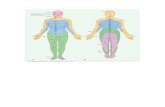
AC joint & scapula - lower limbs
-
Upload
louella-jamora -
Category
Health & Medicine
-
view
1.077 -
download
3
description
Transcript of AC joint & scapula - lower limbs

Acromioclavicular Joint
Discussed By:Louella Eunice Andrea E. Jamora, RRT

FS: 7x17” CW or 2 pcs of 8x10” CWBP: UPRIGHT, either in seating or standing position(dislocation of the AC joints tends to reduce itself in the recumbent position. Positioning can be easily modified to obtain a PA projection)PP: Ensure that the weight of the body is equally distributed on the feet to avoid rotation. It is important that the arms hang, unsupported.Make two exposures: one in which the patient is in standing without weights attached and a second in which the patient has equal weights (5 to 8 lbs.) affixed to each wrists.
Acromioclavicular ArticulationsAP Projection (Bilateral – Pearson
Method)

Note: Avoid having the patient hold weights in each hand; this tends to make the shoulder muscles contract, thus reducing the possibility of demonstrating a small acromioclavicular separation.RP: AC joint/sCR: 1. ┴ to the midline of the body at the level of the AC joints for a single projection;2. directed ┴ at each respective AC joint when two separateexposures are needed for each shoulder in broad-shouldered patientsSS: Bilateral images of the AC joints used to demonstrate dislocation, separation and function of the joints.
Acromioclavicular ArticulationsAP Projection (Bilateral – Pearson
Method)

EC: The ff. should be clearly demonstrated:• Acromioclavicular joints visualized with some soft tissue and without excessive density• Both AC joints, with and without weight , entirely included on one or two single radiographs• No rotation or leaning by the patient• Right or left and weight or non-weight markers• Separation, if done, clearly seen on the images with weight
Acromioclavicular ArticulationsAP Projection (Bilateral – Pearson
Method)

Alexander suggested that both AP and PA axial oblique projections be used in cases of suspected acromioclavicular subluxation or dislocation. Each side is examined separately. FS: 8x10” LWBP: UPRIGHT, either in seating or standing positionPP: Center the affected shoulder under examination to the grid. Adjust the patient's position to center the coracoid process to the IR.RP: coracoid processCR: 15˚ cephalad (which projects the AC joint above the acromion).
Acromioclavicular ArticulationsAP Axial Projection
(Alexander Method)

SS: The resulting image will show the AC joint projected slightly superiorly compared with an AP projection.
EC:• AC joint & clavicle projected above the acromion.• AC joint visualized with some soft tissue & w/o excessive density.
Acromioclavicular ArticulationsAP Axial Projection (Alexander Method)

FS: 8x10” LWBP: UPRIGHT, either in seating or standing position (RAO or LAO position)PP: Rotate the patient so that the MCP is 45-60˚ from the IR (to place the scapula ┴ to the IR). Pull the adjacent arm firmly across the chest (this draws the scapula laterally & forward.Although the projection can be done with the arm at the side, pulling the arm across the chest places the joint as close as possible to the IR . The scapula and AC joint are thus placed in the lateral position.RP: acromioclavicular jointCR: 15˚ caudad
Acromioclavicular Articulations
PA Axial Oblique Projection
(Alexander Method)

Acromioclavicular ArticulationsPA Axial Oblique Projection
(Alexander Method)SS: The PA axial oblique image demons the AC joint & the relationshipof the bones of the shoulder
EC:• AC joint in profile.• AC joint visualized with some soft tissue & w/o excessive density.

RAO or LAO position. FS: 10x12” CWBP: Supine or upright (If the clavicle is being examined for a fracture or a destructive disease or if the patient cannot be placed in the upright position, use the supine position to reduce the possibility of fragment displacement or additional injury.)
PP: Adjust the body to center the clavicle to the midline of the table or vertical grid device. Place the arms along the sides of the body, and adjust the shoulders to lie in the same horizontal plane.PI: Suspend respiration at the end of exhalation to obtain a more uniform density image.
Clavicle
AP Projection

RP: clavicleBP: ┴ to the midshaft of the clavicleSS: This projection demonstrates a frontal image of the clavicle.EC: • Entire clavicle centered on the image• Uniform density• Lateral half of the clavicle above the scapula, with the medial half superimposing the thorax
Clavicle
AP Projection

The PA projection is generally well accepted by the patient who is able to stand, and it is most useful when improved recorded detail is desired. The advantage of the PA projection is that the clavicle is closer to the IR, thus reducing the OID. Positioning is similar to that of the AP projection. The differences are as follows:• The patient is standing upright (PA) or prone.• The perpendicular central ray exits midshaft of the clavicle.Structures shown and evaluation Criteria are the same as for the AP projection.
Clavicle
PA Projection

RAO or LAO position. FS: 10x12” CWBP: UPRIGHT, standing or seatedPosition the patient in supine position, if unable to stand or assume the lordotic position.
PP: Have the patient lean backward in aposition of extreme lordosis, and rest the neck and shoulder against the vertical grid device. The neck will be in extreme flexion.
Center the IR to the clavicle.
PI: Suspend respiration at the end of exhalation to obtain a more uniform density image.
Clavicle
AP Axial Projection
Lordotic Position

RP: Midshaft of the clavicle.CR: *standing lordotic position, 0-15˚cephalad*supine position, 15-30˚cephaladThinner patients require more angulationto project the clavicle off the scapula and ribs.SS: An axial image of the clavicle is projected above the ribs.EC: • Most of the clavicle projected above the ribs and scapula with the medial endoverlapping the first or second rib• Clavicle in a horizontal placement• Entire clavicle along with the AC joint and SC joints
Clavicle
AP Axial Projection
Lordotic Position

Clavicle
AP Axial Projection Lordotic Position

Positioning of the PA axial clavicle is similar to the AP axial projection just described. The differences are as follow:• The patient is prone or standing, facing the vertical grid device.• The central ray is angled 15 to 30 degrees caudad.Structures shown and evaluation criteria are the same as for the AP axial projection described previously.
Clavicle
PA Axial Projection

This is particularly useful with patients who have multiple injuries/ who cannot assume the lordotic or recumbent pos.FS: 10x12” CW BP: Seated uprightPP: Adjust a sheet of leaded rubber over the gonad area. Using the collimator light as the indicator, center the IR to the projected clavicle area, and have the patient hold the IR in position.Ask the patient to lean slightly forward.RP: midshaft of the clavicleCR: Directed anterior and inferior to the midshaft of the clavicle at a 25-35˚angle, passing ┴ to the longitudinal axis of the clavicle.
Clavicle
Tangential Projection Tarrant Method

SS: The clavicle above the thoracic cage is demonstrated.EC: • Most of the clavicle above the ribs and scapula with the medial end overlapping the first or second ribs.• Clavicle in a horizontal orientation.• Entire clavicle along with the acromioclavicular and sternoclavicular joints.
Clavicle
Tangential Projection Tarrant Method

FS: 10x12” CW BP: Upright or supine (upright preferred if shoulder is tender)PP: Abduct the arm to a right angle with the body to draw the scapula laterally. Then flex the elbow, and support the hand in a comfortable position.For this projection, do not rotate the body toward the affected side because the resultant obliquity would offset the effect of drawing the scapula laterally.RP: midscapular areaCR: ┴ to a point approx. 2” inferior to coracoid process
Scapula
AP Projection

SS: An AP projection of the scapula is demonstrated.
EC: • Lateral portion of the scapula free of superimposition from the ribs.• Scapula horizontal and not obliqued.• Scapular detail through the superimposed lung and ribs (Shallow breathing should help obliterate lung detail)• Acromion process and inferior angle.
Scapula
AP Projection

Scapula
AP Projection

FS: 10x12” LW BP: Upright (RAO or LAO); the prone position can be used, but the projection will be more difficult to perform. The supine position can also be used; however, the scapula will be magnified.PP: Rotate the patient’s body 45-60˚ towards the IR. RP: midscapular areaCR: ┴ to a point approx. 2” inferior to coracoid processSS: A lateral image of the scapula is demonstrated by this projection. The placement of the arm determine the portion of the superior scapula that is superimpoedover the humerus.
Scapula
Lateral Projection

Scapula
Lateral Projection
EC: • Lateral and medial border superimposed• No superimposition of the scapular body on the ribs• No superimposition of the humerus on the area of interest• Inclusion of the acromion process andinferior angle• Lateral thickness of scapula with proper density

Scapula
Lateral Projection

FS: 10x12” LW BP: Upright (RAO or LAO); or lateral recumbent position. When the shoulder is painful, use the upright position.PP: Adjust the arm according to the projection desired.Lorenz Method: Adjust the arm of the affected side at a right angle to the long axis of the body, flex the elbow, and rest the hand againstthe patient's head.Rotate the body slightly forward, andhave the patient grasp the side of the table or the stand for support.
Scapula
PA Oblique ProjectionLorenz & Lilienfeld Method
Lorenz Method
Lilienfeld Method

PP: Lilienfeld Method:Extend the arm of the affected side obliquely upward, and have the patient rest the hand on his head.Rotate the body lightly forward, &have the patient grasp the side of the table or the stand for support
Grasp the lateral and medial borders of the scapula between the thumb & index fingers of one hand, and adjust the rotation of the body so that the scapula will be projected free of the rib cage.
Scapula
PA Oblique ProjectionLorenz & Lilienfeld Method
Lorenz Method
Lilienfeld Method

RP: protruding scapulaCR: ┴ between the chest wall & midarea of the protruding scapulaSS: An oblique image of the scapula is shown. The degree of obliquity depends on the position of the arm. The delineation of the different parts of the bone in the two oblique proj.EC: • Oblique scapula• Medial border adjacent to the ribs• Acromion process and inferior angle
Scapula
PA Oblique ProjectionLorenz & Lilienfeld Method
Lorenz Method
Lilienfeld Method

Scapula
PA Oblique ProjectionLorenz & Lilienfeld Method
Lorenz Method Lilienfeld Method

FS: 10x12” LW
BP: Supine or Upright Use the upright position when the shoulder is painful unless contraindicated.
PP: For moderate AP oblique projection,extend the arm superiorly, flex the elbow, & place the supinated hand under the head or have the patient extend the affected arm across the anterior chest.Rotate the shoulder away from the side being examined, 15-25˚.
ScapulaAP Oblique Projection
20˚ body rotation
30˚ body rotation

PP: For a steeper oblique projection: Extend the arm, rest the flexed elbow on the forehead, and rotate the body away from the affected side 25-35˚
Grasp the lateral and medial borders ofthe scapula between the thumb andindex fingers of one hand, and adjust the rotation of the body to project the scapula free of the rib cage.
For a direct lateral projection of the scapula using this position, draw the arm across the chest, and adjust the bodyrotation to place the scapula ┴ to the plane of the IR.
ScapulaAP Oblique Projection
20˚ body rotation
30˚ body rotation

CR: ┴ to the lateral border of the rib cage at the midscapular area
SS: This projection show oblique image of the scapula, projected free or nearly free of rib superimposition.
EC:• Oblique scapula• Lateral border adjacent to the ribs• Acromion process and inferior angle
ScapulaAP Oblique Projection

15-25˚ body rotation
25-30˚ body rotation
ScapulaAP Oblique Projection

FS: 10x12” CW
BP: SupinePP: Slightly abduct the affected arm, supinate the hand, immobilize with sand bags.RP: Coracoid processCR: Directed 15-45˚ cephalad. Kwak, Espiniella, & Kattan recommend 30˚.The degree of angulation depends on the shape of the patient’s back. Round-shouldered patients require a greater angulation than those with a straight back.SS: A slightly elongated inferosuperior imageof the coracoid process is illustrated.Because the coracoid is curved onitself, it casts a small, oval shadow in thedirect AP projection of the shoulder.
Scapula: Coracoid ProcessAP Axial Projection

EC: The following should be clearly demonstrated:• Coracoid process with minimal self-superimposition.• Clavicle slightly superimposing the coracoid process
Scapula: Coracoid ProcessAP Axial Projection

FS: 8x10” CW BP: SupinePP: Adjust the patient's rotation to place the body of the scapula in a horizontal position. When this requires elevation of the opposite shoulder, support it on sandbags or radiolucent sponge. Turn the head away from the shoulder being examined enough to prevent superimposition.Funke found that in the examination of patients with small breasts, clavicular superimposition can be prevented by using a 15˚ radiolucent sponge.RP: shoulderCR: Directed 45˚ caudad through the posterosuperior region of the shoulder. A 35˚ angulation suffices for obese & round shouldered patients.
Scapula: Scapular SpineTangential Projection:
Laquerriére-Pierquin Method

SS: The spine of the scapula is shown in profile and is free of bony superimposition, except for the lateral end of the clavicle.
Scapula: Scapular SpineTangential Projection: Laquerriére-Pierquin
Method

EC: • Scapular spine superior to the scapular body• Scapular spine with some soft tissue around it and without excessive density
NOTE: When the shoulder is too painful to tolerate the supine position, this projection can be obtained with the patient in the prone or upright position
Scapula: Scapular SpineTangential Projection: Laquerriére-Pierquin
Method

Scapula: Scapular SpineTangential
Projection: Prone Position
FS: 8x10” CW BP: PronePP: Adjust the shoulders & arms to lie in the same horizontal plane .Take care to prevent lateral rotation of the scapula. Have the patient rest the head on the chin or the cheek of the affected side. Supinate the hand of the affected side. Adjust a radiolucent wedge under the side of the shoulder and upper arm to place the scapula in the horizontal position.RP: Scapular spineCR: Directed 45˚ cephalad through the scapular spine then exits at the anterosuperior aspect of the shoulder. An increase in SID is recommended because of the greater OID.

Scapula: Scapular SpineTangential
Projection: Seated Upright
PositionFS: 8x10” CW BP: SeatedPP: Seat the patient with his backtoward and resting against the end of the table.Place the IR on the table, center it in line with the shoulder, & adjust the IR on a support to place it at an angle of 45˚. RP: Scapular spineCR: Directed at a 45˚ posteroinfero cephalic angle through the anterosuperior aspect of the shoulder, ┴ to the IR.An increase in SID is recommended because of the greater OID.SS: The tangential image shows the scapular spine in profile and free of superimposition of the scapular body.

Scapula: Scapular
SpineTangential Projection
EC: • Scapular spine above the scapular wing• Scapular spine with some soft tissue around it & w/o excessive density

Low
er
Lim
bs
Louella Eunice Andrea E. Jamora, RRT
Discussed by:

FS: 8x10 CW (2in1)BP: Either in seating or supine positionPP: AP: Flex the knee until foot is flat on the IR or AP Axial: Flex the knee then place a 15˚ foam wedge under the foot & place the toes near the elevated base of the wedge.RP: Third metatarsophalangeal (MTP) jointCR: 1. ┴ through the third MTP joint, when demonstration of the joint paces is not critical; 2. direct the CR 15˚ posteriorly through the third MTP joint, to open the joint spaces, or3. when a 15˚ foam wedge is used, direct the CR ┴, also to open the joint spaces.
Toes
AP or AP axial ProjectionsAP, CR ┴
AP axial, CR 15˚
AP axial, CR ┴ w/ foam wedge

Toes
AP or AP axial ProjectionsCR ┴
CR 15˚
CR ┴ w/ foam wedge
SS: The image demonstrate the 14 phalanges of the toes; the distal portions of the metatarsals; and, on the axial projections, the interphalangeal joints.
EC: The following should be clearly demonstrated:• No rotation of phalanges• Open interphalangeal & metatarsophalangealjoint spaces on the axial projections• Toes separated from each other• Distal ends of the metatarsals• Soft tissues and bony trabecular detail

FS: 8x10 CW (2in1)BP: Prone, this position naturally turnsthe foot over so that the dorsal aspect is in contact with the IR.PP: Place the toes in the appropriate position by elevating them on one or two small sandbags and adjusting the support to place the toes horizontal.Place the third metatarsophalangeal joint to the center of the unmasked half of the IR.RP: Third metatarsophalangeal (MTP) jointCR: ┴ through the third MTP joint. *The interphalangeal joint spaces are shown well because the natural divergence of the x-ray beam coincides closely with the position of the toes.SS: This projection demonstrates the 14 phalanges of the toes, the interphalangeal joints, & the distal portions of the metatarsals.
Toes
PA Projection

Toes
EC: The following should be clearly demonstrated:• No rotation of phalanges• Open interphalangeal & metatarsophalangeal joint spaces on the axial projections• Toes separated from each other• Distal ends of the metatarsals• Soft tissues and bony trabecular detail
PA Projection

FS: 8x10 CW (2in1)BP: AP Oblq: Either in seating or supine positionPA Oblq: Lateral recumbent on the affected side
PP: AP Oblq: Flex the knee until foot is flat on the IR then medially rotate the lower leg & foot, and adjust the plantar surface of the foot to form a 30-45˚ angle from the IR.PA Oblq: Have the patient turn toward the prone position until the ball of the foot formsan angle of approx. 30˚ to the horizontal, or have the patient rest the foot against a foam wedge or sandbag.
Toes
AP & PA Oblique Projections (Medial Rotation)
AP Oblique, medial rotation
PA Oblique, medial rotation

RP: Third metatarsophalangeal (MTP) jointCR: ┴ through the third MTP joint
NOTE: Oblique projections of individual toes may be obtained by centering the affected toe to the portion of the IR being used and collimating closely.
For the first and second toes: the foot may be placed in a medial oblique position; and for the fourth and fifth toes: the foot may be placed in a lateral oblique position.
*Either oblique position is adequate for the third (middle) toe.
Toes
AP & PA Oblique Projections (Medial Rotation)
AP Oblique, medial rotation
PA Oblique, medial rotation

SS: AP Oblq: An AP oblique projection of the phalanges shows the toes and the distal portion of the metatarsals rotated medially. PA Oblq: A PA oblique projection of the phalanges shows the toes and the distal portion of the metatarsals rotated laterally.EC: The following should be clearly demonstrated:• All phalanges• Oblique toes• Open interphalangeal and second through fifth metatarsophalangeal joint spaces• First metatarsophalangeal joint (not alwaysopened)• Toes separated from each other• Distal ends of the metatarsals• Soft tissue and bony trabecular detail
Toes
AP & PA Oblique Projections (Medial Rotation)
AP Oblique, medial rotation
PA Oblique, medial rotation

FS: 8x10 CW (2in1)BP: Lateral recumbent. Support the affected limb on sandbags & adjust it in a comfortable position. To prevent superimposition, tape the toes above the one being examined into a flexed position; a 4x4 inch gauze pad also may be used to separate the toes.
PP: Patient lying on the unaffected side.Great toe - 2nd toe (lateromedial projection): Center the proximal phalanx to the unmasked part of the IR, adjust to place the toe in a true lateral position. Adjust the long axis of the IR so that it is parallel with the long axis of the toe.*If the occlusal film is used, place it with the pebbled surface up between the toe being examined and the subadjacent toe.
Toes
Lateral Projection (Mediolateral or Lateromedial)
Great toe
2nd Toe
2nd Toe, w/occlusal film

PP: Patient lying on the affected side.3rd – 5th toe (mediolateral projection): Adjust the position of the limb to place the toe of I nterest and the IR or film in a parallel position, placing the toe as close to the IR or film as possible.Support the elevated heel on a sandbag orsponge for immobilization.
RP: Metatarsophalangeal joint for the great toe and Proximal interphalangeal joint of the lesser toes
CR: Perpendicular to the joint of interest.
Toes
Lateral Projection (Mediolateral or Lateromedial)
3rd Toe
5th Toe
4th Toe

PP: The resulting images show a lateral projection of the phalanges of the toe & the IP articulations projected free of the other toes.
EC: The ff. should be clearly demonstrated:• Phalanges in profile (toenail should appear lateral).• Phalanx, without superimposition of adjacent toes. When superimposition cannot be avoided, the proximal phalanx must be demonstrated.• Open interphalangeal joint spaces. The metatarsophalangeal joints will be overlapped but may be seen in some patients.• Soft tissue and bony trabecular detail.
Toes
Lateral Projection
Great Toe 2nd Toe 3rd Toe 4th Toe 5th Toe

FS: 8x10 CW (for multiple exposures)BP: Prone. Elevate the ankle of the affected side on sandbags for stability, if needed. A folded towel may be placed under the knee for comfort.PP: Rest the great toe on the table in a positionof dorsiflexion, and adjust it to place the ball of the foot perpendicular to the horizontal plane.Center the IR to the second metatarsal.RP: First metatarsophalangeal jointCR: ┴ and tangential to the 1st MTP jointSS: The resulting image shows a tangentialprojection of the metatarsal head in profileand the sesamoids.
Sesamoids
Tangential Projection Lewis Method

EC: The following should be clearly demonstrated:• Sesamoids free of any portion of the first metatarsal• Metatarsal heads
Sesamoids
Tangential Projection Lewis Method

Holly described a position that he believed was more comfortable for the patient (as compared to Lewis method). With the patient seated on the table, the foot is adjusted so that the medial border is vertical and the plantar surface is at an angle of 75˚ with the plane of the IR. The patient holds the toes in a flexed position with a strip of gauze bandage. The central ray is directed ┴ to the head of the first metatarsal bone.
Sesamoids
Tangential Projection Holly Method

Sesamoids
Tangential ProjectionCauston Method
FS: 8x10 CW (for multiple exposures)BP: Lateral recumbent, on the unaffected side & flex the knees.PP: Partially extend the limb being examined and put sandbags under the knee and foot. Adjust the height of a sandbag under the knee to place the foot in the lateral position, with the first MTP joint ┴ to the horizontal plane of the IR. Place the IR under the distal metatarsal region, and adjust it so that the midpoint will coincide with the central ray.

Sesamoids
Tangential ProjectionCauston Method
RP: First metatarsophalangeal jointCR: directed to the prominence of the 1st MTP joint at an angle of 40˚ toward the heel SS: The tangential image shows the sesamoid bones projected axiolaterally with a slight overlap.EC: • First MTP sesamoids with little overlap• Occlusal film technique• For improved detail , a similar projection may be performed using an occlusal film. The film is placed on a sandbag as illustrated and then is appropriately processed.

FootAP or AP Axial ProjectionFS: 10x12” LWBP: SupinePP: Flex the knee of the affected side enough to rest the sole of the foot firmly on the radiographic table. Center the IR to the base of the third metatarsal, and adjust it so that its long axis is parallel with the long axis of the foot. Hold the leg in the vertical position by having the patient flex the opposite knee and lean it against the knee of the affected side. In this foot position the entire plantar surface rests on the IR; thus it is necessary to take precautions against the IR slipping.Ensure that no rotation of the foot occurs.
CR ┴
CR 10˚

FootAP or AP Axial ProjectionRP: base of the 3rd MetatarsalCR: Directed in either:1. ┴ to the IR & toward the base of the 3rd metatarsal2. 10 toward the heel to the base to the 3rd metatarsal (when the CR is angled the central ray is perpendicular to the metatarsals,therefore reducing foreshortening. The tarsometatarsal joint spaces of the midfoot are Also demonstrated better)SS: The resulting image shows an AP (dorsoplantar) projection of the tarsal anterior to the talus, metatarsals, and phalanges. This projection is used for localizing foreign bodies, determining the location of fragments in fractures of the metatarsals and anterior tarsals, and performing general surveys of the bones of the foot.
CR ┴
CR 10˚

FootAP or AP Axial Projection
EC: • No rotation of the foot• Equal amount of space between the adjacentmidshafts of the second through fourth metatarsals• Overlap of the 2nd through 5th metatarsal bases• Visualization of the phalanges & tarsals distal to the talus, as well as themetatarsal s.

FootAP or AP Axial Projection

FootAP or AP Axial Projection

FootAP Oblique Projection(Medial & Lateral Rotation)
FS: 10x12” LWBP: SupinePP: Flex the knee of the affected side enough to rest the sole of the foot firmly on the radiographic table. Medial Rotation: Rotate the patient's leg medially until the plantar surface of the foot forms an angle of 30˚ to the plane of theIR. If the angle of the foot is increased more than 30˚, the lateral cuneiform tends to be thrown over the other cuneiforms.
A greater rotation can be helpful in demonstrating the joint spaces of the foot.
Medial Rotation
Lateral Rotation

FootAP Oblique Projection(Medial & Lateral Rotation)
PP: Lateral Rotation: Rotate the leg laterally until the plantar surface of the foot forms an angle of 30˚ to the IR. Support the elevated side of the foot on a 30˚ foam wedge to ensure consistent results.
RP: base of the 3rd metatarsalCR: ┴ to the base of the third metatarsal
Medial Rotation
Lateral Rotation

FootAP Oblique Projection(Medial & Lateral Rotation)
SS: Medial Rotation: The resulting image shows the interspaces between the ff.: 1. the cuboid & the calcaneus; 2. the cuboid & the fourth & fifth metatarsals; 3. the cuboid & the lateral cuneiform; and 4. the talus and the navicular bone.
The cuboid is shown in profile. The sinus tarsi is also well demonstrated.
Medial Rotation

FootAP Oblique Projection(Medial & Lateral Rotation)
EC: The following should be clearly demonstrated:• Third through fifth metatarsal basesfree of superimposition• Lateral tarsals with less superimposition than in the AP projection• Lateral tarsometatarsal & intertarsaljoints• Sinus tarsi• Tuberosity of the fifth metatarsal• Bases of the 1st & 2nd metatarsal• Equal amount of space between the shafts of the 2nd -5th metatarsals• Sufficient density to demonstrate thephalanges, metatarsals, and tarsals.
Medial Rotation

FootAP Oblique Projection(Medial & Lateral Rotation)
SS: The resulting image show the interspaces between the 1st & 2nd metatarsals and between the medial & intermediate cuneiforms.
EC: The following should be clearly demonstrated:• Separate first and second metatarsalbases• No superimposition of the medial &intermediate cuneifonns• Navicular bone more clearly demonstrated than in the medial rotation• Sufficient density to demonstrate thephalanges, metatarsals, and tarsals
Lateral Rotation

FootPA Oblique ProjectionGrashey Methods
(Medial or Lateral Rotation)FS: 10x12” LWBP: PronePP: Elevate the affected foot on sandbags.Adjust the elevation of the patient's foot to place its dorsal surface in contact with the IR.Position the IR under the foot, // with its long axis, & center it to the base of the 3rd metatarsal.*To demonstrate the interspace betweenthe first and second metatarsals, rotatethe heel medially approximately 30 degrees.*To demonstrate the interspaces between the second and third, the third and fourth, and the fourth and fifth metatarsals, adjustthe foot so that the heel is rotated laterally approximately 20 degrees.
PAO, 30˚ lateral rot.
PAO, 20˚ medial rot.

FootPA Oblique ProjectionGrashey Methods
(Medial or Lateral Rotation)RP: base of the 3rd metatarsalCR: Perpendicular to the base of the 3rd MTSS: The resulting image shows a PA obliqueprojection of the bones of the foot & theinterspaces of the proximal ends of the metatararsal.EC: The following should be clearly demonstrated:Heel medially rotated 30 degrees:• 1st & 2nd metatarsal bases free of superimposition• Medial cuneiform projected w/o superimposition• Navicular bone seen in profileHeel laterally rotated 20 degrees: • Third through fifth metatarsal base free of superimposition• Tuberosity of the fifth metatarsal and cuboid
PAO, 30˚ lateral rot.
PAO, 20˚ medial rot.

FootGrashey Methods (Medial or Lateral Rotation)
PAO, 30˚ lateral rot.
PAO, 20˚ medial rot.

FootPA Oblique ProjectionMedial Rotation
This is essentially the same proj. as the AP oblique foot projection. Placing the lateral aspect of the foot closer to the IR & using a 45˚ medial rotation can provide better visualization of the bones of the foot.FS: 10x12” LWBP: Lateral recumbent on the affected side, & flex the knees.PP: Fully extend the leg of the side being examined.• Have the patient turn toward the prone position until the plantar surface of the foot forms an angle of 45˚ to the IR.• Center the IR opposite the base of the fifth metatarsal, and adjust it so that its midline is // with the long axis of the foot.• Rest the dorsum of the foot against a foam wedge. The general survey study is usually made with the foot at an angleof 45˚ to obtain uniform results.
PAO medial rot.

FootPA Oblique ProjectionMedial Rotation
RP: base of the fifth metatarsalCR: ┴ to the midline of the foot at the level of the base of the fifth metatarsalSS: The resulting image shows a PA oblique projection of the bones of the foot. The articulations between the cuboid and the adjacent bones (the calcaneus, lateral cuneiform, and fourth and fifth metatarsals) are clearly shown. The articulations between the following bones are usually shown:
1. talus and navicular bone; 2. navicular bone and cuneiforms; and 3. sustentaculum tali and talus.
The cuboid is shown in profile.
PAO medial rot.

Foot PA Oblique Projection Medial RotationEC: The following should be clearly demonstrated:
• A more oblique projection than obtained with the Grashey method• 3rd to 5th metatarsal bases and the tarsals• Tarometatarsal and intertarsal joints• Tuberosity of the fifth metatarsal• Some superimposition of the first & second metatarsals• Sufficient density to demonstrate the phalanges, metatarsals, and tarsals.

Foot Lateral ProjectionMediolateral & Lateromedial
RotationThe mediolateral projection is routinely used in most radiology departments because it is a comfortable position for the patient to assume.
The lateromedial projection, however, is the recommended alternative when the patient's condition permits (in the absence of an unusually prominent medial malleolus, hallux valgus, or other deformity). The foot assumes an exact or nearly exact lateral position when resting on its medial side. Although the medial position may be more difficult for some patients to achieve, true lateral projections are more easily & consistently obtained with the foot in this position.
mediolateral rot.
lateromedial rot.

Foot Lateral ProjectionMediolateral & Lateromedial
RotationFS: 10x12” LWBP: For the mediolateral: Recumbent, turn toward the affected side;For the lateromedial: Semi-supine (RPO or LPO) then turn toward the unaffected side, until the leg & foot are lateral. Place the opposite leg behind the patient.
PP: Elevate the patient‘s knee enough to place the patella ┴ to the horizontal plane, and adjusta sandbag support under the knee. Center the IR to the midarea of the foot, and adjust it so that its long axis is parallel with the long axis of the foot.ML: Dorsiflex the foot to form a 90˚ angle with the lower leg.LM: Adjust plantar surface to be ┴ to the IR.
mediolateral rot.
lateromedial rot.

Foot Lateral ProjectionMediolateral & Lateromedial
Rotation
mediolateral rot.
lateromedial rot.
RP: base of the third metatarsal
CR: ┴ to the base of the third metatarsal
SS: ML: The resulting image shows the entire foot in profile, the ankle joint, & the distal ends of the tibia & fibula.
LM: The resulting image shows a true lateromedial projection of the foot, ankle joint,and distal ends of the tibia and fibula

Foot Lateral Projection Mediolateral & Lateromedial Rotation
EC: The following should be clearly demonstrated:Mediolateral:• Metatarsals nearly superimposed• Distal leg• Fibula overlapping the posterior portion of the tibia• Tibiotalar joint• Sufficient density to demonstrate the superimposed tarsals and metatarsals
EC: The ff. should be clearly demons:Lateromedial:• Metatarsals usually more superimposed than in the mediolateral image, depending on the transverse arch of the foot• Distal leg• Fibula overlapping the posterior portion of the tibia• Tibiotalar joint• Sufficient density to demonstrate the superimposed tarsals and metatarsals

FootLa
tera
l Pro
ject
ion
M
ed
iola
tera
l &
Late
rom
edia
l R
ota
tion
mediolateral rot.
lateromedial rot.

Foot: Longitudinal ArchLateral Projection
(Lateromedial) Weight-Bearing Method (standing)FS: 10x12” LW
BP: Upright position, preferably on a low riser that has an IR groove. If such a riser is not available, use blocks to elevate the feet to the level of the x-ray tube.PP: Place the IR in the IR groove of the stool. Have the patient stand in a natural position, one foot on each side of the IR, with the weight of the body equally distributed on the feet.Adjust the IR so that it is centered to the base of the 3rd metatarsal.After the exposure, replace the IR & position the new one to image the opposite foot.

Demo:
Pes Planus / Status of
Longitudinal Arch
Bohler’s Critical Angle
angle between the superior apex of the
midcalcaneous to the ant.
process of the calcaneous
Foot: Longitudinal ArchLateral Projection
(Lateromedial) Weight-Bearing Method (standing)RP: base of the third
metatarsalCR: ┴ to a point just above the base of 3rd metatarsalSS: The resulting image shows a lateromedialprojection of the bones of the foot with weight-bearing. The projection is used to demonstrate the structural status of the longitudinal arch. The right and left ides are examined for comparison.

Foot: Longitudinal Arch
Lateral Projection (Lateromedial) Weight-Bearing Method (standing)
EC: • Superimposed plantar surfaces of themetatarsal heads• Entire foot and distal leg• Fibula overlapping the posterior portionof the tibia• Sufficient density to visualize the superimposedtarsals and metatarsals

Foot AP Axial Projection Weight-Bearing Method
(standing)FS: 10x12” LW SID: 48 inches. This SID is used to reduce magnification and improve recorded detail in the image.BP: Upright position, preferably on a low riser that has an IR groove. If such a riser is not available, use blocks to elevate the feet to the level of the x-ray tube.PP: • Place the IR on the floor, & have the patient stand on the IR with the feet centered on each side.• Ensure that right and left markers and an upright marker are placed on the IR.• Ensure that the patient's weight is distributed equally on each foot.• The patient may hold the x-ray tube crane for stability.

Foot AP Axial Projection Weight-Bearing Method
(standing)RP: base of the third metatarsalCR: 10-15˚ towards the heel at the level of the base of the third metatarsalSS: The resulting image demonstrates a weight-bearing AP axial projection of both feet permitting an accurate evaluation and comparison of the tarsal and metatarsal.EC: The ff. should be clearly demonstrated:• Both feet centered on one image• Phalanges, metatarsal , and distal tarsals• Correct right and left marker placementand a weight-bearing marker• Correct exposure technique to visualizeall the components

Foot AP Axial Projection Weight-Bearing Method
(standing)

Foot AP Axial Projection Weight-Bearing
Composite Method (standing)FS: 10x12” LW BP: Standing-upright position. The patient should stand at a comfortable height on a low stool or on the floor.PP: With the patient standing upright, adjustthe IR under the foot and center its midline to the long axis of the foot.
To prevent superimposition of the leg shadow on that of the ankle joint, have the patient place the opposite foot one step backward for the exposure of the forefoot (1st exposure) and one step forward for the exposure of the hind foot or calcaneus (2nd exposure).

Foot AP Axial Projection Weight-Bearing Composite Method
(standing)RP: Level of the third metatarsal & ankleCR: To use the masking effect of the leg, direct the CR along the plane of alignment of the foot in both exposures.1st exposure. With the tube in front of the patient & adjusted for a posterior angulation of 15˚, center the CR to the base of the 3rd metatarsal for the 1st exposure.Caution the patient to carefully maintainthe position of the affected foot & place the opposite foot one step forward in preparation for the 2nd exposure.

Foot AP Axial Projection Weight-Bearing Composite Method
(standing)CR: 2nd exposure. Move the tube behind the patient, adjust it for an anterior angulation of 25˚, and direct the central ray to theposterior surface of the ankle.
The central ray emerges on the plantar surface at the level of the lateral malleolus.
An increase in technical factors is recommended for this exposure.
SS: The resulting image shows a weight-bearing AP axial projection of all bones of the foot. The full outline of the foot is projected free of the leg.

FootAP Axial Projection
Weight-Bearing Composite Method
(standing)
EC: The ff. should be clearly demonstrated:• All tarsals• Shadow of leg not overlapping the tarsals• Foot not rotated• Tarsal , metatarsals, and toe with similardensities