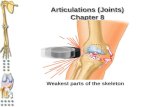
Ch 8. Joints (Articulations) Weakest parts of the skeleton Articulation – site where two or more...
-
Upload
cathleen-sheryl-heath -
Category
Documents
-
view
238 -
download
2
Transcript of Ch 8. Joints (Articulations) Weakest parts of the skeleton Articulation – site where two or more...

Ch 8

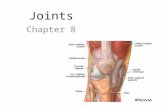
Joints (Articulations)
Weakest parts of the skeleton Articulation – site where two or more
bones meet Functions
Give the skeleton mobility Hold the skeleton together

Classification of Joints: Structural Structural classification focuses on the
material binding bones together and whether or not a joint cavity is present
The three structural classifications are: Fibrous Cartilaginous Synovial

Classification of Joints: Functional Functional classification is based on the
amount of movement allowed by the joint
The three functional class of joints are: Synarthroses – immovable Amphiarthroses – slightly movable Diarthroses – freely movable

Fibrous Structural Joints The bones are jointed by fibrous tissues There is no joint cavity Most are immovable There are three types:
Sutures Syndesmoses Gomphoses

Fibrous Structural Joints: Sutures Occur between the bones of the skull Comprised of interlocking junctions
completely filled with CT fibers Bind bones tightly together, but allow for
growth during youth In middle age, skull bones fuse and are
called synostoses

Fibrous Structural Joints: Syndesmoses Bones are connected by a fibrous tissue
ligament Movement varies from immovable to
slightly variable Examples include the connection
between the tibia and fibula, and the radius and ulna

Fibrous Structural Joints: Gomphoses The peg-in-socket fibrous joint between
a tooth and its alveolar socket The fibrous connection is the periodontal
ligament

Cartilaginous Joints
Articulating bones are united by cartilage
Lack a joint cavity Two types – synchondroses and
symphyses

Cartilaginous Joints: Synchondroses A bar or plate of hyaline cartilage unites
the bones All synchondroses are synarthrotic Examples include:
Epiphyseal plates of children Joint between the costal cartilage of the
first rib and the sternum

Cartilaginous Joints: Symphyses Hyaline cartilage covers the articulating
surface of the bone and is fused to an intervening pad of fibrocartilage
Amphiarthrotic joints designed for strength and flexibility
Examples include intervertebral joints and the pubic symphysis of the pelvis

Synovial Joints
Those joints in which the articulating bones are separated by a fluid-containing joint cavity
All are freely movable diarthroses Examples – all limb joints, and most
joints of the body

Synovial Joints: General Structure Synovial joints all have the following:
Articular cartilage Joint (synovial) cavity Articular capsule Synovial fluid Reinforcing ligaments


Synovial Joints: Friction-Reducing Structures Bursae – flattened, fibrous sacs lined
with synovial membranes and containing synovial fluid
Common where ligaments, muscles, skin, tendons, or bones rub together
Tendon sheath – elongated bursa that wraps completely around a tendon

Synovial Joints: Stability
Stability is determined by: Articular surfaces – shape determines
what movements are possible Ligaments – unite bones and prevent
excessive or undesirable motion Muscle tone is accomplished by:
Muscle tendons across joints are the most important stabilizing factor
Tendons are kept tight at all times by muscle tone

Synovial Joints: Movement Muscle attachment across a joint Origin – attachment to the immovable
bone Insertion – attachment to the movable
bone Described as movement along
transverse, frontal, or sagittal planes

Synovial Joints: Range of Motion
Nonaxial – slipping movements only Uniaxial – movement in one plane Biaxial – movement in two planes Multiaxial – movement in or around all
three planes

Gliding Movements
One flat bone surface glides or slips over another similar surface
Examples – intercarpal and intertarsal joints, and between the flat articular processes of the vertebrae

Angular Movement
Flexion Extension Dorsiflexion and plantar flexion of the
foot Abduction Adduction Circumduction

Rotation
The turning of a bone around its own long axis
Examples: Between first two vertebrae Hip and shoulder joints

Special Movements
Supination and pronation Inversion and eversion Protraction and retraction Elevation and depression Opposition

Types of Synovial Joints Plane joints
Articular surfaces are essentially flat Allow only slipping or gliding movements Only examples of nonaxial joints
Hinge joints Cylindrical projections of one bone fits into a
trough-shaped surface on another Motion is along a single plane Uniaxial joints permit flexion and extension
only Examples: elbow and interphalangeal joints

Pivot Joints
Rounded end of one bone protrudes into a “sleeve,” or ring, composed of bone (and possibly ligaments) of another
Only uniaxial movement allowed Examples: joint between the axis and
the dens, and the proximal radioulnar joint

Pivot Joints

Condyloid, or Ellipsoidal, Joints
Oval articular surface of one bone fits into a complementary depression in another
Both articular surfaces are oval Biaxial joints permit all angular motions Examples: radiocarpal (wrist) joints, and
metacarpophalangeal (knuckle) joints

Saddle Joints
Similar to condyloid joints but with greater movement
Each articular surface has both a concave and a convex surface
Example: carpometacarpal joint of the thumb

Ball-and-Socket Joints
A spherical or hemispherical head of one bone articulates with a cuplike socket of another
Multiaxial joints permit the most freely moving synovial joints
Examples: shoulder and hip joints

Synovial Joints: Shoulder (Glenohumeral)
Ball-and-socket joint in which stability is sacrificed to obtain greater freedom of movement
Head of humerus articulates with the glenoid fossa of the scapula


Synovial Joints: Shoulder Stability
Weak stability is maintained by: Thin, loose joint capsule Four ligaments – coracohumeral, and
three glenohumeral Tendon of the long head of biceps, which
travels through the intertubercular groove and secures the humerus to the glenoid cavity
Rotator cuff (four tendons) encircles the shoulder joint and blends with the articular capsule

Synovial Joints: Knee
Largest and most complex joint of the body
Allow flexion, extension, and some rotation
Three joints in one surrounded by a single joint cavity Femoropatellar Lateral and medial tibiofemoral joints


Synovial Joints: Major Ligaments and Tendons – Anterior View
Tendon of the quadriceps femoris muscle
Lateral and medial patellar retinacula Fibular collateral ligament Tibial collateral ligament Patellar ligament

Synovial Joints: Knee – Other Supporting Structures
Anterior cruciate ligament Posterior cruciate ligament Medial meniscus (semilunar cartilage) Lateral meniscus

Synovial Joints: Knee – Posterior Superficial View
Adductor magnus tendon Articular capsule Oblique popliteal ligament Arcuate popliteal ligament Semimembranosus tendon

Sprains
The ligaments reinforcing a joint are stretched or torn
Partially torn ligaments slowly repair themselves
Completely torn ligaments require prompt surgical repair

Sprain

Cartilage Injuries
The snap and pop of overstressed cartilage
Common aerobics injury Repaired with arthroscopic surgery

Cartilage Injuries

Dislocations
Occur when bones are forced out of alignment
Usually accompanied by sprains, inflammation, and joint immobilization
Caused by serious falls and are common sports injuries
Subluxation – partial dislocation of a joint

Dislocation

Dislocation

Inflammatory and Degenerative Conditions Bursitis
An inflammation of a bursa, usually caused by a blow or friction
Symptoms are pain and swelling Treated with anti-inflammatory drugs;
excessive fluid may be aspirated Tendonitis
Inflammation of tendon sheaths typically caused by overuse
Symptoms and treatment are similar to bursitis

Arthritis More than 100 different types of
inflammatory or degenerative diseases that damage the joints
Most widespread crippling disease in the U.S.
Symptoms – pain, stiffness, and swelling of a joint
Acute forms are caused by bacteria and are treated with antibiotics
Chronic forms include osteoarthritis, rheumatoid arthritis, and gouty arthritis

Osteoarthritis (OA)
Most common chronic arthritis; often called “wear-and-tear” arthritis
Affects women more than men 85% of all Americans develop OA More prevalent in the aged, and is
probably related to the normal aging process


Osteoarthritis: Course OA reflects the years of abrasion and
compression causing increased production of metalloproteinase enzymes that break down cartilage
As one ages, cartilage is destroyed more quickly than it is replaced
The exposed bone ends thicken, enlarge, form bone spurs, and restrict movement
Joints most affected are the cervical and lumbar spine, fingers, knuckles, knees, and hips


Osteoarthritis: Treatments OA is slow and irreversible Treatments include:
Mild pain relievers, along with moderate activity
Magnetic therapy Glucosamine sulfate decreases pain and
inflammation SAM-e (s-adenosylmethionine) builds up
cartilage matrix and regenerates tissue

Rheumatoid Arthritis (RA) Chronic, inflammatory, autoimmune
disease of unknown cause, with an insidious onset
Usually arises between the ages of 40 to 50, but may occur at any age
Signs and symptoms include joint tenderness, anemia, osteoporosis, muscle atrophy, and cardiovascular problems
The course of RA is marked with exacerbations and remissions

Rheumatoid Arthritis: Course RA begins with synovitis of the affected
joint Inflammatory blood cells migrate to the
joint, causing swelling Inflamed synovial membrane thickens
into a pannus Pannus erodes cartilage, scar tissue
forms, articulating bone ends connect The end result, ankylosis, produces
bent, deformed fingers

Rheumatoid Arthritis: Treatment Conservative therapy – aspirin, long-
term use of antibiotics, and physical therapy
Progressive treatment – anti-inflammatory drugs or immunosuppressants
The drug Embrel, a biological response modifier, removes cells that promote inflammation

Gouty Arthritis Deposition of uric acid crystals in joints
and soft tissues, followed by an inflammation response
Typically, gouty arthritis affects the joint at the base of the great toe
In untreated gouty arthritis, the bone ends fuse and immobilize the joint
Treatment – colchicine, nonsteroidal anti-inflammatory drugs, and glucocorticoids

Developmental Aspects of Joints By embryonic week 8, synovial joints resemble adult joints Few problems occur until late middle age Advancing years take their toll on joints including: Ligaments and tendons shorten and weaken Intervertebral discs become more likely to herniate OA is inevitable, and all people of 70 have some degree of
OA Prudent exercise (especially swimming) that coaxes joints
through their full range of motion is key to postponing joint problems