Bile duct injuries in Laparocsopic cholecystectomy
-
Upload
ucms-th-bhairahwa-nepal -
Category
Education
-
view
2.024 -
download
8
description
Transcript of Bile duct injuries in Laparocsopic cholecystectomy

Biliary Injuries During
Laparoscopic Cholecystectomy
Dr.Atul kumar Mishra M.S (Gen.Surgery)

Historical perspective First planned cholecystectomy in the
world was performed by Carl Langenbuch in 1882.
First choledochotomy was performed by Couvoisser in 1890.
First iatrogenic bile duct injury was described by Sprengel in 1891.
Prof. Dr. Med Erich Muhe of Boblingen, Germany, performed the first laparoscopic cholecystectomy in 1985.

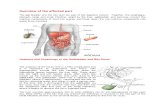
Biliary Anatomy
a. Right hepatic duct.b. Left hepatic duct.c. Common hepatic duct.d. Portal vein.e. Hepatic artery.f. Gastroduodenal artery.g. Right gastroepiploic artery.h. Common bile duct.i. Fundus of the gallbladder.j. Body of the gallbladder.k. Infundibulum.l. Cystic duct.m. Cystic artery.n. Superior pancreaticoduodenal artery.
Schwartz’s Principles of Surgery, 8th Ed.,McGraw-Hill Companies, 2005.

Stewart et al. Bile Duct Injuries During Laparoscopic Cholecystectomy
Classic anatomy of biliary tree is present in only 30% of individuals, so it may be said that anomalies are rule, not
the exception. ( Maingot’s abdominal operations)

Anatomy
Calot's triangle bounded by cystic duct,
cystic artery, and common hepatic duct.
Hepatocystic triangle bounded by gallbladder wall and cystic duct, liver edge, and common hepatic duct; the cystic artery (and hence Calot's triangle) lies within this space.
(Maingot’s abdominal operation)

Aim of the laparoscopic cholecystectomy
Surgery (TODAY)->Discharge on same/next day
Complicated / InjuryLong hospital stayRepeated investigations like USG and ERCPRadiologic interventionsRe-operations

Laparoscopic cholecystectomy Pros and cons
General advantages Shorter stay in hospital Faster recovery period Reduced post-op recovery time Less postoperative pain Improved cosmetic outcome
Disadvantage Increase in serious bile duct
complications and injuries

• Reverse Trendelenburg (30 degrees) with left arm out at 90 degrees relative to the body’s axis
• Titled left 15 degrees after optical trocar placement
Operating Room Setup

Trocar PlacementEpigastric region, below XP
Mid-A, between 12th rib and iliac crest
Subcostal, Mid-Clavicular Umbilical
region

Introduction Open cholecystectomy was standard practice for
treatment of symptomatic gall bladder disease until late 1980’s.
At present 90% of cholecystectomies performed by LC which is one of the commonest surgical procedure in world.
Unfortunately, widespread application of LC led to concurrent rise in incidence of major bile duct injuries (BDI),which are more complicated than after open procedures.
Since its introduction and routine use in 1990s, the incidence of biliary injuries has doubled from 0.2% to 0.4% and remained constant despite advances in knowledge, technique, and technology.

Mistaking common bile duct for the cystic duct
Classic Laparoscopic Injury

Inappropriate use of electrocautery near biliary ducts
May lead to stricture and/or bile leaks
Mechanical trauma can have similar effects
Thermal Injuries
Lahey Clinic, Burlington, MA.1994

Bile duct injuries during cholecystectomy
In 1990s, high rate of biliary injury was due to learning curve effect.
Surgeon had 1.7% chance of a bile duct injury occuring in first case and 0.17% at the 50th case.
However most surgeons passed through learning curve, steady – state reached, but there has been no significant improvement in the incidence of biliary duct injuries.

Biliary Injuries during Cholecystectomy
Open cholecystectomy has been associated historically with 0.2% to 0.5% risk of postoperative Biliary tract injuries.
On other hand LC has been associated with 2.5-fold to 4-fold increase in the incidence of postoperative BDI compared with OC.

These preventable injuries can be devastating, increasing morbidity, mortality, and medical cost, while decreasing the patient’s quality of life.
Biliary injuries will always exist, and we need to be aware of the best methods to avoid, evaluate, and treat them.

Incidence of IBDI following cholecystectomy (%)
Author IBDI incidence following OC
IBDI Incidence following LC
Mc Mohan et al,1995 0.2 0.81
Strassberg et al, 1995 0.07 0.5
Shea et al,1996 0.19-0.29 0.36-0.47
Targarona et al, 1998 0.6 0.95
Lillemoe et al, 2000 0.3 0.4-0.6
Gazzaniga et al, 2001 0.0-0.5 0.07-0.95
Savar et al,2004 0.18 0.21
Moore et al,2004 0.2 0.4
Misra et al,2004 0.1-0.3 0.4-0.6
Gentileschi et al,2004 0.0-0.7 0.1-1.1
Kaman et al,2006 0.3 0.6

Risk Factors for Biliary tract injury
Surgeon related factors Lack of experience (learning curve) Misidentification of biliary anatomy Intraoperative bleeding Lack of recognition of anatomical
variations of biliary tree Improper interpretation of IOC Improperly functioning equipment

Risk for biliary tract injury
Patient related Acute and chronic cholecystitis Empyema Long standing recurrent disease ->
fibrosis Porcelain gallbladder Obesity Previous surgery Male sex Advanced age

The Effect of Acute Cholecystitis on Lap. cholecystectomy
complications Complication rate three times
greater than for elective LC. Early cholecystectomy (72 h)
outcome better than delayed cholecystectomy.
Conversion rate to open cholecystectomy is higher than elective cholecystectomy 35% vs 9%.

Risk Factors for biliary tract injuries Anatomic Variations
Present in 18 – 39% cases Dangerous variations predisposing to BTI are present in only 3-6% of cases
Abnormal biliary anatomy
Short cystic duct, cystic duct entering in the right duct- Accessory right hepatic duct
Arterial anomalies Right hepatic artery
running parallel to the cystic duct
Anomalous or accessory right hepatic artery

(Sabiston text book of surgery 19thedtn.)


Summary of Causes of Bile Duct Injuries
Misidentification of Common bile duct Common hepatic duct An aberrant duct (usually on the right side)
Technical failure such as Slippage of clips placed on the cystic duct Inadvertent thermal injury to CBD Tenting of CBD during clip placement Disruption of a bile duct entering directly into gallbladder fossa .
(Goal of dissection should be conclusive identification of cystic structure within Calot triangle)
(If the cystic duct and cystic artery are conclusively and correctly identified before dividing, more than 70% of bile duct injuries would be avoided )

Technique Four methods of identification of cystic
structures during cholecystectomy
1) Routine cholangiography2) Critical view technique3) Infundibular technique-> widely used4) Dissection of main bile duct with visualization
of cystic duct or common duct insertion->
( increased chance of either thermal or retraction injury to CBD, aberrant insertion
of cystic duct can also complicate this approach)

Routine intra-op cholangiogram (IOC)Laparoscopic ultrasonography
Performed routinely or not ?
Done via presumed cystic duct
If this happens to be CBD, injury has already occurred!!
IOC does not identify all aberrant ducts
Arterial anatomy not identified
IOC does not prevent BDI but may reduce its severity ( if correctly performed & interpreted, IOC can prevent complete CBD transection)
IOC higher rate of intra-op identification of BDI decreased cost of treatment & shorter hospital stay

If critical view not obtained due to inflamation or hostile anatomy perform IOC prior to dividing cystic duct .Routine IOC reduces CBD injuries from 0.58% to 0.39% (American Medicare data base study)

Critical view of safety
Calot’s triangle dissected free of all tissue except cystic duct & artery
Base of liver bed exposed When this view is
achieved, the two structures entering GB can only be cystic duct & artery
Not necessary to see CBD

Infundibular technique, although widely used, is prone to failure in situations where cystic duct is hidden because of diffuculty retracting the gallbladder as a result of severe inflammation or one or more large stone effacing or fusing the cystic duct-common duct junction.
In such situation, area where infundibulum narrows can be interpreted to be cystic duct when it is actually the cystic duct and common duct together.

(A)Usual anatomy when infundibular technique applied. Cyst duct-gallbladder junction is characterized by a flaring tunnel shape(boldlines). Arrow represents circumferential dissection of CD-gallbladder junction during infundibular technique.
(B) Inflammation can pull CBD on the gallbladder creating similar flaring tunnel shape. As a result, CBD mistaken for cystic duct, resulting in classic injuries.
CD, cystic duct;CHD, common hepatic duct. (Strasberg S. Error traps and vasculo-biliary injury in laparoscopic and open cholecystectomy. J Hepatobiliary Pancreat Surg 2008;15(3):285;)

Cystic duct or CBD?2 – 3mm wide 5mm wide CD > 5mm – Is it CBD?
Even with low cystic duct insertion, CD rarely goes behind duodenum
CBD goes behind duodenum
Duct behind duodenum must be CBD
Double cystic duct very rare
-- 2 ducts seem to go towards inflammed Gallbladder – one must be CBD
No vessels on surface
Vessels on surface
--

Classical LC BDI

Type A Cystic duct leaks or leaks from small ducts in liver bed
Type B Occlusion of aberrant right hepatic ducts
Type C Transection of aberrant right hepatic ducts
Type D Partial (<50%) transection of major bile duct
Type E Transection involve >50%
Subdivided as per Bismuth classification into E1 to E5
Strasburg Classification

E: injury to main duct (Bismuth)
E1: Transection >2cm from confluence
E2: Transection <2cm from confluence
E3: Transection in hilum E4: Seperation of major
ducts in hilum E5: Type C plus injury in
hilum
Strasburg Classification, cont’d

Class I CBD mistaken for cystic duct, but error recognized before CBD is divided.Class II Damage to CHD from clips or cautery placed on duct. Often occurs where visibility is limited due to inflammation or bleeding.Class III Most common (60%), CBD mistaken for cystic duct. Common duct is transected and variable portion that includes junction of cystic and common duct is excised .Class IV Damage to right hepatic duct , either because this structure is mistaken for cystic duct, or injured during dissection.

Bile duct injury
Prevention should be main point (much more important than treatment)
ALL laparoscopic cholecystectomies ARE difficult! None of them is easy!
If injury occurred, …who should treat it?when should it be treated?how should it be treated?

Prevention 30° laparoscope, high quality imaging equipment Firm cephalic traction on fundus & lateral
traction on infundibulum, so cystic duct perpendicular to CBD
Dissect infundibulo-cystic junction Expose “Critical view of safety” before dividing
cystic duct Convert to open, if unable to mobilise
infundibulum or bleeding or inflammation in Calot’s triangle
Routine intra-op cholangiogram Intraoperative laparoscopic ultrasound (IOUS) .
Mastery of Surgery 6th ed.

Changing the Culture of Cholecystectomy: Stopping Rules
Safety and avoiding BDI should be paramount concern to surgeon performing LC.
LC can be converted to open procedure or even aborted if local conditions present unacceptable risks of danger.
As Strasberg points out, the negative effects of conversion or even aborting procedure and placing a cholecystostomy tube are minor compared with the negative effect of a BDI.
Failure of progression of dissection, inability to grasp and retract gallbladder, anatomic ambiguity, poor visualization of field due to hemorrhage, should trigger the surgeon to consider alternate approach.
Conversion rate < 5% can be expected in hands of a well trained laparoscopic surgeon.

Timing of Identification
• Intra-op
• Unexpected ductal structures seen• Bile leak into field from lacerated or
transected duct
• Post-op
• Depends on continuity of bile duct & • Presence or absence of bile leak

Presentation of Bile Duct Injuries
About 25% recognized intraoperatively. About 25% discovered within 24 hours post- operative About 50% present weeks to years post-operative. Most BDI are not recognized intraoperatively, and patients sent
home after or within 24 hours. Patients who fails to recover within first few days or develop
progressive vague abdominal symptoms. Abdominal fullness, distension, nausea, vomiting, abdominal pain,
fever and chills. Symptoms can leads to bilomas, biliary fistula, cholangitis, sepsis,
or multi organ system failure. Clinical presentation- Biliary obstructions-> anorexia, jaundice, liver enzyme
elevation Bile leaks Both can occur simultaneously Concomitant vascular injuries (complicate matter) Obstruction secondary to biliary stricture appear weeks to month
later and may present with recurrent colangitis, obstructive jaundice, or secondary biliary cirrosis.

If experienced, convert to Open Procedure and perform Cholangiography (determine extent of injury)
If not experienced, perform cholangiogram laparoscopically with intent of referring patient (placement of drains)
Consult an experienced hepatobiliary surgeon
Quicker the repair, better the outcome!!!
Acute Management Biliary catheter for decompression of biliary
tract and control of bile leaks Percutaneous drainage of intraperitoneal bile
collection
Intraoperative Detection

Clinical Presentation (post-op)
• Obstruction• Clip ligation or resection of CBD
obstructive jaundice, cholangitis
• Bile Leak• Bile from intra-op drain or• More commonly, localized biloma or
free bile ascites / peritonitis, if no drain• Diffuse abdominal pain & persistent
ileus several days post-op high index of suspicion possible unrecognized BDI

Controlling sepsis, establish biliary drainage, postulate diagnosis, type and extent of bile duct injury.
Broad-spectrum antibiotics No need for an urgent laparotomy. Biliary
reconstruction in presence of peritonitis results a statistically worse outcome.
No need for urgent with reconstruction of biliary tree. Inflammation, scar formation and development of fibrosis take several weeks to subside.
Reconstruction of biliary tract is best performed electively after interval of at least 6 to 8 weeks.
Post-Operative Detection Plan

Investigation Ultrasonagraphy and CT -- Ductal dilatation
intra-abdominal collection and dilatation of biliary tree.
Cholangiogram ERCP—biliary anatomy and assess the
injury PTC—define biliary anatomy proximal to
injury MRCP—noninvasive (can miss minor
leaks)
HIDA scan -- If doubt exists, HIDA scan can confirm leak but not the specific leak site
MR angiography—vascular injuries
BDI Management

When realise that there is an injury, ASK for HELP!
If possible do not try to repair, even you are experienced
An experienced and FRESH surgeon should repair the injury.
If it is impossible AND it is a difficult injury that you can not treat, place catheters and refer the patient.There is no ‘Tissue Lost’, primary repair (end to end CBD repair) over T-tube???
stricture rate is high!!!
There is ‘Tissue Lost’, biliodigestive anastomosis:
choledocoduodenostomy/ Roux-en-Y hepaticojejunostomy Primary repair high incidence of failure percutaneous or endoscopic balloon dilatation later

Preoperative Investigation and Preparation for the Procedure
■ Communication with previous surgeon■ Previous surgical report■ Laboratory tests: bilirubin, alkaline phosphatase, ALT, AST, albumin, coagulation parameters, white blood cell count
Principles of Repair ■ Anastomosis should be tension free, with good
blood supply, mucosa to mucosa and of adequate caliber.■ Hepaticojejunostomy should be used in preference to either choledochocholedocotomy or choledochoduodenostomy.■ Anterior longitudinal opening in the bile duct with a long side-to-side anastomosis is preferred.■ Dissection behind the ducts should be minimized in order to minimize devascularization of the duct.

Timing of RepairFactors favoring immediate repair are: (1) Early referral (2) Lack of right upper quadrant bile collection (3) Simple injuries (4) No vascular injury and (5) Stable patient Factors favoring delayed repair are: (1) Late (less than 1week after injury) referral (2) Complex injuries (types E4, E5) (3) Thermal etiology (4) Concomitant ischemic injury

Strasburg classification
Type A
No reconstructionTreated endoscopicaly
Type B & CPotentialy serious injuriesMore common since introduction of LC
Type B
Silent
Asymptomatic atrophy of involved liverCompensated by hypertrophy of normally drained liver
Pain or cholangitis many yrs. after injury
Type C
Biliary fistula
Volume less
Converted to silent Type B
Persistence
Reconstruction
Type D
<25%
25% - 50% or Caused by diathermy orSmall bile duct
Type E (>50%)
Repaired primarily Over T-tube
Reconstruction by hepaticojejunostomy
B,C and E1 to E5 are major biliary injuries

ERCP – multiple stents
• Lateral duct wall injury or cystic duct leak transampullary stent controls leak & provides definitive treatment
• Distal CBD must be intact to augment internal
drainage with endoscopic stent

Simpler injuries types A and D may be treated in
community
setting when discovered intraoperatively by endoscopic or
percutaneous techniques when they present in postoperative
period.
More complex injuries that require hepaticojejunostomy
for repair (types B and C injuries and most to type E
injuries).
More complex injuries types E1 and E2 may also be treated
by nonsurgical techniques when they present as
strictures.
Notations >2 cm and <2 cm in types E1 and E2 indicate
length of common hepatic duct remaining.

Bile leak
Immediate intra operative diagnosis
Delayed diagnosis
injurMinor y Major injury
Repair over T-tube
No experienced hepato-Biliary surgeon Clip open ductDrainIV antibioticsTransfer to tertiary centre
Experienced hepatobiliary surgeon available
Call second surgeonRoux-en-Y hepatico-jejunostomy
Drainage
Low -output High-output
Observe
Resolve < 5-7 daysContinued ERCP
Duct of Luschka
Cystic duct stump leak
Suspected CBD injury
SphinctrectomyStent± sphincterectomy
PTC to deliniate anatomyControl drainageRepair by experienced hepatobiliary surgeon

Cholangiography (ERCP + PTC)
Percutaneous transhepatic cholangiography (PTC)
Defines proximal anatomy
Allows placement of percutaneous transhepatic biliary catheters to decompress biliary tree treats or prevents cholangitis & controls bile leak

ERCP – clips across CBD
CBD transection normal-sized distal CBD upto site of transection
Percutaneous transhepatic cholangiography (PTC) necessary
Surgery

Intraoperative repair

Surgical repairCholedocho-choledochostomy

Surgical repair Choledocho-duodenostomy

Biliary enteric anastomosis Most laparoscopic
BDI – complete discontinuity of biliary tree
Surgical reconstruction, Roux-en-Y hepaticojejunostomy
Tension-free, mucosa-to-mucosa anastomosis with healthy, nonischemic bile duct

Surgical repair Hepatico-jejunostomy (Roux-en-Y)

Definitive management Goal
Reestablishment of bile flow into proximal GIT
In a manner that prevents cholangitis, sludge or stone formation, restricturing & progressive liver injury
Bile duct intact & simply narrowed percutaneous or endoscopic dilatation

Treatment summary Strasberg Type A – ERCP +
sphincterotomy + stent
Type B & C – Traditional surgical hepaticojejunostomy
Type D – Primary repair over an adjacently placed T-tube (if no evidence of significant ischemia or cautery damage at site of injury)
More extensive type D & E injuries –
Roux an-Y hepaticojejunostomy over a 5-F pediatric feeding tube to serve as a biliary stent

Summary
• Multidisciplinary management of BDI expertise of surgeons, radiologists & gastroenterologists
• Mismanagement lifelong disability & chronic liver disease
• BDI with lap. Chole results of operative repair, excellent in Specialist Centres