2020.11.04 Lecture PNS tumor and tumorlike
Transcript of 2020.11.04 Lecture PNS tumor and tumorlike

03/11/2020
1
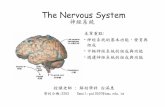
Paranasal sinus Tumors and tumor like lesions
Carolina Tramontini, M.D.Neuroradiologist
Clínica Reina Sofía
Clínica Infantil Santa María del Lago
Fundación Universitaria Sanitas
ECHNR, November 4th, 2020
Paranasal sinus Tumors and tumor like lesions
I have no relevant disclosures for this lecture
• Introduction
• Benign lesions
• Malignant lesions
• Bone lesions
• External lesions
• Take home messages
Paranasal sinus Tumors and tumor like lesions
• Introduction
• Benign lesions
• Malignant lesions
• Bone lesions
• External lesions
• Take home messages
Paranasal sinus Tumors and tumor like lesions
1 2
3 4

03/11/2020
2
• Malignant tumors of the sinonasal tract are extremely rare
• The clinical presentation is non‐specific and often mimics
benign disease
• Delay in diagnosis is common
• 75% of all paranasal sinus tumors are Stage T3 or T4 at the
time of diagnosis
• Treatment depends on histological type, location and
extent
• Prognosis depends on location and stage
Introduction
Loevner L, Radiology Assistant 2009,Koeller K, Head and Neck Pathol, 2016Szewczyk-Bieda et al. Clinical Radiology ,2014
• Considerable overlap in imaging appearance
• Specific manifestations often are lacking
• Virtually all sinonasal tumors requiere histopathology for specific diagnosis
• “It is not about the histology but about answering the question 'is it tumor or not?’” (L Loevner)
Imaging in PNS tumors
• Role of imaging
Imaging in PNS tumors
Identification of the mass
Location and extension
Valuable guide for biopsy and surgical resection
CT• Excellent to determine anatomic landmarks and variants
• Effect of the lesions on adjacent bone structures
• Calcifications
• Density
MR• Distinguishes mass from fluid or mucosal thickening
• Mass characteristics
• Define extension into soft tissues, orbit or intracranial
Introduction
CT and MR are complementaryKoeller K, Head and Neck Pathol, 2016
5 6
7 8

03/11/2020
3
• Bone erosion or remodelling in benign or slowly growing tumors
• Osseous lytic destruction in more aggresive tumors (SCC)
• Bone sclerosis in chronicinflammation, radiation, osteomielitis
• Intratumoral calcifications– True tumoral or residual bone
– In chondroid and fibro‐osseous tumors, olfactory neuroblastoma and invertedpapilloma
CT
Koeller K, Head and Neck Pathol, 2016
• Fluid
• Inflammatory changes
• Low grade tumors
MR
Hypointensity in T2
Hyperintensity in T2
Superior to CT in identifying soft tissue tumor portion
• High cellularity
• Lack of fluid
Secretions do not have solid enhancement. If you have an enhancing mass, you must rule out tumor.
• Define invasion of the skull base
– Replacement of the high signal of the fatty marrow on T1WI by hypointense signal of the tumor
• Review for foraminal extension
– Perineural spread
– Direct invasion of the tumor
• Detect intracranial extension
MR
Loevner, The Radiology Assistant, 2009
• Different protein contents result in different signal intensities on T1 and T2W‐ images
• Fungus – Usually has a high protein content of more than 28%
– Can mimic an aerated sinus: low on T1‐ and T2WI
– You need CT to make the distinction
• Bright signal on T2 is a sign of benign disease– Fluid and mucosal disease usually have a high water content
MR
Loevner, The Radiology Assistant, 2009
9 10
11 12

03/11/2020
4
• Introduction
• Benign lesions
• Malignant lesions
• Bone lesions
• External lesions
• Take home messages
Paranasal sinus Tumors and tumor like lesions
BenignTumors2017 WHO classification
Tatekawa et al, Japanese Journal of Radiology, 2018
Sinonasal papillomas
• Benign epithelial lesions arising from Schneiderian mucosa
• Three subtypes:
– Inverted 62%
– Oncocytic 6%
– Exophytic 32%
• Clinically: nasal obstruction, polyps, epistaxis, hyposmia, headache
Tatekawa et al, Japanese Journal of Radiology, 2018
Inverted papilloma
• The most frequent papilloma
• Inverted growth of the neoplastic epithelium into the underlying stroma
• Most frequent in the 5th and 6th decade
• 2,5 to 3 times more frequent in males
• Locally aggressive, multicentric, malignant transformation
• 1,9‐27% become SCC
Tatekawa et al, Japanese Journal of Radiology, 2018
13 14
15 16

03/11/2020
5
Inverted papillomaImaging
CT
• Location: lateral nasal wall and middle meatus
• Focal hyperostosis at the sites of origin
MR
• Lobulated shape
• Hyper on T2, iso ‐ hypo on T1
• Convoluted cerebriform pattern (CCP)
Tatekawa et al, Japanese Journal of Radiology, 2018
Inverted papillomaImaging
Lee et al, AJNR 2007
CT
• Focal hyperostosis at the site of origin
• Corresponded to site of origin in 89% correlating with surgical findings
• Two patterns
– Plaque like : lateral wall
– Cone shaped : paranasal sinuses and septum
Inverted papillomaImaging
Lee et al, AJNR 2007
Plaque like: lateral wall
Inverted papillomaImaging
Lee et al, AJNR 2007
Cone shaped: paranasal sinuses and septum
17 18
19 20

03/11/2020
6
Inverted papillomaImaging
MR
• Lobulated shape
• Hyper on T2, iso ‐ hypo on T1
• Convoluted cerebriform pattern (CCP)
Jeon et al, AJNR 2008
Inverted papillomaImaging
Convoluted cerebriform pattern (CCP)
• Present in 100% of IP (Jeon 2008)
• Present in 13% of malignant PNS tumors
Jeon et al, AJNR 2008
Inverted papillomaSquamous cellcarcinoma
Inverted papillomaImaging
• Signs that indicate the presence of coexistent SCC
Jeon et al, AJNR 2008
Focal loss of CCP
Necrotic lesion
Invasion to the surrounding tissue
Respiratory epitelial adenomatoidhamartoma ‐ REAH
• Benign neoplasm of the nasal cavity and PNS
• Submucosal glandular proliferation with polypoid appearance
• 3rd to 9th decade, median age is the 6th decade
• Male : female ratio is 7:1
• Most located at the anterior half of the olfactory clefts (OC) or posterior nasal septum
Tatekawa et al, Japanese Jurnal of Radiology, 2018
21 22
23 24

03/11/2020
7
Respiratory epitelial adenomatoidhamartoma ‐ Imaging
CT
• Homogeneous mass
• Enlargment of the OC without bone destruction
MR
• Well delineated soft tissue filling
• Homogeneous contrast enhancement
Tatekawa et al, Japanese Jurnal of Radiology, 2018
REAH‐ Imaging
CT
• Homogeneous mass
• Enlargment of the OC without bone destruction
Tatekawa et al, Japanese Jurnal of Radiology, 2018
Respiratory epitelial adenomatoidhamartoma ‐ Imaging
MR
• Well delineated soft tissue filling
• Homogeneous contrast enhancement
Tatekawa et al, Japanese Jurnal of Radiology, 2018
Other benign lesions
Salivary gland tumors• Pleomorphic adenoma
Benign soft tissue tumors• Leiomyoma (angioleiomyoma)
• Capillary hemangioma
• Cavernous hemangioma
• Schwannoma
Other tumorsMeningiomas
Ectopic pituitary adenoma
Tatekawa et al, Japanese Jurnal of Radiology, 2018
25 26
27 28

03/11/2020
8
Nerve sheat tumors
• Arise from nerve sheath cells
• Schwannomas and neurofibromas
• 25‐40% occur in the H&N
• <4% arise in the sinonasal region
• Usually originate from ophthalmic and maxillary branches of the trigeminal nerve
Koeller, Head and Neck Pathol 2016Szewczyk-Bieda et al, Clinical Radiology 2014
Nerve sheat tumorsCT
• Homogeneous soft‐tissue density
• Can be mistaken for inflammatory polyps or inspissated secretions
MRI• Well‐defined
• Intermediate signal on T1W, variable T2W signal
• Variable enhancement
Koeller, Head and Neck Pathol 2016Szewczyk-Bieda et al, Clinical Radiology 2014
Lobular capillary hemangioma
Szewczyk-Bieda et al, Clinical Radiology 2014
• AKA Granuloma gravidarum (misnomer)
• Capillary proliferation affecting mucous membranes of oral and nasal cavity
• At Kisselbachs plexus at the septum or inferior turbinate
• CT– Enhancing mass with hypoattenuating cap
– Bone destruction or remodelling
• MR– Early enhancement and flow voids
Pleomorphic adenoma
• Epithelial/ myoepithelial and mesenchymal stromal components
• 65% of PAs major salivary glands, 35% of PAs accessory salivary glands
• Nasal cavities and paranasal sinuses only rarely involved
• Intranasal PAs
– 3rd to 6th decade
– Slightly more frequent in females
– 80% of PAs arise in the nasal septal submucosa
– Malignant transformation in 2.4–10%
29 30
31 32

03/11/2020
9
Pleomorphic adenomaImaging
• Multilobulated appearance is one of the key findings
• CT
– Adjacent bony changes (displacement, expanding erosion)
– Intratumoral calcifications
• MR
– Shows iso‐ to hyperintensity on T2, hypointensity on T1
– Heterogeneous curvilinear contrast enhancement
• Clinical and diagnostic tips
– Complete excision is curative
– It is important to identify the origin of intranasal PAs
Benign mass lesion with CE Clinical and diagnostic tips
Tatekawa et al, Japanese Jurnal of Radiology, 2018
33 34
35 36

03/11/2020
10
Clinical and diagnostic tips
• Identify de hyperostotic region of origin to avoid inadecuate resection
• Focal loss of CCP, necrotic lesion, invasion to the surrounding tissue are signs that indicate the presence of coexistent SCC
• Significant widening of the OC (anterior half)
Tatekawa et al, Japanese Jurnal of Radiology, 2018
Inverted papilloma
REAHs
• Introduction
• Benign lesions
• Malignant lesions
• Bone lesions
• External lesions
• Take home messages
Paranasal sinus Tumors and tumor like lesions
Malignant sinonasal tumors
• Nasal and PNS malignancies account for 1% of allmalignancies and 3% of H/N malignancies
• Malignant sinonasal tumors are more frequent thanbenign tumors
• 50% arise in nasal cavity, most of the rest in maxillaryand ethmoid sinuses
• Invasion of adjacent structures affects prognosis
Kawaguchi et al. Journal of Clinical Medicine, 2017Szewczyk-Bieda et al. Clinical Radiology ,2014Koeller K, Head and Neck Pathol, 2016
Malignant sinonasal tumors
Epithelial Non‐epithelial
Squamous cell carcinoma (SCC) Melanoma
Adenoid cystic carcinoma Lymphoma
AdenomaOlfactory neuroblastoma (Estesioneuroblastoma)
Adenocarcinoma Fibrous histiocytoma
Sinonasal Undifferentiated Carcinoma
Sarcomas (rabdomyosarcoma, fibrosarcoma
Fibromixoma, mixoma
37 38
39 40

03/11/2020
11
Squamous cell carcinoma SCC
• Is the most common histological subtype
• Accounts for more than half of all sinonasal malignant tumors
• 6th and 7th decade , male predominance
• Maxillary sinus >> nasal cavity >>ethmoid sinus.
• Formerly linked to cigarette smoking and occupational exposures
• In recent years increased positivity rate for HPV (in 32–62% of all sinonasal SCCs )
• Patients with a HPV‐positive sinonasal SCC have a better prognosis than patients with a HPV‐negative sinonasal SCC
Kawaguchi, J. Clin. Med. 2017
Squamous cell carcinoma SCCImaging
CT• Sinonasal soft tissue mass
with prominent bone destruction
• Invasion of the contralateral sinonasal area, orbital wall, infratemporal fossa, and skull base is sometimes observed
Kawaguchi, J. Clin. Med. 2017
Squamous cell carcinoma SCCImaging
MR• Intermediate signal on T1
• Hypointense on T2 (to liquid)
• Larger tumors are heterogeneous (necrosis, hemorrhage)
• Moderate variable contrast enhancement
• Invasion into the anterior and middle cranial fossae
Kawaguchi, J. Clin. Med. 2017
Squamous cell carcinoma SCCImaging
41 42
43 44

03/11/2020
12
Olfactory neuroblastoma
• AKA esthesioneuroblastoma
• Neuroectodermal tumor
• Any age, with peaks in the 2nd en 6th decades
• Accounts 3‐5% of intranasal neoplasms
• Arise from the specialized sensory neuroepithelial olfactory cells (cribriform plate, superior turbinate, upper third of the nasal septum)
• Direct tumor extension into paranasal sinuses, cribriform plate, skull base, orbit, and intracranial cavity is frequent.
• Cervical lymph node metastasis (20–25%) and distant metastases (10–40%)
Kawaguchi, J. Clin. Med. 2017.Szewczyk-Bieda et al. Clinical Radiology ,2014Koeller K, Head and Neck Pathol, 2016
Olfactory neuroblastoma
CT
• Involves the superior portion of the nasal cavity and ipsilateral ethmoid and maxillary sinuses
• Well defined, homogeneous
• Expansile soft tissue mass
• Homogeneous enhancement
Szewczyk-Bieda et al. Clinical Radiology ,2014Koeller K, Head and Neck Pathol, 2016Kawaguchi, J. Clin. Med. 2017
CT is essential for the evaluation of osseous involvement of the cribriform plate, fovea ethmoidalis, and lamina papyracea.
Olfactory neuroblastoma
MR
• Heterogeneous hypointensity compared to gray matter on T1
• Predominant hyperintensity on T2
• Homogeneous, often intense enhancement
• Commonly invades the orbits and extends intracranially
• Peritumoral cysts along the intracranial portion strongly suggests the diagnosis
Dublin A, Bobinsky M. J Neurol Surg B 2016 Szewczyk-Bieda et al. Clinical Radiology ,2014Koeller K, Head and Neck Pathol, 2016
• Head and neck region is the second most common site for extranodal lymphomas
• NHL is the second most common malignancy in the sinonasal tract after SCC.
• 6th 8th decade
• Male‐to‐female ratio 2:1
• Diffuse large B‐cell lymphoma (DLBCL) : maxillary sinus the most common site although may arise from the nasal cavity.
• NK/T‐cell lymphoma most commonly involves the nasal cavity
• B‐cell lymphoma has a better prognosis than T‐cell lymphoma.
Lymphoma
Kawaguchi, J. Clin. Med. 2017
45 46
47 48

03/11/2020
13
CT
• Infiltrative or permeative bone changes
• Varying degrees of bone destruction
• Resorption or remodeling may be accompanied by sclerosis
MR
• NHLs: isointense on T1, slightly hyperintense on T2
• ADC lower than SCCs
• Usually homogeneously enhanced mass
• Necrotic areas within the tumor are occasionally observed in NK/T‐cell lymphoma
LymphomaImaging
Kawaguchi, J. Clin. Med. 2017
Lymphoma
Case courtesy : Camilo Caicedo
Lymphoma
Case courtesy : Camilo Caicedo
• Introduction
• Benign lesions
• Malignant lesions
• Bone lesions
• External lesions
• Take home messages
Paranasal sinus Tumors and tumor like lesions
49 50
51 52

03/11/2020
14
Osseous and fibroosseous lesions
• Comprise nearly 25 % of nonepithelial tumors involving the sinonasal cavities
• Are very common incidental findings
• Often misinterpreted as tumor
• CT is usually diagnostic
Osseous and fibroosseous lesions
Most common skull base lesion
Fibrous dysplasia
Followed by osteomas
OsteomasUsually located in the sino‐nasal cavities
Fibromas Less common Can be
ossifying or non‐ossifying
Malignancies Are rare
Fibrous displasia
• Enfermedad idiopática, asintomática.
• En senos paranasales se asocia a obstrucción de vías de drenaje.
• Reemplazo de hueso medular por tejido fibrosoinmaduro, puede dar apariencia en vidrio esmerilado.
• Enfermedad poliostótica se asocia a síndrome deMcCune Albright (manchas café con leche y pubertad precoz).
• Enfermedad monostótica afecta principalmentela base del cráneo.
Fibrous displasia
Case courtesy : Camilo Caicedo
53 54
55 56

03/11/2020
15
Osteoma
• Benign intraosseous proliferation of mature bone with predominant lamellar structure
• In 1% of individuals
• 5th‐6th decade
• M:F ratio 1.3‐2:1
• Most common within the frontal sinuses
• Followed by ethmoid sinuses
• Rarely involve maxillary or sphenoid sinuses
• Arises from the sinus wall
Schuknecht B, ECNR Antwerp, 2017
Osteoma• Osteoma is primarily composed
of mature bone similar to normal bone apart from increased bony elements and decreased marrow
• Hyperdense on CT
• Well defined
• May be completely inconspicuous on non‐contrast MRI
• Heterogeneous low‐to‐intermediate signal intensity
• Some Gd enhancement
Gupta et al, 2018Schuknecht B, ECNR Antwerp, 2017
Osteoblastoma
• Fibrous elements and osteoblasts
• Expansile
• Sclerotic or mixed lesion, cortical shell
• Frontoethmoid, orbit or jaw
• 2nd decade
• More frequent in males
Kim J, Kwon S. Medicine, 2017.Schuknecht B, ECNR Antwerp, 2017
Malignant bone lesions
Chondrosarcoma
• Origin in hyalina cartilage
• Lobulated, myxoid changes
• Osteolysis, cortical destruction
• Good prognosis with complete resection
Schuknecht B, ECNR Antwerp, 2017
Osteosarcoma
• Malignancy producing osteoid or bone
• Lobulated
• Lytic‐mixed or sclerotic lesion
57 58
59 60

03/11/2020
16
• Benign expansive and locally agressive bone lesionLesión ósea Middle aged women
• Frequently monostotic involvement of sphenoid or ethmoid bone
• Less frequent in maxilary sinus
• Well defined, central area of soft tissue density, surrounded by sclerotic border
• Always look for orbital and dental involvement
Ossifying fibroma
• Introduction
• Benign lesions
• Malignant lesions
• Bone lesions
• External lesions
• Take home messages
Paranasal sinus Tumors and tumor like lesions
• CNS tumors
– Direct extension or due to embriologic remnants
– Include meningioma, craniopharyngioma, chordoma and nasal glioma
• Juvenile nasoangiofibroma
• Pituitary adenoma
External lesions
61 62
63 64

03/11/2020
17
• Malignant tumors of the NC and PNS are rare
• Clinical findings are non specific
• Role of imaging is
• CT and MR are complementary
Take home messages
Identification of the mass
Location and extension
Valuable guide for biopsy and surgical resection
• Always keep tumor and tumor like lesions in mind when reporting PNS
• Be familiar with the imaging characteristics of
– Inverted papilloma
–Osteoma
–SSC
–Olfactory neuroblastoma
Take home messages
65 66
67