)cSX · TheXYfemaleinsport:L.J. Hipkin Gonadaldevelopment Until the fetus is approximately 46 days...
Transcript of )cSX · TheXYfemaleinsport:L.J. Hipkin Gonadaldevelopment Until the fetus is approximately 46 days...

Br J Sp Med 1992; 27(3)
The XY female in sport: the controversy continues
L. J. Hipkin MD FRCPathDepartment of Chemical Pathology, University of Liverpool, Liverpool, UK
The summer and winter Olympic Games have beenaccompanied by much press coverage of the controversyand confusion over sex tests for sportswomen. Much ofthis has centred on the eligibility of subjects withandrogen insensitivity to compete in women's events. Thepurpose of this paper is to review the process of sexdifferentiation and its abnormalities, highlighting thoseconditions in which biologically active testosterone issecreted which might confer an advantage in women'ssporting events.
Keywords: Sport, sex testing
The historical basis for the need for sex testing hasbeen reviewed by Professor Ferguson-Smith and DrFerris'. They pointed out that initially inspection thenmanual examination of the external genitalia werecarried out but these were replaced by sex chromatintesting by the buccal smear method in 1968. Theauthors heavily criticized this method since theythought it unfairly excluded those with androgeninsensitivity or gonadal dysgenesis whom theybelieve account for the majority of XY females insport. One problem is that competitors who fail thesex chromatin test withdraw without a diagnosisbeing made so statistics about those without viriliza-tion who are unfairly excluded are difficult to obtain.It is even possible that the proportion of XY femaleswith virilization due to biologically active androgensecretion and a consequent advantage in competitivesport is greater than assumed2. There are severalconditions in which this occurs and in order for thenonspecialist to understand the pathogenesis, areview of normal sexual development and differentia-tion is helpful.
Normal sex developmentSexual differentiation is a complex process starting inthe early embryo and being completed with thedevelopment of secondary sex characteristics atpuberty. The early mammalian embryo has thepotential to become either male or female with aninherent trend towards the latter. However, if thechromosomal sex is male then testes develop, and the
Address for correspondence: Dr L. J. Hipkin, Endocrine Laboratory,UniversityDepartment ofChemical Pathology, RoyalLiverpoolUniversity Hospital, PrescotStreet, LiverpoolL78XP, UK
(© 1993Butterworth-Heinemann Ltd0306-3674/93/030150-07
hormonal secretions from these cause male differen-tiation of the internal and external genitalia. Theseprocesses will now be examined in more detail (forreviews see Bercovitz et al.3 or Batch et al.4).
ChromosomesIn the human there are 46 chromosomes consisting of22 pairs of autosomes and two sex chromosomesthese being XX in females and XY in males (Figure 1).In the female, part of one X is inactivated and stainsheterochromatically (Barr body) in nuclei from buccalscrapings (Figure 2). If more than 20% of these nucleicontain Barr bodies then it can be confidentlypredicted that at least two X chromosomes arepresent and the subject is chromatin positive.Chromatin negative subjects have a single X chromo-some.
_ )cSXI IA
G 7 9C
'.' .. , ............ ~ l
14 I5!
4 1-a
to I1s 1K
Eft
Figure 1. Normal male chromosome constitution (46,XY)
.~~~~~~~~~~~~~~~~~~~~~~~~....
!!M teatcl
Figure 2 !ijaNulu ih arbd (hoai ostv)ibuccalsmear from a nor~~~~~~~~maliffe."Amale
150 Br J Sp Med 1993; 27(3)
91.11l.k. SL I I % #
4e ."U
on July 6, 2020 by guest. Protected by copyright.
http://bjsm.bm
j.com/
Br J S
ports Med: first published as 10.1136/bjsm
.27.3.150 on 1 Septem
ber 1993. Dow
nloaded from

The XY female in sport: L. J. Hipkin
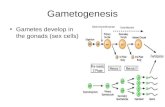
Gonadal developmentUntil the fetus is approximately 46 days old thegonads of males and females are indistinguishable.Thereafter it is thought that, in the male, a locus onthe Y chromosome (SRY gene) is responsible for theexpression of a male-specific cell membrane compo-nent called the H-Y antigen. This is disseminated bycells in the primitive gonad inducing its differentia-tion into a testis.The ovary does not develop from the undifferen-
tiated state until 3 months. Genes on both Xchromosomes and possibly on an autosome areresponsible, but whether there is a mechanismsimilar to the H-Y antigen in the male is uncertain.
Mechanism of testosterone synthesis and androgenaction
Before discussing male differentiation of the internaland external genitalia it is important to discusstestosterone synthesis and the mechanism of andro-gen action.
Testosterone is synthesized from cholesterol in aseries of enzymatic steps as depicted in Figure 3. Themost potent androgen in the majority of tissues is notin fact testosterone but another steroid calleddihydrotestosterone (DHT) which is formed fromtestosterone within androgen dependent cells by theaction of the enzyme 5ot-reductase (Figure 4).
Full biological expression of testosterone or DHTaction requires the presence of an intra-cytoplasmicandrogen receptor. Binding of the sex steroids to thereceptor initiates the chain of cellular events whichleads to the synthesis of androgen-induced proteins.Both sexes have the capacity to respond to androgenbut this is limited in females because of the relativelylow testosterone secretion.
Cholesterol
AS Pregnenolone'2Progesterone
3
17 a Hydroxyprogesterone
4 4
A4 Androstenedione Oestrone
Testosterone
OH
0
Testosterone
OH
5 a reductase
H
Dihydrotestosterone (DHT)
Figure 4. Conversion of testosterone to dihydrotesto-sterone by 5ix-reductase
Differentiation of the internal genitaliaThere are two sets of genital ducts in the 7-week-oldfetus, the Wolffian ducts and the Mullerian ducts.During the first 3 months of pregnancy, the testicularLeydig cells of a male fetus are stimulated bychrorionic gonadotrophin to produce testosterone.The high local levels of testosterone on each sidecauses the Wolffian duct (which lacks 5ox-reductase)to differentiate into the epididymis, vas deferens,seminal vesicles and ejaculatory duct. Anothertesticular secretion called Mullerian inhibitory subst-ance (MIS) or hormone causes the Mullerian systemto degenerate.
In the female fetus, on the other hand, lack oftestosterone leads to atrophy of the Wolffian systemand the absence of Mullerian inhibitory substanceallows maturation of these structures into thefallopian tubes, uterus and upper part of the vagina(Figure 5).
Differentiation of the external genitaliaIn the early embryo there is a common cloaca butfrom this a urogenital sinus develops which until theseventh fetal week is identical in both sexes. On eachside of the sinus there is an inner urethral and outerlabioscrotal fold, while anteriorly there is a genitaltubercle which is the anlage of the penis.
Testosterone No testosteroneand orMIS MIS
Oestradiol
Figure 3. Enzymes involved in the synthesis of testosteroneand oestradiol from cholesterol (1, cholesterol desmo-lase; 2, 33-hydroxysteroid dehydrogenase; 3, 17x-hydroxylase; 4, 17,20-desmolase; 5, 17p3-hydroxysteroiddehydrogenase; 6, aromatase)
Figure 5. Diagram showing internal genital development.In the male the testis produces testosterone and Mullerianinhibitory substance (MIS) which favours development ofthe Wolffian system. In the female these hormones areabsent and the Mullerian ducts develop
Br J Sp Med 1993; 27(3) 151
on July 6, 2020 by guest. Protected by copyright.
http://bjsm.bm
j.com/
Br J S
ports Med: first published as 10.1136/bjsm
.27.3.150 on 1 Septem
ber 1993. Dow
nloaded from

The XY female in sport: L. J. Hipkin
Differentiation of the external genitalia is com-pleted by 12-14 weeks. The tissues are rich in5x-reductase and unlike differentiation of the maleinternal genitalia, that of the external genitalia isstimulated by DHT. The steroid causes closure of theinner folds to form a urethra which extends along thephallus, while fusion of the outer folds forms thescrotum and ventral skin of the penis. DHTstimulates the prostate to develop as an outgrowth ofthe urogenital sinus.
In females the folds which bound the sinus becomethe labia minora and majora while a septum developswhich separates the urethral and vaginal openings.The vagina has a contribution from the Mullerianducts already referred to.Throughout gestation the penis lengthens while in
females the phallus remains rudimentary and be-comes the clitoris. Another difference between thesexes is that, after 28 weeks, the testes descend intothe scrotum under androgen action stimulated byboth pituitary and placental gonadotrophins.
Development of the secondary sex characteristics
Completion of sexual differentiation and develop-ment occurs at puberty. Although the mechanism forthe onset of puberty is poorly understood, a feature isthe pulsatile secretion of gonadotrophins from thepituitary, initially at night. This stimulates the gonadsof both sexes to produce sex steroids.
In males testosterone causes muscular develop-ment, deepening of the voice and inhibition of breastdevelopment. The steroid causes some scrotal ruga-tion and growth of the penis, the latter presumablybecause testosterone levels are much higher inrelation to DHT at puberty than during fetal life.Testosterone is also a requirement for normalspermatogenesis and it seems to play a part in malepsychosocial orientation at puberty but not beforewhen environmental factors predominate. In themale, DHT is responsible for facial and body hairdistribution as well as activating sebaceous glandswhich can lead to acne. Male pattern baldness is aDHT mediated event.Females going through puberty experience breast
development and redistribution of fat to give thefemale habitus. There is uterine and particularlyendometrial growth, the latter undergoing cyclicalshedding with the waxing and waning oestrogenlevels to give rise to the menses. Female body hairdevelops following adrenal androgen action.
Non-virilized XY femalesThere are two main subgroups of females with an XYchromosome constitution and who have no evidenceof androgen activity and consequently are notvirilized. They are pure XY gonadal dysgenesis5 andcomplete androgen insensitivity3 4. In the clinicaldomain patients usually present because they havenever menstruated. Some are discovered whensiblings of affected individuals are investigatedbecause of the familial nature of the genetic defects,and some because of the finding of gonads in thelabial folds.
Pure XY gonadal dysgenesisIn the complete form of pure XY gonadal dysgenesis,as well as amenorrhoea there is sexual infantilismwith eunuchoidism and lack of breast development.The external and internal genitalia are completelyfemale. The gonads do not develop and are repre-sented by streaks which are thought to be due tofailure of H-Y antigen production or action. There is,therefore, no production of sex steroids or MIS whichexplains the clinical findings. The plasma testo-sterone and oestradiol are low even for females andthe gonadotrophins are high through failure of theinhibitory feedback mechanism. Because the uterus,tubes and vagina are present, cyclical oestrogen-pro-gestogen therapy results in withdrawal bleeding fromthe endometrium.
Complete androgen insensitivitySubjects with complete androgen insensitivity, alsosometimes referred to as testicular feminization, havea feminine appearance (Figure 6). The externalgenitalia are female (Figure 7) but with a short blindending vagina, there is excellent breast developmentand delicate skin devoid of acne. However, the maincharacteristic is the absence or extreme sparsity of theaxillary and pubic hair.
..........' .. .....................
..
';',':.t ..:
S.............
S~~~~~~~~~~~~~~~~~.
Figure 6. Patient with complete androgen insensitivity,aged 19 years. From Simmer, H. H., Pion, R. J. andDignam, W. J., Testicular Feminization, 1965. Courtesy ofCharles C. Thomas, Springfield, Illinois, USA
152 Br J Sp Med 1993; 27(3)
on July 6, 2020 by guest. Protected by copyright.
http://bjsm.bm
j.com/
Br J S
ports Med: first published as 10.1136/bjsm
.27.3.150 on 1 Septem
ber 1993. Dow
nloaded from

The XY female in sport: L. J. Hipkin
~~~~~~~~~~~~......T
Figure 7. External genitalia of a patient with completeandrogen insensitivity, aged 48 years. From Simmer,H. H., Pion, R. J. and Dignam, W. J., Testicular Feminiza-tion, 1965. Courtesy of Charles C. Thomas, Publisher,Springfield, Illinois, USA
The internal genital structures are absent and thegonads, which may be in the pelvis, inguinal canal orlabia, are testes devoid of spermatogenesis.The gonadotrophins are elevated, luteinizing hor-
mone causing Leydig cell hyperplasia and conse-quent supranormal levels of plasma testosteroneeven for a male. Testicular secretion of oestradiol isincreased but elevation of this steroid is mainly fromperipheral conversion from testosterone. Hence thebreast development.The defect is, therefore, one of insensitivity of the
tissues to androgen. Studies of DHT uptake bycultured fibroblasts from genital skin have showndeficiency or qualitative abnormality of the androgenreceptor. A post-receptor defect is supposed in thefew in whom normal androgen receptors have beenfound. Androgen insensitivity accounts for the faileddevelopment of the Wolffian system but the Muller-ian ducts regress because of normal testicularproduction of the inhibitory hormone. Androgeninsensitivity enhances the oestrogen induced breastdevelopment.
Virilized XY femalesThere are several subgroups of females with an XYchromosome constitution or genotype who may havesome ambiguity of the external genitalia and whomay show some signs of virilization at puberty.Clinically it may be the effects of androgen activitywhich prompt referral rather than the amenorrhoea.These conditions have been reviewed by Savage6.
Partial androgen insensitivityInsensitivity to androgen encompasses a wide spec-trum of abnormalities from complete testicularfeminization already described to a normal malehabitus but with perineal hypospadias and gynaeco-mastia (Reifenstein's syndrome). At the female end ofthis spectrum there are variants of testicular feminiza-tion which are caused by partial or incompleteandrogen insensitivity. They are similar in every wayto those with the complete form of the disorderexcept at birth there may be some enlargement of theclitoris and slight labioscrotal fusion. At pubertythere is some breast development and normal growthof pubic and axillary hair. The derivatives of theWolffian system are hypoplastic.The androgen receptor abnormalities are similar to
those found in the complete form but some havenormal binding. The reason for androgen insensiti-vity in the latter is obscure.
Incomplete XY gonadal dysgenesisIn the incomplete form of pure gonadal dysgenesisthere may be some evidence of androgen activity infetal life in the form of sexual ambiguity but thisbecomes more apparent at puberty when citoro-megaly and facial hirsutes develop. The breasts donot develop.The internal genitalia may be of either sex but they
are rudimentary or hypoplastic. The gonads aredysgenetic testes which may be in streak form withislands of Leydig cells being found at the hilus. It issupposed that there is insufficient androgen fromthese cells to masculinize the fetus but the levelsbecome significant at puberty under the influence ofhigh levels of luteinizing hormone. The plasmatestosterone is thus above the normal female rangewhich differentiates the incomplete form from thecomplete in which testosterone levels are low.
Mixed or asymmetric gonadal dysgenesisAlthough a 45,XO/46,XY mosaic chromosome consti-tution (chromatin negative) is sometimes found inpure gonadal dysgenesis, this genotype is more oftenfound in mixed gonadal dysgenesis. The clinicalfeatures and hormone profile are similar to those inincomplete gonadal dysgenesis except individuals areshort and stocky, resembling Turner's syndromebecause of the 45,XO cell line.Gonadal development is asymmetric, classically a
rudimentary or normal testis with a vas is found onone side and a streak with a fallopian tube on theother. A small uterus and poorly developed vaginaare present. The internal genitalia appearances are,therefore, those anticipated from the morphology ofthe ipsilateral gonad.
Defects in testosterone biosynthesisAll the enzymes involved in testosterone biosyn-thesis may be completely or partially deficient. Indeficiency of cholesterol desmolase, 3,-hydroxy-steroid dehydrogenase or 17ot-hydroxylase, cortisol
Br J Sp Med 1993; 27(3) 153
on July 6, 2020 by guest. Protected by copyright.
http://bjsm.bm
j.com/
Br J S
ports Med: first published as 10.1136/bjsm
.27.3.150 on 1 Septem
ber 1993. Dow
nloaded from

The XY female in sport: L. J. Hipkin
synthesis is also impaired while lack of the first twoenzymes decreases mineralocorticoid production.These are, therefore, forms of congenital adrenalhyperplasia which, without recognition and approp-riate treatment at birth, cause death from lack ofcorticosteroids. With treatment some have survivedto adulthood and together with deficiency of theother two enzymes involved in testosterone synthesis(17,20-desmolase and 1713-hydroxysteroid dehydro-genase) present a fairly similar clinical picture.The external genitalia may vary from completely
female to ambiguous with a small hypospadic phallusand blind vaginal pouch. At puberty secondary sexcharacteristics may or may not develop but if they dothe combination of virilization (Figure 8) and breastdevelopment is often recorded.The Wolffian duct derivatives are absent, rudimen-
tary or normal but female internal genitalia are neverfound. The gonads are testes, devoid of spermato-genesis and with Leydig cell hyperplasia (Figure 9).They are located in the abdomen, inguinal canal orlabia.The spectrum of abnormalities depends on the
degree of enzyme deficiency, those in whom it iscomplete tending to have a female habitus with lowsteroid levels, while those with partial defectsundergo some virilization. The picture is furthercomplicated because precursors proximal to theenzyme block are produced excessively under stimu-lation from luteinizing hormone. These can beconverted to androgen and oestrogen in the peri-
Figure 8. Enlarged clitoris in a 19-year-old patient with17,-hydroxysteroid dehydrogenase deficiency
Figure 9. Section of testis from a 19-year-old patient with17p-hydroxysteroid dehydrogenase deficiency showingLeydig cell hyperplasia and no spermatogenesis
pheral tissues, thus accounting for virilization andbreast development at puberty.
Diagnosis is made after puberty by finding elevatedplasma steroid levels on the proximal side of theblock and low levels distally, e.g. a higher level ofandrostenedione and oestrone compared with testo-sterone and oestradiol is diagnostic of 17p-hydroxy-steroid dehydrogenase deficiency (Figure 3). Beforepuberty the steroid pathways have to be stimulatedwith gonadotrophin or adrenocorticotrophic hor-mone to unmask the block.
5x-Reductase deficiencyThe effects of 5(x-reductase deficiency are discussedby Imperato-McGinley et al.7 . At birth, affectedsubjects have incompletely masculinized externalgenitalia. There is a small hypospadic phallusresembling a clitoris, bifid scrotal folds, the sinusopens into the perineum and there is a blind vaginalpouch. Because of this phenotype rearing is in thefemale role.At puberty varying degrees of masculinization
occur. The phallus enlarges to form a small penis andthe testes enlarge and appear in the inguinal regionor in the scrotal folds which become pigmented andrugose. The voice deepens and muscular develop-ment is prominent. Normal female body hairdevelops but there is very little facial hair or acne.There is no breast development. The incidence of thedisorder is relatively high in the Dominican Republicand many of those brought up there as females, atpuberty adopt a male gender role.There are no female internal genital structures. The
male internal genitalia, except for the prostate whichis tiny, are normal and the vas opens into the vaginalpouch. Normal spermatogenesis occurs and seminalfluid can reveal a normal sperm count.
All these somatic changes are predictable from theknown effects of testosterone and DHT. Biochemi-cally after puberty the diagnosis of 5ac-reductasedeficiency is suggested by the finding of a hightestosterone:DHT ratio. The plasma testosteronelevel is normal or high for a male while plasma
154 Br J Sp Med 1993; 27(3)
on July 6, 2020 by guest. Protected by copyright.
http://bjsm.bm
j.com/
Br J S
ports Med: first published as 10.1136/bjsm
.27.3.150 on 1 Septem
ber 1993. Dow
nloaded from

oestradiol is normal. Prepubertally the enzymedeficiency has to be unmasked with studies pre- andpost-injection with chorionic gonadotrophin.
Confirmation of 5ot-reductase deficiency can bemade with enzyme studies on tissue or culturedfibroblasts from genital skin. The enzyme may bedeficient or abnormal.The reason for the masculinization of the external
genitalia at puberty is obscure but may reflect acombination of the high plasma testosterone8 andlow but detectable 5ax-reductase activity.
DiscussionThe purpose of sex verification testing is to ensurethat sportswomen compete on an equal basis9. Theproblem is that genetic testing, using either thetraditional sex chromatin pattern or the recentlyintroduced detection of the male determining geneon the Y chromosome, does not separate out onlythose who would have an unfair advantage incompetition'0. The purpose of this review is toexplain the differences between nonvirilized andvirilized XY females. The former would theoreticallycompete on equal terms but the latter would have anunfair advantage because the excessive endogenoustestosterone secretion is biologically active. Purely onthe basis of genetic tests both groups would bedisqualified.A second problem is that such disorders are
extremely rare in the population yet relatively muchmore frequent following testing of participants atvarious prestigious sports meetings2. Since there islittle follow-up information on diagnoses in thesecompetitors, it is impossible to decide whether thediscrepancy is due to excessive numbers of virilizedXY females, which is of concern to the MedicalCommission of the International Olympic Committee(IOC), or whether some other gene on the Ychromosome is conferring benefit. If the latter thenthe eligibility of non-virilized XY females may bequestioned.
In spite of criticism of genetic testing for sexdetermination in sport, the IOC continued to use thismethod in their recent winter and summer Games".Although using the modern techniques they statedthey were backing up questionable results with otherevidence to determine sex.The International Amateur Athletic Federation
(IAAF) on the other hand, bowed to pressure from anumber of quarters and announced that the buccalsmear test would be abandoned'2. Instead allmember federations were instructed to arrange fortheir male and female athletes to undergo a physicalexamination to ascertain their state of health andgender. The female athlete would then be issued witha gender certificate if not already on the IAAFfemininity list.
It follows from the account of the differencesbetween non-virilized and virilized XY females thatphysical examination, particularly searching for evi-dence of androgen activity is preferable to genetictesting. However, the latter had to be introduced andis still preferred by sportswomen because they found
The XY female in sport: L. J. Hipkin
inspection of the genital region demeaning and theyresented manual examination'. It is for this reasonthere is the lack of clinical data referred to; chromatinnegative sportswomen preferred to withdraw fromcompetition rather than be investigated.Not all sports medical officers agree with the IAAF
approach, although it seems no different than thepre-employment medical examination required inmany occupations. The British team doctor at theTokyo World Championships refused to carry outsuch examination, expressing confidence in hisability to assess the gender of team members withtheir clothes on! It is also rumoured that the IAAF isreconsidering whether to impose femininity testingand this has encouraged an Australian male-to-female transsexual to train for athletic competition.Needless to say this controversy and confusion
which has received much press and televisioncoverage must cause sportswomen to lack confidencein gender determination methods and to lose faith inthe medical profession. A statement that a sports-woman had to withdraw from competition because aroutine test showed she was a 'man' only for her to bereinstated 3 years later does not help'0.As pointed out many times the main problem is in
defining sex, and in particular assigning sex on thebasis of one characteristic. Based purely on genotypeit is true to say that the female chromosome sex is XXand male XY. However, it is the physical appearanceor phenotype which is the main determinant of thesex of rearing. Those with 5ot-reductase deficiencyregard themselves as female but some change to themale gender role at puberty when the externalgenitalia appearances change. Similarly there is aspectrum of androgen insensitivity states fromtesticular feminization through to Reifenstein's syn-drome and sex of rearing is selected according towhether the genitalia are masculine or feminine. It isfor this reason that throughout this review, thesubjects have been referred to as XY females.There is another aspect and that is psychosocial
sex. Transsexuals have the genotype and phenotypeof one sex but their sexual orientation is that of theopposite sex. Because of this difference betweenpsyche and soma, transsexuals seek gender reasign-ment surgery, again showing the importanceattached to phenotypic sex.
In clinical practice, XY females are never told theyare really men but that they have abnormal gonadswhich need to be removed because of the risk oftumour development. Testosterone can also beproduced excessively in XX females with suchconditions as congenital adrenal hyperplasia and thefar more common polycystic ovarian syndrome.These can also lead to virilization, so in some waysinspection of the genitalia is to assess androgen statusrather than to determine sex. Whether sportswomenwould accept this different interpretation for the needfor genital inspection is open to speculation. It is ofsome relevance that there have been no adversecomments about the need for doping control inde-pendent sampling officers to view the source of urineduring specimen collection.
If genetic testing unfairly disqualifies some femalecompetitors and if women object to phenotypic sex
Br J Sp Med 1993; 27(3) 155
on July 6, 2020 by guest. Protected by copyright.
http://bjsm.bm
j.com/
Br J S
ports Med: first published as 10.1136/bjsm
.27.3.150 on 1 Septem
ber 1993. Dow
nloaded from

The XY female in sport: L. J. Hipkin
being ascertained by genital inspection or examina-tion, is there any other approach? The InternationalSki Federation (FIS) carries out serum testosteroneestimations as part of their gender verificationprotocol (Dr Michael Turner, personal communica-tion). This has two advantages; unlike tests ofgenotype it does not exclude those with completegonadal dysgenesis, and it is a direct measure of asteroid that could be giving a female competitor anadvantage. It has the disadvantage that suppressivemedication could be employed to lower plasmatestosterone levels. However, random drug controlsampling would reveal this or, alternatively, long-term suppression of androgens would cause loss oftheir virilizing benefit. However, as with genetictests, assay of plasma testosterone would only be ascreen for those requiring physical examination.Whether sportswomen will develop a different
attitude to 'femininity' testing, with better educationand with the knowledge there is a general desire toprove eligibility rather than to find grounds fordisqualification, remains to be seen.
AcknowledgementsI would like to thank Mr P. J. Howard, Head of the CytogeneticsDepartment of the Royal Liverpool University Hospital, for Figure 1,and Dr R A. Fisken, Consultant Endocrinologist at FriarageHospital, Northallerton, for Figure 5.
References1 Ferguson-Smith MA, Ferris EA. Gender verification in sport:
the need for change? Br J Sports Med 1991; 25: 17-20.2 Hipkin Q. Gender verification in sport. Br J Sports Med 1991;
25: 171.3 Bercovitz GD, Brown TR, Migeon CJ. Androgen receptors.
Clin Endocrinol Metab 1983; 12: 155-73.4 Batch JA, Patterson MN, Hughes IA. Androgen insensitivity
syndrome. Reprod Rev Med 1992; 1: 131-50.5 Grumbach MM, Conte FE. Disorders of sex differentiation.
In: Williams RH, ed. Textbook of Endocrinology. 6th ed.Philadelphia, USA: WB Saunders, 1981; 423-514.
6 Savage MO. Ambiguous genitalia, small genitalia andundescended testes. Clin Endocrinol Metab 1982; 11: 127-58.
7 Imperato-McGinley J, Peterson RE, Gautier T, Sturla E. Malepseudohermaphroditism secondary to 5ot-reductase defici-ency - a model for the role of androgens in both thedevelopment of the male phenotype and the evolution of amale gender identity. J Steroid Biochem 1979; 11: 637-45.
8 Maes M, Sultan C, Zerhouni N, Rothwell SW, Migeon CJ.Role of testosterone binding to the androgen receptor in malesexual differentiation of patients with 5a-reductase defici-ency. J Steroid Biochem 1979; 11: 1385-90.
9 Hay E. Sex determination in putative female athletes. JAMA1972; 221: 998-9.
10 Editorial. Experts slam Olympic gene test. Science 1992; 255:1073.
11 Editorial. Olympic committee will do genetic tests on womenathletes. Br Med J 1992; 304: 306.
12 Editor's note. Br J Sports Med 1991; 25: 104.
BRITISH ASSOCIATION OF SPORT AND MEDICINE
Annual Congress 1993
19-21 November 1993
The 1993 BASM congress is to be held in The Garden House Hotel,Cambridge, and has an interesting line-up of activities. Some of the country'sleading experts have been invited to speak on such topics as HumanPhysiology, Exercise Cardiology, Immunology and Shoulder Surgery. Theguest speaker will be Mr R. Thome6e from the University of Goteborg.
Topics of discussion:
Exercise Physiology 1993 - A critical reviewExercise MedicineSport and the Mind, Sport and the BrainAdvances in Surgical Treatment of Sport-induced
Shoulder InjuriesAdvances in Physical Therapy
For further details please contact: Dr Colin Crosby, Chairman BASM EasternRegion, The Department of Exercise and Sport Medicine, The GardenHospital, Sunny Gardens Road, London NW4 1RX, UK. Tel: (0582) 841158
156 Br J Sp Med 1993; 27(3)
on July 6, 2020 by guest. Protected by copyright.
http://bjsm.bm
j.com/
Br J S
ports Med: first published as 10.1136/bjsm
.27.3.150 on 1 Septem
ber 1993. Dow
nloaded from