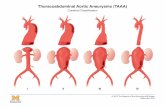
Aortic aneurysms and dissection 2016
-
Upload
ashraf-banoub -
Category
Health & Medicine
-
view
291 -
download
0
Transcript of Aortic aneurysms and dissection 2016

Thoracic Aortic Aneurysm
Ashraf banoub, MD, MBA
09/30/2016

Thoracic Aortic Aneurysm
• Thoracic aortic aneurysm is a permanent localized thoracic aortic dilatation that has at least a 50% diameter increase and three aortic wall
• Pseudoaneurysm or a false aneurysm is a localized dilation of the aorta that does not contain all three layers of the vessel wall and instead consists of connective tissue and clot
• Thoracic aortic aneurysms are common and are the 15th most common cause of death in people older than 65
H.L. Lazar, M. McDonnell, S.R. Chipkin, et al.: The Society of Thoracic Surgeons practice guideline series: Blood glucose management during adult cardiac surgery. Ann Thorac Surg. 87:663 2009 19161815

Risk Factors
• Hypertension • Hypercholesterolemia• Smoking• Genetic inheritance

Genetic Factors
• Thoracic aortic aneurysms divide into two groups at the level of the ligamentum arteriosum.
• Above the ligamentum arteriosum, the disease is not related to typical arterial risk factors and has a smooth, noncalcified wall accompanied by no debris or clot.
• Below the ligamentum arteriosum, the disease process primarily is atherosclerotic, with an irregular calcified wall accompanied by copious debris and clot
G. Albornoz, M.A. Coady, M. Roberts, et al.: Familial thoracic aortic aneurysms and dissections—incidence, modes of inheritance, and phenotypic patterns. Ann Thorac Surg. 82:1400 2006 16996941

Inflammatory Causes
• Syphilis• Mycotic aneurysm from endocarditis• Giant-cell arteritis• Takayasu arteritis.

Complications of Thoracic Aortic Aneurysms
• Aortic rupture
• Aortic regurgitation
• Tracheobronchial and esophageal compression
• Right pulmonary artery or right ventricular outflow tract obstruction
• Systemic embolism from mural thrombus

Classifications of Aortic Aneurysms
Safi modification of Crawford TAA classification
Safi HJ, Winnerkvist A, Miller CC 3rd, et al. Effect of extended cross-clamp time during thoracoabdominal aortic aneurysm repair. Ann Thorac Surg 1998; 66:1204.

The shape of thoracic aortic aneurysms
• Fusiform aneurysms are more common
• Associated with atherosclerotic or collagen vascular disease, and usually affect a longer segment of the aorta
• Saccular aneurysms are more localized, confined to an isolated segment of the aorta

Symptoms
• Chest and back pain caused by aneurysmal dissection, rupture, or bony erosion.
• Mass effect from a large thoracic aortic aneurysm
• Hoarseness (recurrent laryngeal nerve)
• Dyspnea (trachea, mainstem bronchus, pulmonary artery)
• Central venous hypertension (superior vena cava syndrome)
• Dysphagia (esophagus).
• Rupture of thoracic aortic aneurysms is a surgical emergency and is often accompanied with
• Acute pain with or without hypotension
• Rupture of an ascending aortic aneurysm may cause cardiac tamponade
• Rupture in the descending thoracic aorta may cause hemothorax, aortobronchial fistula, or aortoesophageal fistula.

Diagnostic Imaging for Thoracic Aortic
• Typically, transthoracic echocardiography can provide a reasonable examination of the thoracic aorta
• The contemporary imaging modalities of choice are CT, MRI, and TEE.

CTA Imaging for Thoracic Aortic
• Computed tomographic angiography (CTA) images the thoracic aorta during the arterial phase of an intravenous radiocontrast agent injection.
• Advantages include high resolution, wide availability, rapid acquisition, imaging in patients with metallic implants, and generation of volumetric aortic images for stent design.
• CTA requires iodinated contrast agents, it carries a risk for contrast nephropathy that can be attenuated by administration of acetylcysteine and sodium bicarbonate.
J.R. Brown, C.A. Block, D.J. Malenka, et al.: Sodium bicarbonate plus N-acetylcysteine prophylaxis: A meta-analysis. JACC Cardiovasc Interv. 2:1116 2009 19926054

Contrast-enhanced magnetic resonance angiography with
gadolinium• Advantages are
• Avoidance of ionizing radiation
• Lack of renal toxicity
• Allows for degrees of tissue and fluid characterization.
• Disadvantages include
• Limited availability
• Lack of imaging in patients with metallic implants
• Imaging difficulty in the setting of need for continuous hemodynamic monitoring
• Time required for image acquisition

TEE
• TEE can image the thoracic aorta from the aortic valve to the distal ascending aorta and from the distal aortic arch to the proximal abdominal aorta. The distal ascending aorta and proximal aortic arch cannot be reliably imaged by TEE because the intervening trachea and left mainstem bronchus obstruct the acoustic window
• The advantages of TEE include its portability, its real-time interpretation, its compatibility at the bedside and in the OR, and its multiple imaging modalities for complete aortic and cardiac assessment.
• Its disadvantages include the requirement for sedation or general anesthesia and the risks for upper gastrointestinal injury.

Indications for Surgical Repair of Thoracic Aortic Aneurysms
Atherosclerotic aneurysm diameterAscending aorta >/=5.5 cmDescending aorta >/=6.5 cm
Marfan’s or familial thoracic aneurysm diameterAscending aorta >/=5.0 cmDescending aorta >/=6.0cm
Severe aortic regurgitationAortoannular ectasia with aortic root aneurysmRuptureRefractory painJ.A. Elefteriades, E.A. Farkas: Thoracic aortic aneurysm. J Am Coll Cardiol. 55:841 2010 20185035J.G. Augoustides, T. Plappert, J.E. Bavaria: Aortic decision-making in the Loeys-Dietz syndrome: Aortic root aneurysm and a normal-caliber ascending aorta and aortic arch. J Thorac Cardiovasc Surg. 138:502 2009 19619806R.R. Davies, A. Gallo, M.A. Coady, et al.: Novel measurement of relative aortic size predicts rupture of thoracic aortic aneurysms. Ann Thorac Surg. 81:169 2006 16368358

Surgical Repair of Ascending Aortic and Arch Aneurysms
• The type of surgical repair depends on aortic valve function and the aneurysm extent.
• Perioperative TEE can evaluate the aortic valve structure and function to guide and assess the surgical intervention (reimplantation, repair, replacement).

If the aortic valve and aortic root are normal, a simple tube graft can be used to replace the ascending aortaIf the aortic valve is diseased but the sinuses of Valsalva are normal, an aortic valve replacement combined with a tube
graft for the ascending aorta without need for reimplantation of the coronary arteries can be performed (Wheat procedure

Dilated Aortic Root

Aortic Root Replacement
(modified Bentall Procedure)

Repairing aortic aneurysms that extend into or involve the aortic arch requires CPB with DHCA with or without perfusion adjuncts
Elephant Trunk Repair

The trifurcated graft technique for replacing the aortic arch.

Anesthetic Management for Ascending Aorta and Arch Aneurysms
• The imaging studies should be reviewed for aneurysm compression of mediastinal structures such as the right pulmonary artery and left mainstem bronchus
• Prevention of hypertension increases forward flow in AR and minimizes the risk for aneurysm rupture
• A right radial arterial catheter is preferred for most cases
• If arterial cannulation of the right axillary, subclavian, or innominate artery is planned for CPB and ACP, bilateral radial arterial catheters often are required to measure cerebral and systemic perfusion pressures
• Nasopharyngeal, tympanic, and bladder temperatures are important for estimating brain and core temperatures for monitoring the conduct of DHCA

• Intraoperative TEE is essential to guide and assess the surgical interventions
• In patients with AR, TEE can assist in the conduct of CPB by guiding placement of cannulae such as the retrograde cardioplegia cannula (coronary sinus) and by monitoring left ventricular (LV) volume
• Intraoperative TEE is reasonable in thoracic aortic procedures, including endovascular interventions, in which it assists in hemodynamic monitoring, procedural guidance, and endoleak detection
1L.F. Hiratzka, G.L. Bakris, J.A. Beckman, et al.: ACCF/AHA/AATS/ACR/ASA/SCA/SCAI/SIR/STS/SVM guidelines for the diagnosis and management of patients with thoracic aortic disease: Executive summary. A report of the American College of Cardiology Foundation, American
Heart Association Task Force on Practice Guidelines, American Association for Thoracic Surgery, American College of Radiology, American Stroke Association, Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society for Vascular
Medicine. J Am Coll Cardiol. 55:1509 2010

Neuroprotection Strategies for Temporary Interruption of
Cerebral Blood Flow
• Hypoperfusion or temporary circulatory arrest during aortic arch repair.
• Cerebral ischemia due to embolization secondary to CPB and atheroma
• Air
• Atherosclerotic particulate debris
• CPB may result in the microparticulate aggregates of platelets and fat
• Retrograde blood flow through a diseased descending thoracic aorta
L.H. Stein, J.A. Elefteriades: Protecting the brain during aortic surgery: An enduring debate with unanswered questions. J Cardiothorac Vasc Anesth. 24:316-321 2010 19646900

Brain Protection for Aortic Arch Reconstruction
• Deep systemic hypothermia
• Topical cerebral cooling
• Retrograde cerebral perfusion
• Selective antegrade cerebral perfusion
• Cerebral hyperthermia prevention during rewarming

Deep Hypothermic Circulatory Arrest
• The physiologic basis for deep hypothermia as a neuroprotection strategy is to decrease cerebral metabolic rate and oxygen demands to increase the period that the brain can tolerate circulatory arrest
• Autoregulation of cerebral blood flow is maintained during deliberate hypothermia with alpha-stat blood gas management without compromise of clinical outcome
D.K. Harrington, F. Fragomeni, R.S. Bonser: Cerebral perfusion. Ann Thorac Surg. 83:S799 2007 17257930K.A. Abdul Aziz, A. Meduoye: Is pH-stat or alpha-stat the best technique to follow in patients undergoing deep hypothermic circulatory arrest?. Interact
Cardiovasc Thorac Surg. 10:271 2010 19914925

Adapted from Cheung AT, Bavaria JE, Pochettino A, et al: Oxygen delivery during retrograde cerebral perfusion in humans. Anesth Analg 88:14, 1999

• The median nasopharyngeal temperature for electrocortical silence was 18° C
• A nasopharyngeal temperature of 12.5° C or cooling on CPB for at least 50 minutes achieved electrocortical silence in 99.5% of cases
M.M. Stecker, A.T. Cheung, A. Pochettino, et al.: Deep hypothermic circulatory arrest: I. Effects of cooling on electroencephalogram and evoked potentials. Ann Thorac Surg. 71:14 2001
11216734

(A) The cumulative probability of electrocerebral silence on electroencephalogram (EEG) as a function of cooling time. (B)
The cumulative probability that electrocerebral silence (ECS) is not achieved for temperatures above that indicated.
Stecker MM, Cheung AT, Pochettino A, et al: Deep hypothermic circulatory arrest: I. Effects of cooling on electroencephalogram and evoked potentials. Ann Thorac Surg 71:19, 2001, by permission of the Society of Thoracic Surgeons

Retrograde Cerebral Perfusion
• RCP is performed by infusing cold oxygenated blood into the superior vena cava cannula at a temperature of 8° C to 14° C via CPB
A. Pochettino, A.T. Cheung: Pro: Retrograde cerebral perfusion is useful for deep hypothermic circulatory arrest. J Cardiothorac Vasc Anesth. 17:764 2003 14689421

Retrograde Cerebral Perfusion
• The internal jugular venous pressure is maintained at less than 25 mm Hg to prevent cerebral edema
• The patient is positioned in 10 degrees of Trendelenburg to decrease the risk for cerebral air embolism and prevent trapping of air within the cerebral circulation in the presence of an open aortic arch. RCP flow rates of 200 to 600 mL/min usually can be achieved
A. Pochettino, A.T. Cheung: Pro: Retrograde cerebral perfusion is useful for deep hypothermic circulatory arrest. J Cardiothorac Vasc Anesth. 17:764 2003 14689421

Retrograde Cerebral Perfusion
• The potential benefits of RCP include• partial supply of cerebral metabolic
substrate• cerebral embolic washout• maintenance of cerebral hypothermia
A. Pochettino, A.T. Cheung: Pro: Retrograde cerebral perfusion is useful for deep hypothermic circulatory arrest. J Cardiothorac Vasc Anesth. 17:764 2003 14689421

Retrograde Cerebral Perfusion
• The perioperative rates for mortality and stroke in this series were 10.4% and 2.8%, respectively. The application of RCP was significantly protective against mortality (odds ratio, 0.42; 95% confidence interval, 0.25-0.70; P = 0.0009) and stroke (odds ratio, 0.35; 95% confidence interval, 0.15-0.81; P = 0.02
A.L. Estrera, C.C. Miller, T.Y. Lee, et al.: Ascending and transverse aortic arch repair: The impact of retrograde cerebral perfusion. Circulation. 118:S160 2008 18824749

Selective Antegrade Cerebral Perfusion
• Selective ACP should be considered for aortic arch repairs longer than 45 minutes
• ACP typically is initiated during DHCA by selective cannulation of the right axillary artery, right subclavian artery, innominate artery, or left common carotid artery
L.H. Stein, J.A. Elefteriades: Protecting the brain during aortic surgery: An enduring debate with unanswered questions. J Cardiothorac Vasc Anesth. 24:316-321 2010

Selective Antegrade Cerebral Perfusion
• In transverse aortic arch reconstruction procedures, ACP can be accomplished by inserting individual perfusion cannulae into the open end of the aortic branch vessels after

Selective Antegrade Cerebral Perfusion
• Unilateral ACP via right axillary arterial cannulation is a popular technique for adult aortic repair
• This technique assumes an adequate circle of Willis; however, the anatomic completeness of the circle of Willis does not guarantee adequate cerebral cross-perfusion during aortic arch repair
C.D. Etz, K.A. Plestis, F.A. Kan, et al.: Axillary cannulation significantly improves survival and neurologic outcome after atherosclerotic aneurysm repair of the aortic root and ascending aorta. Ann Thorac Surg. 86:441 2008

Selective Antegrade Cerebral Perfusion
• Safe ACP was significantly prolonged with bilateral ACP (86–164 minutes) compared with unilateral ACP (30–50 minutes). The evidence favors bilateral ACP in the setting of aortic arch repair times longer than 60 minutes
• ACP with oxygenated blood at 10° C to 14° C at flow rates in the range of 250 to 1000 mL/min typically achieves a cerebral perfusion pressure in the range of 50 to 80 mm Hg
P.G. Malvindi, G. Scrascia, N. Vitale: Is unilateral antegrade cerebral perfusion equivalent to bilateral cerebral perfusion for patients undergoing aortic arch surgery?. Interact Cardiovasc Thorac Surg. 7:891 2008

Pharmacologic Neuroprotection Strategies for Deep Hypothermic Circulatory Arrest
• Neuroprotective effects of such drugs may decrease any cerebral metabolic activity that remains at temperatures less than 18°C
• When thiopental was available, doses of 20 mg/kg were administered prior to DHCA to provide EEG silence.
• Propofol in DHCA has not demonstrated neuroprotective effects, but do show effect EEG burst suppression
Woodcock TE, Murkin JM, Farrar JK Tweed WA, Guiraudon GM, McKenzie FN. Pharmacologic EEG suppression during cardiopulmonary bypass: cerebral hemodynamic and metabolic effects of thiopental or
isoflurane during hypothermia and normothermia. Anesthesiology 1987;67:218-24

Pharmacologic Neuroprotection Strategies for Deep Hypothermic Circulatory Arrest
• Steroids do provide anti-inflammatory and spinal cord protection during CPB, but neuroprotection during DHCA has not been proven
• Mechanisms include anti-oxidant effects, cytoprotective effects, reduced release of excitatory amino acids, inhibition of proinflammatory pathways activated by CPB and ischemia, and attenuation of altered CBF resulting from hypothermic arrest
• Support for the clinical use of corticosteroids for neuroprotection during DHCA is in part based on the positive effects of large doses of methylprednisolone (30 mg/kg) after spinal cord injury, although these data are controversial
• Corticosteroid may lead to hyperglycemia. Even mild glucose elevation (i.e., >140 mg/dL) is associated with poor outcome after stroke mandating close monitoring of glucose during surgery
Shine TSJ, Uchikado M, Crawford CC, Murray MJ. Importance of perioperative blood glucose management in cardiac surgical patients. Asian Cardiovasc Thorac Ann 2007;15:534-538


Aortic Dissection
• Aortic dissection results from an intimal tear that exposes the media to the pulsatile force of blood within the aortic lumen
• The aortic dissection may remain localized at the primary entry site at the original intimal tear, or it may extend proximally, distally, or both

Aortic Dissection• DeBakey Classification
• Type I: The entire aorta is involved (ascending, arch, and descending)
• Type II: Confined to the ascending aorta
• Type III: Intimal tear originating in the descending aorta with either distal or retrograde extension
• Type IIIA: Intimal tear originating in the descending aorta with extension distally to the diaphragm or proximally into the aortic arch
• Type IIIB: Intimal tear originating in the descending aorta with extension below the diaphragm or proximally into the aortic arch
• Stanford Classification
• Type A: Involvement of the ascending aorta or aortic arch regardless of the site of origin or distal extent
• Type B: Confined to the descending aorta distal to the origin of the left subclavian artery

Type A Aortic Dissection
• Aortic dissections that involve the ascending aorta (Stanford type A) are considered surgical emergencies
• The mortality rate without emergency surgery is about 1% per hour for the first 48 hours, 60% by about 1 week, 74% by 2 weeks, and 91% by 6 months

Potential Complications of Acute Type a Aortic Dissection
• Cardiac tamponade
• Aortic regurgitation
• Myocardial infarction
• Stroke
• Limb ischemia
• Mesenteric ischemia

Mortality in Acute Aortic Dissection According to Dissection Type and
Management
Hagan PG, Nienaber CA, Isselbacher EM, et al: The International Registry of Acute Aortic Dissection (IRAD). New insights into an old disease. JAMA 283:897, 2000
Dissection Type N Hospital Mortality(%)
Stanford Type A 289 101 (34.9)
Medical Management 81 47 (58.0)
Surgical Management 208 54 (26.0)
Stanford Type B 175 26 (14.9)
Medical Management 140 15 (10.7)
Surgical Management 35 11 (31.4)

Modified Crawford Classification

Descending Thoracic and Thoracoabdominal Aortic Aneurysms
• Surgical therapy for thoracic and TAAAs is to replace aneurysmal aorta with a prosthetic tube graft
• Surgical access is via lateral thoracotomy or thoracoabdominal incision
• The risks for spinal, mesenteric, renal, and lower extremity ischemia are significant due to thromboembolism, loss of collateral vascular networks, temporary interruption of blood

Clinical Outcomes of Thoracoabdominal Aortic Aneurysm (TAAA) Repair
Cowan JA, Dimick JB, Henke PK, et al: Surgical treatment of intact thoracoabdominal aortic aneurysms in the United States: Hospital and surgeon volume-related outcomes. J Vasc Surg 37:1169, 2003; and Cowan JA, Dimick JB, Wainess RM, et al: Ruptured thoracoabdominal aortic aneurysm
treatment in the United States: 1988 to 1998. J Vasc Surg 38: 312, 2003.. Yamauchi T, Takano H, Nishimura M, Matsumiya G, Sawa Y. Paraplegia and para- paresis after descending thoracic aortic aneurysm
repair: a risk factor analysis. Ann Thorac Cardiovasc Surg. 2006;12(3) 179-83
Complications Intact TAAA (n=1542) Ruptured TAAA (n=321)
Cardiac 14.8% 18.1%
Pulmonary 19% 12.7%
Hemorrhage 12.4% 10.9%
Acute renal failure 14.2% 28%
Paraplegia 2.7%-12% 3.4%-16%
In-hospital mortality 22.3% 53.8%



Operative techniques for repair of thoracic or thoracoabdominal aortic
aneurysms
• (1) aortic cross-clamping
• (2) aortic cross-clamping with a Gott shunt
• (3) aortic cross-clamping with PLHB or partial CPB

Spinal Cord Ischemia

Spinal Cord Ischemia
• The largest of the radicular arteries is the artery of Adamkiewicz, often given off at the level of T10 but it can vary in position from T7 to L4

Spinal Cord Ischemia • Paraplegia/ paraparesis occurs in 2.7 to 12% in
thoracic and 3.6 to 16% in thoracoabdominal open surgical procedures
• Paraplegia post thoracic stenting varies from 0 to 9.8%, with a permanent paraplegia risk of 5.5%.
• Isolated descending thoracic stents is 0.9%
• Complex procedures involving fenes- trated and branched stents (7.1%) and visceral hybrid procedures (11.3%)
. Yamauchi T, Takano H, Nishimura M, Matsumiya G, Sawa Y. Paraplegia and para- paresis after descending thoracic aortic aneurysm repair: a risk factor analysis. Ann Thorac Cardiovasc Surg. 2006;12(3) 179-83
. Drinkwater SL, Goebells A, Haydar A, Bourke P, Brown L, Hamady M, Gibbs RG; Regional Vascular Unit, St Mary's Hospital, Imperial College NHS Trust. The inci- dence of spinal cord ischaemia following thoracic and thoracoabdominal aortic endo- vascular intervention. Eur J Vasc
Endovasc Surg. 2010;40(6) 729-35

Spinal Cord Ischemia
• Spinal cord perfusion pressure is a balance between the inflow and outflow pressures within the closed confines of the spinal canal, calculated as mean arterial pressure (MAP) minus CSF pressure
• Theoretically therefore, decreasing the CSF pressure or increasing the blood pressure/MAP will improve spinal cord perfusion pressure

Risk factors for spinal cord ischemia
• Blood Supply
• Perfusion Pressure
• Reperfusion Injury
• Critical Intercostal Artey Coverage
• Collateral Circulation
• Hypotension

Blood Supply
• Spinal cord blood supply is often segmental and dependent upon contribution from collateral arteries
• The need for more extensive aortic replacement requires interruption of an increasing number of intercostal arteries providing spinal cord perfusion, thereby posing a higher risk of SCI
. Carroccio A, Marin ML, Ellozy S, Hollier LH. Pathophysiology of paraplegia follow- ing endovascular thoracic aortic aneurysm repair. J Card Surg. 2003;18(4) 359-66.

Blood Supply
• Proximal aortic clamp interferes with the autoregulatory response controlling cerebral perfusion with resulting fluctuations in cerebral blood flow
• Lowering proximal pressure decreases distal mean arterial pressure, which in the presence of an unchanged or possibly increased CSF pressure, results in decreased perfusion pressure of the distal cord
. Carroccio A, Marin ML, Ellozy S, Hollier LH. Pathophysiology of paraplegia follow- ing endovascular thoracic aortic aneurysm repair. J Card Surg. 2003;18(4) 359-66.

Reperfusion Injury
• Ischemia and reperfusion initiate neurochemical cellular responses that can exacerbate ischemia
• Lipid peroxidation with cell membrane destruction
• Inflammatory cells including leukocytes adhere to the microvasculature and release cytotoxic mediators
. Acher C, Wynn M. Paraplegia after thoracoabdominal aortic surgery: not just assist- ed circulation, hypothermic arrest, clamp and sew, or TEVAR. Ann Cardiothorac Surg. 2012;1(3) 365-72

Critical intercostal artery coverage
• Stent-graft coverage of the critical thoracic intercostal arteries results in reduced perfusion of the thoracic spinal cord and watershed infarction.
• Loss of the artery of Adamkiewitz in prior abdominal aortic repairs may explain why patients with prior repair are at higher risk of SCI during subsequent TAA repair
. McGarvey ML, Mullen MT, Woo EY, Bavaria JE, Augoustides YG, Messé SR, Cheung AT. The treatment of spinal cord ischemia following thoracic endovascular aortic re- pair. Neurocrit Care. 2007;6(1) 35-9.

Collateral circulation
• SCI following stent-graft deployment can also be dependent upon the extent of existing collateral circulation

Real-time Monitoring of the Paraspinous Collateral Network Oxygenation by Near Infrared Spectroscopy During and After
Open and Endovascular Descending and Thoracoabdominal Aortic Repair
Real-time Monitoring of the Paraspinous Collateral Network Oxygenation by Near Infrared Spectroscopy During and After Open and Endovascular Descending and Thoracoabdominal Aortic Repair
M. Luehr1, K. von Aspern1, A. Hoyer1, C. Mukherjee2, J. Banusch2, J. Ender2, F. Mohr1, C. D. Etz1. 1Cardiac Surgery, Leipzig Heart Center, Leipzig, Germany, 2Anesthesiology, Leipzig Heart Center, Leipzig, Germany

Hypotension
• Hypotension that precipitates spinal cord injury within the first 48 hours after open surgical intervention is quite subtle
• Maintaining blood pressures at high levels not only intraoperatively but for at least 48 hours postoperatively

Hypotension
• Following TEVAR, MAP should be maintained at greater than 80mmHg with the use of vasopressors when required
. Etz CD, Luehr M, Kari FA, Bodian CA, Smego D, Plestis KA, Griepp RB. Paraplegia after extensive thoracic and thoracoabdominal aortic aneurysm repair: does critical spinal cord ischemia occur postoperatively? J Thorac Cardiovasc Surg. 2008;135(2) 324-30.

Adjuncts for the prevention of paraplegia
• Intercostal artery re-implantation
• Internal iliac revascularization
• Left subclavian artery revascularization
• Elective sac perfusion via temporary controlled endoleak
• Cerebrospinal fluid drainage

Intercostal artery re-implantation or presevation
• Reduced paraplegia risk index by 75%
• Based on magnetic resonance angiography identification of intercostal arteries that supplied radicular arteries
• The incidence of paralysis after TAAA repair decreased from 4.83% to 0.88%
Acher CW, Wynn MM, Mell MW, Tefera G, Hoch JR. A quantitative assessment of the impact of intercostal artery reimplantation on paralysis risk in thoracoabdominal aortic aneurysm repair. Ann Surg. 2008 Oct;248(4):529-40

Adjuncts for the prevention of paraplegia
• Internal iliac revascularization
• Left subclavian artery revascularization
Bicknell CD, Riga CV, Wolfe JH. Prevention of paraplegia during thoracoabdominal aortic aneurysm repair. Eur J Vasc Endovasc Surg. 2009 Jun;37(6) 654-60Peterson BG, Eskandari MK, Gleason TG, Morasch MD. Utility of left subclavian artery revascularization in association with endoluminal repair of acute and chronic thoracic aortic
pathology. J Vasc Surg. 2006;43(3) 433-9
Left common carotid (CC) to left subclavian artery (LSCA, arrow) bypass with Dacron graft (arrow head) performed
prior to endovascular stenting across origin of LSCA (star) to createadequate landing zone for exclusion of thoracic aortic
aneurysm while maintaining flow to LSCA

Elective sac perfusion via temporary controlled endoleak
• The perfusion branches are left open in order to perfuse segmental vessels.
• Five to ten days postoperatively the branches are then closed with Amplatzer plugs to complete exclusion
Harrison SC, Agu O, Harris PL, Ivancev K. Elective sac perfusion to reduce the riskof neurologic events following endovascular repair of thoracoabdominal aneurysms.
J Vasc Surg. 2012;55(4) 1202-5.

Cerebrospinal fluid drainage
• Two meta-analyses concluded that CSFD significantly reduces the risk of perioperative paraplegia or paraparesis.
• A Cochrane review concluded CSFD may increase the perfusion pressure to the spinal cord and hence reduce the risk of ischemic spinal cord injury
Cinà CS, Abouzahr L, Arena GO, Laganà A, Devereaux PJ, Farrokhyar F. Cerebrospinalfluid drainage to prevent paraplegia during thoracic and thoracoabdominal aortic
aneurysm surgery: a systematic review and meta-analysis. J Vasc Surg. 2004;4036-44.

Cerebrospinal fluid drainage
• CSF drainage through insertion of a spinal drain (usually controlled to maintain a CSF pressure of less than 10-12mmHg) can reduce CSF pressure, thereby improving spinal cord perfusion