In Flight Patient Care Considerations for: Burns Neurological Spinal Cord.
-
Upload
reece-tremelling -
Category
Documents
-
view
220 -
download
0
Transcript of In Flight Patient Care Considerations for: Burns Neurological Spinal Cord.

In Flight Patient Care Considerations for:
BurnsNeurologicalSpinal Cord

Objective
• Apply knowledge of flight physiology and aviation environmental stressors in the planning and delivery of pre-flight and in-flight care of patients with cardiopulmonary, gastrointestinal, genitourinary, neurological, ophthalmologic, otorhinolaryngologic, orthopedic, and burn injuries and conditions

General Considerations
• Preflight Mode of transportPatient AssessmentSuppliesEquipment

General Considerations
• IV flow rates without pump
• O2 conversion table – sea level equivalent
• Securing patient and equipment
• Securing self
• Reliance on low tech physical assessment
• Hearing protection for patient and ERC personnel

Burn Injuries
• Preflight Assessment%TBSA burned, location and sourceStatus of airway and patencyVascular accessFluid requirementsPatency of foley, NGVital signs, POX, urine output

Burn Injuries
• Preflight AssessmentPain medication, sedationPeripheral pulsesPresent wound managementAssociated injuries and need for altitude
restriction (CXR)Secure vascular access, ET tube with
sutures

Burn Injuries
• Preflight AssessmentAssess Hct and transfuse if < 30% prior to
flightIf MD orders topical cream, apply evenly
1/16 to 1/8 inch thick and cover with absorbent dressing and Kling

Burn Injuries
• Stresses of flightAll stresses of flight will affect the burn
victim Thermal Decreased partial pressure of oxygenDecreased barometric pressureDecreased humidity

Burn Injuries
• In-flight considerationsMonitor mental statusAdminister warmed, humidified oxygen –
exception for face, head, neck burnsElevate headContinue with fluid resuscitation- second 24
hours add colloids – 200ml salt poor albumin/800ml LR at 0.5ml/kg/%TBSA

Burn Injuries
• In-flight considerationsSecond 24 hours addition of dextrose to
meet metabolic demands – D51/4 NSMaintain urine output >50ml/hr(75-100ml
for electrical) monitor for myoglobinuriaNG to gravity or suction -monitorHourly evaluation of all peripheral pulses

Burn Injuries
• In-flight considerationsProtect from convection heat losses – shield
from drafts and airflowMaintain core body temperature 99-100Dressings should be occlusive, NEVER
change en routeMedicate frequently – use small doses
Morphine 2-4 mg IVP. Avoid Demerol

Neurological Injuries
• Preflight AssessmentDiagnosis, treatmentAirway, Mechanical ventilation settingsLOC, GCSPupil assessmentVital signsMotor, sensory evaluation

Neurological Injuries
• Preflight AssessmentDiagnosis, treatmentAirway, Mechanical ventilation settingsLOC, GCSPupil assessmentVital signsMotor, sensory eval

Neurological Injuries
• Preflight Assessment Seizure activity, medicationsIVF, NG, Foley and patency

Neurological Injuries
• Stresses of flightDecreased partial pressure of oxygenBarometric Pressure ChangesDecreased HumidityG-Forces

Neurological Injuries
• In-flight considerationsField-level altitude restriction for all
penetrating, PBI induced head injuriesMaintain POX>/=95%, tight ETCO2
control between 25-27(pCO2 30-32)Administer paralytics, sedation as neededAvoid succinylcholine use for RSI – IIP

Neurological Injuries
• In-flight Considerations IVF in absence of causes of hypovolemia at 80ml
NS/hr – maintain MAP 65-70Closely monitor GCS, pupils –for deterioration in
GCS or pupil changes evidencing IIP administer 20% Mannitol 1-1.5 g/kg bolus
Maintain normothermic – protect from thermal changes

Neurological Injuries
• In-flight ConsiderationsElevate headNG/OG to gravity/suctionMonitor for seizure activity – administer
Dilantin prophylaxis, Valium for seizuresHypertension – administer MetoprololHearing protection, eye protection

ACCELERATION/DECELERATION FORCES
POSITIONING THE LITTER PATIENT
DURING TAKE-OFF/ LANDING

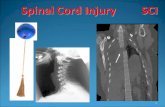
Spinal Cord Injuries
• Preflight Assessment
• Diagnosis and treatment
• Level of function
• Airway secured, mech ventilation settings
• Vital signs, POX,
• Foley, NG
• Medications

Spinal Cord Injuries
• Preflight AssessmentIVF and rateSpinal cord immobilization – goal to
preserve current level of function. Avoid logrolling patient
Spring loaded traction

Spinal Cord Injuries
• Stresses of flightALL!

Spinal Cord Injuries
• In-flight ConsiderationMaintain spinal immobilizationMaintain POX 95% or >, EtCO2 30-40
unless concomitant head injury then 25-27Altitude restriction if associated head injuryIVF 80ml/hr NSMonitor vital signs – Neosynephrine for
neurogenic shock? Dopamine?

Spinal Cord Injuries
• In-flight ConsiderationMaintain Methylprednisolone drip if in
progressProtect from hypothermiaProtect from G forces-loss of vasomotor
tone in spinal shock

ACCELERATION/DECELERATION FORCES
POSITIONING THE LITTER PATIENT
DURING TAKE-OFF/ LANDING

Questions????