; have characterized extracellular lipase
produced by Asperigillus japonicus in response to Calotropis gigantea
latex.
Shin Whanchul et al. 1990; have elucidated the structure of 12β –
benzoyloxy - 3β, 8β, 14β, 17β – tetrahydroxy – 5 – pregnen – 20 –
one extracted from the root of Calotropis gigantea.
Kitagawa Isao et al. 1992; have reported the presence of two new
Oxypregnane – oligoglycosides: calotroposide A and calotroposide B.
The structures were established as 12-O-benzoyllineolon-3-O-β-D-
cymaropyranosyl (1 → 4) – β-D-oleandropyranosyl (1 → 4) – β – D –
oleandropyranosyl(1 → 4) – β – D –cymaropyranoside and 12-O-
benzoyldeacetylmetaplexigenin-3-O-β-D-cymaropyranosyl (1 → 4) –
β-D-oleandropyranosyl (1 → 4) – β – D – cymaropyranosyl(1 → 4) –
β – D –cymaropyranoside .

58
Shibuya Hirotaka et al. 1992; have isolated and developed the
chemical structure of calotroposides A and B; five oxypregnane –
oligoglycosides named- calotroposides C(I), D(II), E(III), F(IV), and
G(V) from the root of Calotropis gigantea.
Sen Sucharita et al. 1992; have isolated and characterized
isorhamnetin – 3 – O – rutinoside, isorhamnetin – 3 – O –
glucopyranoside and taraxasteryl acetate along with new flavonol
trisaccharide as isorhamnetin – 3 – O – [2 – O – β – D –
galalactopyranosyl – 6 – O – α – L – rhamnopyranosyl] – β – D –
glycopyranoside (calotropiside) from aerial parts of Calotropis
gigantea.
Julie S et al. 1996; have reported the presence of quercetin and
phenolic acids in leaves, bark and wood, which impart resistance
against fungal pathogen Cuscuta chinensis.
Pari K et al. 1998; have isolated giganticine (I), a novel nonprotein
amino acid from a methanol extract of the root and bark of Calotropis
gigantea and studied antifeedant activity.
NH
OMe
NH
O
MeH
OHO
O

59
Ali M et al. 1998; have isolated urs - 18α – H – 6(7), 12, 20 (30) –
triene - 3α – yl acetate, urs - 18α – H – 12, 20 (30)-diene - 3α – yl
acetate, urs - 18α – H – 12, 20 (30)- diene - 7α – yl acetate and urs -
18β – H – 20 (30)- ene – 12β – yl acetate on the basis of spectral
analysis and chemical reactions.
Ali Mohd et al. 1999; have isolated lupene type triterpene as lup –
13(18), 20(29) – dien - 9α – yl acetate and lupeol acetate; two ursane
type triterpenes as urs - 18β- H – 12, 20(30) – dien - 3β – yl acetate
and 17β – hydroxyl – 28 – norurs - 18α-H – 12, 20 (30) – dien - 3β –
yl acetate on the basis of spectral data analysis and chemical
reactions.
Gupta Jyoti et al. 2000; have isolated chemical constituents from
roots of Calotropis gigantea which comprised of naphthalene
derivative – calotropnaphthalene; two terpenes –
calotropisesquiterpenol and calotropisesterterpenol; and an aromatic
compound – calotropbenzofuranone.
Mathur Akhleswar et al. 2003; have reported the presence of
linoleic acid as fatty acid component of seed of Calotropis gigantea.
Lhinhatrakool Thitima et al. 2006; have isolated two new
cardenolides (1 & 2) along with twelve known compounds from
dichloromethane extract of the leaves of Calotropis gigantea. All
cardenolides tested for anticancer activity due to presence of

60
deoxysugar at C – 3, a formyl group at C – 10, and β – unsaturated γ
– lactone.
Habib M Rowshanul et al. 2007; have isolated stigmasterol and β –
sitosterol from a methanol extract of root and bark of Calotropis
gigantea.
4.2.2 Pharmacological investigation
Hesse Gerhard et al. 1938; have studied about heart poison in
Calotropis gigantea latex used as African arrow poison.
Ganapathy CV et al. 1940; have studied the milk clotting activity of
papain from calotropis gigantea.
Chen KK et al. 1942; have studied digitalis like principles of
Calotropis gigantea and compare their activity with other cardioactive
substances.
Rathnasabapathy V et al. 1953; have studied the cardiovascular
action of gigantin obtained from latex of Calotropis gigantea.
Bose SM et al. 1957; have studied the standardization and
evaluation of different methods for the quantitative estimation of
protease activity.
Rao D Seshagiri et al. 1957; have studied insecticidal properties of
petals of Calotropis gigantea.

61
Dhawan BN et al. 1958; have studied stimulant effect of Calotropis
gigantea milk on the rat uterus.
Krishna W Madhiva et al. 1959; have studied the enzymic unhairing
and degreasing properties of proteolytic enzymes and amylolytic
enzymes used for production of leather.
Shukla OP et al. 1961; have studied bacteriolytic activity of plant
latex.
Deng SH et al. 1962; have studied cardiotonic action and biological
potency of an extract from Calotropis gigantea.
Saha JC et al. 1963; have studied histaminic action of latex of
Calotropis gigantea.
Pant Radha et al. 1966; have studied proteolytic activity of plant
latex.
Kulkarni SD et al. 1976; have studied the effect of Calotropis
gigantea on dog E.C.G.
Muthukrishnan J et al. 1979; have studied antimicrobial activity of
Calotropis gigantea leaf soaked in distil water, caffeine and
theophylline on larvae of Danaus chrysippus.
Williams Lyall R et al. 1981; have studied the potential as fuel and
energy for producing hydrocarbon- producing crops.
Kadam Shivaji Shankerrao et al. 1981; have studied weedicide
activity of Calotropis leaf extract for weed such as parthenium grass.

62
Chary M Pravindra et al. 1983; have studied protease activity of
latex.
Amin AR et al. 1985; have studied microbial transformation of plant
latex.
Pati L S et al. 1993; have reported that milky sap from Calotropis
gigantea is used as a proteolytic enzyme in blood group serology.
Pham Xuan Sinh et al. 1994; have reported antiasthmatic,
antitussive activity due to presence of alkaloids and gylcosides.
Dey Srilekha et al. 1995; have reported the metabolic activity like
catalase peroxidase in the latex of Calotropis gigantea.
Pugalenthi Poomalai et al. 1997; have reported the efficacy of
cardenolides secondary metabolites of Calotropis gigantea as
deterrent for phytosuccivorous, sucking pets Aphis gossypii Glov, and
Tettigoneiella spectra Dist, in bhendi fields.
Kiuchi Fumiyuki et al. 1998; have reported the cytotoxic activity in
three cardenolide glycosides: calotropin, frugoside and 4’ – O - β – D
– glucopyranosyl frugoside obtained from akond mul (roots of
Calotropis gigantea).
Verma Smita A et al. 1998; have reported the effect of acid extracts
of Calotropis gigantea latex on HCl corrosion of mild steel.

63
Pushkerlal M et al. 2002; have reported the application of plant latex
for the treatment of industrial effluents. A significant reduction in
T.D.S. (Total dissolved solid) was reported.
Patil SV et al. 2003; have reported that the juice from Calotropis
gigantea provides a cheap, readily available alternative to the rennet
of animal and microbial origin as it posses milk coagulating activity.
Rawat Puran Singh et al. 2003; have reported the use of Calotropis
root and bark in the treatment of leukoderma.
Desouza Anita Mary et al. 2004; have reported the production of
dehaired skins and hides in extracts of Calotropis gigantea.
Kim Hang Rim et al. 2004; have reported P – glycoprotein inhibitory
activity of chloroform extract of Calotropis gigantea in human breast
cancer cells. The activity is comparable to anticancer agent
Daunomycin and Varapamil.
Chitme Havagiray R et al. 2004; have reported antidiarrhoeal
activity in plant extract of Calotropis gigantea in experimental
animals. The roots of Calotropis gigantea have been used for
treatment of leprosy, eczema, syphilis, elephantiasis, ulcer and
cough.
Chitme HR et al. 2005; have reported antipyretic activity of
Calotropis gigantea roots in experimental animals.

64
Rajesh R et al. 2005; have studied that Calotropis gigantea latex
posses procoagulant activity similar to fibrinolytic activity.
Eapen Susan et al. 2006; have reported the potential of Calotropis
gigantea to remove radionuclide/toxic substances like Sr – 90, Cs –
137, from soil and solutions.
Adak Manoranjan et al. 2006; have reported anti inflammatory
activity of Calotropis gigantea.
Argal Ameeta et al. 2006; have reported that alcoholic extract of
peeled roots of Calotropis gigantea posses the CNS activity in albino
rats. The results showed analgesic activity, anticonvulsant activity,
anxiolytic and sedative activity.
Pathak AK et al. 2007; have reported analgesic activity of alcoholic
extract of flowers of Calotropis gigantea.
Srivastava Shobha Rani et al. 2007; have evaluated that extract of
the roots of Calotropis gigantea posses the pregnancy interceptive
activity of the colony-bred adult Sprague – Dawley rats.
Shilpkar Prateek et al. 2007; have reported the use of Calotropis
gigantea in biomethanation.
Jacob Zacharia (India) 2007; has developed a method of
preparation of potential herbal anti – cancer medicine from fresh
extracts of leaves and twigs of Calotropis gigantea fortified with

65
unrefined sugarcane sugar (Jaggery), which was proved for
prevention and treatment of all types of cancer.
Rajesh Rajaiah et al. 2007; have reported clot inducing effect of
plant latex protease, which was proved to stop bleeding and had
wound healing properties.
Arulprakash R et al. 2007; have studied biochemical changes in the
tissues of Callosobruchus maculatus, Sitophilus oryzae, Tribolium
castaneum adult on treatment with Calotropis gigantea plant parts
extracts.
Siddiqui Mohammad Khalid et al. 2008; have prepared a herbal
preparation containing Gul – e – Madar (Calotropis gigantea) which
was effective against cholera and gastroenteritis.
Nair Kesavapanicker Sasikumaran et al. 2008; have prepared
natural pesticides from crushed leaves, flowers, fruits and tender
stems of Calotropis gigantea.
Oman Medical Journal 2011; has reported hypoglycemic effect in
chloroform extract of leaves of Calotropis gigantea in streptozotocin
induced diabetic rats.

66
5. EXPERIMENTS

67
5. EXPERIMENTS
5.1 Collection and authentication of plant material
Calotropis gigantea was collected from the forest area of
Ghaziabad, U.P., India and Sphaeranthus indicus was obtained from
the market of Ghaziabad, U.P and both plants were identified from
the School of Pharmacy, Vishveshwariya Institute of Medical Science,
Greater Noida, Gautam Budha, Nagar, UP India. They were assigned
voucher specimen Ref. VIMS/CONSULT/2009/02/10 and Ref.
VIMS/CONSULT/2009/02/11.
5.2 Physical-chemical evaluation
Evaluation of ash values helps in the detection of low grade
products, exhausted drugs and sandy or earthy material. Water
soluble ash and acid insoluble ash helps in detection of chemical
constituents.
About 3 gm of air dried powder of the parts of the plants
Calotropis gigantea and Sphaeranthus indicus were accurately
weighed in a tared silica crucible. They were incinerated at a
temperature below 450ºC until all carbon content was lost. The
material was cooled and weighed. The percentage of total ash was
calculated with reference to the air dried powdered drug.

68
25 ml of dilute hydrochloric acid was added to the acid insoluble
ash obtained from above method and boiled for 5 minutes. The
material was filtered through ashless filter paper. Washing was done
with hot water followed by ignition and then accurately weighed. The
percentage of acid insoluble ash with reference to the air dried
powdered drug was calculated.
25 ml of water was added to the water soluble ash obtained in
total ash and boiled for 5 minutes. Filtration was done through
ashless filter paper.The filtrate was washed with hot water followed
by ignition and then accurately weighed. The weight of water soluble
ash was calculated by subtracting the weight of insoluble matter from
the weight of the total ash. The percentage of water-soluble ash was
calculated with reference to the air-dried powdered drug.
The percentage of sulphated ash was calculated by moistening
3 gm of air dried powder of the parts of plants Calotropis gigantea
and Sphaeranthus indicus with sulphuric acid. The matter was ignited
at low temperature to constant weight and the percentage was
calculated with reference to the air dried powdered drug.

69
The percentage of alcohol soluble extract was calculated by
macerating 5 gm of air dried powder of the parts of the plants
Calotropis gigantea and Sphaeranthus indicus with 100 ml of alcohol
in a closed flask for 24 hours.It was shaked frequently for 6 hours and
allowed to stand for 18 hours.Filtration was done with a precaution
against loss of alcohol and 25 ml of the filtrate was evaporated in a
tared flat bottomed shallow dish and dried at 1050C to constant
weight and then accurately weighed. The percentage was calculated
with reference to the air dried powdered drug.
The percentage of water-soluble extract was calculated by
macerating 5 gm of air dried powder of the part of the plants
Calotropis gigantea and Sphaeranthus indicus with 100 ml of
chloroform water in a closed flask for 24 hours. It was shaked for 6
hours and allowed to stand for 18 hours. Filtration was done and 25
ml of the filtrate was evaporated in a tared flat bottomed shallow dish
and dried at 1050C to constant weight and then accurately weighed.
The percentage with reference to air dried powdered drug was
calculated (Khandelwal, 2004).

70
5.3 Method of extraction
Powdered plant material was evenly packed in soxhlet
apparatus and extracted with organic solvent from polar to non polar
solvent separately. The aqueous extraction was carried out by cold
maceration process separately. The extraction was carried out with
various solvents, except water, by hot continous extraction for about
20 hours. The solvents used were purified before use. After each
solvent extraction, the extract was separated and concentrated by
vaccum distillation to reduce the volume to 1/10. The concentrated
extracts were transfered to 100 ml beaker and the remaining solvents
were evaporated on water bath. The dried extracts were collected
and placed in a desiccator to remove excessive moisture. The dried
extracts were packed in separate air tight containers, labelled and
used for further studies such as phytochemical screening and
pharmacological activities as well as their formulations.
5.4 Identification of phytochemical constituents
Alkaloids were tested by Mayer’s test, Dragendroff’s test,
Hager’s test and Wagner’s test. Carbohydrates and glycosides were
tested by Molisch’s test, Fehling’s test, Legal’s test, Borntrager’s test
and Anthrone test. Fixed oils and fats were tested by Spot test and

71
Saponification test. Proteins and free amino acids were tested by
Million’s test, Ninhydrin test and Biuret test. Phenolic compounds and
tannins were tested by Test for phytosterol, Salkowski test,
Liebermann- Burchard’s test, Test for gums and mucilage, Test for
flavonoids and Shinoda’s Test (Kokate, 1990).
5.5 Total phenol and flavonoid contents
Total phenolic contents in the extracts were determined by using
the Folin Ciocalteu method (Mc Donald et al., 2001). A dilute solution
of each plant extract of Calotropis gigantea and Sphaeranthus indicus
(0.5 ml of 1:10 g ml-1) and gallic acids were mixed with 5 ml of Folin
Ciocalteu reagent and diluted with distilled water in a ratio of 1: 10
(Slinkard and Singleton, 1977), 4 ml of aqueous sodium carbonate
(1M) was added and allowed to stand for 15 minutes. The total
phenollic contents were determined by UV-VIS spectrophotometeric
method by measuring absorbtion at 765 nm (Pharmaspec 1700,
Shimadzu). Total phenolic content was expressed in terms of gallic
acid equivalent using the following equation based on the calibration
curve:
y = 0.045 x R2 = 0.960

72
Where x was the absorbance and y was gallic acid equivalent
(mg/g).
Flavonoid contents of various extracts were determined by
aluminium chloride colorimetric method (Chang et al., 2002). Each
plant extract of Calotropis gigantea and Sphaeranthus indicus (0.5 ml
of 1:10 g ml-1) in methanol were separately added to 1.5 ml of
potassium acetate (1M) and 2.8 ml of distilled water was added. This
was allowed to stand at room temperature for 30 minutes. The
flavonoid contents were estimated by measuring the absorbance of
mixture at 415 nm with UV-VIS spectrophotometer (Pharmaspec
1700, Shimadzu). Total flavonoid contents were evaluated in terms of
catechin equivalent using the following equation based on the
calibration curve:
y = 0.05 x R2 = 0.992
Where x was the absorbance and y was catechin equivalent (mg/g).
5.6 Drugs and chemicals used
Alloxan monohydrate was purchased from Sigma chemical;
streptozotocin (STZ) was purchased from Sigma Aldrich chemical
Co., Bangalore; citrate buffer (pH 4.5), glibenclamide and metformin
were procured from Aventis Pharma, Mumbai, India.

73
5.7 Antidiabetic activity of extracts of Calotropis gigantea
5.7.1 Hypoglycemic activity of extracts of Calotropis gigantea on
blood glucose level in normal wistar rats (Single dose)
All animals used in this study were kept and maintained at
laboratory conditions of temperature, humidity and 12 hour day- night
cycles and were allowed free access to food (Standard pellet diet)
and water ad libitum. After a period of 4 days acclimatization, the
animals were kept fasting for 16 hours (allowed free access to water
throughout the fasting period). At the end of a period of 16 hour
fasting, blood glucose levels of the fasted normoglycemic rats at zero
time (i.e. 0 hour) were measured and recorded (Akbarzadeh et al.,
2007).
Group I: Received vehicle (normal control).
Group II, III and IV: Received 250 mg/kg BW (body weight) of
petroleum ether, methanolic and aqueous extracts of leaves of
Calotropis gigantea, respectively.
Group V, VI and VII: Received 250 mg/kg BW of petroleum
ether, methanolic and aqueous extracts of roots of Calotropis
gigantea, respectively.

74
All the rats were maintained with standard pellet diet and water
ad libitum. The blood glucose levels of all the rats were
measured at 0, 1, 4, 8 and 12 hour and analyzed statistically.
5.7.2 Streptozotocin induced diabetes
Streptozotocin (STZ) was dissolved in 0.9% ice-cold saline
immediately before use. Diabetes was induced in rats by intra
peritoneal (i.p.) injection of streptozotocin at a dose of 60 mg/kg BW.
Forty eight hours after STZ administration, blood samples were
drawn from tail and glucose levels were determined to confirm the
onset of diabetes. During this period, the rats had free access to both
food and water. The diabetic rats, exhibiting blood glucose levels,
higher than 200 mg/dl, were selected for the studies. The dose of
standard drug glibenclamide was 600µg/kg BW. Animals were
divided into different groups, each group had six rats.
Streptozotocin (STZ) is a broad spectrum anti-biotic isolated
from Streptomyces archromogenes in 1959 (Her, 1959-1960). Earlier
this compound was reported to have anti-cancer activity (Evans,
1965; Arison, 1967) and its diabetic property was first reported by
Rakieten and co-workers. Chemically, STZ is 1-methyl-1-nitrosourea
linked to a position of second carbon atom of D-glucose. It is freely

75
soluble in water, unstable at room temperature and has to be stored
below 200C. Its stability is optimum at pH 4 and at low temperatures.
The biological half life was found to be 5 minutes in rats. STZ induces
diabetes in almost all the species. The elevated blood glucose level
was observed within 48 to 72 hours (Peak effect) and was maintained
thereafter. Rats treated with STZ showed many of the features seen
in human subjects with uncontrolled diabetes mellitus including
hyperglycemia, polydipsia and weight loss.
5.7.3 Effect of extracts of Calotropis gigantea on oral glucose
tolerance test
The oral glucose tolerance test (OGTT) was performed by
feeding glucose solution (0.25 g/kg BW) orally to all the groups and
blood samples were collected at 0, 30, 60, 120 minutes after the
administration of glucose. The oral glucose tolerance test was
performed according to the method of Du Vigneaud (1925). The
mean blood glucose concentrations of control, standard drug and
extract-treated animals at various time intervals were evaluated to
determine whether there were statistically significant differences in
hypoglycemia achieved by different doses of the test extracts.

76
OGTT was carried out to screen the hypoglycemic activity of
petroleum ether, methanolic and aqueous extracts of Calotropis
gigantea on laboratory animals with orally loaded glucose. Overnight
fasted wistar rats weighing between 180-200 g were divided into
different groups; each group consisted of six animals.
Group I: Received vehicle (normal control).
Group II: Diabetic control.
Group III: Received glibenclamide 600 µg/kg.
Group IV, V and VI: Received 250 mg/kg BW of petroleum
ether, methanolic and aqueous extracts of leaves of Calotropis
gigantean, respectively.
Group VII, VIII and IX: Received 250 mg/kg BW of petroleum
ether, methanolic and aqueous extracts of roots of Calotropis
gigantean, respectively.
After the administration of the standard and test extracts, from all
the groups, blood samples were collected at 0, 30, 60 and 120
minutes after the glucose loading and blood glucose levels were
determined.

77
5.7.4 Anti-hyperglycemic activity of extracts of Calotropis
gigantea on STZ induced diabetic rats (multiple doses)
Group I: Received vehicle (normal control).
Group II: Diabetic control.
Group III: Received glibenclamide 600 µg/kg BW.
Group IV, V and VI: Received 250 mg/kg BW of petroleum ether,
methanolic and aqueous extracts of leaves of Calotropis
gigantea, respectively.
Group VII, VIII and IX: Received 250 mg/kg BW of petroleum
ether, methanolic and aqueous extracts of roots of Calotropis
gigantea, respectively.
Drug samples were given every day upto 15 days and blood
samples were collected from the tail, for glucose estimation just
before drug administration on 1st day (commencement of the
experiment) and 1 hour after drug administration on day 1, 5, 10 and
15.
5.8 Antihyperlipidemic activity of extracts of Calotropis gigantea
Rats of all groups were anaesthetized by ether and the blood
samples of each were taken from rat tail tip in 2ml eppendorf tubes
containing anticoagulant. Serum was separated by centrifugation at

78
2500-3000 rpm at 250C for 15 minutes and analyzed for assorted
biochemical parameters.
5.8.1 Estimation of cholesterol
About 10 µl plasma and 1 ml of glucose diagnostic kit reagents
(Spineract) were mixed and incubated for 10 minutes at 20-250 C and
the cholesterol values were determined at 546 nm using
autoanalyzer.
5.8.2 Estimation of triglycerides
About 10 µl plasma and 1 ml triglycerides diagnostic kit
reagent (Spineract) were mixed and incubated for 10 minutes at 20-
250C. The triglyceride values were observed using autoanalyzer at
546 nm.
5.8.3 Estimation of very low density lipoprotein (VLDL)
The very low density lipoproteins were determined by using
Friedwald formula:
VLDL cholesterol = Triglycerides/5.

79
5.8.4 Estimation of high density lipoprotein (HDL)
About 500 µl plasma and 0.05 ml precipitation reagent
(Spineract) were mixed well and allowed to stand for 10 minutes at
room temperature. 1 ml of cholesterol diagnostic kit reagent
(Spineract) was mixed and incubated at 370 C for 5 minutes or at
room temperature for 10 minutes. The HDL values were observed in
autoanalyzer at 546 nm.
5.8.5 Estimation of low density lipoprotein (LDL)
The LDL was calculated using Friedewald formula:
LDL = Total cholesterol – (HDL + Triglycerides/5)
5.8.6 Estimation of:
Glycosylated haemoglobin (HbA1c) % by Spinreact kit
Albumin (g/L)
Total protein (g/L)
Creatinine (mg/dl)
Body weight (g)
Kidney weight(g)
Haemoglobin (g %)
Urine sugar and albumin

80
5.9 Hypoglycemic effect of Calotropis gigantea leaves via
different routes of administration in normal and alloxan induced
diabetic rats
5.9.1 Preparation of water extract
The leaves of Calotropis gigantea were air dried and powdered
in a grinder. 300g of powdered mixture of the plant part was extracted
overnight with 360 ml of water with magnetic stirring in cold room
(4oC). The water extract was separated and the residue was re-
extracted with water. The water extract was concentrated to produce
semisolid mass and dried in lyophilizer (Mini Lyotrap, Serial No
J8199/5, LET Scientific Ltd UK).
5.9.2 Animal and experimental set-up
Colony bred, healthy wistar albino rats either male or female
with a body weight of 150 to 200 gm were selected for the
experimental work. The animals were kept at room temperature and
fed on standard laboratory diet with water ad libitum. The rats were
kept on fast during the night and all the rats were allowed a free
access to water during the experiment in the ambience. The animals
were divided into eight groups of six animals each. 1 ml of blood
sample was taken by capillary tube for the evaluation of blood

81
glucose level from the orbital sinus of each rat. The Institutional
Ethical Committee had approved all experiment protocols.
5.9.3 Hypoglycemic effect in normal rats
Groups of six rats each (fasted for 18 hours) received 10 ml/kg
BW infusions, intragastrically and intraperitoneally (i.p.) Blood
samples were drawn from the tail immediately before administration
in the time intervals of 20, 60, 120, 240 and 360 minutes later.
Control group received an equal volume (10 ml/kg BW) of normal
saline, glibenclamide (0.13 mg/kg BW) and metformin (11.3 mg/kg
BW), calculated on the basis of the daily doses.
5.9.4 Hypoglycemic effect on alloxan-diabetic rats
Chronically hyperglycemic rats were obtained by i.p. injection of
150 mg/kg BW of alloxan dissolved in distilled water. After 8 hours of
administration, the hyperglycemic rats were selected (plasma glucose
level 2-2.8 g/L) and used in the experiments. The same experimental
protocol described above was then adopted.
5.9.5 Glucose tolerance test (GTT) in glucose loaded rats
A polyethylene cannula was injected into the jugular vein under
ethyl carbonate anesthesia. Another catheter was injected into right

82
carotid. All rats received orally 10 ml/kg BW of 25% glucose solution.
One group of animals received the plant infusion (10 ml/kg BW)
through the venous catheter, while the control group received normal
saline. Blood samples (0.2 ml) were taken from the carotid catheter at
time intervals of 5, 10, 20, 30, 40, 50 and 60 minutes after injection.
The coefficient of glucose assimilation (KG) was determined with the
formula:
KG = (log C - log C/2) t½= 0.639 t½
Where, C = glycaemia (g/L); t½ = time for the blood glucose
concentration equal to C/.2.
5.9.6 Statistical analysis
Results were reported as mean ± SEM. Statistical analysis was
carried out using analysis of variance (Anova). The difference of the
means was calculated using Newman – Keuls test. P values of 0.05
or less were taken as significant.

83
5.10 Effect of Calotropis gigantea and Sphaeranthus indicus on
glycemia and lipidemia in streptozotocin induced diabetic rats
5.10.1 Preparation of water extract
300 gm of powdered mixture of the parts of two plant Calotropis
gigantea and Sphaeranthus indicus was extracted overnight with 360
ml of water with magnetic stirring in cold room (4oC). The water
extract was separated and the residue was re-extracted with water.
The combined water extract was concentrated in lyophilizer.
5.10.2 Animals
Wistar albino rats were obtained from R.V. Northland Institute,
Greater Noida, Gautam Budha, Nagar, U.P., India and clearance was
taken from Institutional Animal Ethics Committee (IAEC). Adult rats of
either sex weighing between 150-200 gm were selected for the study.
The animals were acclimatized to laboratory conditions and divided
into various groups. Animals were housed and kept on the light and
dark cycle throughout.
5.10.3 Induction of diabetes and associated neuropathy
Healthy adult wistar albino rats of both sex weighing between
150-200 gm were obtained from the R.V. Northland Institute, Greater

84
Noida, Gautam Budha, Nagar, U.P., India, and used in this study.
The animals were fed on a pellet diet (Hindustan Lever, India) and
water provided ad libitum. Diabetes was experimentally induced to
produce diabetic neuropathy. Sorbitol induced dysfunction of inositol /
metabolites leading to neuron-infraction by causing microangiopathy
of vasa nervosum. It decreases blood flow to nerves. Overnight
fasting animals were injected with streptozotocin (STZ) 60 mg/kg BW
dissolved in 3 mM citrate buffer (pH 4.5) intraperitoneally (i. p.). After
10 days only those rats which showed plasma glucose level > 300
mg/dl were classified as diabetic and were included in study as
described earlier. Animals were divided into three groups of five rats
each. Group 1 animals served as healthy control, while those of the
group 2 were untreated diabetic rats. Rats of group 3 were diabetic
and treated for 8 weeks with 300 mg/kg BW of water extract of
mixture of Calotropis gigantea leaves and Sphaeranthus indicus.
Blood samples were collected from overnight fasted rats at 0 and 8
weeks. Blood glucose serum total cholesterol, HDL and LDL
cholesterol, triglyceride, and glycosylated haemoglobin were
determined using kits from SPINREACT Crta, Sta. Coloma 7-E-
17176 Esteve den Bas GIRONA-Spain (supplied by ARK Diagnostic
Private Limited). Total proteins albumin and creatinine in serum were
determined by the method of Reinhold. Assay of plasma glucose,

85
albumin, creatinine, total cholesterol, LDL, VLDL, HDL cholesterol
and triglycerides were estimated as described earlier. Lipid
peroxidation products were estimated as thiobarbituric acid reactive
substance (TBARS) in plasma and tissues.
5.10.4 Statistical analysis
All the data were statistically evaluated and the significance was
calculated using student’s test. All the results were expressed as
mean ± SD.
5.11 Antioxidant activity of extracts of Calotropis gigantea
Antioxidant potential of the ethanolic extract was determined on
the basis of their scavenging activity of the stable 1, 1- diphenyl-2-
picryl hydrazyl free radical.IUPAC name of DPPH is di(phenyl)-2,4,6-
trinitrophenyl)iminoazanium. DPPH method is most widely used and
easiest method to determine antioxidant activity. In the structure of
DPPH an odd electron is present and is commonally used to
determine free radical scavenging activity.
The aliquots of the different concentrations (1-500 μg/ml) of the
extract were added to 3 ml of a 0.004% w/v solution of DPPH.
Absorbance at 517 nm was determined after 30 minutes, and IC50
(Inhibitory concentration 50%) was determined. IC50 value denotes

86
the concentration of sample required to scavenge 50% of the DPPH
free radicals. At first 6 test tubes were taken to make aliquots of 6
concentrations: 1, 5, 10, 50, 100 and 500 μg/ml. Plant extract and
ascorbic acid were weighed accurately and dissolved in ethanol to
make the required concentration by dilution technique. Here ascorbic
acid was taken as standard. DPPH was weighed and dissolved in
ethanol to make 0.004% w/v solution. To dissolve homogeneously
magnetic stirrer was used. After making the desired concentration, 4
ml of 0.004% w/v DPPH solution was applied on each test tube by
pipette. The room temperature was recorded and kept the test tubes
for 30 minutes in light to complete the reactions. DPPH was also
applied to the blank test tube at the same time where only ethanol
was taken as a blank. After 30 minutes, absorbance of each test tube
was determined by UV spectrophotometer. IC50 was determined
from percentage inhibition vs. concentration graph.
5.12 Antimicrobial activity of extracts of Calotropis gigantea
5.12.1 Preparation of plant material
Plant leaves were collected and washed properly with distilled
water. The leaves were air dried under shade at room temperature.

87
Dried leaves were grinded in the mechanical grinder.The powdered
material was extracted with distilled water.
Ten gram of powdered material was soaked in 100 ml of
distilled water in a conical flask and loaded on an orbit shaker at a
speed of 120 rpm for 24 hours. The mixture was filtered using
Whatman filter paper number 1. Rotary evaporator was used to
concentrate the filtrate and dried by using lyophilizer. Dried extract
was kept in an air tight closed container and stored in cold room at
4°C. The extracted powder was dissolved in sterilized distilled water
to make 1000 μg/ml solution. This mixture was used to perform
antibacterial assay.
5.12.2 Test Microorganism
The following six clinical isolates of bacteria were used for the
study: S. aureus, K.pneumoniae, B. cereus, P. aeruginosa, M. luteus
and E. coli. All these cultures were maintained on nutrient agar plates
at 4°C.
5.12.3 Disc diffusion method
The extract of Calotropis gigantea leaves was obtained by
maceration process by using water as a solvent. Extracts were
screened for antimicrobial activity using disc diffusion method. A
suspension of organism was added to sufficient quantity of nutrient

88
agar at 45ºC. The mixture was aseptically transferred to sterile petri
dish and allowed to solidify. The overnight culture grown in broth was
used for inoculation. The plant extracts to be tested were prepared in
various concentrations i.e. 25%, 50%, 75% and 100%. The sterile
impregnated discs with plant extracts were placed on the agar
surface with framed forceps and gently pressed down to ensure
complete contact of the disc with agar and dextrose surfaces.
Positive control discs were also prepared in the same manner using
ampicillin, a bactericide. But it was not used for fungi. The prepared
control discs were placed using respective solvents.
All the plates including control plates were incubated at 37°C
for 24 hours. After incubation, the size (diameter) of the inhibition
zones was measured. Triplicates were maintained for each sample of
the extract respectively. The results were expressed in terms of the
diameter of the inhibition zone: <9 mm - inactive; 9-12mm - partially
active; 13-18mm - active; >18mm - very active. After the confirmation
of antibacterial activity with 100 mg/kg BW dose, the experiment was
carried out in triplicate and average values were taken into
consideration. Similar procedure was carried out with standard drug
ampicillin 100mg/ml and the zone of inhibition was compared with

89
test sample and control and the percentage of inhibition was
calculated.
5.12.4 Pharmacokinetic parameter of antimicrobial acitivity
Minimum bactericidal concentration
The Minimum bactericidal concentration (MBC) is the least
antibiotic concentration that is used to destroy any bacteria. MBC can
be evaluated by broth dilution Minimum Inhibitory Concentration test.
The test is performed by subculturing to agar medium in which test
organism is not present. MBC is a dose which decreases the original
microorganism concentration by more than 99%.
Minimum inhibitory concentration
The least concentration of antimicrobial agent which prevents
the growth of microbes during an incubation period of 24 hours is
referred to as Minimum Inhibitory Concentration (MIC). MIC is a
significant tool to find out the dose of an antimicrobial agent required
to inhibit the growth of a microorganism and to study the resistance
shown by a microorganism towards an antimicrobial agent. So MIC
has become an important parameter to evaluate antimicrobial activity
in laboratory. MIC testing helps in evaluating MIC50 which represent
the dose of an antimicrobial agent effective in destroying the 50% of

90
the population of bacterial isolate and MIC90 which represent the
dose of an antimicrobial agent effective in destroying 90% of the
population of the bacterial isolate in a bacterium inoculum.
Calculation of relative percentage inhibition
The relative percentage inhibition of the test extract with
respect to positive control was calculated by using the following
formula:
Relative percentage inhibition of the test extract
=
Where, X: total area of inhibition of the test extract
Y: total area of inhibition of the solvent
Z: total area of inhibition of the standard drug
The total area of the inhibition was calculated by using
Area = πr2; where, r = radius of zone of inhibition

91
5.13 Effect of extract of Calotropis gigantea on the skeletal
muscle of the rat
Since the antimigraine drugs were reported to have muscle
relaxant activity, so this experiment was attempted to assess the
effect of extract of Calotropis gigantea on the rat rectus abdominis
muscle preparation. The experiment was carried out as per the
method described by Kulkarni. Rats weighing 20‐25 g were used in
this study. The rat was stunned and decapitated and the spinal cord
was destroyed. The skin of the anterior and abdominal wall of pithed
rat was cut by a midline incision and then it was cut laterally to
expose the anterior abdominal wall. The rectus was seen running
from the base of sternum. The muscles above the sternum and a pair
of muscles attached to it were dissected and kept in a dish containing
ringer solution at room temperature. The muscles were then carefully
cleaned and one muscle of apropriate size was mounted to an organ
bath containing ringer solution and aerated by stream of fine bubbles
emerging near the bottom of the bath.Gimble lever with sideways
writing point adjusted to provide a tension of 2-5 gm was used to
record isotonic contractions of the muscles. An extra load of arround
1 g was applied on long arm so that lever may return back to its
original position after washing. The drug period allowed for
stabilization was 30 minutes during which the muscle was subjected

92
to 1 g stretch. The kymograph was started at 0 minute after raising
the extra load. The drug was added in the 1st minute. The kymograph
was stopped in the 2nd minute. The tissue was washed and relaxed
by applying an extra load. At the 5th minute, the lever point was
brought to the base line and the next cycle was started. The graded
responses to different log doses of acetylcholine were recorded. Then
the test drug (extract) was added and their effects upon acetylcholine
induced contractions as well as the effect of its own on the tissue was
studied.

93
6. RESULTS AND DISCUSSION

94
6. RESULTS AND DISCUSSION
6.1 Macroscopic and microscopic features 6.1.1 Calotropis gigantea Macroscopy Leaves
Simple, opposite, sub-sessile, thick, 10-15 cm long and 4.5-6.5
cm broad; tender leaf: covered with ashy grey hairs; mature leaf:
smooth.
Roots
The root occurs in the entire condition bearing root hairs; 0.5-2
cm in diameter; bark 0.2-0.5 cm thick; whitish grey in colour; wrinkled
in stress condition; with latex excuding from the cuts and wounds of
the bark; facture is tough; taste and odour is characteristic.
Microscopy of Calotropis gigantea leaves
T.S. of leaves shows an upper epidermis with elliptical or oval
shaped cells followed by three layers of closely packed palisade cells
filled with chloroplast; the palisade cells are 11.4-19.0 µ X 13.2-14.2µ
in T.S. palisade layers are parenchymatous which have large intense
cellular space. The cells are thin walled and measure 19.0-54.6µ X
15.2- 40.8µ; Vascular bundles are distributed throughout the spongy
paranchymatous region. The vessels show angular and spiral

95
thickening. The lower epidermal cells are more or less of the same
size and shape as the upper epidermal cell. Stomatas are of
rubiaceous (paracytic) type and scattered in the lower epidermis.
Multicellular thin walled trichomes are found, distributed throughout
the leaf. The T.S. of petiole shows bicollateral bundles besides the
thin walled parenchymatous cells.
Microscopy of Calotropis gigantea root
The T.S. of mature root shows multilayered cork, composed of
rectangular and tangentially elongated cell. Phelloderm is narrow
zone of thin walled parenchymatous cells, most of them filled with
starch grains; lactiferous ducts are also present in the region.
Phloem is very broad zone consisting of sieve tubes, companion
cells and thin walled parenchyma; being transversed by 2-4 layer of
thin walled medullary ray cells; some of them showing calcium-
oxalate crystals and a few starch grains; laticiferous dust is also
present in phloem region; wood is composed of thick walled and
lignified vessels, tracheids, fiber, being transversed by 2-4 layers of
thick walled radially elongated medullary rays.

96
Powder microscopy of Calotropis gigantea leaves
(a)Sclerenchyma cells (b) Stomata
(c) Fiber (d) Fiber
(e) Calcium crystals (f) Vessels

97
(g) Sclerides (h) Epidermal cells
(i)Unicellular trichome
Figure 3: Powder microscopy of Calotropis gigantea leaves

98
(a)Stomata of apex: (b) Stomata of midrib:
Stomata Epidermal cells (c) Stomata of basal:
Figure 4: T.S. of leaf surface for quantitative analysis of Calotropis gigantea (stomata)
Prismatic like Ca oxalate crystal

99
Vein islet number and vein termination number
(a) Veination of apex: (b) Veination of midrib:
Vein termination Vein islet
(c) Veination of basal:
Secondary Veins Figure 5: T.S. of leaf surface for quantitative analysis of Calotropis gigantea (Vein islet number and vein termination number)
Primary Veins

100
Table 1: Stomatal number of upper surface of Calotropis gigantea (leaves)
Observation Apex Midrib Basal
Lowest range 5.3 3.0 3.3
Average range 6.3 6.7 6.5
Highest range 7.5 9.7 9.7 Table 2: Stomatal number of lower surface of Calotropis gigantea (leaves)
Observation Apex Midrib Basal
Lowest range 5.6 4.4 2.8
Average range 6.3 8.2 6.7
Highest range 7.0 12.8 9.8
Table 3: Vein islet number of Calotropis gigantea (leaves) per sq. mm
Observation Apex Midrib Basal
Lowest range 15 12 10
Average range 22.3 13.3 12.7
Highest range 27 15
17.0

101
Table 4: Veinlet termination number of Calotropis gigantea (leaves)
Observation Apex Midrib Basal
Lowest range 16 16 10
Average range 22.3 20.3 13.7
Highest range
27 25 17
Table 5: Palisade ratio of Calotropis gigantea (leaves)
Observation Apex Midrib Basal
Lowest range 1 2 1
Average range 2.5 3.2 2.6
Highest range
4 6 4

102
6.1.2 Sphaeranthus indicus
Macroscopy
A highly branched, strongly-scented annual weed with winged
stem. Leaf: obovate-oblong, narrowed at the base, dentate and
serrate. Flower: compound heads, globose ovoid, glandular hairy,
achene staled; flowering time is November to January.
Microscopy
Figure 6: Powder microscopy of Sphaeranthus indicus stem
Cork in surface view (Polygonal cells)
Stone cell Cells with brownish content
Prismatic crystals of calcium oxalate

103
Fiber
Figure 7: Microscopy of Sphaeranthus indicus stem Epidermis single layered, covered with thick cuticle; cortex
consisting of 4 to 6 layers of oval to polygonal, thin-walled,
parenchymatous cells; endodermis single layer of barrel-shaped
cells; pericyclic fibers, lignified arranged in discontinuous ring;
secondary phloem narrow, having usual elements; groups of
cellulosic fibers found scattered in this zone; secondary xylem
composed of usual elements; vessels with spiral thickening or simple
pitted; pith very wide composed of oval to polygonal, thin-walled,
parenchymatous cells
Stone cell Cells with brownish content
Calcium oxalate
Phloem
Cork

104
Upper epidermis devoid of stomata
Figure 8: Powder microscopy of leaf of Sphaeranthus indicus
Powder microscopy of leaf of Sphaeranthus indicus contains
lower epidermis with stomata and upper epidermis is devoid of
stomata. Cluster crystals also observed.
Lower epidermis containing stomata
Crystal
Cluster crystal

105
Midrib Lamina
Figure 9: Microscopy of Sphaeranthus indicus leaf
Midrib : Shows a single layered epidermis, covered with ordinary
trichomes upto five cells high and glandular trichomes having
unicellular stalk and group of 4 – 10 cells head, on both surfaces,
followed in turn by 4 – 6 layered collenchymatous and 3 – 4 layers
parenchymatous cells at both surfaces; vascular bundles 3- 4,
situated centrally having usual elements, xylem vessels arranged
radially.
Lamina : Shows a single layered epidermis having numerous
trichomes similar to those of midrib on both surfaces; mesophyll not
differentiated into palisade and spongy parenchyma cells; stomata
anisocytic present on both surfaces, stomatal index 32- 38 on lower
and upper surface, vein islet number 20 – 26.

106
Figure 10: Microscopy of Sphaeranthus indicus root
Epidermis single layered, rectangular; secondary cortex
composed of oval to tangentially elongated, thin-walled,
parenchymatous cells having aerenchyma; secondary phloem
composed of thin-walled, oval to polygonal cells, a large number of
groups of lignified phloem fibers found scattered in this zone; central
portion occupied by lignified, secondary xylem having usual
elements; vessels simple pitted; starch grains simple, round to oval
with concentric striations and distinct hilum, measuring 13 to 27 µ in
diameter, present in secondary cortex.
MEDULLARY RAY PERICYCLIC FIBER
METADERMAL
XYLEM
CORTEX

107
6.2 Physiochemical evaluation
Fresh plant material of Calotropis gigantea and Sphaeranthus
indicus was collected and subjected to various physiochemical
parameters such as moisture content and foreign material were
observed and recorded.
Ash values are helpful in determining the quality and purity of
crude drug, especially in the powdered form. Total ash reflects the
care taken in its preparation as all traces of organic matters were
removed during ash formation and usually consists of carbonates,
phosphates and silicates of sodium, potassium, calcium and
magnesium. A higher limit of acid insoluble ash reflects the cases
where silica may be present or when the calcium oxalate content of
the drug is very high. The total percentage of ash values, acid
insoluble ash, water soluble ash and percentage yield of extracts in
different solvents are constant features of a part of the plant which
may constitute individual drug. These reports would be of much
significance in finding out the genuineness of the drug sample.
Medicinal plants are valuable natural sources and regarded as
potential and safe drugs. They have been playing an important role
as natural drugs to alleviate human suffering by contributing herbal
medicines to the primary health care systems of rural and remote

108
areas, where more than 70 % of population in India depend on
folklore and traditional systems of medicines.
The powdered parts of Calotropis gigantea and
Sphaeranthus indicus in different solutions shows different
fluorescence which are tabulated below:

109
Table 6: Physicochemical parameters of Calotropis gigantea
Parameters (w/w %)
Values in percentage
Leaf Root
Moisture content 0.40 1.20
Foreign matters 1.95 2.15
Total ash 9.50 1.00
Acid insoluble ash 3.00 2.30
Water soluble ash 4.80 5.70
Sulphated ash 5.40 5.60
Pet. ether extract 5.70 4.87
Benzene extract 2.52 5.64
Chloroform extract 3.69 5.58
Ethyl acetate 2.73 5.49
Ethanol extract 1.00 8.13
Aqueous extract 1.95 8.67

110
Table 7: Fluorescent analysis of leaves of Calotropis gigantea
Powder drug Observation
Day Light UV (254 nm) UV (366 nm)
Dry powder as
such Reddish brown No change No change
H2SO4 Dark Reddish brown Grayish green
H2SO4 + water Black Brownish black Black
HCl Light yellowish
green Dark green Light green
HCl + water Faint green Light green Violet
HNO3 Light Brick color Grayish green
HNO3 + water Light lemon Yellowish green Green
Acetic acid Green dark green Pink
Methanol Green Faint light green Pink
Ethanol Green Light green Pink
Chloroform Green Light yellowish
green Pink
Petroleum ether No change Dark green Blackish violet
Dist. water Brownish
yellow
Light yellowish
green Violet
10% NaOH Brick red Light green Grayish violet
5% Iodine
Brick color Green
Picric acid
Yellowish green Light green
FeCl3 solution Brown Yellowish green Green
NH3 solution Brown Green Violet

111
Table 8: Fluorescent analysis of root of Calotropis gigantea
Powder drug Observation
Ordinary Light UV (254 nm) UV (366 nm)
Dry powder as such
Green No change No change
H2SO4 Blood red No change No change
H2SO4 + water Yellowish green Light green Green
HCl Green No change No change
HCl + water No change Light green Dark green HNO3 Yellow Green Green HNO3 + water
Yellow Light green
Acetic acid Light green No change Blood red Methanol Light green No change Brick red Ethanol Light green No change Light red Chloroform Green Yellow Pink Petroleum ether Dark green Dark yellow Buff
Dist. water Light yellow Dark yellow Green
10% NaOH Light brown No change No change
5% Iodine Cherry red Brick red No change
Picric acid Yellowish green
No change Green
FeCl3 solution Dark brown No change No change
NH3 solution Light brown Grayish black Black

112
Table 9: Physicochemical parameters of Sphaeranthus indicus
fruit
Parameters (w/w %) Values in percentage
Fruit
Moisture content 0.20
Foreign matters 1.00
Total ash 5.30
Acid insoluble ash 1.00
Water soluble ash 2.35
Sulphated ash 2.90
Pet. ether extract 3.75
Benzene extract 1.22
Chloroform extract 1.05
Ethyl acetate 0.93
Ethanol extract 0.70
Aqueous extract 0.45

113
Table 10: Fluorescent analysis of fruit of Sphaeranthus indicus
Powder drugs
Observation Day Light UV (254 nm) UV (366 nm)
Dry powder as such Dark brown No change No change
H2SO4 Light brown Brown No change H2SO4 +
water Black No change Black
HCl Light yellowish Dark yellow Light yellow
HCl + water Light Light green Violet
HNO3 No change Brick color Cherry
HNO3 + water Lemon Green Dark green
Acetic acid Light brown Brown Light brown
Methanol Brown Light brown Light brown
Ethanol Brown Light brown Light brown
Chloroform Brown Light brown Light brown
Petroleum ether Light green Dark green Blackish violet
Dist. water Brownish yellow
Light yellowish Violet
10% NaOH Brick red Light green Grayish violet
5% Iodine No change Brick color Green
Picric acid No change Green Light green
FeCl3 solution Brown Yellowish green Dark Green
NH3 solution Brown Dark green Violet

114
6.3 Phytochemical evaluation
6.3.1 Phytochemical evaluation of Calotropis gigantea
Extractive values of selected medicinal plants were observed
and tabulated (Table 11).
Table 11: Preliminary phytochemical screening of various
extracts of Calotropis gigantea
Extract Alkaloid Glycoside Tannin Protein Carbohydrates Phenol Saponin Flavonoid
s
Fixed
oils &
Fats
Leaves
PEE - - - - + - - - ++
BE - - - - + - + + -
CE - - ++ - - + + ++ -
EAE - - - - - + - ++ -
ME + ++ - + + ++ - ++ -
AE + ++ - - + ++ - ++ -
Roots
PEE - - - + - - + -
BE - - - + - + + -
CE ++ - - - - ++ - + -
EAE ++ - - - - + - + -
ME +++ ++ - - + ++ - +++ -
AE + ++ - - + ++ - ++ -

115
Discussion
Preliminary phytochemical studies reveal the presence of
phytoconstituents like alkaloids, phytosterols, carbohydrates, phenolic
compounds, tannins, triterpenoids and flavonoids in all three selected
plant extracts and fixed oil was found in methanolic extract of
Calotropis gigantea.
The amount of total phenolic compounds varied in different
plants and ranged from 3.1 to 32.3 mg gallic acid equivalent (GAE/g)
of dry material. The highest amount of total phenolic levels has been
detected in methanolic extract. From analysis we can deduce that
plant extracts contain rich amount of flavonoids.

116
6.3.2 Phytochemical evaluation of Sphaeranthus indicus
Extractive values of selected medicinal plant were observed and
tabulated (Table 12).
Table 12: Preliminary phytochemical screening of various
extracts of Sphaeranthus indicus fruit
PEE = Petroleum ether extract, BE= Benzene extract, CE=
Chloroform extract, EAE = Ethyl acetate extract, ME = Methanolic
extract, AE= Aqueous extract
Extract Alkaloid Glycoside Tannin Protein Carbohydrates Phenol Saponin Flavonoids Fixed oils & Fats
PEE - - - - - - - - +
BE - - - - ++ + - - -
CE - - + + - - ++ ++ -
EAE - - - - - - + + -
ME +++ + - + + + - +++ -
AE + ++ - - + ++ - +++ -

117
Discussion `
Preliminary phytochemical studies reveal the presence of
phytoconstituents like alkaloids, phytosterols, carbohydrates,
phenolic compounds, tannins, triterpenoids and flavonoids in all three
selected plant extracts and fixed oil was found in methanolic extract
of Sphaeranthus indicus.
6.4 Hypoglycemic effect of extracts of Calotropis gigantea
6.4.1 Hypoglycemic effect of extracts of Calotropis gigantea in
normal rats
Hypoglycemic effects of extracts of Calotropis gigantea in various
solvents after 0, 1, 4, 8 and 12 hours in normal rats were observed and
were tabulated (Table 13).

118
Table 13: Hypoglycemic effect of extracts of Calotropis gigantea in
normal rats
Discussion
A single dose of petroleum ether, methanolic and aqueous extracts
of Calotropis gigantea leaf and root (250 mg/kg BW, respectively)
exhibited no significant hypoglycemic effect (p<0.05) after 8th hour.The
effect was felt at 12 hours post dose (p<0.01). Glibenclamide had
significant effect on blood glucose level 4 hours post dose (p<0.01).
Treatment
0hr
1hr
4hr
8hr
12hr
Normal control 97.2 ± 3.4 96.5 ± 5.2 96.1 ± 2.0 94.5 ± 1.8 96.1 ± 3.5
Pet. Ether extract (L) 250mg/kg 97.3 ± 1.9 97.1 ± 4.5 96.3 ± 2.8 96.3 ± 3.4 96.5 ± 5.6
**
Methanolic extract (L)250mg/kg
96.5 ± 4.7 96.4 ± 6.0 95.6 ± 3.2 95.7 ± 3.1 96.4 ± 2.4**
Aqueous extract (L) 250mg/kg 96.3 ± 2.0 94.1 ± 2.2 93.4 ± 0.2 94.4 ± 2.6 94.3 ± 0.12
**
Pet. ether extract (R) 250mg/kg 96.4 ± 4.2 96.6 ± 2.2 97.3 ± 2.6 96.7 ± 6.8 96.2± 2.2
**
Methanolic extract (R) 250mg/kg
96.3 ± 2.8 96.7± 4.6 96.5± 0.2 96.9± 2.2 96.6± 4.8**
Aqueous extract (R) 250mg/kg 97.5 ± 4.8 97.5± 2.2 97.7±0.2 97.8 ± 0.6 97.7 ± 0.8
**

119
6.4.2 Effect of extracts of Calotropis gigantea on oral glucose
tolerance test.
Results of the OGTT conducted on control rats and different
experimental groups of rats were observed and tabulated (table 14).
Table 14: Effect of extracts of Calotropis gigantea on oral
glucose tolerance test
Values are mean ±SEM, n= 6. (One way ANOVA Followed by
Dunnette multiple Comparisons test). Super script *, **, denotes
statistically significance of P<0.01, P<0.001, when compared with
respective diabetic control.
Treatment / mg/kg Blood glucose levels (mg/dL)
0 min 30 min 60 min 120 min
Normal control 94.3 ± 2.0 94.5 ± 2.7 93.5 ± 2.3 94.2 ± 2.6
Diabetic control 142.6 ± 7.3 147.3 ± 7.2 150.6 ± 6.9 157.5 ± 7.0
Glibenclamide 600
µg/kg
131.7 ± 5.4 124.8 ± 6.3 123.6 ± 4.9* 113.1± 4.9
**
Pet. ether extract (L)
250mg/kg
128.6±0.42 130.4±0.26 128.2±2.24* 126.3±0.22
**
Methanolic extract
(L) 250mg/kg
130.3 ± 5.9 144.4 ± 6.0 140.7 ± 5.0* 120.5 ± 5.6
**
Aqueous extract (L)
250mg/kg
129.5 ± 5.6 136.8 ± 4.9 135. ± 5.8* 123.2± 4.9
**
Pet. ether extract
(R) 250mg/kg
130.2±2.2 134.2±4.2 130.3±2.42* 128.8±0.22
**
Methanolic extract
(R) 250mg/kg
129.5±2.2 131.28±4.2 129.2±2.46* 122.4±0.26
**
Aqueous extract (R)
250mg/kg
128.2±0.22 130.2±0.22 129.4±0.44* 127.6±2.22
**

120
Discussion
The blood glucose level of the normal control rats reached a peak,
30 minutes after the oral administration of glucose and gradually
decreased to the nearly glucose load level. In diabetic control rats, the
blood glucose level reached a peak at 120 minutes, the glucose levels
remained higher even after 2 hours. STZ diabetic rats treated with
extracts and standard drug showed significant decrease in blood glucose
levels at 2 hours. OGTT is a well accepted and frequently used assay to
screen antihyperglycemic activity. Extracts and standard drug might
enhance glucose utilization because they significantly reduced the blood
glucose level in STZ diabetic rats. In glucose fed diabetic rats, the
elevated blood glucose levels remained higher after 2 hours. In rats
treated with extracts and standard drug, the glucose levels reached peak
at 30 minutes and returned to the nearly control content after 2 hours.
The extracts at the dose of 250 mg/kg BW significantly increased the
tolerance for glucose. The findings of this OGTT study probably suggest
that the hypoglycemic effect of plant extracts were dose dependent and
facilitates or enhances the clearance of post prudential blood glucose in
rats.

121
6.4.3 Antihyperglycemic effects of extracts of Calotropis gigantea
on STZ induced diabetic rats (15 Days Model)
Antihyperglycemic effects of extracts of Calotropis gigantea on STZ
induced diabetic rats (15 Days Model) were observed and tabulated
(Table 15).

122
Table 15: Anti-hyperglycemic effect of extracts of Calotropis gigantea on blood
Values are mean ±SEM, n= 6. (One way Anova followed by
Dunnette multiple comparisons test). Super script *, **, denotes
statistically significance of P<0.01, P<0.001, when compared with
respective diabetic control.
Treatment Blood glucose level (mg/dl) Day 1 Day 5 Day 10 Day 15
Normal control 124.891.47 124.22.26 123.22.46 123.10.22
Diabetic control 236.22.22 242.52.24 240.74.24 247.64.48
Glibenclamide 600
µg/kg
235.41.00 206.82.58** 192.62.07
** 138.33.11
**
Pet. ether extract (L)
250mg/kg 237.62.30 219.21.92
** 190.81.82
* 153.01.58
*
Methanolic extract (L)
250mg/kg 235.01.58 206.22.77
** 185.02.00
** 140.62.07
**
Aqueous extract (L)
250mg/kg
237.22-64 215.42.07** 193.62.30
** 162.92.70
*
Pet. ether extract (R)
250mg/kg 238.62.30 218.82.74
** 216.21.92
* 205.21.59
*
Methanolic extract (R)
250mg/kg 234.61.48 210.81.58
** 195.61.58
** 142.72.22
**
Aqueous extract (R)
250mg/kg
235.91.58 229.23.11** 219.22.91
* 163.91.30
*

123
Discussion
The petroleum ether, methanolic and aqueous extracts exhibited
anti-diabetic property in streptozotocin-induced diabetic rats as evident
from blood glucose levels. In untreated control (Diabetic) rats the blood
glucose levels increased from 236.22.22 to 247.64.48 mg/dl on the
fifteenth day. In petroleum ether extract (leaves and roots) treated rats
(250 mg/kg BW), the blood glucose levels steadily decreased and they
were found to be 237.62.30 to 153.01.58 mg/dl and 238.62.30 to
205.21.59 mg/dl respectively. In methanolic extract (leaves and roots)
treated rats (250 mg/kg BW), the blood glucose levels were found to be
235.01.58 to 140.62.07 mg/dl and 234.61.48 to 142.72.22 mg/dl
respectively. In aqueous extract (leaves and roots) treated rats (250
mg/kg BW), the blood glucose levels were found to be 237.22.64 to
162.92.70 mg/dl and 235.91.58 to 163.91.30 mg/dl respectively. In
standard drug treated rats the blood glucose levels were found to be
235.41.00 to 138.33.11mg/dl respectively at the end of experiment
(15th day). The result demonstrated that anti-hyperglycemic activity was
concentration dependent.

124
6.5 Hypoglycemic effect of Calotropis gigantea leaves via different
routes of administration in normal and alloxan induced
diabetic rats
6.5.1 Effect of water extract of Calotropis gigantea leaves on plasma
glucose levels after intragastric (p.o) and intraperitoneal (i.p.)
administration to normoglycemic rats
The results of effects of water extract of Calotropis gigantea leaves
on plasma glucose levels after intragastric (p.o) and intraperitoneal (i.p.)
administration to normoglycemic rats after a interval of 0, 20, 60, 120,
240 and 360 minutes were tabulated (Table 16).

125
Table 16: Effect of water extract of Calotropis gigantea leaves on
plasma glucose levels after intragastric (p.o) and intraperitoneal
(i.p.) administration to normoglycemic rats
Treatment Route Plasma glucose (g/L) at time ( min) after treatment
0 20 60 120 240 360
Control(Saline.10 ml/kg)
p.o. 0.99±0.05 0.99±0.08 0.98±0.09 0.90±0.16 0.95±0.06 0.96±0.07
i.p. 0.98±0.04 0.96±0.06 0.89±0.08 0.93±0.09 0.93±0.08 0.94±0.08
Glibenclamide(0.13 mg/kg)
p.o. 0.96±0.09` 0.69±0.11* 0.46±0.07++ 0.57±0.07+ 0.73±0.06 0.83±0.05
i.p. 0.98±0.08 0.73±0.1* 0.48±0.06++ 0.63±0.05+ 0.75±0.06* 0.93±0.13
Metformin(11.3 mg/kg)
p.o. 0.99±0.05 0.73±0.06* 0.65±0.1* 0.54±0.08+ 0.75±0.06* 0.93±0.13
i.p. 0.93±0.04 0.79±0.05* 0.57±0.06+ 0.71±0.05* 0.74±0.05 0.80±0.05
C. gigantea(0.7
g/kg)
p.o. 0.93±0.05 0.59±0.06++ 0.58±0.14++ 0.51±0.07++ 0.83±0.13 1.02±0.06
i.p. 0.98±0.07 0.68±0.06++ 0.56±0.22++ 0.54±0.19++ 0.63±0.09+ 0.67±0.08
+
Values are mean ± SEM, n= 8; *p< 0.05; +p<0.01; ++p<0.001 vs.
Control; Anova and Newman - Keuls test

126
Discussion
The infusion of Calotropis gigantea exhibited a remarkable
hypoglycemic action within 20 minutes after oral and i.p. administration to
normal rats. Blood glucose level reached a mean value of 0.59 ± 0.06 g/L
and 0.68 ± 0.06 g/L, respectively as compared to 0.99 ± 0.08 g/L and
0.96 ± 0.06 g/L respectively obtained in the control group. The lowest
hypoglycemic effect was observed after 2 hours i.e 0.51 ± 0.07 g/L and
0.54 ± 0.19 g/L respectively with oral and i.p administration. After 4
hours of administration, the blood glucose level reached nearly to the
initial glycemic values for orally treated animals, while i.p. administration
still showed hypoglycemic effect even after 6 hours. Hypoglycemic effects
of Calotropis gigantea were comparable and sometimes higher than that
obtained with 0.13 mg/kg BW of glibenclamide or 11.3 mg/kg BW of
metformin.
6.5.2 Effect of water extract of Calotropis gigantea leaves on plasma
insulin levels in normoglycemic rats after intragastric (p.o.) and
intraperitoneal (i.p.) administration
Results were observed and tabulated (Table 17).

127
Table 17: Plasma insulin levels in normoglycemic rats after
intragastric (p.o.) and intraperitoneal (i.p.) administration of water
extract of Calotropis gigantea leaves
Treatment Route
Insulinemia (12.42 µlU/mL) at time ( min) after treatment
0 20 60 120 240 360
Control (Saline.10
ml/kg)
p.o. 58.08±4.41 68.56±10.26 63.11±8.42 56.64±11 60.06±10 72.32±6.16
i.p. 88.88±14.96 71.89±8.25 60.41±7.89 61.57±9.15 67.27±8.01 84.94±7.91
C. gigantea (0.7 g/kg)
p.o. 82.06±14.35 68.96±8.52 54.14±9.56 51.88±3.03 63.17±19.04 75.03±19.42
i.p. 64.22±8.56 78.07±12.62 90.19±7.16* 73.02±16.9 121.42±10.01++ 113.37±20.52+
Values are mean ± SEM, n= 8; *p< 0.01; ++p<0.001 vs. Control; Anova
and Newman - Keuls test.

128
Discussion
After i.p. administration, the variation in insulin plasma levels
showed an opposite trend to that of glucose. The increase became
significant after 1 hour of administration and persisted for at least 6 hour.
Plasma insulin reached a maximum level (12.42µlU/mL) 4 hour after i.p.
administration. On the other hand, no variation in blood insulin level was
found in normal rats orally treated with the water extract of Calotropis
gigantea leaves.
6.5.3 Effect of water extract of Calotropis gigantea leaves on plasma
glucose levels after intragastric (p.o) and intraperitoneal (i.p)
administration to alloxan-diabetic rats
Effect of water extract of Calotropis gigantea leaves on plasma
glucose levels after intragastric (p.o) and intraperitoneal (i.p)
administration to alloxan-diabetic rats after a interval of 0, 20, 60, 120,
240 and 360 minutes were observed and tabulated (Table 18).

129
Table 18: Effect of water extract of Calotropis gigantea leaves on
plasma glucose levels after intragastric (p.o) and intraperitoneal (i.p)
administration to alloxan-diabetic rats
Values are mean ± SEM, n= 8; *p< 0.05; +p<0.01; ++p< 0.001 vs.
control; bp<0.05 vs. glibenclamide; xp<0.05; yp<0.01 vs. metformin;
Anova and Newman - Keuls test.
Treatment Route Plasma glucose (g/L) at time(minutes) after treatment
0 20 60 120 240 360
Control (Saline.10
ml/kg)
p.o. 2.82±0.2 2.57±0.14 2.14±0.72 2.20±0.45 2.35±0.39 3.00±0.48
i.p. 2.71±0.2 2.61±0.18 2.59±0.65 2.15±0.5 2.28±0.49 2.92±0.51
Glibenclamide(0.13 mg/kg)
p.o. 2.88±0. 2 2.15±0.26 1.44±0.39+ 0.91±0.08++ 1.44±0.22++ 1.70±0.34+
i.p. 3.01±0.03 2.36±0.35 1.21±0.47* 0.88±0.11* 1.44±0.22* 1.70±0.34
Metformin (11.3
mg/kg)
p.o. 2.96±0.1 2.66±0.2 1.21±0.09+ 0.99±0.06+ 1.37±0.25+ 2.00±0.47
i.p. 3.01±0.09 1.30±0.4 0.74±0.41* 1.63±0.25* 1.50±0.35* 1.80±0.30*
C. gigantea
(0.7 g/kg)
p.o. 2.90±0.08 2.02±0.53* 1.05±0.16++ 1.01±0.07++ 1.03±0.12++ 0.92±0.20+yx
i.p. 2.86±0.3 1.74±0.25+ 1.60±0.22+ 0.79±0.3++ 1.189±0.21++ 1.32±0.19++bx

130
Discussion
When compared with control, Calotropis gigantea significantly
reduced the blood glucose levels in diabetic rats. The maximum
decrease was observed 2 hours after the administration and plasma
glucose level recorded as 1.01±0.07 g/L (-69.96%) and 0.79±0.3 g/L (-
53.29%), respectively after oral and i.p. treatment.
6.5.4 Effect of before and after the intravenous administration of
water extract of Calotropis gigantea leaves on blood glucose levels
in glucose loaded (0.25 g/kg BW) rats
The results of the effect of before and after the intravenous
administration of water extract of Calotropis gigantea leaves on blood
glucose levels in glucose loaded (0.25 g/kg BW) rats after 0, 5, 10, 20,
30, 40, 50 and 60 minutes were observed and tabulated (Table 19).

131
Table 19: Blood glucose levels in glucose loaded (0.25 g/kg BW) rats
before and after the intravenous administration of water extract of
Calotropis gigantea leaves
Treatment
Blood glucose (g/L) at time ( min) after load
0 5 10 20 30 40 50
60
Control (0.25g/kg glucose)
0.99±0.08 1.26±0.08 1.47±0.11 1.59±0.14 1.71±0.09 1.69±0.11 1.46±0.08 1.33±0.07
C. gigantea (0.7 g/kg)
0.98±0.09 1.15±0.1 1.35±0.06 1.48±0.1 1.51±0.08* 1.31±0.1+ 1.25±0.11+ 1.16±0.13++
Values are mean ± SEM, n= 5; *p< 0.05; +p<0.01; ++p<0.001 vs.
Control; Anova and Newman - Keuls test.
Discussion
In a glucose tolerance test, intravenous treatment with Calotropis
gigantea plasma glucose level significantly reduced at time intervals of
40, 50 and 60 minutes as compared to plasma glucose level induced in
control by a glucose load administration. Glycemic values returned to
basal levels more rapidly than in control group. The coefficient of glucose
assimilation (KG) showed significant increase in treated rats compared to
control (8.17×10-3 vs 6.96×10-3).

132
6.6 Effect of Calotropis gigantea and Sphaeranthus indicus on
glycemia and lipidemia in streptozotocin induced diabetic rats
6.6.1 Effect of treatment of 8 weeks with water extract (300 mg/kg
BW) of Calotropis gigantea and Sphaeranthus indicus and a mixture
of the two plants on fasting plasma glucose level in streptozotocin
(STZ) diabetic rats
Effect of treatment of 8 weeks with water extract (300 mg/kg BW) of
Calotropis gigantea and Sphaeranthus indicus and a mixture of the two
plants on fasting plasma glucose level in streptozotocin (STZ) diabetic
rats were observed and tabulated (table 20).

133
Table 20: Effect of treatment of 8 weeks with water extract (300
mg/kg BW) of Calotropis gigantea and Sphaeranthus indicus and a
mixture of the two plants on fasting plasma glucose level in
streptozotocin (STZ) diabetic rats
Plasma glucose ( mg/dl) mean ± S.D. Group 0 Weeks 8 Weeks
Control 99.4 ± 19.5 89.8 ± 5.21 Diabetic untreated 172.2 ± 5.4 285.6 ± 42.6 Diabetic + Calotropis gigantea
164.6 ± 25.0 105.4 ± 26.6
Diabetic + S. indicus
158.6 ± 10.0a 98.2 ± 25.2a
Diabetic + Calotropis gigantea + S. Indicus
166.9 ± 25.4 85.4 ± 2.3
a = p < 0.001
Group of 5 animals were used for each set of experiments.
All the data were statistically evaluated and the significance was
calculated using student’s‘t’- test. All the results were expressed as mean
± S.D.

134
Discussion
Water extract of Calotropis gigantea plus Sphaeranthus indicus
administered at a dose of 300 mg/kg BW (body weight) brought down
fasting blood glucose, from a higher value of 166.9 ± 25.4 mg/dl to a
normal value of 85.4 ± 2.3 mg/dl while in the untreated group the fasting
blood glucose (FBG) increased from the initial value of 172.2 ± 5.4 mg/dl
to 285.6 ± 42.6 mg/dl.
6.6.2 Effect of water extract (300 mg/kg BW) of Calotropis gigantea
and Sphaeranthus indicus and mixture of the two plants on plasma
glucose tolerance in diabetic rats after 8 weeks
Effect of water extract (300 mg/kg BW) of Calotropis gigantea and
Sphaeranthus indicus and mixture of the two plants on plasma glucose
tolerance in diabetic rats after 8 weeks were recorded and tabulated
(Table 21).

135
Table 21: Effect of water extract (300 mg/kg BW) of Calotropis
gigantea and Sphaeranthus indicus and mixture of the two plants on
plasma glucose tolerance in diabetic rats after 8 weeks
Blood glucose ( mg/dl) mean ± S.D. Group 0 hr 0.5
hr 1 hr 1.5
hr 2 hr
Control 94.3 ± 21.0
140.2 ±11.2
132.6 ±27.3
116.2 ±10.0
102.0 ±12.0
Diabetic untreated
160.5 ±32.1
245.0 ±68.6
273.4 ±89.3
290.6 ±82.6
269.0 ±92.2
Diabetic + Calotropis gigantea
87.9 ±25.6
112.2 ±20.6
114.3 ±15.0
102.0 ±10.3
95.6 ±24.0
Diabetic + S. indicus
82.0 ± 4.2
86.0 ± 4.3
81.0 ± 3.9
80.0 ± 3.2
84.0 ± 3.2
Diabetic + C. gigantea + S. indicus
81.0 ± 3.5
84.0 ± 4.2
86.0 ±3.3
81.0 ±3.6
75.2 ± 1.0

136
Discussion
In plasma glucose tolerance in diabetic rats after 8 weeks the blood
sugar with untreated rats after 2 hours is 269.0 ± 92.2 mg/dl and with
Calotropis gigantea plus Sphaeranthus indicus the blood sugar is 75.2 ±
1.0 mg /dl. The fasting (0 hour) blood glucose values which were higher
in the diabetic animals (160.5 ± 32.1 mg/dl) were brought down to 81.0 ±
3.5 mg/dl, when 300 mg/kg BW of the extract of the mixture of the two
plants was administered for 8 weeks.
6.6.3 Effect of treatment for 8 weeks with water extract of (300 mg/kg
BW) Calotropis gigantea and Sphaeranthus indicus and both
Calotropis gigantea + Sphaeranthus indicus on plasma lipids in
diabetic rats
Effect of treatment for 8 weeks with water extract of (300 mg/kg
BW) Calotropis gigantea and Sphaeranthus indicus and both Calotropis
gigantea + Sphaeranthus indicus on plasma lipids in diabetic rats were
observed and tabulated (Table 22).

137
Table 22: Effect of treatment for 8 weeks with water extracts of (300
mg/kg BW) Calotropis gigantea and Sphaeranthus indicus and both
Calotropis gigantea + Sphaeranthus indicus on plasma lipids in
diabetic rats
Group TC ( mg/dl) mean ± S.D.
LDL-C ( mg/dl) mean ± S.D.
HDL-C (mg/dl) mean ± S.D.
LDL-C/HDL-C ( mg/dl) mean ± S.D.
TG (mg/dl) mean ± S.D.
Control 170.3 ± 10.3 78.0 ± 12.2 44.9 ±13.3 1.7 ±0.3 115.6 ± 42.6
Diabetic untreated
250.0 ± 14.9 152.2± 12.6
45.0 ±12.0 3.3 ±0.4 181.8 ±18.8
Diabetic + Calotropis gigantea
175.0 ± 12.3 99.7 ±16.8 51.3 ±8.4 1.9 ±0.4 174.0 ±15.8
Diabetic + S. indicus
187.0 ± 14.9 95.6 ±15.7 50.2 ±8.5 1.6 ±0.3 135.0 ±13.2
Diabetic + C. gigantea + S. indius
174.0 ± 10.3 51.3 ±6.3 48.3 ±8.2 1.8 ± 0.5 131.0 ±11.2
TC, LDL-C, HDL-C, TG = Total cholesterol, Low density lipoprotein
cholesterol, High density lipoprotein cholesterol and Triglyceride. Number
of animals was 5 in each group.

138
Discussion
The changes in the lipid profile have also been studied. In the case
of diabetic treated animals, with Calotropis gigantea alone, total
cholesterol, LDL cholesterol and LDL-C/HDL-C values returned to near
normal values. There was very slight fall in TG values probably because
these plants could not show much effect on triglycerols. But further
improvement in increase in HDL-C value was seen. With Calotropis
gigantea plus Sphaeranthus indicus treatments similar values were
obtained. Further there was reduction in TG values also.
6.6.4 Effect of water extract of Calotropis gigantea plus
Sphaeranthus indicus on glycosylated haemoglobin, body weight,
serum albumin, total proteins and creatinine, urine sugar and
albumin values shown at the end of 8 weeks treatment
Effect of water extract of Calotropis gigantea plus Sphaeranthus
indicus on glycosylated haemoglobin, body weight, serum albumin, total
proteins and creatinine, urine sugar and albumin values shown at the end
of 8 weeks treatment were recorded and tabulated (Table 23).

139
Table 23: Effect of water extract of Calotropis gigantea plus
Sphaeranthus indicus on glycosylated haemoglobin, body weight,
serum albumin, total proteins and creatinine, urine sugar and
albumin values shown at the end of 8 weeks treatment
Parameter Normal mean ± SD
Diabetic mean ± SD
Diabetic treated mean ± SD
Glycosylated haemoglobin (HbA1c) %
3.04 ± 0.02
9.4 ± 2.4
4.8 ± 0.1
Albumin (g/L) 55.0 ± 1.4 45.0 ± 3.1
52.9 ± 3.0a
Total protein (g/L) 69.0 ± 3.0 73.2 ± 2.9
78.2 ± 3.8a
Creatinine (mg/dl) 0.75 ± 0.04
1.30 ± 0.15
0.91 ± 0.05a
Body weight (g) 283.6 ± 25.8
225.5 ± 45.0
280.4 ± 9.0
Kidney weight (g) 1.40 ± 0.05 2.92 ± 0.08
1.06 ± 0.10
Haemoglobin (g/dl) 16.0 ± 1.2 16.4± 1.4 16.3± 1.1 Urine sugar ND +++ ++ Urine albumin ND ++ ND
The values are mean ± SD.
*a p < 0.05 when compared with diabetic untreated group.

140
Discussion
The total proteins, albumin and creatinine in serum, glycosylated
haemoglobin in blood and total body weight and weight of kidneys (in the
animals killed after the experiment) were also analyzed after 8 weeks of
treatment. An interesting observation is that glycosylated haemoglobin
(HbA1c) % decreased to 4.8 ± 0.1 and returned to normal values after 8
weeks of treatment.
6.6.5 Effect of water extract of Calotropis gigantea plus
Sphaeranthus indicus on the serum lipid profile and on liver and
kidney weights in rats fed on high fat diet
Effect of water extract of Calotropis gigantea plus Sphaeranthus
indicus on the serum lipid profile and on liver and kidney weights in rats
fed on high fat diet were recorded and tabulated (Table 24 and Table 25,
respectively).

141
Table 24: Effect of water extract of Calotropis gigantea plus
Sphaeranthus indicus on the serum lipid profile in rats fed on high
fat diet
Group TC (mg/dl) TG (mg/dl) LDL(mg/dl) HDL-C(mg/dl)
Normal 198.7 ± 44.9 94.9 ± 7.1 83.8 ± 16.2 42.3 ± 19.2
High-fat rats untreated
622.3 ± 1.4 34.7 ± 0.9 3.58 ± 0.11 31.0 ± 0.10
High-fat diet plus extracts
182.5 ± 4.2 171.8 ± 0 148.8 ± 8.0 173.1 ± 23.4
Table 25: Effect of water extract on liver and kidney weight in rats
fed on high fat diet.
Tissues Normal rats High-fat diet untreated
High-fat diet plus extracts of two plants
Liver (g) 7.82 ± 0.33 10.4 ± 0.41 9.8 ± 0.18b
Kidney (g)
0.99 ± 0.05 1.08 ± 0.08 0.99 ± 0.06 b
*b p<0.0005 *c p<0.01
Discussion
Herbal treatment improves the weight of liver and kidney in diabetic
rats fed on high fat diet, although it was not completely reversible in liver.

142
6.7 Antioxidant activity
Antioxidant activity of methanol, ethanol and aqueous extracts of the
leaves of Calotropis gigantea was carried out and the results were
compared graphically (figure 11).
Figure 11: Comparison of antioxidant activity of various extracts Discussion
In the present study, methanol extract of the leaves of Calotropis
gigantea showed potential free-radical scavenging activity but aqueous
extract showed very little free-radical scavenging activity. The ethanol
extract showed lowest activity.
6.8 Antimicrobial activity
The bacterial suspensions were seeded on Mueller-Hinton Agar
(MHA) plates using a sterilized cotton swab. In each of these plates four
wells were cut out using a standard cork borer (7 mm). Using a
Meth. extract
Eth. extract
Aq. extract

143
micropipette, 100 μl of each dilution was added into the wells. All the
plates were incubated at 37ºC for 24 hours. Antimicrobial activity of the
leaf extract was evaluated by measuring the zone of inhibition.
Experiment was carried out in triplicates for each test organism. The
results were recorded and illustrated below.
.

144
Figure 12: Antimicrobial activity of Calotropis gigantea
Test bacteria

145
Table 26: Test organisms’ relative percentage inhibition (%)
Test organism Relative percentage inhibition (%)
Staphylococcus aureus 48.05
Klebsiella pneumoniae 75.64
Bacillus cereus 175.36
Pseudomonas
aeruginosa
108.16
Micrococcus luteus 26.67
Escherichia coli 155.89

146
Figure 13: Relative percentage inhibition of Calotropis gigantea
Relative percentage inhibition
Rel
ativ
e pe
rcen
tage
inhi
bitio
n (%
)
Microorganism

147
Table 27: MIC values of methanol and aqueous extracts of
Calotropis gigantea on test organism
MIC in mg/ml
S.aureus K.pneumonia B.cereus P.aeruginosa M.luteus E. coli
52 23 5.25 4.1 1.7 11.65
Table 28: Antimicrobial activity of Calotropis gigantea
AE: aqueous extract, PC: positive control, NC: negative control. Values
are expressed as mean ± standard deviation of the three replicates. Zone
of inhibition not include the diameter of the well.
Test organisms
Inhibition zone diameter (mm)
AE PC NC
Staphylococcus aureus
14.3±1.15 18.6±1.52 0
Klebsiella pneumonia
13.6±1.52 13.3±0.57 0
Bacillus cereus
16.3±1.52 15.6±1.15 0
Pseudomonas aeruginosa
14.0±1.73 16.6±1.52 0
Micrococcus luteus
16.6±1.52 33.3±1.52 0
Escherichia coli
18.6±1.15 16.6±2.08 0

148
Discussion
The crude extract showed 52, 23, 11.65, 5.25, 4.1 and 1.7 mg/ml MIC
values for S. aureus, K. pneumoniae, E. coli, B. subtilis, P. aeruginosa
and M. luteus, respectively. Aqueous extract of Calotropis gigantea
showed high inhibitory activity followed by methanol extract, whereas
ethanol and petroleum ether extracts showed low activity. Previous
studies reported the presence of phytochemicals like cardenolides,
flavonoids, terpenes, pregnanes, amino acids and cardiac glycosides as
major constituents in Calotropis gigantea may acknowledge the medicinal
properties of this plant.

149
6.9 Muscle relaxant activity
Muscle relaxant activity of aqueous and ethanolic extracts was
carried out and the results were illustrated below in tabular and
graphical forms.
Figure 14: Muscle relaxant activity of Calotropis gigantea
Mus
cle
rela
xant
act
ivity
(mm
)

150
Figure 15: Comparison of muscle relaxant activity of acetylcholine
and test drug at different concentrations
Mus
cle
rela
xant
act
ivity
(mm
)

151
Table 29: Muscle relaxant activity of extract from Calotropis
gigantea
Drug Volume
(ml)
Dose
(μg)
Height(mm) Responses
Acetylcholine 0.1 1 3 Increased Acetylcholine 0.4 4 5 Increased Acetylcholine 0.8 8 9 Increased Acetylcholine 1.2 12 11 Increased T1 (1:100) 0.4 4 - - T1 + ach 0.1 1 6 Increased T1 + ach 0.4 4 9 Increased T1 + ach 0.8 8 12 Increased T2 (1:500) 0.4 4 - Increased T2 + ach 0.1 1 24 - T2 + ach 0.2 2 13 Increased T3(1:1000) + ach 0.3 3 15 Increased T3 + ach 0.4 4 16 Increased T3 + ach 0.8 8 18 Increased T3 + ach 1.6 16 24 Increased

152
Discussion
The aqueous and ethanolic extracts of Calotropis gigantea were
found to have skeletal muscle relaxant property at T1 (1:100), T2 (1:500)
and T3 (1:1000), when tested along with acetylcholine. When the
relaxant property was compared with the standard drug acetylcholine,
ethanolic extract tested along with the acetylcholine produced more
relaxant property than the standard drug acetylcholine. Lesser the
concentration of the test drug (ethanolic extract) more was the response
of the muscle relaxant property. Maximum relaxant effect in T1 and T3
was found i.e. 22 mm and 23 mm at the dose of 16 μg and T2 was 13
mm at 2 μg. Earlier studies have proved that chloroform extract of
Ervatamia crispa revealed skeletal muscle relaxant effect on an isolated
rat rectus abdominis muscle preparation.

153
7. SUMMARY AND CONCLUSION

154
7. SUMMARY AND CONCLUSION
Many studies have shown that flavonoids and phenolic contents
decrease the blood glucose levels and oxidative stress and increase
serum insulin concentrations (Azuma, 2007; Jalal, 2007; Stanley, 2006).
Flavonoids, steroids, triterpenoids, alkaloids and phenols are
known to be bioactive anti-diabetic principles (Oliver Bever, 1986; Ivorra,
1989; Attar, 1989; Kameswara Rao, 1997). Flavonoids are known to
regenerate the damaged beta cells of islets of Langerhans in diabetic
rats. Phenolic contents are found to be effective anti-hyperglycemic
agents (Manickam, 1997).
In the present study, an attempt was made to investigate the
efficacy of Calotropis gigantea and Sphaeranthus indicus as antidiabetic,
antilipidemic, muscle relaxant, antioxidant and antibacterial agent.
Detailed pharmacognostical, phytochemical and pharmacological studies
were carried out as per standard procedures. The evaluation of the plant
extracts for their antidiabetic, antilipidemic, muscle relaxant, antioxidant
and antibacterial activities were carried out.
The phytochemical screening of various extracts of selected plants
revealed the presence of alkaloids, flavonoids, phenolic compounds,
phytosterols, triterpenoids, glycosides and tannins.
In this study, extracts showed hypolipidemic effects in STZ-induced
diabetic rats. The serum triglycerides (TG), total cholesterol (TC) and

155
serum low density lipoproteins (LDL) and very low density lipoproteins
(VLDL) cholesterol concentrations were significantly increased by STZ
injection, but Calotropis gigantea suppressed the increase in these
levels. In contrast, high density lipoproteins (HDL) cholesterol
concentration and total cholesterol (TC) ratio were decreased by STZ-
injection, but were normalized by extracts of Calotropis gigantea
administration.
Glibenclamide is commonally used as a standard drug in
streptozotocin induced diabetes to compare the efficacy of variety of
hypoglycemic compounds (Paredes, 2001).
The Calotropis gigantea showed hypoglycemic effect in normal and
diabetic rats after both oral and intraperitoneal administration. The effects
produced were comparable to that of well-known oral hypoglycemic
compounds like metformin and glibenclamide used at a dose of 11.3
mg/kg BW and 0.13 mg/kg BW, respectively.
As far as the mechanism of action is concerned, in the light of the
obtained results, it can be speculated that Calotropis gigantea activity
could be due to enhancement of peripheral metabolism of glucose.
There was considerable fall in fasting blood glucose (FBG) in
diabetic rats treated with Caloptropis gigantea leaves alone or
Sphaeranthus indicus alone. The effect was more with Sphaeranthus
indicus. But the effect of the two plants in combination was more than

156
that with either of the plants alone. In conclusion it can be stated that the
two plants Calotropis gigantea and Sphaeranthus indicus, have
synergistic effect when given together. They have a strong anti-
hyperglycemic and anti-hyperlipidemic effect.
In conclusion it appears that the water extract of combination of
Calotropis gigantea plus Sphaeranthus indicus has got good
hypoglycemic and hypolipidemic effect and also corrects complications
associated with diabetes such as retinopathy, nephropathy, neuropathy
and musculopathy.
The antioxidant, antibacterial and muscle relaxant activities of
Calotropis gigantea from methanolic, ethanolic and aqueous extracts
were studied and compared to each other. Extract of Calotropis gigantea
had a slower onset of action and lesser degree of muscle relaxant
activity.
Further, the active constituents responsible for antihyperglycemic,
muscle relaxant, antioxidant and antibacterial activities can be isolated
from the plant extracts and the structure may be elucidated. The
mechanism of action and clinical trials may be carried out in future which
may be useful for the society in the management of diabetes,
hepatotoxicity and related disorders. Further studies to identify the active
constituents of Calotropis gigantea and Sphaeranthus indicus and their
mechanism of action are in progress. Extensive research is needed to

157
corroborate the same beneficial effects and to discuss the underlying
mechanism involved in the above findings to eradicate the diabetes.

158
8. REFERENCE

159
8. REFERENCE
1. Adak M, Gupta JK. Nepal Med Coll J. 2006; 3: 156.
2. Addae-Menzah I and Munenger RW. Fitoterapia. 1989; 60: 359.
3. Aghaskar. Medicinal Plant of Bombay Presidency Scientific
Publication, India. 48-49.
4. Ajay KK, Lokanatha RMK, Umesha KB. Evaluation of antibacterial
activity of 3, 5- dicyano-4, 6-diaryl-4- ethoxycarbonyl-piperid-2-ones,
Journal of Pharmaceutical and Biomedical Analysis. 2003; 27: 837-
840.
5. Alam MA, Habib MR, Nikkon R, Rahman M, Karim MR.
Antimicrobial activity of akanda (Calotropis gigantea L.) on some
pathogenic bacteria. Bangladesh J Sci Ind Res. 2008; 43: 397-404.
6. Ali M, Gupta J. New pentacyclic triterpenic esters from the roots of
Calotropis procera, Indian J Chem. 1999; 38: 877-881.
7. American Diabetes Association. Screening for type II diabetes.
Diabetes Care. 1998; 21(1): S20-S31.
8. Amos AF, McCarty DJ, Zimmet P. The rising global burden of
diabetes and its complications: Estimates and projections to the
year 2010. Diabetic Medicine. 1997; 14: 51-85.

160
9. Atta-ur-Rahman and Khurshid Zaman. Medicinal plants with
hypoglycaemic Activity.Journal of Ethnpharmacology. 1989; 1: 26-
55.
10. Bajaj JS, Madan R. Diabetes in tropics and developing
countries.International Diabetic Federation (IDF) bull. 1993; 2: 5-6.
11. Chitme HR, Chandra R, Kaushik S. Evaluation of antipyretic
activity of Calotropis gigantea (Asclepiadaceae) in experimental
animals. Phytotherapy Research. 2005; 19: 454-456.
12. Chitme HR, Chandra M, Kaushik S, J Pharma Pharma Sci. (2004);
7(1): 70.
13. Chitme HR, Chandra M, Kaushik S. Phytother Res. 2005; 19: 454.
14. Chopra J and S. Rajasekharan, Indian 13. Gupta M, Mazumdar UK,
Sivakumar T, Pharmacological Aspects, World journal of
pharmaceutical research. 1958; 55: 87-95
15. Choudhary NK, Jha AK, Sharma S, Goyal S, Dwivedi J. Anti-
diabetic potential of chloroform extract of flower of Calotropis
gigantea: an in vitro and in vivo study. International Journal of Green
Pharmacy. 2011; 4: 296-301.
16. Das BB, Rasraj Mahodadhi, Khemraj Shri Krishnadas Prakashan,
Bombay. 1996.

161
17. David MN. The pathophysiology of diabetes complications: How
much does the glucose hypothesis explain? Ann. Intern. Med. 1996;
174: 286-289.
18. Deshmukh PT, Frenandes J, Atul A, Toppo E. J Ethnopharmacol.
2009; 125(1): 178.
19. Dixit VP and Joshi S. Antiatherrosclerotic effects of alfalfa meal
injection in chicks: A biochemical evaluation. Ind. J. Physiol.
Pharmacy 1985; 29: 47-50.
20. Drury M. I. Diabetes Mellitus second edition. Blackwell Scientific
Publication Oxford London. Edinburgh. 1986; 68-78.
21. Ferrington. Clinical Materia Medica B.Jain Publication Pvt. Ltd. New
Delhi. Ganapathm Kalyani Publisher. Ludhiyana, India. 1990; 347 -
353.
22. Ghosh. Comparative Materia Medica Hannemann Publication
company pvt. Ltd. Colicata, India.
23. Hiroshi O, Nobuko and Kunio V. Assay for lipid peroxides in animal
tissues by thiobarbituric acid reaction. Anal. Biochem. 1979; 5: 351-
358.
24. Hussain Hema. Reversal of diabetic retinopathy in streptozotocin
induced diabetic rats using traditional Indian anti-diabetic plant,
Azadirachta indica (L). Ind. J. Clin. Biochem. 2002; 17(2): 115-123.
25. India Today ‘Striking the young’. October 6, 2003; 15-22.

162
26. Kiritikar KR and Basu BD. Indian Medicinal Plant 1, 2 and 3.
Antihepatotoxic activity of crude drug: Basu Allahabad. 1933; 105
(2): 109-118.
27. Klimes I, Sebokova E, Gasperikova D, Mitkova A, Kuklova S, Bohov
P., Endocr Regul. 1998; 32(3): 115.
28. Kokate CK, Practical pharmacognosy. 1994; 3: 107-109.
29. Kulkarni SK. Handbook of experimental Pharmacology. New Delhi:
Vallabh Prakashan. 1999; 3.
30. Lodhi G, Singh HK, Pant KK, Hussain Z. Acta Pharma. 2009; 59(1):
89.
31. Luo J, Fort DM, Carlson TJ, Noamesi BK, nii-Amon-Kotei D, King S.
R. Diabet Med. 1998; 15(5): 367
32. Malhotra RP. Compendium of Indian medicinal plants, Vol. 2.
Central Drug Research Institute, Lucknow and information
directorate: CSIR New Delhi. 1991; 137-138.
33. Mueen Ahmed KK, Rana AC, Dixit VK. Calotropis Species
(Ascelpediaceae) – A Comprehensive Review. Phcog. Mag. 2005; 2
Suppl 1: 48.
34. Mueen Ahmed KK, Rana AC, Dixit VK. Free radical scavenging
activity of Calotropis species. Indian Drugs 2003; 40 Suppl 11: 54.

163
35. Nagarajan, S. Jain, HC. Aulakh, GS. Indigenous plants used in the
control of Diabetes.Cultivation and Utilization of Medicinal Plants
CSIR Jammu Tawi. 1982; 589-602.
36. Nanu R Rathod, Havagiray R Chitme, Raghuveer Irchhaiya and
Ramesh Chandra. Hypoglycemic effect of Calotropis gigantea Linn
leaves and flowers in streptozotocine induced diabetic rats. Oman
Med. J. 2011; 26(2): 104-108.
37. Okunji CO, Okeke CN, Gugnani HC, Iwu MM, An antifungal saponin
from fruit pulp of Dracaena manni, International Journal of Crude
Drug Research. 1990; 28: 193-199.
38. Oudhia. a, b, c, d.1999.
39. Oudhia and Dixit. Weeds News. 1994; 1 (2): 19-21.
40. Ramachandran K, Subramanian B, Scarlet G. Coccinia grandis, little
known tropical drug plant. Econ. Bot, Springer. 1983; 73: 80-82.
41. Rastogi and Mehrotra. Compendium of Indian Medicinal Plants,
Lucknow, New Delhi. 1991; 70-73.
42. Rathod NR, Raghuveer I, Chitme HR, Chandra R. Indian J Pharm
Sci. 2009; 71(6): 615.
43. Reinhold JG and Reiner M. Standard methods in clinical chemistry
Vol. 1. New York: Academic press. 1953; 88-89.

164
44. Rios JL, Recio MC, Vilar A, Screening methods for natural products
with antimicrobial activity: A review of literature, Journal of
Ethnopharmacology.1988; 23: 127-149.
45. Roy RK, Ray NM, Das AK. skeletal muscle relaxant effect of
Chonemorpha macrophylla in experimental animals. Indian. J.
Pharmacol 2005; 37: 116‐119.
46. Roy S, Sehgal R, Padhy BM, Kumar VL. J Ethnopharmacol. 2005;
102(3): 470-473.
47. Sadhu SK, Okuyama E, Fujumoto H and Ishibashi M. Separartion of
leucas, aspara from a medicinal plant of Bangladesh,guided by
prostaglandin inhibitory and anti oxidant activities. 2003.
48. Saratha V, Subramanian S, Sivakumar S, Evaluation of wound
healing potential of Calotropis gigantea latex studied on excision
wounds in experimental animals, Med Chem Res. 2009; DOI:
10.1007/s00044-009- 9240-6.
49. Sastry CST and Kavathekar KY. Plants for reclamation of
wastelands. Publication and Information Directorate, CSIR, New
Delhiscince news. 1991; 175-179.
50. Sen S, Sahu NP, Mahato SB, Phytochemistry. 1992; 8: 2919
51. Shukla R, Sharma SB, Puri D, Prabhu KM and Murthy PS. Medicinal
plants for treatment of diabetes mellitus. Ind. J. Clin. Biochem. 2000;
15: 169-177.

165
52. Singh U, Wadhwani AM and Johri BM. Dictionary of Economic
Plants of India. Indian Council of Agricultural Research, New Delhi.
1999; 38-39.
53. Swanston-flatt SK, Day C, Bailey CJ, Flatt PR. Diabetologia. 1990;
33(8): 462-4.
54. Taft. P. Diabetes Mellitus, A Guide to Treatment ADIS Health
Science Press, Australia. 1920; 1-19.
55. Tagg TR, Dajani AS, Wannamaker LW, Bacteriocin of Gram positive
bacteria, Bacteriological Reviews.1976; 40: 722-756.
56. Thakur S, Das P, Itoh T, Kazunori Imai, Taro M, Phytochemistry.
1984; 9: 2085.
57. The Hindustan Times ‘Treat diabetes as priority’ September 24,
2004.
58. The Week, Managing Diabetes. November 16, 2003; 13.
59. Thitima L, Somyot S. J Nat Prod. 2006; 8: 1249.
60. Trovato T, Forestie RI, Lauk L, Barbera R, Monforter MT and Galati
EM. Plant Med.,Phytother. 1993; 26: 300.
61. Usha K, Singh B, Praseetha P, Deepa N, Agarwal DK, Agarwal R,
Nagaraja A. Antifungal activity of Datura stramonium, Calotropis
gigantea and Azadirachta indica against Fusarium mangiferae and
floral malformation in mango. European Journal of Plant Pathology.
2009; 124: 637-657.

166
62. Vamis MLM, Karkis S, Sambathkumar R, L Dhanukar KA, Kulkarni
RA, Rege NN. Pharmacology of medicinal plants and national
products. Indian J Pharmacol. 2000; 32: 81.
63. Venkatesh S, Reddy GD, ReddyYS, Satayavathy D, Reddy BM.
Fitoterapia. 2004; 75: 364.
64. Wang Z, Wang M, Mei W, Han Z, Dai H, A New Cytotoxic
Pregnanone from Calotropis gigantea, Molecules. 2008; 13: 3033-
3039.
65. Warnier, et.al. Indian Medicinal Plants Orient longman Chennai,
India.1996; 341-345.
66. World Health Organization. Prevention of diabetes mellitus:
Technical Report Series. WHO. Geneva. 1994; 844-848.
67. Yusuf M, Chowdhury JU, Wahab MA, Begum J. Medicinal Plant of
Bangladesh. Inflammatory activities of Acalypha fruticasa. Nig. J.
1994; 3: 234-235.

167
9. PUBLICATIONS

168
9. PUBLICATIONS
1. “Impact of Calotropis gigantea leaves via different routes of
administration in normal and alloxan induced diabetic rats”, Deepak
Teotia, S. P. Chakrabarti, S. S. Ajay. International Journal of
Scientific and Research Publications, Volume 3, Issue 5, May 2013,
ISSN 2250-3153.
2. “Evaluation of Calotropis gigantea (l.) And S. indicus on glycemia
and lipidemia in sterptozotocin induced diabetic rats”, Deepak
Teotia, S. P. Chakrabarti, S. S. Ajay. Int. J. Pharm. Sci. Rev. Res.,
21(1), Jul – Aug 2013; n° 28, 164-168, ISSN 0976 – 044X.
3. “Ethnopharmacological evaluation of Calotropis gigantea”, Vaibhav
and Deepak Teotia et al. World journal of pharmaceutical research.
Aug 2013; vol 2, issue 5: 1826 – 1839.
The published papers are enclosed.

169
International Journal of Scientific and Research Publications, Volume 3, Issue 5, May 2013 1 ISSN 2250-3153
Impact of Calotropis Gigantea Leaves via Different Routes of Administration in Normal and Alloxan
Induced Diabetic Rats
Deepak Teotia*, S. P. Chakrabarti**, S. S. Ajay***
* School of Pharmacy, VIshveshwariya Institute of Medical Science, Greater Noida, Gautam Budha Nagar, Pin- 203207, India ** IMT Pharmacy College, Puri, New Nabakalabara Road, Gopalpur, Puri, , Pin- 752001, (Orisaa), India. *** School of Pharmacy, VIshveshwariya Institute of Medical Science, Greater Noida, Gautam Budha Nagar, Pin- 203207, India
Abstract- The present study was carried out to evaluate the anti-diabetic activity of water extract of Calotropis gigantea leaves in alloxan induced diabetic rats for 0, 20, 60, 120, 240, 360 minutes. The water extract at the dose (0.7 gm/kg) exhibited significant anti-hyperglycemic activity. Oral and intraperitoneally administration of the plant produced significant hypoglycemic effect in normal as well as hyperglycemic rats. The water extract of Calotripis gigantea leaves showed hypoglycemic effect in normoglycemic and hyperglycemic rats after both oral and intraperitoneal administration. The effect could be comparable to that of well-known hypoglycemic compound like metformin and glibenclamide used at 11.3 and 0.13 mg/kg, respectively. Index Terms- Calotropis gigantea; Asclepiadaceae; Alloxan monohydrate ; Route of administration
I. INTRODUCTION Diabetes mellitus is an endocrine disorder characterized by hyperglycemic effecting nearly 10% of the population all over the world. Insulin and oral hypoglycemic agents like sulfonylureas and biguanides are still the major players in the management of the disease. However, complete cure of the disease has been eluding physicians for centuries and the quest for the development of more effective anti-diabetic agents is pursued relentlessly. Many herbal products, including several metals and minerals have been described for the cure of diabetes mellitus in ancient literature. Herbal preparations alone or in combination with oral hypoglycemic agents sometimes produce a good therapeutic response in some resistant cases where modern medicines alone fail. There is increasing demand by patients to use natural products with anti-diabetic activity due to side effect associated with the use of insulin and oral hypoglycemic agents [1]. The World Health Organization has also recommended the evaluation of the effectiveness of plants in condition where there is a lack of safe made drugs.
Currently available treatment for this disorder is far from satisfactory and expensive. Calotropis gigantea leaves (Family : Asclepiadaceae) is a small tree variety found throughout India. It is commonly called Swallow –
Wort. Leaves contain the cardiac glycoside; Calotropin; Uscharin; Calotoxin; Calactin; Uscharidin and gigantin [2-3-4]. It is used widely used for healing of wounds; anthelmintic; expectorant; useful in leprosy scabies ring warm of the scalp; piles, eruptions on the body; asthma;

170
prevention of insulin resistance [5], hepatoprotective [6], anti-diarrhoeal [6], antipyretic and analgesic [7-8], anti-inflammatory[9] and wound healing activity [10]. The calotropin Uscharin and gigantin show digitalis – like action on the heart.
The preliminary phytochemical studies reveal the presence of flavonoids; glycosides; alkaloids; tannins. The focus of the present study is to evaluate water extract of Calotropis gigantea leaves material at various doses in normal and alloxan induced diabetic rats. However, no scientific data are available regarding the effect of water extract of Calotropis gigantea leaves on blood glucose level. The present study is undertaken to explore the effect of water extract of Calotropis gigantea leaves on the blood glucose level of experimental animals and to determine the probable mechanism of action. The effect of water extract of Calotropis gigantea leaves on fasting blood sugar level has been evaluated as compared to the standard drug glibenclamide, both in normal and diabetic albino rats. The effect of Calotropis gigantea extract on glucose uptake by rat hemi-diaphragm and the glycogen content of the liver, skeletal muscle and cardiac muscle are evaluated to study its probable mechanism of action as a hypoglycemic agent.
II. EXPERIMENTAL 2.1. Material required:
Alloxan monohydrate was purchased from Sigma Chemical
Co St Louis, USA. All other chemicals were obtained from local sources and were analytical grade. Calotropis gigantea was collected from the forest area of Ghaziabad, U.P., India in March 2008. The plants was identified from the School of Pharmacy, Vishveshwariya Institute of Medical Science, Greater Noida, Gautam Budha, Nagar, India. They were assigned voucher specimen Ref. VIMS/CONSULT/2009/02/10. 2.2. Methods: 2.2.1. Preparation of water extract:
The leaves of Calotropis gigantea was air dried and powdered in a grinder. 300g of Powder mixture of the plant parts was extracted overnight with 360 ml of water with magnetic stirring in cold room (4oC). The water extract was separated and the residue was re-extracted with water. The water extract was concentrated to produce semisolid mass and dried in lyophilizer (Mini Lyotrap, Serial No J8199/5, LET Scientific Ltd UK).

171
International Journal of Scientific and Research Publications, Volume 3, Issue 5, May 2013 2 ISSN 2250-3153
2.2,2 Preliminary phytochemical screening:
The extracts were subjected to preliminary screening for various active phytochemical constituents [11]. 2.2,3. Animal and experimental set-up:
Colony bred, healthy male wistar albino rats of either sex weighing 150 – 200 g were taken for the study. The animals fed on standard laboratory diet with water ad libitum and housed at room temperature. The rats were kept fasting overnight with free access to water during the experiment in the ambience. The animals were divided into eight groups of six animals each. 1 ml of blood was taken from the orbital sinus of each rat with the help of a capillary tube for the estimation of blood sugar. The institutional Ethical Committee approved all experiment protocols. 2.2.4. Hypoglycemic effect in normal rats [12-13]:
Groups of six rats each (fasted for18 hrs) received 10 ml/kg infusion, intragastrically or intraperitoneally (i.p.) Blood samples were drawn by puncture from the tail immediately before administration in the time intervals of 20, 60, 120, 240 and 360 min later. Control group received an equal volume (10 ml/ kg) of normal saline, glibenclamide (0.13 mg/kg) and metformin (11.3 mg/kg), calculated on the basis of the daily doses [14]. 2.2.5. Hypoglycemic effect on alloxan-diabetic rats [15]:
Chronically hyperglycemic rats were obtained by i.p. injection of 150 mg/kg of alloxan dissolved in distilled water
[16 ]. After 8 hrs administration, the hyper-glycemic rats were selected (plasma glucose level 2-2.8 g/L) and used in the experiments. The same experimental protocol described above was then adopted. 2.2.6. Glucose tolerance test (GTT) in rats [17-18]:
A polyethylene cannula was injected into the jugular vein under ethyl carbonate anesthesia. Another catheter was injected into right carotid. All rats received orally 10 ml/kg of 25% glucose solution. One group of animals received the plant infusion (10 ml/kg) through the venous catheter, while the control group received normal saline. Blood samples (0.2 ml) were taken from the carotid catheter at time intervals of 5, 10, 20, 30, 40, 50 and 60 min after injection. The coefficient of glucose assimilation (KG) was determined with the formula.
KG = (log C - log C/2) t½= 0.639 t½
Where : C = glycaemia (g/L); t½: Time for the blood glucose concentration C/2. 2.2.7. Statistical analysis:
Results are reported as mean ± SEM statistical analysis was carried out using analysis of variance (Anova). The difference of the means was calculated using Newman – Keuls test. P values of 0.05 or less were taken as significant.
Table 1.
Effect water extract of Calotropis gigantea leaves on plasma glucose levels after intragastric (p.o) and intraperitoneal (i.p.)
administration to normoglycaemic rats.
Treatment Route Plasma glucose (g/L) at time ( min) after treatment 0 20 60 120 240 360
Control(Saline.10 ml/kg) p.o. 0.99±0.05 0.99±0.08 0.98±0.09 0.90±0.16 0.95±0.06 0.96±0.07 i.p. 0.98±0.04 0.96±0.06 0.89±0.08 0.93±0.09 0.93±0.08 0.94±0.08
Glibenclamide(0.13 mg/kg) p.o. 0.96±0.09` 0.69±0.11* 0.46±0.07++ 0.57±0.07+ 0.73±0.06 0.83±0.05 i.p. 0.98±0.08 0.73±0.1* 0.48±0.06++ 0.63±0.05+ 0.75±0.06* 0.93±0.13
Metformin(11.3 mg/kg) p.o. 0.99±0.05 0.73±0.06* 0.65±0.1* 0.54±0.08+ 0.75±0.06* 0.93±0.13 i.p. 0.93±0.04 0.79±0.05* 0.57±0.06+ 0.71±0.05* 0.74±0.05 0.80±0.05
C. gigantea(0.7 g/kg) p.o. 0.93±0.05 0.59±0.06++ 0.58±0.14++ 0.51±0.07++ 0.83±0.13 1.02±0.06 i.p. 0.98±0.07 0.68±0.06++ 0.56±0.22++ 0.54±0.19++ 0.63±0.09+ 0.67±0.08+
avalues are mean ± SEM, n= 8; *p< 0.05; +p<0.01; ++p<0.001 vs. Control; Anova and Newman - Keuls test.

172
International Journal of Scientific and Research Publications, Volume 3, Issue 5, May 2013 3 ISSN 2250-3153
Table 2.
Plasma insulin in normoglycemic rats after intragastric (p.o.) and intraperitoneal (i.p.) administration water extract
of Calotropis gigantea leaves.
Values are mean ± SEM, n= 8; *p< 0.01; ++p<0.001 vs. Control; Anova and Newman - Keuls test.
Table 3.
Effect water extract of Calotropis gigantea leaves on Plasma glucose levels after intragastric and intraperitoneal (i.p.) administration to alloxan-diabetic rats.
Treatment Route Plasma glucose (g/L) at time ( min) after treatment
0 20 60 120 240 360
Control(Saline.10 ml/kg)
p.o. 2.82±0.2 2.57±0.14 2.14±0.72 2.20±0.45 2.35±0.39 3.00±0.4
8 i.p. 2.71±0.2 2.61±0.18 2.59±0.65 2.15±0.5 2.28±0.49 2.92±0.5
1 Glibenclamide(
0.13 mg/kg) p.o. 2.88±0. 2 2.15±0.26 1.44±0.39+ 0.91±0.08++ 1.44±0.22++ 1.70±0.3
4+ i.p. 3.01±0.03 2.36±0.35 1.21±0.47* 0.88±0.11* 1.44±0.22* 1.70±0.34
Metformin(11.3 mg/kg)
p.o. 2.96±0.1 2.66±0.2 1.21±0.09+ 0.99±0.06+ 1.37±0.25+ 2.00±0.47
i.p. 3.01±0.09 1.30±0.4 0.74±0.41* 1.63±0.25* 1.50±0.35* 1.80±0.30*
C. gigantea(0.7 g/kg)
p.o. 2.90±0.08 2.02±0.53* 1.05±0.16++ 1.01±0.07++ 1.03±0.12++ 0.92±0.20+yx
i.p. 2.86±0.3 1.74±0.25+ 1.60±0.22+ 0.79±0.3++ 1.189±0.21++
1.32±0.19++bx
Values are mean ± SEM, n= 8; *p< 0.05; +p<0.01; ++p< 0.001 vs. control; bp<0.05 vs. glibenclamide; xp<0.05; yp<0.01 vs. metformin; Anova and Newman - Keuls test. Ajay1
Treatment Route Insulinmia (12.42 µlU/mL) at time ( min) after treatment 0 20 60 120 240 360
Control(Saline.10 ml/kg) p.o. 58.08±4.4
1 68.56±10.2
6 63.11±8.4
2 56.64±
11 60.06±10 72.32±6.16
i.p. 88.88±14.96
71.89±8.25
60.41±7.89
61.57±9.15
67.27±8.01
84.94±7.91
C. gigantea(0.7 g/kg) p.o. 82.06±14.3
5 68.96±8.5
2 54.14±9.5
6 51.88±3
.03 63.17±19.
04 75.03±19.
42 i.p. 64.22±8.56 78.07±12.
62 90.19±7.1
6* 73.02±1
6.9 121.42±10
.01++ 113.37±20
.52+

173
International Journal of Scientific and Research Publications, Volume 3, Issue 5, May 2013 4 ISSN 2250-3153
Table 4.
Blood glucose in glucose loaded (0.25 g/kg) rats before and after the intravenous administration water extract of
Calotropis gigantea leaves.
Values are mean ± SEM, n= 5; *p< 0.05; +p<0.01; ++p<0.001 vs. Control; Anova and Newman - Keuls test.
III. RESULT AND DISCUSSION The infusion of Calotropis gigantea exhibited a remarkable
hypoglycemic action 20 min after oral and i.p. administration to normal rats. (Table 1.). Blood glucose level reached a mean value of 0.59 and 0.68 g/L, respectively as compared to 0.99 g/L and 0.96g/L. respectively obtained in the control group. The lowest hypoglycemic effect was observed after 2 hr of administration. After 4 hrs of administration, the blood glucose level reached nearly to the initial glycemic values for orally treated animals, while i.p. administration still showed hypoglycemic effect even after 6 hr. Calotropis gigantea hypoglycemic effect was comparable and sometimes higher than that obtained with 0.13 mg/kg of glibenclamide or 11.3 mg/kg of metformin. After i.p. administration, the variation in insulin plasma levels showed an opposite trend to that of glucose (Table 2). The increase became significant after 1 hr of administration and persisted for at least 6 hr. Plasma insulin reached a maximum level (12.42 µlU/mL) 4hr after i.p. administration. On the other hand, no variation in blood insulin level was found in normal rats orally treated with the water extract of Calotropis gigantea leaves. When compared with control, Calotropis gigantea (Table 3) significantly reduced the blood glucose levels in diabetic rats. The maximum decrease observed 2 hr after the administration in plasma glucose level recorded as 1.01 g/L (-69.96%) and 0.79 g/L (-53.29%), respectively after oral and i.p. treatment. In a glucose tolerance test, intravenous treatment with Calotropis gigantea plasma glucose level significantly reduced at time intervals of 40, 50 and 60 min as compared to plasma glucose level induced in control by a glucose load administration (Table 4). Glycemic values returned to basal levels more rapidly than in control group. The coefficient of glucose assimilation (KG) showed significant increase in treated rats compared to control (8.17×10-3 vs 6.96×10-3).
IV. CONCLUSION
The Calotropis gigantea showed hypoglycemic effect in normoglycemic and hyperglycemic rats after both oral and intraperitoneal administration. The effect could be comparable to that of well-known hypoglycemic compound like metformin and glibenclamide [19] used at 11.3 and 0.13 mg/kg, respectively. As far as the mechanism of action is concerned, in the light of the obtained results it can be speculated that Calotropis gigantea activity could be due to enhancement of peripheral metabolism of glucose. An increase of insulin release can not be excluded. Further studies to identify the active constituents of Calotropis gigantea and their mechanism of action are in progress.
REFERENCES [1] Luo J, Fort DM, Carlson TJ, Noamesi BK, nii-A-Kotei D, King SR, Diabet
Med., 15(5), 367 (1998). [2] Thakur S, Das P, Itoh T. Kazunori Imai, Taro M, Phytochemistry, 9, 2085
(1984). [3] Thitima L, Somyot S, J Nat Prod., 8, 1249 (2006). [4] Sen S, Sahu NP, Mahato SB, Phytochemistry, 8, 2919 (1992). [5] Rathod NR, Raghuveer I, Chitme HR, Chandra R, Indian J Pharm Sci.,
71(6), 615 (2009). [6] Lodhi G, Singh HK, Pant KK, Hussain Z, Acta Pharma., 59(1), 89 (2009). [7] Chitme HR, Chandra M, Kaushik S, J Pharma Pharma Sci., 7(1), 70 (2004). [8] Chitme HR, Chandra M, Kaushik S, Phytother Res., 19, 454 (2005). [9] Adak M, Gupta JK, Nepal Med Coll J., 3, 156 (2006). [10] Deshmukh PT, Frenandes J, Atul A, Toppo E, J Ethnopharmacol, 125(1),
178 (2009). [11] Kokate CK, Practical pharmacognosy, 3rd ed, pp., 107-109 (1994). [12] Swaston-Flatt SK, Day C, Bailey CJ, Flatt PR., 33, 462 (1990). [13] Klimes II, I, Sebokova E, Gasperikova D, Mitkova A, Kuklova S, Bohov P.,
Endocr Regul, 32(3), 115 (1998). [14] I. Addae-Menzah and R. W. Munenger, Fitoterapia, 60, 359 (1989) [15] Roy S, Sehgal R, Padhy BM, Kumar VL, J Ethnoharmacol, 102(3), 470
(2005). [16] T. Trovato, R.I. Forestie, L. lauk, R. Barbera, M.T. Monforter and E.M.
Galati, Plant Med.,Phytother., 26, 300 (1993). [17] Venkatesh S, Reddy GD, ReddyYS, Satayavathy D, Reddy BM, Fitoterapia,
75, 364 (2004).
Treatment Blood glucose (g/L) at time ( min) after load 0 5 10 20 30 40 50 60
Control(0.25g/kg glucose)
0.99±0.08 1.26±0.08 1.47±0.11 1.59±0.1
4 1.71±0.09 1.69±0.11 1.46±0.08 1.33±0.07
C. gigantea(0.7 g/kg) 0.98±0.09 1.15±0.1 1.35±0.06 1.48±0.1 1.51±0.08* 1.31±0.1+ 1.25±0.11
+ 1.16±0.13++

174
International Journal of Scientific and Research Publications, Volume 3, Issue 5, May 2013 5 ISSN 2250-3153
[18] Tuomilehto J, Lindstrom J, Eriksson JG, Valle TT, Hamalainen H,
llanne-Parikka P, Keinanen- Kiukaanniemi S, Laakso M, Louheranta A, Rastas M., Salminen V, Uusitupa M, N Engl J Med., 344, 1343 (2001).
[19] Tuzun S, Girgin FK, Sozmen EY, Exp Toxicol Pathol., 51, 431 (1999).
[20] Deb L, Durra A, Int J Green Pharm., 1, 7-28 (2006). [21] Lu YX, Zhang Q, Li J, Sun YX, Wang LY, Cheng WM, Am J
Chin Med., 38, 713 (2010). [22] Yamamoto H, Uchigata Y, Okamoto H, Nature, 294, 284 (1981).
AUTHORS First Author – Deepak Teotia , M.Pharm, School of Pharmacy, VIshveshwariya Institute of Medical Science, Greater Noida, Gautam Budha Nagar, Pin- 203207, India,
Second Author – S. P. Chakrabarti, PhD M.Pharm, IMT Pharmacy College, Puri, New Nabakalabara Road, Gopalpur, Puri, , Pin- 752001, (Orisaa), India. Third Author – S. S. Ajay, PhD M.Pharm, School of Pharmacy, VIshveshwariya Institute of Medical Science, Greater Noida, Gautam Budha Nagar, Pin- 203207, India, Correspondence Author – Deepak Teotia, School of Pharmacy, VIshveshwariya Institute of Medical Science, Greater Noida, Gautam Budha Nagar, Pin- 203207, (U.P.), India, Tel - +91 9990049211,9410491620 Email: [email protected]

175
Int. J. Pharm. Sci. Rev. Res., 21(1), Jul – Aug 2013; n° 28, 164-168 ISSN 0976 – 044X
Research Article
Evaluation of Calotropis Gigantea (l.) and S. Indicus on Glycemia and Lipidemia in Sterptozotocin induced Diabetic Rats
Deepak Teotia1*, S. P. Chakrabarti2, S.S. Ajay3
1*Vishveshwaraya School of Pharmacy, Greater Noida, Gautam Budha Nagar, UP, India. 2IMT Pharmacy College Puri, New Nabakalabara Road, Gopalpur, Puri, Orisaa, India.
3Vishveshwaraya School of Pharmacy, Greater Noida, Gautam Budha Nagar, UP, India. *Corresponding author’s E-mail: [email protected]
Accepted on: 15-04-2013; Finalized on: 30-06-2013.
ABSTRACT In Ayurvedic system of medicine in India, not only extracts of one plant or the other but also a combination of plant extracts are used for the treatment of diabetes mellitus. The present paper reports the combined effect of Calotropis gigantea and S. indicus known to be useful for the treatment of diabetes in Ayurveda on the fasting blood sugar, glucose tolerance and lipid profile of Streptozotocin (STZ) induced albino rats. 300mg of water extract of the mixture of dried powdered leaves of Calotropis gigantea leaves and S.
indicus in equal proportions was given once daily for 8 weeks. After 8 weeks of treatment of Streptozotocin (STZ) diabetic rats, the fasting blood sugar came down to almost normal value and improvement in glucose tolerance and serum lipid profile were also observed. Keywords: Calotropis gigantea leaves, S. Indicus, Streptozotocin (STZ), type 2 diabetes.
INTRODUCTION Diabetes, a metabolic disorder involving high blood sugar levels due to the non functioning of a key hormone called insulin, has been on the risk across the world. Diabetes mellitus(DM) is a metabolic disorder characterized by hyperglycemia resulting from defects in insulin secretion, insulin action or both.1 The risk of diabetic complications, particularly cardiovascular diseases (CVD) peripheral vascular disease (PVD).2 Complications such as coronary artery disease (CAD), stroke, neuropathy, renal failure, retinopathy amputations, and blindness etc are known to be associated with DM.3 Insulin and various types of hypoglycemic agents such as biguanides and sulfonylureas including some of the recently developed ones are available for the treatment of diabetes. But none are ideal in treatment due to the toxic side effect and sometimes diminution in response after prolonged use.3-4 The disadvantages of the presently available drugs are that they have to be given throughout the life and produce side effect.4 A variety of plant preparations have been mentioned in Ayurveda and other indigenous systems of medicine, which are claimed to be useful in the treatment of diabetes mellitus.5 World Health Organization (WHO) has suggested the evaluation of the potential of plants as effective therapeutic agents, especially in areas where we lack safe modern drugs.6 In the ongoing search for more effective and safer drugs attention is being paid to new and safe drugs.6-8 There are many studies on Calotropis
gigantea which show that it exhibits anti-ulcer, anti-syphilis and anti-diabetic activities. Some of the plants useful for the treatment of diabetes mellitus including those from which some active constituents were isolated have been recently revived by Shukala et. Al.9 Reported that Calotropis gigantea
possesses not only anti-hyperglycemic effect but also hypolipidemic effect.10-11 S. indicus is also known to be a drug useful for the treatment of diabetes mellitus.12 In this paper the combined effect of water extract of a mixture Calotropis gigantea leaves and S. indicus in streptozotocin (STZ) induced diabetic in rats is reported. MATERIALS AND METHODS Calotropis gigantea was collected from the forest area of Ghaziabad, U.P., India and S. Indicus was obtained from the market of Ghaziabad, U.P and both plants were identified from the School of Pharmacy, Vishveshwariya Institute of Medical Science, Greater Noida, Gautam Budha, Nagar, U.P., India. They were assigned voucher specimen Ref. VIMS/CONSULT/2009/02/10 and Ref. VIMS/CONSULT/2009/02/11. The leaves of Calotropis
gigantea leaves and S. indicus were air dried and powdered in a grinder and mixed in equal proportions. Preparation of water extract 300 gm of powdered mixture of the two plant parts was extracted overnight with 360 ml of water with magnetic stirring in cold room (4oC). The water extract was separated and the residue was re-extracted with water. The combined water extract was concentrated in lyophilizer. Animals Wistar albino rats were obtained from R.V. Northland Institute, Greater Noida, Gautam Budha, Nagar, U.P., India, clearance is taken from animal ethics committee (IEC). Adult rats of either sex weighing between 150-200 g were selected for the study. The animals were acclimatized to laboratory conditions and divided into various groups. Animals were housed and kept on the light and dark cycle throughout.
International Journal of Pharmaceutical Sciences Review and
Research 164

176
Int. J. Pharm. Sci. Rev. Res., 21(1), Jul – Aug 2013; n° 28, 164-168 ISSN 0976 – 044X Induction of diabetes and associated neuropathy Healthy adult albino wistar rats of both sex weighing between 150-200 gm were obtained from R.V. Northland Institute, Greater Noida, Gautam Budha, Nagar, U.P., India, and used in this study. The animals were fed on a pellet diet (Hindustan Lever, India) and water provided ad libitum. Diabetes was experimentally induced to produce diabetic neuropathy.13 Sorbitol induced disfunction of inositol / metabolites leading to neuron-infraction by causing microangiopathy of vasa nervosum it deceases blood flow to nerves. Overnight fasting animals were injected with streptozotocin (STZ) 60 mg / kg dissolved in 3 mM citrate buffer (pH 4.5) intraperitoneally (i. p.). After 10 days only those rats which showed plasma glucose level > 300 mg / dl were classified as diabetic and were included in study as described earlier.14 Animals were divided into three groups of five each. Group1 animals served as healthy controls, while those of the group 2 were untreated diabetic rats. Rats of group 3 were diabetic and treated for 8 weeks with 300 mg of water extract of Calotropis gigantea leaves plus S. indicus.
13-14 Blood samples were collected from overnight fasted rats at 0 and 8 weeks. Blood glucose serum total cholesterol, HDL and LDL cholesterol, triglyceride, and Glycosylated haemoglobin were determined using kits from Randox Mumbai. Total proteins albumin and creatinine in serum were determined by the method of Reinhold. Assay of plasma glucose and albumin and creatinine and total cholesterol, LDL – VLDL and HDL cholesterol and triglycerides were estimated as described earlier. Lipid peroxidation products were estimated as thiobarbituric acid reactive substance (TBARS) in plasma and tissues.15-16 Statistical analysis All the data were statistically evaluated and the significance calculated using student’s test. All the results were expressed as mean ± SD. RESULTS AND DISCUSSION The result obtained with untreated diabetic rats and diabetic rats treated with Calotropis gigantea plus S. indicus on fasting blood glucose and GTT are compared with normal healthy controls and shown in Table 1 and Table 1A. It is seen that treatment with water extract of Calotropis gigantea plus S. Indicus at a dose of 300 mg / kg body weight brought down fasting blood glucose (Table 1), from a higher value of 166.9 ± 25.4 mg / dl to a normal value of 85.4 ± 2.3 mg / dl while in the untreated group the FBG increased from the initial value of 172.2 ± 5.4 to 285.6 ± 42.6 mg / dl. There was considerable fall in FBG in diabetic rats treated with Caloptropis gigantea leaves alone or S. indicus alone. The effect was more with S. indicus. But the effect of the two plants in combination was more than that with either of the plants alone. Similar improvement to normal glucose tolerance was seen (Table 1A). In the diabetic untreated rats the blood sugar was 269.0 ± 92.2 mg / dl even after 2 hrs of glucose load in GTT. But in the Calotropis gigantea plus S. indicus treated rats the 2 hrs blood glucose value was in the
normal range of 75.2 ± 1.0 mg /dl. The fasting (0hr) blood glucose values which were higher in the diabetic animals (160.5 ± 32.1) were brought down to 81.0 ± 3.5 mg / dl, when 300 mg of the extract of the mixture of the two plants was administered for 8 weeks. There was improvement in glucose tolerance in diabetic rats treated alone with either of the plants. The exact mechanism of action of the plant extracts either alone or in combination cannot be stated. However it is possible that these extracts increase blood insulin levels and also stimulate utilization of glucose by liver and extrahepatic tissues. The changes in the lipid profile have also been studied (Table 2). Before treatment the total cholesterol (TC), LDL cholesterol (LDL-C) and TG were higher than in normal animals. After 8 weeks, the TC, LDL-C, LDL-C/HDL-C and TG values were still higher in diabetic untreated animals then in control animals. There was no change in HDL-C in untreated diabetic animals. However in the case of diabetic treated animals, with Calotropis gigantea alone, total cholesterol, LDL cholesterol and LDL-C/HDL-C values returned close to normal values. There was very slight fall in TG values probably because these plants could not show much effect on triglycerols. But further improvement in increase in HDL-C value was seen. With Calotropis
gigantea and S. indicus plus Calotropis gigantea
treatments similar values were obtained. Further there was reduction in TG values also. This shows again that the water extract of the mixture of two plants, which contains less than 300 mg of each of the two plants is as effective as 300 mg of water extract of each of the two plants. Improvement in lipid profile is suggestive of the action of the two plants on enzymes and lipid metabolism. The total proteins, albumin and creatinine in serum, glycosylated hemoglobin in blood and total body weight and weight of kidneys (in the animals killed after the experiment) were also analyzed after 8 weeks of treatment and the values are shown in Table 3 and Table 4. The untreated diabetic animals showed signs of neuropathy e.g. tropic ulcer on tail, slight edema in the paws of the legs. The animals looked lethargic and sickly. All these symptoms disappeared after treatment for 8 weeks with water extract of the two plants Calotropis gigantea and S. indicus. The treatment with water extract was so effective that the above mentioned complications seen in untreated diabetic rats disappeared. The treated diabetic animals showed appearance almost like normal rats. The overall behavior of the rats was normal. In conclusion it can be stated that the two plants Calotropis gigantea and S. indicus, have synergistic effect when given together. They have a strong anti-hyperglycemic and anti-hyperlipidemic effect. In table, only values of with water extract of combination of the two plants are shown. An interesting observation is that glycosylated hemoglobin (HbA1c) decreased to 4.8 ± 0.1 and returned to normal values after 8 weeks of treatment. Glycosylated hemoglobin content rather than FBG is considered as a more reliable index of glycemic control in the management of diabetes mellitus. Return to normal of HbA1c (Table 3) after treatment is a clear indication that

177
Int. J. Pharm. Sci. Rev. Res., 21(1), Jul – Aug 2013; n° 28, 164-168 ISSN 0976 – 044X the diabetic state was well regulated after the treatment of diabetic animals. Serum albumin, total body weight and kidney weight increases in diabetic untreated animals. There was increase in total proteins, serum creatinine and serum acid in diabetic animals. After treatment there was decrease except in total protein. But after treatment the values were closer to the normal value. There was an improvement in the hemoglobin content of the blood also (Table 3). Herbal treatment improves the weight of liver and kidney in diabetic rats fed high fat diet, although it was not completely reversible in liver (Tables 4 and Table 5). Recovery from this type of neuropathy is eluting, although months and
even years may elapse before it happens. This form of neuropathy is often referred to as diabetic myotrophy. When the clinical picture is dominated by deep sensory loss, ataxia and stone of the bladder, with only slight weakness of limbs, the similarity can be heightened by the presence of lancinating pains in the legs, unreactive pupils and neuropathic arthropathy. Loss of nerve fibers is a prominent pathologic finding in the distal symmetric form of neuropathy. Since myelin is formed from the cell membranes of Schwan cells, one may infer that the Schwan cell is a primary target of the pathologic process in this type of diabetic neuropathy.
Table 1: Effect of treatment for 8 weeks with water extract of (300 mg/kg BW) Calotropis gigantea and S. indicus and mixture of the two plants on fasting plasma glucose level in streptozotocin (STZ) diabetic rats.
Plasma glucose ( mg/dl) mean ± S.D. Group 0 Weeks 8 Weeks
Control 99.4 ± 19.5 89.8 ± 5.21
Diabetic untreated 172.2 ± 5.4 285.6 ± 42.6
Diabetic + Calotropis gigantea 164.6 ± 25.0 105.4 ± 26.6
Diabetic + S. indicus 158.6 ± 10.0a 98.2 ± 25.2a
Diabetic + Calotropis gigantea + S. Indicus 166.9 ± 25.4 85.4 ± 2.3
a = p < 0.001; Group of 5 animals were used for each set of experiments; All the data were statistically evaluated and the significance was calculated using students’’- test. All the results were expressed as mean ± S.D. Table 1A: Effect of water extract (300 mg/kg BW.) of Calotropis gigantea and S. indicus and mixture of the two plants on plasma glucose tolerance in diabetic rats after 8 weeks
Blood glucose (mg/dl) mean ± S.D. Group 0 hr 0.5 hr 1 hr 1.5 hr 2 hr
Control 94.3 ± 21.0 140.2 ±11.2 132.6 ±27.3 116.2 ±10.0 102.0 ±12.0
Diabetic untreated 160.5 ±32.1 245.0 ±68.6 273.4 ±89.3 290.6 ±82.6 269.0 ±92.2
Diabetic + Calotropis gigantea 87.9 ±25.6 112.2 ±20.6 114.3 ±15.0 102.0 ±10.3 95.6 ±24.0
Diabetic + S. indicus 82.0 ± 4.2 86.0 ± 4.3 81.0 ± 3.9 80.0 ± 3.2 84.0 ± 3.2
Diabetic + C. gigantea + S. indicus 81.0 ± 3.5 84.0 ± 4.2 86.0 ±3.3 81.0 ±3.6 75.2 ± 1.0
Table 2: Effect of treatment for 8 weeks with water extract of (300 mg/kg BW) Calotropis gigantea and S. indicus and both Calotropis gigantea + S indicus on plasma lipid in diabetic rats
Group
Control Diabetic untreated Diabetic + Calotropis
gigantea Diabetic + S. indicus Diabetic + C. gigantea
+ S. indius
TC ( mg/dl) LDLC ( mg/dl) HDLC LDLC/HDLC (mg/dl) TG mean ± S.D. mean ± S.D. (mg/dl) mean ± S.D. mean ± S.D. (mg/dl) mean ± S.D. 170.3 ± 10.3 78.0 ± 12.2 44.9 ±13.3 1.7 ±0.3 115.6 ± 42.6
250.0 ± 14.9 152.2± 12.6 45.0 ±12.0 3.3 ±0.4 181.8 ±18.8
175.0 ± 12.3 99.7 ±16.8 51.3 ±8.4 1.9 ±0.4 174.0 ±15.8
187.0 ± 14.9 95.6 ±15.7 50.2 ±8.5 1.6 ±0.3 135.0 ±13.2
174.0 ± 10.3 51.3 ±6.3 48.3 ±8.2 1.8 ± 0.5 131.0 ±11.2
TC, LDL-C, HDL-C, TG = Total Cholesterol, Low Density and High Density Lipoprotein Cholesterol respectively and Triglyceride. Number of animals is 5 in each group.

178
Int. J. Pharm. Sci. Rev. Res., 21(1), Jul – Aug 2013; n° 28, 164-168 ISSN 0976 – 044X Table 3: Effect of water extract of Calotropis gigantea plus S. indicus on glycosylated haemoglobin and body weight, values shown are those at the end of 8 weeks treatment, haemoglobin in blood and serum albumin total proteins and creatinine
Parameter Normal mean ±
S.D. Diabetic mean ± S.D. Diabetic treated mean ± S.D.
Glycosylated haemoglobin 3.04 ± 0.02
9.4 ± 2.4 4.8 ± 0.1
(HbA1c) %
Albumin (g/l) 55.0 ± 1.4 45.0 ± 3.1 52.9 ± 3.0a
Total protein (g/l) 69.0 ± 3.0 73.2 ± 2.9 78.2 ± 3.8a
Creatinine ml/min 0.75 ± 0.04 1.30 ± 0.15 0.91 ± 0.05a
Body weight (g) 283.6 ± 25.8 225.5 ± 45.0 280.4 ± 9.0
Kidney weight (g) 1.40 ± 0.05 2.92 ± 0.08 1.06 ± 0.10
Haemoglobin 16.0 ± 4.2 ____ ND
Urine sugar 10.5 ± 1.2 +++ ++
Urine albumin ND ++ ND
The values are mean ± S.D; *a p < 0.05 when compared with diabetic untreated group.
Table 4: Effect of water extract of Calotropis gigantea plus S. indicus on the serum lipid profile in rats fed on high fat diet
TC mg/dl TG mg/dl LDL HDL-C Normal 198.7 ± 44.9 94.9 ± 7.1 83.8 ± 16.2 42.3 ± 19.2
High-fat rats 622.3 ± 1.4 34.7 ± 0.9 3.58 ± 0.11 31.0 ± 0.10
High-fat diet plus extracts 182.5 ± 4.2 171.8 ± 0 148.8 ± 8.0 173.1 ± 23.4
Table 5: Effect of water extract on liver and kidney weight in rats fed on high fat diet
Tissues Normal rats High-fat diet untreated High-fat diet plus extracts of two plants Liver (gm) 7.82 ± 0.33 10.4 ± 0.41 9.8 ± 0.18b Kidney (gm) 0.99 ± 0.05 1.08 ± 0.08 0.99 ± 0.06 b
*b p<0.0005 *c p<0.01 CONCLUSION In conclusion it appears that the water extract of combination of Calotropis gigantea plus S. indicus has got good hypoglycemic and hypolipidemic effect and also corrects complications associated with diabetes such as, retinopathy, nephropathy, neuropathy and musculopathy. Further research is needed to corroborate the same beneficial effects and to discuss the underlying mechanism involved in the above findings. REFERENCES * Amos AF, McCarty D.J, Zimmet P, The rising global burden
of diabetes and its complications: Estimates and projections to the year 2010. Diabetic Medicine, 14, 1997, 51-85.
* Bajaj J.S, Madan R, Diabetes in tropics and developing
countries. IDF bull, 2, 1993, 5-6. * David M.N, The pathophysiology of diabetes complications:
How much does the glucose hypothesis explain, Ann. Intern. Med, 174, 1996, 286-289.
* Dixit VP, Joshi S, Antiatherrosclerotic effects of alfalfa
meal injection in chicks: A biochemical evaluation, Ind. J. Physiol. Pharmacy, 29, 1985, 47-50.
* American Diabetes Association. Screening for type II
diabetes, Diabetes Care, 21(1), 1998, S20-S31.
6. World Health Organization. Prevention of diabetes mellitus:
Technical Report Series, WHO, Geneva, 1994, 844-848. 7. Kiritikar KR, Basu BD, Antihepatotoxic activity of crud
drug: Indian Medicinal Plant 1, 2 and 3, Basu Allahabad, 105(2), 1933, 109-118.
8. Malhotra RP, Compendium of Indian medicinal plants.
Central Drug Research Institute, Lucknow and information directorate: CSIR New Delhi, Vol. 2, 1991, 137-138.
9. Shukla R, Sharma SB, Puri D, Prabhu KM, Murthy PS,
Medicinal plants for treatment of diabetes mellitus. Ind. J. Clin. Biochem, 15, 2000, 169-177.
10. Rathod NR, Chitme HR, Irchhaiya R, Chandra R,
Hypoglycemic effect of Calotropis gigantea Linn leaves and flowers in streptozotocine induced diabetic rats, Oman Med. J, 26(2), 2011, 104-108.
11. Choudhary NK, Jha AK, Sharma S, Goyal S, Dwivedi J,
Anti-diabetic potential of chloroform extract of flower of Calotropis gigantean: an in vitro and in vivo study. International Journal of Green Pharmacy, 4, 2011, 296-301.
12. Ramacandran K, Subramanaian B, Scarlet G, Coccinia
grandis, little known tropical drug plant. Econ. Bot, 73, 1983, 80-82.
13. Hussain HEA, Reversal of diabetic retinopathy in
streptozotocin induced diabetic rats using traditional Indian anti-diabetic plant, Azadirachta indica (L). Ind. J. Clin. Biochem, 17(2), 2002, 115-123.

179
Int. J. Pharm. Sci. Rev. Res., 21(1), Jul – Aug 2013; n° 28, 164-168 ISSN 0976 – 044X 14. Reinhold JG, Reiner M, Standard methods in clinical
chemistry Vol. 1. New York: Academic press, 1953, 88-89. 15. Hiroshi O, Nobuko, Kunio V, Assay for lipid peroxides in
animal tissues by thiobarbituric acid reaction, Anal. Biochem, 5, 1979, 351-358.
16. Salimath BP, Sundaresh C.S, Srinivas L, Dietary
compounds inhibit lipid peroxidation in erythrocyte membrane, Nut Resi, 6, 1985, 1171-1178.

180
World Journal of Pharmaceutical research
Volume 2, Issue 5, 1826-1839. Research Article ISSN 2277 –
7105
ETHNOPHARMACOLOGICAL EVALUATION OF CALOTROPIS
GIGANTEA
Vaibhav Prakash Srivastava*1, Shaundarya Kumar2, Usha Rai 3, Sonika 4, Deepak Teotia5, Dr. Rakesh Singh6
1* ,4,5,Vishveshwarya Institute of Medical Science, G.B.Nagar. 2,3,6, Kamala Nehru Institute of Technology & Management, Faridipur, Sultanpur U.P. India. ABSTRACT Calotropis gigantea, commonly known as milkweed or swallow-
wort, is a common wasteland weed (Singh et al. 1996).
Calotropis belongs to Asclepiadaceae or Milkweed or Ak family
which includes 280 genera and 2,000 species of world-wide
distribution but most abundant in the sub-tropics and tropics,
and rare in cold countries. Calotropis gigantea Linn. (Asclepiadaceae) a widely growing plant has been
reported to possess number of medicinal properties. The aim of
the present study was to screen leaves of Calotropis gigantea to
study & compare
Antioxidant, Antibacterial, Anti-inflammatory & wound healing
Activity of Calotropis gigantea Linn. Calotropis gigantea, with
ethanolic extract. It has been reported as a traditional folk
medicine for
a variety of aliments. The stages of wound healing are inflammatory phase,
proliferation phase, fibroblastic phase and maturation phase. Extract treated animals
exhibit 83.42 % shows the Anti-inflammatory area when compared to controls which
was 76.22 %. The extract treated wounds are found to epithelize faster as compared
to controls. The plant C. gigantea is also used in some parts of India for wound
healing in combination with other plants. However there are no scientific reports on
India.
prakashsrivastava.vaibhav@gm
Medical Science, G.B. Nagar,
Vishveshwarya Institute of
Vaibhav Prakash Srivastava,
*Correspondence for
Revised on 24 July 2013, Accepted on 30 August 2013
Article Received on 16 June 2013,
ail.com,
Author:

181
wound healing activity of the plant C.gigantea. The oral administration of 400mg/kg of C.gigantea and 300 mg/kg of
C.gigantea were showed significant anti-inflammatory activity more than that of
100mg/kg of Ibuprofen. This study also proved the greater anti-inflammatory action
due to the effect of C. gigantea with Acetyl Choline than Acetyl Choline alone.
KEY WORDS: Antioxidant, Antibacterial, Muscle Relaxant Activities, Calotropis
gigantea, Ethanolic extract, Acetylcholine.

182
INTRODUCTION
Medicinal plants are usually of medicine for the treatment of leprosy, ulcers, tumors,
used for Ayuerbedic, Unani and other rural areas. Recent discovery shows that these
plants have fewer side effects than the Allopathic medicine. So, herbal medicine
becoming popular for medication among whole over the world. The number of plants
with medicinal properties included in the Materia Medica of traditional medicine in
this subcontinentat present stands at about 2000 [1]. More than 500 of such medicinal
plants have so far been enlisted as growing in Bangladesh [2]. Thus the human race
started using plants as a means of treatment of diseases and injuries from the early
days of civilization on earth and its long journey from ancient time to modern age the
human race has successfully used plants products as effective therapeutic tools for
fitting against diseases and various other health hazards [3]. C. gigantea is a common
wasteland weed found abundant throughout India right from Himalayas to southern
India. C. gigantea was regarded as a useful medicinal plant and used in folk
medicine1, 2. Traditionally it is used for the treatment of different aliments in
ayurvedic and unani systems of medicines. The plant has been known as “Vegetable
Mercury” since it is used as a remedy for syphilitic affections, also advocated for a
variety of diseased conditions including leprosy, ulcers, tumours and piles. The plant
is reported to have diverse pharmacological actions like antifertility, cardiotonic,
antimicrobial activities4. The Ethanolic extract of the root has been shown to exhibit
protective activity against carbon tetrachloride induced liver damage [10]. Methanol
extract possess antioxidant activity in Trema orientalis [11] and Senna tora12. So, the
present work was designated to investigate the antioxidant and antibacterial activities
of of Calotropis gigantea Linn to know the scientific basis of ascorbic acid were
weighed three times and dissolved in ethanol to make the required concentration by
dilution technique. Here ascorbic acid was taken as standard. DPPH was weighed
and dissolved in ethanol to make 0.005% (w/v) solution. To dissolve homogeneously
magnetic stirrer was used. After making the desired concentration 4 ml of 0.004
DPPH solution was applied on each test tube by pipette. The room temperature was
recorded and kept the test tubes for 30 mins in light to complete the reactions. DPPH
was also applied on the blank test tube at the same time where only ethanol taken as
blank. 13

183
MATERIALS AND METHODS PLANT MATERIALS Fresh leaves of Calotropis gigantea were collected from Lucknow local area of 2011. The plant was identified by the expert of National Botanical Research Institute (NBRI), Lucknow and a voucher specimen was kept for future reference. The dried leaves of Calotropis gigantea were ground into a fine powder with the help of suitable grinder. About 400 g of powder grinded material was extracted by soxhlet apparatus with 90% methanol at 55°C temperature. PROCESSING OF THE PLANT Plant leaves were collected and washed properly with distilled water. The leaves
were shade dried at room temperature. Dried leaves were uniformly grinded using
mechanical grinder. The leaves powder was extracted in distilled water.
Fig 1. Crude Leaves and Dried Powder of Calotropis gigantea Ten gram of plant powder was soaked in 100 ml of distilled water in a conical flask
and loaded on an orbit shaker at a speed of 120 rpm for 24 hours. The mixture was
filtered using Whatman filter paper number 1. The filtrate was concentrated using
rotary evaporator and dried using lyophilizer. Dried extract was collected in an air
tight container and stored at 4°C. The extracted powder was dissolved in sterilized
distilled water to make 1000 µg/ml solution. This mixture was used to perform
antibacterial assay.
TEST MICROORGANISM The following six clinical isolates of bacteria were used for the study: S. aureus, K.
pneumoniae, B. cereus, P. aeruginosa, M. luteus and E. coli. All these cultures were
maintained on nutrient agar plates at 4°C. scavenging activity of the stable 1,1-

184
diphenyl-2-picryl hydrazyl free radical. DPPH method is most widely used and
easiest method to determine Antioxidant activity DPPH is a stable free radical
containing an odd electron in its structure and usually utilized for detection of the
radical scavenging activity in chemical analysis. 13 The aliquots of the different
concentrations (1-500 µg/ml) of the extract was added to 3 ml of a 0.004 %w/v
solution of DPPH. Absorbance at 517 nm was determined after 30 min, and IC50 (Inhibitory
concentration 50%) was determined. IC50 value denotes the concentration of sample
required to scavenge 50% of the DPPH free radicals. At first 6 test tubes were taken to
make aliquots of 6 conc.(1,5,10,50,100,500 µg/ml).Plant extract and ascorbic acid were
weighed 3 times and dissolved in ethanol to make the required concentration by dilution
technique. Here ascorbic acid was taken as standard. DPPH was weighed and dissolved
in ethanol to make 0.004% (w/v) solution. To dissolve homogeneously magnetic stirrer
was used. After making the desired concentration 4 ml of 0.004 DPPH solution was
applied on each test tube by pipette. The room temperature was recorded and kept the
test tubes for 30 mins in light to complete the reactions. DPPH was also applied on the
blank test tube at the same time where only ethanol taken as blank. After 30 mins,
absorbance of each test tubes were determined by UV spectrophotometer. IC50 was
determined from % inhibition vs. concentration graph. 14,15
ANTIMICROBIAL ACTIVITY DISC DIFFUSION METHOD The extracts of C.gigantea leaf obtained by maceration process by using water as a
solvent. Extracts were screened for antimicrobial activity using by disc diffusion
method. A suspension of organism was added to sufficient quantity of nutrient agar
at 450C. The mixture was aseptically transferred to sterile petri dish and allowed to
solidify. The overnight culture grown in broth was used for inoculation. The plant
extracts to be tested were prepared in various concentrations i.e. 25%, 50%, 75%
and 100%. The sterile impregnated discs with plant extracts were placed on the agar
surface with framed forceps and gently pressed down to ensure complete contact of
the disc with agar and dextrose surfaces. Positive control discs were also prepared
in the same manner using Ampicillin, a bactericide. But it was not used for fungi. The
prepared control discs were placed using respective solvents. 16,17

185
All the plates including control plates were incubated at 37°C for 24 hours. After
incubation, the size (diameter) of the inhibition zones was measured. Triplicates
were maintained for each sample of the extract respectively. The results were
expressed in terms of the diameter of the inhibition zone: <9 mm - inactive; 9-12mm -
partially active; 13-18mm - active; >18mm - very active. After the confirmation of
antibacterial activity with 100mg/kg dose the experiment was carried out in triplicate
and average values were taken into consideration. Similar procedure was carried out
with standard drug Ampicillin 100mg/ml. And the zone of inhibition was compared
with test sample and control and the percentage of inhibition was calculated which
are given below in table. 16,18
PHARMACOKINETIC PARAMETER OF ANTIMICROBIAL ACTIVITY MINIMUM BACTERICIDAL CONCENTRATION The Minimum Bactericidal Concentration (MBC) is the lowest concentration of
antibiotic required to kill the germ not as commonly seen as the Minimum inhibitory
concentration (MIC). It can be determined from broth dilution MIC tests by sub
culturing to agar media without antibiotics. The minimum bactericidal concentration
(MBC) is the lowest dilution where the culture has been completely sterilized. It is not
routinely determined. Treatment decisions are made related to MICs, and more
specifically, the breakpoint MICs.19
MINIMUM INHIBITORY CONCENTRATION The minimum inhibitory concentration (MIC) is the concentration required to inhibit
growth of a specific isolate in vitro under standardized conditions. It is determined by
finding the lowest dilution without visible growth during serial dilution testing. In
microbiology, is the lowest concentration of an antimicrobial that will inhibit the visible
growth of a microorganism after overnight incubation. Minimum inhibitory
concentrations are important in diagnostic laboratories to confirm resistance of
microorganisms to an antimicrobial agent and also to monitor the activity of new
antimicrobial agents. An MIC is generally regarded as the most basic laboratory
measurement of the activity of an antimicrobial agent against an organism. 19.20
DETERMINATION OF RELATIVE PERCENTAGE INHIBITION The relative percentage inhibition of the test extract with respect to positive control
was calculated by using the following formula 6, 11.

186
Relative percentage inhibition of the test extract =
Where, * total area of inhibition of the test extract * total area of inhibition of the solvent * total area of inhibition of the standard drug The total area of the inhibition was calculated by using
area = πr2; where, r = radius of zone of inhibition. 16,17
EFFECT OF EXTRACT FROM CALOTROPIS GIGANTEA ON THE SKELETAL MUSCLE OF THE RAT Since the antimigrain drugs were reported to have muscle relaxant activity, so this
experiment was attempted to assess the effect of extract from C. gigantea on the rat
rectus abdominis muscle preparation. The experiment was carried as per the method
described by Kulkarni 5. Rats weighing 20‐25 g were used in this study. The rat was
stunned and decapitated and the spinal cord was destroyed. A rat was pithed and the skin of the anterior and abdominal wall was cut by a midline
incision and then it was cut laterally to expose the anterior abdominal wall. 18,19 The two rectus were seen running from the base of sternum. The muscles were cut
across just above the sternum at its base and the pair of muscles attached to it were
dissected and transferred to a dish containing frog ringer solution at room
temperature. The muscles were then carefully cleaned and one of them was trimmed
to the desired size and mounted in an organ bath filled with ringer solution at room
temperature and aerated by stream of fine bubbles emerging near the bottom of the
bath. Isotonic contractions were recorded using gimbel lever with a sideways writing
point. The lever was balanced for a tension of approximately 2‐5 g. An extra load of
approximately 1g on the long arm was supplied because sometime the lever may not
return to the base line after washing. 18, 20

187
The drug period allowed for stabilization was 30 minutes during which the muscle
was subjected to 1g stretch. At 0 min ‐ the kymograph was started after raising the
extra load; in the 1st min‐ the drug was added and in the 2nd min‐ the kymograph
was stopped. The tissue was washed and allowed to relax by applying an extra load.
At the 5th min‐ the lever point was brought to the base line and the next cycle was
started. After recording the graded responses to different log dose of acetylcholine,
the test drug (Extract) was added and their effects upon acetylcholine induced
contractions as well as the effect of its own in the tissue was studied. 21 DETERMINATION OF MINIMUM INHIBITORY CONCENTRATION (MIC) MICs can be determined by agar or broth dilution methods usually following the
guidelines of a reference body such as the CLSI, BSAC or EUCAST. There are
several commercial methods available, including the well established Etest strips and
the recently launched Oxoid MIC Evaluator method. The Etest system comprises a predefined and continuous concentration gradient of
different antimicrobial agents, which when applied to inoculated agar plates and
incubated, create ellipses of microbial inhibition. The MIC is determined where the
ellipse of inhibition intersects the strip, nand is easily read off the MIC reading scale
on the strip. 20.21

188
RESULTS AND DISCUSSION FOR ANTIOXIDANT ACTIVITIES TEST
In the present study, methanol extracts of the leaves of C.gigantea showed potential
free-radical scavenging activity but aqueous extract showed very little free-radical
scavenging activity.
Fig. 2 Comparison of Antioxidant activity of Various Extract FOR ANTIMICROBIAL ACTIVITIES TEST The bacterial suspensions were seeded on MHA plates using a sterilized cotton
swab. In each of these plates four wells were cut out using a standard cork borer (7
mm). Using a micropipette, 100 µl of each dilution was added in to wells. All the
plates were incubated at 37ºC for 24 hours. Antimicrobial activity of the leaf extract
was evaluated by measuring the zone of inhibition. Experiment was carried out in
triplicates for each test organism.
Figure 3: Antimicrobial activity of Calotropis gigantea

189
Table 1: Test organisms Relative percentage inhibition (%)
Test organisms Relative percentage inhibition (%)
Staphylococcus aureus 48.05
Klebsiella pneumoniae 75.64
Bacillus cereus 175.36
Pseudomonas aeruginosa 108.16
Micrococcus luteus 26.67
Escherichia coli 155.89
Figure 4: Relative percentage inhibition of Calotropis gigantea

190
Table 2: MIC values of methanol and aqueous extracts of Calotropis
gigantea on test organisms
MIC in mg/ml
S. aureus K. pneumonia B. cereus P. aeruginosa M. luteus E. coli
52 23 5.25 4.1 1.7 11.65
Table -3 Antimicrobial activity of Calotropis gigantea
Inhibition zone diameter (mm)
Test organisms
AE PC NC
Staphylococcus aureus 14.3±1.15 18.6±1.52 0
Klebsiella pneumoniae 13.6±1.52 13.3±0.57 0
Bacillus cereus 16.3±1.52 15.6±1.15 0
Pseudomonas 14.0±1.73
16.6±1.52
0
aeruginosa
Micrococcus luteus 16.6±1.52 33.3±1.52 0
Escherichia coli 18.6±1.15 16.6±2.08 0
AE: aqueous extract, PC: positive control, NC: negative control. Values are
expressed as mean ± standard deviation of the three replicates. Zone of inhibition
not include the diameter of the well. Results of MIC are reported in Table 2 . The crude extract showed 52, 23, 11.65,
5.25, 4.1 and 1.7 mg/ml MIC values for S. aureus, K. pneumoniae, E. coli, B. subtilis,
P. aeruginosa and M. luteus respectively. Aqueous extract of Calotropis gigantea showed high inhibitory activity followed by
methanol extract, where as ethanol and petroleum ether extracts showed low activity
6. Previous studies report the presence of phytochemicals like cardenolides,
flavonoids, terpenes, pregnanes, nonprotein amino acid and cardiac glycoside as
major constituents in C. gigantean may acknowledge the medicinal property of this
plant.

191
FOR MUSCLE RELAXANT ACTIVITIES TEST The Aqueous and Ethanolic Extract of C. gigantea was found to have skeletal
muscle relaxant property at T1 (1:100), T2 (1:500) and T3 (1:1000), when tested
along with acetylcholine. When the relaxant property was compared with the
standard drug acetylcholine, Ethanolic Extract tested along with the acetylcholine
produces more relaxant property than the standard drug acetylcholine (Table 1 &
Fig. 1‐2). Lesser the concentration of the test drug (Ethanolic Extract ) increases the
responses of the muscle relaxant property. Maximum relaxant effect in T1 and T3
was found i.e. 22mm and 23mm at the dose of 16µg and T2 was 13mm at 2µg.
Earlier studies have proved that chloroform extract of Ervatamia crispa revealed
skeletal muscle relaxant effect on an isolated rat rectus abdominis muscle preparation16.
Fig-5: Muscle Relaxant Activity of Calotropis gigantea

192
Fig-6 Fig. 5-6.Comparison of Muscle Relaxant activity of acetylcholine and test drug at different concentration. Table 4: Muscle Relaxant activity extract from Calotropis gigantea
Drug Volume (ml) Dose (µg) Height(mm) Responses
Acetylcholine 0.1 1 3 Increased Acetylcholine 0.4 4 5 Increased
Acetylcholine 0.8 8 9 Increased
Acetylcholine 1.2 12 11 Increased
T1 (1:100) 0.4 4 - -
T1 + ach 0.1 1 6 Increased
T1 + ach 0.4 4 9 Increased
T1 + ach 0.8 8 12 Increased
T2 (1:500) 0.4 4 - Increased
T2 + ach 0.1 1 24 -
T2 + ach 0.2 2 13 Increased
T3(1:1000) + ach 0.3 3 15 Increased
T3 + ach 0.4 4 16 Increased
T3 + ach 0.8 8 18 Increased
T3 + ach 1.6 16 24 Increased
Increased

193
CONCLUSION The results obtained in the MES test in rats that, the standard drug as well as the different extracts of stem barks of Calotropis gigantea protected against MES induced seizures. Extract of Calotropis gigantea had a slower onset of action and lesser degree of Muscle relaxant activity.The Antioxidant , Antibacterial, Muscle Relaxant Activities of Calotropis gigantea from Ethanolic, & Aqueous extract was studied and compare to each other. ACKNOWLEDGEMENT The authors wish to thank the Management and Staff of RITM, Lucknow And Vishveshwarya Institute of Medical Science, G.B. Nagar , providing necessary facilities to carry out the research work successfully heartfelt thanks to the Professor and head Deepak Teotia and my Dearest friend Mr. Shaundarya Kumar for their encouragement and Faithful support. REFERENCES
1. Chopra, J. and S. Rajasekharan, 1958. Indian 13. Gupta, M., U.K. Mazumdar, T.
Sivakumar, Pharmacological Aspects, 55:87-95.
2. M.L.M. Vamis, S. Karkis, R. Sambathkumar and L. Dhanukar KA, Kulkarni RA,
Rege M.N. Pharmacology of medicinal plants and national products. Indian J
Pharmacol 2000; 32 : 81
3. Yusuf, M., J.U. Chowdhury, M.A. Wahab and Mainkandan, 2003. Antioxidant and
Anti- J. Begum, 1994. Medicinal Plant of Bangladesh. inflammatory activities of
Acalypha fruticasa. Nig. J. 3rd Edn., pp: 234-235.
4. Mueen Ahmed KK, Rana AC, Dixit VK. Calotropis Species (Ascelpediaceae) – A
Comprehensive Review. Phcog. Mag 2005; 2 Suppl 1: 48
5. Mueen Ahmed KK, Rana AC, Dixit VK. Free radical scavenging activity of
Calotropis species. Indian Drugs 2003; 40 Suppl 11: 54
6. Kulkarni SK. Handbook of experimental Pharmacology. 3 rd edition, New Delhi:
Vallabh Prakashan; 1999.
7. Roy RK, Ray NM, Das A k. Skeletal muscle relaxant effect of chonemorpha
macrophylla in experimental animals. Indian. J. Pharmacol 2005; 37: 116‐119.
8. Wang Z, Wang M, Mei W, Han Z, Dai H, A New Cytotoxic Pregnanone from
Calotropis gigantea, Molecules, 13, 2008, 3033- 3039.
9. Chitme HR, Chandra R, Kaushik S, Evaluation of antipyretic activity of Calotropis
gigantean (Asclepiadaceae) in experimental animals, Phytotherapy Research,
19, 2005, 454-456.

194
10. Saratha V, Subramanian S, Sivakumar S, Evaluation of wound healing potential
of Calotropis gigantea latex studied on excision wounds in experimental animals,
Med Chem Res, 2009; DOI: 10.1007/s00044-009- 9240-6.
11. Tagg TR, Dajani AS, Wannamaker LW, Bacteriocin of Gram positive bacteria,
Bacteriological Reviews, 40, 1976, 722-756.
12. Ajay KK, Lokanatha RMK, Umesha KB, Evaluation of antibacterial activity of 3,5-
dicyano-4,6-diaryl-4- ethoxycarbonyl-piperid-2-ones, Journal of Pharmaceutical
and Biomedical Analysis, 27, 2003, 837-840.
13. Rios JL, Recio MC, Vilar A, Screening methods for natural products with
antimicrobial activity: A review of literature, Journal of Ethnopharmacology, 23,
1988, 127-149.
14. Okunji CO, Okeke CN, Gugnani HC, Iwu MM, An antifungal saponin from fruit
pulp of Dracaena manni, International Journal of Crude Drug Research, 28,
1990, 193-199.
15. Alam MA, Habib MR, Nikkon R, Rahman M, Karim MR, Antimicrobial activity of
akanda (Calotropis gigantea L.) on some pathogenic bacteria, Bangladesh J Sci
Ind Res, 43, 2008, 397-404.
16. Usha K, Singh B, Praseetha P, Deepa N, Agarwal DK, Agarwal R, Nagaraja A,
Antifungal activity of Datura stramonium, Calotropis gigantea and Azadirachta
indica against Fusarium mangiferae and floral malformation in mango, European
Journal of Plant Pathology, 124, 2009, 637-657.
17. Ali M, Gupta J, New pentacyclic triterpenic esters from the roots of Calotropis
procera, Indian J Chem, 38, 1999, 877-881.
18. Sadhu, S.K., E. Okuyama, H. Fujumoto and M. Ishibashi, 2003. Seperartion of
leucas, aspara amedicinal plant of Bangladesh,guided by prostaglandin inhibitory
and anti oxidant activities
19. Singh, U., A.M. Wadhwani, and B.M. Johri, 1996. Dictionary of Economic Plants
of India. Indian Council of Agricultural Research, New Delhi. p. 38-39.
20. Sastry, C.S.T. and K.Y. Kavathekar. 1990. In: Plants for reclamation of
wasteland. Publication and Information Directorate, CSIR, New Delhi. p. 175-179.