Neck of Femur Fractures Wayne Hoskins. Background NOF #s common with advancing age High morbidity &...
-
Upload
anna-mccann -
Category
Documents
-
view
214 -
download
0
Transcript of Neck of Femur Fractures Wayne Hoskins. Background NOF #s common with advancing age High morbidity &...

Neck of Femur Fractures
Wayne Hoskins

Background
• NOF #’s common with advancing age
• High morbidity & mortality
• Only 1/3 return to living environment
• Death: 20-35% at 1 year in patients aged 82 +/-7

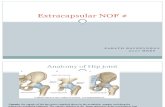
Anatomy

Fracture location

Head blood supply
• Profunda femoris gives off medial & lateral circumflex femoral arteries– Extracapsular anastomosis at base of neck– Ascending cervical branches– Intracapsular branches
• Majority via MCFA, ↓ via ligamentum teres


Garden classification
1. Incomplete impacted #
2. Complete # undisplaced
3. Displaced capsule intact
4. Displaced

Fracture classification
• Garden classification: poor inter-observer reliability:– displaced = 1 & 2– undisplaced = 3 & 4

Shenton’s Line

Mechanism of #
• Direct or indirect:
1. Direct blow to GT
2. ER: impinging posterior cortex on rim
3. Bending torque – major trauma
4. Violent muscle contraction
5. Cyclical loading / insufficiency #

NOF # complications
• AVN– Undisplaced 5-10%– Displaced 10-20%– RFs: displacement, velocity of injury, delay in
reduction, non-anatomical reduction• Non-union
– Undisplaced 5-10%– Displaced 20-30%– RFs - initial displacement, non anatomical
reduction, instability, no compression across #, vascularity

Presentation
• Typically elderly female
• Low energy fall
• Hip pain
• Short & ER leg
• Unable to weight bear

NOF # risk factors
• Osteoporosis
• Co-morbidities
• Dementia
• Poor mobility / vision

Work up – not just a #
• History– Mechanism of injury– Cause of fall - exclude medical cause: TIA, UTI,
MI, arrythmia, electrolyte imbalance etc– Other injuries from fall– Risk factors for osteoporosis– Co-morbidities/medications: ?anaesthetic review
pre-op, ?choice of operation
• ? Gen Med vs. Ortho admission– Ortho Geri’s consult

Work up
• Examination: pain, unable to weight bear, short ER leg, ?delirium
• Investigations:– ECG, FWT, urine MCS– Bloods: FBE, UEC, CMP, albumin, ESR,
Vit D, Coags, G&H– DEXA bone scan

Imaging
• Pelvis & hip XR
• ?undisplaced # - gold standard = MRI
• CT if MRI unavailable
• Bone scan less useful, changes take up to 1week in elderly
• Pre-op CXR

Medical management
• Treat co-morbidities whilst await OT:- electrolyte imbalances- anemia- pneumonia / UTI / infection- arrythmia / MI etc
• Post-op manage co-morbidities, RFs falls & osteoporosis: consider Vit D, Ca, bisphosphonates

Surgical management
• Surgical option based on:1. Displaced vs. undisplaced
2. Age of patient
3. Mobility/independence
4. Bone stock
• Aim perfect anatomical reduction and rigid fixation

Anti-coagulants
• Operate if on clopidogrel / aspirin
• If on warfarin: Vit K / FFP to reduce INR <1.5

Time to surgery
• Aim: surgery < 24 hours
• Jain JBJS Am 2002: significant reduction in AVN if fixed <12 hours

Surgical results
• Best results with healed # in anatomical position without AVN
• Quality of reduction is best predictor

Undisplaced subcapital #
• Cannulated screws used in young– 1 x inferior screw, 2x superior screws,
ensure threads cross # site, 5mm from surface, inferior screw above LT
• DHS + derotation screw used in old, independent walker

Displaced subcapital #
• Expected life > prosthesis survival (<65): aim to preserve the joint
• DHS + derotation screw– Closed or open anatomical reduction
• Union rates ↑ with anatomical reduction: accept no varus, <15 valgus, <10 AP plane

DHS technique
• Set up on traction table• Lateral incision: divide fascia lata• Ensure 2 guide wires centrally in femoral
heard1. Allows reaming for DHS2. Derotation screw
• Screws to attach plate• DHS Blade noe being used with osteoporotic
bone ↑ rotational stability

X-rays

Post-operative Mx
• DHS/Screws/Nail – admit to med ward– Surg ward: Hemi/THR/High energy trauma
• Young patients – PWB
• Elderly – WBAT to prevent complications
• Watch for AVN in subcapital #’s (usually 8-12 weeks, but up to 2 years)

Displaced subcapital #
• Expected life < prosthesis survival (>65)• Hemiarthroplasty < 5 year survival
– Bipolar no better than unipolar, difficult to reduce if Ds– No difference cemented vs uncemented outcome measures– Cemented hemi: ↑ operative time, blood loss, cement
pressurization complications, difficult revision• Moore’s if severe comorbidities/non walker – 30%
revision at 2 years• Gjertsen JBSB 2010 cf ORIF: both 25% mortality, 3
vs. 22% reoperation, more pain, lower QoL with ORIF

Displaced subcapital #
• Expected life < prosthesis survival (>65)
• THR 5-15 year survival young, active, mobile, associated joint disease (RA, OA, etc)– better ROM & pain relief vs hemi– Higher early Ds rate & early loosening– Long term Ds rate equal to hemi

Hemi/THR approach
• Posterior approach
- preserves gluteus medius
- observe sciatic n. ? ↓/↑damage
- ? ↓ Ds rate with bone anchors• Hardinge/anterolateral approach
- Trendelenburg gate
- Previous data ↓ Ds rate• Surgeon preference

Complications
• Infection
• Dislocation
• GT or Femoral shaft #
• Leg length discrepancy
• Loosening / pain
• Revision

Summary
• Full medical history and work up think medical admission with ortho consult
• Time to theatre
• Surgical choice based on age, # type, mobility, comorbidities
• High morbidity and mortality






![NOF Clinicians Guide[1]](https://static.fdocuments.net/doc/165x107/577d2a461a28ab4e1ea8d8a8/nof-clinicians-guide1.jpg)