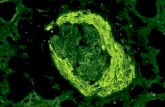
Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic...
-
Upload
anil-valiyaveettil -
Category
Documents
-
view
229 -
download
0
Transcript of Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic...
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
1/85
Nearly all forms of acute glomerulonephritis have a
tendency to progress to chronic glomerulonephritis. The
condition is characterized by irreversible and progressiveglomerular and tubulointerstitial fibrosis, ultimately leading
to a reduction in the glomerular filtration rate (GFR) and
retention of uremic toxins. If disease progression is not
halted with therapy, the net result is chronic kidney disease
(CKD), end-stage renal disease (ESRD), and cardiovasculardisease. The diagnosis of CKD can be made without
knowledge of the specific cause.
The National Kidney Foundation defines CKD as (1)
evidence of kidney damage based on abnormal urinalysis
results (eg, proteinuria, hematuria) or structural
abnormalities observed on ultrasound images or (2) a GFR
of less than 60 mL/min for 3 or more months. Based on this
definition, the National Kidney Foundation developed
guidelines that classify the progression of renal disease into 5
stages, from kidney disease with a preserved GFR to end-
stage kidney failure. This classification includes treatment
strategies for each progressive level, as follows:
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
2/85
y Stage 1: This stage is characterized by kidney damagewith a normal GFR ( 90 mL/min). The action plan is
diagnosis and treatment, treatment of comorbidconditions, slowing of the progressing of kidney disease,
and reduction of cardiovascular disease risks.
y Stage 2: This stage is characterized by kidney damagewith a mild decrease in the GFR (60-90 mL/min). The
action plan is estimation of the progression of kidneydisease.
y Stage 3: This stage is characterized by a moderatelydecreased GFR (30-59 mL/min). The action plan is
evaluation and treatment of complications.
y Stage 4: This stage is characterized by a severe decreasein the GFR (15-29 mL/min). The action plan is
preparation for renal replacement therapy.
y Stage 5: This stage is characterized by kidney failure.The action plan is kidney replacement if the patient is
uremic.
At the later stages of glomerular injury, biopsy results
cannot help distinguish the primary disease. Histology and
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
3/85
clues to the etiology are often derived from other systemic
diseases, if present. Considerable cause-specific variability is
observed in the rate at which acute glomerulonephritisprogresses to chronic glomerulonephritis.
Pathophysiology
Reduction in nephron mass from the initial injury reduces
the GFR. This reduction leads to hypertrophy and
hyperfiltration of the remaining nephrons and to the
initiation of intraglomerular hypertension. These changes
occur in order to increase the GFR of the remaining
nephrons, thus minimizing the functional consequences of
nephron loss. The changes, however, are ultimately
detrimental because they lead to glomerulosclerosis and
further nephron loss.
In early renal disease (stages 1-3), a substantial decline in the
GFR may lead to only slight increases in serum creatinine
levels. Azotemia (ie, a rise in BUN and serum creatinine
levels) is apparent when the GFR decreases to less than 60-
70 mL/min. In addition to a rise in BUN and
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
4/85
creatininelevels, the substantial reduction in the GFR results
in decreased production of (1) erythropoietin, thus resulting
in anemia; (2) decreased production of vitamin D, resultingin hypocalcemia, secondary hyperparathyroidism,
hyperphosphatemia, and renal osteodystrophy; (3) reduction
in acid, potassium, salt, and water excretion, resulting in
acidosis, hyperkalemia, hypertension, and edema; and (4)
platelet dysfunction, leading to increased bleedingtendencies.
Accumulation of toxic waste products (uremic toxins) affects
virtually all organ systems. Azotemia occurring with the
signs and symptoms listed above is known as uremia.
Uremia occurs at a GFR of approximately 10 mL/min. Some
of these toxins (eg, BUN, creatinine, phenols, guanidines)
have been identified, but none has been found to be
responsible for all the symptoms.
Epidemiology
Frequency
United States
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
5/85
Chronic glomerulonephritis is the third leading cause of
ESRD and accounts for 10% of patients on dialysis in the
United States.
International
Chronic glomerulonephritis accounted for up to 40% of
patients on dialysis in Japan and some Asian countries.
However, more recent data suggest that, in Japan forinstance, the rate of chronic glomerulonephritis in patients
on dialysis is 28%. The cause of this declining rate is not
known. Concurrent with the decline in chronic
glomerulonephritis in these countries is an increase in
diabetic nephropathy in up to 40% of patients on dialysis.
Mortality/Morbidity
ESRD and death are common outcomes unless renal
replacement therapy is instituted.
Physical
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
6/85
Cause-specific physical examination findings are discussed
in articles on the specific causes. See Causes for links to such
articles.
y Uremia-specific findingso Hypertensiono Jugular venous distension (if severe volume
overload is present)
o Pulmonary rales (if pulmonary edema is present)o Pericardial friction rub in pericarditiso Tenderness in the epigastric region or blood in the
stool (possible indicators for uremic gastritis or
enteropathy)
o Decreased sensation and asterixis (indicators foradvanced uremia)
Causes
The progression from acute glomerulonephritis to chronic
glomerulonephritis is variable. Whereas complete recovery
of renal function is the rule for patients with
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
7/85
poststreptococcal glomerulonephritis, several other
glomerulonephritides, such as immunoglobulin A (IgA)
nephropathy, often have a relatively benign course andmany do not progress to ESRD.
y Rapidly progressive glomerulonephritis or crescenticglomerulonephritis: Approximately 90% of patients
progress to ESRD within weeks or months.
y Focal segmental glomerulosclerosis: Approximately80% of patients progress to ESRD in 10 years. Patients
with the collapsing variant, which is termed malignant
focal segmental glomerulosclerosis, have a more rapid
progression. This form may be idiopathic or related to
HIV infection.
y Membranous nephropathy: Approximately 20-30% ofpatients with membranous nephropathy progress to
chronic renal failure (CRF) and ESRD in 10 years.
y Membranoproliferative glomerulonephritis:Approximately 40% of patients with
membranoproliferative glomerulonephritis progress to
CRF and ESRD in 10 years.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
8/85
y IgA nephropathy: Approximately 10% of patients withIgA nephropathy progress to CRF and ESRD in 10
years.
[1]
y Poststreptococcal glomerulonephritis: Approximately 1-2% of patients with poststreptococcal
glomerulonephritis progress to CRF and ESRD. Older
children who present with crescentic
glomerulonephritis are at greatest risk.y Lupus nephritis: Overall, approximately 20% of
patients with lupus nephritis progress to CRF and
ESRD in 10 years; however, patients with certain
histologic variants (eg, class IV) may have a more rapid
decline.
Differentials
y Azotemiay Chronic Renal Failurey Glomerulonephritis, Acutey Glomerulonephritis, Crescenticy Glomerulonephritis, Diffuse Proliferative
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
9/85
y Glomerulonephritis, Membranoproliferativey Glomerulonephritis, Membranousy
Glomerulonephritis, Nonstreptococcal Associated WithInfection
y Glomerulonephritis, Poststreptococcaly Glomerulonephritis, Rapidly Progressivey Uremia
Laboratory Studies
y Urinalysiso The presence of dysmorphic RBCs, albumin, or
RBC casts suggests glomerulonephritis as the cause
of renal failure.
o Waxy or broad casts are observed in all forms ofCKD, including chronic glomerulonephritis.
o Low urine-specific gravity indicates loss of tubularconcentrating ability, an early finding in persons
with CDK.
y Urinary protein excretion
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
10/85
o This can be estimated by calculating the protein-to-creatinine ratio on a spot morning urine sample.
The ratio of urinary protein concentration (inmg/dL) to urinary creatinine (in mg/dL) reflects
24-hour protein excretion in grams. For instance, if
the spot urine protein value is 300 mg/dL and the
creatinine value is 150 mg/dL, then the ratio is 300
divided by 150, which equals 2. Thus, in thisexample, the 24-hour urine protein excretion is 2 g.
o The estimated creatinine clearance rate is used toassess and monitor the GFR. The 2 formulas
available to calculate the value are the Cockroft-
Gault formula, which estimates creatinine
clearance, and the Modification of Diet in Renal
Disease Study (MDRD) formula, which is used to
calculate the GFR. The Cockroft-Gault formula is
simple to use but overestimates the GFR by 10-
15% because creatinine is both filtered and
secreted. The MDRD formula is much more
complex but is available as a PDA through the
National Kidney Foundation or can be calculated
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
11/85
online through the Hypertension, Dialysis, and
Clinical Nephrology Web site.
oThe estimated creatinine clearance rate is also usedto monitor response to therapy and to initiate an
early transition to renal replacement therapy (eg,
dialysis access placement, transplantation
evaluation). The degree of proteinuria, especially
albuminuria, helps predict renal prognosis inpatients with chronic glomerulonephritis. Patients
with greater than 1 g/d have an increased risk of
progression to ESRD.
o In a study of 38 patients with chronic
glomerulonephritis, Hayakawa et al examined the
relationship between plasma adiponectin, leptin,
and proteinuria levels; glomerular filtration rate;
and metabolic risk factors.[2] They found that
plasma adiponectin levels were much higher in
patients with heavy proteinuria (38.8 +/- 27.8
g/mL) than they were in patients who had mild
(13.3 +/- 5.1 g/mL, P < 0.001) or moderate
proteinuria (18.1 +/- 8.0 g/mL, P < 0.01). Serum
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
12/85
leptin levels, however, did not differ according to
the degree of proteinuria.
yCBC count
o Anemia is a significant finding in patients withsome decline in the GFR.
o Physicians must be aware that anemia can occureven in patients with serum creatinine levels of less
than 2 mg/dL. Even severe anemia can occur at lowserum creatinine levels. Anemia is the result of
marked impairment of erythropoietin production.
y Serum chemistryo Serum creatinine and urea nitrogen levels are
elevated.
o Impaired excretion of potassium, free water, andacid results in hyperkalemia, hyponatremia, and
low serum bicarbonate levels, respectively.
o Impaired vitamin D-3 production results in
hypocalcemia, hyperphosphatemia, and high levels
of parathyroid hormone.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
13/85
o Low serum albumin levels may be present ifuremia interferes with nutrition or if the patient is
nephrotic.
Imaging Studies
y Renal ultrasonogramo Obtain a renal ultrasonogram to determine renal
size, to assess for the presence of both kidneys, and
to exclude structural lesions that may be
responsible for azotemia.
o Small kidneys often indicate an irreversibleprocess.
Procedures
y Kidney biopsyo If the kidney is small, kidney biopsy is usually
unnecessary; no specific pattern of disease can be
discerned at this point.
o A kidney biopsy may be considered in the minorityof patients who exhibit an acute exacerbation of
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
14/85
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
15/85
hypocalcemia, hyperparathyroidism) before renal
replacement therapy. Also, aggressively manage comorbid
conditions, such as heart disease and diabetes.
y The target pressure for patients with proteinuriagreater than 1 g/d is less than 125/75 mm Hg; for
patients with proteinuria less than 1 g/d, the target
pressure is less than 130/80 mm Hg.
o Angiotensin-converting enzyme inhibitors (ACEIs)are commonly used and are usually the first choice
for treatment of hypertension in patients with
CRF. ACEIs are renoprotective agents that have
additional benefits beyond lowering pressure.
ACEIs effectively reduce proteinuria, in part by
reducing the efferent arteriolar vascular tone,
thereby decreasing intraglomerular hypertension.
Particularly, ACEIs have been shown to be
superior to conventional therapy in slowing the
decline of the GFR in patients with diabetic and
nondiabeticproteinuric nephropathies. Therefore,
consider ACEIs for treatment of even
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
16/85
normotensive patients with significant
proteinuria.[3]
oThe role of angiotensin II receptor blockers (ARBs)in renal protection is increasingly being
established, and these medications have been found
to retard the progression of CKD in patients with
diabetic or nondiabetic nephropathy in a manner
similar to that of ACEIs.o Combination therapy with ACEIs and ARBs has
been shown to confer superior pressure control and
preservation of renal function than either therapy
alone. Therefore, in patients without hyperkalemia
or an acute rise in serum creatinine levels following
the use of either therapy, combination therapy
should be attempted.
o Diuretics are often required because of decreasedfree-water clearance, and high doses may be
required to control edema and hypertension when
the GFR falls to less than 25 mL/min. Diuretics are
also useful in counteracting the hyperkalemic
potential of ACEIs and ARBs. However, diuretics
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
17/85
should be used with caution when given together
with ACEIs or ARBs because the decline in
intraglomerular pressure induced by ACEIs orARBs may be exacerbated by volume depletion
induced by diuretics, potentially precipitating acute
renal failure.
o Beta-blockers, calcium channel blockers, central
alpha-2 agonists (eg, clonidine), alpha-1antagonists, and direct vasodilators (eg, minoxidil,
nitrates) may be used to achieve the target
pressure.
y Because progressive fibrosis is the hallmark of chronic
glomerulonephritis, some investigators have focused
their work on finding inhibitors of fibrosis in an
attempt to slow progression. Of many compounds,
pirfenidone, an inhibitor of transforming growth factor
beta, and hence of collagen synthesis, has emerged as
the candidate compound. Cho et al performed an open
label study on 21 patients with idiopathic and
postadaptive focal segmental glomerulosclerosis.[4] They
found a median 25% improvement in the rate of decline
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
18/85
of the estimated GFR (P < 0.01). Pirfenidone did not
effect proteinuria or blood pressure. Among the adverse
events attributed to therapy were dyspepsia, sedation,and photosensitive dermatitis. Pirfenidone offers hope
in slowing progressive fibrosis; however, more studies
are needed.
y Renal osteodystrophy can be managed early by
replacing vitamin D and by administering phosphatebinders. Seek and treat nonuremic causes of anemia,
such as iron deficiency, before instituting therapy with
erythropoietin.
y Discuss options for renal replacement therapy (eg,
hemodialysis, peritoneal dialysis, renal transplantation).
Arrange permanent vascular access when the GFR
decreases to less than 20-25 mL/min, when the serum
creatinine level is greater than 4 mg/dL, or if the rate of
rise in the serum creatinine level indicates the need for
dialysis within 1 year. Arteriovenous fistulas are
preferred to arteriovenous grafts because of their long-
term high-patency rates and should be placed whenever
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
19/85
possible. Place peritoneal dialysis catheters 2-3 weeks
prior to anticipated dialysis therapy.
yTreat hyperlipidemia (if present) to reduce overallcardiovascular comorbidity, even though evidence for
renal protection is lacking.
y Expose patients to educational programs for earlyrehabilitation from dialysis or transplantation.
y Surgical Carey Create access for dialysis when the GFR decreases to
less than 25 mL/min
Consultations
y Nephrologists: Early referral of patients with CRF to anephrologist is important for the management of
complications and the organization of the transition to
renal replacement therapy (eg, hemodialysis, peritoneal
dialysis, renal transplantation). Some evidence indicates
that early referral of a patient with CRF (serum
creatinine, 1.5-2 mg/dL) to a nephrologist improves the
short-term outcome.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
20/85
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
21/85
y Encourage patients to increase their activity level astolerated. Increased activity may aid in blood pressure
control
y Medication Summary
y The goals of pharmacotherapy are to reduce morbidityand to prevent complications.
y Angiotensin-converting enzyme inhibitors
y Class Summaryy For renoprotection. Decrease intraglomerular pressure
and, consequently, glomerular protein filtration, by
decreasing efferent arteriolar constriction.[3]
y View full drug information
y Enalapril (Vasotec)y Competitive inhibitor of ACE. Reduces angiotensin II
levels, thus decreases aldosterone secretion. Decreases
intraglomerular pressure and glomerular protein
filtration by decreasing efferent arteriolar constriction.
y Diuretics
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
22/85
y Class Summaryy Treat edema and hypertension. Increase urine excretion
by inhibiting sodium and chloride transporters.
y View full drug information
y Furosemide (Lasix)y DOC as a diuretic. Increases excretion of water by
interfering with chloride-binding cotransport system,
which, in turn, inhibits sodium and chloride
reabsorption in ascending loop of Henle and distal renal
tubule.
y View full drug information
y Metolazo
ne (
Mykrox, Zaroxoly
n)
y Treats edema in congestive heart failure. Increasesexcretion of sodium, water, potassium, and hydrogen
ions by inhibiting reabsorption of sodium in distal
tubules. May be more effective in impaired renal
function.
y Calcium channel blockers
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
23/85
y Class Summaryy Treat hypertension, angina, and atrial fibrillation.[5]
y View full drug informationy Amlodipine (Norvasc)y Blocks slow calcium channels, causing relaxation of
vascular smooth muscles.
y View full drug information
y Nifedipine (Procardia)y Relaxes coronary smooth muscle and produces
coronary vasodilation, which, in turn, improves
myocardial oxygen delivery. SL administration
generally safe, despite theoretical concerns.
y Beta-adrenergic blockers
y Class Summaryy Compete with beta-adrenergic agonists for available
beta-receptor sites. Propranolol, nadolol, timolol,
penbutolol, carteolol, sotalol, and pindolol inhibit both
beta-1 receptors (located mainly in cardiac muscle) and
beta-2 receptors (located mainly in bronchial and
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
24/85
vascular musculature), thus inhibiting chronotropic,
inotropic, and vasodilatory responses to beta-adrenergic
stimulation.
y View full drug information
y Metoprolol (Lopressor)y Selective beta1-adrenergic receptor blocker that
decreases automaticity of contractions. During IV
administration, carefully monitor blood pressure, heart
rate, and ECG.
y Alpha-adrenergic agonists
y Class Summaryy Used in combination with other agents for management
of hypertension.
y View full drug information
y Clonidine (Catapres)y
Stimulates presynaptic (central) alpha-2 agonist,thereby reducing norepinephrine release and peripheral
vasoconstriction
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
25/85
y Further Inpatient Care
y Patients with CKD admitted to the hospital should have
careful monitoring of weight, intake, output, and renal
function so that acute renal failure, if it occurs, can be
diagnosed and treated early. All potentially nephrotoxic
agents must be adjusted for the degree of CKD.
Furthermore, agents, such as nonsteroidal anti-
inflammatory drugs (NSAIDs), aminoglycosides, and
intravenous contrast, must be avoided, unless the
benefits clearly outweigh the risks, because these agents
are highly associated with acute renal failure.
yFurther Outpatient Care
y Patients with any evidence of kidney disease should bereferred to a kidney specialist (nephrologist). Data
suggest that early referral to a nephrologist improves
the overall outcome. The nephrologist will usually
determine the frequency of visits based on the degree of
CKD.
Complications
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
26/85
y The presence of the following complications generallyindicates a need for urgent dialysis:
oMetabolic acidosis
o Pulmonary edemao Pericarditiso Uremic encephalopathyo Uremic gastrointestinal bleeding
o Uremic neuropathyo Severe anemia and hypocalcemiao Hyperkalemia
y Prognosis
y The prognosis depends on the type of chronicglomerulonephritis (see Causes).
Patient Education
y For further information, see Mayo Clinic - KidneyTransplant Information.
y Dietary education is paramount in managing patientswith CKD. The typical dietary restriction is 2 g of
sodium, 2 g of potassium, and 40-60 g of protein a day.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
27/85
Additional restrictions may apply for diabetes,
hyperlipidemia, and fluid overload.
yPatients should be educated regarding the types ofESRD therapy. The specific choices of ESRD therapy
include hemodialysis, peritoneal dialysis, and renal
transplantation.
o Patients opting for hemodialysis should be
educated on home hemodialysis (ie, patients aretrained to do their dialysis at home) and center
hemodialysis (ie, patients must come to a center 3
times a week for 3.5- to 4-hour dialysis sessions).
They should also be educated on the types of
vascular access. Arteriovenous fistulae should be
created when the GFR falls below 25 mL/min or
the serum creatinine level is greater than 4 mg/dL
to allow for maturation of the access prior to the
initiation of dialysis.
o Peritoneal dialysis catheters can be placed ifdialysis is anticipated within 2-3 weeks.
o Preemptive transplantation before the initiation ofdialysis improves survival as compared with
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
28/85
transplantation after the initiation of dialysis;
therefore, preemptive transplantation should be
explored from live donors. In patients without livedonors, they can be placed on the deceased donor
wait list when the GFR falls below 20 mL/min to
accrue time. Patients who opt for no treatment
when it is indicated should be informed of
imminent renal failure in a shorter time.y In the United States and most developed countries,
patients on dialysis can travel. In fact, there are even
dialysis cruises. However, patients should inform their
social workers to make the necessary arrangements
prior to any travel to ensure that the destination has the
right resources to continue dialysis.
y Sexual dysfunction and loss of libido is common inpatients with kidney disease, especially in men. Patients
should be told to seek medical therapy if they
experience these symptoms
Adult Dosing & Uses
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
29/85
Dosing Forms & Strengths
injectable solution
y 1.25mg/mL
oral solution
y 1mg/mL
tablet
y 2.5mgy 5mgy 10mgy 20mg
Hypertension
Initial: 2.5-5 mg PO qDay
Maintenance: 10-40 mg/day PO qDay or divided BID
Left Ventricular Dysfunction
Initial 2.5 mg PO BID, may titrate up to 20 mg/day
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
30/85
Congestive Heart Failure
Initial: 2.5 mg PO qDay/BID
Maintenance: 5-20 mg/day PO
IV: 1.25-5 mg q6hr
Renal Impairment
CrCl
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
31/85
Good choice in hyperlipidemia pts
Requires weeks for full effect; to start, use low dose & titrate
q1-2wk
Abrupt discontinuance not associated with rapid increase in
BP
See also combo with HCTZ
Other Indications & Uses
Off-label: Diabetic nephropathy
Pediatric Dosing & Uses
Dosing Forms & Strengths
injectable solution
y 1.25mg/mL
oral solution
y 1mg/mL
tablet
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
32/85
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
33/85
inhibitors. D/C ACE inhibitor 72h prior to use of
protein A column.
Serious - Use Alternative (2)
y allopurinol
enalapril, allopurinol. Mechanism: unknown. Serious -
Use Alternative.Risk of anaphylaxis, Stevens Johnson
syndrome.
y pregabalin
enalapril, pregabalin. Either increases toxcity of the
other by pharmacodynamic synergism. Serious - Use
Alternative.Additive risk of developing angioedema of
face, mouth, and neck, including respiratory
compromise.
Significant - Monitor Closely (98)
y acetohexamide
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
34/85
enalapril increases effects of acetohexamide by
pharmacodynamic synergism. Significant - Monitor
Closely.
y aldesleukin
aldesleukin increases effects of enalapril by
pharmacodynamic synergism. Significant - Monitor
Closely. Risk of hypotension.
y alfuzosin
enalapril, alfuzosin. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Exaggerated
first dose hypotensive response.
y aluminum hydroxide
aluminum hydroxide decreases effects of enalapril by
unspecified interaction mechanism. Significant -
Monitor Closely.
y amifostine
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
35/85
amifostine increases effects of enalapril by
pharmacodynamic synergism. Significant - Monitor
Closely. Risk of hypotension.
y amiloride
enalapril, amiloride. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Risk of
hyperkalemia.
y asenapine
enalapril, asenapine. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Exaggerated
first dose hypotensive response.
y aspirin
aspirin decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
36/85
enalapril, aspirin. Either increases toxcity of the other
by Other (see comment). Significant - Monitor Closely.
Comment: May result in renal function deterioration,particularly in elderly or volume depleted individuals.
y azathioprine
enalapril, azathioprine. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Risk ofneutropenia.
y bumetanide
enalapril, bumetanide. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Risk of acutehypotension, renal insufficiency.
y calcium carbonate
calcium carbonate decreases effects of enalapril by
unspecified interaction mechanism. Significant -Monitor Closely.
y carbamazepine
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
37/85
enalapril increases levels of carbamazepine by
decreasing metabolism. Significant - Monitor Closely.
y carbidopa
carbidopa increases effects of enalapril by
pharmacodynamic synergism. Significant - Monitor
Closely. Consider decreasing dosage of antihypertensive
agent.
y carbonyl iron
enalapril, carbonyl iron. Mechanism: unknown.
Significant - Monitor Closely. Risk of GI symptoms,
hypotension.
y celecoxib
celecoxib decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
38/85
enalapril, celecoxib. Either increases toxcity of the other
by Other (see comment). Significant - Monitor Closely.
Comment: May result in renal function deterioration,particularly in elderly or volume depleted individuals.
y chlorpropamide
enalapril increases effects of chlorpropamide by
pharmacodynamic synergism. Significant - MonitorClosely.
y choline magnesium trisalicylate
choline magnesium trisalicylate decreases effects of
enalapril by pharmacodynamic antagonism. Significant- Monitor Closely. NSAIDs decrease synthesis of
vasodilating renal prostaglandins, and thus affect fluid
homeostasis and may diminish antihypertensive effect.
enalapril, choline magnesium trisalicylate. Eitherincreases toxcity of the other by Other (see comment).
Significant - Monitor Closely. Comment: May result in
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
39/85
renal function deterioration, particularly in elderly or
volume depleted individuals.
y cyclosporine
enalapril increases levels of cyclosporine by unknown
mechanism. Significant - Monitor Closely.
enalapril, cyclosporine. Mechanism: unspecifiedinteraction mechanism. Significant - Monitor Closely.
Risk of acute renal failure.
y diclofenac
diclofenac decreases effects of enalapril bypharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, diclofenac. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal function
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
40/85
deterioration, particularly in elderly or volume depleted
individuals.
y diflunisal
diflunisal decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasisand may diminish antihypertensive effect.
enalapril, diflunisal. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal functiondeterioration, particularly in elderly or volume depleted
individuals.
y digoxin
enalapril increases levels of digoxin by unspecifiedinteraction mechanism. Significant - Monitor Closely.
y doxazosin
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
41/85
enalapril, doxazosin. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Exaggerated
first dose hypotensive response.
y drospirenone
enalapril, drospirenone. Mechanism:
pharmacodynamic synergism. Significant - Monitor
Closely. Risk of hyperkalemia.
y eplerenone
enalapril, eplerenone. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Risk of
hyperkalemia.
y ethacrynic acid
enalapril, ethacrynic acid. Mechanism:
pharmacodynamic synergism. Significant - Monitor
Closely. Risk of acute hypotension, renal insufficiency.
y etodolac
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
42/85
etodolac decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, etodolac. Either increases toxcity of the other
by Other (see comment). Significant - Monitor Closely.Comment: May result in renal function deterioration,
particularly in elderly or volume depleted individuals.
y exenatide
enalapril increases effects of exenatide by Other (seecomment). Significant - Monitor Closely. Comment:
ACE inhibitors may increase hypoglycemic effect.
Monitor glycemic control especially during the first
month of treatment with an ACE inhibitor. .
y fenoprofen
fenoprofen decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
43/85
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, fenoprofen. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal function
deterioration, particularly in elderly or volume depletedindividuals.
y ferric carboxymaltose
enalapril, ferric carboxymaltose. Mechanism: unknown.
Significant - Monitor Closely. Risk of GI symptoms,hypotension.
y ferric gluconate
enalapril, ferric gluconate. Mechanism: unknown.
Significant - Monitor Closely. Risk of GI symptoms,hypotension.
y ferrous fumarate
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
44/85
enalapril, ferrous fumarate. Mechanism: unknown.
Significant - Monitor Closely. Risk of GI symptoms,
hypotension.
y ferrous sulfate
enalapril, ferrous sulfate. Mechanism: unknown.
Significant - Monitor Closely. Risk of GI symptoms,
hypotension.
y floctafenine
floctafenine decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, floctafenine. Either increases toxcity of the
other by Other (see comment). Significant - MonitorClosely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
45/85
y flurbiprofen
flurbiprofen decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, flurbiprofen. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
y furosemide
enalapril, furosemide. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Risk of acute
hypotension, renal insufficiency.
y glimepiride
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
46/85
enalapril increases effects of glimepiride by
pharmacodynamic synergism. Significant - Monitor
Closely.
y glipizide
enalapril increases effects of glipizide by
pharmacodynamic synergism. Significant - Monitor
Closely.
y gliquidone
enalapril increases effects of gliquidone by
pharmacodynamic synergism. Significant - Monitor
Closely.
y glyburide
enalapril increases effects of glyburide by
pharmacodynamic synergism. Significant - Monitor
Closely.
y gold sodium thiomalate
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
47/85
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
48/85
indomethacin decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, indomethacin. Either increases toxcity of the
other by Other (see comment). Significant - MonitorClosely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
y insulin aspart
enalapril increases effects of insulin aspart by
pharmacodynamic synergism. Significant - Monitor
Closely.
y insulin detemir
enalapril increases effects of insulin detemir by
pharmacodynamic synergism. Significant - Monitor
Closely.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
49/85
y insulin glargine
enalapril increases effects of insulin glargine by
pharmacodynamic synergism. Significant - Monitor
Closely.
y insulin glulisine
enalapril increases effects of insulin glulisine by
pharmacodynamic synergism. Significant - Monitor
Closely.
y insulin lispro
enalapril increases effects of insulin lispro by
pharmacodynamic synergism. Significant - Monitor
Closely.
y insulin nph
enalapril increases effects of insulin nph by
pharmacodynamic synergism. Significant - Monitor
Closely.
y insulin regular human
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
50/85
enalapril increases effects of insulin regular human by
pharmacodynamic synergism. Significant - Monitor
Closely.
y iron dextran complex
enalapril, iron dextran complex. Mechanism: unknown.
Significant - Monitor Closely. Risk of GI symptoms,
hypotension.
y iron sucrose
enalapril, iron sucrose. Mechanism: unknown.
Significant - Monitor Closely. Risk of GI symptoms,
hypotension.
y itraconazole
itraconazole increases levels of enalapril by decreasing
metabolism. Significant - Monitor Closely.
y ketoconazole
ketoconazole increases levels of enalapril by decreasing
metabolism. Significant - Monitor Closely.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
51/85
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
52/85
enalapril, ketorolac. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal functiondeterioration, particularly in elderly or volume depleted
individuals.
y ketorolac intranasal
ketorolac intranasal decreases effects of enalapril bypharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, ketorolac intranasal. Either increases toxcity
of the other by Other (see comment). Significant -
Monitor Closely. Comment: May result in renal
function deterioration, particularly in elderly or volume
depleted individuals.
y levodopa
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
53/85
levodopa increases effects of enalapril by
pharmacodynamic synergism. Significant - Monitor
Closely. Consider decreasing dosage of antihypertensiveagent.
y liraglutide
enalapril increases effects of liraglutide by unknown
mechanism. Significant - Monitor Closely. ACEinhibitors may increase hypoglycemic effect. Monitor
glycemic control especially during the first month of
treatment with an ACE inhibitor. .
y lithium
enalapril increases toxcity of lithium by unknown
mechanism. Significant - Monitor Closely. ACE
inhibitor induced Na+ depletion may increase
reabsorption of lithium from renal tubule.
y lurasidone
lurasidone increases effects of enalapril by Other (see
comment). Significant - Monitor Closely. Comment:
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
54/85
Potential for increased risk of hypotension with
concurrent use. Monitor blood pressure and adjust dose
of antihypertensive agent as needed.
y meclofenamate
meclofenamate decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, meclofenamate. Either increases toxcity of the
other by Other (see comment). Significant - MonitorClosely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
y mefenamic acid
mefenamic acid decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
55/85
prostaglandins, and thus affect fluid homeostasis and
may diminish antihypertensive effect.
enalapril, mefenamic acid. Either increases toxcity of
the other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
y meloxicam
meloxicam decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, meloxicam. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
56/85
y moxisylyte
enalapril, moxisylyte. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Exaggerated
first dose hypotensive response.
y nabumetone
nabumetone decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, nabumetone. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
y naproxen
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
57/85
naproxen decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, naproxen. Either increases toxcity of the
other by Other (see comment). Significant - MonitorClosely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
y oxaprozin
oxaprozin decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, oxaprozin. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
58/85
Closely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
y phenoxybenzamine
enalapril, phenoxybenzamine. Mechanism:
pharmacodynamic synergism. Significant - Monitor
Closely. Exaggerated first dose hypotensive response.
y phentolamine
enalapril, phentolamine. Mechanism:
pharmacodynamic synergism. Significant - Monitor
Closely. Exaggerated first dose hypotensive response.
y phenylbutazone
phenylbutazone decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
59/85
enalapril, phenylbutazone. Either increases toxcity of
the other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal functiondeterioration, particularly in elderly or volume depleted
individuals.
y piroxicam
piroxicam decreases effects of enalapril bypharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, piroxicam. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
y polysaccharide iron
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
60/85
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
61/85
enalapril, prazosin. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Exaggerated
first dose hypotensive response.
y rofecoxib
rofecoxib, enalapril. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Risk of
hyperkalemia.
rofecoxib decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasisand may diminish antihypertensive effect.
enalapril, rofecoxib. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
62/85
y rose hips
enalapril, rose hips. Mechanism: unknown. Significant -
Monitor Closely. Risk of GI symptoms, hypotension.
y salsalate
salsalate decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, salsalate. Either increases toxcity of the other
by Other (see comment). Significant - Monitor Closely.
Comment: May result in renal function deterioration,
particularly in elderly or volume depleted individuals.
y silodosin
enalapril, silodosin. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Exaggerated
first dose hypotensive response.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
63/85
y sodium bicarbonate
sodium bicarbonate decreases effects of enalapril by
unspecified interaction mechanism. Significant -
Monitor Closely.
y sodium citrate/citric acid
sodium citrate/citric acid decreases effects of enalapril
by unspecified interaction mechanism. Significant -
Monitor Closely.
y spironolactone
enalapril, spironolactone. Mechanism:
pharmacodynamic synergism. Significant - Monitor
Closely. Risk of hyperkalemia.
y sulfamethoxazole
sulfamethoxazole, enalapril. Mechanism:
pharmacodynamic synergism. Significant - Monitor
Closely. Risk of hyperkalemia.
y sulfasalazine
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
64/85
sulfasalazine decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, sulfasalazine. Either increases toxcity of the
other by Other (see comment). Significant - MonitorClosely. Comment: May result in renal function
deterioration, particularly in elderly or volume depleted
individuals.
y sulindac
sulindac decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, sulindac. Either increases toxcity of the other
by Other (see comment). Significant - Monitor Closely.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
65/85
Comment: May result in renal function deterioration,
particularly in elderly or volume depleted individuals.
y tenoxicam
tenoxicam decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasisand may diminish antihypertensive effect.
enalapril, tenoxicam. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal functiondeterioration, particularly in elderly or volume depleted
individuals.
y terazosin
enalapril, terazosin. Mechanism: pharmacodynamicsynergism. Significant - Monitor Closely. Exaggerated
first dose hypotensive response.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
66/85
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
67/85
enalapril increases effects of tolbutamide by
pharmacodynamic synergism. Significant - Monitor
Closely.
y tolmetin
tolmetin decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilatingrenal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
enalapril, tolmetin. Either increases toxcity of the other
by Other (see comment). Significant - Monitor Closely.Comment: May result in renal function deterioration,
particularly in elderly or volume depleted individuals.
y torsemide
enalapril, torsemide. Mechanism: pharmacodynamicsynergism. Significant - Monitor Closely. Risk of acute
hypotension, renal insufficiency.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
68/85
y triamterene
enalapril, triamterene. Mechanism: pharmacodynamic
synergism. Significant - Monitor Closely. Risk of
hyperkalemia.
y trimethoprim
trimethoprim and enalapril both increase serum
potassium. Significant - Monitor Closely. Trimethoprim
decreases urinary potassium excretion. May cause
hyperkalemia, particularly with high doses, renal
insufficiency, or when combined with other drugs that
cause hyperkalemia.
y valdecoxib
valdecoxib decreases effects of enalapril by
pharmacodynamic antagonism. Significant - Monitor
Closely. NSAIDs decrease synthesis of vasodilating
renal prostaglandins, and thus affect fluid homeostasis
and may diminish antihypertensive effect.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
69/85
enalapril, valdecoxib. Either increases toxcity of the
other by Other (see comment). Significant - Monitor
Closely. Comment: May result in renal functiondeterioration, particularly in elderly or volume depleted
individuals.
y xipamide
xipamide increases effects of enalapril bypharmacodynamic synergism. Significant - Monitor
Closely.
y zotepine
enalapril, zotepine. Mechanism: pharmacodynamicsynergism. Significant - Monitor Closely. Exaggerated
first dose hypotensive response.
Minor (39)
yaceclofenac
aceclofenac decreases effects of enalapril by
pharmacodynamic antagonism. Minor or non-
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
70/85
significant interaction. NSAIDs decrease prostaglandin
synthesis.
y acemetacin
acemetacin decreases effects of enalapril by
pharmacodynamic antagonism. Minor or non-
significant interaction. NSAIDs decrease prostaglandin
synthesis.
y agrimony
agrimony increases effects of enalapril by
pharmacodynamic synergism. Minor or non-significant
interaction.
y albumin
albumin, enalapril. Mechanism: unspecified interaction
mechanism. Minor or non-significant
interaction.Vasodilation.
y aspirin rectal
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
71/85
aspirin rectal decreases effects of enalapril by
pharmacodynamic antagonism. Minor or non-
significant interaction. NSAIDs decrease prostaglandinsynthesis.
y brimonidine
brimonidine increases effects of enalapril by
pharmacodynamic synergism. Minor or non-significantinteraction.
y capsicum
capsicum, enalapril. Mechanism: pharmacodynamic
synergism. Minor or non-significant interaction.Increase ACE inhibitor induced cough.
y chlorpromazine
chlorpromazine increases effects of enalapril by
unspecified interaction mechanism. Minor or non-significant interaction.
y cornsilk
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
72/85
cornsilk increases effects of enalapril by
pharmacodynamic synergism. Minor or non-significant
interaction.
y creatine
creatine, enalapril. Mechanism: pharmacodynamic
synergism. Minor or non-significant interaction.
(Theoretical interaction) Combination may haveadditive nephrotoxic effects.
y etoricoxib
etoricoxib decreases effects of enalapril by
pharmacodynamic antagonism. Minor or non-significant interaction. NSAIDs decrease prostaglandin
synthesis.
y fenbufen
fenbufen decreases effects of enalapril bypharmacodynamic antagonism. Minor or non-
significant interaction. NSAIDs decrease prostaglandin
synthesis.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
73/85
y fluphenazine
fluphenazine increases effects of enalapril by
unspecified interaction mechanism. Minor or non-
significant interaction.
y lofexidine
lofexidine increases effects of enalapril by
pharmacodynamic synergism. Minor or non-significant
interaction.
y lornoxicam
lornoxicam decreases effects of enalapril by
pharmacodynamic antagonism. Minor or non-
significant interaction. NSAIDs decrease prostaglandin
synthesis.
y maitake
maitake increases effects of enalapril by
pharmacodynamic synergism. Minor or non-significant
interaction.
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
74/85
y mercaptopurine
enalapril, mercaptopurine. Mechanism:
pharmacodynamic synergism. Minor or non-significant
interaction.Risk of neutropenia.
y mesoridazine
mesoridazine increases effects of enalapril by
unspecified interaction mechanism. Minor or non-
significant interaction.
y nesiritide
nesiritide, enalapril. Either increases effects of the other
by pharmacodynamic synergism. Minor or non-
significant interaction.Additive hypotensive effects.
y octacosanol
octacosanol increases effects of enalapril by
pharmacodynamic synergism. Minor or non-significant
interaction.
y parecoxib
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
75/85
parecoxib decreases effects of enalapril by
pharmacodynamic antagonism. Minor or non-
significant interaction. NSAIDs decrease prostaglandinsynthesis.
y pericyazine
pericyazine increases effects of enalapril by unspecified
interaction mechanism. Minor or non-significantinteraction.
y perphenazine
perphenazine increases effects of enalapril by
unspecified interaction mechanism. Minor or non-significant interaction.
y pipotiazine
pipotiazine increases effects of enalapril by unspecified
interaction mechanism. Minor or non-significantinteraction.
y probenecid
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
76/85
probenecid increases effects of enalapril by unspecified
interaction mechanism. Minor or non-significant
interaction.
y prochlorperazine
prochlorperazine increases effects of enalapril by
unspecified interaction mechanism. Minor or non-
significant interaction.
y promazine
promazine increases effects of enalapril by unspecified
interaction mechanism. Minor or non-significant
interaction.
y promethazine
promethazine increases effects of enalapril by
unspecified interaction mechanism. Minor or non-
significant interaction.
y reishi
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
77/85
reishi increases effects of enalapril by
pharmacodynamic synergism. Minor or non-significant
interaction.
y rifampin
rifampin decreases levels of enalapril by increasing
metabolism. Minor or non-significant interaction.
y salicylates (non-asa)
salicylates (non-asa) decreases effects of enalapril by
pharmacodynamic antagonism. Minor or non-
significant interaction. NSAIDs decrease prostaglandin
synthesis.
y shepherd's purse
shepherd's purse, enalapril. Other (see comment).Minor
or non-significant interaction. Comment: Theoretically,
shepherd's purse may interfere with BP control.
y thioproperazine
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
78/85
thioproperazine increases effects of enalapril by
unspecified interaction mechanism. Minor or non-
significant interaction.
y thioridazine
thioridazine increases effects of enalapril by unspecified
interaction mechanism. Minor or non-significant
interaction.
y tizanidine
tizanidine increases effects of enalapril by
pharmacodynamic synergism. Minor or non-significant
interaction.Risk of hypotension.
y tolfenamic acid
tolfenamic acid decreases effects of enalapril by
pharmacodynamic antagonism. Minor or non-
significant interaction. NSAIDs decrease prostaglandinsynthesis.
y treprostinil
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
79/85
treprostinil increases effects of enalapril by
pharmacodynamic synergism. Minor or non-significant
interaction.
y trifluoperazine
trifluoperazine increases effects of enalapril by
unspecified interaction mechanism. Minor or non-
significant interaction.
y trimeprazine
trimeprazine increases effects of enalapril by
unspecified interaction mechanism. Minor or non-
significant interaction.
Adverse Effects
1-10%
Dizziness (4-8%)
Hypotension (0.9-6.7%)
Headache (2-5%)
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
80/85
Chest pain (2%)
Cough (1-2%)
Rash (1.5%)
Frequency not defined
Asthenia
Nausea
Vomiting
Hyperkalemia
Contraindications & Cautions
Black Box Warnings
Discontinue as soon as possible when pregnancy is detected;
affects renin-angiotensin system causing oligohydramnios,
which may result in fetal injury and/or death
Contraindications
Hypersensitivity to enalapril/other ACE inhibitors
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
81/85
History of ACEI-induced angioedema, hereditary or
idiopathic angioedema
Pregnancy (2nd & 3rd trimesters): significant risk of fetal &
neonatal morbidity & mortality
Bilateral renal artery stenosis
Cautions
Apheresis (LDL) with dextran sulfate, hypertrophic
cardiomyopathy, collagen vascular disease, hemodialysis
with high flux membrane, renal or arotic stenosis
For HTN pts on diuretics, if possible discontinue diuretics 2-
3 d before starting enalapril
Excessive hypotension if concomitant diuretics,
hypovolemia, hyponatremia
Risk of hyperkalemia, esp in pts w/ renal impairment, DM
or those taking concomitant K+-elevating drugs
Inj contains benzyl alcohol preservative (linked to
potentially fatal 'gasping syndrome' in preemies)
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
82/85
ACE inhibition also causes increased bradykinin levels
which putatively mediates angioedema
Discontinue STAT if pt becomes pregnant
Less effective in blacks
Renal impairment
Pregnancy & Lactation
Pregnancy Category: C (1st trimester); D (2nd & 3rd
trimesters). During the second and third trimesters of
pregnancy, these drugs have been associated with fetal
injury that includes hypotension, neonatal skull hypoplasia,
anuria, reversible or irreversible renal failure, and death.
Lactation: enters breast milk/not recommended (AAP
Committee states "compatible with nursing")
Pharmacology
Half-Life: parent drug: 1.3 hr, active met (enalaprilat): 11
hr
Onset
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
83/85
Initial response for HTN: IV: 0.5-4 hr, PO: 1-4 hr
Peak response for HTN: IV: 30 min, PO: 8-18 hr
Excretion
Urine: 61%
Feces: 33% (6% as enalapril, 27% as enalaprilat)
Other Information
Duration: IV: 360 min, PO (multiple dose): 12-24 hr
Peak Plasma Time: IV: 15 min; PO: 1 hr
Bioavailability: 60%
Protein Bound: 50-60%
Metabolism: liver (70%); enalapril undergoes hepatic
biotransformation to enalaprilat within 4 hr following oral
administration
Metabolites: enalaprilat (active)
Renal Clearance: 158 mL/min
Dialyzable: HD: yes
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
84/85
Mechanism of Action
Enalapril is a prodrug hydrolyzed in vivo to enalaprilat;
enalaprilat prevents conversion of angiotensin I to
angiotensin II (a potent vasoconstrictor) through competitive
inhibition of angiotensin coverting enzyme (ACE) resulting
in decreased plasma angiotensin II concentrations &
consequently, blood pressure may be reduced in part
through decreased vasoconstriction, increased renin activity,
and decreased aldosterone secretion
Also increases renal blood flow
IV & IM Information
IV Incompatibilities
Y-site: ampho B, ampho B chol SO4, cefepime, phenytoin
IV Compatibilities
Solution: D5W, Normosol R
Additive: dobutamine, dopamine, heparin, meropenem,
nitroglycerin, KCl, sodium nitroprusside
-
8/6/2019 Nearly All Forms of Acute Glomerulonephritis Have a Tendency to Progress to Chronic Glomerulonephritis
85/85
Y-site (partial list): allopurinol, ampicillin, ampicillin-
sulbactam, cefazolin, clindamycin, dobutamine, dopamine,
esmolol, fentanyl, heparin, labetalol, linezolid, MgSO4,metronidazole, morphine SO4, nicardipine, KCl, propofol,
tobramyin, TMP-SMX, vancomycin
IV Administration
Slow IVP over at least 5 min if undiluted, or
Infused in up to 50 mL of compatible IV infusion solution
Storage
Clear colorless solution
Store below 30C