Abdominoperineal Resection Miles
description
Transcript of Abdominoperineal Resection Miles

A
C
Otttsst4sesslsdflrpd
tceswiawcd
iTwhpas
T
5
2
bdominoperineal Resection
lifford L. Simmang, MD, MS, FACS, FASCRS
pf
tcbolnspattCgd
mplftmccpgap
cpcwdescadiosTa
ver the past few decades there have been significantadvances in adjuvant therapy for malignant condi-
ions of the anus and low rectum, as well as medicalherapy for inflammatory bowel disease involving the rec-um and anal canal. Many of these advances have allowedphincter-sparing operations and in some cases, the pos-ibility to delay or avoid surgery. In 2003, it is predictedhat there will be 42,000 new cases of rectal cancer and000 cases of anal cancer.1 Although the possibility ofphincter sparing surgery following neoadjuvant therapyither with a low double stapled anastomosis or an inter-phincteric dissection and hand sewn coloanal anastomo-is may be possible in many patients with cancer of theow rectum, when the sphincter complex is involved,phincter sparing operations are not possible. In addition,espite significant advances in medical therapy for in-ammatory bowel disease, abdominoperineal excision isequired for most patients undergoing surgery for Crohn’sroctitis and is occasionally selected as the operative proce-ure of choice by a few patients with ulcerative colitis.Indications for abdominoperineal resection include
hose patients with a malignancy involving the sphincteromplex,2 patients with Crohn’s proctitis and anal dis-ase,3 patients with ulcerative colitis preferring to have atoma or those patients with any of the above conditionsho already suffer with incontinence and would be debil-
tated by a low anterior, coloanal, or ileal pouch analnastomosis. These patients have a superior quality of lifeith their stool evacuation from either an ileostomy or a
olostomy into a contained bag allowing them the free-om to live a normal life.Preoperative preparation and education of the patient
s important before creating a stoma. An Enterostomalherapist (ET) should visit with the patient and discusshat a stoma is and what appliances are available andow they would function. The ET nurse will then performreoperative stoma siting. The stoma should be sitedway from creases and in a location that the patient canee. It is preferable to mark more than one location in the
From the University of Texas Southwestern Medical Center at Dallas, Dallas,X.Address reprint requests to Clifford L. Simmang, MD, MS, FACS, FASCRS,
323 Harry Hines Blvd., Dallas, TX 75390-9156.© 2004 Elsevier Inc. All rights reserved.1524-153X/04/0504-0006$30.00/0
pdoi:10.1053/joptechgensurg.2003.10.005
40 Operative Techniq
ossibility that the bowel may not easily reach the pre-erred location and an alternative site should be marked.
In preparation for an abdominoperineal resection, pa-ients undergo a standard bowel preparation with me-hanical evacuation of the large bowel often using aalanced electrolyte solution (GoLytely�, Braintree Lab-ratories, Braintree, MA) along with an antibiotic prophy-axis. We use a combination of neomycin 1 g and metro-idazole 1 g at 1 PM, 2 PM, and 9 PM the evening beforeurgery. Bowel preparation is performed at home and theatients arrive to the hospital before their planned oper-tive procedure. Before the start of the operation, addi-ional antibiotic prophylaxis is given intravenously. Al-hough many antibiotic regimens are appropriate, we useefotetan� (Astra-Zeneca, Wilmington, DE) 2 g before sur-ery and 1 g at 12 and 24 hours later. After the perioperativeosing of antibiotics, further antibiotics are not used.In the operative room the patient is positioned in aodified lithotomy position (Fig 1). The rectum is pre-
ared by insertion of a 32 French Malecot catheter fol-owed by lavage with normal saline solution. Once clear,ull strength Betadine solution is instilled within the rec-um for its tumorocidal properties. The Malecot catheteray be left as a drainage tube for evacuation of residual
olonic contents during the operation and to prevent ac-umulation of residual stool in the rectum during theelvic or perineal dissection. Alternatively, some sur-eons prefer to encircle the anal canal with a suture such as#1 Prolene to occlude the anal orifice. If the procedure iserformed for anal cancer, this often is not possible.Most commonly, a midline incision is created and
urves around the umbilicus opposite the side of thelanned stoma. If a colostomy is planned the incision willurve to the right of the umbilicus and if an ileostomyere planned it would then curve to the left. The fascia isivided along the linea alba and the peritoneal cavity isntered. On entering the peritoneal cavity explorationhould be performed. In patients with malignant disease,areful palpation of the liver is important and intraoper-tive ultrasonography can be performed. The upper ab-ominal contents should be gently palpated and then thentestines inspected. After palpating the stomach and du-denum, the small bowel should be palpated and in-pected from the ligament of Treitz to the ileocecal valve.his is to identify concomitant pathology that may needttention at the time of this operation. The colon is then
alpated throughout, as are the retroperitoneal structures.ues in General Surgery, Vol 5, No 4 (December), 2003: pp 240-256

alctrntdacuwvcdlttt
dIIAfp
ptacv
tCbthdni4ftrfcdniws
1oEScoo
241Abdominoperineal Resection
Mobilization is begun by incising the lateral peritonealttachments just above the white line of Toldt. This al-ows entry into an areolar fusion plane (Fig 2). As theolon is further mobilized, a second fusion plane is iden-ified and dissection continues in this plane allowing theetroperitoneal structures to remain posterior. The go-adal vessels are seen and identified first (Fig 2). The nextubular structure is the ureter and it is important in allissections of the left colon to clearly identify the ureternd avoid injury. Following mobilization of the sigmoidolon this can be carried superiorly and the splenic flex-re mobilized. Once lateral mobilization is complete, aindow is created underneath the superior hemorrhoidalessels at the level of the sacrum (Fig 2). The peritoneuman be opened distally to allow enlargement of this win-ow. The peritoneum is then incised proximally at thisevel just below the superior hemorrhoidal vessel. Con-inuing in this plane superiorly will lead to the origin ofhe inferior mesenteric artery (IMA). Once encountered,he IMA is ligated near its origin from the aorta.
Adjacent is the inferior mesenteric vein, which is thenivided between clamps. Although I prefer to divide theMA near its origin (Fig 3), some surgeons will divide theMA after the take off of the left ascending colic artery.lthough no oncologic benefit has been demonstrated
rom a high ligation of the IMA, a high ligation does
rovide a significant increase in the mobility of the colon. iperation. Once in position, the anal canal may be closed with a he
Once the major arterial trunk is divided this defines theroximal margin of resection. The mesentery is divided tohe colon, which will be near the junction of the descendingnd sigmoid colon. The colon is then divided with a linearutting stapling device, which allows separation and pre-ents spillage or contamination of colonic contents (Fig 3).
Once the colon is divided, attention is directed towardhe pelvic dissection. This is begun in the posterior plane.ontinuing to mobilize the rectum in the avascular em-ryonic fusion plane will allow a total mesorectal excisiono be performed using a nerve sparing technique as theypogastric nerves can be readily identified during thisissection (Fig 4). There will be branches given off as theerves traverse the pelvis, but the main trunk should be
dentified and preserved during the main dissection (Fig). A deep pelvic St. Mark’s type retractor is very usefulor getting lift on the rectum and allowing this areolarissue plane to become readily visible. Dissection of theectum should be performed sharply under vision. I pre-er to use electrocautery as it does aid in hemostasis espe-ially in the area of the lateral stalks (Fig 5). As progressissecting the posterior rectum continues and tethering isoted from the lateral peritoneal reflection, this should be
ncised and divided. This will allow for further mobilityith the rectum. Sharp dissection will allow sharp divi-
ion of Waldeyer’s fascia. Blunt pelvic dissection by slid-
ng the operator’s hand behind the rectum has led to aLithotomy positioning. The operative position for a synchronous abdominoperineal resection is low lithotomy. This is mostften accomplished with the use of adjustable stirrups to allow for a gentle flex at the knees and elevation of the lower extremities.levation of the lower extremities assists in promoting venous drainage, which may reduce the incidence of venous thrombosis.equential compression devices are also used for prophylaxis not only for venous thromboembolism, but also as an additionalushion to prevent nerve injury. The patient’s position must be inspected for appropriate padding. A soft roll, which may be a sheetr a blanket, may be placed underneath the patient’s buttocks to aid in elevation and exposure for the perineal portion of the
avy suture to prevent perineal contamination.

hhsstctvtDouatr7vtttIppsrsn(pmDcwcTac
cAbaadgasctcsprpsi
ubtnbIdacm1ar
fotpwipcsamp
2pwasctotap
sTlmttTscipleima
242 Clifford L. Simmang
igher incidence of rectal perforation because of the ad-erence of Waldeyer’s fascia. Sharp dissection and divi-ion will decrease this complication. Circumferential dis-ection is now performed by incising the peritoneum athe base of the cul-de-sac. For a low rectal cancer, espe-ially if this is in an anterior location, the anterior dissec-ion should be performed on the prostate side of Denon-illiers’ fascia (Fig 6). If the tumor is posterior, and thenhe anterior dissection in men may be on the rectal side ofenonvilliers’ fascia, which will decrease the likelihoodf nerve injury. This circumferential dissection is contin-ed until a complete mesorectal dissection is performednd the rectum has coned down to the narrow muscularube as it enters into the anal canal. In women, the ante-ior dissection begins at the depth of the cul-de-sac (Fig) and proceeds through the avascular plane in the recto-aginal septum. If adherence is noted during this dissec-ion, especially anteriorly, it may be prudent to wait forhe perineal operator to begin and approach the mostethered area simultaneously abdominally and perineally.f the tumor is tethered to the posterior vaginal wall, aosterior vaginectomy should be performed (Fig 8). Theerineal approach begins with a standard posterior inci-ion, however the anterior incision proceeds to incorpo-ate an ellipse of the posterior vagina (Fig 9). Once thepecimen is delivered, the posterior vagina and the peri-eal body can be reconstructed with absorbable suturesFig 10). The proximal end of the colon can be passedosteriorly to better visualize the last anterior attach-ents (Fig 10). In men, if the tumor appears tethered toenonvilliers’ fascia, a superficial layer of the prostate
apsule can be encorporated. However, if there is invasionithin the prostate, a combined en bloc proctectomy with
ystoprostatectomy (anterior exenteration) is required.his possibility should have been detected, discussed,nd planned for preoperatively and a surprise in this lo-ation should not occur.
The perineal dissection is most often performed syn-hronously with the completion of the pelvic dissection.n elliptical incision is made centering on the perinealody anteriorly and the mid point between the anal canalnd the coccyx posteriorly (Fig 11A). The skin is incisednd the incision is carried into the ischiorectal fat. Thisissection is performed circumferentially by continuallyoing from one location and one side to another tochieve length and advance the dissection. The dissectionhould be in the ischiorectal fat outside of the sphincteromplex. The neurovascular bundle to the anus enters inhe posterolateral location and caution should be exer-ised with dissection in this area and anticipate the pos-ible need for hemostatic control. I prefer to enter theeritoneal cavity in the posterior location. A malleableetractor can be inserted deep into the pelvis and easilyalpated by the perineal surgeon. Using cautery, the inci-ion can be carried directly onto this retractor. Once entry
nto the peritoneal cavity is gained, the dissection contin- tes circumferentially on either side. At times a finger cane placed through this opening and the surgeon can cau-erize through the levators onto his finger on the perito-eal pelvic side (Fig 11B). This division is continued onoth sides leaving the anterior dissection yet to complete.f the plane of dissection is clearly defined, the anteriorissection is completed (Fig 11C). However, if there isdherence or the operative planes are difficult, exposurean be improved by passing the proximal end of the sig-oid colon out the posterior opening of the levators (Fig
0). This allows traction from both the proximal and distalspects of the rectum and can aid in helping define the planeequired for transection to achieve a grossly clear margin.
There are special considerations when performing APRor anal cancer or IBD. For patients with IBD where thisperation is being performed for an inflammatory condi-ion of the rectum, an intersphincteric proctectomy isreferred.4 This achieves resection of all diseased bowelhile limiting the size of the perineal wound and increas-
ng the likelihood for primary healing. However, for thoseatients with anal cancer, especially if there is a significantomponent onto the anal margin, a wide perineal skin exci-ion will be required. This wound cannot be closed primarilynd must then be repaired with a flap. A very difficult wounday be treated with wound care or even a wound vac to
romote healing or allow the addition of a flap.The perineal wound is closed in layers. I use a series of
-0 figure of eight absorbable sutures and attempt to ap-roximate the levators, if possible. If this has been a veryide excision, there will be little left and all that can be
pproximated is the subcutaneous ischiorectal fat. There areufficient fibrous septae running through this fat to allow forlosure. The skin is closed with subcuticular sutures. One orwo pelvic drains are placed abdominally and are broughtut through separate abdominal stab incisions. I believe thatransabdominal drainage is preferable to perineal drainage,s this is as effective and much more comfortable for theatient. Some surgeons omit drainage all together.The colostomy is fashioned by excising a quarter-
ized disc of skin and core of subcutaneous fat (Fig 12).he anterior rectus sheath is identified and incised
ongitudinally. The skin and fascia are kept in align-ent by the use of Kocher clamps to assure that after
he colostomy is brought straight through and whenhe skin is later closed, that the angle does not change.he abdominal wall is then elevated as a curved Mayocissors is passed between the fibers of the rectus mus-le and the tips are opened to allow a longitudinalncision of the posterior rectus sheath to be made. Theassage through the rectus is then maintained and di-
ated to allow two fingers to easily pass through. Thend of the colon is then brought up through this open-ng and will be allowed to remain there until the abdo-
en is closed (Fig 13). It is matured as the last step tovoid contamination of the incision. It is not necessary
o tack the colostomy to the posterior fascia. The mid-
ltbndsA
tfpttpt
2tlifttpF
243Abdominoperineal Resection
ine incision is closed and the staple line excised fromhe distal end of the colon. The colostomy is maturedy performing interrupted sutures in the colon begin-ing at the mucoserosal junction with about 1 cm ofistal colon within this suture and then placing theuture through the skin about 5 mm from the edge.lthough subcuticular sutures are preferable when ma-
uring ileostomies, colostomies can be matured with aull thickness of skin. Some surgeons will also encor-orate a three-point suture fixation everting the colos-omy much like a Brooke ileostomy is performed. Al-hough this is not necessary for a colostomy, it will helprevent retraction. A stoma appliance it then placed aroundhe stoma and a dressing placed over the incision.
Left colon mobilization. After entry into the abdominal cavity and thorough exploration, the operation is begun by mobiliza-ion of the left colon. Although some surgeons will begin with a high ligation of the IMA, performing the “no touch” technique byigating the vascular pedicle before colonic manipulation, most surgeons begin with lateral mobilization. The peritoneal reflections incised with electrocautery. This incision lies just inside the white line of Toldt. As the colon is elevated a second retroperionealusion plane is identified and dissection progresses in the avascular areolar tissue plane. As this progresses medially, the first set ofubular structures to be encountered will be the gonadal vessels. Key to avoiding injury to the ureter is to recognize that inferior tohe IMA, the ureter lies medial to the gonadal vessels. The ureter is identified next and the colon is mobilized proximally. Thisroximal mobilization is carried superiorly and around the splenic flexure to provide adequate mobility of the left colon, as needed.ollowing mobilization of the left colon a plane is developed underneath the superior hemorrhoidal artery.

3utcp
244 Clifford L. Simmang
High ligation of the inferior mesenteric artery. A window is created on the right, medial side of the sigmoid colon mesenterynderneath the superior hemorrhoidal artery. The peritoneum is then incised just inferior to the superior hemorrhoidal artery andhis window is enlarged until the inferior mesenteric artery is encountered. The inferior mesenteric artery is then divided betweenlamps and ligated. This division defines the mesenteric dissection leading to the site on the colon, which will represent the
roximal margin that was defined by division of its vascular mesentery. The colon is divided with a linear cutting stapling device.
4tsSpsgattlst
245Abdominoperineal Resection
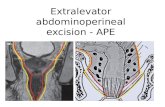
Autonomic nervous plexus and innerva-ion of the pelvic structures. The most commonites for potential nerve injury can be seen.ympathetic injury may occur at the aorticlexus near the origin of the IMA or over theacral promontory at the division of the hypo-astric nerves from the hypogastric plexus. Inddition to sympathetic injury, parasympa-hetic injury may occur during lateral dissec-ion, especially when there is division of theateral ligaments or anterolaterally during dis-ection behind the seminal vesicles and pros-ate.

5lvpCE
246 Clifford L. Simmang
Division of lateral ligaments. A fibrous condensation containing the middle hemorrhoidal vascular pedicle makes up the lateraligaments. Traction on the rectum to the opposite side will allow this structure to be identified as a curtain of tissue. Often, thisascular pedicle is not prominent and can be divided by cautery, especially if the patient has undergone neoadjuvant therapy. If arominent vascular pedicle is present, it may be divided between ties, clips, with an ultrasonic device (Autosonics� US Surgicalorporation, Harmonic Scalpel� Ethicon Endosurgery) or using a vascular endoscopic stapler (US Surgical Corporation, Ethiconndosurgery).

6astFa
247Abdominoperineal Resection
Anterior dissection in men. Following the posterior dissection the lateral peritoneum is incised. An incision is made 5 mmnterior to the fold of the cul-de-sac. The seminal vesicles are exposed and using sharp dissection most commonly with cautery, theeminal vesicles are cleared. The plane of dissection continues anterior to encompass Denonvilliers’ fascia until the junction withhe prostatic capsule. Further distal dissection is between the mesorectal fat and the prostatic capsule, staying as wide as possible.or a tumor in the anterior location Denonvilliers’ fascia should be separated from the prostatic capsule as needed to provide a clear
nd free radial margin from the tumor.
248 Clifford L. Simmang
7 Anterior dissection in women.When present, uterine traction su-periorly helps lift the anterior as-pect of the cul-de-sac. The perito-neum is incised with cautery at theperitoneal reflection. Dissectionproceeds along the rectovaginalseptum in an areolar tissue plane.The posterior vaginal surface canbe identified by its white encom-passing visceral fascial layer. Dis-section proceeds throughout therectovaginal space exposing the an-terior junction of the levators at thelevel of the perineal body. At thispoint the lateral sidewalls dissec-tion can be completed.

8vTcgpnhiv
249Abdominoperineal Resection
Anterior rectal cancer involving the recto-aginal septum requiring posterior vaginectomy.his dissection may be performed either by a syn-hronous team in the lithotomy position or a sin-le operative team approach where the abdominalortion has been completed and the operation isow performed in prone position as demonstratedere. Lines for transection are shown encorporat-
ng the colon, sphincter complex and posterioragina next to where the rectal lesion is located.

250 Clifford L. Simmang
9 Outlines the lines ofthe perineal dissection in-cluding the posterior wallof the vagina.

1ibaa
251Abdominoperineal Resection
0 Posterior vaginal wall is resectedn continuity with the rectum beginningelow the cervix at the level needed forn adequate margin. The vagina is closednd perineum reconstructed.

252 Clifford L. Simmang
11 Perineal dissection. (A)The lines of transection are dia-gramed. The posterior pelvis isentered by an incision throughthe anococcygeal raphe and theposterior levators. This can befacilitated by placement of anabdominal retractor at the depthof the pelvis serving as a target.(B) Once the posterior plane hasbeen entered, the levators aretransected laterally and can beguided by placement of a fingeror instrument into the pelvisthrough the open area of the le-vators and they are transectedon both sides.

1io
253Abdominoperineal Resection
1 (continued) (C) The remaining anterior attachments are now divided. This is often performed last to minimize the risk ofnjury to the urethra and prostate in males which lie directly anterior to this dissection (at times this can be facilitated by delivery
f the proximal rectum through the posterior wound helping to define the remaining anterior attachments).
1plr
254 Clifford L. Simmang
2 Construction of an end colostomy. Selection of stoma location. A quarter-sized disc of skin is excised at the colostomy sitereviously marked. The anterior rectus sheath is split longitudinally. The rectus muscles are separated and the peritoneum is incised
ongitudinally as well. The skin and fascia should remain at the same level to provide for a straight tunnel or opening through theectus that does not change at the end of the operation when the skin is closed.

Pawottpich
Occmrt5c1japba
btbpbuhpppipFfttsnbncn
hsc
1tcAt
255Abdominoperineal Resection
POSTOPERATIVE CARE
ostoperatively, a Foley catheter is left for urinary drain-ge for 4 to 5 days. Men, especially, may have difficultyith voiding. After pelvic dissection, there is some laxityf the anterior support as well as swelling and edema fromhe procedure, which may lead to voiding difficulties inhe first few days. The pelvic drains are left until theyroduce less than 50 mL of drainage per day or have beenn for 5 to 7 days and the patient is preparing for dis-harge. I remove pelvic drains before the patient goesome.
RESULTS
perating within the confined space of the pelvis in-reases the difficulty and complexity of surgery for rectalancer. Difficulty in achieving circumferential and radialargin has been associated with a much higher local
ecurrence rate in patients with rectal cancer than pa-ients with colon cancer. Recurrence rates of 31%5 to3%2 have been reported. However, results from otherenters have reported recurrence rates as low as 6%6 to0%.7 These centers have used a combination of neoad-uvant, intraoperative, and postoperative adjuvant ther-py to reduce local recurrence. Most centers have re-orted no significant difference in the local recurrenceetween patients undergoing an anterior resection and an
3 The colon is delivered throughhe abdominal wound and remainslosed until after the skin is closed.fter closure of the wound the colos-
omy is matured.
bdominoperineal resection. p
The morbidity of abdominoperineal resection haseen found to be significantly worse than those pa-ients undergoing anterior resection.6,8 Overall mor-idity with complications occurring in 50% to 60% ofatients are reported.6,8 An increase in intraoperativeleeding, requirement for transfusion, operative time,rinary and sexual dysfunction, and delayed healingave been reported. Sexual dysfunction has been re-orted in 8% to 55% of patients undergoing abdomino-erineal resection. Perineal wound dehiscence of ap-roximately 10% is reported, however, perineal wound
nfection and dehiscence is found in 30% to 40% ofatients who have undergone preoperative radiation.8
or patients undergoing abdominoperineal resectionor inflammatory bowel disease, intersphincteric pro-ectomy has been associated with complete healing ofhe perineal wound in 84% of patients by 6 months,exual dysfunction with impotence in 6%, and report ofo bladder dysfunction.4 Creation of omentoplasty haseen reported to facilitate perineal healing.9 This tech-ique was reported in 20 cases where an omental pedi-le graft was placed and primary healing of the peri-eum occurred in all patients.Although laparoscopic abdominoperineal resection
as been reported and compared favorably with openurgery,10 abdominoperineal resection is a compli-ated operative procedure and laparoscopic ap-
roaches should be reserved for experienced laparo-
stacpno
1
256 Clifford L. Simmang
copic surgeons. Despite advances in surgicalechnique along with improvements in neoadjuvantnd adjuvant therapy, the surgical treatment of rectalancer involving the pelvic floor and sphincter com-lex remains complicated. Strict attention to the tech-ical details of this operation are required to achieve anptimal surgical outcome.
REFERENCES
1. Jemal A, Murray T, Samuels A, et al: Cancer statistics, 2003. CACancer J Clin 53:5-26, 2003
2. Fegiz G, Indinnimea M, Gozzo P, et al: Low rectal cancer—what isthe choice? Dis Colon Rectum 37:535-541, 1994
3. Regimbeau J, Panis Y, Marteaus P, et al: Crohn’s disease: Canabdominoperineal resection be predicted? J Am Coll Surg 189:
171-176, 19994. Zeitels J, Fiddian-Green R, Dent T: Intersphincteric proctatec-tomy. Surgery 96(4):617-623, 1984
5. Rullier E, Laurent C, Carles J, et al: Local recurrence of low rectalcancer after abdominoperineal and anterior resection. Br J Surg84:525-528, 1997
6. Nissan A, Guillem J, Paty P, et al: Abdominoperineal resection forrectal cancer at a specialty center. Dis Colon Rectum 44:27-35,2001
7. Tschmelitsch J, Kranberger P, Prommegger R, et al: Survivaland local recurrence after anterior resection and abdomino-perineal excision for rectal cancer. Eur J Surg Oncol 21:640-643,1995
8. Farid H, O’Connell T: Methods to decrease the morbidity of ab-dominoperineal resection. Am Surg 61:1061-1064
9. Rice M, Hay A, Hurlow R: Omentoplasty in abdominoperinealresection of the rectum. Aust NZ J Surg 62:147-149, 1992
0. Fleshman J, Wexner S, Anvari M, et al: Laparoscopic vs openabdominoperineal resection for cancer. Dis Colon Rectum 42:
930-939, 1999