E learning mycobacteria 15.pdf
-
Upload
anonymous-91vyyeka3i -
Category
Documents
-
view
220 -
download
0
Transcript of E learning mycobacteria 15.pdf
-
7/26/2019 E learning mycobacteria 15.pdf
1/49
Mycobacteria
-
7/26/2019 E learning mycobacteria 15.pdf
2/49
Introduction
Order: Actinomycetales
Family: Mycobacteriaceae
Genus: Mycobacterium
> 100 species
-
7/26/2019 E learning mycobacteria 15.pdf
3/49
-
7/26/2019 E learning mycobacteria 15.pdf
4/49
Classification
1. Mycobacteriumtuberculosis
complex(MTBC)
M.tuberculosis
M.bovis
M.africanum
M.pinnnipedii
M.microti
M.caprae
M.canettii
2. Mycobacterium le3. Atypical mycobact
M.avium avium
M.avium intracel
M. kansasiiM. fortuitum
M. chelonae
M.abscessus
-
7/26/2019 E learning mycobacteria 15.pdf
5/49
-
7/26/2019 E learning mycobacteria 15.pdf
6/49
General characteristics
Cell wall rich in lipids(mycolic acids)- comprise 60% owall weight
Slow growers: > 7 days to form colonies
Acid-fast: do not decolourise in acid and alcohol
-
7/26/2019 E learning mycobacteria 15.pdf
7/49
Virulence factors
Virulence attributed to ability to survive within macr
-
7/26/2019 E learning mycobacteria 15.pdf
8/49
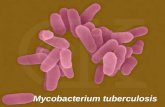
Mycobacteriumtuberculosis
-
7/26/2019 E learning mycobacteria 15.pdf
9/49
Epidemiology
In 2013, 9M infected, 1.5M deaths- 360,000 HIV-pos Leading killer of HIV-positive individuals- of all HIV
deaths
480,000 developed MDR-TB
2 billion latently Mtb-infected(LTBI) reservoirs The 2015 MDG of halting and reversing TB incidence
been achieved
Kenya among 22 high burden countries
-
7/26/2019 E learning mycobacteria 15.pdf
10/49
Modes of transmission
Droplet infection Person to person by inhalation aerosols
Mycobacterium tuberculosis (Pulmonary tuberculosis
Ingestion of milk
Infected cattle
Mycobacterium bovis (Intestinal tuberculosis)
Contamination of abrasions
Laboratory workers (Skin infection)
-
7/26/2019 E learning mycobacteria 15.pdf
11/49
Pathogenesis
Penetrate the alveoli Phagocytosis by resident alveolar macrophages & de
cells
Prevent fusion of the phagosome with lysosomes
Alveolar macrophages produce cytokines and chem Circulating macrophages and lymphocytes are attra
infectious focus
-
7/26/2019 E learning mycobacteria 15.pdf
12/49
Pathogenesis
Macrophages may fuse to form multinucleated giancells(MGCs=Langhans cells)
May also differentiate to form lipid-rich foamy macr
Results in granuloma formation
Infected macrophages can also spread to local lymphblood
Subsequent spread to other tissues, BM, spleen, kid
-
7/26/2019 E learning mycobacteria 15.pdf
13/49
-
7/26/2019 E learning mycobacteria 15.pdf
14/49
-
7/26/2019 E learning mycobacteria 15.pdf
15/49
Pathogenesis
1. Primary infection 10% of immune competent individuals
Bacilli grow unimpeded in host macrophages
2. Latent infection
90% of immune competent individuals
Controlled bacillary growth
Bacilli either killed or survive within cellular granua non-replicating state
Can persist for decades
-
7/26/2019 E learning mycobacteria 15.pdf
16/49
Pathogenesis
3. Post-primary infection May develop directly from a primary lesion= progres
primary tuberculosis
OR
Endogenous reactivation of latent infectionOR
Infection or exogenous reinfection
-
7/26/2019 E learning mycobacteria 15.pdf
17/49
Pathogenesis
Post-primary lesions often develop in the upper regi Immune-mediated control of bacillary growth fails
Tuberculoma formation- granuloma formation but wtissue destruction and caseation
Liquefication of caseous material Erosion into a bronchus
-
7/26/2019 E learning mycobacteria 15.pdf
18/49
Pathogenesis
Cavity is formed= characteristic feature of post-primpulmonary TB
*Granuloma formation= central event in the immunresponse against M.tb
Spread of bacilli from cavities
Though bronchus- other areas of the lung, trache
Swallowed-intestinal tract, anal fistulas
Through bloodstream to other organs
-
7/26/2019 E learning mycobacteria 15.pdf
19/49
Factors affecting susceptibility to
Age Immune status
Medical conditions
Genetic factors e.g. HLA-DR allele
Environmental factors- exposure to populations ofenvironmental mycobacteria
Mycobacterial factors- strain variation in virulence
-
7/26/2019 E learning mycobacteria 15.pdf
20/49
Clinical manifestations
Weight loss 10% PTB
Low grade fever, malaise, night sweats, chest paincough(>2 weeks), haemoptysis
EPTB
Depends on the site: skeletal, genital tract, urinarCNS, GIT, adrenal, cardiac
-
7/26/2019 E learning mycobacteria 15.pdf
21/49
Laboratory diagnosis
Specimen:sputum, gastric washings, urine, aspiratespathological material, etc
Staining of specimen using
Ziehl Neelsen (ZN) stainacid-fast bacilli (AFBs)-bacilli on a blue or green background
Kinyoun staining
Fluorescence stains -auramine O or rhodamine stfluorescent microscopy
-
7/26/2019 E learning mycobacteria 15.pdf
22/49
-
7/26/2019 E learning mycobacteria 15.pdf
23/49
-
7/26/2019 E learning mycobacteria 15.pdf
24/49
Laboratory diagnosis
Culture Gold standard in TB diagnosis Require incubation for 6 8 weeks before declari
negative
Solid culture (Lowenstein Jensen(LJ), Middlebroo& 7H11
Liquid culture -Middlebrook 7H12, Bactec, MGITmycobacterial growth indicator tube
-
7/26/2019 E learning mycobacteria 15.pdf
25/49
Laboratory diagnosis
To confirm M.tuberculosis from culture: Slow growth
Colonial morphology
Nitrate reductase test positive
Niacin test positive
-
7/26/2019 E learning mycobacteria 15.pdf
26/49
-
7/26/2019 E learning mycobacteria 15.pdf
27/49
-
7/26/2019 E learning mycobacteria 15.pdf
28/49
Laboratory diagnosis
Molecular techniques
PCR from culture; some direct from sputum
Immunological tests
Tuberculin skin test does not distinguish betweevaccination and disease. Usually negative in patie
advanced AIDS QuantiFERON , T-SPOT TB Detect interferon . F
& latent TB
-
7/26/2019 E learning mycobacteria 15.pdf
29/49
Tuberculin skin test
-
7/26/2019 E learning mycobacteria 15.pdf
30/49
reatment
1
st
line: isoniazid,
rifampicin/ rifabutin,
ethambutol,
pyrazinamide, streptomycin
2nd line:
para-amino salicy
cycloserine,
fluoroquinolone(ofloxacin/ ciprof
levofloxacin/ etc) amikacin,
kanamycin,
capreomycin,
ethionamide
-
7/26/2019 E learning mycobacteria 15.pdf
31/49
Drug resistance
Multidrug resistant TB (MDR TB):
resistant to at least rifampicin & isoniazid
Extensively drug resistant TB (XDR TB):
MDR strains that are also resistant to a fluoroquiand at least one second-line injectable agent (amkanamycin or capreomycin)
-
7/26/2019 E learning mycobacteria 15.pdf
32/49
ontrol
Prompt detection of cases & effective Rx
Isolation of cases on Rx until non-infectious
Follow up contacts of cases
Reducing overcrowding
Vaccination with BCGvariable results contraindicated in patients with AIDS
-
7/26/2019 E learning mycobacteria 15.pdf
33/49
Mycobacteriumleprae
-
7/26/2019 E learning mycobacteria 15.pdf
34/49
Introduction
Obligate intracellular organism- can grow in the moor in the armadillo
=Hansens bacilli
Reservoir- infected humans, low infectivity
Transmission- skin to skin contact, respiratory route
Incubation: 3 5 years, can be as long as 30 years
Bacilli resemble tuberculous bacilli but are not so stracid fast
-
7/26/2019 E learning mycobacteria 15.pdf
35/49
Pathogenesis
Principal target is the schwann cell
Resulting nerve damage is responsible for the anaesand muscle paralysis
Repeated injuries lead to gradual destruction of ext
Infiltration of skin and cutaneous nerves leads to forof visible lesions with pigmentary changes
-
7/26/2019 E learning mycobacteria 15.pdf
36/49
Clinical manifestations
Depends on patients immune reaction
Ranges from tuberculoid to lepromatous form
1. Tuberculoid leprosy(Paucibacillary)
Strong cellular immune reaction but a weak humoral res
Infected tissues- mainly lymphocytes and granulomas, re
few bacilli
2. Lepromatous leprosy(multibacillary)
Strong antibody response but a specific defect in the maand Schwann cells
-
7/26/2019 E learning mycobacteria 15.pdf
37/49
Clinical manifestations
1. Intermediate forms
Borderline tuberculoid(BT)
Mid-borderline(BB)
Borderline lepromatous(BL)
-
7/26/2019 E learning mycobacteria 15.pdf
38/49
Tuberculoid leprosy
http://upload.wikimedia.org/wikipedia/commons/e/e2/Leprosy_thigh_demarcated_cutaneous_lesions.jpghttp://upload.wikimedia.org/wikipedia/commons/e/e2/Leprosy_thigh_demarcated_cutaneous_lesions.jpg -
7/26/2019 E learning mycobacteria 15.pdf
39/49
Lepromatous leprosy
-
7/26/2019 E learning mycobacteria 15.pdf
40/49
Laboratory diagnosis
Does not grow in cell-free cultures therefore histopafindings
Detection of acid fast bacilli in nasal discharges, scrafrom the nasal mucosa
PCR
-
7/26/2019 E learning mycobacteria 15.pdf
41/49
Treatment, prevention and contr
Multidrug therapy
Dapsone
Rifampicin
Clofazimine
-
7/26/2019 E learning mycobacteria 15.pdf
42/49
Environmental mycobacteria
-
7/26/2019 E learning mycobacteria 15.pdf
43/49
Introduction
= Atypical, opportunistic, MOTTs(mycobacterial othetuberculous), NTM(non-tuberculous mycobacteria)
Saprophytes of soil and water
Cause opportunistic disease
Low virulence
Cause disease in profound immunosuppression
-
7/26/2019 E learning mycobacteria 15.pdf
44/49
-
7/26/2019 E learning mycobacteria 15.pdf
45/49
Clinical importance
Most prevalent= MAC
M.avium intracellulare
M.avium avium
Cause lymphadenitis and pulmonary lesions
Disseminated disease in profound immunosuppressi
M.ulcerans- causes Buruli ulcer
M.xenopi- pulmonary lesions in man
l l
-
7/26/2019 E learning mycobacteria 15.pdf
46/49
Clinical importance
M.chelonae; M.absessus; M.fortuitum; M.peregrinum
Responsible for post-injection abscesses and wouinfections including corneal ulcers
Opportunistic diseases caused b
-
7/26/2019 E learning mycobacteria 15.pdf
47/49
Opportunistic diseases caused b
MOTTs1. Localized lymphadenitis
2. Skin lesions following traumatic inoculation of bact
3. Tuberculosis-like pulmonary lesions
4. Tuberculosis-like non-pulmonary lesions
5. Disseminated disease
L b di i T
-
7/26/2019 E learning mycobacteria 15.pdf
48/49
Laboratory diagnosis, Treatment
Microscopy, culture
Resistant to many anti-TB drugs
Rifampicin + Ethambutol- 18-24 months
Macrolides
Fluoroquinolones
-
7/26/2019 E learning mycobacteria 15.pdf
49/49