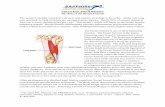
Common Knee Injuries in Distance Runners. Introduction Runners that average > 25 miles/wk have...
-
Upload
bernadette-parsons -
Category
Documents
-
view
223 -
download
1
Transcript of Common Knee Injuries in Distance Runners. Introduction Runners that average > 25 miles/wk have...
Introduction
• Runners that average > 25 miles/wk have injury rate > 30% per year
• Production of better shoes ---> decreased number of foot injuries, but not as effective in protecting knees
Biomechanics
• Rule of “too’s” common in runners
• Runners court disaster if they exercise too often, too hard, too soon and too much after injury, and attempt treatment too late
Biomechanics
• 67% of running injuries are result of training errors
• Body needs time to accommodate new stress levels
• Injury often due to sudden increase in frequency, duration, or intensity of training
Biomechanics
• Running -----> great forces across knee, especially during push off
• During running, force across kneecap is 7 x body wt.
Knee Problems: History
• High % of runner’s injuries are reaggravation of old injuries
• High % due to change in running style to compensate for prior injury
Physical Exam
• Thorough exam of knee
• Limb alignment
• Heel alignment
• Examine shoes’ patterns of wear
Anterior Knee Pain
• Termed “runner’s knee” in 1970’s
• Pain in front aspect of knee
• Several causes
Lateral Pressure Syndrome
• c/o “pain under kneecap”
• Increased pain running downhill, or sitting prolonged period in one position
• Due to poor tracking of kneecap
Lateral Pressure Syndrome
• Tight band on outer portion of kneecap - lateral retinaculum
• Treatment = conservative (6 mos. VMO strengthening)
• If fails, lateral release w/ arthroscope
• Outpatient surg.- 8 wk before running
Patellar Instability
• Maltracking or slight dislocation of kneecap
• Changes joint compression forces
• Symptoms of “pain in front of knee” or “knee giving way”
Patellar Instability
• If maltracking is subtle, treatment conservative -VMO strengthening
• If strengthening fails, lateral release for subtle maltracking
• If major maltracking, realign kneecap
Patellar Tendinitis
• Inflammation of patellar tendon
• “Jumper’s knee” but common in runners
• Symptoms = pain in front of knee just below kneecap
Patellar Tendinitis
• Excess stress on tendon ---> “microtears”
• Pain comes on gradually during run
• Runners often “run through it”, but as tendinitis worsens, often cannot run
Patellar Tendinitis
• Easily diagnosed by physical exam
• Treatment = REST, Iontophoresis in therapy
• DO NOT allow M.D. to inject cortisone in this region (may lead to rupture!)
Patellar Tendinitis
• If no relief w/ 3-6 mo of rest, get MRI
• Depending on severity of findings on MRI, may surgically excise area of pathology
Meniscal Tears
• Meniscus = “shock absorber” of knee
• Torn meniscus uncommon in young runners, but very common in middle age runners
Meniscal Tears
• Young runner - torn meniscus usually secondary to inciting incident (twisting injury)
• Middle aged runner - gradual onset of pain/clicking
Meniscal Tears
• Recurrent swelling
• “Catching” in knee
• “Giving way” or “locking” in younger runner
• Great difficulty squatting
Meniscal Tears
• Easily dx by exam
• Definitive dx = MRI
• Treatment = arthroscopic repair vs resection
• Back to running in 4-6 wk
Stress Fractures
• common in runners
• usually in mid to lower tibia (shin)
• less commonly, just below knee
Degenerative Arthritis
• Significant rise in runners age 60-70
• No direct evidence citing running as a cause of arthritis
• With older runners, arthritis more commonly seen
Degenerative Arthritis
• Must modify running program once Dx made
• Begin cross-training w/ biking, swimming, non-impact activities
• Arthroscopic “clean up” effective in only 65 %
Iliotibial Band Syndrome
• Pain = outer portion of knee
• Aggravated by running downhill
• Pain starts at 1-2 miles, progresses, and ceases after run
• Usually no pain w/ other sports
Iliotibial Band Syndrome
• “Bow-legged” alignment ?
• “Turning in” of forefoot
• Weak hip abductors ---> pelvic sag---> ITB
• Wear on outer sole of shoe
ITB: Treatment
• Stretch ITB
• Strengthen hip abductors
• Steroid injection vs iontophoresis
• Surgery = LAST RESORT !!
– Partial release of ITB
– Out for 4 wk
Summary
• Most injuries will resolve w/ modification of training program
• May need change in running surface, style, shoe, or mileage
Training Program
• May not need to stop running
• May need to reduce mileage, intensity
• Cross-train !!
• Aqua-jogging ---> non wt.bearing aerobic workout - maintains strength, endurance, mobility
Shoe Types
• Motion Control Shoe - prevents pronation
• Cushion Shoe - for rigid arches; provides more flexibility
• Support Shoe
Muscle Reconditioning
• Must restore muscle strength, endurance after all injuries
• If deficits persist - runner modifies running style ------> different injury !
Conclusions
• Knee remains most common site of injury in runners
• Most injuries are due to training errors
• Remember “Rule of Too’s”
Conclusions• Avoid surgery at all costs!!
• Most injuries can be treated w/ modification of training program, NSAIDS, P.T., time!!!
• Remember: HAVE PATIENCE
Introduction
• Complex issue
• Must consider material properties of graft (graft strength)
• Consider needs of patient
Introduction
• Patient weight, size, sex
• Patient’s activity level
• Type of sport
• Job requirements
Graft Types
• Bone-patellar tendon-bone
• Allograft (cadaveric achilles, b-pt-b)• Quadruple Hamstring
Bone-Patellar Tendon-Bone
• Central 1/3 of patellar tendon w/ bone plugs
• Most common graft in USA
• “Gold Standard”
Bone-Patellar Tendon-Bone
• Convenient - 1 incision ; readily available
• Bone block allows excellent fixation w/ screws
• Bone block allows bone to bone healing
Bone-Patellar Tendon-Bone
• Animal studies - graft shows faster incorporation than allograft
• Ultimate strength initially greater than native ACL
Bone-Patellar Tendon-Bone
• Loses 50% strength over time ---> strength approaches native ACL
• Among graft choices, shown to have greatest strength in most biomechanical studies
Disadvantages
• Anterior knee pain (16% in some reports)
• Patellar tendinitis
• Patellar tendon rupture, patellar fracture
Disadvantages
• Don’t recover motion as quickly
• ? increase in Quadriceps weakness
• May not be available in revision cases
• Increased operative time
Bone-Patellar Tendon-Bone
• Ideal candidate = high performance athlete who requires intense rehab / future performance
• Prefer no hx of patellofemoral Sx
• Larger athletes
Hamstring Graft
• Harvest semitendinosus and gracilis - 2 cm incision
• Quadruple loop ---> size and strength approaches bone-p.t.- bone graft
Hamstrings: Advantages
• Smaller, more cosmetic incision
• Lower complications from harvest
• Earlier return of motion; less pain
• ? Less anterior knee pain later
Hamstrings: Disadvantages
• No bone to bone fixation - weaker initial strength?
• Some feel rehab should be less aggressive due to decreased initial strength
Hamstring Graft
• Ideal candidate - smaller female athletes
• Any athlete with hx of patellofemoral pain
• Athletes who do a lot of kneeling (baseball catcher, volleyball players)
Allograft
• Harvested from cadaver
• Achilles tendon & patellar tendon most common
• Risk HIV transmission = 1 in 1.7 million
Allograft
• Controversial evidence that immune response occurs
• Controversial evidence - graft incorporates more slowly
Allograft
• Some studies show lower knee scores at f/u
• Slightly more inconsistent results
• ? increased laxity at 2-5 yrs
Allograft: Advantages
• No harvest site morbidity
• No size deficits
• Faster surgery
• Smaller incision
Allograft: Disadvantages
• Infection risk (but negligible)
• Possible immune response (effusion, tunnel enlargement)
• Increased $$
Allograft: Disadvantages
• Slower healing rate
• Less predictable results
• ? increased laxity at 2-5 yrs