Is it Or isn’t it? · Nasolacrimal Duct Obstruction Membranous obstruction at valve of Hasner...
Transcript of Is it Or isn’t it? · Nasolacrimal Duct Obstruction Membranous obstruction at valve of Hasner...

Is it.....
Or isn’t it?Commonly confused
ophthalmologic diagnoses in the
outpatient setting
B. Christian Carter, MD
Albemarle Pediatric Ophthalmology and Strabismus
April 2019

I have no financial
interests to disclose

Adolescent red eye
Toddler red eye
The tearing infant
Preseptal or orbital cellulitis
Strabismus vs pseudostrabismus

Adolescent Red Eye
Acute conjunctivitis
Viral
Follicular response
Thin, watery discharge
Unilateral progressing to bilateral
Concomitant URI
Pre-auricular node
Self-limited, hygiene is key

Adolescent Red Eye
Bacterial
Papillary response
Thick, mucous discharge
Unilateral
Topical antibiotic drops
Beware GC/Chlamydia

Adolescent Red Eye
Allergic
Papillary response
Aqueous based discharge
Bilateral but can be asymmetric
Antihistamine gtts; systemic therapy

Contact lens induced conjunctivitis
More common in soft lenses
Etiology:
Mechanical trauma to superior tarsus by SCL
Hypersensitivity response to SCL polymer
Hypersensitivity response to surface deposits
on SCL
Clinical signs:
Injection, FBS, discharge
Decreased vision
Decreased SCL tolerance
Increased mobility / decentration of lens

Contact lenses
Cornea is avascular
Cornea extracts O2 from environment and returns CO2
as well
Complications
Contact lens induced conjunctivitis
Contact lens overwear (microcystic epitheliopathy)

Contact lens induced conjunctivitis
Papillary conjunctivitis
Papillary hypertrophy
(>0.3mm)
GPC (>1.0mm)
Punctate epithelial
erosions
Peripheral infiltrates
Corneal
neovascularization

Contact lens overwear
Epithelial damage
Central epithelial edema
(Sattler’s veil)
Decreased vision
Acute epithelial necrosis
Microcytic epitheliopathy
(epithelial cysts)
Extended wear
Pain, epiphora

Contact lens overwear
Keratitis
10-20 fold increase with
overnight wear
Gram negative organisms
Multifactorial
Corneal hypoxia
Decreased tear
secretion (20 fold)
Stagnant bacteria laden
tear film behind lens

Contact lens induced conjunctivitis
Medical therapy
Discontinue/decrease contact lens wear
Never overnight!
Consider change to daily disposable
Improve lens hygiene
Vigorous cleaning
Change lenses/cases routinely
Topical therapy
Discuss chronic nature of the condition

Toddler red eye
Corneal abrasion
Trauma may be unknown to parents
Epiphora often with photophobia and eye rubbing
Injected conjunctiva, +/- mucopurulent discharge
Flourescein staining
Lid eversion
Erythromycin ointment TID
Follow up in 1-2 days

Toddler red eye
Foreign body retention
Examine both eyes!
Eyelid eversion
check for hyphema, red reflex

Toddler red eye
HSV epithelial keratitis
Usually HSV-1
Endemic (90%, 2-5% with ocular
involvement)
Unilateral > bilateral
Exposure
Direct contact
Via trigeminal nerve from prior oral
infection

HSV Keratitis
Associated or preceding
blepharoconjunctivitis
Folliculosis, injection
Preauricular node involvement
Epithelial dendrites (“terminal bulbs”)
Preceding punctate keratopathy
Geographic ulcer
Stain with fluorescein or rose bengal

HSV geographic ulcer

HSV keratitis
Photophobia, ocular injection / pain
Clinical diagnosis
Corneal or conjunctival (cul-de-sac) swab
Treatment
Depends on comorbidities (uveitis, stromal disease)
Self limited
Trifluridine 1% 9x/day x 1 week
Not greater than 2 weeks (toxicity)
Oral acyclovir

HSV keratitis
Recurrence
As high as 25%
Immunocompetent status
Sunlight, temperature
Stress, menstruation
Long term low dose acyclovir
Amblyogenic!

The Tearing Infant

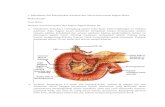
Nasolacrimal Duct Obstruction
Membranous obstruction at valve of Hasner
Mucopurulent d/c and epiphora in setting of non-injected conjunctiva
Assoc with angular blepharitis
Present in up to 20% of newborns
50% resolution by 3mo
80% resolution by 6mo
95% resolution by 11mo
Increased rate of recurrence after probing after 12mo (3% vs. 45%)*
Refer prior to 12 months!
Conservative nasolacrimal massage
Probe and irrigation vs. silicone tube
Katowitz JA, Welsh MG. Timing of initial probe and irrigation in congenital nasolacrimal duct obstruction. Ophthalmology 1987; 94:698-705.

Congenital Glaucoma
1:10,000 births; 66% bilateral
VA < 20/50 in 50%; blindness in 2-15%
Epiphora, photophobia, blepharospasm
Corneal edema (presence of Haab striae), increased CD (>11.5 in newborn, >12.5 in 1yo; buphthalmos)
Onset within first year in >80%
5% chance of affected parent having child (same with sibs)


Dacryocele
Proximal and distal obstruction
of tear outflow
Failure of mesodermal
canalization
Mucocele formation within
lacrimal sac (or nasal cavity)
Bluish discoloration inferior to
MCT
Unilateral or bilateral; 1% of all
NLDO
Female > male
Can progress to dacryocystitis

Dacryocele

Dacryocele
Mucocele extension into nasal cavity can impede breathing
DDx
Encephalocele
Hemangioma
Dermoid
Manual decompression
20-25% spontaneous resolution
Coverage with topical antibiotics after decompression
Systemic antibiotic coverage

Dacryocele
Surgical intervention if no
resolution with
conservative measures
By 6-8 weeks of life

Inflammatory Lid Disease

Preseptal cellulitis
Infection/inflammation of the orbital
tissues anterior to the septum
Etiologies
Direct (trauma, localized infection)
Contiguous spread (paranasal
sinuses, hordeolum, dacryocystitis)
Hematogenous (otitis, URI)
Sterile (retinoblastoma)
Gram positive cocci

Preseptal cellulitis
Lid edema, erythema
Absence of ocular injection
Absence of vision loss
Typically afebrile
Outpatient management
Response to oral antibiotics within 48
hours
IM/IV antibiotics for infants/toddlers,
febrile

Orbital cellulitis
Progression of preseptal
infection posterior to
septum
Gram positive cocci
Shared etiology
Ethmoid sinusitis
URI
10% subperiosteal
abscess

Orbital cellulitis
Chemosis
Proptosis
Motility restriction / diplopia
APD

Orbital cellulitis
Prompt neuroimaging
CT
Admission, broad spectrum IV
antibiotics
ENT consultation
Complications
Exposure keratitis
CRVO, optic neuropathy
Cavernous sinus thrombosis
Meningitis

Strabismus
heterotropia: a manifest strabismus
alternate fixation or strong fixation preference
Esotropia = image falls nasal to fovea
Exotropia = image temporal to fovea
Hypertropia = image superior to fovea
by convention, hypertropia unless restrictive
process
Excyclotropia = temporal rotation of 12 o'clock
Incyclotropia = nasal rotation of 12 o'clock

Strabismus
Heterophoria = latent deviation; tendency
for eyes to drift, but held in alignment by
interaction between binocular fusion and
muscular control
motor fusion = ability to keep eyes in
alignment
intermittent tropia = large, difficult to fuse
phoria in which latent deviation becomes
manifest (tired, sick, drunk)

Strabismus vs pseudostrabismus
Epicanthus: bilateral medial canthal fold
Superciliaris: below eyebrow to lacrimal sac
Palpebralis: equally distributed
Tarsalis: most prominent in upper eyelid
Inversus: most prominent in lower eyelid

Fixation Target
Use the smallest age appropriate target that will hold attention
Child’s shoulders square to yours
Head in primary position

Fixation Target

Abnormal Head Posture
Ocular causes
Superior oblique palsy
Abducens palsy
Nystagmus
Vertically incomitant strabismus
(A or V pattern)
Brown’s syndrome
Duane’s syndrome

Abnormal head posture

Cover Test
Good cover-uncover testing technique
Cover-uncover = manifest strabismus (“-tropia”)
Cross-cover = latent strabismus (“-phoria”)

Cover test

Alternate Cover Test
Cover is alternated between the two eyes rapidly breaking down fusion
Elicits phoric deviation

Corneal light reflex
Positive angle kappa
Visual axis slightly
temporal to pupillary
axis
Nasal displacement of
corneal light reflex,
simulating XT

Corneal light reflex
Remember, light is a
nonaccommodative
target
Most common ET is
accommodative
ET
Fixation target will
ensure
accommodation

Multiple choice
A 3 yo boy has a 2 week history of ocular injection
and photophobia. His fluorescein staining reveals
the following image. Appropriate management
would include:
A. Topical erythromycin ophthalmic ointment QID
with instructions to follow up in 1 week
B. HSV conjunctival culture with referral to
ophthalmology
C. Prednisolone 1% gtts QID with 5 day follow up

Multiple choice
A 7 yo boy presents with a 4 day history of increasing
periorbital edema and erythema, and remains
afebrile. Acuity is 20/20 OS and color vision is 12/12
OU. There is no chemosis, proptosis or APD. His only
complaint is pain on attempted adduction OS.
Appropriate next step would include:
A. Topical erythromycin ointment QID to the eye, lids
and lashes with 5 day follow up
B. Augmentin x 14 days with 2 day follow up
C. ED referral for parenteral antibiotics and orbital CT
scan, ophtho consult

Multiple choice
This 6 year old young man presents with
maternal complaints for “lazy eye.” Visual
acuity is 20/20 OU and stereotesting is intact.
Your cover/uncover test is unremarkable, as
well as an alternate cover test. Corneal light
reflex is symmetric OU. The next appropriate
step would be:
A. Reassurance to mom that all is well, RTC in 1
year/PRN
B. Repeat cover testing in forced primary
position
C. Referral to local developmental optometrist
for vision therapy (urgent)

Multiple choice

Thank you!