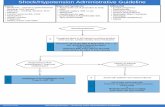
2 Unstable : Altered mental status Ischemic chest discomfort Acute heart failure Hypotension ...
-
Upload
rodger-hall -
Category
Documents
-
view
221 -
download
0
Transcript of 2 Unstable : Altered mental status Ischemic chest discomfort Acute heart failure Hypotension ...

BRADYCARDIA & TACHYCARDIA

2

Bradycardia & Tachycardia
3
ARRHYTHMIA
Unstable : Altered mental status Ischemic chest discomfort Acute heart failure Hypotension Other signs of shock
Symptomatic: Palpitations Lightheadedness Dyspnea
07/07/1392

Bradycardia & Tachycardia
4
BRADYCARDIA IS DEFINED AS
A heart rate of <60 beats per minute.
When bradycardia is the cause of symptoms, the rate is generally <50 beats per minute, which is the working definition of bradycardia used here.
07/07/1392

Bradycardia & Tachycardia
5
BRADYCARDIA ALGORITHM FOCUSES ON
Management of
clinically significant bradycardia.
07/07/1392

07/07/1392

Bradycardia & Tachycardia
7
INITIAL EVALUATION OF ANY PATIENT WITH BRADYCARDIA:
Should focus on : signs of increased work of breathing
Tachypnea Intercostal retractions Suprasternal retractions Paradoxical abdominal breathing
oxyhemoglobin saturation as determined by pulse oximetry.
07/07/1392

Bradycardia & Tachycardia
8
IF OXYGENATION IS INADEQUATE OR THE PATIENT SHOWS SIGNS OF INCREASED WORK OF BREATHING
Provide supplementary oxygen
Attach a monitor to the patient
Evaluate blood pressure
Establish IV access.
If possible, obtain a 12-lead ECG to better define the rhythm.
07/07/1392

07/07/1392

Bradycardia & Tachycardia
10
ASYMPTOMATIC OR MINIMALLY SYMPTOMATIC PATIENTS
Do not necessarily require treatment
Unless: There is suspicion that the rhythm is likely
to progress to symptoms Or become life-threatening (eg, Mobitz type
II second-degree AV block in the setting of acute myocardial infarction [AMI])
07/07/1392

Bradycardia & Tachycardia
11
IF THE BRADYCARDIA
Is suspected to be the cause of: Acute altered mental status Ischemic chest discomfort Acute heart failure Hypotension Or other signs of shock
The patient should receive immediate treatment
07/07/1392

Bradycardia & Tachycardia
12
07/07/1392
Immediate treatment

Bradycardia & Tachycardia
13
SINUS BRADYCARDIA:
07/07/1392

Bradycardia & Tachycardia
14
ATRIOVENTRICULAR (AV) BLOCKS:
Are classified as: First Second Third-degree
Blocks may be caused by :Medications Electrolyte disturbancesStructural problems resulting from AMI or othermyocardial diseases
07/07/1392

Bradycardia & Tachycardia
15
FIRST-DEGREE AV BLOCK:
07/07/1392

Bradycardia & Tachycardia
16
SECOND-DEGREE AV BLOCK:
Is divided into Mobitz types I and II Mobitz types I:
07/07/1392

Bradycardia & Tachycardia
17
MOBITZ TYPES II:
07/07/1392

Bradycardia & Tachycardia
18
THIRD DEGREE AV BLOCK:
07/07/1392

Bradycardia & Tachycardia
19
THERAPY:
Atropine remains the first-line drug for acute symptomatic bradycardia
Atropine : Should be considered a temporizing measure
while awaiting a transcutaneous or transvenous pacemaker
For patients with Symptomatic sinus bradycardia Conduction block at the level of the AV node Sinus arrest.
07/07/1392

Bradycardia & Tachycardia
20
CONT. ATROPINE:
The recommended dose is: 0.5 mg IV every 3 to 5 minutes to a
maximum total dose of 3 mg.
Doses of ‹0.5 mg may paradoxically result in further slowing of the heart rate
07/07/1392

Bradycardia & Tachycardia
21
CONT. ATROPINE:
Use atropine cautiously in the presence of acute coronary ischemia or MI
Increased heart rate may worsen ischemia or increase infarction size.
07/07/1392

Bradycardia & Tachycardia
22
CONT. ATROPINE:
Atropine will likely be :
Ineffective in patients who have undergone cardiac transplantation
Because the transplanted heart lacks vagal innervation
07/07/1392

Bradycardia & Tachycardia
23
CONT. ATROPINE:
Avoid relying on atropine in : Type II second-degree or third degree AV block
These bradyarrhythmias are not likely to be responsive to reversal of cholinergic effects by atropine
These are preferably treated with TCP or adrenergic support as temporizing measures while the patient is prepared for transvenous pacing
07/07/1392

Bradycardia & Tachycardia
24
PACING:
TCP may be useful for the treatment of symptomatic bradycardias
TCP is, at best, a temporizing measure
TCP is painful in conscious patients whether effective or not :
The patient should be prepared for transvenous pacing
And expert consultation should be obtained.
07/07/1392

Bradycardia & Tachycardia
25
CONT. PACING:
It is reasonable to initiate TCP in unstable patients who do not respond to atropine
Immediate pacing might be considered in unstable patients with high-degree AV block when IV access is not available
If the patient does not respond to drugs or TCP, transvenous pacing is probably indicated
07/07/1392

Bradycardia & Tachycardia
26
ALTERNATIVE DRUGS TO CONSIDER: Although not first-line agents for
treatment of symptomatic bradycardia: Dopamine Epinephrine Isoproterenol
Use alternatives when a bradyarrhythmia is : Unresponsive to or inappropriate for treatment with
atropine, Or as a temporizing measure while awaiting the
availability of a pacemaker.
07/07/1392

Bradycardia & Tachycardia
27
DOPAMINE:
Dopamine infusion may be used for : Patients with symptomatic bradycardia Particularly if associated with:
Hypotension, In whom atropine may be inappropriate Or after atropine fails
Begin dopamine infusion at 2 to 10 mcg/kg per minute and titrate to patient response.
07/07/1392

Bradycardia & Tachycardia
28
EPINEPHRINE:
Epinephrine infusion may be used for: Patients with symptomatic bradycardia Particularly if associated with:
Hypotension Whom atropine may be inappropriate After atropine fails
Begin the infusion at 2 to 10 mcg/min and titrate to patient response
07/07/1392

Bradycardia & Tachycardia
29
ISOPROTERENOL:
The recommended adult dose is 2 to 10 mcg/ min by IV infusion, titrated according to heart rate and rhythm response
07/07/1392

Bradycardia & Tachycardia
30
07/07/1392

07/07/1392

Bradycardia & Tachycardia
32
TACHYARRHYTHMIA
07/07/1392

Bradycardia & Tachycardia
33
TACHYCARDIA IS DEFINED AS :
An arrhythmia with a rate of 100 beats per minute
As with defining bradycardia: Rate of 150 beats per minute is more
likely attributable to an arrhythmia
07/07/1392

Bradycardia & Tachycardia
34
PRIMARY OR SECONDARY CAUSE: Fever Dehydration Other underlying conditions
When a heart rate is <150 beats per minute: It is unlikely that symptoms of instability
are caused primarily by the tachycardia
07/07/1392

Bradycardia & Tachycardia
35
INITIAL EVALUATION OF ANY PATIENT WITH TACHYCARDIA:
Should focus on : signs of increased work of breathing
Tachypnea Intercostal retractions Suprasternal retractions Paradoxical abdominal breathing
oxyhemoglobin saturation as determined by pulse oximetry.
07/07/1392

Bradycardia & Tachycardia
36
IF OXYGENATION IS INADEQUATE OR THE PATIENT SHOWS SIGNS OF INCREASED WORK OF BREATHING
Provide supplementary oxygen
Attach a monitor to the patient
Evaluate blood pressure
Establish IV access.
If possible, obtain a 12-lead ECG to better define the rhythm.
07/07/1392

07/07/1392

Bradycardia & Tachycardia
38
IF SIGNS AND SYMPTOMS PERSIST:
The provider should assess the patient’s degree of instability and determine if the instability is related to the tachycardia
07/07/1392

Bradycardia & Tachycardia
39
IF THE TACHYCARDIA:
Is suspected to be the cause of: Acute altered mental status Ischemic chest discomfort Acute heart failure Hypotension Or other signs of shock
The patient should receive immediate syn- chronized cardioversion
07/07/1392

Bradycardia & Tachycardia
40
IF NOT HYPOTENSIVE:
The patient with a regular narrow-complex : May be treated with adenosine while
preparations are made for synchronized cardioversion
07/07/1392

07/07/1392

07/07/1392

Bradycardia & Tachycardia
43
CARDIOVERSION:
If possible: Establish IV access before cardioversion Administer sedation if the patient is
conscious
Do not delay cardioversion if the patient is extremely unstable
07/07/1392

Bradycardia & Tachycardia
44
CONT. CARDIOVERSION:
Synchronized Cardioversion
Vs
Unsynchronized Shocks(defibrillation)
07/07/1392

Bradycardia & Tachycardia
45
CONT. CARDIOVERSION:
Synchronized cardioversion is recommended to treat : Unstable SVT Unstable atrial fibrillation Unstable atrial flutter Unstable monomorphic (regular) VT
07/07/1392

Bradycardia & Tachycardia
46
WAVEFORM AND ENERGY:
Biphasic energy dose for cardioversion of : Atrial fibrillation is 120 to 200 J
Atrial flutter and other SVTs 50 J to 100 J
Monomorphic VT (regular form and rate) with a pulse 100 J If there is
07/07/1392

Bradycardia & Tachycardia
47
WAVEFORM AND ENERGY:
Polymorphic VT : Treat as VF deliver high-energy
unsynchronized shocks (defibrillation doses)
Any doubt whether monomorphic or polymorphic VT in the unstable patient : Defibrillation doses
07/07/1392

Bradycardia & Tachycardia
48
IF THE PATIENT WITH TACHYCARDIA IS STABLE:
The provider has time to : Obtain a 12-lead ECG Evaluate the rhythm Determine the width of the QRS complex Determine treatment options.
Stable patients may await expert consultation
07/07/1392

07/07/1392

Bradycardia & Tachycardia
50
CLASSIFICATION OF TACHYARRHYTHMIAS
Appearance of the QRS complex Heart rate Regularity
07/07/1392

Bradycardia & Tachycardia
51
THERAPY:
Vagal maneuvers: Valsalva maneuver or carotid sinus massage
Adenosine: If PSVT does not respond to vagal maneuvers Give 6 mg of IV adenosine as a rapid IV push
through a large vein followed by a 20 mL saline flush
Calcium Channel Blockers and B-Blockers: Verapamil, Diltiazem, Metoprolol,Atenolol,
Propranolol,
07/07/1392

Bradycardia & Tachycardia
52
SINUS TACHYCARDIA
07/07/1392

Bradycardia & Tachycardia
53
PAROXYSMAL SUPRAVENTRICULAR TACHYCARDY(PSVT):
07/07/1392

Bradycardia & Tachycardia
54
ATRIAL FLUTTER
07/07/1392

Bradycardia & Tachycardia
55
ATRIAL FIBRILLATION
07/07/1392

Bradycardia & Tachycardia
56
MULTIFOCAL ATRIAL TACHYCARDIA
07/07/1392

Bradycardia & Tachycardia
57
WIDE–QRS-COMPLEX TACHYCARDIAS: Ventricular tachycardia (VT) Ventricular fibrillation(VF) SVT with aberrancy Pre-excited tachycardias (Wolff-
Parkinson-White syndrome) Ventricular paced rhythms
07/07/1392

Bradycardia & Tachycardia
58
THERAPY:
Determine if the rhythm is regular or irregular
A regular wide-complex tachycardia: Adenosine Procainamide Amiodarone Sotalol Cardioversion
An irregular wide-complex tachycardia: Procainamide Amiodarone Magnesium Isoproterenol Cardioversion
07/07/1392

Bradycardia & Tachycardia
59
VENTRICULAR TACHYCARDIA (VT)
07/07/1392

Bradycardia & Tachycardia
60
VENTRICULAR FIBRILLATION(VF)
07/07/1392

Bradycardia & Tachycardia
61
WPW
07/07/1392

Bradycardia & Tachycardia
62
POLYMORPHIC VT(TORSADES DE POINTES)
07/07/1392

Bradycardia & Tachycardia
63
07/07/1392

Bradycardia & Tachycardia
64
THE END
07/07/1392
















![Intradialytic hypotension [투석 중 저혈압]](https://static.fdocuments.net/doc/165x107/558406e7d8b42a6a148b4edc/intradialytic-hypotension--5584b8e435e7e.jpg)