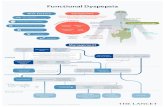
Functional Dyspepsia
description
Transcript of Functional Dyspepsia

10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
Functional Dyspepsia patient bupa.co.uk

2
10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
Functional dyspepsia, sometimes referred to as non-ulcer dyspepsia, is a common functional disorder of the upper digestive tract (stomach and upper small intestine). Functional dyspepsia is characterised by chronic or recurrent upper abdominal pain or discomfort, often in conjunction with feelings of early satiety (fullness), pressure in the abdomen, burning, bloating, belching or nausea. Symptoms may occur after eating a meal, but can happen at any time. Similarly, certain foods or drinks may worsen symptoms for some people.
As with other functional disorders, there is no evidence of organic disease or other structural abnormality in the gut (such as an ulcer or inflamed esophagus) that can account for the symptoms that are present.
While the condition is uncomfortable and can be distressing, especially if symptoms are chronic, functional dyspepsia does not cause other, more serious conditions. The symptoms associated with functional dyspepsia can be addressed, as outlined further in this leaflet, and the prognosis for the condition is generally quite good.
INTRODUCTION

3
10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
The exact cause of functional dyspepsia is not known, however symptoms are thought to be linked to an increased sensitivity in the esophagus and upper gastrointestinal system, which can be triggered by a variety of factors.
these may include: impaired peristalsis (contraction and relaxation of the intestinal muscles that move food through the upper digestive tract), acid secretion, diet, lifestyle, and psychological factors. Many people with functional dyspepsia have an increased awareness of their stomach and upper gut activity and can have impaired digestion or be sensitive to food intake. Many people with functional dyspepsia find that certain foods can make symptoms worse, however, food is not the cause of functional dyspepsia.
Functional Dyspepsia is one of several conditions known as functional gastrointestinal disorders. The term ‘functional disorder’ refers to the presence of symptoms with a normal clinical examination and normal investigations. In other words there is nothing visibly wrong with the body. In the case of functional dyspepsia, the lining of the gut is not inflamed and the amount of acid in the stomach is normal. This can be very frustrating for patient and clinicians especially when the symptoms are very severe. An ‘organic disorder’ refers to conditions where symptoms are associated with findings on clinical examination and/or abnormal diagnostic tests which identify the source of symptoms and direct future treatment.
CAUSES

4
10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
CONTRIbUTORy ElEMENTS TO ThE DEvElOpMENT OF FUNCTIONAl DySpEpSIA
Biological factors
Functional dyspepsia can be caused by a failure of the stomach or upper digestive system to move food through the body in a normal way. Typically, the body moves food through the digestive system by rhythmically contracting and relaxing the muscles of the digestive system. In this way, food moves from the stomach through the intestinal tract. however, in those with functional dyspepsia, this process is often disturbed and the stomach or small intestine may not relax, contract, or empty normally after a meal.
Issues relating to the brain-gut axis
The link between the brain and the gut has been well established. Research using MRI scans showed that certain areas in the gut and in the brain are more active in functional dyspepsia than in non-functional dyspepsia subjects. It is therefore believed that functional dyspepsia is related to excessive nerve transmission between the gut and the brain, which is mediated by nerve chemicals (neurotransmitters). In other words, a primary trigger driving functional dyspepsia symptoms is that the gut is hypersensitive to stimuli and that food does not pass through the digestive systems of people
with functional dyspepsia properly. This is because the signals that travel back and forth from the brain to the gut, controlling the nerves, are disrupted in some way. because of this, food, drinks, and emotions may trigger pain. The sensitivity, as mentioned above, stems from hypersensitive gut nerves that send excess signals to the brain, particularly to the area that processes pain. The brain then sends abnormal signals back to the gut to alter its motility or relax muscles. This back and forth electrical communication between the brain and gut is represented by the brain-gut axis and understanding this interaction forms the basis of current treatment approaches to functional dyspepsia.
Emotional factorsIt has recently become evident that stress and other psychological factors, such as anxiety and depression, can affect the gastrointestinal system. These psychological factors can make functional dyspepsia symptoms worse, and sufferers more sensitive and less tolerant of food. heightened emotional states can lead to chemical changes in the body that can hinder the process of digestion. This can be cyclical as well, as the uncomfortable nature of functional dyspepsia can lead to more stress, depression, anxiety or anger.

5
10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
General SymptomsThe symptoms of functional dyspepsia vary between each individual, as does their severity. At times, symptoms and signs can be mild, and at other times they can be painful and debilitating. Symptoms are often worse after eating and tend to come and go in bouts.
Core symptoms of functional dyspepsia often include the following:
o pain or discomfort in your upper abdomen or chest
o A feeling of fullness in your upper abdomen
o A burning feeling in your neck or esophagus (heartburn)
o loss of appetite
o belching
o bloating
o Nausea
o vomiting
SyMpTOMS
Stress/depression/anxietyThe symptoms of functional dyspepsia can mostly be managed at home and do not require urgent care. however, due to the discomfort, pain and/or distress of functional dyspepsia, the clinical picture may well be accompanied by feelings of depression, anxiety and/or stress. These psychological factors should be related to your doctor, who can help to manage or treat them, along with your physical symptoms.
Alarm symptomsIt is important to see a doctor if you have:
o a noticeable change in any of the general or associated symptoms of functional dyspepsia
o difficulty swallowing
o difficulty breathing
o frequent vomiting or blood in your vomit
o family history of stomach cancer
o family history of gastric cancer
o shortness of breath
o unintentional weight loss
o or if you are 55 or older

6
09659 IBS Medical Brochure • 297x210mm • CMYK • 13.12.13 • DL 09659 IBS Medical Brochure • 297x210mm • CMYK • 12.12.13 • JA
DIAGNOSISFunctional dyspepsia is a functional gastrointestinal disorder, with no obvious physical abnormalities of the digestive tract, and so there is no specific test that can determine if it is present. Therefore, functional dyspepsia is largely a diagnosis of exclusion. your doctor will need to ask you a series of health questions, take your medical history, and complete a physical exam in order to rule out other causes. A diagnosis is made based on the symptoms you describe and the exclusion of other causes.
An international working group developed a list of diagnostic criteria for functional dyspepsia. These criteria were developed in Rome and are now at their third version hence they are being referred to as the ‘Rome III criteria’.
In some cases, particularly if you have alarm symptoms (see previous heading), your doctor may want to carry out additional tests. This is to rule out the possibility of other, more serious conditions, or infection or inflammation or the upper GI tract.
FUNCTIONAl DySpEpSIA ROME III DIAGNOSTIC CRITERIA
Symptoms must include one or more of the following:
bothersome postprandial fullness
Early satiation
Epigastric pain
Epigastric burning
AND
No evidence of structural disease (including at upper endoscopy) that is likely to explain symptoms
1
2
3
4
5
These criteria need to be fulfilled for the last three months with symptom onset at least six months prior to diagnosis

7
09659 IBS Medical Brochure • 297x210mm • CMYK • 13.12.13 • DL 09659 IBS Medical Brochure • 297x210mm • CMYK • 12.12.13 • JA
In some cases, particularly if you have alarm symptoms (see previous heading), your doctor may want to carry out additional tests. This is to rule out the possibility of other, more serious conditions, or infection or inflammation or the upper GI tract.
FURThER TESTSIf alarm symptoms are raised, further tests may be recommended in order to rule out other conditions. Further investigations may include the following, depending on your symptoms and concerns:
Endoscopy This test is used to examine the oesophagus, stomach, and duodenum by inserting a thin, flexible tube down the oesophagus.
Helicobacter pylori test A stool or breath test may be performed to rule out the presence of h. pylori, which is a type of infection sometimes associated with dyspeptic symptoms.
Blood testsA blood sample may be required to rule out more serious conditions.
Barium swallow and meal X-rayThis test involves ingesting a drink that contains barium prior to having an abdominal X-ray. barium is a substance that can be seen on X-ray images, enabling your doctor to more clearly see the inside of your gut
Computerised tomography (CT) scan A CT scan may be used to scan the abdomen and pelvis, producing cross-sectional images of the abdominal organs, which can be used to help rule out other physical causes for symptoms.
Food allergy testsIf your doctor suspects your symptoms may be linked to an intolerance of certain foods, he or she may order a food allergy test or ask you to eliminate certain products from your diet for a period of time.

8
10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
Once diagnosed with functional dyspepsia, there are a number of treatment options that can help you alleviate your symptoms. Sometimes, with mild to moderate cases of functional dyspepsia, symptoms can be managed at home by changing elements of your diet and lifestyle. When symptoms are more severe, or if your functional dyspepsia has become chronic, medication and psychological treatments can also be useful. The different psychological treatments for functional dyspepsia are cognitive behavioural therapy (CbT), psychodynamic psychotherapy and hypnotherapy.
Discussing these treatment options with your doctor, while considering your symptoms and how functional dyspepsia is affecting your daily life, can help identify the most appropriate treatment options.
Diet, Lifestyle, and ExerciseIf a dietary or lifestyle cause is suspected, it may be helpful to change your diet or exercise regime. your Gp may also refer you to a dietician or recommend some of the following dietary changes to see if they help reduce your symptoms.
Diet
identify problem foods
In many cases, certain foods and drinks can exacerbate the symptoms of functional dyspepsia. Foods with a high fat or sugar content, for example, can slow down the passage of food through the gut and break down producing gas and liquid, which may make dyspeptic symptoms worse. While these foods are not the cause of functional dyspepsia, your gut may not tolerate them well. Identifying and limiting your intake of certain types of foods, in conjunction with a healthy, balanced diet, may improve your symptoms.
Consider the following list of foods and drinks that are sometimes associated with functional dyspepsia and consider limiting your intake if you are finding any of these make your symptoms worse:
o fatty foods (such as fried food, higher fat meats, cheese, nuts, etc)
o acidic foods (such as citrus fruits/juice or tomatoes and tomato-based products)
o spicy foods
o alcohol
o caffeinated beverages (such as coffee, tea or soda)
o carbonated beverages
o lactose
o chocolate
Eat regularlyIrregular eating patterns have been proven to exacerbate the symptoms of functional dyspepsia. Try to eat meals at regular intervals and avoiding skipping meals or going a long time without eating, which can make symptoms worse. Eating small to moderate portions and eating slowly have also been known to decrease symptoms of functional dyspepsia.
Lifestyle
smoking
Smoking is known to greatly exacerbate the symptoms of functional dyspepsia. If you smoke, it is recommended that you quit.
caffeine and alcohol
Caffeine and alcohol are known to worsen the symptoms of functional dyspepsia. If you consume caffeinated or alcoholic beverages, it is recommended that you reduce your intake of these, or exclude them altogether.
Weight Management
If you are overweight, your doctor may recommend losing weight or seeing a nutritionist who can help you identify and address your diet. being overweight can contribute to the symptoms of functional dyspepsia and losing weight may help improve or alleviate your symptoms.
exercise
your doctor will likely recommend that you exercise regularly. Many people find a light to moderate exercise regime helps alleviate symptoms of functional dyspepsia and reduces stress. Talk to your Gp about finding the type of exercise programme that would be most suitable and enjoyable for you. Try to exercise three times per week, for a minimum of 30 minutes, doing something that increases your heart rate and breathing, such as brisk walking, swimming, cycling or using a cardiovascular machine.
Therapeutic InterventionsIf more conservative treatment, such as changes to diet and exercise routines do not help relieve your symptoms, or if functional dyspepsia is having a significant impact on your daily activities and quality of life, a talking therapy or counseling can often be helpful. This is particularly true for those who experience high levels of stress, or who feel stress worsens their symptoms. Reducing the amount of tension you experience or learning tools to manage stress and anxiety can often reduce the severity and frequency of functional dyspepsia symptoms and improve
TREATMENT

9
10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
your overall quality of life. It can also be helpful to talk to someone who understands how difficult such conditions can be, and to discuss the correlation functional dyspepsia may have to your mood, troubling thoughts, or negative feelings. There are a range of therapeutic treatment options available which your doctor may recommend and that can help alleviate stress or manage feelings of depression. The main therapeutic approaches available for functional dyspepsia are cognitive behavioural therapy, psychodynamic psychotherapy and hypnotherapy
cognitive behavioural therapy (cBt)
CbT is a psychotherapeutic approach based on cognitive and behavioural principles that aims to identify and understand negative thoughts, beliefs and patterns of behaviour. Once these emotions and patterns are recognized, you can then better understand and change them based on a series of action oriented and problem solving strategies. Many studies show that if you can train yourself to react differently to stress, anxiety and depression (i.e. to think more positively or incorporate relaxation techniques), your physical symptoms of pain and discomfort can be alleviated. Thus, the task in CbT is to break the chain in terms of how you may be responding to anxiety.
psychodynamic psychotherapy
psychodynamic psychotherapy is a more explorative therapy, which focuses on gaining an understanding of unconscious processes that lie behind current presentations. These processes often relate to the past and so the objective is to gain insight into how our past affects and influences our current feelings and behaviour. psychodynamic psychotherapists can help you to explore your feelings of stress and discomfort around functional dyspepsia, how this might relate to other parts of your life, and how you might go about addressing these in a psychologically healthy way. psychodynamic psychotherapy, therefore, involves bringing less conscious psychological dynamics into awareness, finding words to describe such feelings, and working through them in a safe and confidential setting.
Hypnotherapy
hypnotherapy has been shown to help some people with functional disorders reduce their symptoms of pain and discomfort. hypnosis is used to change your unconscious mind’s attitude towards your symptoms. you can have hypnotherapy as an outpatient, or you can learn self-hypnosis techniques to practice at home.
Medication
If other more conservative treatments do not have an effect on your functional dyspepsia, medication can sometimes be prescribed to reduce the severity of symptoms. For further more specialised medications consult your gastroenterologist.
acid-suppressing medications
There are a range of over-the-counter medications from your pharmacist that may help reduce the amount of acid in the stomach. If your stomach is sensitive to acid, these antacid medications may reduce dyspeptic symptoms, such as bloating or upper abdominal discomfort. Acid-suppressing medications are not a long-term solution however, and should only be used as needed and in the short-term.
prescription-only medications
If other means of controlling symptoms do not work, your Gp or gastroenterologist may try another type of prescription medication, such as a prokinetic drug, to address your symptoms.
anti-depressant medications
If you are experiencing high levels of stress and/or depression, your doctor may recommend an antidepressant medication in addition to diet and exercise, or in conjunction with psychotherapy treatment. These medications can help with symptoms of depression and via the brain-gut axis can inhibit the activity of neurons that control the intestines. Sometimes antidepressant medications are prescribed at a very low dose in the absence of depression as these have been shown to reduce the pain signals that eminate from the gut in functional bowel disorders.

1 0
10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
COMplICATIONS
While functional dyspepsia is not linked to any life-threatening condition or illness, there can often be an impact on day-to-day activities and quality of life. For some people, the difficulties of coping with the symptoms of functional dyspepsia (ie frequently belching or experiencing discomfort in the abdomen) may limit their ability or desire to make plans, maintain social commitments and recreational activities. The pain and discomfort of functional dyspepsia, combined with the effect it can have on one’s social, work, or personal activities can be very taxing. Over time, this may lead to feelings of discouragement, stress, depression, and anxiety.
If you are experiencing any of these symptoms, or if you feel functional dyspepsia is limiting your activities or negatively affecting your quality of life, it is recommended that you visit your Gp, who will be able to help identify an appropriate and effective treatment for you.

1 1
10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
SUppORT AND FURThER RESOURCESliving with functional dyspepsia can be uncomfortable and challenging and it can be difficult to know where to turn for help. While your first point of contact should always be your Gp or gastroenterologist, educational and community resources may help you to cope more effectively with functional dyspepsia and improve your quality of life.
The Core Charity (www.corecharity.org.uk) is such a non-profit organisation that raises awareness and funds research on gut and liver disease, promotes education on gut function, and provides contacts for patient organisations and support groups.

10168 Functional Dyspepsia Patient • 297x210mm • CMYK • 29.01.14 • JA
bupa health insurance is provided by bupa Insurance limited. Registered in England and Wales No. 3956433 bupa Insurance limited is authorised by the prudential Regulation Authority and regulated by the Financial Conduct Authority and the prudential Regulation Authority. Arranged and administered by bupa Insurance Services limited, which is authorised and regulated by the Financial Conduct Authority. Registered in England and Wales No. 3829851.
Registered office: bupa house, 15-19 bloomsbury Way, london WC1A 2bA.
© bupa 2014
bupa.co.uk
Care homesCash plansDental insuranceDental serviceshealth assessmentshealth at work serviceshealth coachinghealth informationhealth insurancehome healthcareInternational health insuranceTravel insurance
XX/XXXX/XXX13 09659_XXXX