Cervical Spine Trauma
description
Transcript of Cervical Spine Trauma

Cervical Spine Trauma
Aaron B. Welk, DCResident, Department of Radiology
Logan College of Chiropractic

Three Column Model• Anterior
– ALL– Anterior half of vertebral body, disc, and supporting soft tissues
• Middle– PLL– Posterior half of vertebral body, disc, and supporting soft
tissues• Posterior
– Posterior elements– Facet joints– Associated soft tissues

Three Column Model
• Disruption of only one column is generally stable
• Disruption of 2 or 3 columns implies instability• Flexion and extension films may highlight
instability that is not evident on neutral lateral.

Evaluation Of Alignment-Instability may be subtle.
-Disruption of any one of the anatomical lines may indicate injury.
-Evaluation of 4 lines must be done on all lateral films.
-Anterior body line (A)-Posterior body line (B)-Spinolaminar line (C)-Posterior spinous line

Flexion Injury • Unilateral Locked Facet
– Flexion with rotation– Most common location is C4/5 and C5/6– Little or no body displacement– Bow-tie Sign
• Bilateral Locked Facet– Flexion with enough force to distract facets– 50% anterolisthesis on lower segment

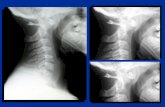
Unilateral Locked Facet

Bilateral Locked Facet

Bilateral Locked Facet
Left Right

Bilateral Locked Facet
Sag T2 FSE Sag STIR

Spinal Cord Contusion
• Non-Hemorrhagic bruising of spinal cord
• MRI Appearance:– T1: Low signal intensity– T2: High signal intensity

Spinal Cord Contusion

Spinal Cord Hemorrhage• Hyperacute:
– T1: isointense– T2: high signal intensity
• Acute:– T1: Low signal intensity– T2: Low signal intensity
• Subacute (early):– T1: high signal intensity– T2: low signal intensity
• Subacute (late):– T1: high signal intensity– T2: high signal intensity
• Chronic:– T1: isointense– T2: high signal intensity

Spinal Cord Hemorrhage
T1 T2

Flexion Injury• Anterior Wedge Compression
– Usually Stable unless posterior ligaments are disrupted– Disrupted posterior elements may appear stable initially due to muscle spasm
• Teardrop Burst– Most severe injury compatible with life.– 80% with neurologic injury– Posterior body is displaced into neural canal

Teardrop Burst Fracture

Teardrop Burst Fracture

Teardrop Burst Fracture

Clay-Shoveler’s Fracture
• Oblique Fracture through the spinous process of C6-T3 (C6 and C7 are most common)
• The name is derived from the common occurrence of this fracture in Australian clay miners.
• Usually caused by hyperflexion, although a direct blow can also cause this injury

Clay-Shoveler’s fracture

Clay-Shoveler’s Fracture

Extension Injury• Extension Teardrop
– Avulsion of ALL from inferior corner of vertebral body– Usually at C2 or C3
• Hangman’s Fracture– Fracture of the neural arch of C2 with varying degrees of C2/3 disk
involvement– Type I- Fracture of neural arch w/o disk involvement– Type II- >3mm displacement or 15˚ angulation at C2/3– Type III- Anterior displacement of C2 due to unilateral or bilateral
facet dislocation. • Pillar/Facet Fracture
– Extension injury while head is rotated

Extension Teardrop

Extension Teardrop

Hangman’s Fracture- Type I

Hangman’s Fracture- Type II

Hangman’s Fracture- Type III

Pillar Fracture

Pillar Fracture

Odontoid Fractures
• Mechanism of injury is not fully understood and experimental attempts to recreate have been unsuccessful.
• Injury is result of major force and usually results from MVA or falls.
• 3 Classifications:– Type I- Fracture of upper portion of dens (Stable)– Type II- Fracture at base of dens at C2 body junction
(Unstable)– Type III- Fracture into C2 body (Stable)*

Type I Odontoid Fracture

Type II Odontoid Fracture

Type III Odontoid Fracture

Jefferson’s (Burst) Fracture
• Ring fracture of C1 due to axial loading• Lateral displacement of lateral masses• May have little or no neurologic deficit unless
transverse ligament is ruptured

Jefferson’s Fracture

References
• Musculoskeletal Imaging: The Requisites, 3rd ed. B.J. Manaster, David G. Disler, David A. May, editors. St. Louis: Mosby; 2007. pp 164-174
• Diagnosis of Bone and Joint Disorders. 4th ed. Donald Resnick. Philadelphia: W.B. Saunders; 2002. pp 2958-2981

Images• http://thejns.org• http://radiographics.rsna.org• http://download.imaging.consult.com• www.medcyclopedia.com• http://emedicine.medscape.com• http://handbook.muh.ie• http://int.prop.if2.cuni.cz• http://radiologyinthai.blogspot.com• www.aafp.org• www.learningradiology.com• http://img.orthobullets.com• http://img04.webshots.com• www.mypacs.net• www.medifax.com• www.medscape.com• http://gentili.us• www.med.wayne.edu• www.radiologyassistant.nl