Castration inhibits biliary proliferation induced by bile ... · Castration inhibits biliary...
Transcript of Castration inhibits biliary proliferation induced by bile ... · Castration inhibits biliary...
Castration inhibits biliary proliferation induced by bile duct obstruction: novelrole for the autocrine trophic effect of testosterone
Fuquan Yang,1,6* Sally Priester,1,3* Paolo Onori,7 Julie Venter,1 Anastasia Renzi,1,10
Antonio Franchitto,10,11 Md Kamruzzaman Munshi,1,11 Candace Wise,1 David E. Dostal,2,5
Marco Marzioni,8 Stefania Saccomanno,8 Yoshiyuki Ueno,9 Eugenio Gaudio,10 and Shannon Glaser1,4,5
Department of Medicine, Division of 1Gastroenterology and 2Molecular Cardiology, Scott & White and Texas A&M HealthScience Center, College of Medicine, 3Research & Education, Scott & White, 4Scott & White Digestive Disease ResearchCenter, and 5Central Texas Veterans Health Care System, Temple, Texas; 6Department of Hepatobiliary Surgery, ShengjingHospital, China Medical University, Shenyang, Liaoning Province, China; 7Experimental Medicine, University of L’Aquila,L’Aquila; 10Department of Anatomical, Histological, Forensic Medicine and Orthopedics Sciences, University of Rome “LaSapienza”, Rome; Fondazione Eleonora Lorillard Spencer-Cenci, Rome; 8Department of Gastroenterology, UniversitaPolitecnica delle Marche, Ancona, Italy, 9Division of Gastroenterology, Tohoku Graduate University School of Medicine,Sendai, Japan; and 11Institute of Food and Radiation Safety, Dhaka, Bangladesh
Submitted 15 February 2011; accepted in final form 29 August 2011
Yang F, Priester S, Onori P, Venter J, Renzi A, Franchitto A, MunshiMK, Wise C, Dostal DE, Marzioni M, Saccomanno S, Ueno Y, GaudioE, Glaser S. Castration inhibits biliary proliferation induced by bile ductobstruction: novel role for the autocrine trophic effect of testosterone. Am JPhysiol Gastrointest Liver Physiol 301: G981–G991, 2011. First publishedSeptember 8, 2011; doi:10.1152/ajpgi.00061.2011.—Increased cholangio-cyte growth is critical for the maintenance of biliary mass during liver injuryby bile duct ligation (BDL). Circulating levels of testosterone decline follow-ing castration and during cholestasis. Cholangiocytes secrete sex hormonessustaining cholangiocyte growth by autocrine mechanisms. We tested thehypothesis that testosterone is an autocrine trophic factor stimulating biliarygrowth. The expression of androgen receptor (AR) was determined in liversections, male cholangiocytes, and cholangiocyte cultures [normal rat intra-hepatic cholangiocyte cultures (NRICC)]. Normal or BDL (immediatelyafter surgery) rats were treated with testosterone or antitestosterone antibodyor underwent surgical castration (followed by administration of testosterone)for 1 wk. We evaluated testosterone serum levels; intrahepatic bile duct mass(IBDM) in liver sections of female and male rats following the administrationof testosterone; and secretin-stimulated cAMP levels and bile secretion. Weevaluated the expression of 17�-hydroxysteroid dehydrogenase 3 (17�-HSD3, the enzyme regulating testosterone synthesis) in cholangiocytes. Weevaluated the effect of testosterone on the proliferation of NRICC in theabsence/presence of flutamide (AR antagonist) and antitestosterone antibodyand the expression of 17�-HSD3. Proliferation of NRICC was evaluatedfollowing stable knock down of 17�-HSD3. We found that cholangiocytesand NRICC expressed AR. Testosterone serum levels decreased in castratedrats (prevented by the administration of testosterone) and rats receivingantitestosterone antibody. Castration decreased IBDM and secretin-stimulated cAMP levels and ductal secretion of BDL rats. Testosteroneincreased 17�-HSD3 expression and proliferation in NRICC that wasblocked by flutamide and antitestosterone antibody. Knock down of 17�-HSD3 blocks the proliferation of NRICC. Drug targeting of 17�-HSD3 maybe important for managing cholangiopathies.
biliary epithelium; biliary secretion; 17�-hydroxysteroid dehydroge-nase 3; secretin; sex hormones
IN ADDITION TO PLAYING A KEY role in the ductal secretion ofwater and bicarbonate (mainly regulated by secretin) (3, 30),
cholangiocytes are the target cells in a number of chroniccholestatic liver diseases (termed cholangiopathies), includingprimary sclerosing cholangitis and primary biliary cirrhosis(PBC) (5, 8). During the progression of cholangiopathies, thebalance between the proliferation/loss of cholangiocytes iscritical for the maintenance of biliary secretory function andintrahepatic bile ductal mass (5, 8, 34, 36). Cholangiocytesrespond to cholestasis and liver injury with changes in prolif-eration and ductal bile secretion (2, 3, 18, 22). In response tobile duct ligation (BDL), there is enhanced biliary hyperplasiaand secretin-stimulated choleresis (a functional marker ofcholangiocyte growth) (2, 3, 18, 22), whereas, following theadministration of hepatotoxins (e.g., carbon tetrachloride),there is loss of cholangiocyte mass and secretory function (36).Indeed, proliferating cholangiocytes serve as neuroendocrinecells secreting and responding to a number of hormones andneuropeptides contributing to the autocrine and paracrine path-ways that modulate the homeostasis of the biliary epithelium(8, 16, 18, 19, 22, 23, 39).
Cholangiocyte growth/apoptosis is regulated by a number offactors, including gastrointestinal hormones, the second mes-senger system, cAMP, and sex hormones, including estrogens,prolactin, follicle-stimulating hormone, and progesterone (7, 8,17, 23, 39, 49). Regarding sex hormones, estrogens have beenshown to sustain cholangiocyte proliferation and reducecholangiocyte apoptosis (6, 7). Prolactin is expressed andsecreted by cholangiocytes and stimulates the growth ofcholangiocytes by an autocrine mechanism (49). Progesteroneenhances the proliferative activity of female and male cholan-giocytes via autocrine mechanisms, since cholangiocytes pos-sess the enzymatic pathway for steroidogenesis (23). Follicle-stimulating hormone increases cholangiocyte proliferation byan autocrine mechanism via cAMP-dependent phosphorylationof ERK1/2 and Elk-1 (39).
Testosterone is an anabolic steroid that is primarily secretedin the testes of males and the ovaries of females, althoughsmall amounts are also secreted by the adrenal glands. Testos-terone is thought to predominantly mediate its biological ef-fects through binding to the androgen receptor (AR) (43).Similar to other members of the nuclear receptor superfamily,ARs function as a ligand-inducible transcription factor. ARsare expressed in the liver by hepatocellular carcinoma, hepa-
* F. Yang and S. Priester contributed equally to this work.Address for reprint requests and other correspondence: S. S. Glaser, Dept. of
Medicine, Texas A&M Health Science Center, Central Texas Veterans HealthCare System, VA Bldg. 205, 1901 South 1st St., Temple, TX, 76504 (e-mail:[email protected]).
Am J Physiol Gastrointest Liver Physiol 301: G981–G991, 2011.First published September 8, 2011; doi:10.1152/ajpgi.00061.2011.
0193-1857/11 Copyright © 2011 the American Physiological Societyhttp://www.ajpgi.org G981
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
tocytes in areas of ductular metaplasia, and in a number ofmetastatic adenocarcinomas, including bile duct cholangiocar-cinoma (26, 44, 47). However, no information exists regardingthe expression and role of testosterone and its receptors in theregulation of cholangiocyte growth and ductal secretory activ-ity in cholestasis. The rate-limiting step in the synthesis oftestosterone from androstenedione (a product of dehydroepi-androsterone and progesterone, both of which are products ofpregnenolone and cholesterol) depends on the enzyme 17�-hydroxysteroid dehydrogenase 3 (17�-HSD3) (20). On thebasis of these findings, we performed experiments aimed todemonstrate that: 1) reduction of testosterone serum levelsdecreases cholangiocyte proliferation; 2) testosterone adminis-tration stimulates biliary growth and prevents the decrease inbiliary hyperplasia induced by castration; 3) cholangiocytesexpress 17�-HSD3 and secrete testosterone regulating biliaryby an autocrine mechanism; and 4) silencing of 17�-HSD3 (theenzyme regulating testosterone synthesis) (20) decreases bili-ary proliferation in vitro. The data suggest an autocrine com-pensatory role of testosterone in sustaining cholangiocyte pro-liferation in cholestasis, a pathological condition characterizedby testicular atrophy and lowered serum testosterone levels(14, 33, 54, 57).
MATERIALS AND METHODS
Materials. Reagents were purchased from Sigma Chemical (St.Louis, MO) unless otherwise stated. The monoclonal mouse antibody(clone PC-10) reacting with proliferating cellular nuclear antigen(PCNA) and the goat polyclonal antibody (antibody raised against apeptide mapping within an internal region of AR of human origin)reacting with both subtypes of AR were purchased from Santa CruzBiotechnology (Santa Cruz, CA). The AR antibody (G-13) is recom-mended for the detection of AR of mouse, rat, and human origin. Thesubstrate for �-glutamyltranspeptidase (�-GT), N-(�-L-glutamyl)-4-methoxy-2-naphthylamide, was purchased from Polysciences (War-rington, PA). The enzyme-linked immunosorbebt assay (ELISA) kitused for measuring testosterone levels in serum and supernatant ofprimary cultures (after 6 h of incubation at 37°C) of isolated cholan-giocytes from the selected groups of rats and primary cultures of ratintrahepatic cholangiocyte cultures [normal rat intrahepatic cholan-giocyte cultures (NRICC)] from normal male rats (4) was purchasedfrom Cayman Chemical (Ann Arbor, MI). The RIA kit (125I-cAMPBiotrak Assay System, RPA509) for the determination of intracellularcAMP levels in purified cholangiocytes was purchased from GEHealthcare (Piscataway, NJ).
Animals. Female and male 344 Fischer rats (150–175 g) werepurchased from Charles River (Wilmington, MA) and maintained in atemperature-controlled environment (20–22°C) with 12:12-h light-dark cycles. Animals were fed ad libitum standard chow and had freeaccess to drinking water. The studies were performed in: 1) normaland BDL female and male rats treated with sesame oil (vehicle) ortestosterone in sesame oil (2.0 mg/100 g body wt) (10); 2) normalmale rats with castration (bilateral orchiectomy) (40) or sham; and3) BDL (for collection of liver blocks and cell isolation) (3) male rats(immediately after surgery) (3) that underwent sham or castration (40)followed by daily intraperitoneal injections of sesame oil or testos-terone in sesame oil (2.0 mg/100 g body wt) (10) for 7 days. In otherexperiments, we treated BDL (immediately after surgery) male ratswith nonimmune serum or a polyclonal immune-neutralizing testos-terone antibody (6.5 nmol/dose ip every day, a dose similar to thatused by us for immunoneutralizing other sex hormones such asprogesterone) (23) for 7 days before collecting serum and liver blocksfor the determination of biliary growth and apoptosis. Immediatelyafter bile duct incannulation (for bile collection) (3), male rats under-
went sham for castration or castration (followed by the administrationof sesame oil or testosterone in sesame oil, 2.0 mg/100 g body wt for1 wk) (10) before evaluating the effect of intravenous infusion ofsecretin on bile and bicarbonate secretion (3). Because there was nodifference in biliary growth (data not shown) between normal ratstreated with sesame oil and sham rats for castration or BDL ratstreated with sesame oil or nonimmune serum and BDL sham rats forcastration, we used only normal and BDL rats as controls in our study.Seven days later, the animals were killed for the collection of serum,liver block, bile, and cholangiocytes. Before each procedure, animalswere anesthetized with pentobarbital sodium (50 mg/kg body wt ip)according to the regulations of the panel on euthanasia of the Amer-ican Veterinarian Medical Association and local authorities. All ex-periments were reviewed and approved by the Scott & White Hospi-tal/Texas A&M Health Science Center Institutional Animal Care andUse Committee.
Purification of cholangiocytes and hepatocytes. Virtually purecholangiocytes (�98% by �-GT histochemistry) (46) were isolated byimmunoaffinity separation (27) using a mouse monoclonal antibody(IgM, kindly provided by Dr. R. Faris, Brown University, Providence,RI) that recognizes an unidentified antigen expressed by all intrahe-patic rat cholangiocytes (27). Cell viability (by trypan blue exclusion)was �98%. Hepatocytes were isolated from normal and BDL malerats as described (27). Male NRICC, which display morphological,phenotypic, and functional phenotypes similar to that of freshlyisolated cholangiocytes, were developed, characterized, and main-tained in culture as described by us (4).
Expression of AR and 17�-HSD3. The presence of AR was eval-uated by: 1) immunofluorescence (16) in frozen liver sections (4–5�m thick) and immunohistochemistry (39) in paraffin-embedded liversections (4–5 �m thick) from normal and BDL male rats; and2) RT-PCR (1) and fluorescence-activated cell sorter (FACS) analysis(45) in cholangiocytes and hepatocytes from normal and BDL malerats. In NRICC, the expression of AR was also evaluated by RT-PCRand immunofluorescence (39). For all immunoreactions, negativecontrols (with normal serum from the same species substituted for theprimary antibody) were included.
With regard to RT-PCR (performed using the GeneAmp RNA PCRkit from Perkin-Elmer, Branchburg, NJ), specific oligonucleotideprimers were based on the sequence of the rat AR (11) (sense,5=-CCCTGTGTGTGCAGCTAGAA-3= and antisense, 5=-TAGACA-GGATCTGCCCTGCT-3=), with an expected fragment length of 247bp; we used RNA (1 �g) from rat testicles and yeast-transfer RNA aspositive and negative controls, respectively. The comparability of theRNA used was assessed by RT-PCR for the housekeeping geneglyceraldehyde-3-phosphate dehydrogenase (GAPDH) (sense 5=-GT-GACTTCAACAGCAACTCCCATTC-3= and antisense 5=-GTTA-TGGGGTCTGGGATGGAATTGTG-3=), with an expected fragmentlength of 294 bp; primers were based on the rat GAPDH sequence(15); rat kidney and yeast transfer RNA were the positive and negativecontrols for the GAPDH gene, respectively. Standard RT-PCR con-ditions were used, consisting of 35 step cycles: 30 s at 94°C, 30 s at60°C for AR and 52°C for GAPDH for 45 s at 72°C. FACS analysisfor AR was performed in isolated cholangiocytes and hepatocytesfrom normal and BDL rats using a C6 flow cytometer and analyzed byCFlow Software (Accuri Cytometers, Ann Arbor, MI). At least 20,000events in the light scatter (side scatter/forward scatter) were acquired.The expression of AR was identified and gated on fluorescencechannel 1-A (FL1-A)/count plots. The relative quantity of AR (meanselected protein fluorescence) was expressed as mean FL1-A (sam-ples) per mean FL-1A (secondary antibodies only). The standarderrors were calculated as (CV FL1-A) � (mean FL1-A)/SQR(count1), where CV is coefficient of variation and SQR is square root.
We evaluated the expression of 17�-HSD3 (37) by: 1) immuno-fluorescence (16) in frozen liver sections (4–5 �m thick) and immu-nohistochemistry (39) in paraffin-embedded liver sections (4–5 �mthick) from normal and BDL male rats; 2) real-time PCR (16) and
G982 TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
FACS analysis (45) (see above) in freshly isolated male cholangio-cytes; and 3) real-time PCR and immunofluorescence (16) in maleNRICC. For all immunoreactions, negative controls (with normalserum from the same species substituted for the primary antibody)were included. Following immunofluorescence for AR and 17�-HSD3, images were visualized using an Olympus IX-71 confocalmicroscope. Light microscopy photographs of liver sections stainedfor AR and 17�-HSD3 were taken by Leica Microsystems DM4500 B Light Microscopy (Weltzlar, Germany) with a JenoptikProg Res C10 Plus Videocam (Jena, Germany). The positivity ofbile ducts for AR and 17�-HSD3 was evaluated as described by us(25). When 0 –5% of bile ducts were positive for AR and 17�-HSD3, we assigned a negative score; a � score was assigned when6 –10% of bile ducts were positive; a � score was assigned when11–30% of bile ducts were positive; a �� score was assigned with
31– 60% of bile ducts positive; and a ��� score was assignedwhen �61% of bile ducts were positive. Two pathologists per-formed the evaluations in a blinded manner.
For real-time PCR, total RNA was extracted from cholangio-cytes by the RNeasy Mini Kit (Qiagen, Valencia, CA) and reversetranscribed using the Reaction Ready First-Strand cDNA synthesiskit (SuperArray, Frederick, MD). These reactions were used astemplates for the PCR assays using a SYBR Green PCR master mixand specific primers designed against the rat 17�-HSD3NM_054007 (51) and GAPDH, the housekeeping gene (SuperAr-ray), in the real-time thermal cycler (ABI Prism 7900HT sequencedetection system). A CT (delta delta of the threshold cycle)analysis was performed using normal cholangiocytes as the cont-rol sample. Data are expressed as fold change of relative mRNAlevels � SE (n 6).
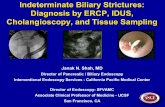
Fig. 1. A: image showing that intrahepaticbile ducts from normal and bile duct ligation(BDL) male rats express androgen receptor(AR) (red staining). Colocalization withCK-19 (green staining) of bile ducts express-ing the AR (red staining) is also visible. Bar 50�m. B: by immunohistochemistry, normalcholangiocytes and hepatocytes express lowlevels of AR, expression that increased follow-ing BDL (A and B; see Table 1). Originalmagnification, �40. C: by RT-PCR, the messagefor AR was expressed by freshly isolated cholan-giocytes from normal (NR) and BDL rats andnormal rat intrahepatic cholangiocyte cultures(NRICC); the housekeeping gene, glyceralde-hyde-3-phosphate dehydrogenase (GAPDH),was expressed similarly by these cells. MW,mol wt. D: by immunofluorescence, NRICCalso expressed the protein for AR. Bar 20�m. E and F: fluorescence-activated cell sorter(FACS) analysis shows the presence of theprotein for AR in freshly isolated cholangio-cytes and hepatocytes from normal and BDLmale rats; the expression of AR seemed up-regulated (*P � 0.05) in BDL cholangiocytescompared with normal cholangiocytes. Dataare means � SE of 3 determinations.
G983TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
Evaluation of testosterone serum levels, cholangiocyte apoptosis,and intrahepatic bile duct mass in liver sections. Testosterone serumlevels in female and male rats were measured by commerciallyavailable ELISA kits (Cayman Chemical). Cholangiocyte apoptosiswas evaluated in paraffin-embedded liver sections (4–5 �m thick) bya quantitative terminal deoxynucleotidyl transferase biotin-dUTP nickend-labeling (TUNEL) kit (Apoptag; Chemicon International) (39).The percentage of TUNEL-positive cholangiocytes was counted in sixnonoverlapping fields (magnification �40) for each slide; the data areexpressed as the percentage of TUNEL-positive cholangiocytes. Thenumber of intrahepatic bile ducts in frozen liver sections (4–5 �mthick) was determined by the evaluation of intrahepatic bile duct mass(IBDM) by point-counting analysis (35, 56). IBDM was measured asthe percentage area occupied by �-GT-bile duct/total area � 100 (35,56). Morphometric data were obtained in six different slides for eachgroup; for each slide, we performed the counts in six nonoverlappingfields (n 36). Following the selected staining, sections were coun-
terstained with hematoxylin and eosin and analyzed for each groupusing a BX-51 light microscopy (Olympus, Tokyo, Japan).
Measurement of basal and secretin-stimulated cAMP levels andbile secretion. At the functional level, cholangiocyte proliferation wasevaluated by measurement of basal and secretin-stimulated cAMPlevels in purified cholangiocytes by RIA (17, 22, 32) and bile andbicarbonate secretion in bile fistula rats (3), two functional indexes ofcholangiocyte proliferation (3, 17, 22). For the measurement of cAMPlevels (17, 22), purified cholangiocytes (1 � 105) were incubated for1 h at 37°C and incubated for 5 min at room temperature with 0.2%BSA (basal) or 100 nM secretin with 0.2% BSA (17, 22, 32).Following anesthesia with pentobarbital sodium, rats were surgicallyprepared for bile collection (3). When steady-state bile flow wasreached [60–70 min from the infusion of Krebs-Ringer-Henseleit(KRH) solution], the animals were infused by a jugular vein withsecretin (100 nM) for 30 min followed by a final infusion of KRH for30 min. Bile was collected every 10 min in preweighed tubes thatwere used for determining bicarbonate concentration. Bicarbonateconcentration (measured as total CO2) in the selected bile sample wasdetermined by an ABL 520 Blood Gas System (Radiometer Medical,Copenhagen, Denmark).
Effect of testosterone on the expression of 17�-HSD3 and prolif-eration of NRICC: Effect of pharmacological inhibition and molecu-lar silencing of 17�-HSD3 on NRICC proliferation. To obtain adose-response curve, NRICC were treated with vehicle (1% methanol,where testosterone is dissolved, basal value) or testosterone (10�5 to10�11 M for 7 days in 1% methanol) before evaluating cell prolifer-ation by MTS assays (16). We also evaluated the effects of testoster-
Table 1. Semiquantitative analysis of AR expression in liversections from normal and BDL male rats
Normal BDL
Cholangiocytes � ��Hepatocytes � �
AR, androgen receptor; BDL, bile duct ligation. Grading scale: - 0–5%; � 6–10%; � 11–30%; �� 31–60%; ��� �61%.
Fig. 2. Measurement of serum testosteronelevels in the selected groups of animals.Testosterone serum levels were lower in fe-male and male BDL rats compared with theircorresponding normal rats. The administra-tion of testosterone increased testosteroneserum levels in normal and BDL female andmale rats. Castration significantly decreasedtestosterone serum levels in normal andBDL rats. Administration of neutralizing an-titestosterone antibody decreased testoster-one serum levels in both normal and BDLrats compared with rats treated with nonim-mune serum. The administration of testoster-one to BDL castrated rats partly preventedcastration-induced reduction of testosteroneserum levels. Data are means � SE of 12cumulative determinations. *P � 0.05 com-pared with the corresponding values of nor-mal rats. #P � 0.05 compared with thecorresponding values of normal rats. &P �0.05 compared with the corresponding val-ues of BDL rats.
G984 TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
one on the expression of message for 17�-HSD3 in NRICC. NRICCwere stimulated with vehicle (1% methanol, where testosterone isdissolved, basal value) or testosterone (100 nM for 6, 24, 48, and 72h in 1% methanol) before measuring 17�-HSD3 mRNA expression byreal-time PCR (see above) (16).
In separate experiments, NRICC (after trypsinization) were seededinto 96-well plates (10,000/well) in a final volume of 200 �l ofmedium and allowed to adhere to the plate overnight. NRICC wereincubated at 37°C with 0.2% BSA (basal), flutamide (a specificantagonist of AR, 10 �M) (28), or antitestosterone antibody (100ng/ml with 0.2% BSA) for 48 h before evaluation of proliferation byMTS assays (16).
Furthermore, following stable transfection of 17�-HSD3 in NRICC(24), we measured the basal proliferative rates of the cells (afterincubation for 24, 48, and 72 h at 37°C) by PCNA immunoblots andMTS assays (16). NRICC lacking 17�-HSD3 was established usingSureSilencing shRNA (SuperArray) plasmid for rat 17�-HSD3 con-taining a marker for neomycin resistance for the selection of stablytransfected cells, according to the instructions provided by thevendor as described by us (13). A total of four clones wereassessed for the relative knock down of the 17�-HSD3 gene usingreal-time PCR (�80% knock down), and a single clone with thegreatest degree of knock down was selected for subsequent exper-iments. In control vector- and 17�-HSD3-knocked cells, we alsoevaluated the amount of secreted testosterone (by ELISA kits) afterincubation for 24 h at 37°C.
Statistical analysis. All data are expressed as means � SE. Differ-ences between groups were analyzed by the Student’s unpaired t-testwhen two groups were analyzed and ANOVA when more than twogroups were analyzed, followed by an appropriate post hoc test. Avalue of P � 0.05 was considered significant.
RESULTS
Expression of AR. By both immunofluorescence and immu-nohistochemistry in liver sections, we demonstrated that intra-hepatic bile ducts from normal and BDL male rats express AR(Fig. 1, A and B). Colocalization of CK-19 (a cholangiocyte-specific marker) (18) with intrahepatic bile ducts expressingAR is visible in Fig. 1A. By immunohistochemistry, normalcholangiocytes and hepatocytes express low levels of AR,expression that increased following BDL (Fig. 1, A and B, andTable 1). By RT-PCR, the message for AR (247 bp) wasexpressed by freshly isolated cholangiocytes and hepatocytesfrom normal and BDL male rats and NRICC (Fig. 1C); thehousekeeping gene, GAPDH mRNA (294 bp), was similarlyexpressed by these cells (Fig. 1C). By immunofluorescence,NRICC also expressed the protein for AR (Fig. 1D). We alsodemonstrated by FACS analysis the presence of AR in freshlyisolated cholangiocytes and hepatocytes from normal and BDLmale rats (Fig. 1, E and F); the expression of AR was upregu-lated in BDL compared with normal cholangiocytes (Fig. 1E).
Evaluation of testosterone serum levels, cholangiocyte apop-tosis, and IBDM in liver sections. Parallel to previous studies(53, 54), testosterone serum levels were lower in female andmale BDL rats compared with their corresponding normal rats(Fig. 2A). The serum levels of testosterone were lower infemale rats compared with the corresponding values of malerats (Fig. 2B). The administration of testosterone increasedtestosterone serum levels in normal and BDL male rats (Fig. 2,A and B). Castration significantly decreased testosterone serumlevels in normal and BDL male rats (Fig. 2B) (31). Similarly,administration of neutralizing antitestosterone antibody de-creased testosterone serum levels in both normal and BDLmale rats compared with rats treated with nonimmune serum(Fig. 2B). The administration of testosterone to BDL castratedrats partly prevented castration-induced reduction of testoster-one serum levels (Fig. 2B). In female and male BDL rats, there
Table 2. Measurement of IBDM in the experimental groupsof animals
Treatments IBDM, %
Male
Normal 0.26 � 0.04BDL 6.32 � 0.67a
BDL testosterone 10.4 � 0.80b
BDL � antitestosterone antibody 1.8 � 0.14b
BDL � castration 0.32 � 0.04b
BDL � castration � testosterone 5.48 � 0.63
Female
Normal 0.77 � 0.14BDL 4.01 � 0.21a
BDL � testosterone 6.68 � 0.89b
Values are means � SE. IBDM, intrahepatic bile duct mass. P � 0.05 vs.IBDM of normal rats (a) and vs. IBDM of BDL rats (b).
Fig. 3. Measurement of basal and secretin-stimulated cAMPlevels in purified cholangiocytes. In normal and BDL rats(without castration), secretin increases cAMP levels of purifiedcholangiocytes. In purified cholangiocytes from normal andBDL castrated rats, there was ablation of the stimulatory effectsof secretin on cAMP levels. *P � 0.05 vs. the correspondingbasal cAMP levels. #P � 0.05 vs. basal cAMP levels of normalcholangiocytes. Data are means � SE of 6 experiments.
G985TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
was increased IBDM compared with their corresponding nor-mal rats (Table 2) (3). Also, testosterone increased IBDM innormal (data not shown) and BDL female and male rats (Table2) compared with rats treated with vehicle. Consistent with theconcept that testosterone is a trophic factor for cholangiocytegrowth, castration (which reduces serum testosterone levels)(31) decreased IBDM in both normal (data not shown) andBDL rats compared with rats without castration (Table 2). Wenext demonstrated that administration of an antitestosteroneantibody (which reduces the circulating levels of testosterone)decreased IBDM compared with control BDL rats (Table 2),and administration of testosterone partly prevented castration-induced loss of IBDM (Table 2). In BDL castrated rats andBDL rats treated with antitestosterone antibody, there was anincrease in apoptosis compared with BDL rats (data notshown).
Castration inhibits secretin-stimulated cAMP levels and bilesecretion. Secretin increased cAMP levels of cholangiocytesfrom normal but not normal castrated rats (Fig. 3). Basal cAMPlevels of cholangiocytes from BDL rats were higher thancAMP levels of normal cholangiocytes (Fig. 3). As expected(3, 35), secretin did not induce changes in bile and bicarbonatesecretion in normal rats with or without castration (Table 3). Inagreement with previous studies (2, 3), in BDL rats (withoutcastration), secretin increased cAMP levels in purified cholan-giocytes (Fig. 3) and bicarbonate-rich choleresis in bile fistularats (Table 2). After castration to BDL rats, the stimulatoryeffects of secretin on cAMP levels in purified cholangiocytes(Fig. 3) and bile and bicarbonate secretion in bile fistula rats
(Table 2) were ablated. Chronic administration (1 wk) oftestosterone to BDL castrated rats restored the functionalsecretory activity of cholangiocytes, since secretin was able tostimulate bile and bicarbonate secretion (Table 3) in these rats.
Expression of 17�-HSD3 in liver sections and cholangio-cytes: Evaluation of testosterone secretion in NRICC anddetermination of the effect of pharmacological inhibition andmolecular silencing of 17�-HSD3 on NRICC growth. Byimmunofluorescence and immunohistochemistry in liver sec-tions, 17�-HSD3 was expressed by intrahepatic bile ducts fromnormal and BDL male rats (Fig. 4, A and B). The immunore-activity was higher in bile ducts from male BDL rats comparedwith their corresponding normal rats. mRNA (by real-timePCR) and protein (by FACS) for 17�-HSD3 was expressed bynormal male cholangiocytes and increased following BDL(Fig. 4, C and D). In purified cholangiocytes from male BDLrats with castration or receiving antitestosterone antibody, theexpression of 17�-HSD3 mRNA was similar to or higher thanthat of BDL cholangiocytes (Fig. 4C), which is likely due to acompensatory mechanism by cholangiocytes in response todecreased testosterone serum levels after castration or theadministration of antitestosterone antibody to BDL rats. Wehave also demonstrated that normal cholangiocytes andNRICC secrete testosterone in the supernatant, and the levelsof testosterone increased in the supernatant of BDL cholangio-cytes compared with normal cholangiocyte supernatant (Fig.4E). In purified cholangiocytes from BDL rats with castrationor receiving antitestosterone antibody, the secretion of testos-terone was similar to that of BDL cholangiocytes (Fig. 4E). By
Fig. 4. A: by immunofluorescence, 17�-hydroxysteroid dehydrogenase 3 (17�-HSD3) was expressed by intrahepatic bile ducts of liver sections from normal andBDL rats with and without castration. Colocalization with CK-19 (green staining) of bile ducts expressing the AR (red staining) is also visible. Bar 50 �m.B: by immunohistochemistry, cholangiocytes from normal and BDL rats express 17�-HSD3. Original magnification, �40. The immunoreactivity was higher inbile ducts from male BDL rats (��) compared with their corresponding normal rats (�). C and D: the message and protein for 17�-HSD3 was expressed bynormal male cholangiocytes and increased following BDL. Data are means � SE of 3 real-time PCR and FACS experiments. C: in purified cholangiocytes fromBDL rats with castration or receiving antitestosterone antibody, the expression of 17�-HSD3 mRNA was similar to that of BDL cholangiocytes. Data aremeans � SE of 3 real-time PCR experiments. *P � 0.05 vs. all of the other groups. D: the protein expression levels of 17�-HSD3 were determined by FACSanalysis. *P � 0.05 vs. normal rat. E: normal cholangiocytes and NRICC secrete testosterone in the supernatant. The levels of testosterone increased in thesupernatant of BDL cholangiocytes compared with normal cholangiocyte supernatant. In purified cholangiocytes from BDL rats with castration or receivingantitestosterone antibody, the secretion of testosterone was similar to that of BDL cholangiocytes. Data are means � SE of 8 evaluations. *P � 0.05 vs. all ofthe other groups. F: by immunofluorescence, NRICC express the protein for 17�-HSD3. Bar 50 �m.
Table 3. Measurement of basal and secretin-stimulated bile flow, bicarbonate concentration and secretion in normal andrats that (immediately after BDI) underwent castration surgery followed by the administration of vehicle or testosterone
Treatment
Bile Flow Bicarbonate Concentration Bicarbonate Secretion
Basal, �l · min�1 · kgbody wt�1
Secretin,�l · min�1 · kg
body wt�1 Basal, meq/l Secretin, meq/lBasal, �l · min�1 · kg
body wt�1Secretin, �l · min�1 · kg
body wt�1
Normal rats (n 4) 81.7 � 6.3 83.0 � 5.8 29.4 � 0.9 26.8 � 0.3 2.4 � 0.2 2.2 � 0.1Normal rats � castration (n 4) 70.2 � 4.3 71.1 � 8.9 30.7 � 3.7 27.5 � 6.1 2.3 � 0.2 1.2 � 0.3BDI rats (n 4) 126.8 � 15.0a 187.8 � 21.9b 37.1 � 3.4a 45.5 � 2.6b 4.9 � 0.2a 8.6 � 1.1b
BDI rats � castration � vehicle (n 4) 114.1 � 24.7 133.0 � 15.7ns 26.8 � 11.2 35.1 � 14.9ns 3.1 � 1.8 4.9 � 2.2ns
BDI rats � castration � testosterone (n 4) 109.1 � 13.3c 146.3 � 13.9c 32.5 � 0.8 41.1 � 1.1c 3.6 � 0.4 6.1 � 0.6c
Values are means � SE; n, no. of rats. BDI, bile duct incannulated.When steady spontaneous bile flow was reached [60-70 min from the infusion ofKrebs-Ringer-Henseleit (KRH)], rats were infused for 30 min with secretin followed by a final infusion of KRH for 30 min. After the rats were surgically preparedfor bile flow experiments, bile was collected every 10 min in preweighed tubes and used for determining bicarbonate concentration. aP � 0.05 vs. correspondingbasal value of bile flow, bicarbonate concentration, or bicarbonate secretion of normal rats without castration. bP � 0.05 vs. corresponding basal value of bileflow, bicarbonate concentration. or bicarbonate secretion of BDI rats. nsVs. corresponding basal value of bile flow, bicarbonate concentration, or bicarbonatesecretion of BDI rats without castration. cP � 0.05 vs. corresponding basal value of bile flow, bicarbonate concentration, or bicarbonate secretion of BDI castratedrats treated with testosterone for 1 wk. Differences between groups were analyzed by the Student’s unpaired t-test when two groups were analyzed and ANOVAwhen more than two groups were analyzed.
G986 TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
immunofluorescence, NRICC express the protein for 17�-HSD3 (Fig. 4F).
Similar to what is shown in vivo (Table 2), testosterone(10�11 to 10�5 M) in vitro increased the proliferation (by
MTS) of NRICC compared with the corresponding basalvalue (Fig. 5A). Also, testosterone (100 nM) increased themRNA expression of 17�-HSD3 (the key enzyme regulatingtestosterone synthesis) (20) in NRICC compared with the
G987TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
corresponding basal value (Fig. 5B). Consistent with theconcept that testosterone (synthesized and secreted byfreshly isolated cholangiocytes and NRICC) regulates thegrowth of these cells by an autocrine mechanism, we haveshown that, when NRICC were incubated with flutamide (aspecific antagonist of AR) (28) or antitestosterone antibodyfor 48 h, there was a decrease in cell growth compared withNRICC treated with 0.2% BSA (basal) (Fig. 5C). Further-more, knock down of 17�-HSD3 (80% decrease by real-time PCR) (Fig. 6A) in NRICC decreased the basal prolif-erative activity of NRICC (Fig. 6B), supporting the conceptthat testosterone is an autocrine factor sustaining biliarygrowth.
DISCUSSION
The present study demonstrates the paracrine and autocrinerole of testosterone in the stimulation of cholangiocyte growthin normal and cholestatic states. We first demonstrated thatintrahepatic bile ducts and hepatocytes (in liver sections) andfreshly isolated cholangiocytes and hepatocytes from normaland BDL rats, and male NRICC express testosterone receptors.We have also shown that: 1) testosterone serum levels werelower in female and male BDL compared with normal rats and2) castration and administration of neutralizing antitestosteroneantibody significantly decreased testosterone serum levels innormal and BDL male rats. The administration of testosteroneincreased testosterone serum levels in both normal and BDLmale rats and partly prevented castration-induced reduction oftestosterone serum levels. We have also demonstrated that:1) testosterone increased IBDM of both normal and BDLfemale and male rats; 2) castration and administration ofantitestosterone antibody decreased IBDM in BDL male rats;and 3) administration of testosterone partly prevented castra-tion-induced loss of IBDM in BDL male rats. At the functionallevel, in BDL castrated rats, there was ablation of secretin-stimulated cAMP levels and bicarbonate-rich choleresis, twofunctional indexes of biliary growth (2, 3, 22, 36). Similar to invivo, in in vitro studies, we have demonstrated that testosteroneincreased the proliferation of male NRICC. We have also
Fig. 5. A: measurement of NRICC proliferation following treatment with 0.2%BSA or testosterone. Testosterone (10�11 to 10�5 M) in vitro increased theproliferation (by MTS) of NRICC compared with the corresponding basalvalue. Data are means � SE of 6 experiments. *P � 0.05 vs. thecorresponding basal value. B: testosterone in vitro increased the mRNAexpression of 17�-HSD3 (the key enzyme regulating testosterone synthe-sis) in NRICC compared with the corresponding basal value. Data aremeans � SE of 6 experiments. *P � 0.05 vs. the corresponding basal value.C: measurement of cell growth (by MTS assays) in NRICC stimulated withBSA (basal), flutamide (a specific antagonist of AR), or antitestosteroneantibody for 48 h. When NRICC were incubated with flutamide or antit-estosterone antibody, there was a decrease in cell growth compared withNRICC treated with BSA. Data are means � SE of 6 experiments. *P �0.05 vs. the corresponding basal value.
Fig. 6. A and B: effect of knock down of 17�-HSD3 on the basal proliferativeactivity of NRICC by MTS assays. Knock down of 17�-HSD3 (�80%) inNRICC (A) decreased the proliferative activity of NRICC (B), supporting theconcept that testosterone is an autocrine factor sustaining biliary growth. Dataare means � SE of 6 experiments. *P � 0.05 vs. the corresponding basalvalue.
G988 TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
shown that: 1) intrahepatic cholangiocytes and NRICC express17�-HSD3 (the key enzyme regulating testosterone synthesis)(20) and secrete testosterone; 2) the biliary expression of17�-HSD3 and secretion of testosterone increases after BDLand in NRICC after in vitro treatment with testosterone; and3) stable transfection of 17�-HSD3 in NRICC decreases theproliferative activity of these cells. The finding that testoster-one stimulates biliary proliferation by an autocrine mechanismmay be an important compensatory mechanism for sustainingbiliary growth and ductal secretory activity in ductopenicpathologies of the biliary epithelium.
Cholangiopathies, which specifically target cholangiocytes,are characterized by dysregulation of the balance betweenbiliary growth/damage (5). Thus, studies aimed to understandthe intracellular mechanisms of this phenomenon are neces-sary. In this context, the cholestatic BDL rodent model hasbeen used widely to pinpoint the mechanisms of biliarygrowth/apoptosis (2, 3, 6, 18, 19, 22, 34, 49). A number ofstudies have demonstrated that 1) gastrointestinal and sexhormones, bioagenic amines, and neuropeptides regulate thegrowth of bile ducts and 2) in the course of chronic cholestasis,cholangiocytes acquire neuroendocrine phenotypes regulatingbiliary functions by both autocrine and paracrine pathways (2,3, 5–8, 18, 19, 22, 34, 49). Our study provides the firstevidence that ARs are expressed by cholangiocytes and testos-terone stimulates biliary growth and secretion during choles-tasis. We propose that testosterone is important in sustainingbiliary proliferation and ductal secretory activity in patholog-ical conditions associated with functional damage of the biliaryepithelium.
We first demonstrated in male rats the expression of func-tional testosterone receptors in bile ducts, cholangiocytes,hepatocytes, and NRICC. Supporting our findings, a number ofstudies have shown the presence of functional ARs in livercells, including hepatocytes and bile ducts from PBC patients(26, 29, 38). Also, the AR mRNA has been detected in humanliver biopsy samples, fetal liver, and HepG2 cells (48). In thenext sets of experiments, we demonstrated that enhancedtestosterone serum levels correlate with increased IBDM inmale rats and decreased testosterone serum levels are associ-ated with reduction of the number of intrahepatic bile ducts inmale rats. We first validated our models, demonstrating thattestosterone serum levels decreased in cholestatic BDL malerats (compared with normal rats) and in castrated rats andincreased in rats chronically treated with testosterone. Thedecrease in testosterone serum levels is likely due to hypotro-phy of seminal vesicles as observed in rats during puberty andBDL-induced cholestasis (33, 54, 57). Testicular atrophy hasbeen observed in cirrhotic patients (52), whereas lower serumtestosterone levels have been shown in patients with PBC (14).Contrasting results exist regarding serum testosterone levels inother liver diseases. For example, while a study has demon-strated lowered serum testosterone levels in cirrhotic rats (53),other studies have shown elevated serum testosterone maypromote the development of hepatocellular carcinoma in cir-rhosis (50). The decrease in serum testosterone levels observedin our animals is supported by a number of studies in rodents(31, 55) in which the decrease is prevented by the chronicadministration of testosterone (55). Similar to our finding,other studies have demonstrated that chronic administration oftestosterone increased testosterone serum levels (9). A number
of studies have shown that sex hormones, including estrogens,prolactin, follicle-stimulating hormone, and progesterone, sus-tain biliary proliferation by both paracrine and autocrine mech-anisms (6, 7, 23, 39, 49). However, no information existsregarding the role of testosterone in modulating the balancebetween cholangiocyte growth/loss. The fact that testosteroneincreases biliary hyperplasia and prevents the loss of biliarygrowth and function (following castration) supports the con-cept that androgens can be important for ameliorating thecholestatic conditions associated with testicular hypotrophyand ductopenic conditions associated with decreased testoster-one levels as occurs in PBC (14). These findings and the factthat the administration of neutralizing antitestosterone anti-body reduces testosterone serum levels and biliary hyperplasiaintroduce the concept that the administration of testosteronereceptor antagonists or antitestosterone antibodies may be newtherapeutic approaches for decreasing the aberrant growth ofcholangiocytes. At the functional level, we demonstrated thatthe decrease in testosterone serum levels was associated withablation of secretin-stimulated cAMP synthesis in cholangio-cytes and bicarbonate-rich choleresis in bile fistula male rats,two functional parameters that were restored by the chronicadministration of testosterone. Indeed, enhanced secretin re-ceptor expression and secretin-stimulated ductal secretory ac-tivity is associated with enhanced biliary hyperplasia (2, 3, 22),whereas reduced secretory capacity in response to secretin is anindex of functional cholangiocyte damage (34, 36).
We next performed experiments in male rats aimed atdemonstrating that: 1) purified cholangiocytes and NRICCexpress 17�-HSD3 (the key enzyme regulating testosteronesynthesis) (20) and secrete testosterone and 2) testosteronestimulates in vitro the growth of NRICC by directly interactingwith ARs on cholangiocytes by an autocrine mechanism stim-ulating the expression of 17�-HSD3. The higher expression of17�-HSD3 and the enhanced secretion of testosterone bypurified cholangiocytes from BDL rats and BDL rats treated invivo with testosterone (that proliferate at higher rates) supportthe concept that testosterone (secreted by cholangiocytes) is atrophic autocrine hormone for sustaining biliary hyperplasia.The concept that testosterone stimulates biliary growth by anautocrine fashion is also supported by the fact that testosteroneincreases the mRNA expression of 17�-HSD3 in vitro inNRICC and flutamide (a specific antagonist of AR) and antit-estosterone antibody inhibit the growth of NRICC in vitro.Conclusive evidence that testosterone is an important autocrinetrophic factor sustaining biliary growth is also supported by thefinding that, in conditions of lowered serum testosterone levels(after castration and administration of neutralizing antitestos-terone antibody to BDL rats), there is enhanced testosteronesecretion likely by a compensatory mechanism. The possiblerole of testosterone as a key autocrine trophic was also sup-ported by knock down of 17�-HSD3, which caused a markeddecreased in NRICC proliferation. In support of our findings, anumber of studies demonstrate the presence of 17�-HSD3 inthe liver (41) and show that this enzyme isoform modulates thestimulatory effects on the mitosis of a number of cells, includ-ing cholangiocytes. This idea is supported by recent studiesshowing that specific inhibitors of 17�-HSD3 have been shownto inhibit hormone-dependent prostate cancer and benign pros-tate hyperplasia (12). The novel concept that cholangiocytesare secretory cells synthesizing a number of factors (including
G989TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
testosterone) regulating the homeostasis of the biliary epithe-lium is supported by a number of studies. For example,cholangiocytes synthesize a number of neuroendocrine factors,such progesterone, prolactin, vascular endothelial growth fac-tor, and nerve growth factor, that stimulate biliary growth (19,21, 23, 49). Also, serotonin inhibits biliary hyperplasia in BDLrats, since cholangiocytes secrete serotonin, the blockage ofwhich enhances cholangiocyte proliferation in the course ofcholestasis (42).
In summary, we have demonstrated the presence of func-tional ARs on cholangiocytes and that testosterone stimulatesbiliary growth by an autocrine mechanism by increasing theexpression of 17�-HSD3 in cholangiocytes. We have alsodemonstrated that testosterone prevents the decrease inbiliary hyperplasia typical of BDL after castration and theadministration of neutralizing antitestosterone antibody. Wepropose that drug targeting of 17�-HSD3 may be importantto regulate the balance between biliary proliferation/loss andductal secretory activity in cholangiopathies.
ACKNOWLEDGMENTS
We acknowledge Dr. G. Alpini for the isolation of cholangiocytes andhepatocytes and constructive suggestions during the development of theproject, Anna Webb and the Texas A&M Health Science Center MicroscopyImaging Center for their assistance with microscopy, Bryan Moss, MedicalIllustration, Scott & White, and the Animal Facility at Scott & White andTexas A&M Health Science Center College of Medicine for technical assis-tance.
GRANTS
This work was supported by National Institute of Diabetes and Digestiveand Kidney Diseases RO1 Grant DK-081442 awarded to S. Glaser and YaleMouse Metabolic Phenotyping Center Grant U24 DK-76169. This work waspartly supported by the Dr. Nicholas C. Hightower Centennial Chair ofGastroenterology from Scott & White to Dr. G. Alpini, Research Programmesof Significant National Interest funds 2005–2007 from the Italian Ministrodell’Istruzione, dell’Universita e della Ricera, Faculty funds from RomeUniversity “La Sapienza” to E. Gaudio, and by Health and Labor SciencesResearch Grants (from the Ministry of Health, Labor and Welfare of Japan) forthe Research on Measures for Intractable Diseases and Grant-in-Aid forScientific Research C (21590822) from the Japan Society for the Promotion ofScience to Y. Ueno.
DISCLOSURES
No conflicts of interest are declared by the authors.
REFERENCES
1. Alpini G, Glaser S, Robertson W, Phinizy JL, Rodgers RE, CaligiuriA, LeSage G. Bile acids stimulate proliferative and secretory events inlarge but not small cholangiocytes. Am J Physiol Gastrointest LiverPhysiol 273: G518–G529, 1997.
2. Alpini G, Glaser S, Ueno Y, Pham L, Podila PV, Caligiuri A, LeSageG, LaRusso NF. Heterogeneity of the proliferative capacity of rat cholan-giocytes after bile duct ligation. Am J Physiol Gastrointest Liver Physiol274: G767–G775, 1998.
3. Alpini G, Lenzi R, Sarkozi L, Tavoloni N. Biliary physiology in ratswith bile ductular cell hyperplasia. Evidence for a secretory function ofproliferated bile ductules. J Clin Invest 81: 569–578, 1988.
4. Alpini G, Phinizy JL, Glaser S, Francis H, Benedetti A, Marucci L,LeSage G. Development and characterization of secretin-stimulated se-cretion of cultured rat cholangiocytes. Am J Physiol Gastrointest LiverPhysiol 284: G1066–G1073, 2003.
5. Alpini G, Prall RT, LaRusso NF. The pathobiology of biliary epithelia.The Liver; Biology & Pathobiology (4th ed.), edited by Arias IM, BoyerJL, Chisari FV, Fausto N, Jakoby W, Schachter D, and Shafritz DA.Philadelphia, PA: Williams & Wilkins, 2001, p. 421–435.
6. Alvaro D, Alpini G, Onori P, Franchitto A, Glaser S, Le Sage G,Gigliozzi A, Vetuschi A, Morini S, Attili AF, Gaudio E. Effect of
ovariectomy on the proliferative capacity of intrahepatic rat cholangio-cytes. Gastroenterology 123: 336–344, 2002.
7. Alvaro D, Alpini G, Onori P, Perego L, Svegliata Baroni G, FranchittoA, Baiocchi L, Glaser S, Le Sage G, Folli F, Gaudio E. Estrogensstimulate proliferation of intrahepatic biliary epithelium in rats. Gastro-enterology 119: 1681–1691, 2000.
8. Alvaro D, Mancino MG, Glaser S, Gaudio E, Marzioni M, Francis H,Alpini G. Proliferating cholangiocytes: a neuroendocrine compartment inthe diseased liver. Gastroenterology 132: 415–431, 2007.
9. Angelsen A, Falkmer S, Sandvik AK, Waldum HL. Pre- and postnataltestosterone administration induces proliferative epithelial lesions withneuroendocrine differentiation in the dorsal lobe of the rat prostate.Prostate 40: 65–75, 1999.
10. Arenas MI, Perez-Marquez J. Cloning, expression, and regulation byandrogens of a putative member of the oxytocinase family of proteins inthe rat prostate. Prostate 53: 218–224, 2002.
11. Chang CS, Kokontis J, Liao ST. Structural analysis of complementaryDNA and amino acid sequences of human and rat androgen receptors.Proc Natl Acad Sci USA 85: 7211–7215, 1988.
12. Day JM, Tutill HJ, Foster PA, Bailey HV, Heaton WB, Sharland CM,Vicker N, Potter BV, Purohit A, Reed MJ. Development of hormone-dependent prostate cancer models for the evaluation of inhibitors of17beta-hydroxysteroid dehydrogenase type 3. Mol Cell Endocrinol 301:251–258, 2009.
13. DeMorrow S, Francis H, Gaudio E, Ueno Y, Venter J, Onori P,Franchitto A, Vaculin B, Vaculin S, Alpini G. Anandamide inhibitscholangiocyte hyperplastic proliferation via activation of thioredoxin 1/re-dox factor 1 and AP-1 activation. Am J Physiol Gastrointest Liver Physiol294: G506–G519, 2008.
14. Floreani A, Paternoster D, Mega A, Farinati F, Plebani M, Baldo V,Grella P. Sex hormone profile and endometrial cancer risk in primarybiliary cirrhosis: a case-control study. Eur J Obstet Gynecol Reprod Biol103: 154–157, 2002.
15. Fort P, Marty L, Piechaczyk M, el Sabrouty S, Dani C, Jeanteur P,Blanchard JM. Various rat adult tissues express only one major mRNAspecies from the glyceraldehyde-3-phosphate-dehydrogenase multigenicfamily. Nucleic Acids Res 13: 1431–1442, 1985.
16. Francis H, Glaser S, DeMorrow S, Gaudio E, Ueno Y, Venter J, DostalD, Onori P, Franchitto A, Marzioni M, Vaculin S, Vaculin B, Katki K,Stutes M, Savage J, Alpini G. Small mouse cholangiocytes proliferate inresponse to H1 histamine receptor stimulation by activation of the IP3/CaMK I/CREB pathway. Am J Physiol Cell Physiol 295: C499–C513,2008.
17. Francis H, Glaser S, Ueno Y, LeSage G, Marucci L, Benedetti A,Taffetani S, Marzioni M, Alvaro D, Venter J, Reichenbach R, Fava G,Phinizy JL, Alpini G. cAMP stimulates the secretory and proliferativecapacity of the rat intrahepatic biliary epithelium through changes in thePKA/Src/MEK/ERK1/2 pathway. J Hepatol 41: 528–537, 2004.
18. Francis H, Onori P, Gaudio E, Franchitto A, DeMorrow S, Venter J,Kopriva S, Carpino G, Mancinelli R, White M, Meng F, Vetuschi A,Sferra R, Alpini G. H3 histamine receptor-mediated activation of proteinkinase Calpha inhibits the growth of cholangiocarcinoma in vitro and invivo. Mol Cancer Res 7: 1704–1713, 2009.
19. Gaudio E, Barbaro B, Alvaro D, Glaser S, Francis H, Ueno Y,Meininger CJ, Franchitto A, Onori P, Marzioni M, Taffetani S, FavaG, Stoica G, Venter J, Reichenbach R, De Morrow S, Summers R,Alpini G. Vascular endothelial growth factor stimulates rat cholangiocyteproliferation via an autocrine mechanism. Gastroenterology 130: 1270–1282, 2006.
20. Geissler WM, Davis DL, Wu L, Bradshaw KD, Patel S, Mendonca BB,Elliston KO, Wilson JD, Russell DW, Andersson S. Male pseudoher-maphroditism caused by mutations of testicular 17 beta-hydroxysteroiddehydrogenase 3. Nat Genet 7: 34–39, 1994.
21. Gigliozzi A, Alpini G, Baroni GS, Marucci L, Metalli VD, Glaser S,Francis H, Mancino MG, Ueno Y, Barbaro B, Benedetti A, Attili AF,Alvaro D. Nerve growth factor modulates the proliferative capacity of theintrahepatic biliary epithelium in experimental cholestasis. Gastroenter-ology 127: 1198–1209, 2004.
22. Glaser S, Benedetti A, Marucci L, Alvaro D, Baiocchi L, Kanno N,Caligiuri A, Phinizy JL, Chowdury U, Papa E, LeSage G, Alpini G.Gastrin inhibits cholangiocyte growth in bile duct-ligated rats by interac-tion with cholecystokinin-B/Gastrin receptors via D-myo-inositol 1,4,5-triphosphate-, Ca(2�)-, and protein kinase C alpha-dependent mechanisms.Hepatology 32: 17–25, 2000.
G990 TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from
23. Glaser S, DeMorrow S, Francis H, Ueno Y, Gaudio E, Vaculin S,Venter J, Franchitto A, Onori P, Vaculin B, Marzioni M, Wise C,Pilanthananond M, Savage J, Pierce L, Mancinelli R, Alpini G.Progesterone stimulates the proliferation of female and male cholangio-cytes via autocrine/paracrine mechanisms. Am J Physiol GastrointestLiver Physiol 295: G124–G136, 2008.
24. Glaser S, Lam IP, Franchitto A, Gaudio E, Onori P, Chow BK, WiseC, Kopriva S, Venter J, White M, Ueno Y, Dostal D, Carpino G,Mancinelli R, Butler W, Chiasson V, DeMorrow S, Francis H, AlpiniG. Knockout of secretin receptor reduces large cholangiocyte hyperplasiain mice with extrahepatic cholestasis induced by bile duct ligation.Hepatology 52: 204–214, 2010.
25. Glaser SS, Gaudio E, Rao A, Pierce LM, Onori P, Franchitto A,Francis HL, Dostal DE, Venter JK, DeMorrow S, Mancinelli R,Carpino G, Alvaro D, Kopriva SE, Savage JM, Alpini GD. Morpho-logical and functional heterogeneity of the mouse intrahepatic biliaryepithelium. Lab Invest 89: 456–469, 2009.
26. Hinchliffe SA, Woods S, Gray S, Burt AD. Cellular distribution ofandrogen receptors in the liver. J Clin Pathol 49: 418–420, 1996.
27. Ishii M, Vroman B, LaRusso NF. Isolation and morphologic character-ization of bile duct epithelial cells from normal rat liver. Gastroenterology97: 1236–1247, 1989.
28. Jin H, Lin J, Fu L, Mei YF, Peng G, Tan X, Wang DM, Wang W, LiYG. Physiological testosterone stimulates tissue plasminogen activatorand tissue factor pathway inhibitor and inhibits plasminogen activatorinhibitor type 1 release in endothelial cells. Biochem Cell Biol 85:246–251, 2007.
29. Jorge AD, Stati AO, Roig LV, Ponce G, Jorge OA, Ciocca DR. Steroidreceptors and heat-shock proteins in patients with primary biliary cirrho-sis. Hepatology 18: 1108–1114, 1993.
30. Kanno N, LeSage G, Glaser S, Alpini G. Regulation of cholangiocytebicarbonate secretion. Am J Physiol Gastrointest Liver Physiol 281:G612–G625, 2001.
31. Kashiwagi B, Shibata Y, Ono Y, Suzuki R, Honma S, Suzuki K.Changes in testosterone and dihydrotestosterone levels in male rat acces-sory sex organs, serum, and seminal fluid after castration: establishment ofa new highly sensitive simultaneous androgen measurement method. JAndrol 26: 586–591, 2005.
32. Kato A, Gores GJ, LaRusso NF. Secretin stimulates exocytosis inisolated bile duct epithelial cells by a cyclic AMP-mediated mechanism. JBiol Chem 267: 15523–15529, 1992.
33. Kiani S, Valizadeh B, Hormazdi B, Samadi H, Najafi T, Samini M,Dehpour AR. Alteration in male reproductive system in experimentalcholestasis: roles for opioids and nitric oxide overproduction. Eur JPharmacol 615: 246–251, 2009.
34. LeSage G, Alvaro D, Benedetti A, Glaser S, Marucci L, Baiocchi L,Eisel W, Caligiuri A, Phinizy JL, Rodgers R, Francis H, Alpini G.Cholinergic system modulates growth, apoptosis, and secretion of cholan-giocytes from bile duct-ligated rats. Gastroenterology 117: 191–199,1999.
35. LeSage G, Glaser S, Gubba S, Robertson WE, Phinizy JL, Lasater J,Rodgers RE, Alpini G. Regrowth of the rat biliary tree after 70% partialhepatectomy is coupled to increased secretin-induced ductal secretion.Gastroenterology 111: 1633–1644, 1996.
36. LeSage G, Glaser S, Marucci L, Benedetti A, Phinizy JL, Rodgers R,Caligiuri A, Papa E, Tretjak Z, Jezequel AM, Holcomb LA, Alpini G.Acute carbon tetrachloride feeding induces damage of large but not smallcholangiocytes from BDL rat liver. Am J Physiol Gastrointest LiverPhysiol 276: G1289–G1301, 1999.
37. Luu-The V, Belanger A, Labrie F. Androgen biosynthetic pathways inthe human prostate. Best Pract Res Clin Endocrinol Metab 22: 207–221,2008.
38. Ma WL, Hsu CL, Wu MH, Wu CT, Wu CC, Lai JJ, Jou YS, ChenCW, Yeh S, Chang C. Androgen receptor is a new potential therapeutictarget for the treatment of hepatocellular carcinoma. Gastroenterology135: 947–955, 2008.
39. Mancinelli R, Onori P, Gaudio E, DeMorrow S, Franchitto A, FrancisH, Glaser S, Carpino G, Venter J, Alvaro D, Kopriva S, White M,Kossie A, Savage J, Alpini G. Follicle-stimulating hormone increases
cholangiocyte proliferation by an autocrine mechanism via cAMP-depen-dent phosphorylation of ERK1/2 and Elk-1. Am J Physiol GastrointestLiver Physiol 297: G11–G26, 2009.
40. Marcantonio D, Chalifour LE, Alaoui J, MAHTH, Alaoui-Jamali MA,Huynh HT. Steroid-sensitive gene-1 is an androgen-regulated gene ex-pressed in prostatic smooth muscle cells in vivo. J Mol Endocrinol 26:175–184, 2001.
41. Martel C, Rheaume E, Takahashi M, Trudel C, Couet J, Luu-The V,Simard J, Labrie F. Distribution of 17 beta-hydroxysteroid dehydroge-nase gene expression and activity in rat and human tissues. J SteroidBiochem Mol Biol 41: 597–603, 1992.
42. Marzioni M, Glaser S, Francis H, Marucci L, Benedetti A, Alvaro D,Taffetani S, Ueno Y, Roskams T, Phinizy JL, Venter J, Fava G,LeSage G, Alpini G. Autocrine/paracrine regulation of the growth of thebiliary tree by the neuroendocrine hormone serotonin. Gastroenterology128: 121–137, 2005.
43. McLachlan RI, Wreford NG, O’Donnell L, de Kretser DM, RobertsonDM. The endocrine regulation of spermatogenesis: independent roles fortestosterone and FSH. J Endocrinol 148: 1–9, 1996.
44. Ohnishi S, Murakami T, Moriyama T, Mitamura K, Imawari M.Androgen and estrogen receptors in hepatocellular carcinoma and in thesurrounding noncancerous liver tissue. Hepatology 6: 440–443, 1986.
45. Onori P, Wise C, Gaudio E, Franchitto A, Francis H, Carpino G, LeeV, Lam I, Miller T, Dostal DE, Glaser S. Secretin inhibits cholangio-carcinoma growth via dysregulation of the cAMP-dependent signalingmechanisms of secretin receptor. Int J Cancer 127: 43–54, 2010.
46. Rutenburg AM, Kim H, Fischbein JW, Hanker JS, Wasserkrug HL,Seligman AM. Histochemical and ultrastructural demonstration of �-glu-tamyl transpeptidase activity. J Histochem Cytochem 17: 517–526, 1969.
47. Shidham VB, Komorowski RA, Machhi JK. Androgen receptor expres-sion in metastatic adenocarcinoma in females favors a breast primary(Abstract). Diagn Pathol 1: 34, 2006.
48. Stubbs AP, Engelman JL, Walker JI, Faik P, Murphy GM, WilkinsonML. Measurement of androgen receptor expression in adult liver, fetalliver, and Hep-G2 cells by the polymerase chain reaction. Gut 35:683–686, 1994.
49. Taffetani S, Glaser S, Francis H, DeMorrow S, Ueno Y, Alvaro D,Marucci L, Marzioni M, Fava G, Venter J, Vaculin S, Vaculin B, LamIP, Lee VH, Gaudio E, Carpino G, Benedetti A, Alpini G. Prolactinstimulates the proliferation of normal female cholangiocytes by differen-tial regulation of Ca2�-dependent PKC isoforms (Abstract). BMC Physiol7: 6, 2007.
50. Tanaka K, Sakai H, Hashizume M, Hirohata T. Serum testosterone:estradiol ratio and the development of hepatocellular carcinoma amongmale cirrhotic patients. Cancer Res 60: 5106–5110, 2000.
51. Tsai-Morris CH, Khanum A, Tang PZ, Dufau ML. The rat 17beta-hydroxysteroid dehydrogenase type III: molecular cloning and gonadotro-pin regulation. Endocrinology 140: 3534–3542, 1999.
52. Tsega E, Nordenfelt E, Hansson BG, Mengesha B, Lindberg J. Chronicliver disease in Ethiopia: a clinical study with emphasis on identifyingcommon causes. Ethiop Med J 30: 1–33, 1992.
53. van der Merwe SW, van den Bogaerde JB, Goosen C, Maree FF,Milner RJ, Schnitzler CM, Biscardi A, Mesquita JM, Engelbrecht G,Kahn D, Fevery J. Hepatic osteodystrophy in rats results mainly fromportasystemic shunting. Gut 52: 580–585, 2003.
54. Van Thiel DH, Gavaler JS, Zajko AB, Cobb CF. Consequences ofcomplete bile-duct ligation on the pubertal process in the male rat. JPediatr Gastroenterol Nutr 4: 616–621, 1985.
55. Ward GR, Abdel-Rahman AA. Effect of testosterone replacement orduration of castration on baroreflex bradycardia in conscious rats (Ab-stract). BMC Pharmacol 5: 9, 2005.
56. Weibel ER, Staubli W, Gnagi HR, Hess FA. Correlated morphometricand biochemical studies on the liver cell. I. Morphometric model, stereo-logic methods, and normal morphometric data for rat liver. J Cell Biol 42:68–91, 1969.
57. Yoshioka K, Sasaki M, Imai S, Tsujio M, Taniguchi K, Mutoh K.Testicular atrophy after bile duct ligation in chickens. Vet Pathol 41:68–72, 2004.
G991TESTOSTERONE REGULATION OF CHOLANGIOCYTE PROLIFERATION
AJP-Gastrointest Liver Physiol • VOL 301 • DECEMBER 2011 • www.ajpgi.org
by 10.220.33.5 on October 29, 2017
http://ajpgi.physiology.org/D
ownloaded from