1 Are Changing Rates of Admission for Chronic Medical Conditions Simply a Reflection of Changes in...
-
Upload
ambrose-kory-thompson -
Category
Documents
-
view
215 -
download
1
Transcript of 1 Are Changing Rates of Admission for Chronic Medical Conditions Simply a Reflection of Changes in...
1
Are Changing Rates of Admission for Chronic Medical Conditions Simply a Reflection of Changes in the Demographics, Health Status and Geographic Migration Patterns of the Elderly?
P.O. Box 12194 · 3040 Cornwallis Road · Research Triangle Park, NC 27709Phone: 202-728-1968 · Fax: 202-728-2095 · [email protected] · www.rti.org
RTI International is a trade name of Research Triangle Institute.
Presented at:the AcademyHealth 2004 Annual Research Meeting, San Diego, CA, June 6–8, 2004
Presented by: Nancy McCall, Sc.D.
2
Acknowledgements
Lee Mobley, Ph.D.
Sujha Subramanian, Ph.D.
Erica Brody, M.P.H.
Mary Kapp, M. Phil
3
Research Question
What is the influence of beneficiary sociodemographic and health status characteristics on the rate of growth of ACSC admissions?
4
Data
Rates of ACSC admissions and average health status of the Medicare FFS population 1992–2000 MQMS Base Analytic Files
Rates of Emergency Room or observation bed stays 1992–2000 Outpatient SAFS
Estimates of the proportion of the Medicare population with specific attributes of interest 1992–2000 MQMS Base Denominator Files
5
Methods
Full Year Part A and B Medicare FFS, including deceased
Age 65 and older and residing in U.S.
Approximately 25 million per year
Defined two ACSCs for beneficiaries with diabetes
Health status measured using the PIP-DCG predictive expenditure model
Age-sex Adjusted to July 1, 1999 FFS Population using direct standardization
6
All Cause Hospitalization Rates
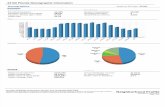
Trend in Age-Sex Adjusted All Cause Admissions (per thousand) Medicare FFS Beneficiaries: 1992-2000
1992 1994 1996 1998 2000% Change 1992–2000
317 316 323 331 336 + 6.0
7
% Change in Inpatient and Outpatient Age-Sex Adjusted Rates for Eleven Selected ACSCs, 1992-2000
Inpatient Outpatient
Cellulitis 12.0 47.0
Asthma -30.0 14.1
COPD 52.2 33.6
Dehydration 20.9 92.7
CHF 0.7 19.8
Acute diabetic events* -6.0 80.7
Lower Limb PVD -23.4 38.0
Pneumonia 14.1 46.8
Septicemia 11.0 51.4
Stroke -14.2 0.20
UTI 12.9 25.3
8
Empirical Model
ACSCjt = f (OUTPATjt, SOCIOjt, HEALTHjt, GEO, YEAR, TIMEt)
ACSCjt = rate of inpatient admissions for the specific ACSC in year t and region j, where each state is divided into one MSA and one non-MSA region;
OUTPAT is rate of ER/observation bed stays for the specific ACSC in year t and region j;
SOCIO = a vector of yearly beneficiary demographic characteristics aggregated to each region;
HEALTH = a yearly health status measure aggregated to each region;
9
Empirical Model
ACSCjt = f (OUTPATjt, SOCIOjt, HEALTHjt, GEO, YEAR, TIMEt)
GEO = a set of census region dummy variables;
YEAR = a set of dummy variables for each year 1993–2000 Interacted with two variables — median age and
outpatient rates
TIME is a continuous time variable — 1993…2000
10
Empirical Model
Three chronic ACSCs: Lower limb peripheral vascular disease (PVD) COPD CHF
Independent variables in the SOCIO vector are specified as proportions, except for the median age
Health status is represented as the median of the PIP-DCG risk score of the population for the year.
For PVD, we add the number of Medicare beneficiaries with diabetes in the prior year
11
Trend Analysis: Methods
We pool the cross sections for each year 1993–2000
We separate inpatient stays from ER/observation bed stays
We aggregate ACSC admissions to MSA and non-MSA regions within states
We tested whether the same relationships exist in MSA and non-MSA subsets of the data, and find they are significantly different
12
Trend Analysis: Methods
We first estimated a simple model with a continuous time variable as the only regressor and found a significant positive trend.
We then stepped in beneficiary demographics, health status and dummy variables for 9 Census divisions
We interacted median age with time and ER/observation bed stays with time to examine whether there are time varying associations
13
Trend Analysis: Time Trend and Variation Explained
Inpatient PVD Rate
Inpatient COPD Rate
Inpatient CHF Rate
Variable MSANon-MSA MSA
Non-MSA MSA
Non-MSA
Continuous Time Variable –
Adjusted R2 40% 38% 66% 75% 82% 71%
Number of Observations 408 400 408 400 408 400
14
Trend Analysis: Demographics
Inpatient PVD Rate
Inpatient COPD Rate
Inpatient CHF Rate
Variable MSANon-MSA MSA
Non-MSA MSA
Non-MSA
Demographics
Proportion Died + + –
Proportion Dual Enrolled in Medicaid – + +
Proportion Men + +
Proportion Black – – +
Proportion with ESRD + – + +
15
Trend Analysis: Median Age and Time
Inpatient PVD Rate
Inpatient COPD Rate
Inpatient CHF Rate
Variable MSANon-MSA MSA
Non-MSA MSA
Non-MSA
Median Age of Medicare FFS Population of each study year interacted with Time Dummy for the year
1993 Median Age *1993 – –
1994 Median Age *1994 – – +
1995 Median Age *1995 + – – – +
1996 Median Age *1996 + – – – +
1997 Median Age *1997 + – – +
1998 Median Age *1998 + – – +
1999 Median Age *1999 + – – +
2000 Median Age *2000 + – – +
16
Trend Analysis: Health Status
Inpatient PVD Rate
Inpatient COPD Rate
Inpatient CHF Rate
Variable MSANon-MSA MSA
Non-MSA MSA
Non-MSA
Health Status
Median PIP-DCG Risk Score + + +
Lag Number of Diabetics – NI NI NI NI
17
Trend Analysis: ER Visit and Time
Inpatient PVD Rate
Inpatient COPD Rate
Inpatient CHF Rate
Variable MSANon-MSA MSA
Non-MSA MSA
Non-MSA
Year Interacted with ER Visit Rate
1993 ER Visit Rate *1993 + +
1994 ER Visit Rate *1994 + +
1995 ER Visit Rate *1995 +
1996 ER Visit Rate *1996 + + +
1997 ER Visit Rate *1997 – + +
1998 ER Visit Rate *1998 – + + +
1999 ER Visit Rate *1999 + + + +
2000 ER Visit Rate *2000 – + + +
18
Trend Analysis: Population Migration
Inpatient PVD Rate
Inpatient COPD Rate
Inpatient CHF Rate
Variable MSANon-MSA MSA
Non-MSA MSA
Non-MSA
Population Migration Patterns
Change in Size of Medicare FFS Beneficiary Population from Current Year to Prior Year
– –
19
Trend Analysis: Census Divisions
Inpatient PVD Rate
Inpatient COPD Rate
Inpatient CHF Rate
Variable MSANon-MSA MSA
Non-MSA MSA
Non-MSA
Set of Dummy Variables for Each Census Division (New England is Reference Division)
Middle Atlantic + + + + +
East North Central + + + +
West North Central – + + – +
South Atlantic + + +
East South Central + + + +
West South Central + +
Mountain – – –
Pacific – – –
20
Conclusions: Trend Analysis
Positive trends in the raw rates over time are substantially explained by demographic-specific factors
Little evidence of substitution of ER for hospitalization for COPD and CHF; some evidence of substitution for lower limb PVD
Rural areas that experienced outbound migration experienced a decline in admission for COPD and CHF
21
Conclusions: Trend Analysis
Observed variation in direction and strength of relationship between explanatory factors and selected chronic conditions suggests that interventions employed to reduction hospitalizations may have to be tailored to the underlying condition
Unexplained geographic variation in hospitalization rates for all three chronic conditions remain