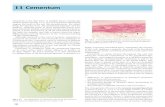
Cementum and Bone
-
Upload
sonia-nath -
Category
Documents
-
view
304 -
download
10
description
Transcript of Cementum and Bone
-
Shaju Jacob
Extension 2755
Senior Lecturer Dentistry
(Periodontology)
-
LEARNING OBJECTIVE
This presentation is a continuation from the previous
lecture on healthy periodontium, in this lecture
cementum and bone will be discussed.
At the end of this lecture you will be able to:
Describe clinical and macroscopic features of
cementum and bone
Describe the microscopic feature of cementum and
bone
Discuss its function and its importance
-
CEMENTUM
IN HEALTH
-
Definition: Cementum is calcified, avascular mesenchymal tissue that forms the outer covering of the anatomic root.
It is also called as substantia ossea.
It was first discovered microscopically demonstrated by two pupils of Purkinje in 1835.
CEMENTUM
-
It serves to invest and
attach the periodontal
fibers
To maintain the thickness of
root in apical region
-
INORGANIC:
Calcium and phosphate in the form of HYDROXYAPATITE
crystals
These crystals are 55nm wide,8nm thick
Highest fluoride content
Calcium and magnesium
TRACE AMOUNT:
Copper, Fluorine, Iron, Lead,
Potassium, Silicon, Sodium and Zinc
COMPOSITION
-
Non-Collagenous Protein:
Cementum is rich in glycoconjugates, which represent either glycolipids, glycoproteins or proteoglycans and harbors a variety of other proteins.
The predominant noncollagenous proteins are:
1) Bone sialoprotein 3) Osteonectin 2) Osteoponitin 4) Fibronectin, Tenasin
ORGANIC: Collagen:
Type I - 90%
Type III - 5%
-
CELLS OF CEMENTUM:
a) Cementoblast
b) Cementocytes
c) Cementoclast
CEMENTOCYTES CEMENTOBLASTS
-
Cemental Fibers
Sharpeys Fibers (extrinsic): These fibers are embedded
portions of the principal fibers
of the periodontal ligament and
are formed by fibroblasts.
Intrinsic Fibers: these are
fibers that belong to the
cemental matrix and are
produced by cementoblasts.
-
Structure of cementum
Under light microscope, two types of cementum are visible. Based on the presence or absence of cells they are classified as:
Acellular Cementum ( Primary cementum)
Cellular cementum ( Secondary cementum)
It will be seen under two headings:
Formation
Anatomical Characteristics
-
Formation of Acellular Extrinsic fiber cementum
The first cells that align along the newly
formed, but not yet mineralized, mantle
dentin surface exhibit fibroblastic
characteristics.
Mineralization of the mantle dentin takes
place
Intermingling of collagen fibers at cementum
and dentin interface.
Then fiber fringe extends towards PDL.
-
Initial acellular extrinsic fiber
cementum thus consists of a thin
mineralized layer with a short
fringe of collagen fibers
implanted perpendicular to the
root surface inserting in mantle
dentin
-
Cells on the root surface
secrete noncollagenous
matrix proteins that fill in the
spaces between the
collagen fibers and regulate
mineralization of the
forming cementum layer.
Bone sialoprotein
-
This activity continues until about
1520 um of cementum has been formed, at which time the intrinsic
fibrous fringe becomes connected to
the developing periodontal ligament
fiber bundles.
-
Anatomic characteristics of acellular
cementum
It is the first formed cementum and is therefore referred to as primary cementum.
It covers approximately the cervical third or half of the root. It does contain any cell.
This cementum is formed before tooth reaches the occlusal plane and its thickness ranges from 30 to 230 microns.
It is thinnest at the cementoenamel junction and thickest towards root apex.
Sharpeys fibers make up most of the structure of acellular cementum.
Acellular cementum also contains intrinsic collagen fibrils that are calcified and are irregularly arranged or parallel to the surface.
-
Formation cellular Intrinsic Fiber
Cementum
Cementoblasts start forming a less mineralized layer.
Matrix proteins that fill in the spaces between the collagen fibrils, regulate mineral deposition and impart cohesion to the mineralized layer.
A layer of unmineralized matrix, termed cementoid.
Collagen fibrils are produced rapidly and deposited haphazardly during the initial phase; however, subsequently the bulk of fibrils organize as bundles oriented mostly parallel to the root surface.
-
cementoblasts start forming a
less mineralized variety of
cementum
-
As the process proceeds, some
cementoblasts become trapped in the
matrix they form. These entrapped cells,
with reduced secretory activity, are
called cementocytes and sit in lacunae.
-
Cellular
Cementum
Canaliculi of
cementocytes
Lacunae of
cementocyte
Some cementoblasts
become trapped in the matrix
to form cementocytes and sit
in lacunae.
-
Cementum
Cementocyte
Cementoid
-
Anatomic Characteristics of
Cellular cementum
It is the cementum is formed after the tooth
reaches the occlusal plane.
It is more irreglular and contains cells within
its matrix called cementocytes.
Cellular cementum is more on the apical half
of the root.
It is less calcified than acellular cementum.
Sharpeys fibers make up smaller portions and
are separated by collagen fibers.
-
Formation of cementum continues throughout the life, it is
the cellular cementum which continuously contributes to
the length of root.
-
Classification of Cementum:
Based on the findings Schroeder 1985 classified cementum:
Acellullar afibrillar cementum: (AAC):
Acellular extrinsic fiber cementum:(AEFC)
Cellular mixed stratified cementum; (CMSC):
Cellular intrinsic fiber cementum (CIFC):
Intermediate cementum:
-
1. Acellular Afibrillar
cementum
2. Acellular Extrinsic fiber
cementum
3. Cellular intrinsic fiber
cementum
4. Cellular Mixed stratified
cementum
-
Intermediate Cementum or hyaline layer of Hopewell Smith.
Periodontal
ligament
cementum
Intermediate
cementum
Dentin
Clinical Significance: hyaline layer contains epithelial derived enamel like
proteins and has an important role in the attachment of cementum to the
dentin surface.
-
60% to 65% Cementum overlapping the enamel
30% End-to-end relationship of enamel and cementum
5% to 10% space between enamel and cementum with dentin
CEMENTO ENAMEL JUNCTION:
-
Cementodentinal Junction:
The terminal apical areas of the
cementum where it joins the internal root
canal dentin is known as the
cementodentinal junction (CDJ).
When root canal treatment is performed
the obturating material should be at CDJ.
It remains stable without any increase or
decrease.
The CDJ is 2 to3 um wide.
-
Anchorage
Attachment
Adaptive and reparative function
Walling in filled canals
Repairing roots (horizontal fracture)
Sealing of necrotic pulps by occluding apical foramen
Protecting underlying dentin
FUNCTIONS:
-
ALVEOLAR
BONE IN
HEALTH
-
Bone is a mineralized connective tissue.
About 60% of its weight is inorganic material, about
25% organic material and about 15% water.
The mineral phase is carbonated hydroxyapatite,
distributed both within the spaces between and on the
surfaces of the collagen fibrils.
The cells through their capacity for osteosynthesis and
resorption, have a pivotal role in the maintenance of the
matrix.
-
Bone consists of two-thirds inorganic matter and one-third organic matrix.
INORGANIC MATTER:
Calcium & Phosphate,
Hydroxyl
Carbonate
Citrate
ORGANIC MATTER:
90% of collagen Type I
Non collagenous proteins;
Osteocalcin
Osteonectin
Bone morphogenetic protein
Phosphoproteins
Proteoglycans.
-
Organization of Adult Bone
Inner and outer
circumferential lamellae
Osteons (Haversian
lamella)
Cementing lines
Haversian canal
Blood vessels,
nerves,
mesenchymal
tissue, endosteum
Interstitial lamella
-
ALVEOLAR PROCESS
The alveolar process is the portion of the maxilla and mandible
that forms and supports the tooth sockets (alveoli). Develops in
response to presence or absence of teeth.
The alveolar process consists of the following:
1. An external plate of cortical bone formed by haversian bone
and compacted bone lamellae.
2. The inner socket wall of thin, compact bone called the
alveolar bone proper, which is seen as the lamina dura in radiographs.
3. Cancellous trabeculae, between these two compact layers,
which act as supporting alveolar bone.
In addition, the jaw bones consists of the basal bone, which is the
portion of the jaw located apically but unrelated to the tooth
-
ALVEOLAR PROCESS
Cortical plate.
Dense outer covering of the spongy bone.
Provides strength and protection.
Serves as attachment site for muscles.
Spongy bone.
Less dense and cancellous bone.
Makes up the central portion of the alveolar process
-
Compact and Spongy Bone
-
INTERDENTAL SEPTUM:
Interdental
septum consists of
cancellous bone
bordered by the
socket wall cribriform
plates of
approximating teeth
and the facial and
lingual cortical plates.
Lamina dura
Thin compact bone that lines the tooth socket.
Has many small
openings for
blood vessels
and nerve fibers.
-
CELLS AND INTERCELLULAR MATRIX:
OSTEOBLASTS OSTEOCLASTS
-
Mineralized matrix
Osteoid
Cell process
Osteoid
(or prebone)
-
SOCKET WALL:
The socket wall consists of dense, lamellated bone, some
of which is arranged in haversian systems, and bundle bone.
Bundle bone is the term given to bone adjacent to the
periodontal ligament that contains a great number of sharpeys
fibers.
Bundle bone is not unique to the jaws; it occurs through
the skeletal system wherever ligaments and muscles are
attached.
-
BONE MARROW:
In the embryo and newborn, the cavities of all bones are
occupied by red hematopoietic marrow.
The red marrow gradually undergoes a physiologic change
to the fatty or yellow inactive type of marrow.
Foci of red bone marrow are occasionally seen in the
jaws, like maxillary tuberosity, maxillary and mandibular molar
and premolar areas, and the mandibular symphysis and ramus
angle, which may be visible radiographically as zones of
radiolucency.
-
Periosteum
The tissue covering the outer surface of bone is termed
periosteum. It consists of;
1. Inner layer composed of osteoblasts surrounded
by osteoprogenitor cells.
2. Outer layer rich in blood vessels and nerves and
composed of collagen fibers and fibroblasts.
Bundles of periosteal collagen fibers penetrate the
bone, binding the periosteum to the bone.
-
Endosteum
The tissue lining the internal bone cavities is called
endosteum.
It consists of
1) Inner layer osteogenic layer
2) Outer layer fibrous layer.
-
Copyright 2007, Thomas G. Hollinger, Gainesville, Fl
Periosteum
Osteocyte in lacuna
Fibrous layer
of periosteum
Osteogenic or
cellular layer
of periosteum
Endosteum
(Osteoblasts)
Osteoblasts
-
REMODELLING:
It is the major pathway of bony changes in shape,
resistance to forces, repair of wounds, and calcium and phosphate
homeostasis in the body.
The interdependency of osteoblasts and osteoclasts in
remodeling is called coupling.
The bone matrix that is laid down by osteoblasts is
nonmineralized osteoid.
Bone resorption is a complex process morphologically
related to the appearance of eroded bone surfaces (Howships
lacunae) and large, multinucleated cells- Ostoclasts.
-
REMODELING OF ALVEOLAR BONE
Alveolar bone is the least stable of the periodontal
tissues because its structure is in a constant state of
flux.
A considerable amount of internal remodeling
takes place by means of resorption and formation, which
are regulated by local and systemic influences.
The remodelling of the alveolar bone affects its
height, contour, and density.
-
REFERENCES
Antonia Nanci, Ten Cates Oral Histology, 7th edition. Antonia Nanci and Dieter D Boohardt: Structure of
periodontal tissues in health and disease. Periodontology 2000 2003; 31: 12-31
Michael G. Newman , Henry Takei, Perry R. Klokkevold, Clinical Periodontology, 10 edi
Jan Lindhe, Karring, Lang, Clinical Periodontology and Implant Dentistry., 5th Edition.
Thomas G. Wilson Fundamentals of Periodontics, 2nd edition, Anatomy of Periodontium.
Bhaskar SN, Orbans Oral Histology and Embryology, 11 th edition




![Microanalysis of Root Cementum in Patients with Rapidly ......at the exposed cementum [4]. Chemical analysis of the exposed cementum has shown an increase in calcium, magnesium, and](https://static.fdocuments.net/doc/165x107/5f237b2b5d795a336e24c740/microanalysis-of-root-cementum-in-patients-with-rapidly-at-the-exposed-cementum.jpg)