Prune Belly Syndrome
-
Upload
demmie-marie-r-fermin -
Category
Documents
-
view
196 -
download
2
Transcript of Prune Belly Syndrome

PRUNE BELLY SYNDROME

Background
The syndrome is named for the mass of wrinkled skin that is often (but not always) present on the abdomens of those with the disorder.
Other names for the syndrome include Abdominal Muscle Deficiency Syndrome, Congenital Absence of the Abdominal Muscles, Eagle-Barrett Syndrome, Obrinsky Syndrome, Fröhlich Syndrome, or rarely, Triad Syndrome.

Background Prune belly syndrome is a group of
birth defects that involve three main problems:
1. A partial or complete lack of abdominal muscles. There may be wrinkly folds of skin covering the abdomen.

2. Undescended testicles in males (cryptorchidism)

Crytorchidism

3. Urinary tract abnormality such as unusually large ureters, distended bladder, accumulation and backflow of urine from the bladder to the ureters and the kidneys

Background Prune belly syndrome is an uncommon
birth defect occurring in about one in 40,000 births.
In 95 percent of the cases, it occurs in males. It may occur if there is a urethral obstruction
during fetal development preventing any urine from flowing through the urinary tract. The urethra is the tube that drains urine from the bladder to the outside of the body for elimination. If there is obstruction, urine can reverse flow and cause an expanded bladder

Prune belly syndrome is associated with trisomy 18 and 21. Patients with prune belly syndrome also have an increased incidence of tetralogy of Fallot (TF) and ventriculoseptal defects.

Diagnosis: Prenatal
A woman who is pregnant with a baby who has prune belly syndrome may not have enough amniotic fluid (oligohydramnios). This can cause the infant to have lung problems.
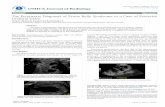
An ultrasound done during pregnancy may show that the baby has a swollen bladder or enlarged kidney.

The abdomen of an infant with prune belly syndrome shows marked distention of the abdomen and bulging flanks secondary to a large urinary system and the absence of abdominal wall musculature.

Diagnosis: Postnatal
Weak abdominal muscles can cause: "Little Buddha" appearance Constipation Delay in sitting and walking Difficulties coughing
Urinary tract problems can cause difficulty urinating.

Diagnostic/Laboratory Tests Renal ultrasound - a diagnostic imaging technique that
uses high-frequency sound waves and a computer to create images of blood vessels, tissues, and organs. Ultrasounds are used to view internal organs as they function, and to assess blood flow through various vessels.
Voiding cystourethrogram (VCUG) - a specific x-ray that examines the urinary tract. A catheter (hollow tube) is placed in the urethra (tube that drains urine from the bladder to the outside of the body) and the bladder is filled with a liquid dye. X-ray images will be taken as the bladder fills and empties. The images will show if there is any reverse flow of urine into the ureters and kidneys.

Intravenous pyelogram (IVP) - a diagnostic imaging technique which uses an x-ray to view the structures of the urinary tract. An intravenous contrast of dye is given so that the structures can be seen on film. An IVP also reveals the rate and path of urine flow through the urinary tract.
Blood tests (to determine how well the kidneys may be functioning).

Prognosis
Prune belly syndrome is a serious and often life-threatening problem.
Many infants with prune belly syndrome are either stillborn or die within the first few weeks of life from severe lung or kidney problems, or a combination of birth problems.
Some newborns survive but continue to have problems.

Treatment: Medical Therapy
Antibioticso Surgical intervention is not warranted in
these patients as long as they remain free of infection. Once infections start occurring frequently, the reflux should be corrected.
Management of the undescended testis with human chorionic gonadotropin (hCG) is not warranted in these cases.

Treatment: Surgical therapy Undescended testis
Orchiopexy is a surgery to move an
undescended testicle into the scrotum and permanently fix it there. It is performed by a pediatric urologist or surgeon on boys withcryptorchidism, typically before they reach the age of two. Some patients remain undiagnosed until their teenage years and undergo the surgery at that time.


Abdominal wall reconstruction Abdominal wall reconstruction is
performed in most patients with prune belly syndrome to improve respiratory function and to improve cosmesis.
innovations in abdominal wall reconstruction have been developed. The Monfort and Ehrlich variations of the Randolph operation have improved results, with decreased morbidity and the ability to preserve the umbilicus.



Placement of a percutaneous nephrostomy Obstruction at the ureteropelvic junction
(UPJ) has been observed in patients with prune belly syndrome. In some cases, diagnosing this can be difficult; however, the diagnosis can be confirmed with the placement of a percutaneous nephrostomy. This procedure can be performed under ultrasound guidance with relative ease in a dilated system and provides the opportunity to perform a renal biopsy, which could help with the later management of the urinary tract.

Placement of a percutaneous nephrostomy provides the surgeon with several options. The surgeon can confirm the diagnosis of UPJ obstruction. The urinary tract can be decompressed in an ill child or in a child who is too small to safely undergo reconstructive surgery at the time. Finally, the technique also allows the surgeon to evaluate the renal function of the obstructed unit

Standard pyeloplasty
If conditions are right and the child is stable, a standard pyeloplasty can be performed as another means of treating the obstructed UPJ. The surgeon should be meticulous in the dissection of the upper ureter. The proximal ureteral blood supply should be preserved as much as possible in case ureteral tapering or reimplantation becomes necessary later.

Cutaneous pyelostomy still carries the risk of resultant scarring from excessive dissection, which may be required to take down the pyelostomy at a later stage.
At the time of reconstruction, ureteral tapering or reimplantation that is necessary creates a difficult situation. Recently, these problems have been overcome with the increasing use of percutaneous nephrostomy drainage and with the use of vesicostomy as a means of draining the upper tracts.
Some believe that vesicostomy can decompress the upper tracts just as well as high diversion. Subsequently, since the introduction of these 2 procedures, the use of high diversion has declined significantly over the last few years, and reconstruction in these patients has become easier.

Nephrostomy


Infravesical obstruction or obstruction at the prostatic urethra Blocksom vesicostomy performed in
the early newborn period is the simplest and best treatment in patients with documented obstruction. Bringing the dome of the bladder out to the skin is essential when creating the vesicostomy; this approach prevents the resultant herniation of the bladder in an improperly created vesicostomy.

Herniation of the bladder is quite prevalent in patients with prune belly syndrome because the bladder is quite large and redundant. A patent urachus can be found frequently in patients with urethral obstruction. The patent urachus is the means by which patients are able to survive; early deaths usually are observed in patients with urethral obstruction without a patent urachus. In these patients, once a vesicostomy is performed, the surgeon should try to identify the urachus and ligate it at that time.


Preoperative
Preoperatively, all patients should have stable respiration. This is critical because postoperative respiratory infections pose a serious risk to these patients.
The urine should be sterile prior to surgery. In patients undergoing abdominal wall
reconstruction, the presence of a peg gastrostomy precludes the safe reconstruction of the abdominal wall. The author prefers to not have a gastrostomy in place before abdominal wall reconstruction.

Postoperative Details
Postoperatively, these patients must be monitored closely. They can easily become fatigued and may experience respiratory arrest. Judicious use of narcotics is critical, and the use of ketorolac (Toradol) is recommended for postoperative pain control. The author has also used postoperative epidural anesthesia, with excellent results.

Complications
Undescended testis The most obvious complication of
orchidopexy is incomplete descent of the testis. Atrophy of the testis is another possible complication. This can occur in some cases (as many as 50%) of Fowler-Stephens orchidopexy. For this reason, the author does not suggest performing simultaneous Fowler-Stephens orchidopexies.

Abdominal wall reconstruction After reconstruction, persistent laxity of
the abdominal wall is a concern, regardless of the technique used. Using the laparoscope to perform the abdominal wall plication significantly reduces the risk of this complication.
The abdominal wall skin can slough when the skin flaps are raised. Care should be taken to avoid incisions that cut the blood supply to the flaps.

Ureteral reimplants Ureteral strictures are not uncommon in
tapered reimplants of ureters in patients with prune belly syndrome. This can be avoided using Kaliscinski-type tapering of the ureters.