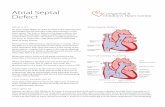
Atrial Septal Defect Kendra Marsh, MD Division of Cardiology, UIC Fellow.
-
Upload
precious-imes -
Category
Documents
-
view
219 -
download
3
Transcript of Atrial Septal Defect Kendra Marsh, MD Division of Cardiology, UIC Fellow.
Atrial Septal DefectAtrial Septal Defect
Kendra Marsh, MDKendra Marsh, MD
Division of Cardiology, UICDivision of Cardiology, UIC
FellowFellow
EmbryologyEmbryology
Gestational Week 4 Gestational Gestational Week 4 Gestational Week 4-6 • Week 4-6 •
A thin, crescent shaped wedge A thin, crescent shaped wedge of tissue of (septum primum) of tissue of (septum primum) grows towards and fuses with grows towards and fuses with endocardial cushions. endocardial cushions.
The remaining opening is called The remaining opening is called the ostuim primum. • the ostuim primum. •
As the septum primum is As the septum primum is growing down, the endocardial growing down, the endocardial cushions fuse and the ostium cushions fuse and the ostium primum is eventually obliterated. primum is eventually obliterated.
EmbryologyEmbryology The interatrial septum forms The interatrial septum forms
during the first and second during the first and second months of months of fetal developmentfetal development. .
Stage I is the formation of the Stage I is the formation of the septum septum primumprimum..
The septum primum walls off a The septum primum walls off a crescent-shaped portion of the crescent-shaped portion of the hole between the right and left hole between the right and left atria.atria.FFooramen ramen primumprimum (also called (also called the the ostiumostium primumprimum) stays open) stays open
The remaining part of the The remaining part of the opening between the right and opening between the right and left atria is closed by the left atria is closed by the septum septum secundumsecundum. .
The 2 tissue layers overlap like The 2 tissue layers overlap like a flap, allowing blood flow to a flap, allowing blood flow to continue during fetal life.continue during fetal life.
Changes in circulation at Changes in circulation at birthbirth, , closes the flap permanently.closes the flap permanently.
Anatomy and PhysiologyAnatomy and Physiology
Extends from cavo-Extends from cavo-atrial junction with atrial junction with superior and inferior superior and inferior vena cavaevena cavae
Ends near the atrio-Ends near the atrio-ventricular canal near ventricular canal near the tricuspid valvethe tricuspid valve
Ostium SecundumOstium Secundum
Most common type of Most common type of ASDASD
Center of the septum Center of the septum between the right and between the right and left atriumleft atrium
Variant of this type of Variant of this type of ASD is called a Patent ASD is called a Patent Foramen Ovale (PFO) Foramen Ovale (PFO) which is very small. which is very small.
Ostium PrimumOstium Primum
Next most common type Next most common type
Located in the lower portion of Located in the lower portion of the atrial septum. the atrial septum.
Will often have a mitral valve Will often have a mitral valve defect associated with it called a defect associated with it called a mitral valve cleft. mitral valve cleft.
A mitral valve cleft is a slit-like A mitral valve cleft is a slit-like or elongated hole usually or elongated hole usually involves the anterior leaflet of involves the anterior leaflet of the mitral valve. the mitral valve.
Sinus VenosusSinus Venosus Least common type of ASD Least common type of ASD Located in the upper portion of the atrial Located in the upper portion of the atrial
septum. septum.
Association with an abnormal pulmonary Association with an abnormal pulmonary vein connection vein connection
Four pulmonary veins, two from the right Four pulmonary veins, two from the right lung and two from the left lung, normally lung and two from the left lung, normally return red blood to the left atrium. return red blood to the left atrium.
Usually with a sinus venosus ASD, a Usually with a sinus venosus ASD, a pulmonary vein from the right lung will pulmonary vein from the right lung will be abnormally connected to the right be abnormally connected to the right atrium instead of the left atrium. atrium instead of the left atrium.
This is called an anomalous pulmonary This is called an anomalous pulmonary vein. vein.
..\..\asd-veno.jpgasd-veno.jpg
Foramen OvaleForamen Ovale
Remnant of fetal Remnant of fetal circulationcirculation
Behaves like flap valveBehaves like flap valve Opens during Opens during
increased intra-increased intra-thoracic pressurethoracic pressure
Incidence and PrevalenceIncidence and Prevalence
one of the most common congenital heart one of the most common congenital heart defects seen in pediatric cardiologydefects seen in pediatric cardiology
7-10% of all patients with congenital heart 7-10% of all patients with congenital heart diseasedisease
Twice as frequent in females than malesTwice as frequent in females than males
Presentation Presentation
Fatigue Fatigue Shortness of BreathShortness of Breath Growth retardationGrowth retardation Frequent respiratory infectionsFrequent respiratory infections Persistent murmurPersistent murmur
DiagnosticsDiagnostics
ECGECG X-RAYX-RAY ECHOCARDIOGRAPHYECHOCARDIOGRAPHY Sometimes cardiac catheterizationSometimes cardiac catheterization
Shunt DeterminationShunt Determination
Normally…Normally… Pulmonary Blood Flow = Systemic Blood FlowPulmonary Blood Flow = Systemic Blood Flow
• Shunt Suspected If…Shunt Suspected If…Pulmonary Artery Saturation >80% (?Left-Right)Pulmonary Artery Saturation >80% (?Left-Right)Unexplained Arterial Saturation less than 93% Unexplained Arterial Saturation less than 93% (Right to Left)(Right to Left)
may also see in Pulmonary Edema, Pulmonary Disease, over may also see in Pulmonary Edema, Pulmonary Disease, over sedation and cardiogenic shocksedation and cardiogenic shock
Types of ShuntsTypes of Shunts Systemic Circulation to Pulmonary CirculationSystemic Circulation to Pulmonary Circulation
Left to right Left to right Pulmonary Circulation to Systemic CirculationPulmonary Circulation to Systemic Circulation
Right to LeftRight to Left
Invasive Methods to Diagnose Invasive Methods to Diagnose ShuntingShunting
Oximetric MethodOximetric Method Indicator Dilution MethodIndicator Dilution Method
Principles of the Oxymetric MethodPrinciples of the Oxymetric Method
Blood Sampling from various chambers to Blood Sampling from various chambers to determine Oxygen Saturationdetermine Oxygen Saturation
Left to Right Shunt is present when a Left to Right Shunt is present when a significant increase in blood oxygen significant increase in blood oxygen saturation is found between 2 right sided saturation is found between 2 right sided vessels or chambersvessels or chambers
Oximetric MethodOximetric Method
““Shunt Run” is performed if a difference of Shunt Run” is performed if a difference of 8% or more is noted in blood sampling 8% or more is noted in blood sampling between chambersbetween chambers
Blood samples taken from all right sided Blood samples taken from all right sided locations: IVC, SVC, Right Atrium, Right locations: IVC, SVC, Right Atrium, Right Ventricle and Pulmonary ArteryVentricle and Pulmonary Artery
In case of Inter-atrial shunt multiple samples In case of Inter-atrial shunt multiple samples should be collected from the High, middle should be collected from the High, middle and low right atriumand low right atrium
Saturation RunSaturation Run
Obtain Samples from…Obtain Samples from…– IVC: High and LowIVC: High and Low– SVC: High and LowSVC: High and Low– Right Atrium: High, Middle and LowRight Atrium: High, Middle and Low– Right Ventricle: Inflow and Outflow tracts, mid-cavityRight Ventricle: Inflow and Outflow tracts, mid-cavity– Pulmonary Artery: Main, Left or RightPulmonary Artery: Main, Left or Right
Localizing Right to Left Shunts one should also Localizing Right to Left Shunts one should also obtain….obtain….– Pulmonary VeinPulmonary Vein– Left AtriumLeft Atrium– Left Ventricle Left Ventricle – Distal AortaDistal Aorta
Fick Equation to Calculate Oxygen Fick Equation to Calculate Oxygen ContentContent
Assumes in steady state that…Assumes in steady state that…
that rate of substance entering that rate of substance entering (C in x Qflow) is equal to the (C in x Qflow) is equal to the raterate of substance leaving of substance leaving
(C out x Qflow) + the rate at (C out x Qflow) + the rate at which indicator, V, is added.which indicator, V, is added.
Flow= Oxygen consumption/Arterial-Flow= Oxygen consumption/Arterial-Venous oxygen content differenceVenous oxygen content difference
Where oxygen content is determined Where oxygen content is determined by automated methods by automated methods
oxygen consumption is assumed oxygen consumption is assumed based on patient’s age, gender and based on patient’s age, gender and body surface area when not directly body surface area when not directly measuredmeasured
Shunt QuantificationShunt Quantification Pulmonary Blood FlowPulmonary Blood Flow
Oxygen consumptionOxygen consumption__________________________________________________________________________________Difference in oxygen content across pulmonary bedDifference in oxygen content across pulmonary bed(PvO2-PaO2)(PvO2-PaO2)
Systemic Blood FlowSystemic Blood FlowOxygen ConsumptionOxygen Consumption__________________________________________________________________________________Difference in oxygen content across systemic bedDifference in oxygen content across systemic bed(SaO2- MvO2)(SaO2- MvO2)
Effective Blood Flow: Fraction of Mixed Venous blood received by the Effective Blood Flow: Fraction of Mixed Venous blood received by the lungs without contamination from shuntlungs without contamination from shunt
Oxygen ConsumptionOxygen Consumption____________________________________(PvO2-MvO2)(PvO2-MvO2)
Flamm Formula Flamm Formula
Average Oxygen Content in Chambers proximal to Average Oxygen Content in Chambers proximal to the Shuntthe Shunt
Method to calculate Mixed Venous Oxygen Method to calculate Mixed Venous Oxygen content content
Need to factor in Contribution from IVC and SVC Need to factor in Contribution from IVC and SVC which is not equalwhich is not equal
Flamm Equation:Flamm Equation:3xSVC Oxygen Content + IVC Oxygen Content3xSVC Oxygen Content + IVC Oxygen Content
____________________________________________________________________________
44
How Significant is the Shunt?How Significant is the Shunt?
Flow Ratio PBF/SBFFlow Ratio PBF/SBF 2.0 or more = Large Left to Right Shunt2.0 or more = Large Left to Right Shunt 1.0 or less= Net Right to left Shunt1.0 or less= Net Right to left Shunt No need to measure Oxygen consumption No need to measure Oxygen consumption
Since this number will cancel out of the Since this number will cancel out of the equationequation
Indicator Dilution Method Indicator Dilution Method
More Sensitive for smaller shuntsMore Sensitive for smaller shunts
Cannot localize the level of left to right shuntCannot localize the level of left to right shunt
Left to Right : Dye (indocyanine green) is injected Left to Right : Dye (indocyanine green) is injected into pulmonary artery and a sample is taken from into pulmonary artery and a sample is taken from the systemic arterythe systemic artery
Right to Left: dye injected just proximal to the Right to Left: dye injected just proximal to the presumed shunt and blood sample is taken from presumed shunt and blood sample is taken from systemic artery systemic artery
Eisenmenger SyndromeEisenmenger Syndrome defect in the septum between the atriadefect in the septum between the atria increased flow through the lungs after birth. increased flow through the lungs after birth. eventually result in pulmonary hypertension. eventually result in pulmonary hypertension. The first indication of this may be a reduction in heart size The first indication of this may be a reduction in heart size
– flow overload is converted to a flow overload is converted to a pressure overloadpressure overload ( to which the heart responds with ( to which the heart responds with hypertrophy, rather than dilatation ). Reduction in heart-size,hypertrophy, rather than dilatation ). Reduction in heart-size,
As the left-to-right shunt is converted by reversal of flow across the septum to right-to-left As the left-to-right shunt is converted by reversal of flow across the septum to right-to-left shunt, the patient becomes cyanotic from mixing of un-oxygenated blood.shunt, the patient becomes cyanotic from mixing of un-oxygenated blood.
Cyanosis is thus a late feature of Atrial Septal defect.Cyanosis is thus a late feature of Atrial Septal defect.
If cyanosis is present from birth, ASD will be complicated by one or more contributions:If cyanosis is present from birth, ASD will be complicated by one or more contributions:– Pulmonary Stenosis. Pulmonary Stenosis. – Patent Ductus, usually causes a very large pulmonary artery and enlargement of the aorta. Patent Ductus, usually causes a very large pulmonary artery and enlargement of the aorta. – Common Atrium, allowing complete mixing of oxygenated and unoxygenated blood. Common Atrium, allowing complete mixing of oxygenated and unoxygenated blood. – Truncus arteriosus, complete mixing at aortic level. Truncus arteriosus, complete mixing at aortic level.
Pregnancy and ASDPregnancy and ASD
Well tolerated after closureWell tolerated after closure Increased risk of paradoxical emboli peri Increased risk of paradoxical emboli peri
and post partumand post partum Contraindicated in Eisenmenger SyndromeContraindicated in Eisenmenger Syndrome
– Maternal mortality 50%Maternal mortality 50%– Fetal Mortality 60%Fetal Mortality 60%
TTE and ASDTTE and ASD
Transthoracic Transthoracic echocardiogram four echocardiogram four chamber view to chamber view to evaluate atrial septal evaluate atrial septal defect. Note presence defect. Note presence of inter-atrial of inter-atrial communication communication between left and right between left and right atrium. atrium.
Indications for InterventionIndications for Intervention
Asymptomatic ChildrenAsymptomatic Children– Right Heart dilationRight Heart dilation– ASD> 5mmASD> 5mm– No signs of Spontaneous No signs of Spontaneous
ClosureClosure
Older Patients Older Patients – Hemodynamically Hemodynamically
insignificant ASD with insignificant ASD with Qp/Qs<1.5 if concern for Qp/Qs<1.5 if concern for strokestroke
Pulmonary Hypertension Pulmonary Hypertension – PA pressures> 2/3 systemic PA pressures> 2/3 systemic
arterial resistance arterial resistance – Pulmonary artery reactivity Pulmonary artery reactivity
with vasodilator challengewith vasodilator challenge– Reversible changes on lung Reversible changes on lung
biopsybiopsy Net L->R Shunt of 1.5:1Net L->R Shunt of 1.5:1
Treatment OptionsTreatment Options
1976, King et al published the first attempt 1976, King et al published the first attempt to close an ASD with a double umbrella to close an ASD with a double umbrella devicedevice
Size of the sheath was 23 FrSize of the sheath was 23 Fr Primary Method of to date for closure is Primary Method of to date for closure is
surgicalsurgical Recent advances in interventional closure Recent advances in interventional closure
techniquestechniques
Trans-catheter Closure TechniqueTrans-catheter Closure Technique
Implantation of one or more devices via Implantation of one or more devices via catheter methodcatheter method
Eliminates need for cardio-pulmonary Eliminates need for cardio-pulmonary bypassbypass
No need to stop the heart with cardioplegic No need to stop the heart with cardioplegic agentsagents
Patient SelectionPatient Selection
Strict Food and Drug Administration Strict Food and Drug Administration guidelinesguidelines
Efficacy measured using data from strict Efficacy measured using data from strict follow upfollow up
Follow-up at regular intervals- 3, 6, and 12 Follow-up at regular intervals- 3, 6, and 12 months the year following the initial months the year following the initial procedureprocedure
Any adverse events require follow up for 5-7 Any adverse events require follow up for 5-7 years years
Patient Selection Patient Selection
Defects smaller than 20-25mm in diameterDefects smaller than 20-25mm in diameter Should not have defects in the very upper or lower Should not have defects in the very upper or lower
portions of the septumportions of the septum Ostium Primum or Sinus Venosus, not good Ostium Primum or Sinus Venosus, not good
candidates because defect usually involves heart candidates because defect usually involves heart valves or abnormal venous drainage from the valves or abnormal venous drainage from the lungslungs
Only benefit Ostium Secundum defectsOnly benefit Ostium Secundum defects No lower age limit, but must weigh more than 8-10 No lower age limit, but must weigh more than 8-10
kgkg
Trans-catheter ApproachTrans-catheter Approach
Device is advance through an introducer sheathDevice is advance through an introducer sheath One- Half of the device is deployed on left side of One- Half of the device is deployed on left side of
atrial septum, the second half is deployed on the atrial septum, the second half is deployed on the right side right side
A “sandwich” is formed over the defectA “sandwich” is formed over the defect 6-8 weeks, device as a frame work for scar tissue 6-8 weeks, device as a frame work for scar tissue
to form to form In children the new tissue formation with continue In children the new tissue formation with continue
to growto grow
TTE post InterventionTTE post Intervention
Transesophageal Transesophageal echocardiogram echocardiogram showing Amplatzer showing Amplatzer device placed across device placed across the defect forming a the defect forming a “sandwich” over the “sandwich” over the atrial septal defect atrial septal defect
TTE after interventionTTE after intervention
Transthoracic Transthoracic echocardiogram four echocardiogram four chamber view one day chamber view one day after Amplatzer device after Amplatzer device placement placement
Complete resolution of shuntComplete resolution of shunt
Transthoracic Transthoracic echocardiogram one echocardiogram one day after Amplatzer day after Amplatzer device placed with device placed with highlighted area that highlighted area that shows no further shows no further shunting of blood shunting of blood across atrial septum. across atrial septum.
Tissue formation over Helex device Tissue formation over Helex device in canine model in canine model
In vivo tissue response In vivo tissue response demonstrating flat profile, demonstrating flat profile, conformance to the conformance to the septum, and septum, and nonthrombogenic Occluder nonthrombogenic Occluder material; top photo shows material; top photo shows left atrial view; bottom left atrial view; bottom photo shows right atrial photo shows right atrial side view. side view.
Amplitizer Atrial Septal Defect Amplitizer Atrial Septal Defect OccluderOccluder
AGA Medical, Golden AGA Medical, Golden Valley MnValley Mn
2001- FDA approved for 2001- FDA approved for Secundum lesionsSecundum lesions
Nitinol mesh frame work Nitinol mesh frame work and left/right atrial disksand left/right atrial disks
Filled with poly-fabric to Filled with poly-fabric to promote thrombosuspromote thrombosus
Cost $11K, Surgery$ 21KCost $11K, Surgery$ 21K
Helex atrial septal defect device. Helex atrial septal defect device.
W.L. Gore & AssociatesW.L. Gore & Associates July 1999July 1999 Nitinol, nickel/titanium alloyNitinol, nickel/titanium alloy Wire frame in shape of coil with Gore-TexWire frame in shape of coil with Gore-Tex 9 Fr introducer sheath9 Fr introducer sheath Cost: $6000Cost: $6000
OutcomesOutcomes
Amplatzer study 100 children and adultsAmplatzer study 100 children and adults– Mean age 13.3Mean age 13.3– 93 patients successful implantation93 patients successful implantation– Occlusion rate at 3 months total occlusionOcclusion rate at 3 months total occlusion– Improve RV and LV function and decreased LA volumesImprove RV and LV function and decreased LA volumes
Percutaneous Closure and Functional CapacityPercutaneous Closure and Functional Capacity– 32 adults mean age 43 yo32 adults mean age 43 yo– Qp/Qs 2.0+Qp/Qs 2.0+– 6 months-improved O2 uptake with exercise as 6 months-improved O2 uptake with exercise as
compared pre-closure statuscompared pre-closure status
Comparison to SurgeryComparison to Surgery
Study of children and young adultsStudy of children and young adults Median age 9.8 yMedian age 9.8 y 442 underwent Amplatzer placement442 underwent Amplatzer placement 154 underwent surgery154 underwent surgery Success rate 100% surgery, 96 % Success rate 100% surgery, 96 %
AmplatzerAmplatzer Complication 7% Amplatzer, 24 % surgeryComplication 7% Amplatzer, 24 % surgery
Complication of Percutaneous Complication of Percutaneous InterventionIntervention
Early Early – Device EmbolizationDevice Embolization– A. Fib, SVTA. Fib, SVT– Heart BlockHeart Block– Pericardial EffusionPericardial Effusion– Groin HematomaGroin Hematoma– Device FracturesDevice Fractures– Cardiac PerforationCardiac Perforation
Device ErosionDevice Erosion Sudden DeathSudden Death
Participation in sportsParticipation in sports
2005 36th Bethesda Conference on Eligibility 2005 36th Bethesda Conference on Eligibility Recommendations for Competitive Athletes with Recommendations for Competitive Athletes with Cardiovascular Abnormalities…Cardiovascular Abnormalities…
Small defect no Pulmonary HTNSmall defect no Pulmonary HTNpartcipate in all sportspartcipate in all sports
Large Defect, normal PA pressuresLarge Defect, normal PA pressuresall competative sportsall competative sports
Moderate to large ASD and Pulmonary HTN sever-Moderate to large ASD and Pulmonary HTN sever-no competative sportsno competative sports
ASD and mild Pulmonary HTNASD and mild Pulmonary HTNLow intensisty sports Low intensisty sports
Follow UpFollow Up
3-6 months post intervention3-6 months post intervention– May participate in sports if no Pulm HTN, Heart May participate in sports if no Pulm HTN, Heart
Block, or Myocardial DysfunctionBlock, or Myocardial Dysfunction– Exercise evaluation if these conditions existExercise evaluation if these conditions exist– American Heart Association, no endocarditis American Heart Association, no endocarditis
prophylaxis post corrrection of ASD unless prophylaxis post corrrection of ASD unless patient has MR or MV malformationpatient has MR or MV malformation