Gallbladder, Liver, Pancreas and Spleen
Transcript of Gallbladder, Liver, Pancreas and Spleen

GALLBLADDER
functions as a reservoir for bile produced by the liver. It is 7-10 cm long, 3 cm wide at its broadest measure, and has a capacity of 30-50 mL
divided into 3 regions: fundus, body, and neck
bile produced by the left and right portions of the liver travel through the right and left hepatic ducts (1-2 mm in diameter). These two ducts join to form the common hepatic duct
the common hepatic duct lies anterior to the portal vein and to the right of hepatic artery
the common hepatic duct descends roughly 3 cm before the cystic duct (3-4 cm long) from the gallbladder joins it from the right
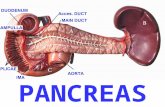
the common bile duct passes posterior to the first portion of the duodenum. It then descends via a groove on the superolateral portions of the posterior head of the pancreas sometimes traveling through the pancreas head. The four portions of the duodenum are labeled in white.
at the head of the pancreas, the common bile duct meets the pancreatic duct, and they exit into the second part of the duodenum, forming the hepatopancreatic ampulla (ampulla of Vater)
Adenomyomatosis one of the many causes for gallbladder wall
thickening pathologically, it is identified by proliferation of the
gallbladder mucosa with diverticular outpuochings known as Rokitansky-Aschoff sinuses
typically cholesterol deposits are seen within the gallbladder wall and cause a comet tail artifact
Causes of GB wall thickening biliary causes include:
-acute cholecystitis, gall bladder carcinoma, polyps, as well as adenomyomatosis
nonbiliary causes include:-CHF, hepatitis, pancreatitis as well as AIDs
cholangiopathy
Acute Acalculous Cholecystitis represents inflammation of the gallbladder in the
absence of demonstrated calculi

the disease process is distinct from the calculous variety, in which the primary initiating event is believed to be obstruction of the cystic duct
typically occurs as a secondary event in patients who are hospitalized and acutely ill from another cause
Pathophysiology at least 3 mechanisms
a. systemic mediators of inflammation and traumab. biliary stasisc. generalized or localized ischemia
in turn, the mechanisms often result in functional or secondary mechanical obstruction of the cystic duct from inflammation and bile viscosity
Sonographic signs compatible with acalculous cholecystitis
gallbladder wall thickening sonographically localized tenderness over the GB subserosal edema pericholecystic fluid gallbladder distention biliary sludge presence of gas
CT findings
gallbladder wall thickening mucosal irregularity luminal distention increased bile density (biliary sludge) intramural or intraluminal gas intraluminal hemorrhage localized pericholecystic fluid collections inflammatory infiltration of pericholecystic fat indistinctiveness of the liver-gallbladder interface
Acute Cholecystitis sonographic criteria for acute cholecystitis
-a thickened gallbladder wall (normal GB wall- <3 mm)
other sonographic findings-gallstones-positive Murphy’s sign-pericholecystic fluid as well as sonolucencies within
the gallbladder wall (indicates gallbladder wall edema)
Complications empyema gangrene perforation
Epigastric Pain
Chronic Cholecystitis with GB polyps chronic inflammation of the gallbladder results from
recurrent attacks of acute cholecystitis fibrotic reaction usually causes the gallbladder to
become small and contracted
Diffuse Wall Thickening most frequent gallbladder wall abnormality detected
by ultrasound the wall is >3mm thick this appearance is neither sensitive nor specific for
an inflammatory process
Case-patient is a 72-year old woman who presents with nausea and vomiting
Porcelain Gallbladder has been termed calcifying cholecystitis,
cholecystopathia chronic calcaria, or calcified gallbladder

are 5 times more common in women than in men most often considered a sequel of low-grade chronic
inflammation some have postulated that it is secondary to
intramural hemorrhage or an imbalance in calcium metabolism
Cholelithiasis is the pathologic state of stones or calculi within the
gallbladder lumen 75-80% of gallstones are of the cholesterol type 10-25% of gallstones are bilirubinate of either black
or brown pigment in Asia, pigmented stones predominate, although
recent studies have shown an increase in cholesterol stones in the Far East
Complications biliary colic- 56 % acute cholecystitis- 36 % acute pancreatitis- 4 % choledocholithiasis- 3 % gall bladder cancer- 0.3 % cholangitis- 0.2 %
Gall Stones
appear as single or multiple filling defects within the gallbladder and are densely calcified, rim calcified, laminated, or have a central nidus of calcification
stones also may present as a soft-tissue density or a lucent filling defect within the bile. Some stones may contain air
most gallstones have no signal on MRI and present as signal void-filling defects within the gallbladder
on T2-weighted sequences where signal-void stones are contrasted against high-signal bile
on T1 weighted sequences, bile usually shows a homogenous low signal

signal-void stones also may be apparent on T1-weighted images
high signal may be seen occasionally on T2-weighted images within stones that contain bile within clefts
stones with high fatty acid content may demonstrate high signal on T1-weighted images
Porcelain gallbladder along with distention and filled with sludge and calculi
associated with chronic gallbladder inflammation and gall stones in 95 % of cases
it appears as an echogenic arc with dense posterior shadowing
Carcinoma of the Gallbladder the most common primary hepatobiliary carcinoma the fifth most common malignancy of the GI tract predominantly affects older persons with long-
standing cholecystolithiasis GB epithelial tumors tend to behave similarly to
other GI adenocarcinomas GB tumors occur in the fundus in 60 % of patients, in
the body in 30 %, and neck 10 % early lymphatic spread occurs to the retroperitoneal,
right celiac, and pancreaticoduodenal nodes direct invasion of the liver, extrahepatic biliary ducts,
and duodenum, and colon occurs intraperitoneal seeding may occur
Ultrasound findings GB wall thickening single or multiple intraluminal mass extraluminal mass extending to the liver polyps larger than 1 cm in diameter
Extraluminal mass extending to the liver this often is accompanied by a large mass replacing
the GB fossa the mass often is complex with areas of necrosis
visible this is the most common manifestation of GB
carcinoma, accounting for 40-65 % of GB carcinomas
US shows echogenic mass adherent to gallbladder fundus (arrows). CT shows enhancing mass within the gallbladder (arrows) with involvement of the liver (arrow head)
LIVER
unique in having a dual blood supply- 75 % originating from the portal venous system and-25 % arising from the hepatic artery
the hepatic veins are responsible for drainage of filtered blood from the liver into the IVC
3 Functional Lobes right left caudate
the right and left lobes are further divided into 2 segments each:
-the anterior and posterior segments of the right lobe
-the medial and lateral segments of the left lobe
Segments

1-Caudate lobe2-Left superior lateral subsegment3-Left inferior lateral subsegment4a-Left superior medial subsegment4b-Left inferior medial subsegment5-Right inferior anterior subsegment6-Right inferior posterior subsegment7-Right superior posterior subsegment8-Right superior anterior subsegment
Bacterial (Pyogenic) Abscess 80-85 % of all abscesses are bacterial in origin bacteria gain access to liver via the portal or biliary
system. Possible causes are iatrogenic, biliary disease, diverticular disease, trauma, and inflammatory bowel disease
E. coli and anaerobes are the two most common offending agents in pyogenic abscess
most pyogenic abscesses occur in the right lobe
Radiogrpahic Findings (US) heterogenous, rounded masses with irregular,
thickened walls and poor peripheral definition fluid and debris inside the abscess can create
internal echoes gas-containing lesion also has acoustic shadowing
CT
heterogenous lesion with irregular margin (arrowhead) and possible peripheral enhancement
internal septations or papillary projections 20 % contain gas
Amebic Abscess trnasmitted by fecal-oral route
the organism, E. histolytica, first infects the colon, then gains access to the liver via portal venous system
patients generally present with right upper quadrant pain
Radiographic Findings (US & CT) indistinguishable from bacterial abscess. Tends to be
peripheral in location
CT Findings
generally non specific including: a peripherally based, round or oval low density
lesion which often demonstrates a peripheral rim of slightly higher attenuation
the peripheral rim will often enhance with contrast administration
Echinococcal Abscess dogs are the main intermediate hosts of hydatid
disease eggs get ingested, hatch in the stomach and
duodenum, travel to the liver via portal venous drainage, encyst in the liver and grow slowly
the cysts can exert mass effect on the surrounding liver and biliary system. The right lobe of the liver is most frequently involved
the cysts can rupture into the pleural cavity, peritoneal cavity, alimentary canal, or biliary tree, causing profound shock, peritonitis, and anaphylaxis
Radiographic Findings (US)

double-layered cyst, “classic” double-line sign, water lily sign, racemose
Diffuse Hepatic Disease
Cirrhosis
Causes alcohol alpha 1-antitrypsin postnecrotic (hepatitis) metabolic disease: Wilson, hemochromatosis,
glycogen storage disease congestive heart failure
Pathology hepatocyte necrosis fibrosis nodular regeneration
Radiographic Findings
Signs of advanced necrosis liver surface nodularity contracted liver with ascites atrophy of the posterior segments (VI, VII) of the
right lobe enlarged caudate lobe (I) and lateral segments (II, III)
of the left lobe prominent umbilical vein irregular enhancement
US- advanced cirrhotic liver appears to be nodular, irregular, and contracted with relatively enlarged caudate lobe (C) and lateral segment (L) of the left lobe. Fatty infiltration and fibrosis give a coarse echotexture of the liver parenchyma
Contrast CT: areas of fibrosis and regeneration may become isodense to parenchyma. The surface of the liver may be very nodular in cirrhosis
development of collateral vessels in portal hypertension
splenomegaly and the presence of ascites

Diffuse Fatty Infiltration a reversible process in which triglyceride
accumulates diffusely in hepatocytes causing abnormal appearance on imaging
normally, less than 5 % of the liver is composed of fat. In diffuse fatty infiltrated liver, fat can make up to 50 % of the liver tissue
commonly seen in acute or chronic alcohol abuse (most common), obesity, diabetes, cystic fibrosis, tetracycline, steroids, chemotherapy, malnutrition, and hyperalimentation
clinically, patients are asymptomatic. Liver can be enlarged but without splenomegaly
Radiographic Findings (US)
the liver has increased focal or diffuse echogenicity when compared to the surrounding organs such as the kidneys
Noncontrast CT- the liver looks hypodense to the spleen due to fatty infiltration, making the hepatic vasculature more prominent
Hemochromatosis iron overload leads to deposition in the liver. The
liver can be enlarged primary hemochromatosis: an autosomal recessive
disease that has abnormal absorption of iron in the intestine and thus causes iron to be deposited in hepatocytes, spleen, pancreas, and the myocardium
secondary hemochromatosis: caused by multiple transfusions with deposition of iron in the reticuloendothelial cells of the liver and the spleen. However, the pancreas is not usually involved. If the pancreas is involved, the hemochromatosis is usually of the primary type
CT: hyperdense liver (>75 HU). There are similar findings in Wilson’s disease, amiodarone toxicity, and previous thorotrast exposure
T1 and T2 weighted MRI: liver and spleen are hyperintense (very dark liver) compared with adjacent muscles owing to paramagnetic effect. Normally, the signal intensity of the liver

parenchyma is equal to or slightly greater than that of muscle
Simple Cysts the most common liver masses may be solitary or multiple cysts are found in 2-10 % of population, has
increased frequency with age and is more common in females aged 50-70
true hepatic cysts have bile duct origin and cuboidal epithelial lining. They are idiopathic, usually asymptomatic and variable in size. They cannot be distinguished from cysts that arise from prior hematomas or abscesses
they can be associated with other disease processes such as tuberous sclerosis and polycystic kidney disease
40 % of patients with polycystic kidney diseae have liver cysts
60 % of patients with multiple liver cysts have polycystic kidney disease
Radiographic Findings
US (95-99 % accurate) anechoic posterior enhancement (increased transmitted
sound) well-defined or imperceptible walls
Non-contrast CT: density of less than 20 HU, well-defined margins, no perceptible wall (arrow)
Contrast CT: no enhancement after contrast administration
MRI
T1 weighted- homogeneously hypointense (arrowhead)
T2 weighted- homogeneously hyperintense (arrow) due to water property (comparable to the intensity of CSF or gallbladder bile
Differential Diagnosis cystic liver mass with internal echoes, thick
septations, or a perceptible wall noted on US include-hemorrhagic cyst-abscess-echinococcal cyst-biliary cystadenoma-cystic metastasis (e.g. ovarian)-HCC with necrosis
Hemangioma is a benign proliferation of vascular tissue lined with
endothelium which has slow hepatic arterial blood flow
two types are capillary (more common) and cavernous
occurs in the right lobe can easily be confused with metastases or hepatoma the most common cause of a hyperechoic liver mass
on US large hemangioma may appear heterogenous. There
may be thrombosis or a central stellate scar with a giant hemangioma

US: hyperechoic and well-defined
T1 weighted MRI- hypointense to liver (arrows). If gadolinium-diethylenetriamine penta-acetic acid (Gd-DTPA) is used, peripheral enhancement is seen initially with central enhancement within 15-30 minutes. Enhancement is persistent
T2-weighted MRI- hyperinetense to the liver (just like a cyst; arrows). Looks as bright as a light bulb! Intensity is as high as that of pure fluid (CSF or bile)
Focal Nodular Hyperplasia most likely seen in young women (3 %)
Pathology a non-capsulated nodular mass was thought to be a vascular/hamartomatous
malformation is composed of normal hepatocytes, Kupffer cells,
and bile ducts but arranged abnormally is less than 5 cm in diameter, most commonly found
peripherally in the right lobe
classic appearance: solitary, well-circumscibed mass with a central stellate scar of fibrosis even though the central scar is seen in only 20 % of the cases
Non-contrast- the lesion has low attenuation (arrows) compared with the normal liver. The central stellate scar may also show low attenuation
Contrast CT: the lesion shows homogenous enhancement early in arterial phase (arrows) with prompt wash out. The central stellate scar will not enhance.
T1-weighted MRI: The lesion is hypo-isointense to the normal liver. The central scar enhances with Gd-DTPA.
T2-weighted MRI: The lesion is isointense to slightly hyperintense to liver. The central scar is hyperintense to the liver (arrows). (In contrast to hypointense appearance of the central scar in large hemangioma)

Hepatocellular Carcinoma (HCC)
the most common primary hepatic tumor and one of the most common cancers worldwide a primary malignancy of hepatocyte origin
3 Growth Patterns of HCC
Solitary mass – often large Multifocal or Nodular Pattern – multiple nodules Diffuse – multiple, small foci scattered diffusely
throughout liver
US Findings
Small HCCs can be homogenously hyperechoic and can mimic hemangioma. This can result when a large proportion of fat is present in the tumor
Small HCCs can appear hypoehcoic with larger HCCs frequency mixed in echogenicity.
In the Portal Venous Phases
Small lesions may be isodense or hypodense and difficult to see, since the remainder of the liver increases in attenuation.
Larger lesions with necrotic regions remain hypodense.
Contrast CT: dense diffuse non-uniform enhancement in arterial phase; some lesions are hypervascular
MRI
T1-weighted: usually hypointense to normal liver. When fatty change, fibrosis, or copper is present, variable signal can be seen.
With Gd-DTPA, hypervascular lesions enhance early in the arterial phase.
Liver Metastasis
The liver is the most commonly involved organ by metastatic disease, after the lymph nodes.
The most common primary sites are the eye, colon, stomach, pancreas, breast and lung.
In children the most common liver metastases are from a neuroblastoma, Wilm’s tumor or leukemia.
Causes of Echogenic Metastases
Mucinous adenocarcinoma of the colon, Pancreatic carcinoma (usually hypoechoic but possibly becoming echogenic as calcification occurs), Gastric carcinoma (usually hypoechoic), HCC, Neuroblastoma, Cholangiocarcinoma, Treated Breast Carcinoma, Renal cell Carcinoma, Carcinoid,

Choriocarcinoma, Pancreatic Islet Cell tumors, Wilm’s Tumor (usually spread to the lungs), Kaposi sarcoma, Myeloma deposit, Hepatic chloroma
Causes of Hypoechoic Metastases
Lymphoma (especially AIDS related), HCC, Pancreatic carcinoma, Lung (particularly adenocarcinoma), Cervix, Melanoma, Nasopharyngeal carcinoma, Kaposi sarcoma (rare, most are hyperechoic), Myeloma deposits, Cystic liver metastases, Mucinous cystadenocarcinoma colon, Cystadenocarcinoma ovary. Cystadenocarcinoma pancreas, Leiomyosarcoma, Squamous cell carcinoma, Testicular CA, Carcinoid, Graunulosa cell ovarian tumor.
Cystic metastases
Two groups of patients tend to get cystic metastases:
(1) Patients who have a primary neoplasm with a cystic component such as a mucinous cystadenocarcinoma of the colon, stomach, pancreas, or ovary and,
(2) Patients with metastases that are undergoing central necrosis, when low-level echoes and wall irregularity is seen. Squamous cell carcinoma, leiomyosarcoma, melanoma, and testicular carcinoma, have a propensity to undergo extensive central necrosis.
Causes of Bull’s Eye or Target, Metastases
The halo is most probably related to a combination of compressed normal hepatic parenchyma around the mass and a zone of cancer cell proliferation
The presence of a halo usually suggests aggressive behavior
Bronchogenic carcinoma Breast and colon as well as Primary malignant liver neoplasms (eg.
HCC) and Benign liver neoplasms (eg. Adenoma in
glycogen storage disease)
Causes of heterogeneously Echogenic Liver Metastases
Breast, colon and/or rectum, stomach (especially anaplastic lesions) and cervix
Other causes of heterogeneously liver metastases include the ff: HCC (especially when complicated with hemorrhage), carcinoid, melanoma, and bronchogenic carcinoma.
Portal Vein Thrombosis
Five causes of portal vein thrombosis:
1. Pancreatitis2. Cirrhosis3. Hepatic or biliary surgery4. Hepatoma with tumor thrombus5. Hypercoagulable states
CT: example of carcinoma in the hepatic vein

PANCREASAcute Pancreatitis
Common cause of pancreatitis include alcohol abuse, choledolithiasis, hypergylceridemia and hypercalcemia. Acute pancreatitis usually presents as an acute episode of upper abdominal pain, with or without accompanying GI symptoms.
Other symptoms may include fever, hypotension, pulmonary edema or shock. Laboratory values reveal elevated WBC, serum amylase and pancreatic lipase. Initial treatment of pancreatitis includes NPO, NG suction, analgesics, parenteral or jejunal feeding. Prophylactic antibiotics may also be of benefit.
Ranson’s score estimates the life threatening complications or death in patients with acute pancreatitis using several factors at the time of admission and during the first 48 hours thereafter.
Ranson’s Score
Values at Admission First 48 Hours
Age>55
WBC >16,000/ml
Glucose >200mg/dl
LDH>350 U/L
AST > 250 U/L
Hct fall >10%
Ca >8mEq/L
BUN rise > 5mg/dl
PaO2 < 60mmHg
Base defect > 4 mEq/L
Fluid sequestration > 6L
Number of Criteria Mortality
0-2
3-4
5-6
≥7
<5%
15-20%
40%
>99%
Balthazar et al developed a classification system for patients with acute pancreatitis based on radiologic findings
Balthazar et al Radiographic Grading of Acute Pancreatitis
Grade Radiographic Findings Prognosis
Grade A
Normal appearing pancreas
Grade B
Focal or diffuse enlargement of the pancreas
Mild, uncomplicated course
Grade C
Pancreatic gland abnormalities associated with pancreatic fat infiltration
High risk of complications associated with acute pancreatitis
Grade D
Single fluid collection
Grade E
Two or more fluid collections.
Nausea, vomiting with abdominal pain that radiates to the back
Acute Necrotizing Pancreatitis
Pancreatic necrosis is a known complication of acute pancreatitis.
Areas of necrosis are usually multifocal and rarely involve the entire gland.
Necrosis develops earl in severe pancreatitis and is usually established within 96 hours of the onset of clinical symptoms.

Pancreatic Pseudocysts
The most common cystic lesions of the pancreas accounting for 75-80% of such masses
A collection of amylase-rich, lipase-rich, and enterokinase-rich fluid
Most frequently located in the lesser peritoneal sac in proximity to the pancreas
Large pseudocysts can extend to the paracolic gutters; pelvis; mediastinum
Some are loculated
Most Common Etiologies
Chronic pancreatitis Acute pancreatitis and Pancreatic trauma In addition, pseudocysts are associated with
pancreatic ductal obstruction and pancreatic neoplasms
US Findings
An anechoic structures associated with acoustic enhancement
Well defined and round or oval, and they are contained within a smooth wall
During the early phases, the more complex, with varying degrees of internal echoes
Usually, this appearance results from the presence of necrotic pancreatic and peripancreatic debris and is more common in pseudocysts that form as a result of acute necrotizing pancreatitis than in others. The debris is cleared over time.
The pseudocysts can appear more complex in 2 other instances: when hemorrhage occurs in the cyst or when infection of the cyst complicates the clinical course
Color Doppler or duplex scanning should always be performed in cystic lesions to ensure that the lesion in question is not a giant pseudoaneurysm
Abdominal CT is an excellent choice for imaging acute fluid collections and pancreatic pseudocysts
CT characteristics of an acute fluid collection include low attenuation and a homogenous appearance
CT attenuation values may measure greater than 20-30 HU because of the presence of necrotic pancreatic or peripancreatic debris or blood within the confines of the acute fluid collection.
Pancreatic Cancer
The findings of an invasive hypodense mass in the had of the pancreas which involves the SMV and SMA along with enlarged lymph nodes are most suggestive of pancreatic CA
The 5th most common cause of cancer deaths It is approximately twice as common in males
compared to females Patients are usually greater than 50 years old Greater than 90% of pancreatic cancers are
ductal adenocarcinoma and its variants Most of the remaining 5-10% are islet cell
tumors Arises in the head of the pancreas 70% of the
time, in the body 20%, and in the tail 10%. Abdominal pain and weight loss are present in
greater than 75% of patients with pancreatic cancer, and jaundice is present in greater than 80% of patients with pancreatic heat tumors secondary to biliary obstruction
CT
The best modality for imaging the pancreas A mass deforming the size and contour of the
pancreas is the most common finding for ductal cell carcinomas occurring in 96% of the cases
A central zone of decreased attenuation is present in 83% of pancreatic head and 60% of pancreatic body carcinomas
CT can be used for staging purposes with the findings of the retroperitoneal extension, major vascular involvement, invasion of contiguous organs, ascites, LN and distant metastases suggesting unresectability.
Adenocarcinoma
The fourth most common cancer The prognosis of the disease is poor and very few
patients survive longer than one year Major role of imaging once the primary diagnosis has
been made is to “stage” the disease to determine operability
The loss of the fat plane indicates encasement of the artery making the patient uncurable
CT Findings of Pancreatic CA

Alteration in the morphology of the gland with abnormalities of CT attenuation values
Obliteration of peripancreatic fat Loss of sharp margins with surrounding structures Involvement of adjacent vessels and regional lymph
nodes Pancreatic ductal dilatation Pancreatic atrophy and, Obstruction of the common bile duct (CBD)
Mucinous Cystic Neoplasm
Mucinous Cystic Tumors
So called macrocystic cystadenomas or, cystadenocarcinomas.
Predominate in the body and tail of pancreas, have a strong female predilection
Most common of cystic pancreatic tumors, accounting for 45-50% of tumors
Multiloculated tumors with a characteristic smooth glistening surface
Arise from oversecretion of the mucus of the hyperplastic columnar lining of the ducts. The cysts contain thickened viscous material, which can also be hemorrhagic
Nonenhanced CT scans show a well-defined unilocular or multilocular, externally smooth, round-to-ovoid mass with fluid attenuation
The attenuation values of the multilocular cysts vary according to the degree of hemorrhage or protein in the mucoid cysts
Larger cysts may demonstrate small daughter cysts along its internal surface. Typically, they show a well defined, multilocular cystic mass with thick internal mass septae separating the separating the different cystic cavities of varying sizes. The cysts are 2-26cm.
Visualization of the nodule with irregular borders of the septae and calcification which is curvilinear or punctate and confined to the cyst wall or septa
CECT show enhancement of the cyst wall, internal septations, mural nodules, and other intracavitary projections
CT may also allow the identification of solid components associated with cystic elements, which are features of borderline or malignant tumors but
not benign variants. MCN’s develop predominantly in the tail of the pancreas (>90%)
CT more clearly demonstrates enhancement of the cystic walls and septa
US Features
Usually larger than 5cm The walls are composed of thick, fibrous stroma
sometimes containing dystrophic calcification A large cystic mass sometimes with numerous septa
and debris The tumor may be 2-23cm, and they usually have
sharply marginated walls and smooth borders Typically show a multilocular, fluid-containing mass
with good transmission and strong acoustic enhancement
Compared with serous cystic tumors, the cysts in MCNs are larger (>20mm in diameter) and less numerous (usually <6). CT-guided aspiration of the cyst can provide further diagnostic clues and enable their differentiation from other pancreatic cystic masses (eg, pseudocyst, serous cystadenoma, and solid and pseudopapillary neoplasm)
MCN cyst fluid typically has a high viscosity, low amylase levels, and high CEA and carbohydrate antigen (CA) 72-4 levels, and they may show malignant cytology in patients with mucinous cystadenocarcinomas. Periodic Acid-Schiff (PAS) and May Grunwald/Giemsa (MGG) stains are usually positive for extracellular as well as intracellular mucin.
Mucinous Cystic Neoplasm
Intraductal Papillary Mucous Neoplasm
Papillary neoplasm that arises within the MPD or its branches
The tumor hypersecretes mucin, which often leads to duct dilatation and/or chronic obstructive pancreatitis

Are premalignant and may histologically demonstrate areas ranging from hyperplasia to carcinoma within in a single tumor
The tumors generally show intraluminal, longitudinal growth but is usually slow to invade periductal tissues radially and slow to metastasize.
Most commonly localized to the head of the pancreas, but they may occur at any site along the pancreatic ductal system
Ductal dilatation is often impressive any may mimic MCNs on CT scans
Is recognized as predominantly a solid tumor with a central cyst. The cystic variety consists microscopically of cyst like spaces with papillary protrusions.
Intraductal Papillary Mucinous Tumor
In these cases, the findings on ERCP may be diagnostic. Rarely, segmental pancreatic duct dilatation may acquire a cystic appearance, whereas the MPD and the rest of the pancreas appears normal.
Microcystic Adenoma
Cystic mass in the region of the tail of the pancreas.
Hypervascular tumor in the pancreatic tail with sunburst calcification. Note the Swiss-cheese enhancement.
SPLEENAccessory Spleens
Or splenculi, are relatively commonly encountered “normal” anatomic variants
Estimated to be present in approximately 10% of the population
May be single or multiple in occurrence Are most frequently discovered in the vicinity of the
splenic hilum or elsewhere within the gastrosplenic ligament
They may, however, be found along the omentum, or anywhere else within the peritoneal cavity
CT Findings
Attenuation and contrast-enhancement characteristics that are identical to those of normal spleen
Measures approximately 1.0-1.5cm in diameter, but may range in size a few millimeters to several centimeters (2.3)
Resection of all accessory spleens is recommended at the time of the splenectomy, as cases of accessory-splenic hypertrophy have been described subsequent to removal of the “main” spleen

Accessory Spleen (s)
Splenic Cysts
The differential diagnosis of large splenic cysts should include posttraumatic cysts (most common), epidermoid cysts, abscess, pancreatic pseudocyst, echinococcal cysts, lymphoma, infarction or cystic lymphangiomas (less common). Splenic cyst shown below as imaged on US.
An example of calcified splenic cyst shown first on plain radiograph (left) with a coronal CT construction (right). Note the clear demarcation of the calcified cyst capsule.
Metastases: the axial CT images demonstrates multiple hypoenhancing lesions in the spleen consistent with metastatic CLL.
Images of splenic metastasis visualized on US. Careful ultrasound examination can determine if these are cysts with increased through transmission of echoes versus solid metastatic lesions.
Lymphoma
Lymphomas is the most common malignant tumor of the spleen. Typically, lymphatic drainage to the spleen serves as the primary mechanism by which extranodal lymphomas of varying types by which extranodal lymphomas of varying types disseminates to the spleen. Of the two broad types of lymphoma (B vs. T cell), B cell lymphomas Hodgkin’s and non Hodgkin’s disease are often diagnosed from splenic

imaging. Primary splenic lymphoma (PSL) is a rare malignancy with a reported incidence of less than 1% of all lymphomas.
Case
Twenty-three year old woman with non-Hodgkin’s lymphoma.
Splenic Calcifications
Infectiouso Previous granulomatous disease
(tuberculosis, histoplasmosis)o Opportunistic infection in AIDS patients
(Pneumocystis carinii) Traumatic Vascular
o “phleboliths”o Post-ischemic/infarction
The plain film shown demonstrates numerous round calcifications diffusely distributed specifically within the spleen. The likely etiology of the calcified granulomata is Histoplasmosis, which have this characteristic appearance in comparison to microabscess.
Case
33-year old woman with fever of unknown origin. Patient is HIV +.
Pneumocystis carinii infection in the spleen
Important cause of pneumonia in an immunocmporomised host
Common sites of dissemination include lymph nodes, liver, bone marrow, and spleen.
Splenic pneumocystic carninii infections have been described typically as low attenuation lesion which may contain internal calcifications.
Differential diagnosis of cystic lesions
Post traumatic Epidermoid Epithelial and Echinococcal cyst Abscess Lymphoma and Metastatic lesions may also appear as regions of
decreased attenuation in the spleen that may mimic cystic lesions
Splenomegaly
lymphoma leukemia cirrhosis portal hypertension