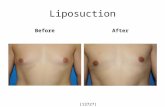
Breasts Cancer
21
-
Upload
nikhilvartaks -
Category
Health & Medicine
-
view
33 -
download
1
Transcript of Breasts Cancer