Nuances of Spinal Radiculopathy - PHEMC · of pain distribution in spinal radiculopathy •...
Transcript of Nuances of Spinal Radiculopathy - PHEMC · of pain distribution in spinal radiculopathy •...

Nuances of Spinal
Radiculopathy
James Mallows

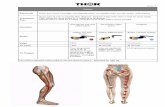
Spinal dermatomes
• A dermatome is an area of skin that is
mainly supplied by a single spinal nerve


History of dermatomes
• Pioneering work by Sherrington (late
19th century), Foester (1933) and
Keegan and Garrett (1948)
• Based on multiple animal experiments
and clinical situations

History of dermatomes
• Sherrington
• Study in monkeys
• Severed multiple spinal nerves above
and below a single spinal nerve and
mapped the sensory supply of that
nerve
• Found very predictable dermatomes

History of dermatomes
• Other clinical data
• Herpes zoster
• War injuries
• Spinal root injections with local anaesthetic
• Human dermatomal maps varied little from
the animal models

Dermatomes
• Most areas of the skin are innervated by
2 or more spinal nerve roots
• Also get intrathecal intersegmental
anastomoses of dorsal spinal rootlets,
allowing sensory neurons at one dorsal
root ganglion to enter the spinal cord at
a different level

Dermatomes
• Thus a single spinal nerve lesion may
not cause noticeable sensory loss,
especially in the trunk
• However in the limbs, complete
interruption of a single peripheral nerve
produces changes in sensation that are
often appreciated by a patient

Diagnosis of radiculopathy
• Clinical decisions are made by
correlating a patient’s symptoms and
imaging with sensory dermatomal maps
• Assumption is that pain and
paraesthesias will follow the same
dermatomal distribution

Dynatomes
• We are now gaining an understanding
of pain distribution in spinal
radiculopathy
• Dynatomes vs dermatomes
• A dynatome is an area of skin that can
experience pain in pathology of a
particular nerve root

Dynatomes
• Slipman CW, Plastaras CT, Palmitier
RA et al. Symptom Provocation of
Fluoroscopically Guided Cervical Nerve
Root Stimulation. Spine 1998;23:2235-
2242.

Slipman et al
• To document the distribution of pain and
paraesthesia that result from stimulation
of specific cervical nerve roots and
compare that to documented
dermatomal maps

Slipman et al
• Consecutive patients undergoing
fluoroscopically guided cervical nerve
root blocks (C4-C8)
• Immediately preceding contrast
injection, mechanical stimulation of the
nerve root was performed
• The site of the pain experienced was
recorded and mapped

Slipman et al
• 134 nerve root stimulations on 87
patients



Slipman et al
• Distinct differences between dynatomal
and dermatomal maps

Dynatomes
• Murphy DR, Hurwitz EL, Gerrard JK and
Clary R. Pain patterns and descriptions
in patients with radicular pain: Does the
pain necessarily follow a specific
dermatome? Chiropractic & Osteopathy
2009;17.

Murphy et al
• To describe the distribution of pain in
patients with cervical and lumbar
radicular pain
• All patients either had:
• disc protrusion or lateral canal stenosis
demonstrated on complex imaging; or
• EMG documentation of nerve root
dysfunction

Murphy et al
• Used a variety of manoeuvres to elicit
spinal root pain
• Patient then mapped where they
experienced their pain
• This map was compared to standard
dermatomal charts and was classified
as either dermatomal or non-
dermatomal

Murphy et al
• 226 nerve roots in 169 patients
• Pain was non-dermatomal in 69.7% in
cervical radiculopathy and in 64.1% in
lumbar radiculopathy
• However in S1 radiculopathy, 64.9% of
pain was dermatomal

Murphy et al
• In most cases nerve root pain should not
be expected to follow along a specific
dermatome, and a dermatomal distribution
of pain is not a useful historical factor in
the diagnosis of radicular pain. The
possible exception to this is the S1 nerve
root, in which the pain does commonly
follow the S1 dermatome

Dynatomes
• Possible reasons
• Referred pain from discs or other tissues
• Overlaps between dermatomes
• Intense and persistent nociceptive input
can expand the size of the receptive fields
of those dorsal horn cells

Dynatomes
• Therefore we must beware the classical
teaching of being able to correlate a
patient’s pain distribution to the
dermatomal nerve root of the site of the
pain

Epidural steroid injections
• Do they work?
• Everyone seems to do them
• “I don’t know, I work in emergency”
• “I’m booked in for one next week but I
just can’t wait for it”

Epidural steroid injections
• Shamilyan TA, Staal JB, Goldman d,
Sands-Lincoln M. Epidural steroid
injections for radicular lumbosacral pain:
a systematic review. Physical Medicine
and Rehabilitation Clinics of North
America. 2014;25:471-89.

Shamilyan et al
• Most guidelines do not recommend
routine use of epidural steroid injections
• Small short term but not long term
improvement in leg pain and function
• Evidence does not support routine use
of off-label epidural steroid injections

Epidural steroid injections
• Quraishi NA. Transforaminal injection of
corticosteroids for lumbar radiculopathy:
a systematic review and meta-analysis.
European Spine Journal. 2012;21:214-
219.

Quraishi
• 126 papers: 5 RCTs with 3 following up
patients for more than 3 months
• 187 patients in the treatment group and
181 in the control group

Quraishi
• Improvement of pain but not disability
was observed in the treatment group
but not statistically significant

Epidural steroid injection
• Carmel A, Argoff CE, Samuels J,
Backonja M-M. Assessment: Use of
epidural steroid injections to treat
radicular lumbosacral pain. Neurology
2007;68:723-729.

Carmel et al
• Report of the Therapeutics and
Technology Assessment Subcommittee
of the American Academy of Neurology

Carmel et al
• Epidural steroid injections may result in
some improvement in radicular
lumbosacral pain when assessed
between 2 and 6 weeks following the
injection, compared to control
treatments (Level C, Class I–III
evidence)

Carmel et al
• Epidural steroid injection for radicular
lumbosacral pain does not impact
average impairment of function, need
for surgery, or provide long-term pain
relief beyond 3 months. Their routine
use for these indications is not
recommended (Level B, Class I–III
evidence)

Carmel et al
• There is insufficient evidence to make
any recommendation for the use of
epidural steroid injections to treat
radicular cervical pain

Epidural steroid injections
• Cohen SP, Hanling S, Bicket MC et al.
Epidural steroid injections compared
with gabapentin for lumbosacral
radicular pain: multicentre randomized
double blind comparative efficacy study.
BMJ 2015;350:h1748.

Cohen et al
• 145 people with lumbosacral radicular
pain secondary to herniated disc or
spinal stenosis for less than four years
in duration and in whom leg pain is as
severe or more severe than back pain

Cohen et al
• Participants received either epidural
steroid injection plus placebo pills or
sham injection plus gabapentin
• A positive outcome was defined as a ≥2
point decrease in leg pain coupled with
a positive global perceived effect

Cohen et al
• Average reduction in pain scores
• 1 month
• Steroids -2.2 (SD 2.4) gabapentin -1.7 (SD 2.6)
(p=0.25)
• 3 months
• Steroids -2.0 (SD 2.6) gabapentin -1.7 (SD 2.7)
(p=0.43)

Cohen et al
• Gabapentin and epidural steroid
injections used to treat lumbosacral
radicular pain both resulted in modest
improvements in pain and function,
which persisted through three months

Cohen et al
• Although some differences favoured
epidural steroid injections, these tended
to be small and transient (and not
significant)
• Similar outcomes between treatment
groups suggest a trial with neuropathic
drugs might be a reasonable first line
treatment option

Cohen et all
Likely causes
1. The treatments are equally effective but
the effect dissipates over time
2. Neither treatment is effective ie placebo
response or natural course of the disease
3. Epidural steroid injections are superior to
gabapentin but sample was too small

Cognitive error
• Commission bias
• Tendency toward action when the evidence
supports inaction
• Illusory correlation
• When 2 actions coexist but are not directly
related to each other
• “I got a steroid injection and the pain got a lot
better” [but then it got worse and I had to have
another one]

Thank you