Anatomy of Lacrimal System
-
Upload
mohammad-faisal -
Category
Documents
-
view
69 -
download
3
Transcript of Anatomy of Lacrimal System

ANATOMY & PHYSIOLOGY OF LACRIMAL SYSTEM
Dr. Adnan

Lacrimal apparatus
Secretory systems:
lacrimal gland: reflex secretion accessory lacrimal gland: basic secretion conjunctival goblet cells: mucoprotein meibomian glands : lipid sebaceous gland of the palpebral margin: lipid
Drainage systems :
upper,lower pancta
upper, lower lacrimal canaliculi common canaliculus lacrimal sac nasolacrimal duct

Embryology
Primitive Cord of cells derived from surface ectoderm, sequestered in the naso-maxillary groove, forms the future lacrimal drainage system.

Punctal membranes open at full term; however, the membrane of Hasner remains imperforate in up to 70% newborns.
This usually opens within the first month but may remain imperforate for a longer time.
Spontaneous opening of an imperforate valve of Hasner usually occurs within 6-12 months.

It consists of:
(a) The Lacrimal gland, which secretes the tears, and its excretory ducts, which convey the fluid to the surface of the eye;
(b) The Lacrimal canaliculi, the Lacrimal sac, and the Nasolacrimal duct, by which the fluid is conveyed into the cavity of the nose.
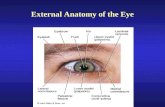
Lacrimal Apparatus

Superolateral , Formed by bones of frontal and Zygomatic
color: grayish - pink 2 lobes orbital: 20× 12× 5mm anterolateral to
globe 0.78 g Palpebral: inferior to levator 1/3 – 1/2 of
orbital lobe 8-12 major lacrimal ducts empty to superior to
cul-de-sac approximately 5mm above the lateral tarsal border.
Main lacrimal gland


The lacrimal gland secretes tears, which contain lysozyme and electrolytes similar to plasma. They look similar to salivary glands, with the typical appearance of serous cells. Tubuloacinar gland


Krause and Wolfring.
Location: deep within the sup. fornix
Accessory lacrimal gland


Puncta
Puncta are openings 0.3 mm in diameter located on the medial aspect of the upper and lower eyelid margins.
Each punctum sits on top of an elevated mound known as the papilla lacrimalis.
The puncta are relatively avascular in comparison with the surrounding tissue, giving them a pale appearance, which is accentuated with lateral traction of the lid. This pallor can be helpful in localizing a stenosed punctum

Puncta are directed posteriorly against the globe; therefore, they are not usually visible unless the eyelid is everted. Punctal ectropion may lead to inadequate tear drainage and resulting epiphora.
The inferior punctum is approximately 0.5 mm lateral to the superior punctum, with distances to the medial canthus of 6.5 mm and 6.0 mm, respectively. Tears within the medial canthal area enter the puncta to pass into the canaliculi.

Congenital atresia, supernumerary or double puncta, and congenital slits of the puncta all may occur from aberrations in the location of the epithelial cord and its opening to the surface epithelium.
Lateral displacement of the puncta may occur in some congenital syndromes such as blepharophimosis.

Canaliculi
Canaliculi have an initial vertical segment, measuring 2 mm, followed by an 8-mm horizontal segment.
The angle between the vertical and horizontal segments is approximately 90 degrees, and the canaliculi dilate at the junction to form the ampulla.
In most individuals, the horizontal portion of the canaliculi converges to form the common canaliculus.

Canaliculi pierce the lacrimal fascia before entering the lacrimal sac. At its entrance to the lacrimal sac, the common canaliculus may dilate slightly, forming the sinus of Maier.


Canaliculi are lined by nonkeratinized, stratified squamous epithelium and are surrounded by elastic tissue, which permits dilation to 2 or 3 times the normal diameter.
The oblique entrance of the common canaliculus into the lacrimal sac forms the valve of Rosenmüller, which prevents retrograde reflux of fluid from the sac into the canaliculi.

However, the posterior angulation of the upper and lower canaliculi followed by anterior angulation of the common canaliculus may also block reflux at the canaliculus-sac junction.
An incompetent valve of Rosenmüller is observed clinically as air escaping from the lacrimal puncta when the individual blows his or her nose.

Atresia or failure of canalization of the lacrimal canaliculi may occur in conjunction with punctal atresia.
In many cases, particularly in patients with mesodermal dysplasia, the lacrimal canaliculi and puncta may be absent and a normal tear sac and nasolacrimal duct may be present but not connected to the eyelid surface.

Lacrimal sac
The lacrimal sac sits within the lacrimal fossa, which is bound anteriorly by the frontal process of the maxillary bone (anterior lacrimal crest) and posteriorly by the lacrimal bone (posterior lacrimal crest).

The lacrimal sac is lined by a double-layered epithelium (superficial is columnar, and deep is flatter). It can be divided into a fundus superiorly and a body inferiorly.
The fundus extends 3-5 mm above the superior portion of the medial canthal tendon, and the body extends approximately 10 mm below the fundus to the osseous opening of the nasolacrimal canal.

At the posterior lacrimal crest, the orbital periosteum splits to envelop the lacrimal sac as a covering known as the lacrimal fascia.
The lacrimal fascia is surrounded by fibers of the orbicularis oculi muscle; the superficial head attaches to the anterior lacrimal crest, and the deep head attaches to the posterior lacrimal crest.
Between the lacrimal fascia and the lacrimal sac lies a venous plexus. The orbital septum attaches to the medial orbital wall at the posterior lacrimal crest, so the lacrimal sac is a preseptal structure.


A congenital fistula of the lacrimal sac, lacrimal anlage duct is commoner than diverticulums.
Autosomal dominant and may coexist with thalassemia. It undoubtedly is the result of canalization of a strand of epithelial cords.
The fistulas often have to be completely excised to prevent drainage of tears externally on the skin.

Lacrimal duct anlage. a congenital lacrimal drainage fistula inferonasal to the medial canthal angle

Nasolacrimal duct
The nasolacrimal duct consists of a 12-mm superior intraosseous portion and a 5-mm inferior membranous portion.
The intraosseous part travels posterolaterally through the nasolacrimal canal within the maxillary bone.
The membranous part runs within the nasal mucosa, eventually opening into the inferior meatus under the inferior nasal turbinate.

The double layer of epithelium similar to that observed in the lacrimal sac. The venous plexus surrounding the lacrimal sac continues inferiorly to surround the nasolacrimal duct.

Dacryostenosis is a common condition in which the extreme end of the nasolacrimal duct underneath the inferior turbinate fails to complete its canalization in the newborn period; it produces clinical symptoms in 2% to 4% of newborns

The Main Blood supply: Lacrimal artery
Branches of the transverse facial or infraorbital arteries.
Venous blood returns via the superior ophthalmic vein.
Blood supply

Ophthalmic division of CN V, which supplies sensory innervation to the lacrimal gland along with the eye lid and conjunctiva.
Innervation

The upper part of the lacrimal sac is covered by the medial palpabral ligament.
Hence abscesses within the sac bulge below the medial palpabrel ligament, where it should bi incised for letting out the pus.
Applied Anatomy

Around the nasolacrimal duct there is the rich plexus of veins, in the form of an erectile tissue, which may engorge and cause obstruction to the duct.

The angular vein is in front of the sac and it should be take care during incising the sac.
Between the lacrimal sac and the fascia coverning the sac there is the collection of venous plexus present hence the incising cause considerable bleeding.

Physiology

The lacrimal gland secretes tears directly into the superior fornix.
The tears are collected at the lacrimal lake and then drained by the superior and inferior lacrimal papillae.
The lacrimal caruncle prevents the papillae from getting stuck to each other.

If there are tears: “Puncta” opens at the
medial part to the “Plica Semilunaris”
Into the Lacunar Caruncle
into the lacrimal canaliculi
Into lacrimal ducts
Into the lacrimal sac (held by lacrimal bone)
Opens to the nasolacrimal duct

Key physiologic point to understand, is that the lacrimal outflow system is based on an active, dynamic pumping mechanism.

With the eyelids open before the start of a blink, the canaliculi are already filled with tears.
The blink acts to compress the canaliculi and lacrimal sac, thus forcing the contained fluid into the nasolacrimal ducts and nasal passages.

Tears flow along the upper and lower marginal strips and enter the upper and lower canaliculi by capillarity and also possibly by suction.

The volume of fluid within the lacrimal outflow system is at its minimum at the point of maximum lid closure during a blink.
As the eyelids begin to open, the muscular compressive force terminates and the elastic walls of the canaliculi and lacrimal sac attempt to restore their original shape.

Other factors contributing to lacrimal elimination
Physical forces such as gravity and capillary attraction of the tears,
Reservoir drainage into the lacrimal sac (so-called Krehbiel flow),
Microcilliation in the nasolacrimal duct and
Evaporation of tears from the ocular surface and absorption of tears by the lacrimal sac mucosa.

More than 90% off the lacrimal fluid isremoved by the Excretory system.
Less than 10% evaporates between blinks.

All efforts should be made to preserve the lacrimal canaliculi.
Repeated instrumentation of the lacrimal system or nasolacrimal duct probings are unlikely to help the underlying pathology and may in and of themselves injure the canaliculi and thus permanently impair lacrimal elimination.
Very little can be done to restore scarred fibrosed canaliculi.

Experimental and clinical studies show that tear elimination is equivalent through the upper and lower canalicular systems.
Surgeons should thus give equal consideration to a patient with lacerations of either the upper or lower canaliculus.
Traditional teachings that upper eyelid canalicular lacerations are unimportant are simply not true.
Ref: Daubert J, Nik N, Chandeyssoun PA et al: Tear flow analysis through the upper and lower systems. Ophthalmol Plast Reconstr Surg 6:193, 1990

Thank U.


![[PPT]PowerPoint Presentation - North Allegheny · Web viewExternal Anatomy of the Eye Lacrimal Apparatus of the Eye Anatomy of the Eyeball Divided into three sections Fibrous Tunic:](https://static.fdocuments.net/doc/165x107/5ae7f9f47f8b9acc268f6a97/pptpowerpoint-presentation-north-viewexternal-anatomy-of-the-eye-lacrimal-apparatus.jpg)












![[PPT]Osteon (Haversian) System - Lone Star College – Start … · Web viewLacrimal Apparatus Lacrimal gland Canaliculi Lacrimal sac Conjunctiva Cornea Anterior cavity w/ Aqueous](https://static.fdocuments.net/doc/165x107/5ae7f9f47f8b9acc268f6a98/pptosteon-haversian-system-lone-star-college-start-viewlacrimal-apparatus.jpg)