Daniel Hirsch, MD Director Neonatology Somerset Medical...
Transcript of Daniel Hirsch, MD Director Neonatology Somerset Medical...
Daniel Hirsch, MDDirector of NeonatologySomerset Medical Center
Assistant Professor of PediatricsUMDNJ ‐
RWJMS
Daniel Hirsch, MDDirector of NeonatologySomerset Medical Center
Assistant Professor of PediatricsUMDNJ ‐
RWJMS
TodayToday’’s Talks TalkCase: Term newborn with vomiting &
abdominal distension
Normal stooling patterns
Pathophysiology of Hirschsprung’s Disease
Signs of Hirschsprung’s
Differential diagnosis
Diagnosis & management of Hirschsprung’s
Treatment of Hirschsprung’s
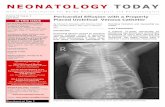
Neonate with vomiting & Neonate with vomiting & abdominal distensionabdominal distension
Mom 25 y.o., primigravidGood prenatal careNormal level II USGBS‐positiveROM 6 hrs (clear fluid)No feverNo meds givenNSVDApgar scores 8@1, 9@5
Neonate with vomiting & Neonate with vomiting & abdominal distensionabdominal distension
Normal phys exam @ 1 hrExclusively nursingPassed meconium @ 20 hrsAbd distension @ 30 hrsVomiting x 1, non‐biliousLethargicTemp 98.8˚ FResp rate 76Room air sat.s 98%
Neonate with vomiting & Neonate with vomiting & abdominal distensionabdominal distension
Initial management ?
Initial ManagementInitial ManagementCR monitor & pulse oximetryComplete physical examBPBedside glucosePlace naso‐ or oro‐gastric tube CBC w differential, lytes, ABG, blood cultureFlat plate of abdomen, consider additional view for intraperitoneal airImmediate consultation with Pediatric surgeonAmpicillin & gentamicin and IV fluids
Normal Stooling PatternsNormal Stooling Patterns95‐99% healthy term newborns pass meconium by 24 hrs100% pass meconium by 48 hrs
Hirschsprung’s Disease: 5% pass meconium by 24 hrs40‐50% pass meconium by 48 hrs
StoolingStoolingPatent GI tract
GI smooth muscle
Peptide Hormones
GI hormones
Enteric nervous system
Nerve fibers
Neurotransmitters & receptors
Anal sphincters (internal & external)
Enteric Nervous SystemEnteric Nervous SystemMost complex part of peripheral nervous systemDerived from neural crest cells
Enteric Nervous SystemEnteric Nervous System
Innervation of GI tract normally complete by
7 ‐
8 weeks gestation
Neural crest cells must then proliferate,
differentiate & migrate ⇒ enteric nervous system
‘Mature’ innervated GI tract by 14 weeks gestation
HirschsprungHirschsprung’’s Diseases Disease
Dr. Harald Hirschsprung
Two children with megacolon , 1887
Dr. Tittel noted absence of ganglion
cells in distal colon 1901
Pathophysiology of Pathophysiology of HirschsprungHirschsprung’’ss
Congenital absence of enteric ganglia (myenteric
& submucosal plexuses), “aganglionosis” in
variable segment of distal bowel
Abnormal peristalsis & motility in aganglionic
segment
Pathophysiology of Pathophysiology of HirschsprungHirschsprung’’ss
Intrinsic
malfunction of intestinal tract
** Intestinal obstruction **
HirschsprungHirschsprung’’s Diseases Disease
80% of cases‐ aganglionosis of rectosigmoid
region ‐ “short segment”
20% of cases‐ also involves colon and even small
intestine
Rare ‐ aganglionosis may be near‐total
Epidemiology of HirschsprungEpidemiology of Hirschsprung’’ssIncidence: 1 in 5000
Males > Females
Long segment: 2 : 1, autosomal dominant
Short segment: 4 : 1 , autosomal recessive
Genetically determined ?
Risk of recurrence in siblings 3‐4% (↑ 200 times)
Other anomalies in 5‐35% of cases
Sporadic cases: 80%
Why does HirschsprungWhy does Hirschsprung’’s occur ?s occur ?
Two theories
1. Neural crest cells differentiate prematurely
2.
Neural crest cells reach their destination but
fail to survive
Signs of HirschsprungSigns of Hirschsprung’’s Dzs DzIn FT newborn:
Failure to pass meconium in first‐24hrsAbdominal distensionVomiting (+/‐ bilious)Poor feedingLethargyIrritabilityDiarrheaFever
Differential DiagnosisDifferential Diagnosis
Intestinal malrotation **
Necrotizing enterocolitis **
Sepsis (non‐GI etiology)
Differential DiagnosisDifferential DiagnosisLeft microcolon
Meconium plug
syndrome
Meconium ileus
+/‐
cystic fibrosis
Intestinal atresia
Enterocolitis
Anal atresia
Abdominal mass
Hypokalemia
Hypermagnesemia
Hypothyroidism
Maternal opiates
Diagnosis & ManagementDiagnosis & Management** Timely & expeditious **
Serial & thorough assessments **
Vitals
Accurate I & O’s
NPO & IV fluids (** may need extra fluids **)
Gavage tube +/‐ decompression
Plain film of abdomen
Consider additional view(s) ‐ intraperitoneal air
Diagnosis & ManagementDiagnosis & ManagementPediatric surgical consultation **
CBC with manual diff, blood culture, electrolyte
panel, LFTs
Urine culture? CSF evaluation & culture?
Contrast enema
Rectal (suction) biopsy – definitive
Genetic consultation if other anomalies present
*Rectal Biopsy **Rectal Biopsy *Size of specimen:
diameter= 2‐3 mm
Depth= 1 mm
Absence of ganglion cells (myenteric & submucosal plexuses)
** Ideal specimen not always obtained
Ancillary criteria may be used:
Large submucosal fibers
Acetycholinesterase staining
TreatmentTreatmentResection of aganglionic segment
Specific procedure dependent upon length of
aganglionic segment
Short segment (rectosigmoid):
Soave endorectal pull‐through
‘Longer’ segment (proximal to rectosigmoid)
Transabdominal & perineal procedure
+/‐ colostomy above aganglionic segment
TreatmentTreatment
Intestinal transplantation ?
Enteric nervous system (ENS) stem cell
transplantation ?
WrapWrap‐‐UpUp
Differential diagnosis
*Consider potential life‐threatening diagnoses*
Serial & thorough assessments
Prompt pediatric surgical consultation
Diagnosis depends on biopsy: no ganglia in
myenteric & submucosal plexuses
↑ risk in subsequent children (genetic?)