Meckel’s Diverticulum Preoperatively Diagnosed by Double ...
Transcript of Meckel’s Diverticulum Preoperatively Diagnosed by Double ...

1023
□ CASE REPORT □
Meckel’s Diverticulum Preoperatively Diagnosed byDouble-balloon Endoscopy
Keisuke Taniuchi 1,2, Hajime Tanaka 1, Shinichi Iwamura 4 and Itsumi Mori 3
Abstract
Symptomatic Meckel’s diverticulum is an uncommon diagnosis in adults, and bleeding Meckel’s diverticu-
lum after childhood is even more infrequent. We present herein the case of a 22-year-old man with gastroin-
testinal hemorrhage secondary to Meckel’s diverticulum containing ectopic gastric mucosa. As the source of
bleeding could not be identified by upper and lower gastrointestinal endoscopy and visceral selective angiog-
raphy, the new methods of capsule endoscopy and double-balloon endoscopy were used. Capsule endoscopy
showed oozing hemorrhage in the ileum, and double-balloon endoscopy demonstrated a large diverticulum in
the distal part of the ileum. Tc-99m pertechnetate Meckel’s scan revealed an abnormal focus of uptake in the
right lower abdomen. The diverticulum was resected laparoscopically. The postoperative course was unevent-
ful, and the patient remains in complete remission as of this writing. Detecting Meckel’s diverticulum endo-
scopically is difficult prior to surgery, but a combination of capsule endoscopy and double-balloon endoscopy
facilitates examination of the entire small intestine, making precise diagnosis of Meckel’s diverticulum possi-
ble.
Key words: Meckel’s diverticulum, lower gastrointestinal hemorrhage, capsule endoscopy, double-balloon
endoscopy, laparotomy
(Intern Med 51: 1023-1026, 2012)(DOI: 10.2169/internalmedicine.51.6594)
Introduction
Meckel’s diverticulum is the most common congenital
anomaly of the gastrointestinal tract, with an incidence on
autopsy of 0.3-4% (1, 2). This condition derives from in-
complete obliteration of the yolk stalk (omphalo-mesenteric
duct). Meckel’s diverticulum is a true diverticulum, with all
of the layers of the intestinal wall present. The diverticulum
is located on the antimesenteric border of the ileum, about
40-130 cm proximal to the ileocecal valve, and it is usually
3-5 cm long (3). Since cells lining the vitelline duct are plu-
ripotent, heterotopic gastric mucosa (50%), pancreatic mu-
cosa (5%), and, less commonly, colonic mucosa, endometri-
osis, and hepatobiliary tissue, may be present, and these are
responsible for other complications like hemorrhage, chronic
peptic ulceration and perforation (4-6).
An individual with Meckel’s diverticulum has a 4-6%
lifetime risk of developing a complication (7). The most
common clinical presentation is gastrointestinal bleeding,
which occurs in 25-50% of patients showing complica-
tions (8). Colonoscopy cannot usually diagnose the bleeding
from Meckel’s diverticulum, as the colonoscope cannot typi-
cally reach the part of the small intestine in which the diver-
ticulum is located. Recent advances in diagnostic methods,
including capsule endoscopy (CE) (9) and double-balloon
endoscopy (DBE) (10), have enabled observation of the
source of small-bowel bleeding. CE has proved to be of di-
agnostic value in some cases of bleeding Meckel’s diverticu-
lum, but reports have been very few and no conclusive
statement regarding the diagnostic value of this method can
be made at this time (11). DBE enables examination of the
entire small intestine (12). Although Tc-99m pertechnetate
scintigraphy is useful, particularly in patients with ectopic
gastric tissue, sensitivity was reported as�60% in a study
of 235 patients with Meckel’s diverticulum and anemia (13).
1Department of Internal Medicine, Tosa Municipal Hospital, Japan, 2Department of Gastroenterology and Hepatology, Kochi University Medical
School, Japan, 3Department of Surgery, Tosa Municipal Hospital, Japan and 4Department of Gastroenterology, Kochi Red Cross Hospital, Japan
Received for publication September 21, 2011; Accepted for publication December 19, 2011
Correspondence to Dr. Keisuke Taniuchi, [email protected]

Intern Med 51: 1023-1026, 2012 DOI: 10.2169/internalmedicine.51.6594
1024
Figure 1. Capsule endoscopy shows oozing hemorrhage in the ileum.
Preoperative diagnosis of a complicated Meckel’s diverticu-
lum may be challenging, because the clinical and imaging
features overlap with those of other causes of acute abdo-
men (14). We were able to identify small bowel bleeding us-
ing CE and visualize Meckel’s diverticulum of the ileum us-
ing DBE. These procedures may thus prove useful in the
preoperative diagnosis of bleeding Meckel’s diverticulum.
Case Report
A 22-year-old man presented to the emergency room with
a 2-day history of massive melena. At 15, 19 and 21 years
old, he had experienced similar episodes of bloody diarrhea
that resolved immediately. Upper gastrointestinal endoscopy
demonstrated no bleeding, while colonoscopy revealed blood
clots but no source of bleeding was seen with the episode of
bloody diarrhea at 21 years old. His family history was non-
contributory. On admission, physical examination did not re-
veal pallor or severe hypotension, and he was anicteric with
normoactive bowel sounds and a soft, flat abdomen without
evidence of tenderness or masses. Hematological analysis on
admission showed a red blood cell count of 320×104/μl, a
hemoglobin level of 8.6 g/dl and a hematocrit level of
25.9%. Platelet count, coagulation studies, and liver and re-
nal function tests were all normal. Emergent upper gastroin-
testinal endoscopy and colonoscopy were performed, reveal-
ing blood clots in the colon. Colonoscopy likewise revealed
that the bleeding was proximal, but did not identify a
source. Abdominal contrast-enhanced computed tomography
(CT) and angiography also failed to detect the source of
bleeding. The patient continued to have massive melena, re-
quiring transfusion of 8 units of packed red blood cells for
correction of anemia. Further investigation with CE on hos-
pital day 4 showed oozing hemorrhage in the ileum (Fig. 1).
CE was able to detect small bowel bleeding with a rough re-
gion of origin. A secondary procedure was therefore consid-
ered necessary according to CE findings. DBE was per-
formed on hospital day 5, revealing a large diverticulum in
the distal part of the ileum (Fig. 2A, arrows). The oozing
hemorrhage was already stopped, and no ulcers were appar-
ent in the diverticulum. On urografin-contrast radiography of
the small intestine from the endoscopy, the ileal diverticu-
lum was evident (Fig. 2B, arrowheads). Tc-99m pertechne-
tate was helpful in determining the existence of Meckel’s di-
verticulum because of its reactivity with the gastric mucosa.
On hospital day 8, a Tc-99m pertechnetate Meckel’s scan
showed an abnormal focus of uptake in the right lower ab-
domen (Fig. 3).
The patient was taken to the operating room with a pre-
sumptive diagnosis of bleeding Meckel’s diverticulum. Lap-
arotomy confirmed the findings of the DBE and Meckel’s
scan, showing a 5-cm long, 2-cm wide Meckel’s diverticu-
lum located approximately 90 cm proximal to the ileocecal
valve (Fig. 4A). Resection of a short segment of the small
bowel, including the diverticulum, with primary anastomosis
was performed (Fig. 4B). The patient experienced no further
hemorrhage and no postoperative complications, and was
discharged 1 week postoperatively with complete resolution
of symptoms. The pathological specimen revealed an area of
ectopic gastric mucosa within the diverticulum (Fig. 4C).
Discussion
Meckel’s diverticulum is difficult to detect nonsurgically.
We preoperatively detected the Meckel’s diverticulum in this
case using DBE. When bleeding is massive and cannot be
controlled using conservative methods, this represents an
emergency situation that needs to be promptly resolved us-
ing surgical resection of Meckel’s diverticulum after initial
resuscitation of the patient with blood transfusion. Making a
precise diagnosis as soon as possible is thus important. In
the present case, even though the patient continued to expe-
rience massive melena, CE was performed on hospital day
4. In retrospect, we should have performed CE and DBE
earlier to determine the exact cause of the bleeding.
The new methods of CE and DBE have revolutionized the
diagnostic approach to small intestinal bleeding in recent
years. CE is a noninvasive technique that allows visualiza-
tion of the entire alimentary tract (9). In the present case,
CE was able to detect the source of bleeding in the ileum,
but did not allow precise diagnosis. It is notable that DBE
enabled preoperative diagnosis in this case. DBE can visual-
ize the entire small intestine, allows detailed examination of
specific areas of interest, and is quicker and less painful

Intern Med 51: 1023-1026, 2012 DOI: 10.2169/internalmedicine.51.6594
1025
Figure 2. Views from double-balloon endoscopy. (A) Endoscopy shows a large diverticulum (ar-rows) in the distal part of the ileum. (B) Urografin-contrast radiography of the small intestine from the endoscopy shows the diverticulum, approximately 5 cm in size, in the ileum (arrowheads).
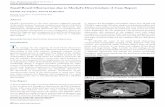
Figure 3. Image of the anterior lower abdomen after intra-venous administration of Tc-99m pertechnetate (Meckel’s scan). The diverticulum is clearly visible (arrow).
than previous endoscopic techniques (15). These results in-
dicate that CE and DBE can play complementary roles in
the preoperative diagnosis of bleeding Meckel’s diverticu-
lum. Overall detection rates of abnormalities in the small
bowel of CE (65%) and DBE (53%) are not significantly
different, nor are overall diagnostic yields of CE (50%) and
DBE (53%) (16). Since positive results on Tc-99m pertech-
netate scintigraphy do not always indicate that Meckel’s di-
verticulum is responsible for the bleeding, if the source of
small intestinal bleeding cannot be determined, subsequent
DBE examination should increase the detection rate of
Meckel’s diverticulum.
The diverticulum in the present patient contained ectopic
gastric mucosa without ulcers or visible vessels. Shinozaki
et al. investigated five cases of Meckel’s diverticulum and
concluded that endoscopic observation of ulcers in Meckel’s
diverticulum provides important evidence of bleeding (17).
However, if no adherent blood clots or vessels are visible in
ulcers within the Meckel’s diverticulum, confirming the ul-
cer as a bleeding source is difficult. The mechanisms of
hemorrhage from Meckel’s diverticulum remain unclear; this
report indicates that Meckel’s diverticulum without ulcera-
tion can cause bleeding. We conclude that DBE enables pre-
cise preoperative diagnosis and reasonable treatment of
bleeding Meckel’s diverticulum.
The authors state that they have no Conflict of Interest (COI).

Intern Med 51: 1023-1026, 2012 DOI: 10.2169/internalmedicine.51.6594
1026
Figure 4. Extraction of Meckel’s diverticulum. (A) A Meckel’s diverticulum measuring 5 cm in length was found approximately 70 cm proximal to the ileocecal junction at laparoscopy. (B) Resec-tion of the intestine containing the diverticulum. Arrows, the Meckel’s diverticulum. (C) Microscop-ic section of the pathological specimen. Arrows, ectopic gastric glands. The glands to the right repre-sent normal intestinal glands.
References
1. Park JJ, Wolff BG, Tollefson MK, Walsh EE, Larson DR. Meckel
diverticulum: the Mayo Clinic experience with 1476 patients
(1950-2002). Ann Surg 241: 529-533, 2005.
2. Sagar J, Kumar V, Shah DK. Meckel’s diverticulum: a systematic
review. J R Soc Med 99: 501-505, 2006.
3. Weinstein EC, Cain JC, Remine WH. Meckel’s diverticulum: 55
years of clinical and surgical experience. JAMA 182: 251-253,
1962.
4. Evers BM. Small intestine. In: Sabiston Textbook of Surgery. 17th
ed. Townsend CM, Ed. Elsevier, 2004: 1366-1368.
5. Whang EE, Ashley SW, Zinner MJ. Small intestine. In:
Schwartz’s Principles of Surgery. 8th ed. Brunicardi FC, Ed.
McGraw-Hill, 2005: 1043-1044.
6. Yamaguchi M, Takeuchi S, Awazu S. Meckel’s diverticulum: in-
vestigation of 600 patients in Japanese literature. Am J Surg 136:
247-249, 1978.
7. Soltero MJ, Bill AH. The natural history of Meckel’s diverticulum
and its relation to incidental removal. Am J Surg 32: 168-173,
1976.
8. Mortensen NJ, Jones O. The small and large intestines. In: Bailey
& Love’s Short Practice of Surgery. 24th ed. 2004: 1159-1160.
9. Iddan G, Meron G, Glukhovsky A, Swain P. Wireless capsule en-
doscopy. Nature 405: 417, 2000.
10. Yamamoto H, Kita H, Sunada K, et al. Clinical outcomes of
double-balloon endoscopy for the diagnosis and treatment of
small-intestinal diseases. Clin Gastroenterol Hepatol 2: 1010-1016,
2004.
11. Pozzato P, Brancaccio M, Sacco S, Virzì S, Ventrucci M. Capsule
endoscopy for the detection of bleeding Meckel’s diverticulum.
Minerva Gastroenterol Dietol 52: 327-331, 2006.
12. Yamamoto H, Sekine Y, Sato Y, et al. Total enteroscopy with a
nonsurgical steerable double-balloon method. Gastrointest Endosc
53: 216-220, 2001.
13. Swaniker F, Soldes O, Hirschl RB. The utility of technetium 99m
pertechnetate scintigraphy in the evaluation of patients with
Meckel’s diverticulum. J Pediatr Surg 34: 760-764, 1999.
14. Kopácová M, Vykouril L, Vacek Z, et al. Inverted Meckel’s diver-
ticulum with ectopic pancreatic tissue as a source of severe gastro-
intestinal bleeding. J Gastrointest Surg 14: 578-581, 2010.
15. Yamamoto H, Sugano K. A new method of enteroscopy--the
double-balloon method. Can J Gastroenterol 17: 273-274, 2003.
16. Ohmiya N, Yano T, Yamamoto H, et al. Diagnosis and treatment
of obscure GI bleeding at double balloon endoscopy. Gastrointest
Endosc 66: S72-S77, 2007.
17. Shinozaki S, Yamamoto H, Ohnishi H, et al. Endoscopic observa-
tion of Meckel’s diverticulum by double balloon endoscopy: re-
port of five cases. J Gastroenterol Hepatol 23: e308-e311, 2008.
Ⓒ 2012 The Japanese Society of Internal Medicine
http://www.naika.or.jp/imindex.html









![Diagnosis of Bleeding Meckel's Diverticulum in Adults · 2020. 7. 27. · [1, 2]. Technetium-99m pertechnetate scintigraphy, commonly known as Meckel’s scan, is considered as the](https://static.fdocuments.net/doc/165x107/61279e6912637b477c1e638d/diagnosis-of-bleeding-meckels-diverticulum-in-adults-2020-7-27-1-2-technetium-99m.jpg)








