Leprosy - Diseases pdf/Lep… · Leprosy or Hansen's disease (HD) is a chronic disease caused by...
Transcript of Leprosy - Diseases pdf/Lep… · Leprosy or Hansen's disease (HD) is a chronic disease caused by...

HEALTH CENTER INTERNATIONAL RESEARCH
http://healthcenterinternationalresearches.webs.com/
Dr. Maddalena Frau
Leprosy

Leprosy or Hansen's disease (HD) is a chronic disease caused by the bacteria Mycobacterium
leprae and Mycobacterium lepromatosis. Named after physician Gerhard Armauer Hansen,
leprosy is primarily a granulomatous disease of the peripheral nerves and mucosa of the upper
respiratory tract; skin lesions are the primary external sign. Left untreated, leprosy can be
progressive, causing permanent damage to the skin, nerves, limbs and eyes. Contrary to folklore,
leprosy does not cause body parts to fall off, although they can become numb or diseased as a
result of secondary infections; these occur as a result of the body's defenses being compromised
by the primary disease. Secondary infections, in turn, can result in tissue loss causing fingers and
toes to become shortened and deformed, as cartilage is absorbed into the body.
Although the mode of transmission of Hansen's disease remains uncertain, most investigators
think that M. leprae is usually spread from person to person in respiratory droplets. Studies have
shown that leprosy can be transmitted to humans by armadillos. Leprosy is now known to be
neither sexually transmitted nor highly infectious after treatment. Approximately 95% of people
are naturally immune and sufferers are no longer infectious after as little as 2 weeks of treatment.
The minimum incubation period reported is as short as a few weeks, based on the very
occasional occurrence of leprosy among young infants. The maximum incubation period
reported is as long as 30 years, or over, as observed among war veterans known to have been
exposed for short periods in endemic areas but otherwise living in non-endemic areas. It is
generally agreed that the average incubation period is between three and five years.
Leprosy has affected humanity for over 4,000 years, and was well-recognized in the civilizations
of ancient China, Egypt, and India. In 1995, the World Health Organization (WHO) estimated
that between 2 and 3 million people were permanently disabled because of leprosy at that time.
In the past 20 years, 15 million people worldwide have been cured of leprosy. Although the
forced quarantine or segregation of patients is unnecessary in places where adequate treatments
are available, many leper colonies still remain around the world in countries such as India (where
there are still more than 1,000 leper colonies), China, Romania, Egypt, Nepal, Somalia, Liberia,
Vietnam, and Japan. Leprosy was once believed to be highly contagious and was treated with
mercury — all of which applied to syphilis, which was first described in 1530. It is now thought
that many early cases of leprosy could have been syphilis.
The age-old social stigma associated with the advanced form of leprosy lingers in many areas,
and remains a major obstacle to self-reporting and early treatment. Effective treatment for
leprosy appeared in the late 1930s with the introduction of dapsone and its derivatives. Leprosy
bacilli resistant to dapsone soon evolved and, due to overuse of dapsone, became widespread. It
was not until the introduction of multidrug therapy (MDT) in the early 1980s that the disease
could be diagnosed and treated successfully within the community.
MDT for multibacillary leprosy consists of rifampicin, dapsone, and clofazimine taken over 12
months. Dosages adjusted appropriately for children and adults are available in all primary health
centres in the form of blister packages. Single dose MDT for single lesion leprosy consists of
rifampicin, ofloxacin, and minocycline. The move toward single-dose treatment strategies has
reduced the prevalence of disease in some regions, since prevalence is dependent on duration of
treatment.

World Leprosy Day was created to draw awareness to leprosy and its sufferers.
There are several different approaches for classifying leprosy; however, parallels exist.
The World Health Organization system distinguishes "paucibacillary" and
"multibacillary" based upon the proliferation of bacteria ("pauci-" refers to a low
quantity.)
The SHAY scale provides five gradations.
The ICD-10, though developed by the WHO, uses Ridley-Jopling and not the WHO
system. It also adds an indeterminate ("I") entry.
In MeSH, three groupings are used.
WHO Ridley-
Jopling
ICD-
10 MeSH Description
Lepromin
test
Immune
target
Paucibacillary
tuberculoid
("TT"),
borderline
tuberculoid
("BT")
A30.1,
A30.2 Tuberculoid
It is characterized by
one or more
hypopigmented skin
macules and
anaesthetic patches,
where skin sensations
are lost because of
damaged peripheral
nerves that have been
attacked by the human
host's immune cells.
Positive bacillus
(Th1)
Multibacillary
midborderline
or borderline
("BB")
A30.3 Borderline
Borderline leprosy is
of intermediate
severity and is the most
common form. Skin
lesions resemble
tuberculoid leprosy but
are more numerous and
irregular; large patches
may affect a whole
limb, and peripheral
nerve involvement
with weakness and loss
of sensation is
common. This type is
unstable and may
become more like
lepromatous leprosy or
may undergo a reversal
reaction, becoming
more like the
tuberculoid form.

Multibacillary
borderline
lepromatous
("BL"), and
lepromatous
("LL")
A30.4,
A30.5 Lepromatous
It is associated with
symmetric skin lesions,
nodules, plaques,
thickened dermis, and
frequent involvement
of the nasal mucosa
resulting in nasal
congestion and
epistaxis (nose bleeds),
but, typically,
detectable nerve
damage is late.
Negative
plasmid
inside
bacillus
(Th2)
There is a difference in immune response to the tuberculoid and lepromatous forms.
Hansen's disease may also be divided into the following types::344-346
Early and indeterminate leprosy
Tuberculoid leprosy
Borderline tuberculoid leprosy
Borderline leprosy
Borderline lepromatous leprosy
Lepromatous leprosy
Histoid leprosy
Diffuse leprosy of Lucio and Latapí
This disease may also occur with only neural involvement, without skin lesions. This disease is
also known as Hansen's Disease.
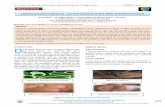
Skin lesions are the primary external sign. Left untreated, leprosy can be progressive, causing
permanent damage to the skin, nerves, limbs, and eyes.
Diagnosis in the U.S. is often delayed because healthcare providers are unaware of leprosy and
its symptoms. Early diagnosis and treatment prevents nerve involvement, the hallmark of
leprosy, and the disability it causes.
There are many kinds of leprosy but there are common symptoms. These include runny nose, dry
scalp, eye problems, skin lesions, and muscle weakness.

Mycobacterium leprae
Mycobacterium leprae, one of the causative agents of leprosy. As acid-fast bacteria, M. leprae
appear red when a Ziehl-Neelsen stain is used.
Main article: Mycobacterium leprae
At highest risk are those living in endemic areas with poor conditions such as inadequate
bedding, contaminated water, and insufficient diet, or other diseases that compromise immune
function. However, though hard evidence is limited, and fringe publications have made
passionate claims to the contrary, professional studies show little evidence that HIV is an
important factor in increasing the risk of leprosy infection. It is presumed that this might be
because of differences between the modes of immunity involved. However, it is plain that the
two infections and their signs and progressions need not be fully independent, so the matter
should be regarded with reserve. For example, a Medscape clinical presentation reports that HIV
infection neither is a risk factor for acquisition nor for increased virulence of leprosy, but that
latent cases of leprosy may emerge after starting HAART. Lewis, F. S. et al. ; Dermatologic
Manifestations of Leprosy Clinical Presentation
Recent research suggests that there is a defect in cell-mediated immunity that causes
susceptibility to Hansen's disease. Less than ten percent of the world's population is capable of
acquiring the disease. The region of DNA responsible for this variability is also involved in
Parkinson disease, giving rise to current speculation that the two disorders may be linked in some
way at the biochemical level. In early 2003, an international team of scientists conducted a
genome scan in Vietnamese multiplex leprosy families and found that susceptibility to leprosy
was significantly linked to region q25 on the long arm of chromosome 6. Further confirmation of
the chromosome 6 locus was provided by high-resolution linkage mapping in simplex leprosy
families. Now, in a continuation of these findings, the team has pinpointed the chromosome 6
susceptibility locus to the 5' regulatory promoter region shared by both the Parkinson's disease
gene PARK2 and its co-regulated gene PACRG. According to The Leprosy Mission Canada,
most people-–about 95% of the population-–are naturally immune to the disease.
The mechanism of transmission of leprosy is prolonged close contact and transmission by nasal
droplet. In addition to humans, leprosy has been observed in nine-banded armadillo, (which, it
has recently been confirmed, are among the primary sources of new cases of leprosy in
Americans), and three species of primates. The bacterium can also be grown in the laboratory by
injection into the footpads of mice. There is evidence that not all people who are infected with
M. leprae develop leprosy, and genetic factors have long been thought to play a role, due to the

observation of clustering of leprosy around certain families, and the failure to understand why
certain individuals develop lepromatous leprosy while others develop other types of leprosy. It is
estimated that due to genetic factors, only 5% of the population is susceptible to leprosy. This is
mostly because the body is naturally immune to the bacteria, and those persons that do become
infected experience severe allergic reactions to the disease. However, the role of genetic factors
is not entirely clear in determining this clinical expression. In addition, malnutrition and
prolonged exposure to infected persons may play a role in development of the overt disease.
The most widely held belief is that the disease is transmitted by contact between infected persons
and healthy persons. In general, closeness of contact is related to the dose of infection, which in
turn is related to the occurrence of disease. Of the various situations that promote close contact,
contact within the household is the only one that is easily identified, although the incidence
among contacts and the relative risk for them appear to vary considerably in different studies. In
incidence studies, infection rates for contacts of lepromatous leprosy have varied from 6.2 per
1000 per year in Cebu, Philippines to 53 per 1000 per year in part of Western India to 55.8 per
1000 per year in a part of Southern India.[
Two exit routes of M. leprae from the human body often described are the skin and the nasal
mucosa, although their relative importance is not clear. Lepromatous cases show large numbers
of organisms deep in the dermis, but whether they reach the skin surface in sufficient numbers is
doubtful. Although there are reports of acid-fast bacilli being found in the desquamating
epithelium (sloughing of superficial layer of skin) of the skin, Weddell et al. had reported in
1963 that they could not find any acid-fast bacilli in the epidermis, even after examining a very
large number of specimens from patients and contacts. In a recent study, Job et al. found fairly
large numbers of M. leprae in the superficial keratin layer of the skin of lepromatous leprosy
patients, suggesting that the organism could exit along with the sebaceous secretions.
The importance of the nasal mucosa was recognized as early as 1898 by Schäffer, in particular
that of the ulcerated mucosa. The quantity of bacilli from nasal mucosal lesions in lepromatous
leprosy was demonstrated by Shepard as large, with counts ranging from 10,000 to 10,000,000.
Pedley reported that the majority of lepromatous patients showed leprosy bacilli in their nasal
secretions as collected through blowing the nose. Davey and Rees indicated that nasal secretions
from lepromatous patients could yield as much as 10 million viable organisms per day.
The entry route of M. leprae into the human body is also not definitively known: The skin and
the upper respiratory tract are most likely. While older research dealt with the skin route, recent
research has increasingly favored the respiratory route. Rees and McDougall succeeded in the
experimental transmission of leprosy through aerosols containing M. leprae in immune-
suppressed mice, suggesting a similar possibility in humans. Successful results have also been
reported on experiments with nude mice when M. leprae were introduced into the nasal cavity by
topical application. In summary, entry through the respiratory route appears the most probable
route, although other routes, particularly broken skin, cannot be ruled out. The CDC notes the
following assertion about the transmission of the disease: "Although the mode of transmission of
Hansen's disease remains uncertain, most investigators think that M. leprae is usually spread
from person to person in respiratory droplets."

In leprosy, both the reference points for measuring the incubation period and the times of
infection and onset of disease are difficult to define, the former because of the lack of adequate
immunological tools and the latter because of the disease's slow onset. Even so, several
investigators have attempted to measure the incubation period for leprosy. The minimum
incubation period reported is as short as a few weeks and this is based on the very occasional
occurrence of leprosy among young infants. The maximum incubation period reported is as long
as 30 years, or over, as observed among war veterans known to have been exposed for short
periods in endemic areas but otherwise living in non-endemic areas. It is generally agreed that
the average incubation period is between three and five years.
Prevention
Because leprosy can be cured with medicines, an early diagnosis will often reduce leprosy
symptoms and complications. Therefore, while prevention of leprosy is not always possible,
especially where leprosy is endemic, control should be possible.
An early diagnosis of help reducing the severeness and complications caused by the disease as
leprosy can be cured with medicines. Although the prevention is often difficult especially in the
places where it is endemic, control can be possible. People in immediate contact with leprosy
patients should examine themselves for the infection. Annual examinations for at least five years
should be conducted for such people following their very last contact with the leprosy patient.
In a recent trial, a single dose of rifampicin reduced the rate at which contacts acquired leprosy in
the two years after contact by 57%; 265 treatments with rifampicin prevented one case of leprosy
in this period. A non-randomized study found that rifampicin reduced the number of new cases
of leprosy by 75% after three years.
BCG offers a variable amount of protection against leprosy as well as against tuberculosis.
Efforts to overcome persistent obstacles to the elimination of the disease include improving
detection, educating patients and the population about its cause, and fighting social taboos about
a disease that has caused its patients throughout history to be considered "unclean" or "cursed by
God" as outcasts. Leprosy is not a hereditary disease. Where taboos are strong, patients may be
forced to hide their condition (and avoid seeking treatment) to avoid discrimination. The lack of

awareness about Hansen's disease can lead people to believe (falsely) that the disease is highly
contagious and incurable.
The ALERT hospital and research facility in Ethiopia provides training to medical personnel
from around the world in the treatment of leprosy, as well as treating many local patients.
Surgical techniques, such as for the restoration of control of movement of thumbs, have been
developed.
In 1988, Jacinto Convit was nominated for the Nobel Prize in Medicine, for developing a vaccine
to fight leprosy, by combining a tuberculosis (TB) vaccines with Mycobacterium Leprae.
MDT anti-leprosy drugs: standard regimens
Enough synthetic pharmaceuticals that are effective against leprosy have by now been identified,
and support a flexible choice of treatments. The WHO Study Group's report on the
Chemotherapy of Leprosy in 1993 recommended two types of standard MDT regimen be
adopted. The first was a 24-month treatment for multibacillary (MB or lepromatous) cases using
rifampicin, clofazimine, and dapsone. The second was a six-month treatment for paucibacillary
(PB or tuberculoid) cases, using rifampicin and dapsone. At the First International Conference on
the Elimination of Leprosy as a Public Health Problem, held in Hanoi the next year, the global
strategy was endorsed and funds provided to WHO for the procurement and supply of MDT to
all endemic countries.
The disease was known in Ancient Greece as elephantiasis (elephantiasis graecorum). At various
times blood was considered to be a treatment either as a beverage or as a bath. That of virgins or
children was considered to be especially potent. This practice seems to have originated with the
Ancient Egyptians but was also known in China. This practice persisted until at least 1790, when
the use of dog blood was mentioned in De Secretis Naturae. Paracelsus recommended the use of
lamb's blood and even blood from dead bodies was used.
Snakes were also used, according to Pliny, Aretaeus of Cappadocia, and Theodorus. Gaucher
recommended treatment with cobra venom. Boinet, in 1913, tried increasing doses of bee stings
(up to 4000). Scorpions and frogs were used occasionally instead of snakes. The excreta of
Anabas (the climbing fish) was also tried.

Alternative treatments included scarification with or without the addition of irritants including
arsenic and hellebore. Castration was also practiced in the Middle Ages.
A common pre-modern treatment of leprosy was chaulmoogra oil.
The oil has long been used in India as an Ayurvedic medicine for the treatment of leprosy and
various skin conditions. It has also been used in China and Burma, and was introduced to the
West by Frederic John Mouat, a professor at Bengal Medical College. He tried the oil as an oral
and topical agent in two cases of leprosy and reported significant improvements in an 1854
paper.
This paper caused some confusion. Mouat indicated that the oil was the product of a tree
Chaulmoogra odorata, which had been described in 1815 by William Roxburgh, a surgeon and
naturalist, while he was cataloging the plants in the East India Company’s botanical garden in
Calcutta. This tree is also known as Gynocardia odorata. For the rest of the 19th century, this
tree was thought to be the source of the oil. In 1901, Sir David Prain identified the true
chaulmoogra seeds of the Calcutta bazaar and of the Paris and London apothecaries as coming
from Taraktogenos kurzii, which is found in Burma and Northeast India. The oil mentioned in
the Ayurvedic texts was from the tree Hydnocarpus wightiana, known as Tuvakara in Sanskrit
and chaulmugra in Hindi and Persian.
The first parenteral administration was given by the Egyptian doctor Tortoulis Bey, personal
physician to the Sultan Hussein Kamel of Egypt. He had been using subcutaneous injections of
creosote for tuberculosis and in 1894 administered subcutaneous injection of chaulmoogra oil in
a 36-year-old Egyptian Copt who had been unable to tolerate oral treatment. After 6 years and
584 injections, the patient was declared cured.
An early scientific analysis of the oil was carried out by Frederick B. Power in London in 1904.
He and his colleagues isolated a new unsaturated fatty acid from the seeds, which they named
'chaulmoogric acid'. They also investigated two closely related species: Hydnocarpus
anthelmintica and Hydnocarpus wightiana. From these two trees they isolated both
chaulmoogric acid and a closely related compound, 'hydnocarpus acid'. They also investigated
Gynocardia odorata and found that it produced neither of these acids. Later investigation
showed that 'taraktogenos' (Hydnocarpus kurzii) also produced chaulmoogric acid.
Another difficulty with the use of this oil was administration. Taken orally it is extremely
nauseating. Given by enema may cause peri-anal ulcers and fissures. Given by injection the drug
caused fever and other local reactions. Despite these difficulties, a series of 170 patients were
reported in 1916 by Ralph Hopkins, the attending physician at the Louisiana Leper Home in
Carville, Louisiana. He divided the patients into two groups - 'incipient' and 'advanced'. In the
advanced cases, 25% (at most) showed any improvement or arrest of their condition; in the
incipient cases, 45% reported an improvement or stabilization of the disease (mortality rates
were 4% and 8%, respectively). The remainder absconded from the Home apparently in
improved condition.

Given the apparent usefulness of this agent, a search began for improved formulations. Victor
Heiser the Chief Quarantine Officer and Director of Health for Manila and Elidoro Mercado the
house physician at the San Lazaro Hospital for lepers in Manila decided to add camphor to a
prescription of chaulmoogra and resorcin, which was typically given orally at the suggestion of
Merck and Company in Germany to whom Heiser had written. They found that this new
compound was readily absorbed without the nausea that had plagued the earlier preparations.
Heiser and Mercado in 1913 then administered the oil by injection to two patients who were
cured of the disease. Since this treatment was administered in conjunction with other materials,
the results were not clear. A further two patients were treated with the oil by injection without
other treatments and again appeared to be cured of the disease. The following year, Heiser
reported a further 12 patients but the results were mixed.
Less toxic injectable forms of this oil were then sought. Between 1920 and 1922, a series of
papers were published describing the esters of these oils. These may have been based on the
work of Alice Ball - the record is not clear on this point and Ms Ball died in 1916. Trials of these
esters were carried out in 1921 and appeared to give useful results.
These attempts had been preceded by others. Merck of Darmstadt had produced a version of the
sodium salts in 1891. They named this sodium gynocardate in the mistaken belief that the origin
of the oil was Gynocardia odorata. Bayer in 1908 marketed a commercial version of the esters
under the name 'Antileprol'.
To ensure a supply of this agent Joseph Rock, Professor of Systematic Botany at the College of
Hawaii, traveled to Burma. The local villagers located a grove of trees in seed, which he used to
establish a plantation in 2,980 trees on the island of Oahu, Hawaii between 1921 and 1922.
The oil remained a popular treatment despite the common side effects until the introduction of
sulfones in the 1940s. Debate about its efficacy continued until it was discontinued.
Modern drug treatment
MDT patient packs and blisters

Epidemiology
Worldwide, two to three million people are estimated to be permanently disabled because of
leprosy. India has the greatest number of cases, with Brazil second and Myanmar third.
In 1999, the world incidence of Hansen's disease was estimated to be 640,000. In 2000, 738,284
cases were identified. In 2000, the World Health Organization (WHO) listed 91 countries in
which Hansen's disease is endemic. India, Burma, and Nepal contained 70% of cases. India
reports over 50% of the world's leprosy cases. In 2002, 763,917 new cases were detected
worldwide, and in that year the WHO listed Brazil, Madagascar, Mozambique, Tanzania, and
Nepal as having 90% of Hansen's disease cases.
Although annual incidence — the number of new leprosy cases occurring each year — is
important as a measure of transmission, it is difficult to measure in leprosy due to its long
incubation period, delays in diagnosis after onset of the disease, and the lack of laboratory tools
to detect leprosy in its very early stages. Instead, the registered prevalence is used. Registered
prevalence is a useful proxy indicator of the disease burden, as it reflects the number of active
leprosy cases diagnosed with the disease and receiving treatment with MDT at a given point in
time. The prevalence rate is defined as the number of cases registered for MDT treatment among
the population in which the cases have occurred, again at a given point in time.
New case detection is another indicator of the disease that is usually reported by countries on an
annual basis. It includes cases diagnosed with onset of disease in the year in question (true
incidence) and a large proportion of cases with onset in previous years (termed a backlog
prevalence of undetected cases).
Endemic countries also report the number of new cases with established disabilities at the time of
detection, as an indicator of the backlog prevalence. Determination of the time of onset of the
disease is, in general, unreliable, is very labor-intensive, and is seldom done in recording these
statistics.

G. H. A. Hansen, discoverer of M. leprae
DNA taken from the shrouded remains of a man discovered in a tomb next to the Old City of
Jerusalem shows him to be the earliest human proven to have suffered from leprosy. The remains
were dated by radiocarbon methods to 1-50 C.E.
After the end of the 17th century, Norway, Iceland and England were the countries in Western
Europe where leprosy was a significant problem. During the 1830s, the number of lepers in
Norway, Iceland and England rose rapidly, believed to be caused by frequent visits of sailors
who visited Western India, causing an increase in medical research into the condition, and the
disease became a political issue. Norway appointed a medical superintendent for leprosy in 1854
and established a national register for lepers in 1856, the first national patient register in the
world. Mycobacterium leprae, the causative agent of leprosy, was discovered by G. H. Armauer
Hansen in Norway in 1873, making it the first bacterium to be identified as causing disease in
humans. The principal opposition to Hansen's view that leprosy was an infectious disease came
from his father-in-law, Daniel Cornelius Danielssen who considered it a hereditary disease and
had stated this in his book, ‘’Traité de la Spedalskhed ou Elephantiasis des Grecs’’ - the standard
reference book on leprosy from 1848 until the death of Danielssen in 1895.
Hansen observed a number of nonrefractile small rods in unstained tissue sections. The rods
were not soluble in potassium lye, and they were acid- and alcohol-fast. In 1879, he was able to
stain these organisms with Ziehl's method and the similarities with Koch's bacillus
(Mycobacterium tuberculosis) were noted. There were three significant differences between
these organisms: (1) the rods in the leprosy lesions were extremely numerous, (2) they formed
characteristic intracellular collections (globii), and (3) the rods had a variety of shapes with
branching and swelling. These differences suggested that leprosy was caused by an organism
related to but distinct from Mycobacterium tuberculosis.
He worked at St. Jørgens Hospital in Bergen, founded early in the fifteenth century. St. Jørgens
is today a museum, Lepramuseet, it can be argued the best-preserved leprosy hospital in
Northern Europe.

References
1. ^ Sasaki S, Takeshita F, Okuda K, Ishii N (2001). "Mycobacterium leprae and leprosy: a
compendium". Microbiol Immunol 45 (11): 729–36. PMID 11791665.
2. ^ a b c "New Leprosy Bacterium: Scientists Use Genetic Fingerprint To Nail 'Killing
Organism'". ScienceDaily. 2008-11-28. Retrieved 2010-01-31.
3. ^ a b c Kenneth J. Ryan, C. George Ray, editors. (2004). Ryan KJ, Ray CG. ed. Sherris
Medical Microbiology (4th ed.). McGraw Hill. pp. 451–3. ISBN 0838585299.
OCLC 61405904 52358530 61405904.
4. ^ a b "Lifting the stigma of leprosy: a new vaccine offers hope against an ancient disease".
Time 119 (19): 87. May 1982. PMID 10255067.
5. ^ a b Kulkarni GS (2008). Textbook of Orthopedics and Trauma (2 ed.). Jaypee Brothers
Publishers. p. 779. ISBN 8184482426, 9788184482423.
6. ^ "Q and A about leprosy". American Leprosy Missions. Retrieved 2011-01-22. "Do
fingers and toes fall off when someone gets leprosy? No. The bacillus attacks nerve
endings and destroys the body's ability to feel pain and injury. Without feeling pain,
people injure themselves on fire, thorns, rocks, even hot coffee cups. Injuries become
infected and result in tissue loss. Fingers and toes become shortened and deformed as the
cartilage is absorbed into the body."
7. ^ City of Houston Government Center, Health and Human Services. (n.d.). Hansen's
disease (leprosy) Retrieved from
http://www.houstontx.gov/health/ComDisease/hansens.html
8. ^ "Probable Zoonotic Leprosy in the Southern United States". The New England Journal
of Medicine. Retrieved April 28, 2011.
9. ^ "Armadillos linked to leprosy in humans". CNN. 2011-04-28.
10. ^ Truman, Richard W.; Singh, Pushpendra; Sharma, Rahul; Busso, Philippe; Rougemont,
Jacques; Paniz-Mondolfi, Alberto; Kapopoulou, Adamandia; Brisse, Sylvain et al (April
2011). "Probable Zoonotic Leprosy in the Southern United States". The New England
Journal of Medicine (Massachusetts Medical Society) 364 (17): 1626–1633.
doi:10.1056/NEJMoa1010536. PMC 3138484. PMID 21524213. Retrieved 3 May 2011.
11. ^ "About leprosy: frequently asked questions". American Leprosy Missions, Inc.
Retrieved October 28, 2011.
12. ^ Holden (2009). "Skeleton Pushes Back Leprosy's Origins". ScienceNOW. Retrieved
2010-01-31.
13. ^ a b c d e f "Leprosy". WHO. 2009-08-01. Retrieved 2010-01-31.
14. ^ a b WHO (1995). "Leprosy disabilities: magnitude of the problem". Weekly
Epidemiological Record 70 (38): 269–75. PMID 7577430.
15. ^ a b Walsh F (2007-03-31). "The hidden suffering of India's lepers". BBC News.
16. ^ Lyn TE (2006-09-13). "Ignorance breeds leper colonies in China". Independat News &
Media. Retrieved 2010-01-31.
17. ^ Radan S, Hutt A (2001-11-06). "Europe's last leper colony lives on". BBC News.
Retrieved 2010-01-31.
18. ^ ""Making Peace With Vietnam" to be screened at Beijing film festival". Radio the
Voice of Vietnam. 2009-02-08. Retrieved 2010-01-31.

19. ^ Japan repealed its "Leprosy Prevention Laws" in 1996 but former patients still reside in
sanatoriums. "Koizumi apologises for leper colonies". BBC News. May 25, 2001. and
Ex-Hansen's disease patients still struggling with prejudice Japan Times June 7, 2007.
20. ^ Syphilis through history Encyclopædia Britannica
21. ^ Jopling WH (March 1991). "Leprosy stigma". Lepr Rev 62 (1): 1–12. PMID 2034017.
22. ^ a b "Communicable Diseases Department, Leprosy FAQ". World Health Organization.
2006-05-25. Retrieved 2010-01-31.
23. ^ Smith DS (2008-08-19). "Leprosy: Overview". eMedicine Infectious Diseases.
Retrieved 2010-02-01.
24. ^ Singh N, Manucha V, Bhattacharya SN, Arora VK, Bhatia A (June 2004). "Pitfalls in
the cytological classification of borderline leprosy in the Ridley-Jopling scale". Diagn.
Cytopathol. 30 (6): 386–8. doi:10.1002/dc.20012. PMID 15176024.
25. ^ Ridley DS, Jopling WH (1966). "Classification of leprosy according to immunity. A
five-group system". Int. J. Lepr. Other Mycobact. Dis. 34 (3): 255–73. PMID 5950347.
26. ^ a b c "What Is Leprosy?" THE MEDICAL NEWS | from News-Medical.Net - Latest
Medical News and Research from Around the World. Web. 20 Nov. 2010.
<http://www.news-medical.net/health/What-is-Leprosy.aspx>.
27. ^ Modlin RL (June 1994). "Th1-Th2 paradigm: insights from leprosy". J. Invest.
Dermatol. 102 (6): 828–32. doi:10.1111/1523-1747.ep12381958. PMID 8006444.
28. ^ James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin:
clinical Dermatology. Saunders Elsevier. ISBN 0-7216-2921-0.
29. ^ Jardim MR, Antunes SL, Santos AR, et al. (July 2003). "Criteria for diagnosis of pure
neural leprosy". J. Neurol. 250 (7): 806–9. doi:10.1007/s00415-003-1081-5.
PMID 12883921.
30. ^ Mendiratta V, Khan A, Jain A (2006). "Primary neuritic leprosy: a reappraisal at a
tertiary care hospital". Indian J Lepr 78 (3): 261–7. PMID 17120509.
31. ^ Ishida Y, Pecorini L, Guglielmelli E (July 2000). "Three cases of pure neuritic (PN)
leprosy at detection in which skin lesions became visible during their course". Nihon
Hansenbyo Gakkai Zasshi 69 (2): 101–6. doi:10.5025/hansen.69.101. PMID 10979277.
32. ^ Mishra B, Mukherjee A, Girdhar A, Husain S, Malaviya GN, Girdhar BK (1995).
"Neuritic leprosy: further progression and significance". Acta Leprol 9 (4): 187–94.
PMID 8711979.
33. ^ Talwar S, Jha PK, Tiwari VD (September 1992). "Neuritic leprosy: epidemiology and
therapeutic responsiveness". Lepr Rev 63 (3): 263–8. PMID 1406021.
34. ^ a b U.S. Department of Health and Human Services, Health Resources and Services
Administration. (n.d.). National hansen's disease (leprosy) program Retrieved from
http://www.hrsa.gov/hansens/
35. ^ McMurray DN (1996). Mycobacteria and Nocardia. in: Baron's Medical Microbiology
(Baron S et al., eds.) (4th ed.). Univ of Texas Medical Branch. ISBN 0-9631172-1-1.
OCLC 33838234.
36. ^ Bhattacharya S, Vijayalakshmi N, Parija SC (1 October 2002). "Uncultivable bacteria:
Implications and recent trends towards identification". Indian journal of medical
microbiology 20 (4): 174–7. PMID 17657065.
37. ^ Pönnighaus, J. K. et al.; Is HIV Infection a Risk Factor for Leprosy? ; International
Journal of Leprosy and Other Mycobacterial Diseases; 1994 Dec;62(4):610-3

38. ^ Batista M. D. et al. ; Leprosy reversal reaction as immune reconstitution inflammatory
syndrome in patients with AIDS. Clin Infect Dis. 2008; 46(6):e56-60 (ISSN: 1537-6591)
39. ^ Menezes VM, Sales AM, Illarramendi X, et al. Leprosy reaction as a manifestation of
immune reconstitution inflammatory syndrome: a case series of a Brazilian cohort. AIDS.
Mar 13 2009;23(5):641-3.
40. ^ a b What is Leprosy?, The Leprosy Mission Canada
41. ^ Buschman, Ellen; Skamene, Emil (Jun 2004). "Linkage of leprosy susceptibility to
Parkinson's disease genes" (PDF). International journal of leprosy and other
mycobacterial diseases 72 (2): 169–70. doi:10.1489/1544-
581X(2004)072<0169:LOLSTP>2.0.CO;2. ISSN 0148-916X. PMID 15301585.
Retrieved January 31, 2011.
42. ^ http://www.nejm.org/doi/full/10.1056/NEJMoa1010536
43. ^ Rojas-Espinosa O, Løvik M (2001). "Mycobacterium leprae and Mycobacterium
lepraemurium infections in domestic and wild animals". Rev. - Off. Int. Epizoot. 20 (1):
219–51. PMID 11288514.
44. ^ Hastings RC, Gillis TP, Krahenbuhl JL, Franzblau SG (1988-07-01). "Leprosy". Clin.
Microbiol. Rev. 1 (3): 330–48. PMC 358054. PMID 3058299.
45. ^ Alcaïs A, Mira M, Casanova JL, Schurr E, Abel L (2005). "Genetic dissection of
immunity in leprosy". Curr. Opin. Immunol. 17 (1): 44–8. doi:10.1016/j.coi.2004.11.006.
PMID 15653309.
46. ^ "AR Dept of Health debunks leprosy fears". 2008-02-08. Retrieved 2008-04-08.
47. ^ Kaur H, Van Brakel W (2002). "Dehabilitation of leprosy-affected people—a study on
leprosy-affected beggars". Leprosy review 73 (4): 346–55. PMID 12549842.
48. ^ Doull JA, Guinto RA, Rodriguez RS, et al. (1942). "The incidence of leprosy in
Cordova and Talisay, Cebu, Philippines". International Journal of Leprosy 10: 107–131.
49. ^ Noordeen S, Neelan P (1978). "Extended studies on chemoprophylaxis against
leprosy". Indian J Med Res 67: 515–27. PMID 355134.
50. ^ Weddell G, Palmer E (1963). "The pathogenesis of leprosy. An experimental
approach". Leprosy Review 34: 57–61. PMID 13999438.
51. ^ Job C, Jayakumar J, Aschhoff M (1999). ""Large numbers" of Mycobacterium leprae
are discharged from the intact skin of lepromatous patients; a preliminary report". Int J
Lepr Other Mycobact Dis 67 (2): 164–7. PMID 10472371.
52. ^ Arch Dermato Syphilis 1898; 44:159–174
53. ^ Shepard C (1960). "Acid-fast bacilli in nasal excretions in leprosy, and results of
inoculation of mice". Am J Hyg 71: 147–57. PMID 14445823.
54. ^ Pedley J (1973). "The nasal mucus in leprosy". Lepr Rev 44 (1): 33–5. PMID 4584261.
55. ^ Davey T, Rees R (1974). "The nasal dicharge in leprosy: clinical and bacteriological
aspects". Lepr Rev 45 (2): 121–34. PMID 4608620.
56. ^ Rees R, McDougall A (1977). "Airborne infection with Mycobacterium leprae in
mice". J Med Microbiol 10 (1): 63–8. doi:10.1099/00222615-10-1-63. PMID 320339.
57. ^ Chehl S, Job C, Hastings R (1985). "Transmission of leprosy in nude mice". Am J Trop
Med Hyg 34 (6): 1161–6. PMID 3914846.
58. ^ CDC Disease Info hansens_disease Hansen's Disease (Leprosy)
59. ^ Montestruc E, Berdonneau R (1954). "2 New cases of leprosy in infants in Martinique"
(in French). Bull Soc Pathol Exot Filiales 47 (6): 781–3. PMID 14378912.

60. ^ Moet FJ, Pahan D, Oskam L, Richardus JH (2008). "Effectiveness of single dose
rifampicin in preventing leprosy in close contacts of patients with newly diagnosed
leprosy: cluster randomised controlled trial". BMJ 336 (7647): 761–4.
doi:10.1136/bmj.39500.885752.BE. PMC 2287265. PMID 18332051.
61. ^ Bakker MI, Hatta M, Kwenang A, et al. (1 April 2005). "Prevention of leprosy using
rifampicin as chemoprophylaxis". Am J Trop Med Hyg 72 (4): 443–8. PMID 15827283.
62. ^ Fine PE, Smith PG (1996). "Vaccination against leprosy—the view from 1996". Lepr
Rev 67 (4): 249–52. PMID 9033195.
63. ^ Karonga prevention trial group (1996). "Randomized controlled trial of single BCG,
repeated BCG, or combined BCG and killed Mycobacterium leprae vaccine for
prevention of leprosy and tuberculosis in Malawi". Lancet 348 (9019): 17–24.
doi:10.1016/S0140-6736(96)02166-6. PMID 8691924.
64. ^ "Chemotherapy of Leprosy". WHO Technical Report Series 847. WHO. 1994.
Retrieved 2007-03-24.
65. ^ "Seventh WHO Expert Committee on Leprosy". WHO Technical Report Series 874.
WHO. 1998. Retrieved 2007-03-24.
66. ^ Indian Annals of Medical Science
67. ^ Ravina, E. and Kubinyi, H. (2011). The Evolution of Drug Discovery: From
Traditional Medicines to Modern Drugs. John Wiley \& Sons. p. 80.
ISBN 9783527326693.
68. ^ Wozel, Gottfried; The Story of Sulfones in Tropical Medicine and Dermatology;
International Journal of Dermatology, Volume 28, Issue 1, pages 17–21, January 1989.
Published online as: DOI: 10.1111/j.1365-4362.1989.tb01301.x at URL:
http://onlinelibrary.wiley.com/doi/10.1111/j.1365-4362.1989.tb01301.x/pdf
69. ^ Rees RJ, Pearson JM, Waters MF (1970). "Experimental and Clinical Studies on
Rifampicin in Treatment of Leprosy". Br Med J 688 (1): 89–92.
doi:10.1136/bmj.1.5688.89. PMC 1699176. PMID 4903972.
70. ^ Yawalkar SJ, McDougall AC, Languillon J, Ghosh S, Hajra SK, Opromolla DV,
Tonello CJ (1982). "Once-monthly rifampicin plus daily dapsone in initial treatment of
lepromatous leprosy". Lancet 8283 (1): 1199–1202. doi:10.1016/S0140-6736(82)92334-
0. PMID 6122970.
71. ^ "Mortality and Burden of Disease Estimates for WHO Member States in 2002" (xls).
World Health Organization. 2002.
72. ^ Last Days Of A Leper Colony. CBC News. March 22, 2003.
73. ^ Surgery grants for leprosy sufferers in India. Times of India. February 2, 2009.
74. ^ Brachman, Philip; Abrutyn, Elias (2009). "Leprosy". Bacterial infections of humans
epidemiology and control: 415–438. Retrieved 12 December 2011.
75. ^ World Health Organization. (1985). "Epidemiology of leprosy in relation to control.
Report of a WHO Study Group". World Health Organ Tech Rep Ser (Geneva: World
Health Organization) 716: 1–60. ISBN 9241207167. OCLC 12095109. PMID 3925646.
76. ^ "Global leprosy situation, 2006" (PDF). Weekly Epidemiological Record 81 (32): 309–
16. August 2006. PMID 16903018.
77. ^ "DNA of Jesus-Era Shrouded Man in Jerusalem Reveals Earliest Case of Leprosy".
ScienceDaily. 2009-12-16. Retrieved 2010-01-31.
78. ^ "The Leprosy Archives in Bergen, Norway". Retrieved 2009-05-30.

79. ^ Hansen GHA (1874). "Undersøgelser Angående Spedalskhedens Årsager
(Investigations concerning the etiology of leprosy)" (in Norwegian). Norsk Mag.
Laegervidenskaben 4: 1–88.
80. ^ Irgens L (2002). "The discovery of the leprosy bacillus". Tidsskr nor Laegeforen 122
(7): 708–9. PMID 11998735.
81. ^ Wayne M Meyers ‘’Reflections on the International Leprosy Congresses and Other
Events in Research, Epidemiology, and Elimination of Leprosy. International Journal of
Leprosy; Volume 62, Number 3; 1991
http://hansen.bvs.ilsl.br/textoc/revistas/intjlepr/1994/pdf/v62n3/v62n3edt02.pdf
82. ^ "Bymuseet i Bergen". Bymuseet.no. Retrieved 2010-09-10.
83. ^ Greek Dictionary Tegopoulos-Fytrakis, Athens, 1999
84. ^ Artscroll Tanakh, 6
85. ^ Kane J, Summerbell RC, Sigler L, Krajden S, Land G (1997). Laboratory Handbook of
Dermatophytes: A clinical guide and laboratory manual of dermatophytes and other
filamentous fungi from skin, hair and nails. Star Publishers (Belmont, CA).
ISBN 0898631572. OCLC 37116438.
86. ^ a b c d e f g McLeod, Katrina C. D. and Robin D. S. Yates (June 1981). "Forms of Ch'in
Law: An Annotated Translation of The Feng-chen shih". Harvard Journal of Asiatic
Studies 41 (1): 111–163. doi:10.2307/2719003. JSTOR 2719003. Angela Leung's
Leprosy in China: A History (New York: Columbia University Press, 2009) is the
authoritative source on leprosy in China.
87. ^ "Leprosy". Catholic Encyclopedia. New York: Robert Appleton Company. 1913.
88. ^ Brody, Saul Nathaniel (1974). The Disease of the Soul: Leprosy in Medieval
Literature. Ithaca: Cornell Press.
89. ^ Lock et al; p. 420
90. ^ a b Kearns & Nash (2008)
91. ^ Aufderheide, A. C.; Rodriguez-Martin, C. & Langsjoen, O. (1998) The Cambridge
Encyclopedia of Human Paleopathology. Cambridge University Press ISBN 0-521-
55203-6; p. 148.
92. ^ Dwivedi & Dwivedi (2007)
93. ^ Kutumbian, P. (2005) Ancient Indian Medicine. Orient Longman ISBN 81-250-1521-3;
pp. XXXII-XXXIII
94. ^ Robbins G, Tripathy VM, Misra VN, Mohanty RK, Shinde VS, et al. (2009). Ancient
Skeletal Evidence for Leprosy in India (2000 B.C.) PLoS ONE 4(5): e5669.
doi:10.1371/journal.pone.0005669
95. ^ a b "Skeleton shows earliest evidence of leprosy". Associated Press. 2009-05-27.
Retrieved 2009-05-29.
96. ^ a b "Skeleton Pushes Back Leprosy's Origins". Science Now. 2009-05-27. Retrieved
2009-05-29.
97. ^ Shinde, Swati (2009-05-29). "Leprosy belonged to Ahar Chalcolithic era: Expert". The
Times of India. Retrieved 2009-05-29.
98. ^ "'Oldest evidence of leprosy found in India'". The Times of India. 2009-05-27.
Retrieved 2009-05-29.
99. ^ Robertson, Jo. "The Leprosy Asylum in India: 1886-1947." journal of the History of
Medicine & Allied Sciences. 64.4 (2009): 474-517. Print.

100. ^ Gould, Tony. A disease Apart: Leprosy in the Modern World. New York: St.
Martin's Press, 2005. Print.
101. ^ Leprosy — Medical History of British India, National Library of Scotland
102. ^ a b c d "Self-Care: Leprosy-related disabilities" in Invisible People: Poverty and
Empowerment in Indonesia, Irfan Kortschak, 2010
103. ^ "Official Permata Website". Permata.or.id. Retrieved 2012-01-15.
104. ^ Hansen's disease in Japan: a brief history Kikuchi I Int J Dermatol 1997:36:629-
633.
105. ^ McCurry, Justin. "Japanese Leprosy Patients Continue to Fight Social Stigma."
Lancet. 14 Feb 2004: 544. Web. 27 Nov. 2011. <www.thelancet.com>.
106. ^ Rafferty, Joy. "Curing the Stigma of Leprosy." Leprosy Review. 76 (2005):
119-126. Web. 8 Dec. 2011. <http://www.kit.nl/-/INS/24155/(57698)-ILS/KIT-ILS-
Dossiers.pdf>.
107. ^ Tayman, John (2007). The Colony: The Harrowing True Story of the Exiles of
Molokai. New York: Simon and Schuster. ISBN 9780743233019.
108. ^ Hamilton, Bernard (2000). The leper king and his heirs: Baldwin IV and the
Crusader Kingdom of Jerusalem. Cambridge, UK: Cambridge University Press. ISBN 0-
521-64187-X.
109. ^ Cung giu Nguyên (1955). "Contemporary Vietnamese Writing". Books Abroad
(University of Oklahoma) 29 (1): 19–25. doi:10.2307/40093803. JSTOR 40093803.
110. ^ Bryant A (1995). Sekigahara 1600: The Final Struggle for Power (Campaign
Series, 40). Osprey Publishing (UK). ISBN 1-85532-395-8. Retrieved 2010-02-28.
111. ^ "Numbers 12:9-16; - Passage Lookup - American Standard Version".
BibleGateway.com. Retrieved 2010-09-10.
112. ^ "Exodus 4:6; - Passage Lookup - American Standard Version".
BibleGateway.com. Retrieved 2010-09-10.
113. ^ "2 Kings; - Passage Lookup - American Standard Version". BibleGateway.com.
Retrieved 2010-09-10.
114. ^ "Luke; - Passage Lookup - American Standard Version". BibleGateway.com.
Retrieved 2010-09-10.
115. ^ "Luke 17:11-19; - Passage Lookup - American Standard Version".
BibleGateway.com. Retrieved 2010-09-10.
116. ^ Using the New World Translation of the Holy Scriptures Published by
Watchtower Bible and Tract Society of New York 1984: Moses was struck with leprosy
in his hand at Exodus 4:6; Moses' sister Miriam had leprosy at Numbers 12:10; Naaman
had leprosy at 2 Kings 5:1-7, 27; Uzziah had leprosy at 2 Chronicles 26:19,20; Simon
had leprosy at Matthew 26:6; and healings of leprosy by Jesus at Matthew 8:1-3, Mark
1:40-42, Luke 5:12,13