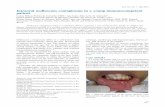
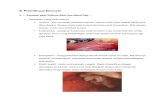
Comparison of intraoral harvest sites for corticocancellous bone grafts
-
Upload
sheetal-kapse -
Category
Health & Medicine
-
view
121 -
download
1
Transcript of Comparison of intraoral harvest sites for corticocancellous bone grafts

David M. Yates, Hans C. Brockhoff, Rick Finn, Ceib Phillips. Comparison of Intraoral Harvest Sites for Corticocancellous Bone Grafts. J Oral Maxillofac Surg 71:497-504, 2013.
PRESENTED BY – DR. SHEETAL KAPSE
GUIDED BY – DR. RAJASEKHAR G.

AUTHORS
1. David M. Yates : 5th Year Resident, University of Texas Southwestern Medical Center/Parkland, Dallas, TX.
2. Hans C. Brockhoff : 5th Year Resident, University of Texas Southwestern Medical Center/Parkland, Dallas, TX.
3. Rick Finn : Director, Section of Oral and Maxillofacial Surgery at the Dallas Veteran’s Affairs Medical Center and Faculty, Department of Cell Biology and Neuroscience, UT Southwestern Medical Center, Dallas, TX.
4. Ceib Phillips : Assistant Dean for Advanced Education/Graduate Programs, Interim Director, Curriculum in Oral Biology Professor, Department of Orthodontics School of Dentistry, University of North Carolina, Chapel Hill, NC.

CONTENTS
IntroductionAim Materials and methodsResults & DiscussionCross referencesConclusionPros and Cons of studyReferences

Introduction
A commonly used method for the repair of maxillofacial bony defects is the utilization of autogenous bone grafts from intraoral donor sites.
There are many advantages associated with intraoral harvesting.
Multiple cadaver studies have looked at individual donor sites but their sample sizes were small and they failed to compare multiple sites within the same specimen.

Introduction
There are many advantages associated with intraoral harvesting: easy accessibility, low rate of morbidity, and decreased cost.

Aim
The aim of this study was to quantify the amount of bone
in terms of area, thickness and volume that can be
harvested from the mandibular symphysis, ascending
ramus/body, coronoid process, and the
zygomaticmaxillary buttress using a within-subject
study design.

Materials and methods
The maxillae and mandibles of 59 cadavers were harvested.
Osteotomies performed with 703 surgical bur & Completed with mallet and chisel.

MANDIBULAR SYMPHYSIS
1.‘‘Superior dimension: dentate mandibles - 14 mm apical to the CEJ, edentulous mandibles - 5 mm from the crest of the alveolar ridge.
2.Inferior dimension: 4 mm superior from inferior border of the mandible.
3.Lateral dimension: 5 mm anterior to the mental foramen.
4.Posterior dimension: Lingual cortex of the mandible.

MANDIBULAR ASCENDING RAMUS/BODY
Superior dimension: Along the anterior border of the ramus approximately 1/3 the width of the mandible.
Superiorly to the base of the coronoid and anteriorly to the distal half of the first molar area.
Inferior dimension: Partial thickness cut made 4mm superior from inferior border of the mandible.
Anterior dimension: The distal half of the first molar area.
Posterior dimension: Made to the extent of the lingula.
Medial dimension: Through the lateral cortex of the mandible.
Mallet and chisel angled towards the buccal.

CORONOID PROCESS
Inferior dimension: Horizontal line extending from the sigmoid notch anteriorly that runs parallel to a line extending from condyle to coronoid tip through both the lingual and buccal cortex

ZYGOMATIC-MAXILLARY BUTTRESS GRAFT
Superior dimension: 5 mm inferior to the infraorbital foramen.
Inferior dimension: Dentate maxillae - 14 mm apical to CEJ; edentulous maxillae - transition zone between the alveolus and the Z-M buttress.
Anterior dimension: Dentate maxillae - distal to second premolar; edentulous maxillae -1 cm anterior to the point of maximum lateral protrusion of the Z-M buttress.
Posterior dimension: Dentate maxillae - distal to second molar; edentulous maxillae -1 cm posterior to the point of maximum lateral protrusion of Z-M buttress.
Medial dimension: Maxillary sinus membrane

VOLUME DETERMINATION
SURFACE AREA DETERMINATION
THICKNESS DETERMINATION
A 3 mL syringe filled with 3 mL of water.
The bone graft was placed in the syringe,
and the displaced water was removed with a pipette and
measured.
Symphysis: Treated as 2 independent rectangles
(midline-lateral). Ascending
ramus/body: Treated as 2 independent non-
overlapping rectangles. Coronoid: From inferior cut to most superior aspect of
coronoid process; b = ½ anterior posterior length. Zygomatic-Maxillary buttress: a = superior inferior height; b1 =
length of anterior posterior superior cut; b2
= length of anterior posterior
inferior cut.
The thickness of each graft was measured at
themaximal dimension of
the graft.
This was performedusing a Boley gauge
and ruler.


Results


Ramus – Greatest avg. Surface Area & Volume (twice the symphysis)
Symphysis – Thickest bone (largest cancellous component)
Coronoid /Zygoma –Substantially less Outcome

Discussion
According to the literature, the treatment of choice in restoring preinjury occlusion in patients with posttraumatic malocclusion is an osteotomy on the affected jaw, sometimes even at the fractured side.
In cases with asymmetric posttraumatic malocclusion due to a condylar process fracture, the only. Surgical option is an osteotomy at the affected side of the mandible, because facial symmetry needs to be corrected.
A posttraumatic anterior open bite due to bilateralcondylar process fractures presents a philosophical dilemma. The open bite can be considered either an entirely posttraumatic situation or an acquired dentofacial deformity.

Discussion
The first statement dictates restoration of ramus heigth; the latter advocates closure of the anterior open bite with (bi)maxillary surgery.
Dorsal impaction of the maxilla and subsequent autorotation of the mandible is reported to prevent relapse.
Ramus osteotomies with counterclockwise rotation of the distal fragment exceeding 40 are unsuitable because of reported relapse.

Cross references

Symphysis
Montazem – 16 dentate cadavers.
8 times more bone compared to this study 9.4 ml could be harvested .
This exponential increase might be due to non consideration of Age/Gender
Morbidity associated- altered sensation to lower incisors, chin, lower lip, chin contour defects, and periapical pathology.
Clavero and Lundgren reported76% cases with altered sensation (1-2 wks post op.) and18 months, 52% of patients continued to have altered sensation of their lower lip/chin area.
Montazem A, Valauri DV, St-Hilaire H, Buchbinder D: The mandibular symphysis as a donor site in maxillofacial bone grafting: A quantitative anatomic study. J Oral Maxillofac Surg 58:1368, 2000
Clavero J, Lundgren S: Ramus or chin grafts for maxillary sinus inlay and local onlay augmentation: Comparison of donor site morbidity and complications. Clin Implant Dent Relat Res 5:154, 2003

Body/Ramus
Gungormus et al 2002 -16 dentate cadavers only age mentioned
Volume obtained was similar to this study , thickness obtained was greater
Morbidity associated – Difficulty in chewing and mouth opening.
Clavero et al -21% cases with altered sensation in buccal nerve area and 4% showed permanent loss in a long term followup
Rabelo reported 4.4% temporary IAN paresthesia .
Persistent minor sensory changes were reported in 15.8 % of the symphysis group versus 2.63% of the ramus group.

Body/Ramus
Rajchel et al evaluated position of the mandibular canal from mandibular foramen to mental foramen in 45 cadavers.
Width of the mandible (10mm1.05 mm)
Thickness of the buccal cortical plate (2.3 mm 0.7 mm) and the width of the cancellous component between the medial side of the buccal cortical plate and the lateral aspect of the mandibular canal ( 4.05 mm 1.10 mm) were found at either the furcation of the first molar or the furcation of the second molar.
Rajchel J, Ellis E 3rd, Fonseca RJ: The anatomical location of the mandibular canal: Its relationship to the sagittal ramus osteotomy. Int J Adult Orthod Orthognath Surg 1:37, 1986

Coronoid Process
Choung and Kim reported a study in 2002 on15 dry Korean cadavers ≥20 years of age.
The surface area obtained was similar to the surface area in our study.
Choung PH, Kim SG: The coronoid process for paranasal augmentation in the correction of midfacial concavity. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 91:28, 2001

Zygomatic-Maxillary Buttress
Gellrich et al reported a case and the surface area was found
similar to the surface area obtained in this study .
Gellrich NC, Held U, Schoen R, et al: Alveolar zygomatic buttress: A new donor site for limited preimplant augmentation procedures. J Oral Maxillofac Surg 65:275, 2007


Pros Cons Good sample size
Largest cadaveric Study
First to compare all the harvest sites in the same specimen including the age and gender of the specimen
Racial variations
CBCT was not used
Pros and Cons of study

Conclusion
Body/ramus harvests have significantly less temporary sensory disturbances however these deficits improve with time.
The ramus provides the greatest volume of bone, as well as the largest amount of cortical bone
If one desires a larger cancellous component, the symphysis is an excellent choice.
The coronoid and zygomatic-buttress grafts provide little bone, but may be useful in unique circumstances.

References
1. Rubens BC, Stoelinga PJW, Weaver TJ, et ai: Management of malunited mandibular condylar fractures. Int J Oral Maxillofac Surg 19:22,1990
2. Ellis E III: Biological considerations concerning treatment of fractures of the mandibular condyle. International conference on management of fractures of the mandibular condyle, Groningen, The Netherlands, 1997
3. B. C. Rubens, P. J. W Stoelinga, T. J. Weaver and P. A. Blijdorp: Management Of maiunited mandibular condylar fractures. Int. J. Oral MaxiIlofae. Surg. 1990; 19: 22-25.
4. N. Zachariades, M. Mezitis, A. Michelis. Posttraumatic osteotomies of the jaws. lnt. J. Oral Maxillofac. Surg. 1993," 22." 328-331.