Cricohyoidoepiglottopexy in Laryngeal Trauma Report Cricohyoidoepiglottopexy in Laryngeal Trauma...
Transcript of Cricohyoidoepiglottopexy in Laryngeal Trauma Report Cricohyoidoepiglottopexy in Laryngeal Trauma...
Case Report
Cricohyoidoepiglottopexy in LaryngealTrauma
Otolaryngology–Head and Neck Surgery2016, Vol. 155(5) 886–887� American Academy ofOtolaryngology—Head and NeckSurgery Foundation 2016Reprints and permission:sagepub.com/journalsPermissions.navDOI: 10.1177/0194599816659059http://otojournal.org
Eduardo Ferreira, MD1, Carlos Nabuco Araujo, MD1,Sandra Agostinho, MD2, and Ana Rita Santos, MD1
No sponsorships or competing interests have been disclosed for this article.
Keywords
laryngeal trauma, cricohyoidoepiglottopexy
Received December 31, 2015; revised June 14, 2016; accepted June 21,
2016.
Laryngeal fractures occur in 1 in 30,000 trauma
patients admitted to dedicated trauma centers.1 Once
a laryngeal fracture is suspected or identified, the
primary goal is to secure the airway, followed by recon-
struction to conserve laryngopharyngeal function.1
Cricohyoidoepiglottopexy is a surgical approach typically
used in the management of glottic carcinoma. In this study, a
case of laryngeal trauma requiring a novel use of cricohyoi-
doepiglottopexy is reviewed. This article was approved by the
Ethics Committee of the Centro Academico de Medicina de
Lisboa (Hospital de Santa Maria, Hospital Pulido Valente,
Faculdade de Medicina de Lisboa e Instituto de Medicina
Molecular).
Case Report
A 33-year-old man survived a motorcycle accident that caused
a penetrating neck wound and a laryngeal fracture. He was
referred to our otorhinolaryngology department after 8 days in
the trauma hospital of an underdeveloped African country. The
patient had undergone a tracheotomy and an attempt to recon-
struct the larynx with sutures at the referring hospital.
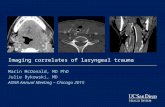
A computed tomography scan at admission showed a cer-
vicomediastinal abscess and a partial destruction of the thyr-
oid cartilage (Figure 1).
The patient was immediately scheduled for surgery, which
began by exploring the dehiscence a few centimeters above
the tracheotomy. This dehiscence was found to penetrate the
supraglottic area and the left piriform sinus, allowing an exter-
nal direct visualization of endolarynx and hypopharynx, which
were severely swollen (Figure 2). The epiglottis was found to
be displaced superiorly to the wound. Necrotic tissue was
excised and the abscess was drained. Friability of tissues and
the need to control infection prevented any attempt to recon-
struct the larynx at this time; thus, the surgical decision was
made to create a pharyngolaryngeal stoma and a gastrostomy
to allow the wound to granulate in by secondary intention.
Over the following weeks, the pharyngolaryngeal stoma’s
dimensions decreased and the hypopharyngeal defects appar-
ently remucosalized. However, at 6 months postoperatively,
the remaining supraglottic and glottic mucosa was still show-
ing significant edema, and granulation tissue was seen cover-
ing the remainder of thyroid cartilage in spite of local care,
antibiotics, steroids, and proton pump inhibitors.
At this stage, a decision was made to perform a supracri-
coid horizontal partial laryngectomy with cricohyoidoepiglotto-
pexy (SCPL-CHEP) to restore laryngopharyngeal function.
Surgery went ahead uneventfully, except for the intraoperative
finding of a mucosal defect on the left pyriform sinus caused
by the initial trauma, which was addressed by covering it with
local sliding flaps of adjacent hypopharyngeal mucosa.
1Otorhinolaryngology Department, Hospital de Santa Maria, Lisbon,
Portugal2Otorhinolaryngology Department, Hospital Divino Espırito Santo, Ponta
Delgada, Portugal
Corresponding Author:
Eduardo Ferreira, MD, Otorhinolaryngology Department, Hospital de Santa
Maria, Av. Professor Egas Moniz, 1649-035 Lisbon, Portugal.
Email: [email protected]
Figure 1. Computed tomography scan at admission showing a par-tial destruction of the thyroid cartilage.
at SOCIEDADE BRASILEIRA DE CIRUR on November 4, 2016oto.sagepub.comDownloaded from
On the third day after SCPL-CHEP, a left pharyngocer-
vical fistula was identified and successfully managed con-
servatively with daily changing of compressive dressings.
The tracheostomy cannula was removed on the 14th day
after the SCPL-CHEP procedure, and the patient was
immediately started on speech rehabilitation. After a nega-
tive methylene blue fistula test on the 30th postoperative
day, the patient began oral intake and the gastrostomy was
closed.
Eight months after SCPL-CHEP, he developed a puru-
lent discharge at the surgical cervical scar. The computed
tomography scan revealed it to be due to a late-appearing
fistula, which was managed by total resection under gen-
eral anesthesia. Twelve months after SCPL-CHEP, the sub-
ject presented a functional larynx with a socially effective
voice.
Discussion
As a rule, laryngeal reconstruction should be performed in
the first 24 to 48 hours after a traumatic fracture,2 and care
should be taken to prevent infection, tissue necrosis, and
denuded mucosal areas.3
SCPL-CHEP is usually indicated in anterior glottic carcino-
mas that spare at least 1 functional cricoarytenoid unit.4,5 In
this nononcologic subject, SCPL-CHEP proved, however, that
it could also be used to achieve laryngeal function in a case
where conventional larynx reconstruction is not possible. It is
our opinion that, due to the described thyroid cartilage lesion
with functional preservation of both cricoarytenoid units,
SCPL-CHEP was the simplest, safest, and more effective way
to restore laryngeal function. To our knowledge, there has
been no previous report of the use of this procedure in a non-
oncologic setting, making this the first description of the possi-
ble use of the technique in laryngeal trauma management.
A final word on the pharyngocutaneous fistulae: as preserva-
tion of the pharyngeal mucosa seems to prevent this complication
in oncologic patients,4 its occurrence is attributed to the pyriform
sinus mucosal laceration caused by the laryngeal trauma.
Conclusions
SCPL-CHEP can be used to restore laryngopharyngeal func-
tion in trauma patients. Such patients, however, may be at
risk for pharyngocutaneous fistula following the procedure.
Acknowledgment
We thank Borges Dinis, MD, for the revision of the manuscript.
Author Contributions
Eduardo Ferreira, conception, drafting and revision of the article,
literature review; Carlos Nabuco Araujo, conception, drafting and
revision of the article, literature review; Sandra Agostinho, draft-
ing and revision of the article, literature review; Ana Rita Santos,
revision of the article, literature review.
Disclosures
Competing interests: None.
Sponsorships: None.
Funding source: None.
References
1. Kim JP, Cho SJ, Son HY, et al. Analysis of clinical feature and
management of laryngeal fracture: recent 22 case review.
Yonsei Med J. 2012;53:992-998.
2. Schaeffer S. Management of acute blunt and penetrating exter-
nal laryngeal trauma. Laryngoscope. 2013;124:233-244.
3. Bent JP III, Silver JR, Porubsky ES. Acute laryngeal trauma: a
review of 77 patients. Otolaryngol Head Neck Surg. 1993;109:
441-449.
4. Weinstein GS, Laccoureye O, Brasnu D, Laccourreye H. Organ
Preservation Surgery for Laryngeal Cancer. San Diego, CA:
Singular; 2000.
5. Bron L, Brossard E, Monnier P, Pasche P. Supracricoid partial
laryngectomy with CHEP and CHEP for glottic and supraglottic
carcinomas. Laryngoscope. 2000;110:627-634.
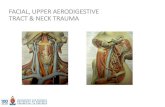
Figure 2. Infected tracheostomy and laryngopharyngostoma: (1)laryngopharyngostoma, (2) nasogastric tube, (3) right arytenoid, (4)left arytenoid, (5) left pyriform sinus, (6) glottic level, (7) infectedtracheostomy made in Africa.
Ferreira et al 887
at SOCIEDADE BRASILEIRA DE CIRUR on November 4, 2016oto.sagepub.comDownloaded from