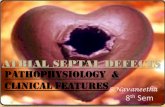
Atrial Septal Defects with Severe Pulmonary Hypertension
Transcript of Atrial Septal Defects with Severe Pulmonary Hypertension

Dr. Mazeni Alwi
Institut Jantung Negara (National Heart Institute)
Kuala Lumpur
Atrial Septal Defects with Severe Pulmonary Hypertension: Shall I close
it? How to close it?
4th Asia Pacific Congenital & Structural Heart Intervention Symposium 2013
Hong Kong

Pulmonary arterial hypertension (PAH): Definition
• mean pulmonary artery pressure of > 25 mmHg at rest • normal pulmonary artery wedge pressure <15mm Hg
4th world symposium of PAH 2008, Dana point
Diagnosis and assessment of PAH Badesch et al , J. Am. Coll. Cardiol. 2009;54;S55-S66
Pulmonary vascular resistance > 3 woods unit

Definition of severe PHT ?
Not clinically Eisenmenger’s Still left right shunt of colour Doppler
Limitations of measuring PVR and Qp:Qs based on Fick’s formula by oxymetry
Mean PA pressure Mean Ao pressure
> ? 0.75 > ? 0.9

MacDonald ST et al. Heart, March 2011 Vol 97 No 5



• ? Why patients with same degree of PAH demonstrate individual differences in symptoms, natural Hx and responses to treatment
• PDA and VSD with severe PHT behave differently from
ASD? • Confounding issue – ? Is primary/iPHT the main issue
and ASD is co-incidental
Problems with Congenital Heart Disease Left Right Shunt

10 year old male Moderate – large ASD “Eisenmenger’s” features at 6 years of age ? 1° PHT

45 years, female Very large ASD PA pressure 80% systemic ~ still left right shunt

• Determine those with PAH-CHD whose lesion is still operable/have reversible pulmonary vascular disease
• How to accurately determination of degree of pulmonary vasoreactiviy/reversibility?
Management Dilemma
• Choose not to close : Patient may progress to Eisenmenger syndrome • Choose to close : Risk of progressive pulmonary vascular disease right heart failure, premature death

How to decide? Evaluation of operability
• Systematic approach
• Combination of clinical & investigative information
• Clinical, ECG, CXR
• Degree of left - right shunt echocardiogram
haemodynamic calculation
• Response to pharmacological vasodilation
(inhaled NO, 100% oxygen or inhaled illoprost)
• Lung biopsy (microscopic finding)

No/mild PAH Moderate-severe PAH
Very severe PAH
Qp: Qs > 2.0 1.5-2.0 < 1.5
Pulmonary vascular resistance ( wood unit)
< 3 >4- 10 > 10
Vasodilator test positive variable negative
Difficult /controversial What value of PVR?
Risk of post operation pulmonary hypertensive crisis Long term risk of progressive pulmonary vascular disease
ASD and PAH : Decision to close

PAH-CHD : IJN experience
• Since 2005 sildenafil used to prime pulmonary bed
• Children & Adults
• CHD (simple ASD, VSD & PDA)
• Pulmonary arterial hypertension PVR 4-?15 woods unit, ( the cut off PVR limit
reduced with time and experience) Mean pulmonary artery pressure to aortic
pressure ratio PA: Ao > 0.5 (ASD) or > 0.8 for VSD, PDA
Qp:Qs ratio 1.5-2

Methods Medical history, P/E
CXR ,ECG, 2 DE
Baseline 6 min walk test
Cardiac catheterization
Baseline ocular test
Sildenafil 50mg tds or 1-2 mg/kg/day
Clinical review
6 min walk test, 2DE
3 months
6 months
Repeat Cardiac catheterization, acute vasoreactivity test dobutamine stress
Trial occlusion/ fenestrated closure of defect/surgical closure
PVR > 4- ?10 w/u PA : Ao >0.5 0r > 0.8
Pre 2005, no sildenafil
Contraception
NT pro BNP

Vasodilator and Stress challenge
• Nebulised Illoprost 20mcg • Omron nebuliser • 15 mins post nebulising : restudy • 100% 0xygen or iNO ( ventilated patients) • Dobutamine stress to achieve 80% targeted heart rate
Positive vasodilator challenge During acute vasodilator testing (with NO, PgI2 or adenosine)
Decrease in mPAP >10 mmHg To reach a mPAP < 40 mmHg With a normal or a high cardiac output

Transcatheter trial occlusion
• Trial of transcatheter occlusion with device • Monitor hemodynamics for 24-48 hours, device still attached
to cable • If stable, release device • If unstable, remove device
(Mainly applicable to PDA, very few ASD cases due to large defect size)


Post procedure
• Surgical patients Precautions during induction, and post op care. (inotropes, ventilation, PAH drugs (iNO ) • Sildenafil continued at least up to 1 year post closure until
repeat cardiac catheterization • Monitor for progression of pulmonary vascular obstructive
disease Clinical, 6MWT, Echo, NT pro BNP • Repeat cardiac catheterization at 1 year, 3-5 years

25 patient enrolled
Baseline cath
trial closure n=23
Suprasystemic PAP
Not Close n=2
SILDENAFIL (7)
PDA close n=18 FAILED
6M post sildenafil n=8, non sildenafil n=15
SURGERY
NONE (11)
SILDENAFIL (10) NO sildenafil (15)
n=2
n=1
Follow up: Alive n=6 Died n=1
Follow up: Alive n= 7 Died n=3 Defaulted n=3
PDA size (mm): 9.93 ± 2.95 Device Use : ASO (n=10) ADO (n=8)
PDA with PHT

0.00
20.00
40.00
60.00
80.00
100.00
PRE SILDENAFIL 6 MONTHS SILDENAFIL
1 YEAR POST 3 YEARS POST 5 YEARS POST
Mean PA
NO
YES
0.00
0.10
0.20
0.30
0.40
0.50
0.60
0.70
0.80
0.90
1.00
PRE SILDENAFIL 6 MONTHS SILDENAFIL
1 YEAR POST 3 YEARS POST 5 YEARS POST
PA:Ao
NO
YES
PDA-PAH :Post occlusion Sildenafil pre occlusion vs no sildenafil

ASD with PAH : IJN experience
• Prospective • Adults > 18yrs • Moderate size secundum ASD (>2cm) • Pulmonary arterial hypertension (PVR 4-10 woods unit, mean pulmonary artery pressure
to aortic pressure ratio > 0.5 (PA: Ao), Qp:Qs ratio <2) • Not clinically Eisenmenger’s
Objective • Review the effect of 6 months of sildenafil 50mg tds on
the hemodynamic parameters • Outcome of closure/fenestration of ASD

ASD and PAH: IJN Experience
Patient on Sildenafil No closure ASD occlusion Fenestrated closure
TOTAL no of patient 14 3 12
AoP (mmhg) 93+21.3 76.7+17.62 91,8+10.5
PAP(mmhg) 54.3+9.21 48.7+16.3 48.9+4.9
PA:Ao 0.66+0.15 0.72+0.26 0.59+0.11
Qp:Qs 1.92+0.43 2.22+1.02 2.35+0.91
Ao Sat (%) 94+6.5 98.3+1.2 96+1.56
PVR (woods unit) 8.24+3.91 6.02+2.1 7.29+2.28
RESULTS
No procedure (n=14) Progression of PHT
Cath 2 – 6 months post Sildenafil n=29
ASD with PAH (n=32) Cath 1 - pre Sildenafil
Suitable for Fenestrated ASD closure (n= 12)
ASD occlusion (n=3) by device
Defaulted n= 3
PVR <8 woods unit Consider closure


HAEMODYNAMICS 3.02.2012 14.09.2012
Room air Post Illoprost Room air Post Illoprost
Qp:Qs 2.2:1 2.4:1 2.46:1 2.39:1
PVR( woods unit) 10.8 16.3 8.29 8.56
3.02.2012 14.09.2012 (post Sildenafil)
Surgical closure with fenestration

ASD and PAH: IJN Experience
OUTCOME
No procedure
(n=15)
Fenestrated ASD closure (n= 12)
ASD occlusion (n=3)
1 died (after 1 year
post closure)
2 died after 3 years sildenafil
11 fenestrated closure
(1 abandoned)
n=1

ASD and PAH: IJN Experience
OUTCOME ON FOLLOW UP
Patients post fenestration had lower PVR and mean PA pressure compared to those closed
Duration follow up YEAR SD
NONE 2.37 1.81
FENESTRATED 2.45 1.22
CLOSE 3.22 1.13

0
10
20
30
40
50
60
70
PRE 6 MONTHS 1 YEAR POST 3 YEARS POST
ME
AN
PA
PA PRESSURE
NAB
PSP
AM
NS
NR
BAJ
FMS
NA
NJ
MM
WNW
FENESTRATED - CATH
Fenesterated ASD Closure
0
0.1
0.2
0.3
0.4
0.5
0.6
0.7
0.8
0.9
PRE 6 MONTHS 1 YEAR POST 3 YEARS POST
PA
:AO
PA:AO RATIO
NAB
PSP
AM
NS
NR
BAJ
FMS
NA
NJ
MM
PA:Ao
RATIO PRE 6M 1Y POST
NS 0.82 0.67 0.77
NAB 0.53 0.53 0.56

Summary
Secundum ASD with severe PHT
• Very difficult management decision No agreed definition (? pre-Eisenmenger’s, PA/Ao pressure > 0.6) Limitations of current methods of evaluation • Role of vasodilator therapy to prime pulmonary vascular bed
before intervention
Intervention
• Selected cases after detailed evaluation – clinical, echo, haemodynamics pre and post vasodilator
Rigorous counselling and consent process • Surgical closure with fenestrated patch for suitable cases • Limited role of device closure (usually very large defects) • ? Role of individualized device size with fenestration