ESSENTIALS OF PHARMACOKINETICS AND DRUG … · Neofax 2010 Increased volume of distribution means...
Transcript of ESSENTIALS OF PHARMACOKINETICS AND DRUG … · Neofax 2010 Increased volume of distribution means...

ESSENTIALS OF
PHARMACOKINETICS AND
DRUG ADMINISTRATION IN PICU
Dre Caroline Fonzo-Christe
Pharmacist, HUG Geneva
CAS DE
PHARMACIE CLINIQUE
Mercredi 25 juin 2014

2
“what the body does to a drug” Pharmacokinetics
-> profile of drug concentration over time
1. Absorption
2. Distribution
3. Metabolism
4. Excretion
Drug administration“what YOU do to a drug”
The right dose for
the right effect
How not to loose
the drug before
reaching the patient

3
YOUR DAILY LIFE IN PICU
From the smallest to the biggest one…
Critically ill children….
High risk IV drugs…

VARIABILITY
4
Adapted from : Tomlin S, EAHP 2014
Survival
phase
Adaptation
Growth,
proliferation
Differentiation
Puberty
Sexual
maturation
<500 g >100kg
Respiratory
distress
syndrome
Necrotising
enterocolitis
Patent ductus
arteriosus
Neonatal asphyxia
Neonatal sepsis
Metabolic disease
Meningitis
Bronchiolitis
Cardiac surgery
Trauma
Near-drowning
Peritonitis
Intoxication
Asthma
Anorexia
nervosa

MEDICATION PROCESS
http://www.ismp.org
5
Non electronic

WHAT INFLUENCE DRUG EFFECT?
6
IV
High concentrations
Drug incompatibilities
In-line filters, infusion
material
Low flow, dead space
Drug effect
Exposition
Receptors
A
D
M
E
Ontogenesis
Pharmaco-
genetics
Environment
Nutritional state
Critically ill
ECMO, CRRT
Drug interactions
Co-morbidities
Drug preparation
and administration

SOME REFRESH ON PK PARAMETERS
7

2 MAIN PK PARAMETERS
Volume of distribution (Vd) Initial (loading) dose
to reach a Cpeak
Clearance Maintenance dose
to maintain a certain Css8
Adapted from Vaughan K,
Dell Children’s Medical Center of Central Texas

VOLUME OF DISTRIBUTION VD
Small Vd : drug mainly within systemic circulation Plasma volume (Vd 0.05 L/kg): large MW or high protein binding (ex. heparin, aspirin)
Extracellular water (Vd 0.2 L/kg): ex. penicillins, gentamicin, vancomycin
Total body water (Vd 0.6 L/kg): ex. paracetamol, indometacine, vancomycin
Large Vd (2-10 L/kg): drug distributed into peripheral
compartments (ex. morphine, hydromorphone, fentanyl)
Useful to determine intial dose
9
Starkey ES et al. Arch Dis Child Educ Pract Ed 2015;100:37-43
Cmax = dose Vd

CLEARANCE CL
CL tot = CL hepatic + CL renal
Hepatic clearance
10
Allorge D, Loriot A. Ann Biol Clin 2004;62:499-511
Starkey ES et al. Arch Dis Child Educ Pract Ed 2015;100:37-43
Phase 1: oxidation, demethylation
by enzymes (CYP450)
Phase II: conjugation
Phase III: excretion – elimination
(renal or biliary)
Drug transport proteines:
P-gP (P-glycoproteine)
MRP (Multidrug resistance protein)
hydrophilic
hydrophobic
Cell
protection
• Renal clearance: unchanged /metabolites
• Glomerular filtration: aminoglycosides, digoxin
• Proximal tubular secretion: penicillins, furosemide

PHARMACOKINETIC PARAMETERS
11
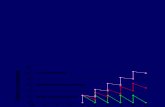
100%
50%
12.5%
25%
6.3 %
1 T1/2
3 %Time, hours
Co
nce
ntr
ation
, m
g/L
Cmax = Peak concentration
Minimal therapeutic concentration
Cmin = Trough concentration
AUC Therapeutic rangeArea under the curve
Cmax = dose
Vd
Vd: Volume of distribution
Elimination half-life T1/2 = ln2 x Vd
CL
T1/2: Time taken for plasma concentration to halve
CL Clearance
ln2 = 0.693

STEADY-STATE
Absorption or infusion rate balanced by
elimination rate Plasma concentration does not increase anymore
Time to reach steady-state: 4-5 T1/2
Time to be completely eliminated: 4-5 T1/2
12
Half-life : 12 hours
Starkey Es et al. Arch Dis Child Educ Pract Ed 2015;100:37-43
Intermittent dosing (x mg at each interval (ex. 12 h)
Css = steady-state concentration
Continuous infusion (mg/h)

3 PAPERS
13
Kearns GL et al. N Engl J Med 2003;349:1157-67

MORE PAPERS
14
https://www.sciencedirect.com/science/article/pii/B9780323401395000334
Anderson BJ. Anaesthesia & Intensive Care Medicine 2017,18:68-74

ONTOGENESIS AND PK
15
Samardzic J et al. Int J Pharmaceutics 2015;492:335–337
renal
CLhepatic
CL
Bioavailability Vd

DISTRIBUTION16
1. Absorption
2. Distribution3. Metabolism
4. Excretion

BODY WATER
17
Anderson BJ. Anaesthesia & Intensive Care Medicine 2017,18:68-74
Fat: 0.7% 12%

BODY COMPOSITION
80% water
12% fat
60% water
20% fat
Neonates
• larger Vd for hydrophilic
drugs (aminoglycosides)
-> risk of underdosing
• lower Vd for fat-soluble drugs
(fentanyl, midazolam)
-> risk of toxicity
Kearns GL et al. N Engl J Med 2003;349:1157-67
18
Vd

VD IN NEONATES
Gentamicin dose has to be increased (in mg/kg) to
reach the same plasma concentration
19
Kearns GL et al. N Engl J Med 2003;349:1157-67
Neofax 2010
Increased volume of distribution means increase the dose (initial
dose in mg/kg), to " fill up all the spaces " and reach target
concentrations
Vd
Cmax = dose
Vd

HEPATIC METABOLISM20
1. Absorption
2. Distribution
3. Metabolism4. Excretion

METABOLIC CAPACITY
AND DEVELOPMENT
21
de Wildt SN, et al. Arch Dis Child 2014
Choonara I, et al. Arch Dis Child 2014;99:1143–1146
Neonates
• Reduced hepatic clearance
-> risk of toxicity
Child
• Increased hepatic clearance
for some drugs
-> risk of underdosing
Hepatic
ClearanceBIRTH

IMPACT ON HALF-LIFE
midazolam
CYP3A4
ibuprofen
CYP2C9,
2C19
indomethacin
CYP2C9
caffeine
CYP1A2
morphine
UGT2B7
paracetamol
UGT1A6,1A9
T1/2 NN 6-12h PNA 3j: 43h
PNA 5j: 27h
PNA<2sem:
20h
PNA>2sem:
11h
NN: 72-96h Premature:
10-20h
NN: 8h
NN: 2-5h
Sulphation
T1/2 child 1-1.5h 1-2h - 5h (at 9
months)
1-2h
Sulphation
T1/2 adult 1.5-3.5h 2-4h - 3-5h 2-4h 1-3h
Glucuro-
conjugation
22
PNA: post natal age
NN: neonate Reduced hepatic clearance and longer half-life in NN
Increased hepatic clearance in childhood
Metabolic clearance of drugs matures at different rates, depending on the
drug metabolism pathways involved.

RENAL EXCRETION23
1. Absorption
2. Distribution
3. Metabolism
4. Excretion

RENAL FUNCTION
Kearns GL et al. N Engl J Med 2003;349:1157-67
Proximal
tubular
secretion
Adult values (100 – 120 ml/min)
at about 1 year24
Reduced renal clearance in
the first year of age for:
• Drugs with high renal
excretion (aminoglycosides,
penicillines, furosemide)
• Active metabolites
(morphine-6-glucuronide,
1-OH-midazolam et 1-OH-
midazolam-glucuronide)
Renal
Clearance

CLEARANCE IN NEONATES
A decreased clearance requires a longer dosing interval
to maintain trough concentrations low (to limit toxicity)
for gentamicin
25
Kearns GL et al. N Engl J Med 2003;349:1157-67
Neofax 2010
Decreased clearance means longer half-life and higher plasma
concentrations. Need to increase dosing interval !
Cl

26
OPIOIDS T1/2 , Vd, onset Metabolism Particularities
Fentanyl
The shortest onset of
action and the most
potent
The most lipophilic
Adult: 2–4h
Child: 11-36h (long-term
infusion)
0-14y: 5-30 L/kg
Adult: 4-6 L/kg
Onset of action IV: < 1 min
CYP3A4 -> inactive
metabolites
No active metabolite
Highly lipophilic (fat,
muscle) -> T1/2
prolongation with
infusion duration
Thorax rigidity (-> IV
over 3-5 min)
Morphine
Active metabolite
Adult: 2-4h
Premature: 10–20h
NN: 8h
Child: 1–2h
Adult: 1-6 L/kg
Onset of action: IV 5-10
min, PO: 30 min
No CYP but
glucuronidation
Active metabolite (6-Mô-
glucuronide) -> risk of
accumulation in renal
insufficiency
Hydromorphone
5-10x more potent than
Morphine
Adult: 2–4h
Adult: 4 L/kg
Onset of action IV: 5min,
PO: 15-30 min
No CYP but
glucuronidation
No active metabolite
Methadone
Very long T1/2
CAVE QT
Risk of IA
Adult: 35h (8-60h)
Child: 20h (3-62h)
Adult: 1–8 L/kg
NN: 2.5 L/kg
Onset of action IV: 15-20
min, PO: 30–60 min
CYP2D6, 3A4… No active metabolite
Risk of IA and QT
prolongation and
accumulation in hepatic
impairment

27
Alpha2 agonists T1/2 Metabolism Particularities
Dexmedetomidine
Affinity α2 1600:1
Adult: 3h
Premature: 7h
NN: 3h
Child: 1.5h
NN: 2 - 6 L/kg
Onset of action IV: 15 min
Glucuronidation
and CYP2A6
No active metabolites
T1/2 increase in hepatic
impairment
Bradycardia
Clonidine
Affinity α2 200:1
Adult: 12 -16h
NN: 40 – 70h
Child: 8 – 12h
Adult: 3 L/kg
Onset of action PO: 30-60 min
No CYP but
glucuronidation
No active metabolites
T1/2 increase in renal
impairment (-> 40h)
Hypotension, rebound
effect
Benzodiazepines T1/2 Metabolism Particularities
Midazolam
Active metabolites
Risk of IA
Adult: 3h
Premature: 6–12h
Child: 1-1.5h
NN: 1 L/kg
Adult: 1–3 L/kg
Onset of action IV: 3-5 min, PO
10-20 min
CYP3A4 -> active
metabolites (1-OH-
midazolam)
Active metabolites ->
risk of accumulation in
renal/hepatic
impairment
Risk of IA
T1/2 increase hepatic
impairment
Lorazepam
No active
metabolites
Long T1/2
Adult: 12-16h
NN: 40h
Child: 6-17h
NN: 0.2-3 L/kg
Adult: 1 L/kg
Onset of action IV: 2-3 min
No CYP but
glucuronidation
No active metabolite

CRITICALLY ILL AND PHARMACOKINETIC
28

IMPACT ON DRUG PK
29
Roberts JA et al. Lancet Infect Dis 2014;14:498-509
Therapeutic failure Toxicity Therapeutic
failure or
Toxicity
Ex. ABs Ex. ABs
Ascites

IMPACT ON DRUG PK
30
Roberts JA et al. Lancet Infect Dis 2014;14:498-509
Udy AA et al. Clin Pharmacokinet 2010; 49:1-16
Sime FB et al. Curr Opin Pharmacol 2015;24:1-6
Therapeutic failure
Ex. ABs Ex. ABs
Ascites
Clinical implications for time-dependent (t>MIC) ABs
• More frequent dosing (shorter dosing interval)
• Increased total daily dose
• Continuous/extended infusions?
• TDM

ANTIBIOTICS CLASSIFICATION
31
= Concentration-dependentAminoglycosides
Metronidazole
= Concentration and time-
dependent (exposition –
dependent)Vancomycin*
Fluoroquinolones*
Macrolides
= Time-dependentCarbapenems
Cephalosporines
Penicillins
Vancomycin *
Minimum inhibitory concentration
Roberts JA et al. Lancet Infect Dis 2014;14:498-509
Jamal JA et al. Curr Opin Crit Care 2012; 18:460–471
Adapted from Huttner A. Séminaire MAS Genève 2015
* May differ depending on publication

IMPACT ON DRUG PK
32
Roberts JA et al. Lancet Infect Dis 2014;14:498-509
Therapeutic failure
Ex. ABs Ex. ABs
Ascites
Clinical implications for hydrophilic drugs ABs
-> Depending on protein binding and renal function
• Loading dose
• Supplementary dose if puncture? «peritoneal dialysis»
• TDM
Vanco
Mero
Teico

IMPACT ON DRUG PK
33
Roberts JA et al. Lancet Infect Dis 2014;14:498-509
Therapeutic
failure or
Toxicity
Ex. ABs

ECMO: IMPACT ON PK
34
Shekar K et al. J Crit Care 2012; 27: 741.e9–741.e18
Often ECMO and CRRT combined !

DRUG SEQUESTRATION
Key factors: drug stability, lipophilicity and protein binding
Dependent of
oxygenator and circuit type (silicone vs polypropylene hollow
fiber membrane, coated vs uncoated circuit) 35
Shekar K et al. Critical Care 2015;19:164
Shekar K et al. J Crit Care 2012; 27: 741.e9–741.e18
-90%
NS
Clinical implications
• For ABs, do TDM
• For analgesia, morphine first
choice (titration)

SEDATION/ANALGESIA
Lipophilic drugs: sequestration
Clonidine, ketamine: no data
Dexmedetomidine: adsorption to PVC?
36
Shekar K et al. Crit Care 2012; 16: R194
Wagner D et al. Perfusion. 2013 ;28:40-6
Lipophilic
Lipophilic
Hydrophilic
Clinical implications
• Titration and use of
sedation/analgesia scores
• Morphine first choice for
analgesia

DRUG INTERACTION
NICU
• Immature hepatic and renal clearance
• Difficult to predict, no data
• At risk patients (?) if: • Presence of drug inhibitors or inducers
• Nephrotoxic drugs (cumulative effect)
PICU
• Cardiac patients (Drugs and QT)
• Transplant (immunosuppressive
agents)
• Epilepsia, Tuberculosis
37
Clinical implications
• Be careful at the beginning and the
end of a treatment
• Need to monitor effect and/or TDM
• Stop of inhibitor -> Normal CYP
activity after 4 T1/2
• Stop of inducer -> Normal CYP
activity >2w after inducer has
disappeared from blood
Amiodarone Multiple CYPs
Fluconazole Multiple CYPs

QT-PROLONGATION AND DRUGS
Mechanism
Dose-dependent blockade of potassium ion channels (Ikr) prolonged cardiacrepolarisation may lead to TdP (torsades de pointe)
Drug related risk factors
Renal or hepatic failure
Drug interactions with hepaticmetabolism inhibition
Management
Use lowest effective dose
Monitoring of baseline values and at steady state (4 T1/2)
38
Beitland S et al. Acta Anaesthesiol Scand 2014; 58: 266–272
Trinkley KE et al. Curr Med Res Opin2013;29:1719-26

QT-PROLONGATION AND TDP
https://www.crediblemeds.org/
39

40
“what the body does to a drug” Pharmacokinetics
-> profile of drug concentration over time
1. Absorption
2. Distribution
3. Metabolism
4. Excretion
Drug administration“what YOU do to a drug”
The right dose for the
right effect
How not to loose the
drug before reaching
the patient

ISSUES WITH DRUG ADMINISTRATION
41
Sherwin CMT et al. Arch Dis Child 2014; 99:590-4

DRUG DISPENSING42

DISPENSING AND SYRINGE ACCURACY
43
Morecroft CW, et al. Arch Dis Child 2013;98:831–832
Right dose?

44
Arenas_Lopez S et al. Arch Dis Child 2017, doi: 10.1136/archdischild-2016-312492
De Giorgi I, 2007 http://pharmacie.hug-ge.ch/rd/posters/jfsph06_idg_precision_seringues.pdf
Take at least 25% of
the volume of a syringe
to limit variability

SEDATION / ANALGESIA
Pharmaceutical
compounding by
hospital pharmacists
45

DRUG INCOMPATIBILITIES46

DRUG PRECIPITATION
47
B.Braun, KIK 2.1 2002 and Drug incompatibility 2011 www.safeinfusiontherapy.com
HUG
caspofungine + heparin

EMULSION CRACKING
Albumin 20% and 3-in-1 parenteral nutrition
Oiling out
Bouchoud L et al. JPEN J Parenter Enteral Nutr. 2013;37:416-24
48
+ 10min + 30minT0
Pharmacie HUG

TYPE OF REACTIONS
Physico - chemical
• Acid-base reactions (pH)
• Solubility
• Emulsion cracking
• Oxydo-reduction
• …
Consequences
• Precipitates (visible)
• Colour change (visible)
• Gaz production (visible)
• pH change (invisible)
• concentration (invisible)
• Catheter occlusion
• Renal and pulmonary embolism
• Reduction of therapeutic effect
• Toxic effects (peroxides)
patient
49

50
ACIDS AND BASES
From: KIK 2.1,
BBraun, 2002
Acid drug molecule basic drug solution
Basic drug molecule acidic drug solution
Don’t mix or infuse
on Y-site
acidic with basic
drug solutions!
Molecule Drug
solution
Molecule Drug
solution
Furosemide (acid) pH 9 Furosemide (acid) pH 9
Vancomycin (base) pH 3 Midazolam (base) pH 4
From: KIK 2.1, BBraun, 2002

51
SOLVENT (DILUENT)
Furosemide in Glucose 5% From: KIK 2.1, BBraun, 2002
Glucose 5% - 20% pH = 3.5 - 6.5 amiodarone, amphotericine B
noradrenaline, nitroprussiate
NaCl 0.9% pH = 5.0 - 7.0 erythromycine, furosemide, phenytoin
Solvent pH Appropriate for

CLINICAL INCIDENTS
Knowles JB et al. JPEN 1989;13:209-13
Hill SE et al. JPEN 1996;20:81-87
McNearney T et al. Dig Dis Sci 2003;48:1352-4

RECENT DATA: DRUG - DRUG
Kalikstad B et al. Arch Dis Child 2010;95:745-748
Zhao B et al. Am J Health-Syst Pharm 2014;71:901-902
Lack of DATA
in NICU
Case-reports of
catheter occlusion
53

CONCLUSION AND KEY MESSAGES
54

KEY MESSAGES
1. Increased Vd means increase the initial dose to “fill up all spaces”
2. Decreased CL means increase dosing interval
3. Critically ill patients:
Hyperdynamic states -> Increased CL means increase frequency for AB’s that need t>MIC
Ascites -> loss of hydrophilic drugs, do TDM and consider dose adaptation for “peritoneal dialysis” if puncture
ECMO -> variable effects, increase the initial dose and do TDM for antibiotics and titration for sedation/analgesia
4. Ask the pharmacist for drug compatibilities, dispensing issues and drug compounding
55

KEY HOME MESSAGE
FROM THE PHARMACIST
56
Prescribing the right dose is not
sufficient…
Don’t forget to ask yourself
where is the drug and
how much drug has been given !

57